Escolar Documentos
Profissional Documentos
Cultura Documentos
Conservative Management of Perforated Peptic Ulcer
Enviado por
Afiani Jannah0 notas0% acharam este documento útil (0 voto)
134 visualizações4 páginasJurnal Penanganan Secara Konservatif terhadap kasus Perforasi Gaster
Direitos autorais
© © All Rights Reserved
Formatos disponíveis
PDF, TXT ou leia online no Scribd
Compartilhar este documento
Compartilhar ou incorporar documento
Você considera este documento útil?
Este conteúdo é inapropriado?
Denunciar este documentoJurnal Penanganan Secara Konservatif terhadap kasus Perforasi Gaster
Direitos autorais:
© All Rights Reserved
Formatos disponíveis
Baixe no formato PDF, TXT ou leia online no Scribd
0 notas0% acharam este documento útil (0 voto)
134 visualizações4 páginasConservative Management of Perforated Peptic Ulcer
Enviado por
Afiani JannahJurnal Penanganan Secara Konservatif terhadap kasus Perforasi Gaster
Direitos autorais:
© All Rights Reserved
Formatos disponíveis
Baixe no formato PDF, TXT ou leia online no Scribd
Você está na página 1de 4
The THAI Journal of SURGERY 2005; 26:5-8.
Official Publication of the Royal College of Surgeons of Thailand
5
INTRODUCTION
The accepted therapeutic options in patients
with perforated peptic ulcer are simple closure or
immediate definitive operation. Conservative
treatment, originally proposed by Wangensteen, was
recommended as the treatment of choice in perforated
acute peptic ulcer by Taylor in 1956
1
. Today it is
reserved for patients considered to be too ill to stand
the stress of surgery or in situations where immediate
surgery is unavailable. A trial of conservative manage-
ment in all cases of perforated peptic ulcer that met the
inclusion criteria was undertaken. Its efficacy and
long-term outcome were assessed.
PATIENTS AND METHODS
Forty-one patients admitted under one surgeon,
with perforated peptic ulcer, from October 1998 to
September 2001 were reviewed. The clinical details
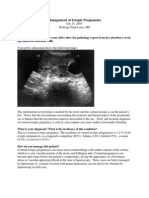
are shown in Table 1. All 41 patients were diagnosed
by history and clinical examination and all had
radiological evidence of perforation (pneumo-
peritoneum). Inclusion criteria consisted of a clinical
Correspondence address : Ruangsak Nusree, MD, Department of Surgery, Chainat General Hospital, Chainat 17000, Thailand.
E-mail: chainath.hospital@hotmail.com
Conservative Management of Perforated Peptic
Ulcer
Ruangsak Nusree, MD
Department of Surgery, Chainat General Hospital, Chainat, Thailand
Abstract Objective: To determine whether surgery could be avoided in selected patients with perforated peptic
ulcer.
Patients and Methods: A prospective study of the outcome of non-operative treatment in patients with
a clinical diagnosis of perforated peptic ulcer was conducted. Of all 41 patients with clinical diagnosis of
perforated peptic ulcer over the 3-year period, 35 were included for conservative treatment consisting of
intravenous fluid resuscitation, nasogastric suction, and intravenous administration of antibiotic (Cefazolin 1
gm. IV every 6 hrs) and Ranidine 50 mg. IV every 8 hrs.
Results: Five (14%) of these 35 patients did not improve after 12 hours of conservative treatment and
required an operation. All had unsealed perforation and were true failure. There was no mortality in this
conservative group and no significant difference in the morbidity, such as complications or median hospital
stay, between the failure group and the conservative group. Patients over 70 years old were less likely to respond
to conservative treatment (P <0.05).
Conclusions: In patients with perforated peptic ulcer, an initial period of non-operative treatment with
careful observation and resuscitation may be safely allowed, except in patients over 70 years old, and that the
use of such an observation period can obviate the need for emergency surgery.
