Escolar Documentos
Profissional Documentos
Cultura Documentos
Cytomegalovirus in Periodontal Disese
Enviado por
Ashok KpDescrição original:
Direitos autorais
Formatos disponíveis
Compartilhar este documento
Compartilhar ou incorporar documento
Você considera este documento útil?
Este conteúdo é inapropriado?
Denunciar este documentoDireitos autorais:
Formatos disponíveis
Cytomegalovirus in Periodontal Disese
Enviado por
Ashok KpDireitos autorais:
Formatos disponíveis
Acta Clin Croat 2011; 50:61-66
Review
THE ROLE OF CYTOMEGALOVIRUS INFECTION IN THE PATHOGENESIS OF PERIODONTAL DISEASES
Nataa Beader1 and Marija Ivi-Kardum 2
Department of Microbiology, School of Medicine, University of Zagreb, Department of Clinical and Molecular Microbiology, Zagreb University Hospital Center, 2Department of Periodontology, School of Dentistry, University of Zagreb, Zagreb, Croatia
1
SUMMARY The main characteristic of periodontal disease is chronic inflammation that leads to progressive destruction of the connective tissues and bone with subsequent tooth mobility and finally tooth loss. Traditionally, the pathogenesis of periodontitis was based on the infection caused by bacteria that colonize tooth surface and gingival sulcus. Accumulated evidence show that host response factors such as inflammatory reaction and activation of the innate immune system are critical to the pathogenesis of periodontal disease. Periodontal disease has been widely recognized as a chronic disease but the nature of chronicity remains unclear. The question is whether periodontal disease is a continuous process or consists of episodes of exacerbations and remissions. Maybe cytomegalovirus infection of the periodontium, depending on the latent or active phase of infection, can partly explain the episodic progressive nature of periodontal disease. Cytomegalovirus infection impairs periodontal defense and permits overgrowth of periodontopathogenic bacteria. Owing to advances in new technologies, experimental evidence show the influence and interrelatedness of genomic, epigenetic, proteomic and metabolic factors in the pathogenesis of periodontal disease. Data on the pathogenesis of periodontal disease are reviewed. Key words: Periodontal diseases etiology; Cytomegalovirus
Introduction
According to new data, clinical characteristics of periodontal disease are influenced by genetic and epigenetic factors such as bacterial accumulation, smoking, or diabetes. Even though the genetic basis of periodontal disease is considered essential for setting the inflammatory process, the epigenetic factors may strongly influence changes in tissue behavior1. On the other hand, infection and inflammation of periodontal disease could reach distant sites via bloodstream and contribute the systemic diseases such as atherosclerosis, diabetes and adverse outcomes in pregnancy2,3.
Correspondence to: Nataa Beader, MD, PhD, Department of Clinical and Molecular Microbiology, Zagreb University Hospital Center, Kipatieva 12, HR-10000 Zagreb, Croatia E-mail: natasaeli@gmail.com Received November 20, 2010, accepted December 26, 2010
Acta Clin Croat, Vol. 48, No. 4, 2009
Over decades, periodontal disease has been recognized as an inflammatory disease initiated by oral microbial biofilm that elicits host response with resultant osseous and soft tissue destruction. Among 500 types of oral bacteria that have been studied to date, only a few of them are considered to be involved in the etiology of periodontal disease. Leaders in the field who gathered at the 1996 World Workshop in Periodontics agreed that these include Aggregatiobacter actinomycetemcomitans (previously Actinobacillus actinomycetemcomitans), Porphyromonas gingivalis, Tannerella (T.) forsythia (previously T. forsythensis) and Treponema denticola 4. Now, it is understood that host response is playing an essential role in the breakdown of connective tissue and bone. The immune and inflammatory responses are critical to the pathogenesis of periodontal disease. Bacteria that colonize tooth surface and gin61
Nataa Beader and Marija Ivi-Kardum
The pathogenesis of periodontitis
gival sulcus initiate local inflammatory reaction that activates the innate immune system. The initial localized response is amplified by the release of many various cytokines and mediators that propagate inflammation through gingival tissues. If the inflammation could not be encapsulated within gingival tissue, the immune response will be expanded to alveolar bone. Then the inflammatory process drives the destruction of connective tissue and adjacent alveolar bone. There are two critical factors that determine if the bone loss will occur in response to an inflammatory reaction. First, the concentration of inflammatory mediators present in gingival tissue must be sufficient to activate the pathways leading to bone resorption, and second, those mediators must penetrate gingival tissue to reach within a critical distance to alveolar bone5. Page and Schroeder have found out that the closer the cells of the inflammatory infiltrate are to the bone, the greater is the number of osteoclasts formed, hence the greater is the amount of bone degraded6.
