Escolar Documentos
Profissional Documentos
Cultura Documentos
Complete Denture Occlusion
Enviado por
Amar BhochhibhoyaDescrição original:
Título original
Direitos autorais
Formatos disponíveis
Compartilhar este documento
Compartilhar ou incorporar documento
Você considera este documento útil?
Este conteúdo é inapropriado?
Denunciar este documentoDireitos autorais:
Formatos disponíveis
Complete Denture Occlusion
Enviado por
Amar BhochhibhoyaDireitos autorais:
Formatos disponíveis
EVALUATION HYPERPLASIA
CHARLES University
OF TREATMENT OF INFLAMMATORY OF THE PALATE
PAPILLARY
L.
BOLENDER,
AND GEORGE YAMANE,
D.D.S., MS.," RALPH D. D.D.S., Ph.D.*"*
School o/ Dentistry,
SWENSON,
D.D.S., M.S.,""
of Washington,
Seattle,
Wash.
have been suggested as being involved in the etiology and V treatment of inflammatory papillary hyperplasia of the palate. Poor oral hyARIOUS FACTORS
giene,r monilial infection,2 relief chambers,3movement of dentures in function,4 illfitting dentures, and faulty occlusion6 are some of the causesof this alteration in the tissues of the palate. These changes have been treated by the use of medicaments,2 removal of the dentures for varying lengths of time,ls fabrication of new, adequately fitting dentures, and different methods of surgical removal of the lesion.4p5,8 The purpose of this investigation was to evaluate the effects of the fabrication of new dentures with and without surgical removal of the lesion.
PATIENT INFORMATION
Twenty wearers of complete dentures exhibiting inflammatory papillary hyperplasia of the palate served as subjects. Four subjects were men and sixteen were women. Their ages ranged from 22 to 75 with a mean of 50 years. They had been wearing dentures from 6 to 30 years. They had been wearing their present dentures from 2 to 30 years with a mean of 10.3 years. All the maxillary dentures had palatal relief, with 11 of the 20 having a deep relief of more than .5 mm. in depth. The retention and stability of all the dentures were evaluated as poor. The oral hygiene of th,e subjects ranged from fair to poor with most of the subjects in the poor category. The overall size of the lesions ranged from 5 mm. by 15 mm. up to coverage of the entire palate. Multiple papillary projections that varied in diameter and depth were evident. The depth of the crevices between the projections observed ranged from 2 to 5 mm. as recorded by a periodontal probe. Erythema was present
Read before the I.A.D.R. in Pittsburgh, Pa.: Pacific Coast Society of Prosthodontists in Vancouver, B. C.; and The American Academy of Prosthetics in Chicago, Ill. *Associate Professor and Chairman, Department of Prosthodontics. **Clinical Associate, Department of Oral Surgery. ***Professor and Chairman, Departments of Oral Diagnosis, Oral Medicine and Oral Roent. genography, School of Dentistry, University of Minnesota, formerly Assistant Professor, Depart. ment of Oral Biology. 1013
BOLENDER,
SWENSON,
AND
YAMANE
J. Pros. Den. November-December, 1965
but varied in severity. Symptoms were reported by only 2 subjects; one symptom was a burning sensation, and the other was an itching sensation. Specimens for biopsy were secured, and clinical evaluation of the oral cavity was conducted. A positive histologic confirmation of the presence of inflammatory papillary hyperplasia was required before placing the subject in the study.
DESCRIPTION OF LESION
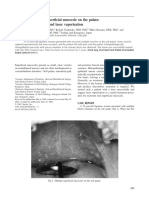
A representative lesion is shown in Fig. 1,A. The lesion is well demarcated from the surrounding tissue ; however, the papillary proj,ections are not clearly seen. A jet of air has been directed to the same palate in Fig. l,B, to demonstrate how the papillary projections become more evident. The use of an air syringe has proved to be the most useful diagnostic instrument to detect clinically the presence of this type of palatal lesion. Fig. 2. is a low magnification view of the lesion shown in Fig. 1. The typical features of an inflammatory papillary hyperplasia of the palate are evident. The epithelium was hyperplastic and thrown into several broad fingerlike projections. Keratinization was not a prominent feature, but many of the crevices were filled with parakeratin. The rete pegs were projecting deep into the underlying lamina propria. The basal cells were well organized, and were sharply demarcated from
Fig. 1.-A reprdsentative lesion from a subject in Group 1. A, are not clearly seen. B, The same palate after a jet of air was directed of distinct papillary projections.
