Escolar Documentos
Profissional Documentos
Cultura Documentos
Health Insurance 11 Bbi
Enviado por
padmajammulaDireitos autorais
Formatos disponíveis
Compartilhar este documento
Compartilhar ou incorporar documento
Você considera este documento útil?
Este conteúdo é inapropriado?
Denunciar este documentoDireitos autorais:
Formatos disponíveis
Health Insurance 11 Bbi
Enviado por
padmajammulaDireitos autorais:
Formatos disponíveis
VIVEK COLLEGE OF COMMERCE CHAPTER NO.
1 INTRODUCTION TO INSURANCE
1.1INTRODUCTION OF INSURANCE Insurance is a mechanism that helps to reduce the effects of adverse situations in the economical way. It promises to pay to the owner or beneficiary of the asset, a certain sum if the loss occurs. The business of insurance is related to the protection of the economic values of assets. The asset would have been created through the efforts of the owner. The asset is valuable to the owner, because he expects to get some benefits from it because it meets some of his needs. This benefit may be an income or in some other form. In the case of a factory or a cow, the product generated by it is sold and income is generated. In the case of a motor car, it provides comfort and convenience in transportation, there is no direct income. Both are assets and provide benefits. Every asset is expected to last for a certain period of time during which it will provide the benefits, after that, the benefit may not be available. There is a life-time for a machine in a factory or a cow or a motor car. None of them will last forever. The owner is aware of this and he can so manage his affairs that by the end of that period or life-time, a substitute is made available.
HEALTH INSURANCE Page 1
VIVEK COLLEGE OF COMMERCE
Thus, he makes sure that the benefit is not lost. However, the asset may get lost earlier. An accident or some other unfortunate event may destroy it or make it incapable of giving the benefits. An epidemic may kill the cow suddenly. In that case, the owner and those enjoying the benefits there from would be deprived of the benefits. The planned substitute would not have been ready. There is an adverse or unpleasant situation. Here, insurance helps to reduce the effects of such adverse situations.
1.2 PURPOSE & NEED OF INSURANCE The risk only means that there is a possibility of loss or damage. The damage may or may not happen. Insurance is done against the possibility that the damage may happen. There has to be an uncertainty about the risk. The earthquake may occur, but the building may not have been affected at all. The word 'possibility' implies uncertainty. Insurance is relevant only if there are uncertainties. In case of a human being, death is certain, but it's time is uncertain. The person is insured, because of the uncertainty about the time of his death. In the case of a person who is ill the time of death is not uncertain, though not exactly known. It would be 'soon'. He can't be insured.
HEALTH INSURANCE
Page 2
VIVEK COLLEGE OF COMMERCE
1.3 HOW INSURANCE WORKS The mechanism of insurance is very simple. People who are exposed to the same risks come together and agree that, if any one of them suffers a loss, the others will share the loss and make good to the person who lost. The manner in which the loss is to be shared can be determined beforehand. It can be equal among all. It can also be proportional to the risk that each person is exposed Insurance is a form of risk management primarily used to hedge against the risk of a contingent, uncertain loss. Insurance is defined as the equitable transfer of the risk of a loss, from one entity to another, in exchange for payment. An insurer is a company selling the insurance; the insured, or policyholder, is the person or entity buying the insurance policy. The amount to be charged for a certain amount of insurance coverage is called the premium. Risk management, the practice of appraising and controlling risk, has evolved as a discrete field of study and practice. The transaction involves the insured assuming a guaranteed and known relatively small loss in the form of payment to the insurer in exchange for the insurer's promise to compensate (indemnify) the insured in the case of a financial (personal) loss. The insured receives a contract, called the insurance policy, which details the conditions and circumstances under which the insured will be financially compensated. Insurance involves pooling funds from many insured entities (known as exposures) to pay for the losses that some may incur. The insured entities
HEALTH INSURANCE Page 3
VIVEK COLLEGE OF COMMERCE
are therefore protected from risk for a fee, with the fee being dependent upon the frequency and severity of the event occurring. In order to be insurable, the risk insured against must meet certain characteristics in order to be an insurable risk. Insurance is a commercial enterprise and a major part of the financial services industry, but individual entities can also self-insure through saving money for possible future losses. Risks which can be insured by private companies typically share seven common characteristics: 1. Large number of similar exposure units: Since insurance operates through pooling resources, the majority of insurance policies are provided for individual members of large classes, allowing insurers to benefit from the law of large numbers in which predicted losses are similar to the actual losses. Exceptions include Lloyd's of London, which is famous for insuring the life or health of actors, sports figures and other famous individuals. However, all exposures will have particular differences, which may lead to different premium rates. 2. Definite loss: The loss takes place at a known time, in a known place, and from a known cause. The classic example is death of an insured person on a life insurance policy. Fire, automobile accidents, and worker injuries may all easily meet this criterion. Other types of losses may only be definite in theory. Occupational disease, for instance, may involve prolonged exposure to injurious conditions where no specific time, place or cause is identifiable. Ideally, the time, place and cause of a loss should be clear enough that a reasonable person, with sufficient information, could objectively verify all three elements.
HEALTH INSURANCE Page 4
VIVEK COLLEGE OF COMMERCE
3. Accidental loss: The event that constitutes the trigger of a claim should be fortuitous, or at least outside the control of the beneficiary of the insurance. The loss should be pure, in the sense that it results from an event for which there is only the opportunity for cost. Events that contain speculative elements, such as ordinary business risks or even purchasing a lottery ticket, are generally not considered insurable. 4. Large loss: The size of the loss must be meaningful from the perspective of the insured. Insurance premiums need to cover both the expected cost of losses, plus the cost of issuing and administering the policy, adjusting losses, and supplying the capital needed to reasonably assure that the insurer will be able to pay claims. For small losses these latter costs may be several times the size of the expected cost of losses. There is hardly any point in paying such costs unless the protection offered has real value to a buyer. 5.Affordable premium: If the likelihood of an insured event is so high, or the cost of the event so large, that the resulting premium is large relative to the amount of protection offered, it is not likely that the insurance will be purchased, even if on offer. Further, as the accounting profession formally recognizes in financial accounting standards, the premium cannot be so large that there is not a reasonable chance of a significant loss to the insurer. If there is no such chance of loss, the transaction may have the form of insurance, but not the substance. (See the US Financial Accounting Standards Board standard number 113)
HEALTH INSURANCE
Page 5
VIVEK COLLEGE OF COMMERCE
6. Calculable loss: There are two elements that must be at least estimable, if not formally calculable: the probability of loss, and the attendant cost. Probability of loss is generally an empirical exercise, while cost has more to do with the ability of a reasonable person in possession of a copy of the insurance policy and a proof of loss associated with a claim presented under that policy to make a reasonably definite and objective evaluation of the amount of the loss recoverable as a result of the claim. 7. Limited risk of catastrophically large losses: Insurable losses are ideally independent and non-catastrophic, meaning that the losses do not happen all at once and individual losses are not severe enough to bankrupt the insurer; insurers may prefer to limit their exposure to a loss from a single event to some small portion of their capital base. Capital constrains insurers' ability to sell earthquake insurance as well as wind insurance in hurricane zones. In the US, flood risk is insured by the federal government. In commercial fire insurance it is possible to find single properties whose total exposed value is well in excess of any individual insurer's capital constraint. Such properties are generally shared among several insurers, or are insured by a single insurer who syndicates the risk into the reinsurance market.
