Escolar Documentos
Profissional Documentos
Cultura Documentos
X Ray
Enviado por
jalimeeDireitos autorais
Formatos disponíveis
Compartilhar este documento
Compartilhar ou incorporar documento
Você considera este documento útil?
Este conteúdo é inapropriado?
Denunciar este documentoDireitos autorais:
Formatos disponíveis
X Ray
Enviado por
jalimeeDireitos autorais:
Formatos disponíveis
Education
Chest x rays made easy
In the third of a five part series, Elizabeth Dick looks at abnormalities of the lung fields
The basics of looking at a chest x ray (recap):
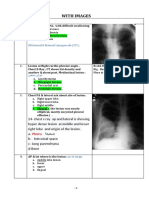
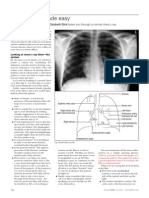
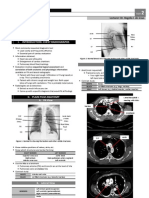
First look at the mediastinal contoursrun your eye down the left side of the patient and then up the right. The trachea should be central. The aortic arch is the first structure on the left, followed by the left pulmonary artery; notice how you can trace the pulmonary artery branches fanning out through the lung (see figure 1). Two thirds of the heart lies on the left side of the chest, with one third on the right. The heart should take up no more than half of the thoracic cavity. The left border of the heart is made up by the left atrium and left ventricle. The right border is made up by the right atrium alone. Above the right heart border lies the edge of the superior vena cava. The pulmonary arteries and main bronchi arise at the left and right hila. Enlarged lymph nodes can also occur here, as can primary tumours. These make the hilum seem bulkynote the normal size of the hila on this film. Now look at the lungs. Apart from the pulmonary vessels (arteries and veins), they should be black (because they are full of air). Scan both lungs, starting at the apices and working down, comparing left with right at the same level, just as you would when listening to the chest with your stethoscope. The lungs extend behind the heart, so look here too. Force your eye to look at the periphery of the lungsyou should not see many lung markings here; if you do then there may be disease of the air spaces or interstitium. Dont forget to look for a pneumothorax. Make sure you can see the surface of the hemidiaphragms curving downwards, and that the costophrenic and cardiophrenic angles are not bluntedsuggesting an effusion. Check there is no free air under the hemidiaphragm. Finally, look at the soft tissues and bones. Are both breast shadows present? Is there a rib fracture? This would make you look even harder for a pneumothorax. Are the bones destroyed or sclerotic?
Fig 1 Right pneumothorax. The right side of the lung is blacker, and the lung edge is seen (arrow). There is no mediastinal shift and therefore no tension
One half of the lung may seem blackerthat is, more radiolucent than the other, which will be more radio-opaque or whiter. In particular, the area beyond the collapsed lung will be very radiolucent because there are no pulmonary vessel markings. You should be able to identify the edge of the collapsed lung (see fig 1).
Pneumothorax
It is important to view around the periphery of the lungs to look for a pneumothorax (air in the pleural space with associated collapsed lung). It is very easy to miss a pneumothorax. Watch out for the following signs: Having identified a pneumothorax you need to look for several more associated abnormalities: Most importantlythis is a pass or fail observationis there evidence of a tension pneumothorax? This occurs
when air can enter the pleural space (via a hole in the lung surface or the chest wall) but, because of a ball-valve effect, air cannot leave by the same route. So more and more air accumulates in the pleural space. This pushes the mediastinum over to the opposite (normal) side and eventually compresses the normal lung so that less inspiration occurs on the normal side, with compression on the heart and decreased venous return until finally the patient arrests (see fig 2). Always look for this and say: There is no shift of the mediastinum and therefore no tension pneumothorax or There is
408
STUDENT BMJ VOLUME 8
NOVEMBER 2000
studentbmj.com
Education
shift of the mediastinum away from the side of the pneumothorax indicating a (right/left) tension pneumothorax. This is a medical emergency which I would treat immediately by inserting a large bore cannula into the (right/left) pleural space. The cause of the pneumothorax may be apparentfor example, fracture of the ribs. There may be associated surgical emphysemathat is, air in the soft tissuesand air in the mediastinum (see fig 3).