The papillary on it. Note
projections the presence
ICE 6
INFLAMMATORY
PAPILLARY
HYPERPLASIA
OF PALATE
101.5
the underlying lamina propria by a distinct basement membrane. The underlying lamina propria consisted of a loose fibrous connective tissue stroma with a variable amount of edema. The lamina propria was heavily infiltrated with lymphocytes and plasma cells.
OUTLINE OF STUDY
The subjects were evenly divided into two groups in regard to age, sex, and lesion size (Fig. 3). The therapy for the 10 subjects in Group I consisted of fabrication of nem complete dentures. The dentures were made by dental students under the direct supervision of one of the investigators (C.L.B.). No treatment of the lesions was attempted except to encourage the patients to leave the dentures out of the mouth as much as possible prior to making the final impressions. This was adopted fol Group I because it is a procedure commonly used in general practice. The neM dentures were processed in a methylmethacrylate acrylic resin with no relief chamber. Any necessary palatal relief was determined by the use of a disclosing paste following the insertion of the dentures. At 12 months following the insertion of the new dentures, the lesions were again clinically and histologically evaluated. The therapy for the 10 subjects in Group II consisted of supraperiosteal removal of the lesions with a high frequency electrical cutting current instrument. A temporary lining was placed in the existing dentures, immediately following the surgery, and changed at the two and three week postoperative intervals. The palate:; of the subjects were evaluated frequently until healing was complete. Following
Fig. hyperplastic
2.-A and
low
power thrown
microscopic
into broad,
view fingerlike
of
the lesion projections.
shown
in
Fig.
1. The
epithelium
is
1016
BOLENDER,
SWENSON,
AND
YAMANE
November-D&i%;
sufficient healing, new dentures were made and inserted following the same procedure as for Group I. At 12 months after operation, the palatal mucosa was again clinically and histologically evaluated.
PROCEDURE
Group I.-A representative lesion from Group I is shown in Fig. 1. The appearance of this same lesion is seen in Fig. 4 after new dentures had been worn for 12 months. Virtually no clinical change was evident for this subject. Following wearing of the new dentures for 12 months, a second biopsy was made. Care was taken to secure the biopsy specimen from an area away from the original biopsy site, yet remaining in the most involved part of the lesion. Fig. 5 is the histologic section of the lesion as shown in Fig. 4. The broad, fingeriike projections and inflammatory, cellular exudate are still present, indicating minimal change from the pretreatment biopsy (Fig. 2). Half the subjects in Group I showed no change in severity of the papillary
SUBJECTS I. Clinical 2. Biopsy (20) Evaluation (preop.)
GROUP
I I
(IO)
GROUP
II
(IO)
Surgery
f
I
New
Dentures
Clinical Biopsy
1 1
New
Dentures
Evaluation
Clinical Biopsy
Evaluation (I2 mo.)
(I2 mod
Fig.
3.-Outline
of the study.
Fig. I.-The of new dentures
clinical appearance for 12 months.
of the
same
lesion
shown
in Fig.
1 following
the wearhig
iz%Z6
INFLAMMATORY
PAPILLARY
HYPERPLASIA
OF PALATE
101.7
hyperplasia. The other half displayed a moderate reduction in erythema that was confirmed histologically, while the remainder of the microscopic and clinical features remained unchanged. Group II.-A representative lesion from Group II is shown in Fig. 6. The lesion covered a large portion of the palate. The histologic picture of the biopsy (Fig. 7) is very similar to those of the subjects in Group 1. Note the projections of epithelium and the inflammatory exudate. Using a wire loop, (Fig. S) one of the investigators (K.D.S.) performed the operation with a high-frequency electrical cutting current. The lesion was removed
Fig. 5.-A of new dentures biopsy.
low-power microscopic
for 12 months. Minimal
view of the lesion shown in Fig. change is evident in comparison
4 following the wearing with the pretreatment
three
Fig. 6.-A fourths
representative of the palate.
lesion from The maximum
a subject in Group II. The lesion covers approximately depth of the papillary projections was 3 mm.
1018
BOLENDER,
SWENSON,
AND
YAMANE
November-D:&%?,
?;%
Fig.
7.-A
low-power
microscopic
view
of the lesion
shown
in Fig. 6.