HEALTH INSURANCE
Page 6
VIVEK COLLEGE OF COMMERCE CHAPTER NO.2 INTRODUCTION TO HEALTH INSURANCE
2.1 DEFINITION Insurance against loss by illness or bodily injury. Health insurance provides coverage for medicine, visits to the doctor or emergency room, hospital stays and other medical expenses. Policies differ in what they cover, the size of the deductible and/or co-payment, limits of coverage and the options for treatment available to the policyholder. Health insurance can be directly purchased by an individual, or it may be provided through an employer. Medicare and Medicaid are programs which provide health insurance to elderly, disabled, or un-insured individuals. There are a number of companies which provide private health insurance, including Blue Cross, United Healthcare, or Aetna. Introduction Health insurance is insurance against the risk of incurring medical expenses among individuals. By estimating the overall risk of health care expenses among a targeted group, an insurer can develop a routine finance structure, such as a monthly premium or payroll tax, to ensure that money is available to pay for the health care benefits specified in the insurance agreement. The benefit is administered by a central organization such as a government agency, private business, or not-forprofit entity.
HEALTH INSURANCE Page 7
VIVEK COLLEGE OF COMMERCE
2.2 HEALTH INSURANCE POLICY IS: 1) A contract between an insurance provider (e.g. an insurance company or a government) and an individual or his sponsor (e.g. an employer or a community organization). The contract can be renewable (e.g. annually, monthly) or lifelong in the case of private insurance, or be mandatory for all citizens in the case of national plans. The type and amount of health care costs that will be covered by the health insurance provider are specified in writing, in a member contract or "Evidence of Coverage" booklet for private insurance, or in a national health policy for public insurance. 2) Insurance coverage is provided by an employer-sponsored self-funded ERISA plan. The company generally advertises that they have one of the big insurance companies. However, in an ERISA case, that insurance company "doesn't engage in the act of insurance", they just administer it. Therefore ERISA plans are not subject to state laws. ERISA plans are governed by federal law under the jurisdiction of the US Department of Labor (USDOL). The specific benefits or coverage details are found in the Summary Plan Description (SPD). An appeal must go through the insurance company, then to the Employer's Plan Fiduciary. If still required, the Fiduciarys decision can be brought to the USDOL to review for ERISA compliance, and then file a lawsuit in federal court.
HEALTH INSURANCE
Page 8
VIVEK COLLEGE OF COMMERCE 2.3 IMPORTANCE OF HEALTH INSURANCE
Important Pointers in Health Insurance We must read the policy exclusions & the limitations in various covers properly before buying a Health Insurance plan because we should know what all covers our policy include & exclude. we should note the number of network hospitals covered in the Insurers list of network hospitals as this will help to get cashless & hassle-free claim. We must read the names of critical diseases being covered before buying a Critical-Care plan. We must know that the medical expenses incurred within the first 30 days of buying the health insurance plan are not covered unless the injury has occurred out of an accident. We must disclose all the Pre-Existing diseases to the insurer before buying the health plan as the insurer doesnt cover them, now a days General Insurers have started covering these diseases normally after 3-4 years varying from company to company. An English proverb says that Health is Wealth. It is not a meaningless saying as it defines a very important fact of life. Health is the most precious wealth that God has given you. It is a own property and we are the sole owner of it. Therefore, it is our responsibility to look after it properly. However, it is also true that the life is full of uncertainties and we never know what will happen in the next few hours. Therefore, it is
HEALTH INSURANCE Page 9
VIVEK COLLEGE OF COMMERCE
also our duty to make certain arrangement so that we can take care of our self as well as our family even if some misfortune falls upon us. Here comes the importance of health insurance program. This health insurance program, as the name itself tells, is entirely meant for the proper care of our body and health. It is a permanent arrangement that we can avail at a time when we need to undergo some serious health disorder. These health disorders are very expensive by nature and we may need the help from some sources to meet the expenses of this treatment. As we all know, the cost of medical treatment has become very costly and a person from the lower or middle income group cannot think about such a costly treatment. A health insurance program is a service of the insurance companies that keeps your ensured against any serious illness like cancer. If, unfortunately, happen to suffer from this serious disease ever in our life, we would not be worried about the cost of treatment as we can get the sum for treatment. As far as success of treatment is concerned, it is not sure, however, our family gets a huge sum of money if we happen to die in the process of our treatment. The advantage of this health insurance program is very unique. we need not spend a penny from our pocket and the whole cost of treatment is borne by the insurance company. It is a great relief for the members of our family as well because they need not worry about our treatment. A health insurance program is a very useful investment because it helps us at the time when you need the money most. If we do not have the health insurance program for our self, then will be in deep trouble when a
HEALTH INSURANCE Page 10
VIVEK COLLEGE OF COMMERCE
situation like occurs in front of you and leaves you in want of a huge sum of money. 2.4 FEATURE OF HEALTH INSURANCE 1. Premium: The amount the policy-holder or his sponsor (e.g. an employer) pays to the health plan to purchase health coverage. 2. Deductible: The amount that the insured must pay out-of-pocket before the health insurer pays its share. For example, policy-holders might have to pay a $500 deductible per year, before any of their health care is covered by the health insurer. It may take several doctor's visits or prescription refills before the insured person reaches the deductible and the insurance company starts to pay for care. 3. Co-payment: The amount that the insured person must pay out of pocket before the health insurer pays for a particular visit or service. For example, an insured person might pay a $45 co-payment for a doctor's visit, or to obtain a prescription. A co-payment must be paid each time a particular service is obtained. 4. Coinsurance: Instead of, or in addition to, paying a fixed amount up front (a co-payment), the co-insurance is a percentage of the total cost that insured person may also pay. For example, the member might have to pay 20% of the cost of a surgery over and above a co-payment, while the insurance company pays the other 80%. If there is an upper limit on coinsurance, the policy-holder could end up owing very little, or a great deal, depending on the actual costs of the services they obtain.
