Escolar Documentos
Profissional Documentos
Cultura Documentos
Level III Clinical Narrative
Enviado por
api-2534511610 notas0% acharam este documento útil (0 voto)
53 visualizações5 páginasTítulo original
level iii clinical narrative
Direitos autorais
© © All Rights Reserved
Formatos disponíveis
DOCX, PDF, TXT ou leia online no Scribd
Compartilhar este documento
Compartilhar ou incorporar documento
Você considera este documento útil?
Este conteúdo é inapropriado?
Denunciar este documentoDireitos autorais:
© All Rights Reserved
Formatos disponíveis
Baixe no formato DOCX, PDF, TXT ou leia online no Scribd
0 notas0% acharam este documento útil (0 voto)
53 visualizações5 páginasLevel III Clinical Narrative
Enviado por
api-253451161Direitos autorais:
© All Rights Reserved
Formatos disponíveis
Baixe no formato DOCX, PDF, TXT ou leia online no Scribd
Você está na página 1de 5
Clinical Narrative
Caitlin Kowalski RN, BSN
Starting as a new graduate nurse on the
Acute Care of the Elderly unit I remember
feeling overwhelmed with the tasks that are
required by nursing. I started my day by
getting to the unit early to look up my
patients for the shift. On my report sheet I would write down tasks that needed to be
completed with boxes next to each one to make sure they were done by the end of the
shift. I would rush in and out of patients rooms completing the different tasks. I felt
uncertain because I thought I would be prepared coming out of school but it was like I
was starting all over again learning new things every day. I have been a nurse for almost
four years, but looking back I can see the extreme growth in my practice and the
interpersonal skills that I have gained while taking care of geriatric patients.
I continue to start each day by arriving early to look up my patients and writing
down tasks for the day, but Ive been able to transition into a nurse that sees my patients
overall story and adapt my day to meet their needs. I have learned that the geriatric
population is unique and requires specific skill sets. My interest in the geriatric
population matured as I was a nurse on the Acute Care of the Elderly Unit. To expand
my knowledge I got involved with Nurses Improving Care for the Healthsystem Elders
(NICHE), became a Geriatric Resource Nurse through NICHE, attended a NICHE
conference, joined the National Gerontological Nursing Association and currently
participate in the NICHE and Geriatric Leadership committees at University of Colorado
Hospital.
I understand not only the physical needs to provide quality geriatric sensitive care
to our patients, but also the emotional needs. Joyce Travelbees nursing theory focuses
on genuine human-to-human relationship between a patient and the nurse. This
relationship is built through five stages until the patient and the nurse attain a rapport.
Joyce Travelbees theory has influence my nursing practice by achieving sincere
relationships with my patients. I have been able to carry this theory with me as my
practice grew into a Level III nurse. I would like to share a specific instance where I was
able to build on this theory, develop a special relationship with my patient and how my
practice has grown to that of a Level III nurse.
It was in the afternoon and I was assigned a patient who was coming from Denver
International Airport (D.I.A.) for altered mental status. I figured it would be the typical
admission from D.I.A. were the patient would stay for a couple days and would be off on
the next plane back to their home. It wasnt the case for this woman. I got the room
ready for the new patient to arrive, grabbing supplies and writing my name on the
whiteboard. I didnt receive report on the patient as she was a direct admit and was
brought in by ambulance. The patient arrived enraged and ranting in Korean. Quickly, I
grabbed the interpreter phone and went to the room to start my first task, the admission
assessment. It did not go over as smoothly as I thought it would. The patient would not
use the interpreter phone but was continuously talking to me in Korean, which I could
not understand. Nothing was getting done and I was unable to communicate with her. I
went to my resources to help with the situation. First, I ensured the new patient was safe
by delegating to the nursing assistant to stay with her when I checked in with my other
three patients. I called my charge nurse to update her on the situation and ordered a live
interpreter to help me communicate with the patient effectively. As a Level II nurse this
situation would have been too overwhelming for me to do anything or I would to have
had to hand off my other patients.