Fig. 8
Fig. 9
Fig. %-Half instrument. Fig. 9.-The
of the lesion
lesion has been
has
been
removed removed.
by
using
the
wire
loop
elLectrical
cu .tting
completely
Volume Number
15 6
INFLAMMATORY
PAPILLARY
HYPERPLASIA
OF PALATE
1019
to a subepithelial level just beneath the grooves in the papillary hyperplasia and was always supraperiosteal. Local anesthesia was used. An outline of the preoperative biopsy site can be seen near the midline. Specimens for biopsy were removed by a scalpel. The operation is complete in Fig. 9. Bleeding was less with the cutting current wire loop than with sharp metal cutting instruments. Following surgery, a lining of hard-setting zinc oxide and eugenol impression paste was placed in the subjects old denture (Fig. 10). This lining was changed at the two and three week postoperative intervals. Discomfort of varying degrees, exhibited during the first week, was controlled most effectively by the application of a topical anesthetic ointment. No bleeding problems were encountered after operation. Considerable healing had occurred after 2 weeks (Fig. 1 1 ), and the soreness had gone. The healing was essentially complete at 4 weeks (Fig. 12). Several small erythematous areas can still be seen. The healing was complete at 4 weeks in nine subjects and at 3 weeks in one subject. At 4 weeks after operation, the old denture was relined by the usual procedures using acrylic resin. New dentures were made shortly thereafter. This procedure was followed for all subjects in Group II. Fig. 13 shows the palate maintaining a normal appearance at 3 months postoperative. At 12 months after operation, the palatal mucosa was again evaluated. Clinically, the palate was normal (Fig. 14). Histologically, the tissue appears to be similar to a normal palatal mucosa9 (Fig. 15). A similar result was seen in all subjects of Group II. The epithelium was well differentiated. The penetration of the rete pegs was fairly uniform and, for the most part, inflammatory cells were absent. In some instances, the epithelium showed a well-keratinized layer.
RESULTS
Group I.-Even after new dentures had been worn for twelve months, there was virtually no change in the clinical appearance of the palatal lesion of the subjects in Group I (2 men, 6 women). Half (4) of the subjects showed no clin-i-
Fig. 10.-A hard-setting zinc oxide denture immediately following surgery.
eugenol
impression
paste
lining
was
placed
in the
old
BOLENDER,
SWENSON,
AND
YAMANE
J. Pros. Den. November-December, 1965
Fig. 12
Fig. 14
Fig. Il.-The 2 week postoperative Fig. 12.-The 4 week postoperative right of the midline. Fig. 13.-The 3 month postoperative Fig. 14.-The 12 month postoperative evidence of the original lesion.
result. result. result. result,
Considerable healing has occurred. Note the localized area of inflammation The tissue is maintaining itself. There
to the is no
Fig.
15.-A
low-power
microscopic
view
of the 12 month
postoperative
result.
Volume Number
15 6
INFLAMMATORY
PAPILLARY
HYPERPLASIA
OF
PALATE
1021
TABLE
I.
CLINICAL
AND
HISTOLOGIC
EVALUATION
GROUP
GROUP
II
SUBJECT
i
BEFORE AFTER SUBJECT PREOPERATIVE POSTOPERATI\E
______
: : 1 : :
+ Lesion present. - Lesion absent. Table I. Summary *Dyskeratosis postoperative
T: T z Not available Not available
FM
LItI MW
:: : : + + :: -* Not a&able Not available
E ww FD isk
of investigation present preoperatively biopsy-did not show
and 12 dyskeratosis.
months
postoperatively.
Subsequent
24-month
cal changes in the severity of the papillary hyperplasia. The size and color of the lesions remained the same. The other half (4) of the subjects displayed a moderate reduction in the erythema of the lesion but not in the size of the lesion. The microscopic examination confirmed these findings. It was impossible to maintain contact with 2 subjects in this group (Table I). Group II.-Where the lesions had been surgically removed, there was no clinical and histologic evidence of a return of the lesion in 7 subjects (2 men, 5 women). However, 2 of these subjects exhibited a small localized area about 3 to 4 mm. in diameter that was granular in appearance. In both instances, the lesions were located in the depression between two rugae. Because of this, it is speculated that these two areas were not entirely removed at the time of surgery. One subject (a woman), marked with the asterisk in Table I, showed a localized erythematous response at 12 months postoperatively which was not present following healing. This inflammatory response, however, disappeared clinically after relining and adjusting the occlusion of the dentures. This same subject was the only one of the entire study who displayed dyskeratosis preoperatively and 12 months postoperatively. Examination of a specimen taken for biopsy 24 months postoperatively did not show dyskeratosis. Also, at 24 months, the clinical and histologic appearance of the palate was well within normal limits. Two subjects were also lost from this group (Table I).