HEALTH INSURANCE
Page 11
VIVEK COLLEGE OF COMMERCE
5. Exclusions: Not all services are covered. The insured are generally expected to pay the full cost of non-covered services out of their own pockets. 6. Coverage limits: Some health insurance policies only pay for health care up to a certain dollar amount. The insured person may be expected to pay any charges in excess of the health plan's maximum payment for a specific service. In addition, some insurance company schemes have annual or lifetime coverage maximums. In these cases, the health plan will stop payment when they reach the benefit maximum, and the policyholder must pay all remaining costs. 7. Out-of-pocket maximums: Similar to coverage limits, except that in this case, the insured person's payment obligation ends when they reach the out-of-pocket maximum, and health insurance pays all further covered costs. Out-of-pocket maximums can be limited to a specific benefit category (such as prescription drugs) or can apply to all coverage provided during a specific benefit year. 8. Capitation: An amount paid by an insurer to a health care provider, for which the provider agrees to treat all members of the insurer. 9. In-Network Provider: (U.S. term) A health care provider on a list of providers preselected by the insurer. The insurer will offer discounted coinsurance or co-payments, or additional benefits, to a plan member to see an in-network provider. Generally, providers in network are providers who have a contract with the insurer to accept rates further discounted
HEALTH INSURANCE
Page 12
VIVEK COLLEGE OF COMMERCE
from the "usual and customary" charges the insurer pays to out-ofnetwork providers. 10. Prior Authorization: A certification or authorization that an insurer provides prior to medical service occurring. Obtaining an authorization means that the insurer is obligated to pay for the service, assuming it matches what was authorized. Many smaller, routine services do not require authorization. 11. Explanation of Benefits: A document that may be sent by an insurer to a patient explaining what was covered for a medical service, and how payment amount and patient responsibility amount were determined. Prescription drug plans are a form of insurance offered through some health insurance plans. In the U.S., the patient usually pays a copayment and the prescription drug insurance part or all of the balance for drugs covered in the formulary of the plan. Such plans are routinely part of national health insurance programs. For example in the province of Quebec, Canada, prescription drug insurance is universally required as part of the public health insurance plan, but may be purchased and administered either through private or group plans, or through the public plan. Some, if not most, health care providers in the United States will agree to bill the insurance company if patients are willing to sign an agreement that they will be responsible for the amount that the insurance company doesn't pay. The insurance company pays out of network providers according to "reasonable and customary" charges, which may be less than
HEALTH INSURANCE Page 13
VIVEK COLLEGE OF COMMERCE
the provider's usual fee. The provider may also have a separate contract with the insurer to accept what amounts to a discounted rate or capitation to the provider's standard charges. It generally costs the patient less to use an in-network provider. 2.5 FUNCTIONS OF HEALTH INSURANCE The primary function of health insurance is to pay those covered expenses, as outlined in the policy, incurred as a result of an accident or illness. It often has two elements, one being hospitalization expenses and the other being for the medical care rendered by a physician or other health care professional. The vast majority of health insurance is employer-based, meaning that people have access to it through their employment. Not all employers offer it, and for those whose employers do not, they are free to obtain individual/family policies on their own. Health insurance comes in a variety of types. These include traditional indemnity plans, which are becoming less common, and an array of managed care plans, including Health Maintenance Organizations and Preferred Provider Organizations. Both of the latter provide medical care on a prepaid basis, but differ in their delivery models, including by the degree of choice of provider that the member retains. Most health insurance plans have deductibles and co-payments, although different terminology may be used. A deductible is an amount that the insured/member must pay before the insurer's liability for payment is
HEALTH INSURANCE Page 14
VIVEK COLLEGE OF COMMERCE
triggered. A co-payment is a form of cost-sharing such that the insurer pays a percentage of a covered expense, and the insured pays the remainder. The size of the deductible and co-payment has an impact on premium. 2.6THE ADVANTAGES OF HEALTH INSURANCE INCLUDE; CUSTOMIZED HEALTH CARE: Her we have direct control over our policy and its benefits, unlike in group coverage. we can negotiate to have certain provisions included or excluded in our policy, and we can choose our deductible amount and co-payments. CHOOSING OUR DOCTOR: Selecting a health care provider including doctors is another advantage of an individual health care policy. THE DISADVANTAGE OF HEALTH INSURANCE INCLUDE The biggest disadvantage is the price. Individual policies can be very expensive, especially if you have high risk potential or pre-existing health problems. Before issuing an health insurance policy, the insurance company usually runs a background check on your personal health history. It is unwise to try to hide any pre-existing conditions from your insurer. Another disadvantage is that all requirements of the insurance company must be fully complied with before you can get health care insurance.
HEALTH INSURANCE
Page 15
VIVEK COLLEGE OF COMMERCE
2.7 CRITERIA FOR CHOOSING A POLICY:Every word of policy terms and conditions is to be read and understood before going for a particular policy. Here are few important points that you can look for while choosing a particular policy. 1. Policy coverage: This term refers to medical conditions under which a policy insures a person. This means a policy may not include every medical condition of a person like most of the policies in India do not include medical expenses from HIV, misuse of drugs and also injuries in riots. 2. Mode of bill payment and claim: This plays a major role during critical situations since certain policies may include conditions wherein the person has to bear part or complete bill expense in the first place and later on can claimed from insurer. This may also depend on the network of hospitals that come under the insurance provider. 3. Network of hospitals: This can be one of the major criteria since the network of hospitals an insurance company covers will give us more options and will make us feel secure during critical situations. This is because cashless claims can be made in these hospitals; the company will have authorized to treat the person while the company takes care of expenses. 4. Premium and other benefits covered: This makes the choice to be economical with added benefits in the basket. For ex: A condition of one of the policies offered by Apollo Munich states includes certain bonuses offered on every claim-free year.
HEALTH INSURANCE Page 16
VIVEK COLLEGE OF COMMERCE
2.8 ELIGIBILITY CRITERIA FOR HEALTH INSURANCE:The person who purchases a policy must be minimum 18 years old. The person who is insured for the policy can be maximum 60-65 years. People who are more than 65 years old can be insured under policies for senior citizens. Certain policies also have a minimum limit for age of the person insured. A policy may cover insurance to people above 3-5 years of age.
Providers of Health Insurance Policy: The following are the popular health insurance policy providers in India HDFC ICICI Apollo Munich Maxbupa
HEALTH INSURANCE
Page 17
VIVEK COLLEGE OF COMMERCE CHAPTER NO. 3 TYPES OF HEALTH INSURANCE
1.TRADITIONAL SERVICE
HEALTH
INSURANCE
OR
FEE-FOR-
Up until about 30 years ago, most people had traditional indemnity coverage. These days, it's often known as "fee-for-service." Indemnity plans are a bit like auto insurance: you pay a certain amount of your medical expenses up front in the form of a deductible and afterward the insurance company pays the majority of the bill. Advances in modern medicine increased the cost of providing health care and made it possible for people to live longer. Those advances caused many insurance companies to look for ways to reduce their costs of doing business, giving managed care the boost it enjoys today. For years, indemnity or fee-for-service coverage was the norm. Under this type of health coverage, we have complete autonomy when it comes to choosing doctors, hospitals and other health care providers. we can refer yourself to any specialist without getting permission, and the insurance company doesn't get to decide whether the visit was necessary. we don't, however, have complete autonomy. Most fee-for-service medicine is managed to a certain extent. For instance, if were not already incapacitated, you may need to get clearance for a visit to the emergency room.