When the interpreter arrived the patient was still infuriated and was repeating
the same thing over and over again, not making any sense and would not listen to what
we were saying. I spent over an hour in the room with the patient and interpreter trying
to help her understand where she was and calm her down but not much was
accomplished. Before the interpreter left I asked if he could write out the translation of
some phrases in Korean (you are in the hospital in Colorado, do you have to go to the
bathroom, are you in pain, etc.) so we could use them as cue cards to communicate
with the patient throughout the shift since the patient refused to use the interpreter
phone. This was not the typical admission I expected and the patient didnt stay for days
but for many months. In this time I built a relationship and rapport with her.
As she stayed on our unit I began to learn her routines. She was fit for her age and
sometimes could not stand staying in her room. Often she would become frustrated and
aggravated when contained to her room. During her long stay in the hospital her sleep-
wake cycle often became disrupted and she would sleep throughout the day and be
awake during the night. When I had her as my patient and even when she wasnt my
patient I would take her for walks in the garden in front of the hospital or do exercises in
the hallway. This kept her stimulated during the day so she could sleep at night to help
prevent delirium and agitation. When I would take her to the gardens outside she would
point to flowers and say something in Korean. I would reply in English talking about the
flowers or plants she was pointing to. We built a relationship even though most of the
time we werent communicating in each others language but through body language. I
remember the first time she wanted to hold my hand as we walked, which showed me I
had gained her trust and established a rapport. Looking back to our initial interaction I
had grown to know this patient as a person and felt empathy. From this relationship
built I felt like I was fulfilling part of Joyce Travelbees theory.
I exhibited growth as a nurse through this experience by being creative and using
different methods to decrease agitation, maintain a healthy sleep routine, and improve
communication with the patient. I helped keep her sleep-wake cycle regular to prevent
delirium and keep her health restored without turning to medication. I improved our
communication by making cue cards which allowed myself and other staff to address
needs quickly when the patient refused the interpreter phone. The cue cards stayed in
her room throughout her 5 month stay as a resource. Four years ago as a new nurse, I
may have went straight to Haldol to calm this patient, viewed ambulating this patient as
a task, or would be become overwhelmed. When caring for her it became my routine and
goal to take her outside as I know the importance behind it for her physical health but
also patient satisfaction. I took the extra time to care and be kind to her not because I
had to but because it was important to me as a nurse. From my first encounter with the
patient I felt frustration but through her stay we communicated in different ways and
spent time together in which we built a relationship.
We experience many complicated patients who stay on our unit for a long time,
but we are often motivated to provide unique care to fit the needs of the patient. I
integrate Travelbees theory of nursing in caring for all of my patients and building an
authentic relationship. During work there will always be tasks to be completed. Through
my experience as a nurse I have learned to be flexible and recognize the needs of the
patient to provide geriatric sensitive patient-centered care. I have also become a
resource and leader for other nurses and many come to me when they have questions
about providing geriatric-sensitive care.
Você também pode gostar
- Jan - Letter of RecDocumento2 páginasJan - Letter of Recapi-253451161Ainda não há avaliações
- Letter of Rec - Melissa MDocumento2 páginasLetter of Rec - Melissa Mapi-253451161Ainda não há avaliações
- Recognition - Ed EmailDocumento2 páginasRecognition - Ed Emailapi-253451161Ainda não há avaliações
- Level III Resume - FinalDocumento2 páginasLevel III Resume - Finalapi-253451161Ainda não há avaliações