Nusree R Thai J Surg Jan. - Mar. 2005 6
diagnosis of perforation in less than 12 hours
1
, with
stable hemodynamic condition
2
and age not exceeding
70 years
1
.
Conservative management consisted of intra-
muscular analgesia, intravenous antibiotic (Cefazolin
1 gram every 6 hours), H
2
-blocker (Ranidine 50 mg
intravenously every 8 hours) and hydration. A large-
bore radio-opaque nasogastric tube was passed to empty
the stomach by intermittent suction. Accurate tube
placement in the distal greater curvature and frequent
re-assessment were mandatory in this regimen.
Conservative treatment was abandoned if the patient
failed to improve or deteriorated (increasing tachy-
cardia, pyrexia, abdominal distension or pain) after 12
hours of conservative treatment.
RESULTS
Six patients who failed to meet the inclusion
criteria underwent immediate surgery. All had
perforation over 12 hours before presentation. A total
of 35 patients entered a trial of conservative therapy
and 30 were successfully managed. Five patients failed
to improve and underwent laparotomy.
There were no significant difference between the
failure group (although consisted of only 5 patients)
and the successfully managed group regarding age
(unpaired students t test), duration of perforation
before presentation [Mann-Whitney (2-tailed) U test],
medications or length of ulcer symptoms (Fishers
exact test). Conservative treatment did not prolong
hospital stay (Table 2).
Failure Group
Five patients underwent laparotomy after 12 hours
of trial. All had unsealed perforations and were true
failure of conservative treatment.
Complications
One patient who underwent immediate surgery
died of valvular heart disease and congestive heart
failure. Two patients developed postoperative pneu-
monia. Complications in the conservative group
included upper GI hemorrhage (N = 2), prolonged
ileus (N = 1) and diarrhea (N = 1). No mortality in the
conservative group.
Subsequent Course
Seven successfully treated patients could not be
traced. Twenty-three patients were followed up for 1-
4 years (mean 2.9 years). All 23 patients did not
require definitive surgery and did not develop re-
perforation. Two patients died of unrelated courses.
Table 1 Clinical characteristic of 41 patients with perforated
peptic ulcer
Characteristics Number of patients
Male 38
Female 3
Mean age in years (range) 47 (26-70)
Previous peptic ulcer 5
Previous perforation 1
NSAIDS or steroid used 10
Table 2 Comparison of clinical characteristics of 41 patients with perforated peptic ulcer in relation to eventual outcome
Emergency Surgery Failed conservative Successful conservative
(n = 6) treatment (n = 5) treatment (n = 30)
Mean age (years) 50 43 47
Median duration of perforation (hrs) 18 5 8
Symptoms
Acute (<3 months) 2 2 10
Chronic (>3 months) 4 3 20
Complications 2 1 3
Median hospital stay (days) 10 9 8
Mortality 1 - -
Vol. 26 No. 1 Conservative Management of Perforated Peptic Ulcer 7
Nine patients had medically managed dyspepsia and
twelve were asymptomatic.
DISCUSSION
The results of conservative treatment were
satisfactory. Thirty (85%) were successfully treated
with conservative management. Complications
occurred in 11%, and there was no mortality. These
results were achieved using strict selection of patients
and regular re-assessment. When conservative
treatment failed, it was promptly abandoned and
operation was performed. Nasogastric suction has
been the vital element in conservative treatment, in
keeping the stomach empty, allowing sealing of the
perforation to take place. Careful positioning of the
tube and regular aspiration are important. Opposition
to conservative treatment is related to the possible
consequences of an error in the diagnosis. However,
as Taylor has shown, with regular re-assessment,
misdiagnosis should become rapidly apparent and
conservative treatment can then be abandoned. Taylor
reported no serious consequences resulting from the
short delay in correcting the diagnosis
1
. The chief
contraindications include lack of patient compliance,
unsuccessful nasogastric intubation and late presen-
tation. Using conservative treatment, definitive surgery
cannot be performed at the time of operation. However,
not all chronic peptic ulcer perforation require
definitive procedures and with the advent of H
2
anta-
gonists, the number may be even less
3
. Conservative
treatment allows time for an accurate ulcer history, for
clinical and interval endoscopic assessment and for
elective definitive treatment if required.