DISCUSSION
The treatment of inflammatory papillary hyperplasia by making new dentures alone did not cause a substantial change in the lesions. It was noted, however, that half the subjects experienced a reduction in the inflammatory response. This was found to be inadequate therapy.
1022
BOLENDER,
SWENSON,
AND
YAMANE
J. Pros. November-December,
Den. 1965
Surgical excision of the lesions by a high-frequency cutting current followed by making new dentures resulted in the lesions complete removal. This method proved to be adequate treatment and resulted in a normal mucosa. It is important to reline the old denture immediately following surgery and to maintain good contact of the denture with the palatal mucosa. One subject of the twenty showed dyskeratosis preoperatively. Conclusions cannot be drawn from the results of this study regarding dyskeratosis because of its incidence in only one subject. Supraperiosteal removal of inflammatory papillary hyperplasia is indicated and adequate treatment. Subperiosteal removal is not indicated except when one is dealing with a malignancy. This project is being continued in order to evaluate the therapy over a longer period of time. At the end of the third year, five subjects remained in Group I and four in Group II. The results so far indicate that the lesion still remained in the subjects in ,Group I, while it was not seen in the subjects in Group II, i.e., it seemed to indicate that similar results will be obtained to those reported at the end of twelve months.
SUMMARY
The results was not effective gical removal of eradication of the
REFERENCES
of this study indicated that the making of new dentures alone in eliminating inflammatory papillary hyperplasia. However, surthe lesion and the making of new dentures was effective in the lesion.
1. Fisher, A. K., and Rashid, P. J.: Inflammatory Papillary Hyperplasia of the Palatal Mucosa, Oral Surg., Oral Med. & Oral Path. 5:192, 1952. 2. Lyon, D. G., and Chick, A. 0. : Denture Sore Mouth and Angular Cheilitis : A Preliminary Investigation Into Their Possible Association With Candida Infection., D. Practitioner & D. Record 7:212-217, 1957. 3. Thoma, K. H., and Robinson, H. B.: Oral and Dental Diagnosis, ed. 4, Philadelphia, 1955, W. B. Saunders Company, pp. 323-324. 4. Robins;;5,H. B. G.: Diagnosis of Lesions Associated With Dentures, J. PROS. DEN. 7:338, 5. Nyquist, 6.: A Study of Denture Sore Mouth: An Investigation of Traumatic Allergic and Toxic Lesions of the Oral Mucosa Arising From the Use of Full Dentures, Acta Odont. Scandinavica 10, Suppl. 9:11-154, 1952. 6. Hickey, J. C., Boucher, C. O., and Woelful, J. B.: Responsibility of the Dentist in Complete Dentures. J. PROS. DEN. 12:638, 1962. 7. Friedman, Samuel: Effective Use of Diagnostic Data, J. PROS. DEN. 9:729, 1959. 8. Waite, D. E.: Inflammatory Papillary Hyperplasia, J. Oral Surg., Anesth. & Hosp. D. Serv. 19:210, 1961. 9. Ostlund, S. G.: Effect of Complete Dentures on the Gum Tissues. A Histological and Histopathological Investigation, Acta Odont. Scandinavica 16:l. 1958.