- Pall Care AttendanceDocumento2 páginasPall Care Attendanceapi-253451161Ainda não há avaliações
- StaffDocumento1 páginaStaffapi-253451161Ainda não há avaliações
- Niche Conference CeDocumento1 páginaNiche Conference Ceapi-253451161Ainda não há avaliações
- NgnamembershipcardDocumento1 páginaNgnamembershipcardapi-253451161Ainda não há avaliações
- Thank You - DesiDocumento1 páginaThank You - Desiapi-253451161Ainda não há avaliações
- 1 Patient Questionnaire - CleanDocumento2 páginas1 Patient Questionnaire - Cleanapi-253451161Ainda não há avaliações
- Palliative Care CommunicationDocumento5 páginasPalliative Care Communicationapi-253451161Ainda não há avaliações
- Communication With KatieDocumento2 páginasCommunication With Katieapi-253451161Ainda não há avaliações
- Prepost Sleep PPDocumento31 páginasPrepost Sleep PPapi-253451161Ainda não há avaliações
- Employee Ce RecordDocumento1 páginaEmployee Ce Recordapi-253451161Ainda não há avaliações
- Quality of Sleep Patients Get in The Hospital - PP Pre Autosaved AutosavedDocumento20 páginasQuality of Sleep Patients Get in The Hospital - PP Pre Autosaved Autosavedapi-253451161Ainda não há avaliações
- Oral Hydration Management Guideline FinalDocumento6 páginasOral Hydration Management Guideline Finalapi-253451161Ainda não há avaliações
- 1 24 14 1 30 13 Car - Live FlyerDocumento1 página1 24 14 1 30 13 Car - Live Flyerapi-253451161Ainda não há avaliações
- Focus Pdca Revised 3Documento2 páginasFocus Pdca Revised 3api-253451161Ainda não há avaliações
- Quiet at Night - Implementing A Nightingale PrincipleDocumento9 páginasQuiet at Night - Implementing A Nightingale Principleapi-253451161Ainda não há avaliações
- The Yellow House: A Memoir (2019 National Book Award Winner)No EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Nota: 4 de 5 estrelas4/5 (98)
- Never Split the Difference: Negotiating As If Your Life Depended On ItNo EverandNever Split the Difference: Negotiating As If Your Life Depended On ItNota: 4.5 de 5 estrelas4.5/5 (838)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceNo EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceNota: 4 de 5 estrelas4/5 (890)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeNo EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeNota: 4 de 5 estrelas4/5 (5794)
- The Little Book of Hygge: Danish Secrets to Happy LivingNo EverandThe Little Book of Hygge: Danish Secrets to Happy LivingNota: 3.5 de 5 estrelas3.5/5 (399)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureNo EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureNota: 4.5 de 5 estrelas4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryNo EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryNota: 3.5 de 5 estrelas3.5/5 (231)
- The Emperor of All Maladies: A Biography of CancerNo EverandThe Emperor of All Maladies: A Biography of CancerNota: 4.5 de 5 estrelas4.5/5 (271)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersNo EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersNota: 4.5 de 5 estrelas4.5/5 (344)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaNo EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaNota: 4.5 de 5 estrelas4.5/5 (265)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyNo EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyNota: 3.5 de 5 estrelas3.5/5 (2219)
- Team of Rivals: The Political Genius of Abraham LincolnNo EverandTeam of Rivals: The Political Genius of Abraham LincolnNota: 4.5 de 5 estrelas4.5/5 (234)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreNo EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreNota: 4 de 5 estrelas4/5 (1090)
- The Unwinding: An Inner History of the New AmericaNo EverandThe Unwinding: An Inner History of the New AmericaNota: 4 de 5 estrelas4/5 (45)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)No EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Nota: 4.5 de 5 estrelas4.5/5 (119)
- PDF 36Documento3 páginasPDF 36Armia GaberAinda não há avaliações
- Universidad Nacional de Cuyo Facultad de Educación: Lengua Extranjera: EnglishDocumento8 páginasUniversidad Nacional de Cuyo Facultad de Educación: Lengua Extranjera: EnglishLiliana AlisaresAinda não há avaliações
- RENAP 2009 Training SchedulesDocumento3 páginasRENAP 2009 Training SchedulesNoel100% (4)