The Mechanisms of the Immune System and Inflammatory Response
The innate immune system provides immediate protection against infection and inflammation acting in several ways:
- recruitment of immune cells (phagocytic cells such as polymorphonuclear neutrophils, monocytes and activated macrophages);
- activation of complement system (induces the release of chemical mediators such as cytokines, e.g., tumor necrosis factor (TNF) or interleukins (IL); - activation of adaptive immune system that represents more specific response to injury or inflammation (proliferation of antigen specific T and B cells with consequent antibody production, assisting macrophages and generating killing cells).
The recruitment of immune cells and releasing of proinflammatory cytokines lead to destructive processes. Several osteoclast related mediators such as metalloproteinases (MMPs) and cathepsins are responsible for the destruction of alveolar bone and the supporting connective tissues7. The main event in the inflammatory process is the infiltration of leukocytes in order to limit the level of bacterial invasion. Leukocytes are recruited by many
62
factors such as bacterial products, cytokines, chemokines, and cross-talk between innate and adaptive immune responses, lipid mediators and complement. These phagocytic cells trigger the release of chemical mediators such as TNF and ILs, which in turn activate complement system and acute phase response in order to assist antibodies in clearing pathogens or mark them for other cells destruction. Finally, activated adaptive immune response will run the proliferation of antigen specific T and B cells. T cells recognize foreign antigen and target it, and B cells produce specific antibodies. T and B cells together assist macrophages and help generate killing cells that mount a response. The role of the immune system is essential. However, if the immune response in the inflammatory disease becomes chronic, the tissues do not return to homeostasis. The production of cytokines, which stimulate the inflammatory process that activates effector mechanisms, is considered the key feature between bacterial stimulation and tissue destruction. The cytokines have been recognized as cell products of different kinds of cells such as leukocytes, keratinocytes, resident mesenchymal cells (fibroblasts and osteoblasts) or their precursor cells, dendritic cells and endothelial cells. Cytokines are organized as innate and acquired immune cytokines or chemokines. Chemokines are chemotactic cytokines important in leukocyte recruitment and regulation of tissue infiltration with Th1 cells in periodontal disease (e.g., CXCl 10 chemokine)8. They are produced by many cell types in the periodontium, such as fibroblasts, endothelial cells, macrophages, osteoclasts, epithelial cells, polymorphonuclear leukocytes, monocytes, lymphocytes and mast cells. Based on the ligand structure, chemokines are divided into two major families: CC and CXC chemokines. Some of them can stimulate one or more steps of bone resorption by recruiting, differentiating or fusing of precursor cells to form osteoclasts or to enhance osteoclast survival9. Chemokines as neutrophil chemoattractants contribute to the process of destruction of mineral tissue during bone resorption because macrophages release MMPs. MMPs are structurally related endopeptidases usually divided into several subclasses according to their substrate specificities and physical structure: interstitial collagenases, gelatinases, membrane-type MMPs, and other kinds of
Acta Clin Croat, Vol. 50, No. 1, 2011
Nataa Beader and Marija Ivi-Kardum
The pathogenesis of periodontitis
MMPs including stromelysins and metalloelastases. Their activity is directed against most extracellular matrix, pericellular and non-matrix macromolecules. They are involved in degradation process of different extracellular molecules such as collagen, elastin, proteoglycans and laminins. The study by Kubota et al. showed that gene expression of MMP-1, -3, -9 and -13 is simultaneously augmented in periodontitis affected gingival tissue10. MMPs are considered to be of great clinical importance in the pathogenesis of periodontal disease due to their ability to activate latent forms of effector proteins, e.g., antimicrobial peptides, chemokines and cytokines. Also, they can alter protein function like shedding of cell-surface proteins7. Accumulated evidence show that the effects of cytokines that promote osteoclast formation and bone resorption seem to be counteracted by other cytokines