UNIVERSITY OF WASHINGTON, SEATTLE, WASH. 98155 SCHOOL OF DENTISTRY,
Você também pode gostar
- Alternative Surgical Approaches For Excision of Dermoid Cyst of The Floor of MouthDocumento3 páginasAlternative Surgical Approaches For Excision of Dermoid Cyst of The Floor of MouthKharismaNisaAinda não há avaliações
- Cyst Decompression ReportDocumento5 páginasCyst Decompression ReportFrederick Alexander TrisnaAinda não há avaliações
- Mixoma 9Documento4 páginasMixoma 9Nicolás MedinaAinda não há avaliações
- Unusual Large and Abiding Fibroepithelial Polyp in Oral Cavity: A Case ReportDocumento4 páginasUnusual Large and Abiding Fibroepithelial Polyp in Oral Cavity: A Case ReportmuharrimahAinda não há avaliações
- ParesthesiaoftheupperlipDocumento4 páginasParesthesiaoftheupperlipikeuchi_ogawaAinda não há avaliações
- 100 103 PDFDocumento4 páginas100 103 PDFdrgeorgejose7818Ainda não há avaliações
- 100 103 PDFDocumento4 páginas100 103 PDFdrgeorgejose7818Ainda não há avaliações
- Treatment of A Large Maxillary Cyst With MarsupializationDocumento8 páginasTreatment of A Large Maxillary Cyst With MarsupializationDinesh SolankiAinda não há avaliações
- Surgical Ciliated Cyst of The Maxilla. Clinical Case: Jorge Cano, Julián Campo, Miguel Angel Alobera, Rafael BacaDocumento4 páginasSurgical Ciliated Cyst of The Maxilla. Clinical Case: Jorge Cano, Julián Campo, Miguel Angel Alobera, Rafael BacaAhmad MustafaAinda não há avaliações
- Pindborg Tumor Presenting in Early Adolescent - A Rare Case ReportDocumento7 páginasPindborg Tumor Presenting in Early Adolescent - A Rare Case ReportIJAR JOURNALAinda não há avaliações
- 100 103 PDFDocumento4 páginas100 103 PDFDanis Diba Sabatillah YaminAinda não há avaliações
- Salusvita v23 n2 2004 Art 13Documento12 páginasSalusvita v23 n2 2004 Art 13dorasani99Ainda não há avaliações
- Gingival Epulis: Report of Two Cases.: Dr. Praful Choudhari, Dr. Praneeta KambleDocumento5 páginasGingival Epulis: Report of Two Cases.: Dr. Praful Choudhari, Dr. Praneeta KambleAnandAinda não há avaliações
- Sialolithiasis - A Report of Two Cases and ReviewDocumento4 páginasSialolithiasis - A Report of Two Cases and Reviewmaharani spAinda não há avaliações
- Artículo PrimaDocumento3 páginasArtículo PrimaemoreraAinda não há avaliações
- Large Lesion Management - Roots0112Documento4 páginasLarge Lesion Management - Roots0112nuriacampoAinda não há avaliações
- Mucocele 9Documento5 páginasMucocele 9Devi AlfianiAinda não há avaliações
- Peripheral Cemento-Ossifying Fibroma - A Case Report With A Glimpse On The Differential DiagnosisDocumento5 páginasPeripheral Cemento-Ossifying Fibroma - A Case Report With A Glimpse On The Differential DiagnosisnjmdrAinda não há avaliações
- FetchDocumento7 páginasFetchJuan Sebastián Pérez GAinda não há avaliações
- Dentj 41 3 07Documento4 páginasDentj 41 3 07Bagoes Ario BimoAinda não há avaliações
- Fibrous Hyperplasia - A Case ReportDocumento4 páginasFibrous Hyperplasia - A Case ReportInternational Journal of Innovative Science and Research TechnologyAinda não há avaliações
- Severe Extrusion From An Apical Abscess - A Case ReportDocumento4 páginasSevere Extrusion From An Apical Abscess - A Case ReportSaca AnastasiaAinda não há avaliações
- Endodontics: Oral Surgery Oral Medicine Oral PathologyDocumento7 páginasEndodontics: Oral Surgery Oral Medicine Oral PathologyUntuk TugasAinda não há avaliações
- Bioabsorbable Root Analogue For Closure of Oroantral Comm After Tooth ExtractionDocumento0 páginaBioabsorbable Root Analogue For Closure of Oroantral Comm After Tooth ExtractionTrinhTaAinda não há avaliações
- Periapical GranulomaDocumento6 páginasPeriapical GranulomaEzza RiezaAinda não há avaliações
- Ameloblastoma Arising From Gorlins Cyst: A Rare Case ReportDocumento4 páginasAmeloblastoma Arising From Gorlins Cyst: A Rare Case ReportInternational Journal of Innovative Science and Research TechnologyAinda não há avaliações