The author does not advocate conservative
treatment for all perforated peptic ulcer but offer as a
reasonable option provided strict criteria and guide-
lines are followed.
That some perforated ulcers sealed themselves
off spontaneously with omentum, even though there
was considerable free air in the peritoneal cavity, had
been noted by Taylor and Visick when they operated
on duodenal ulcers that had perforated acutely.
Rossoff
3
summarized his experience in Los Angeles, of
377 cases, 43% were shown to be sealed off.
Crofts TJ et al, from Hong Kong
4
conducted a
prospective randomized phase 3 trial with 83 patients.
Forty patients were managed conservatively, if there
was no improvement after 12 hours they would undergo
surgery. There were no significant differences in
morbidity and mortality between these two groups of
patients.
Other risk factors, both for operative and
conservative management, have been assessed by
multivariate analysis. Irvin
5
identified risk factors which
included age over 70 years, use of steroidal or non-
steroidal anti-inflammatory drug, and concomitant
medical illness. The presence of shock (systolic B.P.
less than 100 mm. Hg.) and delay in treatment,
combined with these factors, could be used to predict
post-operative death with 87% accuracy. With age
over 70, the mortality rate rose to 34% whereas it was
less than 14% in those under 70. Ball et al
6
also
confirmed the risk of age, with a mortality rate of 47%
in those over 70s, and shock (with mortality rate of
100%). Alizadeh et al
7
analyzed the indications and
results of conservative therapy in 332 patients in 1997
and concluded that conservative treatment was
associated with very high mortality, frequent and careful
clinical monitoring was essential during the first 24
hours and, in the event of deterioration, surgery must
be considered. However, Songne et al
8
in 2004 reported
his prospective study in 82 patients on non-operative
treatment for perforated peptic ulcer and concluded
that more than 50% of patients with perforated peptic
ulcer responded to conservative treatment without
surgery and that the association of few criteria (size of
pneumoperitoneum grerater than size of the first
lumbar vertebra, heart beat over 94, pain at digital
rectal exam and age over 59) required emergency
surgery.
The wide variation in the time delay between
perforation and treatment is also believed to be
important. In the Hong Kong Series
4
, the duration in
the non-operative group was 10.5 hours and in an
earlier Hong Kong series
9
, the median was 12.6 hours.
In the Exeter series
5
, 33% of those over 70s had
perforation for longer than 24 hours. Conservative
treatment is not advised with a history longer than 12
hours
4
.
Concern over peritoneal soilage has led surgeons
to believe that it is important to carefully empty and
wash out the peritoneal cavity with large volume of
normal saline at the time of operation. The results are
quite gratifying, as large volume of foul smelling fluid
is oftenly removed. However the actual benefit of this
Nusree R Thai J Surg Jan. - Mar. 2005 8
part of the operation is not so clear. Rosoff, in discussion
of Donovan et al
3
, reported that of 109 patients treated
non-operatively during the acute phase, only 3
developed intra-abdominal abscesses.
Though there has also been concern about the
ulcer re-leaking, this has been a very unusual
occurrence. In the studies reported by Berne and
Rosoff
10
, this occurred in only 2 of 109 patients treated
non-operatively. Donovan et al
3
reported no re-leaks,
and there were no re-leaks in the patients described
here. However, this knowledge provides surgeons the
opportunity to avoid celiotomy in perforated acute
ulcer disease.
CONCLUSIONS
In patients with perforated peptic ulcer, an initial
period of non-operative treatment with careful
observation may be safely allowed except in patients
over 70 years old, patients with shock, or perforation
over 12 hours. The use of such an observation period
can obviate the need for emergency surgery. This
observation also permits surgeons to adopt non-
operative therapy in selected case, such as when
operative risk is excessive or when only closure of the
perforation is contemplated.