that are anti-inflammatory. IL-1, -6, -11 and -17, tumor necrosis factor-alpha (TNF-), leukemia inhibitory factor, kinins, thrombin and different chemokines are well known as proinflammatory mediators. Opposite, IL-4, -10, -12, -13 and -18 as well as interferon-beta (IFN-) and gamma (INF-) have anti-inflammatory and inhibitory action to bone resorption5. T and B lymphocytes are predominant mononuclear cells in periodontitis of gingival tissues. They can produce IL-1, -6 and -17, TNF- and receptor activator of nuclear factor-kappa B ligand (RANKL). IL-1 and -6 are included in bone resorption via the induction of RANKL. RANKL binds to receptor activator of nuclear factor-kappa B (RANK), one of the most potent inducers of osteoclast formation and activity. This interaction can be stopped with osteoprotegerin (OPG), which binds to RANKL and inhibits the stimulation of RANK, if produced by lymphocytes11. In the initial phase of their study (less than 30 days from the onset of experimental disease), Garlet et al. showed the leukocyte count to have increased just prior to the rapid increase of alveolar bone loss. At the same time, the levels of proinflammatory cytokines, MMPs and RANKL were also elevated. Later when the bone loss rate was slower, the concentration of proinflammatory cytokines, MMPs and RANKL decreased and there was a dramatic increase in the concentrations of antiinflammatory cytokines as well as tissue inhibitors of matrix metalloproteinases (TIMPs) and OPG12. AcActa Clin Croat, Vol. 50, No. 1, 2011
cording to these experimental data, it seems that the type of cytokines produced in periodontal tissues may determine the progression and severity of periodontal disease by controlling the breakdown of soft and bone tissues through the balance between MMPs/TIMP and RANKL/OPG expression in gingival tissues. So far, IL-1, prostanglandin E2, MMPs, neutrophil elastase and -glucuronidase have been identified as potential biomarkers for the diagnosis of periodontal disease, as they are considered as measures of inflammation and mediators of the connective tissue breakdown13,14. However, it seems that there is no ideal marker that can predict the progression from gingivitis to periodontitis, or when periodontitis will turn to its active phase with consequent attachment loss15.
CMV Infection and Immune Response in Periodontal Disease
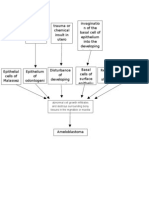
Herpes viruses are found to be more frequently present in periodontal lesions and acute necrotizing ulcerative gingivitis lesions than in gingivitis or periodontally healthy sites. Most of the time, two herpesviruses are implicated in these lesions: Epstein-Barr virus (EBV) that infects periodontal B-lymphocytes and cytomegalovirus (CMV) that infects periodontal monocytes/macrophages and T-lymphocytes. Also, CMV infects salivary glands, epithelial and endothelial cells, and fibroblasts. The seroprevalence of CMV infection in the world varies widely up to 95% of population depending on the geographic area (developed/developing countries)16. Very often, the infection starts early in the childhood, actually, early in gestation because placenta is pivotal in CMV transmission to the fetus17. Jaskoll et al. report that CMV infection involving dental papilla mesenchymal cells induced tooth defects such as amelogenesis imperfecta18. This pathogenesis appears to be mediated by the NF B pathway. Reactivation of CMV in periodontal lesions is considered to be associated with periodontal disease progression, especially in localized juvenile periodontitis19. The number of subgingival periodontopathogenic bacteria in these lesions is elevated probably because active viral infection impairs immune defenses of periodontal tissue. This might explain several hallmarks of periodontal disease such as:
63
Nataa Beader and Marija Ivi-Kardum
The pathogenesis of periodontitis
- episodic progressive nature of periodontal disease (due to transient local immunosuppression depending on active or latent viral infection);
- localized pattern of tissue destruction (due to viral tissue tropism);
odontitis demonstrated higher expression of MMPs than biopsies from CMV negative individuals24. CMV can produce tissue injury as the result of immunopathologic responses to virally infected cells such as:
In general, herpes viruses may give rise to periodontal pathology in two ways, first, by direct viral infection and replication, and second, as virally mediated damage to host defense and by evading the immune host surveillance. They may diminish tissue repair by direct cytopathic effect on inflammatory cells such as polymorphonuclear leukocytes, lymphocytes, macrophages, and other cells such as fibroblasts, endothelial cells, bone cells and others. In turn, this may lead to bacterial superinfection. Gingival herpes virus infection may promote subgingival attachment and colonization of periodontopathogenic bacteria. Even more, viral proteins expressed on eukaryotic cell membranes can act as bacterial receptors and generate new bacterial binding sites. It seems to be most important that viral infections can alter inflammatory mediator and cytokine responses. Concerning the pathology of periodontal disease, it appears that the crucial role belongs to CMV. Accumulated evidence show that CMV has not only developed many strategies to evade the host immune response but also to exploit the host immune response to achieve reactivation from latency and disseminated infection 20. CMV uses NFB to mediate an inflammatory immune response and to induce IE gene expression in order to drive viral replication 21. CMV encodes the chemokines that draw susceptible monocytes and neutrophils to the site of infection. Consequently, the virus can induce production of IL-1 and TNF- by macrophages and monocytes, which in turn may up-regulate MMPs and down regulate TIMPs. MMPs are the key proteolytic enzymes responsible for cleaving interstitial collagens, which make the highest protein part of the extracellular matrix in the periodontium 22,23. In periodontal disease, they eventually degrade periodontal ligamentous attachments and bone matrix proteins, finally leading to bone destruction10. Analyses of gingival biopsies of CMV infected individuals with peri64
- some individuals carry periodontopathogenic bacteria and still maintain periodontal health (due to absence of viral infection).
- induction of cell-mediated immunosuppression by reduction of cell surface expression of major histocompatibility complex (MHC) class I molecules and interfering with T-lymphocyte recognition; - causing metabolic abnormalities in monocytes and lymphocytes;
In their study, Contreras and Slots showed the importance of CMV in the etiology and/or pathogenesis of human periodontal disease. They demonstrated the presence of nucleic acid sequences of CMV in juvenile and adult periodontal lesions; the association between viral infection and acute necrotizing gingivitis; mRNA late gene expression in adult and localized juvenile periodontitis lesions and association with progressive disease; increased frequency of periodontopathogneic bacteria in CMV positive periodontal lesions; detected viral nucleic acid sequences in inflammatory periodontal cells; demonstrated the effect of viral infection on periodontal defense cells; and viral ability to up-regulate the expression of tissue damaging cytokines in periodontal inflammatory cytokines25. According to these data, the main question might be: does active periodontal CMV infection initiate destructive periodontal disease or the disease reactivates latent CMV infection? It seems that the immune system is essential. Acute CMV infection is characterized by significant levels of viral replication and dissemination to multiple organs. Thus, the pathogenesis of acute infection shows a linkage between the levels of viral replication, organ dysfunction and disease in patients. In contrast, the pathogenesis of chronic infection is associated with a bi-directional relationship between viral gene expression and the host inflammatory response: viral persistence (reactivation) is facilitated by the host inflammatory response and the host
Acta Clin Croat, Vol. 50, No. 1, 2011
- suppressing antigen specific cytotoxic T-lymphocyte functions that results in a decrease in circulating CD4+ cells and an increase in CD8+ suppressor cells, which in turn might lead to global impairment of cell-mediated immunity.
Nataa Beader and Marija Ivi-Kardum
The pathogenesis of periodontitis
inflammatory response is stimulated by the presence of the virus. In this case, the disease may be attributed to both viral and host functions. Moreover, it seems that viral gene products that play the main role in chronic inflammation in the body are not needed for replication in vitro. If immune response becomes chronic due to many different factors in inflammatory disease, the injured tissues do not return to homeostasis. Consequently, CMV is being reactivated periodically resulting in transient immunosuppression that gives rise to overgrowth of periodontal pathogenic bacteria.