- Giant Cell Epulis: Report of 2 Cases.: Oral PathologyDocumento11 páginasGiant Cell Epulis: Report of 2 Cases.: Oral PathologyVheen Dee DeeAinda não há avaliações
- Mucocele 5Documento4 páginasMucocele 5Devi Alfiani100% (1)
- Varied Presentations of Inverted Papilloma: Case ReportDocumento4 páginasVaried Presentations of Inverted Papilloma: Case ReportMohankummar MuniandyAinda não há avaliações
- Intraoral Approach To Large Dermoid Cysts of The Floor of The Mouth: A Technical NoteDocumento3 páginasIntraoral Approach To Large Dermoid Cysts of The Floor of The Mouth: A Technical NoteKharismaNisaAinda não há avaliações
- Periodontal Plastic Surgery in The Management of Multiple Gingival Recessions Two Therapeutic ApproachesDocumento5 páginasPeriodontal Plastic Surgery in The Management of Multiple Gingival Recessions Two Therapeutic ApproachesInternational Journal of Innovative Science and Research TechnologyAinda não há avaliações
- Sindrome Van Der WoudeDocumento2 páginasSindrome Van Der WoudeEerrmmaa Ssaarrell Rroommaann PpaarraaAinda não há avaliações
- Zhao 2020Documento2 páginasZhao 2020miraraspopovic020Ainda não há avaliações
- Ijhs 12577+883 892Documento10 páginasIjhs 12577+883 892hai1Ainda não há avaliações
- Chronic Refractory Osteomyelitis of The Mandible and Maxilla Related To Dental Implant PlacementDocumento4 páginasChronic Refractory Osteomyelitis of The Mandible and Maxilla Related To Dental Implant PlacementDiana BărbulescuAinda não há avaliações
- Recurrent Peripheral Odontogenic Keratocyst: A Case ReportDocumento3 páginasRecurrent Peripheral Odontogenic Keratocyst: A Case ReportthedocperuAinda não há avaliações
- Dens Evaginatus and Type V Canal Configuration: A Case ReportDocumento4 páginasDens Evaginatus and Type V Canal Configuration: A Case ReportAmee PatelAinda não há avaliações
- Oroantral FistulaDocumento4 páginasOroantral FistulaMahesh AgrawalAinda não há avaliações
- Management of Infected Radicular Cyst by Surgical Approach: Case ReportDocumento2 páginasManagement of Infected Radicular Cyst by Surgical Approach: Case ReportEzza RiezaAinda não há avaliações
- Management of Extra Oral Sinus Tract Associated With Large Periapical Lesion - A Case ReportDocumento1 páginaManagement of Extra Oral Sinus Tract Associated With Large Periapical Lesion - A Case ReportNgân PhạmAinda não há avaliações
- Periodontal Plastic SurgeryDocumento5 páginasPeriodontal Plastic Surgeryudhai170819Ainda não há avaliações
- Nasopalatine Duct Cyst - A Delayed Complication To Successful Dental Implant Placement - Diagnosis and Surgical Management - As Published in The JOIDocumento6 páginasNasopalatine Duct Cyst - A Delayed Complication To Successful Dental Implant Placement - Diagnosis and Surgical Management - As Published in The JOIHashem Motahir Ali Al-ShamiriAinda não há avaliações
- Recurrent Multiple Superficial Mucocele On The Palate: Histopathology and Laser VaporizationDocumento5 páginasRecurrent Multiple Superficial Mucocele On The Palate: Histopathology and Laser VaporizationFelipeNobreAinda não há avaliações
- Orbital Abscess During Endodontic Treatment: A Case ReportDocumento3 páginasOrbital Abscess During Endodontic Treatment: A Case ReportJing XueAinda não há avaliações
- 5-Surgical Treatment of RanulaDocumento5 páginas5-Surgical Treatment of RanulaDevi AlfianiAinda não há avaliações
- Dentigerous Cyst Over Maxillary Sinus: A Case Report and Literature ReviewDocumento9 páginasDentigerous Cyst Over Maxillary Sinus: A Case Report and Literature Reviewtitin setya ningsihAinda não há avaliações
- Periapical GranulomaDocumento3 páginasPeriapical GranulomaLina BurduhAinda não há avaliações