HEALTH INSURANCE Page 18
VIVEK COLLEGE OF COMMERCE
On the down side, fee-for-service plans usually involve more outof-pocket expenses. Often there is a deductible, usually of about $200$2,500 before the insurance company starts paying. Once you've paid the deductible, the insurer will kick in about 80 percent of any doctor bills. You may have to pay up front and then submit the bill for reimbursement, or your provider may bill your insurer directly. Under fee-for-service plans, insurers will usually only pay for reasonable and customary" medical expenses, taking into account what other practitioners in the area charge for similar services. If your doctor happens to charge more than what the insurance company considers "reasonable and customary," you'll probably have to make up the difference yourself. Traditionally, preventive care services like annual check-ups and pelvic exams haven't been covered under fee-for-service plans. But as the evidence mounts that preventive care can prevent more costly illnesses down the road, some insurers are including them. Fee-for-service plans often include a ceiling for out-of-pocket expenses, after which the insurance company will pay 100 percent of any costs. Needless to say, the ceiling is usually pretty high. In a nutshell, feefor-service coverage offers flexibility in exchange for higher out-ofpocket expenses, more paperwork and higher premiums.
HEALTH INSURANCE
Page 19
VIVEK COLLEGE OF COMMERCE
THE ADVANTAGE FFS OR TRADITIONAL INDEMNITY This plan is rarely provided anymore due to its high cost. The advantage of this health care plan is that it allows you to choose any health care provider you want. People who want the freedom to select their own doctor, and who are willing to pay more for insurance chose this plan. THE DISADVANTAGES OF FFS'S ARE THAT; There are no financial incentives to reduce patient financial responsibility, and There is an absence of cost control which creates high premiums.
2.MANAGED CARE Managed care has been around in one form or another since the 1930s, but it really took off in the last 10 years. As it grew, it evolved, leaving us with three basic types of managed care plans. Today, the majority of people with private health insurance have some type of managed care. Although there are important differences among the different types of managed care plans, there are some similarities. All managed care plans involve an arrangement between the insurer and a selected network of health care providers, and they offer policyholders significant financial incentives to use the providers in that network. There are usually explicit standards for selecting providers and a formal procedure to assure quality care.
HEALTH INSURANCE
Page 20
VIVEK COLLEGE OF COMMERCE
Health care costs have seen a phenomenal rise in the recent times. This has led the customers to insure not only themselves but their family members also. It will cover future medical expenses and other related requirements if it ever arises. The need to insure has gained more importance amongst older generation who is either retired or will retire in the near future. Let us discuss the types of medical insurances available in the market. 3. MEDICAL INSURANCE This is typically a hospitalization cover and reimbursement of the medical expenses incurred in respect of covered disease or surgery while the insured was admitted in the hospital as a patient. Different types of medical insurances are available in the market like individual medical insurance, group medical insurance and overseas medical insurance. There are health policies that reimburse you the actual hospitalization cost for treatment of any disease and are offered by the non-life insurers only. These policies are popularly called "Mediclaim" policies. Other types of health insurances are provided by both the life and non-life insurers.
4. CRITICAL ILLNESS INSURANCE Critical Illness plan insures you against the risk of serious illnesses in return of a premium you are required to pay. This gives you the same security of knowing that a guaranteed cash sum will be paid if the unexpected happens and you are diagnosed with any one of the critical
HEALTH INSURANCE Page 21
VIVEK COLLEGE OF COMMERCE
illness. Sometimes a critical illness can change your lifestyle in addition to help within the home or the family. In this type of health insurance plan, the insured receives a lump sum amount within a few days of diagnosing critical illness. Once this lump sum is paid, the plan ceases to remain in force. Typically, a critical illness plan would provide cover for the illnesses mentioned below. Aorta graft surgery Cancer Coronary artery bypass surgery First heart attack Kidney failure Major organ transplant Multiple sclerosis Paralysis Primary pulmonary arterial hypertension Stroke
5.PREFERRED PROVIDER ORGANIZATIONS (PPOS) One step over the managed care border is the Preferred Provider Organization. PPOs have made arrangements for lower fees with a network of health care providers. PPOs give their policyholders a financial incentive to stay within that network. For example, a visit to an in-network doctor might mean you'd have a $10 co-pay. If you wanted to see an out-of-network doctor, you'd have to pay the entire bill up front and then submit the bill to your insurance
HEALTH INSURANCE Page 22
VIVEK COLLEGE OF COMMERCE
company for an 80 percent reimbursement. In addition, you might have to pay a deductible if you choose to go outside the network, or pay the difference between what the in-network and out-of-network doctors charge. With a PPO, you can refer yourself to a specialist without getting approval and, as long as it's an in-network provider, enjoy the same copay. Staying within the network means less money coming out of your pocket and less paperwork. Preventive care services may not be covered under a PPO. Exclusive Provider Organizations are PPOs that look like HMOs. EPOs raise the financial stakes for staying in the network. If you choose a provider outside the network, you're responsible for the entire cost of the visit. THE ADVANTAGE OF PREFERRED PROVIDER
ORGANIZATION This plan is a combination of a Traditional Indemnity plan and an HMO plan. The advantages this plan offer is that There are financial incentives to see doctors in the PPO network Many services require just a co- payment for outpatient visits or prescriptions You can see a physician who is not part of the PPO network at a reduced rate.
HEALTH INSURANCE
Page 23
VIVEK COLLEGE OF COMMERCE
THE DISADVANTAGES OF PPO'S INCLUDE; Deductibles and coinsurance are applied for many services such as hospitalization. Claims are submitted by the medical provider. The premiums and employee contribution are higher than an HMO plan, but lower than a Traditional Indemnity plan.
6.POINT-OF-SERVICE (POS) Point-of-service plans are similar to PPOs, but they introduce the gatekeeper, or Primary Care Physician. You'll need to choose your PCP from among the plan's network of doctors. As with the PPO, you can choose to go out of network and still get some kind of coverage. In order to get a referral to a specialist, though, you usually must go through your PCP. You can still choose to refer yourself, but it'll mean more hassles and more money coming out of your pocket. If your PCP refers you to a doctor who is out of the network, the plan should pick up most of the cost. But if you refer yourself out, then you'll probably have to deal with more paperwork and a smaller reimbursement. You may also have to pay a deductible if you go outside the network. POS plans may also cover more preventive care services, and may even offer health improvement programs like workshops on nutrition and smoking cessation, and discounts at health clubs.
HEALTH INSURANCE Page 24
VIVEK COLLEGE OF COMMERCE
THE ADVANTAGE OF POINT OF SERVICE This plan is more flexible than an HMO plan, but requires you to select a primary care physician. Its advantages include; The choice to visit a doctor outside the network and still receive coverage, thought the amount covered will be substantially less than if you went to a doctor within the POS network. This plan offers more preventive care and well-being services like workshops on quitting smoking and health club discounts. THE DISADVANTAGES OF POS'S ARE THAT; You must choose a primary care physician & If you may choose to see a doctor outside the network without permission from your PCP, you are likely to receive only a nominal payment, if any at all.