8. Hosokawa Y, Hosokawa I, Ozaki K, Nakae H, Matsuo T. Cytokines differentially regulate CXCl 10 production by interferon- -stimulated or tumor necrosis factor-stimulated human gingival fibroblasts. J Periodontal Res 2008;44:225-31.
Conclusion
Although it has been considered that the pathogenesis of periodontitis is based on the infection caused by bacteria that colonize tooth surface and gingival sulcus, different studies have shown that the host response factors such as inflammatory reaction and activation of the innate immune system are critical to the pathogenesis of periodontal disease. CMV infection due to a variety of viral properties can impair periodontal defenses, thus permitting the overgrowth of periodontopathogenic bacteria. It seems that CMV infection in periodontal tissue depending on the latent or active phase of the infection can partly explain the episodic progressive nature of periodontal disease.
11. Hofbauer LC, Schoppet M. Clinical implications of the osteoprotegerin/RANKL/RANK system for bone and vascular disorders. JAMA 2004;292:490-5.
10. Kubota T, Itagaki M, Hoshino C, Nagata M, Morozumi T, Kobayashi T, Takagi R, Yoshie H. Altered gene expression levels of matrix metalloproteinases and their inhibitors in periodontitis-affected gingival tissue. J Periodontol 2008;79:166-73.
9. Graves D. Cytokines that promote periodontal tissue destruction. J Periodontol 2008;79:1585-91.
13. Lamster IB, Ahlo JK. Analysis of gingival crevicular fluid as applied to the diagnosis of oral and systemic diseases. Ann N Y Acad Sci 2007;1098:216-29.
12. Garlet GP, Cardoso CR, Silava TA, Ferreira BR, Avila-Campos MJ, Cunha FQ , Silva JS. Cytokine pattern determines the progression of experimental periodontal disease induced by Actinobacillus actinomycetemcomitans through the modulation of MMPs, RANKL, and their physiological inhibitors. Oral Microbiol Immunol 2006;21:12-20.
14. Kinney JS, Ramscier CA, Giannobile WV. Oral fluid-based biomarkers of alveolar bone loss in periodontitis. Ann N Y Acad Sci 2007;1098:230-51.
References
1. Offenbacher S, Barros SP, Beck JD. Rethinking periodontal inflammation. J Periodontol 2008;79:1577-84.
15. Thaweboon B, Laohapand P, Amornchat C, Matsuyama J, Sato T, Nunez PP, Uematsu H, Hoshino E. Host -globin gene fragments in crevicular fluid as a biomarker in periodontal health and disease. J Periodontal Res 2010;45:38-44. 16. Beader N, krablin-Kui S, Mihaljevi S, Veir Z. Uloga IgG avidnosti u dijagnostici citomegalovirusne infekcije tijekom trudnoe. Gynaecol Perinatol 2009;18:151-5.
3. King GL. The role of inflammatory cytokines in diabetes and its complications. J Periodontol 2008;79:1527-34.
2. Soder PO, Neuerman JH, Jogestrand T, Nowak J, Soder B. Matrix metalloproteinase-9 and tissue inhibitor of matrix metalloproteinase-1 in blood as markers for early atherosclerosis in subjects with chronic periodontitis. J Periodontal Res 2008;44:452-8.
17. Schleiss MR. The role of placenta in the pathogenesis of congenital cytomegalovirus infection: is the benefit of cytomegalovirus immune globulin for the newborn mediated through improved placental health and function? Clin Infect Dis 2006;43:1001-3. 18. Jaskoll T, Abichaker G, Jangaard N, Bringas P Jr, Melnick M. Cytomegalovirus inhibition of embryonic mouse tooth development: a model of the human amelogenesis imperfecta phenocopy. Arch Oral Biol 2008;53:405-15. 19. Ting M, Contreras A, Slots J. Herpesviruses in localized juvenile periodontitis. J Periodontal Res 2000;35:1725. 20. Hangel H, Brune W, Koszinowski UH. Immune evasion by cytomegalovirus survival strategies of a highly adapted opportunist. Trends Microbiol 1998;6:190-7.