REFERENCE
1. Taylor H, Warren RP. Perforated acute and chronic peptic
ulcer. Conservative treatment. Lancet 1956; i: 397-9.
2. Keane TE, Dillon B, Afdhal NH, McCormack CJ. Conservative
management of perforated duodenal ulcer. Br J Surg 1988;
75: 583-4.
3. Donovan AJ, Vinson TC, Maulsby GO, Gewin JR. Selective
treatment of duodenal ulcer with perforation. Ann Surg
1979; 189: 627-36.
4. Crofts TJ, Park KGM, Steele RJC, Li AKC. A randomized trial
of non-operative treatment for perforated peptic ulcer. N
Engl J Med 1989; 320: 970-3.
5. Irvin T. Mortality and perforated peptic ulcer: case for risk
stratification in elderly patients. Br J Surg 1989; 76: 215-8.
6. Ball AB, Thomas PA, Evans SJ. Operative mortality after
perforated peptic ulcer. Br J Surg 1989; 76: 521-2.
7. Alizadeh N, Buhler L, Huber O, Morel P. Conservative
treatment of gastroduodenal peptic ulcer perforations:
indications and results. Schweiz Med Wochenschr Suppl
1997; 89: 17S-19S.
8. Songne B, Jean F, Foulatier O, Khalil H, Scotte M. Non
operative treatment for perforated peptic ulcer: results of a
prospective study. Ann Chir 2004; 129: 578-82.
9. Boey J, Lee NW, Koo j, Lam PH, Wong J, Ong GP. Immediate
definitive surgery for perforated duodenal ulcer: a
prospective controlled trial. Ann Surg 1982; 196: 338-44.
10. Berne CJ, Rosoff L Sr. Acute perforation of peptic ulcer. In:
Nyhus LN, Wastell O, editors. Surgery of the stomach and
duodenum. Boston, Mass: Little Brown & Co Inc; 1986: 457-
73.
Você também pode gostar
- HINO Dutro Fault Codes List PDFDocumento4 páginasHINO Dutro Fault Codes List PDFANH LÊAinda não há avaliações
- COLORECTAL CANCER FINAL PPT To Be PresentedDocumento53 páginasCOLORECTAL CANCER FINAL PPT To Be Presentedamanuel100% (1)
- Subcontracting Process in Production - SAP BlogsDocumento12 páginasSubcontracting Process in Production - SAP Blogsprasanna0788Ainda não há avaliações
- Perforated Peptic Ulcer LancetDocumento11 páginasPerforated Peptic Ulcer LancetAmy NapitupuluAinda não há avaliações
- 10 Powerful Mudras and How To Use Them: 1. GyanDocumento4 páginas10 Powerful Mudras and How To Use Them: 1. GyanAkrithi Akrithi100% (1)
- Surgical Management of Acute CholecystitisDocumento17 páginasSurgical Management of Acute Cholecystitisgrayburn_1Ainda não há avaliações
- Git DisturbancesDocumento119 páginasGit DisturbancesPeterpan NguyenAinda não há avaliações
- Baltarowich ABD pt1 Hepatobiliary US PDFDocumento22 páginasBaltarowich ABD pt1 Hepatobiliary US PDFEka KusumaningatiAinda não há avaliações
- Acid Related DisordersDocumento18 páginasAcid Related DisordersMinto SanjoyoAinda não há avaliações
- Surgical Treatment of Hemorrhoidal Disease - UpToDateDocumento27 páginasSurgical Treatment of Hemorrhoidal Disease - UpToDateJune DoAinda não há avaliações
- Daniel Madison - BreachDocumento8 páginasDaniel Madison - Breachmrbookman3Ainda não há avaliações
- Management of Ectopic PregnancyDocumento4 páginasManagement of Ectopic PregnancyAfiani JannahAinda não há avaliações
- Antimicrobial Prophylaxis For Prevention of Surgical Site Infection in AdultsDocumento59 páginasAntimicrobial Prophylaxis For Prevention of Surgical Site Infection in Adultsbolohan biatriceAinda não há avaliações