7.HEALTH MAINTENANCE ORGANIZATIONS (HMOS) Most of the time, when you talk about HMOs, you're really talking about closed-panel HMOs -- the least expensive, but least flexible type of health plan. They also tend to be geared more toward members of group plans than individuals. In exchange for a low co-payment (or sometimes no co-pay at all), low premiums and minimal paperwork, an HMO requires that you only
HEALTH INSURANCE Page 25
VIVEK COLLEGE OF COMMERCE
see its doctors, and that you get a referral from your primary care physician before you see a specialist. If you can still pick up the phone, you'll probably need to get clearance before you can visit the emergency room. An HMO may have central medical offices or clinics (such as those used by Kaiser Permanente), or it may consist of a network of individual practices. In general, you must see HMO-approved physicians or pay the entire cost of the visit yourself. HMOs have the best reputation for covering preventive care services and health improvement programs THE ADVANTAGE OF HEALTH MAINTENANCE
ORGANIZATION These plans have become very popular as they are both comprehensive and cheap. With an HMP plan there are no deductibles or coinsurance expenses, only a co-payment. Another advantage of this health care plan is that the cost of premiums and employee contributions are low due to the presence of cost control features. Here paperwork is minimal as there are no claims to submit. THE DISADVANTAGES HOWEVER ARE THAT; You can only see a doctor who belongs to the HMO network Only your primary care doctor can recommend a specialist And there is a larger number of cost controls elements in the plan such as authorizations, referrals, etc.
HEALTH INSURANCE
Page 26
VIVEK COLLEGE OF COMMERCE
8.TRAVEL HEALTH INSURANCE HTH Worldwide is a leader in helping world travelers gain access to quality healthcare services all around the globe. HTH combines ongoing research, a contracted global community of physicians and hospitals, advanced Internet applications, and wide experience in international health insurance to ensure customers' health, safety and peace of mind. Founded in 1997 as Highway To Health, Inc., HTH Worldwide has grown to become a leading provider of international health insurance programs and an innovator in online healthcare information, medical assistance and insurance services around the globe. Presently, HTH annually provides health insurance products or services to over 650,000 individuals who travel, study or live outside of their home country.
HTH Worldwide offers three types of travel health insurance plans. 8.1 TravelGap - Travel Medical Insurance Offers a variety of medical limits and deductibles For trips up to 6 months for ages 84 and younger Covers pre-existing conditions for medical services and medical evacuation Benefits include: Doctor office visits Inpatient hospital services
HEALTH INSURANCE Page 27
VIVEK COLLEGE OF COMMERCE
Emergency services Ambulance services prescription drugs View Single Trip Benefits Brochure View Multi-Trip Benefits Brochure
8.2Trip Protector - Trip Protection Coverage for trip cancellation, interruption and lost baggage Up to $1,000,000 medical and medical evacuation coverage Trip delay, flight delay, rental car damage, terrorism and more view Benefits Brochure
8.3Global Student - For Students Studying Abroad Global Student USA Designed for international students studying in the US $250,000 coverage per year Basic medical covered 100% up to first $5,000 US Students Abroad Designed for US study abroad students $100,000 coverage per year Basic medical covered 100% up to first $10,000
HEALTH INSURANCE
Page 28
VIVEK COLLEGE OF COMMERCE
9.SHORT TERM HEALTH INSURANCE Short Term health insurance from Assurant Health provides you with temporary coverage for periods of up to one year. The plans are designed to fill gaps in your medical coverage and offer the following features. Coverage is available for periods of 30 - 360 days. You may be covered as soon as the next day. You are covered anywhere in the US. You may choose your own doctors and hospitals. Assurant Individual & Family health insurance plans are available in all states EXCEPT: CT, MA, NJ, NY, & VT. Some benefits include: Doctor office visits Prescription drug coverage Hospital, lab, x-ray and ambulance $2 million lifetime benefit The following may benefit from Short Term health insurance: People between jobs People waiting for employer-sponsored benefits to begin Temporary or seasonal employees Early retirees
HEALTH INSURANCE Page 29
VIVEK COLLEGE OF COMMERCE
CHAPTER NO.4 TYPES OF HEALTH INSURANCE PLAN
Health Insurance Plans are segregated into three categories, firstly the Mediclaim Plans by Non-Life or General Insurance Companies, secondly the Hospitalization Cash Policy by both Life & Non-Life Insurers and thirdly the Critical Care Plans offered by both Life & Non-Life Insurers.
1.MEDICLAIM POLICY: It is basically a reimbursement plan offered by General Insurers wherein the insured gets reimbursed of the total bill amount of the medical expenses to the extent of an agreed sum assured. It includes the room charges, ICU charges, surgery & doctor charges etc. It includes a lot of exclusions which the policy holder must read before buying the Mediclaim. The Mediclaim includes the following two further categories: a).Family Floater Plan: It is a very common plan these days which covers your entire family under one premium payment giving coverage to the family members together. This plan is being offered by almost all the General Insurance Companies with a specific criterion of covering individuals in the age group between 90days and 55years.
HEALTH INSURANCE
Page 30
VIVEK COLLEGE OF COMMERCE
For instance a person wants a health insurance for himself, his spouse & their children, the Family Floater plan offers insurance coverage to the entire family under one premium payment. Lets take an example wherein the person insures himself, his spouse & the dependent children with the individual insurance plans with a sum assured of Rs. 1 lakh each, he ends up paying premium ranging between Rs. 1000 - Rs. 2000 for each family member. On the other hand if the person would have opted for the family floater plan with the sum assured of Rs. 3 lakhs, the total premium would surely be less than the separate premium payments in individual health insurance plans. Moreover the separate health plan holds the cover of only Rs. 1 lakh as against Rs. 3 lakh in case of the Floater plan thus helping the family in case the medical treatment costs go beyond that.
b) Group Mediclaim Insurance: It is the second variant of Mediclaim which covers a group of individuals simultaneously. This form of insurance includes the category of Employers Health Insurance Cover wherein the sum assured normally varies between Rs. 15,000 and Rs.5, 00,000.
HEALTH INSURANCE
Page 31
VIVEK COLLEGE OF COMMERCE
2. HOSPITALIZATION CASH POLICY: It is a plan offered by both Life & Non-Life Insurers wherein the Insured gets pre-determined cash benefit on a daily basis irrespective of the hospitalization expenses being incurred. It is not a fully comprehensive health insurance plan because it doesnt cover the cost of medical treatment but pays lump sum amount to the policy holder on per day basis during the treatment/hospitalization. It acts a complimentary plan to the Mediclaim plans. TATA-AIG General Insurance & Royal Sundaram offer Hospital cash benefit plan among Non-Life Insurers. 3.CRITICAL-CARE PLAN: It is offered by both Life & General Insurers covering an individual for certain specified critical illnesses like cancer, stroke etc. This is also offered as a rider by Life Insurance companies for quite some time now attached to their Life Insurance Plans. You must take a cover either as a rider or as a standalone plan in your portfolio. 4.CASHLESS HOSPITALIZATION: Cashless settlement implies that an individual doesnt have to settle a hospital bill out of his pocket; rather the bill gets settled directly by the insurance company. When you buy a Health Plan you are issued a Health Card along with the policy documents which would entitle you to get cashless claim at any of the companys network hospitals.