5. Cochran DL. Inflammation and bone loss in periodontal disease. J Periodontol 2008;79:1569-76.
4. Williams R. Understanding and managing periodontal diseases. A notable past, a promising future. J Periodontol 2008;79:1552-9.
6. Page RC, Schroeder HE. Current status of the host response in chronic marginal periodontitis. J Periodontol 1981;52:477-91.
7. Giannobile WV. Host-response therapeutics for periodontal disease. J Periodontol 2008;79:1592-600.
Acta Clin Croat, Vol. 50, No. 1, 2011
65
Nataa Beader and Marija Ivi-Kardum
The pathogenesis of periodontitis
21. Hummel M, Abecassis MM. A model for reactivation of CMV from latency. J Clin Virol 2002;25:S123-36.
23. Nasatzky E, Rubinstein Y, Goultschin J, Schwartz Z. The role of matrix metalloproteinases in the progression of periodontitis, and the use of specific in-
22. Cao Z, Li C. Xiang J. Effect of matrix metalloproteinase-1 promoter genotype on interleukin-1-beta-induced matrix metalloproteinase-1 production in human periodontal ligament cells. J Periodontal Res 2010;45:109-15.
24. Botero JE, Contreras A, Parra B. Effects of cytomegalovirus infection on the mRNA expression of collagens and matrix metalloproteinases in gingival fibroblasts. J Periodontal Res 2008;43:649-57. 25. Contreras A, Slots J. Herpesviruses in human periodontal disease. J Periodontal Res 2000;35:3-16.
hibitors to these enzymes in the treatment of the periodontal disease. Refuat Hapeh Vehashinayim 2003;20:38-45.
Saetak ULOGA CITOMEGALOVIRUSNE INFEKCIJE U PATOGENEZI PARODONTNE BOLESTI N. Beader i M. Ivi-Kardum Glavna znaajka parodontne bolesti je kronina upala koja vodi progresivnom razaranju vezivnog tkiva i kosti s posljedinim klimanjem i na kraju ispadanjem zuba. Tradicionalno, patogeneza parodontitisa se temelji na infekciji uzrokovanoj bakterijama koje koloniziraju povrinu zuba i gingivnog sulkusa. Dostupna literatura pokazuje da su initelji obrane domaina kao to je upalna reakcija i aktiviranje priroenog imunog sustava presudno vani u patogenezi parodontne bolesti. Openito se smatra da je parodontna bolest kronina, iako narav kroniciteta nije u potpunosti jasna. Pitanje je je li parodontna bolest trajan proces ili se sastoji od niza epizoda egzacerbacija i remisija. Mogue je da citomegalovirusna infekcija parodontnog tkiva, ovisno o latentnoj ili aktivnoj fazi infekcije, moe djelomice objasniti progresivnu narav parodontne bolesti koja se javlja u epizodama. Citomegalovirusna infekcija smanjuje obranu parodontnog tkiva i tako omoguuje prekomjeran rast parodontopatogenih bakterija. Zahvaljujui napretku u razvoju novih tehnologija eksperimentalni podatci pokazuju utjecaj i meusobnu povezanost genomskih, epigenetskih, proteomskih i metabolinih imbenika u patogenezi parodontne bolesti. U ovom se radu daje pregled spoznaja vezanih za parodontnu bolest. Kljune rijei: Parodontne bolesti etiologija; Citomegalovirus
66
Acta Clin Croat, Vol. 50, No. 1, 2011
Você também pode gostar
- Black TriangleDocumento4 páginasBlack TriangleAshok KpAinda não há avaliações
- Drugs For Pain Management in DentistryDocumento9 páginasDrugs For Pain Management in DentistryAshok KpAinda não há avaliações
- Osteomyelitis Classification Read PDFDocumento33 páginasOsteomyelitis Classification Read PDFNavatha MorthaAinda não há avaliações
- Aspergillosis of CNSDocumento11 páginasAspergillosis of CNSAshok KpAinda não há avaliações
- Dexibuprofen PDFDocumento6 páginasDexibuprofen PDFAshok KpAinda não há avaliações
- Smoking and Periodontal Disease A ReviewDocumento7 páginasSmoking and Periodontal Disease A ReviewAshok KpAinda não há avaliações