There is extra shadowing in the lungs
It may be difficult to work out what is causing extra shadowing in the lungs, especially near the mediastinum where normal structures may overlay the extra shadowing. It is useful to look at the periphery of the lungs because normally the outermost edge of the lungs should be fairly black with a few tapering blood vessels. If you do see more shadowing in the periphery then there may be either interstitial or air space disease. As examiners often show films with one of these two types of shadowing, understanding the difference between these two is worth while because it will help you to interpret what you see and lead you to the correct differential diagnosis. The lung is made up of bronchi, which branch, at the end of which are alveoli. The interstitial space (or potential space) surrounds the alveoli. The whole of the lung
Fig 2 Left tension pneumothorax with shift of the mediastinum to the right. The lung edge is arrowed
Fig 3 Surgical emphysema (arrow) and pneumomediastinum (arrowhead)
from bronchi to alveoli is the air space that is, it normally contains air. But the air spaces can fill upwith fluid (such as in severe pulmonary oedema), with pus (as in infection), with blood (as in rare diseases such as Goodpastures syndrome, associated with renal failure), or with tumour cells (alveolar carcinoma). Fluid and pus are more common than the second two. When the air spaces fill up, the alveoli fill first, with the bronchi being relatively spared. Therefore the bronchi, which are still air filled, stand out against the alveoli, which are filled with pus or fluid. This is called an air bronchogram and is simply a sign that there is air space disease. Consolidation is another term for air space shadowing (see figs 4 and 5). If there is air space disease then you need to work out which part of the lungs it is affecting. A quick way is to use the word zone to describe which part of the lung is affected. Say something like There is shadowing in the air spaces of the right mid and lower zone. You can then take your time to work out which lobe is affected. You can
STUDENT BMJ VOLUME 8
NOVEMBER 2000
studentbmj.com
409
Education
Fig 4 Left and right lower lobe air space shadowing in an ITU patient
find out more about lobar anatomy in the later section on collapse and consolidation. Lets turn to the interstitial space. This surrounds bronchi, vessels, and groups of alveoli. When there is disease in the interstitium it manifests itself by reticulonodular shadowing (criss cross lines or tiny nodules or both). The main two processes affecting the interstitium are accumulation of fluid (occurring in pulmonary oedema or in lymphangitis carcinomatosa) and inflammation leading to fibrosis (occurring in industrial lung disease, inflammatory arthritides such as rheumatoid arthritis, inflammation of unknown cause such as cryptogenic fibrosing alveolitis and sarcoidosis). If you see criss cross lines or tiny nodules or both say: There is reticulo-nodular shadowing within the lower zones. (See figure 6.) Use the table to work out whether the extra shadowing you can see is air space or interstitial. Next month: we will look at collapse, consolidation, and pleural effusions. I would like to thank Dr Anju Sahdev, Dr Brian Holloway, and Dr Robert Dick for contributing some of the films which are illustrated.
Elizabeth Dick, specialist registrar in radiology, North Thames Deanery
Fig 6 Recticular-nodular shadowing caused by lung fibrosis (circled). Note how the heart has lost its normal smooth outline and seems shaggy
Features of air space and interstitial lung disease
Air space disease
Zones Appearances Causes (differential diagnoses) Any Confluent shadowing Air bronchograms Fluid (pulmonary oedema, adult respiratory distress syndrome) Pus (infection/consolidation) Blood (Goodpastures syndrome) Tumour cells (alveolar cell carcinoma)
Interstitial lung disease
Any Linear/reticular/nodular shadowing Fluid (pulmonary oedema/ lymphangitis carcinomatosa) Inflammation leading to fibrosis (industrial lung disease, inflammatory arthritides, inflammation of unknown cause, sarcoid)