HEALTH INSURANCE
Page 32
VIVEK COLLEGE OF COMMERCE CHAPTER NO.5 TAX BENEFITS ON HEALTH INSURANCE PLAN
Health Insurance Tax Benefits Health Insurance products are eligible for tax benefits under section 80D of the Income Tax Act, 1961. Premium paid under health insurance holds a tax deduction upto Rs 15,000 for you, your spouse and dependent children. Further more you can also claim another Rs. 15, 000 for tax deduction for your parents, in case of senior citizens (65 years or more) the above deductions are increased to Rs. 20,000 Health insurance has many benefits- health cover, critical illness benefit and additional covers. Along with this you can also avail tax benefits under Section 80D of the Income tax Act 1961. You can avail up to Rs 15,000 and Rs 20,000 for senior citizens. Section 80D as per Income tax Act 1961 is as follows: Deduction in respect of health insurance premia 80D are:
(1). In computing the total income of an assessee, being an individual or a Hindu undivided family, there shall be deducted such sum, as specified in sub-section (2) or sub-section (3), payment of which is made by any mode, other than cash, in the previous year out of his income chargeable to tax.
HEALTH INSURANCE Page 33
VIVEK COLLEGE OF COMMERCE
(2). Where the assessee is an individual, the sum referred to in subsection (1) shall be the aggregate of the following, namely: A. The whole of the amount paid to effect or to keep in force an insurance on the health of the assessee or his family [or any contribution made to the Central Government Health Scheme] as does not exceed in the aggregate fifteen thousand rupees; and B. The whole of the amount paid to effect or to keep in force an insurance on the health of the parent or parents of the assessee as does not exceed in the aggregate fifteen thousand rupees. Explanation - For the purposes of clause (a), family means the spouse and dependent children of the assessee.
(3). Where the assesses is a Hindu undivided family, the sum referred to in sub-section (1) shall be the whole of the amount paid to effect or to keep in force an insurance on the health of any member of that Hindu undivided family as does not exceed in the aggregate fifteen thousand rupees.
(4). Where the sum specified in clause (a) or clause (b) of sub-section (2) or in sub-section (3) is paid to effect or keep in force an insurance on the health of any person specified therein, and who is a senior citizen, the provisions of this section shall have effect as if for the words fifteen
HEALTH INSURANCE Page 34
VIVEK COLLEGE OF COMMERCE
thousand rupees, the words twenty thousand rupees had been substituted. Explanation - For the purposes of this sub-section, senior citizen means an individual resident in India who is of the age of sixty-five years or more at any time during the relevant previous year. (5). The insurance referred to in this section shall be in accordance with a scheme made in this behalf by A .the General Insurance Corporation of India formed under section 9 of the General Insurance Business (Nationalisation) Act, 1972 (57 of 1972) and approved by the Central Government in this behalf; or B .any other insurer and approved by the Insurance Regulatory and Development Authority established under sub-section (1) of section 3 of the Insurance Regulatory and Development Authority Act, 1999 (41 of 1999).] The above act states that if an individual buys health insurance, then the premium paid is deductible from his chargeable income. The premium that is deducted cannot exceed 15,000 for individual and Rs 20,000 for senior citizen (aged above 65). Illustration: a. Anil has annual salary is Rs 8 lacs 10 thousand and buys health insurance for himself for Rs 20,000. Amount of 15,000 would be deducted from his taxable income.
HEALTH INSURANCE
Page 35
VIVEK COLLEGE OF COMMERCE
b. Anil buys health insurance for himself and his parents who are both senior citizens. The annual premium he pays for the same is 50,000. Amount of 35,000 can be deducted from taxable income to avail tax benefits. If Anil is in the tax bracket of 30% already, he gets taxation benefit of Rs 10,815.
Health Insurance Covers & Benefits Room & Boarding expenses: There are further limits to this feature varying from company to company. Ambulance Charges: They are normally covered upto Rs. 1000. ICU charges, doctor, consulting, anesthetist and surgeon fees, operation and other diagnostic and surgical material costs are covered. Day-Care expenses such as Chemotherapy, Dialysis & Radiotherapy etc. Pre & Post Hospitalization Expenses which normally are 30 days prior and 60 days after hospitalization. Cashless Hospitalization is offered by almost all Non-Life Insurers.
HEALTH INSURANCE
Page 36
VIVEK COLLEGE OF COMMERCE
Limited-Benefit Health Plans Health Access is a limited-benefit health plan offered by Assurant Health. The plans cover certain services such as doctor office visits and prescription drugs up to a set dollar amount. They are not major medical health insurance plans and should not be used to replace such coverage.
Some of the covered services include: Doctor office visits Inpatient services (Hospital) Prescription drugs Emergency services Ambulance Outpatient Lab & X-ray Surgical services
HEALTH INSURANCE
Page 37
VIVEK COLLEGE OF COMMERCE
CHAPERT NO.6 CLAIM PROCEDURE
we should walk into a network hospital & get the treatment done & the bills paid through the Health Card. In case of hospitalization we need to give the card number to the network hospital, we must pre-authorize from the TPA (Intermediary between the Insurance Company & the hospital) & will process the cashless settlement after the verification of our policy details.we should know the formalities required for cashless settlement as some insurance companies are required to be notified 48 hours before hospitalization. If we dont opt for cashless settlement, we need to settle bills at the hospital and get them reimbursed later. CLAIM PROCEDURE Claims are broadly of two types: 1. Cashless Claims and 2 .Reimbursement Claims
HEALTH INSURANCE
Page 38
VIVEK COLLEGE OF COMMERCE
GENERAL CLAIM PROCEDURE: As soon as there is a need for hospitalisation, please intimate the HCMT/TPA on 24x7 Customer Helpline number as mentioned in your Health Card/Policy Schedule. You are required to furnish the following information while intimating a claim: a. Contact Numbers b. Policy Number (as on the Health Card//Policy Schedule) c. Name of Insured person who is hospitalised d. Nature of sickness/accident e. Date & Time in case of accident, commencement date of symptom of disease in case of sickness f. Location of accident . The benefit of choosing a network hospital is that we can avail of "Cashless Facility" while we are hospitalised whereas we will have to settle our hospital bills in the hospital which is outside our network. we have to follow the procedures listed below to get the services in different situations.
HEALTH INSURANCE
Page 39
VIVEK COLLEGE OF COMMERCE
1.PROCEDURES FOR "CASHLESS FACILITY" "Cashless Facility" is the service wherein we need not pay our hospitalisation bills to the hospital either at the time of admission or at the time of discharge from the hospital. This facility is available only at our Network Hospitals. To avail the "Cashless Facility" we need to fill "Cashless request form" available in all the network hospitals. The hospitals will co-ordinate to get the authorisation from the HCMT/TPA for such "Cashless Facility". This authorisation along with a copy of the card issued by us needs to be given to the Hospital at the time of admission. we are also required to carry a Photo ID Card. Please Note: HCMT/TPA shall authorise "Cashless Facility" at the Network Hospitals in respect of treatments which are covered under the policy. "Cashless Facility" may be denied by the HCMT/TPA in some of the situations as listed below.