- Management of The Pancreatic Remnant During Whipple OperationDocumento4 páginasManagement of The Pancreatic Remnant During Whipple OperationYacine Tarik Aizel100% (1)
- Subtotal Cholecystectomy-''Fenestrating'' Vs ''Reconstituting'' Subtypes and The Prevention of Bile Duct Injury - Definition of The Optimal Procedure In  Difficult Operative ConditionsDocumento8 páginasSubtotal Cholecystectomy-''Fenestrating'' Vs ''Reconstituting'' Subtypes and The Prevention of Bile Duct Injury - Definition of The Optimal Procedure In  Difficult Operative ConditionsBolivar Isea100% (1)
- Proton Pump Inhibitors - The Beginning of The End or The End of The Beginning PDFDocumento8 páginasProton Pump Inhibitors - The Beginning of The End or The End of The Beginning PDFbravohr98Ainda não há avaliações
- Tonsillectomy Slides 050427Documento62 páginasTonsillectomy Slides 050427Aidiel FikriAinda não há avaliações
- Yes Bank FinalDocumento107 páginasYes Bank FinalDrMehul JoshiAinda não há avaliações
- Schwartz Hour - BurnDocumento62 páginasSchwartz Hour - BurnM3 SURGERY100% (1)
- Management of Anastomotic Complications of Colorectal SurgeryDocumento13 páginasManagement of Anastomotic Complications of Colorectal Surgerydadupipa100% (1)
- Gastroduodenal PerforationDocumento4 páginasGastroduodenal PerforationMaresp21Ainda não há avaliações
- Hepatocellular Carcinoma: Review ArticleDocumento13 páginasHepatocellular Carcinoma: Review ArticleAnnagiulia Gramenzi100% (2)
- Bile Duct InjuryDocumento62 páginasBile Duct InjuryShashidhara Puttaraj100% (1)
- Iec 62031 PDFDocumento16 páginasIec 62031 PDFAlbertoAinda não há avaliações
- Endoscopic SurgeryDocumento152 páginasEndoscopic SurgeryiciAinda não há avaliações
- Tips - Anaphylaxis and Hypersensitivity Reactions PDFDocumento376 páginasTips - Anaphylaxis and Hypersensitivity Reactions PDFsorinproiecteAinda não há avaliações
- Perbedaan Penanganan Antara Laparoskopi Vs Open Repair Pada Perforasi GasterDocumento7 páginasPerbedaan Penanganan Antara Laparoskopi Vs Open Repair Pada Perforasi GasterAfiani JannahAinda não há avaliações
- Perbedaan Penanganan Antara Laparoskopi Vs Open Repair Pada Perforasi GasterDocumento7 páginasPerbedaan Penanganan Antara Laparoskopi Vs Open Repair Pada Perforasi GasterAfiani JannahAinda não há avaliações
- Syphilis CongenitalDocumento5 páginasSyphilis CongenitalElisse StephanieAinda não há avaliações
- Postcholecystectomy SyndromeDocumento27 páginasPostcholecystectomy SyndromeMonica TurnerAinda não há avaliações
- Atlas of Gastrointestinal Endoscopy and Related PathologyDocumento2 páginasAtlas of Gastrointestinal Endoscopy and Related PathologyMaria PatituAinda não há avaliações
- Management of Acute Pancreatitis - UpToDateDocumento33 páginasManagement of Acute Pancreatitis - UpToDateCesar Luna RamirezAinda não há avaliações
- Surgical Management of ObesityDocumento13 páginasSurgical Management of Obesityمحمد حميدانAinda não há avaliações
- CME Trunk, Abdomen, and Pressure Sore ReconstructionDocumento15 páginasCME Trunk, Abdomen, and Pressure Sore ReconstructionVeronica TomaselloAinda não há avaliações