Fig 5 Right middle and lower zone consolidation/air space shadowing. Note air bronchogram (arrow). There is no loss of volume, which is a key feature of consolidation
Erratum: see p407. See Web Extra at studentbmj.com for our web-based x ray quiz
410
STUDENT BMJ VOLUME 8
NOVEMBER 2000
studentbmj.com
Você também pode gostar
- ABC of Reading Chest XrayDocumento1 páginaABC of Reading Chest Xraykrisnochura100% (3)
- Respiratory PhysiologyDocumento30 páginasRespiratory PhysiologyBarbara Sakura RiawanAinda não há avaliações
- Chest PDFDocumento95 páginasChest PDFsherief maroufAinda não há avaliações
- Aortic DissectionDocumento49 páginasAortic DissectionAnonymous ZUaUz1wwAinda não há avaliações
- Atelectasis, (Lung Collapse) A Simple Guide To The Condition, Diagnosis, Treatment And Related DiseasesNo EverandAtelectasis, (Lung Collapse) A Simple Guide To The Condition, Diagnosis, Treatment And Related DiseasesAinda não há avaliações
- Abdominal Xray Interpretation and Cases For FinalsDocumento39 páginasAbdominal Xray Interpretation and Cases For Finalsfahadrock2002Ainda não há avaliações
- Pleural Effusion, A Simple Guide To The Condition, Treatment And Related ConditionsNo EverandPleural Effusion, A Simple Guide To The Condition, Treatment And Related ConditionsAinda não há avaliações
- CXR Made Easy PDFDocumento14 páginasCXR Made Easy PDFyourdirtysocksAinda não há avaliações
- Guide To Clerking 2014Documento24 páginasGuide To Clerking 2014Ridhwan Amid100% (1)
- Interpretation Chest X RayDocumento127 páginasInterpretation Chest X RayVimal NishadAinda não há avaliações
- Basic Interpretation of CXRDocumento84 páginasBasic Interpretation of CXRHaluk AlibazogluAinda não há avaliações
- Barium StudyDocumento34 páginasBarium StudyJahanavi JaluAinda não há avaliações
- Mitral Valve Prolapse, Flailed Mitral Valve Mitral Annular CalcificationDocumento33 páginasMitral Valve Prolapse, Flailed Mitral Valve Mitral Annular CalcificationcafemedAinda não há avaliações
- CHEST X-RAY Presentation CVSDocumento45 páginasCHEST X-RAY Presentation CVSNorsafrini Rita Ahmad100% (1)
- Echo Facts IndexDocumento3 páginasEcho Facts Indexs336336anl100% (1)
- Medico Notes PediatricsDocumento40 páginasMedico Notes PediatricsTrisAinda não há avaliações
- Pediatric Respiratory Distress GuidelinesDocumento1 páginaPediatric Respiratory Distress GuidelinesRick FreaAinda não há avaliações
- CXR Lecture DR Lenora FernandezDocumento70 páginasCXR Lecture DR Lenora Fernandezapi-19431894100% (1)
- Chest RadiographyDocumento39 páginasChest RadiographyBikram PaulAinda não há avaliações
- Chest Radiology: Alex Nguyen FSU College of Medicine MS4Documento62 páginasChest Radiology: Alex Nguyen FSU College of Medicine MS4First Last100% (1)
- (RADIO 250) LEC 06 Chest RadiologyDocumento10 páginas(RADIO 250) LEC 06 Chest Radiologyjmhinos4833Ainda não há avaliações
- Classic Imaging Signs of Congenital Cardiovascular Abnormalities 1Documento45 páginasClassic Imaging Signs of Congenital Cardiovascular Abnormalities 1adhik_deepakAinda não há avaliações
- Interpreting The Chest Radio Graph Friendly)Documento9 páginasInterpreting The Chest Radio Graph Friendly)Vagner BorgesAinda não há avaliações
- Patho Tree COPDDocumento1 páginaPatho Tree COPDLaura MitchellAinda não há avaliações
- 14 - Barium Studies For GIT With NotesDocumento50 páginas14 - Barium Studies For GIT With NotesSunil ThomasAinda não há avaliações
- Plain Chest X RayDocumento154 páginasPlain Chest X RaySamuel Gamadey100% (3)
- A Simple Guide to Pneumothorax (Collapsed Lungs), Diagnosis, Treatment and Related ConditionsNo EverandA Simple Guide to Pneumothorax (Collapsed Lungs), Diagnosis, Treatment and Related ConditionsAinda não há avaliações
- CXR Made EasyDocumento14 páginasCXR Made Easyjaimejm100% (1)
- Cardiac RadiologyDocumento10 páginasCardiac RadiologyHaluk AlibazogluAinda não há avaliações
- Cardiac RadiologyDocumento10 páginasCardiac RadiologyHaluk AlibazogluAinda não há avaliações
- Rheumatoid Arthritis Associated Scleritis OPHTHALMOLOGY MCQSDocumento5 páginasRheumatoid Arthritis Associated Scleritis OPHTHALMOLOGY MCQSkishorechandraAinda não há avaliações
- Radiological Chest SignsDocumento15 páginasRadiological Chest SignsEzekiel ArtetaAinda não há avaliações