In case of any doubt on coverage of the present ailment/ treatment under the policy
If the information sent by you /hospital is insufficient The ailment/condition etc. not being covered under the policy If the request for preauthorization is not sent in time Denial of "Cashless Facility" is not denial of treatment. we may continue with the treatment, pay for the services to the hospital, and later submit the claim for processing and reimbursement.
HEALTH INSURANCE
Page 40
VIVEK COLLEGE OF COMMERCE
1.1 Emergency hospitalization: Step 1. Take admission into the hospital. Step 2. As soon as possible, Intimate the claim at the call centre, obtain the pre-authorisation form from hospital and get the same filled in and signed by the attending doctor. Step 3. Fax the pre-authorisation form to the HCMT/TPA along with necessary medical details like investigation report etc at the number mentioned in our Health Card/Policy Schedule. The hospital will coordinate for the same. Step 4. (Option I) A. If an authorisation for "Cashless Facility" from HCMT/TPA has been received i. At the time of discharge
a. we will be required to pay for all such expenses that are not payable as per the terms of the policy. b. Verify the bills and sign on all the bills c. Leave the original discharge summary and other investigation reports with the hospital. Retain a Xerox copy for your records Step 4. (Option II) B. In case "Cashless Facility" has been denied by HCMT/TPA I. At the time of discharge settle the hospital bills in full and collect all the original bill documents and reports II. Lodge your claim with HCMT/TPA for processing and reimbursement
HEALTH INSURANCE Page 41
VIVEK COLLEGE OF COMMERCE
1.2 Planned hospitalization: Step 1. Please co-ordinate with our doctor and the hospital and send all the details about the planned hospitalisation including the plan of treatment, cost estimates etc. to HCMT/TPA. This may be sent at least 2 days prior to the planned admission. Step 2. (Option I) A. If authorisation for "Cashless Facility" from TPA has been received I. At the time of admission, present the authorisation letter and photo ID card to the hospital II. a. b. c. At the time of discharge Pay for those expenses that are not reimbursable under the policy Verify the bills and sign on all the bills. Leave the original discharge summary and other investigations
reports with the hospital. Retain a Xerox copy for your records Step 2. (Option II) B. In case "Cashless Facility" has been denied by HCMT/TPA a. Get admitted and take treatment b. At the time of discharge settle the hospital bills in full and collect all the original bill documents and reports c. Lodge your claim with HCMT/TPA for processing and reimbursement "Please note that failure to intimate HCMT/TPA as soon as the hospitalisation takes place can invalidate our claim."
HEALTH INSURANCE
Page 42
VIVEK COLLEGE OF COMMERCE
2.PROCEDURES FOR REIMBURSEMENT CLAIMS
EMERGENCY HOSPITALISATION Step 1. Take admission into the hospital. Step 2. As soon as possible, intimate the HCMT/TPA about the hospitalisation. Step 3. At the time of discharge, settle the hospital bills in full and collect all the original bills, documents and reports. Step 4. Lodge our claim with HCMT/TPA for processing and reimbursement, by filling in the claim form and attaching required documents as mentioned in the claim form.
2.1Planned hospitalization: Step 1. Intimate HCMT/TPA of the planned hospitalisation. Step 2. Get admitted into the hospital. Step 3. At the time of discharge, settle the hospital bills in full and collect all the original bills, documents and reports. Step 4. Lodge our claim with HCMT/TPA for processing and reimbursement. How to lodge a claim with HCMT/TPA for processing and reimbursement Within 7 days after discharge, please lodge the claim for processing. While submittiing a claim, please make sure that all the documents listed under the document check list are attached.
HEALTH INSURANCE Page 43
VIVEK COLLEGE OF COMMERCE
Document Check list for Hospitalisation, Domiciliary Hospitalisation & Critical illness claims
2.2 Hospitalisation / Day Care Treatment: a. First prescription of doctor with commencement date of the symptom of disease b. Treatment papers along with doctors prescriptions c. Investigation reports (X-ray/Scan/ECG, Laboratory etc) d. Original medical bills and receipt of hospital, doctors, medical shops, diagnostic centre etc supported by Doctor's advice e. Hospital discharge card, in original f. Copy of FIR (if any in case of accident)
2.3 Critical Illness Claims: a. Claim form duly completed b. Original Specialist Doctor's certificate confirming the diagnosis and when the symptoms first occurred c. Relevant Investigation reports (Radiology, Pathology etc) confirming the diagnosis d. Hospital admission & discharge card / certificate
HEALTH INSURANCE
Page 44
VIVEK COLLEGE OF COMMERCE
2.4 Domiciliary Hospitalisation: a. First prescription of doctor with commencement date of the symptom of disease b. Treatment papers along with doctors prescriptions c. Investigation reports (X-ray/Scan/ECG, Laboratory etc) d. Original medical bills and receipt of doctors, medical shops, diagnostic centre etc supported by Doctor's advice e. Copy of FIR (if any in case of accident) f. Certificate from attending Doctor/Physician stating the condition of the patient is not permissible for him/her to be removed to Hospital/Nursing Home or documentary proof of lack of accommodation in Hospital/Nursing Home.
HEALTH INSURANCE
Page 45
VIVEK COLLEGE OF COMMERCE
CHAPTER NO.7 CONCLUSION
Health and medical insurance in India is of recent origin. It took a concerted effort on part of the Government to make it popular by introducing a simple to-operate Mediclaim policy. The features of this policy borrow heavily from internationally successful models of health insurance, while incorporating features that are peculiar to India. This is available not only for individuals to buy but also as a Group cover for employers to offer to employees. Besides Mediclaim there are a few other popular covers in India. With the advent of the private sector both cashless and cashreimbursement are used as system of claim settlement. Service Providers in this case hospitals, Nursing homes and medical practitioners are increasingly seeking tie-ups with insurers to offer their services under health and medical insurance plans.