- Management of Irritational Fibroma by Three Different Treatment Modalities - A Case SeriesDocumento4 páginasManagement of Irritational Fibroma by Three Different Treatment Modalities - A Case SeriesInternational Journal of Innovative Science and Research TechnologyAinda não há avaliações
- Traumatic UlcersDocumento7 páginasTraumatic UlcersrdindamyrnaAinda não há avaliações
- ABuccal Haematoma Following Administrationofan IANBDocumento6 páginasABuccal Haematoma Following Administrationofan IANBnurfarahainsaidAinda não há avaliações
- Coronally Advanced Flap With and Without VerticalDocumento13 páginasCoronally Advanced Flap With and Without VerticalLEONARDO ALBERTO CRESPIN ZEPEDAAinda não há avaliações
- Novaes 1969Documento13 páginasNovaes 1969Ana OrtizAinda não há avaliações
- PeriapikalDocumento7 páginasPeriapikalHanindyaNoorAgusthaAinda não há avaliações
- BCR 2019 233946Documento2 páginasBCR 2019 233946Paola AlcocerAinda não há avaliações
- OOOO Ricucci 2000Documento6 páginasOOOO Ricucci 2000karlaAinda não há avaliações
- Favorable Response of An Extensive Periapical Lesion To Root Canal TreatmentDocumento0 páginaFavorable Response of An Extensive Periapical Lesion To Root Canal TreatmentAh-ragab HouseAinda não há avaliações
- Selective Pressure Impressions Methods PDFDocumento3 páginasSelective Pressure Impressions Methods PDFAgus PudiantoAinda não há avaliações
- Dental Anxiety QuestionnairesDocumento4 páginasDental Anxiety QuestionnairesAmar BhochhibhoyaAinda não há avaliações
- Story: Submitted By: Siddartha Phaiju Class 6 Submitted To: D.R. Kattel SirDocumento3 páginasStory: Submitted By: Siddartha Phaiju Class 6 Submitted To: D.R. Kattel SirAmar BhochhibhoyaAinda não há avaliações
- Comparison of Two Impression TechniqueDocumento6 páginasComparison of Two Impression TechniqueAmar BhochhibhoyaAinda não há avaliações
- SPLNPROC Author Instructions - Feb2015 PDFDocumento10 páginasSPLNPROC Author Instructions - Feb2015 PDFAmar BhochhibhoyaAinda não há avaliações
- Ocular ProsthesisDocumento3 páginasOcular ProsthesisAmar BhochhibhoyaAinda não há avaliações
- Dental Materials PracticalDocumento1 páginaDental Materials PracticalAmar BhochhibhoyaAinda não há avaliações
- Nepal Medical CouncilDocumento3 páginasNepal Medical CouncilAmar BhochhibhoyaAinda não há avaliações
- Post Op InstructionsDocumento5 páginasPost Op InstructionsAmar Bhochhibhoya0% (1)
- 16 Annual Dental Conference and Trade Exhibition January 31, 2015, KathmanduDocumento2 páginas16 Annual Dental Conference and Trade Exhibition January 31, 2015, KathmanduAmar BhochhibhoyaAinda não há avaliações
- Abrasive & Polishing AgentsDocumento11 páginasAbrasive & Polishing AgentsVishal MalusareAinda não há avaliações
- Complete Denture Selected TopicsDocumento16 páginasComplete Denture Selected TopicsAmar BhochhibhoyaAinda não há avaliações
- Balkwill's Angle For Complete DenturesDocumento4 páginasBalkwill's Angle For Complete DenturesAnisha Mandavia Doshi0% (1)
- Esthetics IllusionDocumento8 páginasEsthetics IllusionAmar BhochhibhoyaAinda não há avaliações
- Sprue DesignDocumento5 páginasSprue DesignAmar BhochhibhoyaAinda não há avaliações
- Mcqs DentistryDocumento2 páginasMcqs DentistryAmar Bhochhibhoya100% (1)
- NotesDocumento639 páginasNotesAmar Bhochhibhoya100% (1)
- Combination SyndroneDocumento5 páginasCombination SyndroneAmar BhochhibhoyaAinda não há avaliações
- Linear OcclusionDocumento8 páginasLinear OcclusionAmar BhochhibhoyaAinda não há avaliações
- Shortened ArchDocumento5 páginasShortened ArchAmaey ParekhAinda não há avaliações
- Implant ProsthodonticsDocumento5 páginasImplant ProsthodonticsAmar BhochhibhoyaAinda não há avaliações
- Implant Supported ProsthesisDocumento3 páginasImplant Supported ProsthesisAmar BhochhibhoyaAinda não há avaliações
- Complete DentureDocumento17 páginasComplete DentureJoanna Mae ShawyerAinda não há avaliações
- SMEA KPIs PresentationDocumento76 páginasSMEA KPIs PresentationRemelyn CortesAinda não há avaliações