- AtelectasisDocumento37 páginasAtelectasisSandara ParkAinda não há avaliações
- Valvular Heart Disease 2Documento46 páginasValvular Heart Disease 2Topea BogdanAinda não há avaliações
- HyphemaDocumento19 páginasHyphemaLiyanti RinceAinda não há avaliações
- Radiology Quiz Medical Students Workbook: Author: DR Aussami Abbas SPR RadiologyDocumento11 páginasRadiology Quiz Medical Students Workbook: Author: DR Aussami Abbas SPR RadiologyMădălina CiobotariuAinda não há avaliações
- NEJM 2014 Fundamentals of Lung AuscultationDocumento7 páginasNEJM 2014 Fundamentals of Lung AuscultationFelipe CeaAinda não há avaliações
- Diaphragmatic ParalysisDocumento32 páginasDiaphragmatic ParalysisSwapnil MehtaAinda não há avaliações
- Pulsus ParadoxusDocumento2 páginasPulsus ParadoxusHassan.shehriAinda não há avaliações
- Cor PulmonaleDocumento8 páginasCor PulmonaleAymen OmerAinda não há avaliações
- How Long Do Partial Thickness Burns Typically Take To Heal?Documento49 páginasHow Long Do Partial Thickness Burns Typically Take To Heal?Farah FarahAinda não há avaliações
- StemiDocumento11 páginasStemidoubleraAinda não há avaliações
- X Thorax BeoordelenDocumento135 páginasX Thorax BeoordelenmtescasuraAinda não há avaliações
- OSCE Marksheet 1Documento7 páginasOSCE Marksheet 1Elias PetrouAinda não há avaliações
- Recent Stemi Extensive Anterior Wall Killip Ii: Supervisor: Prof. Dr. Peter Kabo, PH.D, SP - FK, SP - JP (K), Fiha, FasccDocumento36 páginasRecent Stemi Extensive Anterior Wall Killip Ii: Supervisor: Prof. Dr. Peter Kabo, PH.D, SP - FK, SP - JP (K), Fiha, FasccNurfitasari UdinAinda não há avaliações
- Chest Radiology For DummiesDocumento6 páginasChest Radiology For DummiesTom MallinsonAinda não há avaliações
- Lung AuscultationDocumento62 páginasLung AuscultationOlea CroitorAinda não há avaliações
- Mcem Anatomy MCQDocumento37 páginasMcem Anatomy MCQMOHAMMED ANEEZAinda não há avaliações
- OS205 Cardiac ImagingDocumento7 páginasOS205 Cardiac ImagingLaurisse ManaloAinda não há avaliações
- Atrial Septal DefectDocumento2 páginasAtrial Septal DefectPearl DiBerardinoAinda não há avaliações
- Family Centred CareDocumento20 páginasFamily Centred CareMiftakhul KhoeryAinda não há avaliações
- Anatomy Mnemonics PDFDocumento7 páginasAnatomy Mnemonics PDFHaseebUl haqAinda não há avaliações
- Preview of "Practice Quiz - Heart"Documento2 páginasPreview of "Practice Quiz - Heart"Jose Pagan100% (1)
- The Radiology Assistant - Lung DiseaseDocumento67 páginasThe Radiology Assistant - Lung DiseaseVAISHALI CHOUDHARYAinda não há avaliações
- The Management of Acute Respiratory Distress SyndromeDocumento48 páginasThe Management of Acute Respiratory Distress SyndromeLauraAlvarezMulettAinda não há avaliações
- Examining The PrecordiumDocumento83 páginasExamining The PrecordiumnicolAinda não há avaliações
- Methods of Clinical ExaminationDocumento18 páginasMethods of Clinical ExaminationPaolo BautistaAinda não há avaliações
- Case Study Bronchial-AsthmaDocumento9 páginasCase Study Bronchial-AsthmaGabbii CincoAinda não há avaliações
- FinalDocumento56 páginasFinalvamshidhAinda não há avaliações
- MCEM Anatomy MCQ PDFDocumento44 páginasMCEM Anatomy MCQ PDFUgeshwaran Aristotle Reddy100% (1)
- Websites For Review of RadiologyDocumento1 páginaWebsites For Review of RadiologyHaluk AlibazogluAinda não há avaliações
- Chest X-Ray InterpretationDocumento3 páginasChest X-Ray InterpretationHaluk AlibazogluAinda não há avaliações
- Chest X-Ray InterpretationDocumento3 páginasChest X-Ray InterpretationHaluk AlibazogluAinda não há avaliações
- Chest X Ray InterpretationDocumento2 páginasChest X Ray InterpretationHaluk AlibazogluAinda não há avaliações
- Section II - Chest Radiology: Figure 1ADocumento35 páginasSection II - Chest Radiology: Figure 1AHaluk Alibazoglu100% (1)
- Cardiac Radiology.Documento13 páginasCardiac Radiology.Haluk AlibazogluAinda não há avaliações
- Innovation and Development in Indian HealthcareDocumento29 páginasInnovation and Development in Indian HealthcareSahana BoseAinda não há avaliações
- Printer Sony Upd75mdDocumento2 páginasPrinter Sony Upd75mdHaluk AlibazogluAinda não há avaliações
- TechTips FastSpectDocumento2 páginasTechTips FastSpectHaluk AlibazogluAinda não há avaliações