HEALTH INSURANCE
Page 46
VIVEK COLLEGE OF COMMERCE
BIBLIOGRAPHY WEBSIDE: 1. www.investorwords.com/2289/health_insurance. 2. www.wikipedia.org/wiki/Health_insurance 3. www.healthinsuranceadvice.org/types.html -
BOOKS: 1. Insurance products including pension products. 2. Health insurance
HEALTH INSURANCE
Page 47
Você também pode gostar
- Foregin Direct Investment Finance ProjectDocumento46 páginasForegin Direct Investment Finance ProjectpadmajammulaAinda não há avaliações
- Chanda Kochhar, CEO of ICICI BankDocumento6 páginasChanda Kochhar, CEO of ICICI BankpadmajammulaAinda não há avaliações
- Challenges To Retail Banking in IndiaDocumento2 páginasChallenges To Retail Banking in IndiapadmajammulaAinda não há avaliações
- FDI Finance ProjectDocumento11 páginasFDI Finance ProjectpadmajammulaAinda não há avaliações
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceNo EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceNota: 4 de 5 estrelas4/5 (890)
- The Yellow House: A Memoir (2019 National Book Award Winner)No EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Nota: 4 de 5 estrelas4/5 (98)
- The Little Book of Hygge: Danish Secrets to Happy LivingNo EverandThe Little Book of Hygge: Danish Secrets to Happy LivingNota: 3.5 de 5 estrelas3.5/5 (399)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeNo EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeNota: 4 de 5 estrelas4/5 (5794)
- Never Split the Difference: Negotiating As If Your Life Depended On ItNo EverandNever Split the Difference: Negotiating As If Your Life Depended On ItNota: 4.5 de 5 estrelas4.5/5 (838)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureNo EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureNota: 4.5 de 5 estrelas4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryNo EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryNota: 3.5 de 5 estrelas3.5/5 (231)
- The Emperor of All Maladies: A Biography of CancerNo EverandThe Emperor of All Maladies: A Biography of CancerNota: 4.5 de 5 estrelas4.5/5 (271)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreNo EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreNota: 4 de 5 estrelas4/5 (1090)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyNo EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyNota: 3.5 de 5 estrelas3.5/5 (2219)
- Team of Rivals: The Political Genius of Abraham LincolnNo EverandTeam of Rivals: The Political Genius of Abraham LincolnNota: 4.5 de 5 estrelas4.5/5 (234)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersNo EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersNota: 4.5 de 5 estrelas4.5/5 (344)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaNo EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaNota: 4.5 de 5 estrelas4.5/5 (265)
- The Unwinding: An Inner History of the New AmericaNo EverandThe Unwinding: An Inner History of the New AmericaNota: 4 de 5 estrelas4/5 (45)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)No EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Nota: 4.5 de 5 estrelas4.5/5 (119)
- Day 13 Managed Health CareDocumento30 páginasDay 13 Managed Health CareJonathan DavidAinda não há avaliações
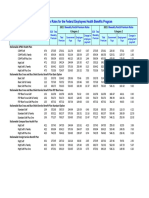
- 2021 FEHB Postal Rates FFSDocumento4 páginas2021 FEHB Postal Rates FFSFedSmith Inc.Ainda não há avaliações
- October 18, 2012 IssueDocumento8 páginasOctober 18, 2012 IssueThe Brown Daily HeraldAinda não há avaliações
- The Doctor Patient Relationship PDFDocumento8 páginasThe Doctor Patient Relationship PDFWagiono Suparan100% (2)
- AHM 250 4 Provider CompensationDocumento16 páginasAHM 250 4 Provider Compensationdeepakraj610Ainda não há avaliações
- Impact of Managed Care On Pharmacy PracticeDocumento18 páginasImpact of Managed Care On Pharmacy Practiceolaakin3Ainda não há avaliações
- Payment in Healthcare OrganizationsDocumento12 páginasPayment in Healthcare Organizationsevans kirimiAinda não há avaliações
- Geriatric Practice PDFDocumento558 páginasGeriatric Practice PDFGemmita Trujillo100% (9)
- AHM 250 SummaryDocumento117 páginasAHM 250 Summarysenthilj82Ainda não há avaliações
- Fee For ServiceDocumento2 páginasFee For ServiceMukoya OdedeAinda não há avaliações
- Finance in Dental CareDocumento42 páginasFinance in Dental CarePuspa AdhikariAinda não há avaliações
- Reading Rehabilitation 11-13-08Documento35 páginasReading Rehabilitation 11-13-08nitin_fernandes29100% (2)
- Canadas Physician ShortageDocumento11 páginasCanadas Physician ShortageFion LamAinda não há avaliações
- Right Care 3. Drivers of Poor Medical CareDocumento13 páginasRight Care 3. Drivers of Poor Medical CareJuan Jose Eraso OsorioAinda não há avaliações
- QBP KidneyDocumento36 páginasQBP KidneyRaka ArifirmandaAinda não há avaliações
- Hospital Business ModelsDocumento8 páginasHospital Business ModelsPOLOKO MHUSIWAAinda não há avaliações
- Clinical Core Laboratory Testing Molinaro, McCudden, Bonhomme & Saenger (Eds.) - 1st Ed. (2017)Documento115 páginasClinical Core Laboratory Testing Molinaro, McCudden, Bonhomme & Saenger (Eds.) - 1st Ed. (2017)Beatriz Belotti100% (1)
- Personal Health NotesDocumento6 páginasPersonal Health NotesMichael ReiferAinda não há avaliações
- Health Policy Brief: Accountable Care OrganizationsDocumento6 páginasHealth Policy Brief: Accountable Care Organizationspalak32Ainda não há avaliações
- Changes in Hospital Competitive StrategyDocumento23 páginasChanges in Hospital Competitive Strategyanantomi100% (1)
- Capitation Payment Method As A Policy Tool, Versus Fee For Services, or The Financial Sustainability of The National Health Insurance in Sudan: Algadarif State Case Study.Documento15 páginasCapitation Payment Method As A Policy Tool, Versus Fee For Services, or The Financial Sustainability of The National Health Insurance in Sudan: Algadarif State Case Study.National Graduate ConferenceAinda não há avaliações
- The Future of Us Healthcare Whats Next For The Industry Post Covid 19Documento13 páginasThe Future of Us Healthcare Whats Next For The Industry Post Covid 19miltechinsightsAinda não há avaliações
- Audit Planning: SGB & CDocumento17 páginasAudit Planning: SGB & CMelanie SamsonaAinda não há avaliações
- Cano Health Investor and Analyst Day Presentation VFFDocumento77 páginasCano Health Investor and Analyst Day Presentation VFFsawilson1Ainda não há avaliações
- Contemporary Nursing Issues Trends and Management 5th Edition Cherry Test BankDocumento39 páginasContemporary Nursing Issues Trends and Management 5th Edition Cherry Test Bankseeressgroined3djz100% (14)
- Hospital Billing ScenariosDocumento7 páginasHospital Billing Scenarioskrishna EnagaluruAinda não há avaliações
- Apollo Hospital CaseDocumento3 páginasApollo Hospital CaseNithya NairAinda não há avaliações
- Evolution of Health Plans and Managed Care ModelsDocumento119 páginasEvolution of Health Plans and Managed Care ModelsMonyNaguAinda não há avaliações
- Banner Page: IHCP Updates Reimbursement Rate For HCPCS Code C9803, Mass Adjusts Claims That Paid IncorrectlyDocumento8 páginasBanner Page: IHCP Updates Reimbursement Rate For HCPCS Code C9803, Mass Adjusts Claims That Paid IncorrectlyIndiana Family to FamilyAinda não há avaliações
- SPR BHB Funding Fact Sheet May 2019Documento5 páginasSPR BHB Funding Fact Sheet May 2019BernewsAdminAinda não há avaliações