- Phyllodes Tumors of The Breast UpToDateDocumento22 páginasPhyllodes Tumors of The Breast UpToDateSean SialanaAinda não há avaliações
- PreOp Evaluation in CKD Patients Up To DateDocumento14 páginasPreOp Evaluation in CKD Patients Up To DateMaría Fernanda RíosAinda não há avaliações
- Management of Acute Appendicitis in Adults - UpToDateDocumento28 páginasManagement of Acute Appendicitis in Adults - UpToDateaulia rachman100% (1)
- Perioperative Management of Patients Receiving Anticoagulants - UpToDateDocumento65 páginasPerioperative Management of Patients Receiving Anticoagulants - UpToDatejames lxAinda não há avaliações
- Surgical Safety ChecklistDocumento2 páginasSurgical Safety ChecklistLian CatindigAinda não há avaliações
- Abdominal Wall IncisionDocumento42 páginasAbdominal Wall IncisionURo KkuAinda não há avaliações
- Causes of Upper Gastrointestinal Bleeding in Adults - UpToDateDocumento37 páginasCauses of Upper Gastrointestinal Bleeding in Adults - UpToDateAline MoraisAinda não há avaliações
- Perforated Peptic UlcerDocumento68 páginasPerforated Peptic UlcerSaibo BoldsaikhanAinda não há avaliações
- Diagnosis and Acute Management of Suspected Nephrolithiasis in Adults - UpToDateDocumento44 páginasDiagnosis and Acute Management of Suspected Nephrolithiasis in Adults - UpToDateManu Luciano100% (1)
- Topical Hemostatic Agents in Surgery PDFDocumento10 páginasTopical Hemostatic Agents in Surgery PDFFernanda SouzaAinda não há avaliações
- Perforated Peptic Ulcer DiseaseDocumento2 páginasPerforated Peptic Ulcer DiseaseRene John FranciscoAinda não há avaliações
- Use of Blood Products in The Critically Ill - UpToDateDocumento13 páginasUse of Blood Products in The Critically Ill - UpToDateOscar F RojasAinda não há avaliações
- Liver Function TestDocumento40 páginasLiver Function TestanojAinda não há avaliações
- Gallstones in Pregnancy - UpToDateDocumento51 páginasGallstones in Pregnancy - UpToDateLeira BarbosaAinda não há avaliações
- Acute Colonic Diverticulitis: Medical Management - UpToDateDocumento20 páginasAcute Colonic Diverticulitis: Medical Management - UpToDateFelipe Orellana MuñozAinda não há avaliações
- Laparoscopic SurgeryDocumento10 páginasLaparoscopic Surgerynainacurthberrt50% (2)
- Surgery II - Pancreas 2014Documento20 páginasSurgery II - Pancreas 2014Medisina101Ainda não há avaliações
- Postoperative Peritoneal Adhesions in Adults and Their Prevention - UpToDateDocumento17 páginasPostoperative Peritoneal Adhesions in Adults and Their Prevention - UpToDateDesak PramestiAinda não há avaliações
- Approach To The Adult With Unexplained Thrombocytopenia - UpToDateDocumento65 páginasApproach To The Adult With Unexplained Thrombocytopenia - UpToDateMagdy GabrAinda não há avaliações
- An Updated Review of Cystic Hepatic LesionsDocumento8 páginasAn Updated Review of Cystic Hepatic LesionsMayerlin CalvacheAinda não há avaliações
- (HLMN 5-19) Evaluation of The Adult With Abdominal Pain - UpToDateDocumento21 páginas(HLMN 5-19) Evaluation of The Adult With Abdominal Pain - UpToDateandylumanAinda não há avaliações
- Acute Pancreatitis - Up To DateDocumento31 páginasAcute Pancreatitis - Up To DateNicole AguilarAinda não há avaliações