- Ccid 11 175Documento11 páginasCcid 11 175Remo Alnovryanda PutraAinda não há avaliações
- Best of Fives For Dentistry 3 ST Ed (2014)Documento179 páginasBest of Fives For Dentistry 3 ST Ed (2014)chimedbator100% (3)
- Nutrition Support in Critically Ill Patients - An OverviewDocumento9 páginasNutrition Support in Critically Ill Patients - An OverviewstarykAinda não há avaliações
- Critical Illness: Nutrition Care ManualDocumento20 páginasCritical Illness: Nutrition Care ManualDiogo JuniorAinda não há avaliações
- DERMATOMYCOSISDocumento114 páginasDERMATOMYCOSISQonita Qurrota AyunAinda não há avaliações
- Diet Nutrition Management For Treatment of Angular: Cheilitis Deseases in ChildrenDocumento4 páginasDiet Nutrition Management For Treatment of Angular: Cheilitis Deseases in ChildrenIftri mellaniAinda não há avaliações
- Denture Insertion and Post Insertion ProblemsDocumento165 páginasDenture Insertion and Post Insertion ProblemsMadhul Singhal100% (2)
- Kundu - Pearls in Medicine For Students@helpmedico PDFDocumento303 páginasKundu - Pearls in Medicine For Students@helpmedico PDFSwarnadeep Mani100% (1)
- By Dr. Smitha B K Post Graduate Student Department of Preventive and Community DentistryDocumento58 páginasBy Dr. Smitha B K Post Graduate Student Department of Preventive and Community DentistryAnnupriya KhannaAinda não há avaliações
- Common Fungal Infections in The Oral Cavity: Acute CandidiasisDocumento6 páginasCommon Fungal Infections in The Oral Cavity: Acute CandidiasisChristineMartinAinda não há avaliações
- Oral Candidiasis An Opportunistic Infection A ReviewDocumento5 páginasOral Candidiasis An Opportunistic Infection A ReviewDino JalerAinda não há avaliações
- Physical Examination Related NutritionDocumento40 páginasPhysical Examination Related NutritionYohan SamudraAinda não há avaliações
- Fungal InfectionsDocumento42 páginasFungal InfectionsleenaloveuAinda não há avaliações
- Picture of Stomatitis, Glossitis, Cheilosis, Petechiae (Javier, BSN - 2B)Documento2 páginasPicture of Stomatitis, Glossitis, Cheilosis, Petechiae (Javier, BSN - 2B)Jan Vier B. JavierAinda não há avaliações
- Health Assessment Chapter 13Documento6 páginasHealth Assessment Chapter 13Shade ElugbajuAinda não há avaliações
- The Complete Denture - Michael I. MacEntee 2nd Ed PDFDocumento121 páginasThe Complete Denture - Michael I. MacEntee 2nd Ed PDFIon Bondari100% (3)
- Oral Manifestations of Denture AbuseDocumento53 páginasOral Manifestations of Denture AbuseBharanija100% (2)
- Nutrition and Oral Health - (Review) : L. Leelavathi, Santa Thoudam and M. AnithaDocumento5 páginasNutrition and Oral Health - (Review) : L. Leelavathi, Santa Thoudam and M. AnithaKhalisahatma BklAinda não há avaliações
- MycologyDocumento117 páginasMycologybanteng wibisonoAinda não há avaliações
- Podj 4 PDFDocumento3 páginasPodj 4 PDFNur Sita DewiAinda não há avaliações
- Angular CheilitisDocumento5 páginasAngular CheilitisReginald RiveraAinda não há avaliações
- Jurnal Dermatitis Perioral 8Documento2 páginasJurnal Dermatitis Perioral 8parlingultomAinda não há avaliações
- Cheilitis 2Documento10 páginasCheilitis 2pelangiAinda não há avaliações
- Angular Cheilitis - An Updated Overview of The Etiology, Diagnosis, and ManagementDocumento7 páginasAngular Cheilitis - An Updated Overview of The Etiology, Diagnosis, and ManagementMuhammad AbdillahAinda não há avaliações
- K7 Jamur Superficial 2020Documento51 páginasK7 Jamur Superficial 2020Jimmy Fran IIAinda não há avaliações
- QBANK PasTest Best of Fives For DentistryDocumento165 páginasQBANK PasTest Best of Fives For DentistrylindajenhaniAinda não há avaliações
- Oral Manifestations of Systemic DiseasesDocumento14 páginasOral Manifestations of Systemic Diseasesshygal1981Ainda não há avaliações
- DietnutritionDocumento84 páginasDietnutritionTuan NguyenAinda não há avaliações