- UNC Charlotte Magazine, 2Q, 2009Documento46 páginasUNC Charlotte Magazine, 2Q, 2009unccharlotteAinda não há avaliações
- Philosophy, Services, Purpose, Nature and Challenges of Special LibrariesDocumento9 páginasPhilosophy, Services, Purpose, Nature and Challenges of Special LibrariesAyotunde Badaru100% (2)
- To Study The Prevalence of Anaemia in Indoor Patients of Tertiary Care CentreDocumento3 páginasTo Study The Prevalence of Anaemia in Indoor Patients of Tertiary Care CentreIJAR JOURNALAinda não há avaliações
- Psychological Hardiness in Relation To Entrepreneurial Orientation Among Youth of PunjabDocumento7 páginasPsychological Hardiness in Relation To Entrepreneurial Orientation Among Youth of PunjabPriyashree RoyAinda não há avaliações
- ECON2206 Course OutlineDocumento12 páginasECON2206 Course OutlineChris Bury0% (1)
- IT Week1Documento11 páginasIT Week1Mustafa AdilAinda não há avaliações
- Cold Calling 26 AugDocumento4 páginasCold Calling 26 AugGajveer SinghAinda não há avaliações
- IppdDocumento133 páginasIppdPonggey YabolAinda não há avaliações
- Unit 2 Expressing Like and Dislike A. Spoken Activity Exercise 1Documento3 páginasUnit 2 Expressing Like and Dislike A. Spoken Activity Exercise 1Faeruz Nur KhaerunnisaAinda não há avaliações
- Enai Recommendations On The Ethical Use of Artificial Intelligence in EducationDocumento5 páginasEnai Recommendations On The Ethical Use of Artificial Intelligence in EducationSaepul HayatAinda não há avaliações
- Varistors Based in The ZnO-Bi2O3 System, Microstructure Control and PropertiesDocumento6 páginasVaristors Based in The ZnO-Bi2O3 System, Microstructure Control and PropertiesJanja TothAinda não há avaliações
- Wsu Mthatha Faculty of Health Sciences Prospectus 2021 FullDocumento144 páginasWsu Mthatha Faculty of Health Sciences Prospectus 2021 FullThandoAinda não há avaliações
- Bharath Kumar: Software Development Engineer IDocumento3 páginasBharath Kumar: Software Development Engineer IAlton AbrahamAinda não há avaliações
- SUPPORT Doctor Letter of Support - BognerDocumento6 páginasSUPPORT Doctor Letter of Support - BognerKen WolskiAinda não há avaliações
- Sample 10762Documento16 páginasSample 10762Nayanjyot SinghAinda não há avaliações
- A Contrastive Analysis Between English and Indonesian LanguageDocumento5 páginasA Contrastive Analysis Between English and Indonesian LanguageLaga AntiEvilhackersAinda não há avaliações
- Lesson Exemplar in Science - Using The IDEA Instructional Process Learning Area Learning Delivery ModalityDocumento5 páginasLesson Exemplar in Science - Using The IDEA Instructional Process Learning Area Learning Delivery ModalityLeilani Pelisigas100% (1)
- RankBook ProfileDocumento5 páginasRankBook ProfilevandanaAinda não há avaliações
- Department of Education Region III Division of Pampanga Basa Air Base National High School Floridablanca, Pampanga S.Y. 2019 - 2020Documento2 páginasDepartment of Education Region III Division of Pampanga Basa Air Base National High School Floridablanca, Pampanga S.Y. 2019 - 2020Edita AquinoAinda não há avaliações
- CV Biographical ReviewDocumento3 páginasCV Biographical ReviewOscar Mauricio Carrillo ViverosAinda não há avaliações
- Human Resource Manager Job DescriptionDocumento2 páginasHuman Resource Manager Job DescriptionPraveenAinda não há avaliações
- Summary of PBB 2019 data for Region IX elementary schoolsDocumento35 páginasSummary of PBB 2019 data for Region IX elementary schoolsVIRGILIO GUZONAinda não há avaliações
- BCM-MS TPDocumento2 páginasBCM-MS TPabdullahazrezarAinda não há avaliações
- New Procedure for Determining Merit and Fitness for Trade and Crafts PositionsDocumento18 páginasNew Procedure for Determining Merit and Fitness for Trade and Crafts PositionsCandice Cabunilas FernandezAinda não há avaliações
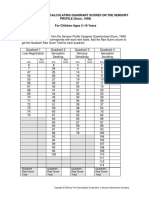
- Quadrant Grid: Worksheet For Calculating Quadrant Scores On The Sensory PROFILE (Dunn, 1999) For Children Ages 3-10 YearsDocumento2 páginasQuadrant Grid: Worksheet For Calculating Quadrant Scores On The Sensory PROFILE (Dunn, 1999) For Children Ages 3-10 YearsLorenzo CastroAinda não há avaliações
- Are Women Better Leaders Than MenDocumento5 páginasAre Women Better Leaders Than MenArijanaAinda não há avaliações
- Commercial building floor plan layoutDocumento1 páginaCommercial building floor plan layoutjitu9918Ainda não há avaliações