- Use of Anticoagulants During Pregnancy and Postpartum - UpToDateDocumento38 páginasUse of Anticoagulants During Pregnancy and Postpartum - UpToDateCristinaCaprosAinda não há avaliações
- General SurgeryDocumento18 páginasGeneral SurgeryYogesh KharcheAinda não há avaliações
- Management of Acute Appendicitis in Adults - UpToDateDocumento28 páginasManagement of Acute Appendicitis in Adults - UpToDateVinicius VieiraAinda não há avaliações
- Current Trends in Management of CholedocholithiasisDocumento35 páginasCurrent Trends in Management of Choledocholithiasisrajan kumar100% (6)
- Approach To The Adult Patient With Anemia - UpToDateDocumento23 páginasApproach To The Adult Patient With Anemia - UpToDateNicole SierraAinda não há avaliações
- Fibromialgia - UptodateDocumento21 páginasFibromialgia - UptodateaeadaAinda não há avaliações
- Initial Management of Trauma in Adults - UpToDateDocumento37 páginasInitial Management of Trauma in Adults - UpToDateAlberto Kenyo Riofrio PalaciosAinda não há avaliações
- Have Half-Lives in The Range 2 - 6 H. Lovenox Is 4.5 Hours. The Anticoagulant Effect ofDocumento37 páginasHave Half-Lives in The Range 2 - 6 H. Lovenox Is 4.5 Hours. The Anticoagulant Effect ofkellixgAinda não há avaliações
- Simple MastectomyDocumento3 páginasSimple MastectomyCindy DayocAinda não há avaliações
- Garcia, Melegrito, Zamuco: Perforated Peptic Ulcer DiseaseDocumento4 páginasGarcia, Melegrito, Zamuco: Perforated Peptic Ulcer DiseasePaulo GarciaAinda não há avaliações
- Portal Hypertension in Adults - UpToDateDocumento12 páginasPortal Hypertension in Adults - UpToDateyessyAinda não há avaliações
- ERCPDocumento11 páginasERCPMalaak BassamAinda não há avaliações
- Sentinal Lymph Node BiopsyDocumento12 páginasSentinal Lymph Node BiopsySahirAinda não há avaliações
- Bariatric SurgeryDocumento26 páginasBariatric SurgeryAmyandAinda não há avaliações
- Definition, Classification, Etiology, and Pathophysiology of Shock in Adults - UpToDateDocumento16 páginasDefinition, Classification, Etiology, and Pathophysiology of Shock in Adults - UpToDatevara prasadAinda não há avaliações
- Urinary System: Cytology, Histology, Cystoscopy, and RadiologyNo EverandUrinary System: Cytology, Histology, Cystoscopy, and RadiologyAinda não há avaliações
- EctopicDocumento15 páginasEctopicquester1515Ainda não há avaliações
- Epidemiologi Perforasi GasterDocumento8 páginasEpidemiologi Perforasi GasterAfiani JannahAinda não há avaliações
- Antibiotics Resistance in GonorrhoeaeDocumento7 páginasAntibiotics Resistance in GonorrhoeaeAfiani JannahAinda não há avaliações
- Treatment of Perforative Peptic UlcerDocumento14 páginasTreatment of Perforative Peptic UlcerAfiani JannahAinda não há avaliações
- History of Coronary ScoringDocumento32 páginasHistory of Coronary ScoringAfiani JannahAinda não há avaliações
- Dermatophytid in Tinea CapitisDocumento7 páginasDermatophytid in Tinea CapitisAfiani JannahAinda não há avaliações
- Tatalaksana Perdarahan ObstetriDocumento10 páginasTatalaksana Perdarahan ObstetriAfiani JannahAinda não há avaliações
- Lymphogranuloma VenereumDocumento14 páginasLymphogranuloma VenereumAfiani JannahAinda não há avaliações
- Pityriasis VersicolorDocumento8 páginasPityriasis VersicolorAfiani JannahAinda não há avaliações
- Interventions of ImpetigoDocumento97 páginasInterventions of ImpetigoAfiani JannahAinda não há avaliações
- Tons Slides 2003 1105Documento44 páginasTons Slides 2003 1105Afiani JannahAinda não há avaliações
- Rajesh CVDocumento3 páginasRajesh CVS R PramodAinda não há avaliações
- Hopf 6870 - 1101Documento58 páginasHopf 6870 - 1101macakafkaAinda não há avaliações
- Midi Fighter Twister - User Guide 2016Documento25 páginasMidi Fighter Twister - User Guide 2016moxmixAinda não há avaliações
- ERIC Section4 Hadrian - C. AlbinusDocumento83 páginasERIC Section4 Hadrian - C. AlbinusDarko SekulicAinda não há avaliações
- Watch Out For Flying Pumpkins: BOE Member PromotedDocumento16 páginasWatch Out For Flying Pumpkins: BOE Member PromotedelauwitAinda não há avaliações
- JNTU Old Question Papers 2007Documento8 páginasJNTU Old Question Papers 2007Srinivasa Rao GAinda não há avaliações
- Assignment Oumh2103 English For Science Technical PurposesDocumento12 páginasAssignment Oumh2103 English For Science Technical PurposesKhairul AnuarAinda não há avaliações
- Pakistan RailwayDocumento38 páginasPakistan RailwayمحمودعليAinda não há avaliações
- BR Safetymatrix enDocumento12 páginasBR Safetymatrix enHamidreza MoaddeliAinda não há avaliações
- Saturated Salt Solutions and %RHDocumento2 páginasSaturated Salt Solutions and %RHsamman149686100% (1)
- Score Fusion of Finger Vein and Face For Human Recognition Based On Convolutional Neural Network ModelDocumento9 páginasScore Fusion of Finger Vein and Face For Human Recognition Based On Convolutional Neural Network ModelFressy NugrohoAinda não há avaliações
- Turnitin Originality ReportDocumento20 páginasTurnitin Originality ReportNaomi Deirdre ReyesAinda não há avaliações
- Mungbean 03india PDFDocumento194 páginasMungbean 03india PDFSrujana PatelAinda não há avaliações
- Laura Gentile Letter On Hampden County CourthouseDocumento6 páginasLaura Gentile Letter On Hampden County CourthouseMassLiveAinda não há avaliações
- Unit 1 - Theoretical Framework PDFDocumento67 páginasUnit 1 - Theoretical Framework PDFMeli EujaniánAinda não há avaliações
- 23 - Eave StrutsDocumento2 páginas23 - Eave StrutsTuanQuachAinda não há avaliações
- Catalyst PreparationDocumento15 páginasCatalyst PreparationVISHAL SHARMAAinda não há avaliações
- 2 2 1 A Productanalysis 2Documento5 páginas2 2 1 A Productanalysis 2api-308131962Ainda não há avaliações
- PVC Duct DesignDocumento10 páginasPVC Duct DesigncitramuaraAinda não há avaliações
- Cantece Copii in EnglezaDocumento10 páginasCantece Copii in EnglezaGeorgi Neacşa100% (1)
- Bolt Group Coefficient For Eccentric Loads PDFDocumento5 páginasBolt Group Coefficient For Eccentric Loads PDFdvelchevAinda não há avaliações
- Commissioning Valve Product BrochureDocumento14 páginasCommissioning Valve Product BrochureblindjaxxAinda não há avaliações
- Design & Fabrication of Low Cost Small-Scale Fatigue Testing MachineDocumento12 páginasDesign & Fabrication of Low Cost Small-Scale Fatigue Testing MachinekshitijAinda não há avaliações
- Zbus and Symmetrical Fault AnalysisDocumento20 páginasZbus and Symmetrical Fault Analysishj203800Ainda não há avaliações