- Oral BiofilmsDocumento12 páginasOral BiofilmsAshok KpAinda não há avaliações
- Salivary Gland NeoplasmsDocumento12 páginasSalivary Gland NeoplasmsAshok KpAinda não há avaliações
- Role of Treponema in Periodontal DiseasesDocumento16 páginasRole of Treponema in Periodontal DiseasesAshok KpAinda não há avaliações
- Oral SubmucousDocumento7 páginasOral SubmucousAshok KpAinda não há avaliações
- Gingivitis and Periodontal Disease in ChildrenDocumento73 páginasGingivitis and Periodontal Disease in ChildrenDrShweta SainiAinda não há avaliações
- 23wasan FDocumento4 páginas23wasan FAshok KpAinda não há avaliações
- Factors Influencing The Outcome of Root-Resection Therapy in Molars: A 10-Year Retrospective StudyDocumento9 páginasFactors Influencing The Outcome of Root-Resection Therapy in Molars: A 10-Year Retrospective StudyAshok KpAinda não há avaliações
- Cell Proliferation Rate in MalignancyDocumento5 páginasCell Proliferation Rate in MalignancyAshok KpAinda não há avaliações
- Squamous Cell CarcinomaDocumento12 páginasSquamous Cell CarcinomaAshok KpAinda não há avaliações
- Ameloblastoma PathophysiologyDocumento2 páginasAmeloblastoma PathophysiologyAshok KpAinda não há avaliações
- Infectious Aspects of Periodontal RegenerationDocumento9 páginasInfectious Aspects of Periodontal RegenerationAshok KpAinda não há avaliações
- Medoralv15 I2 p292Documento5 páginasMedoralv15 I2 p292Ashok KpAinda não há avaliações
- Periodontal Salivary HerpesvirusesDocumento5 páginasPeriodontal Salivary HerpesvirusesAshok KpAinda não há avaliações
- Association Between Periodontal DiseaseDocumento7 páginasAssociation Between Periodontal DiseaseAshok KpAinda não há avaliações
- Human Viruses in PeriodontitisDocumento22 páginasHuman Viruses in PeriodontitisAshok KpAinda não há avaliações
- Herpes Viruses in Periodontal Disease - Reality or Myth..Documento6 páginasHerpes Viruses in Periodontal Disease - Reality or Myth..Ashok KpAinda não há avaliações
- Grading Systems of Oral SQ Cell CADocumento10 páginasGrading Systems of Oral SQ Cell CAAshok KpAinda não há avaliações
- Inflammatory Cytokines in DiabetesDocumento8 páginasInflammatory Cytokines in DiabetesAshok KpAinda não há avaliações
- AnaemiaDocumento44 páginasAnaemiaNemin Ajmera100% (1)
- 1 1 8Documento3 páginas1 1 8sagarjangam123Ainda não há avaliações
- A Note On Diseases Clinically Presenting As Desquamative GingivitisDocumento12 páginasA Note On Diseases Clinically Presenting As Desquamative GingivitisAshok KpAinda não há avaliações
- Gene Therapy in Oral CancerDocumento6 páginasGene Therapy in Oral CancerAshok KpAinda não há avaliações
- History of MicroscopeDocumento6 páginasHistory of MicroscopeAshok KpAinda não há avaliações
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceNo EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceNota: 4 de 5 estrelas4/5 (895)
- Never Split the Difference: Negotiating As If Your Life Depended On ItNo EverandNever Split the Difference: Negotiating As If Your Life Depended On ItNota: 4.5 de 5 estrelas4.5/5 (838)
- The Yellow House: A Memoir (2019 National Book Award Winner)No EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Nota: 4 de 5 estrelas4/5 (98)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeNo EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeNota: 4 de 5 estrelas4/5 (5794)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaNo EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaNota: 4.5 de 5 estrelas4.5/5 (266)
- The Little Book of Hygge: Danish Secrets to Happy LivingNo EverandThe Little Book of Hygge: Danish Secrets to Happy LivingNota: 3.5 de 5 estrelas3.5/5 (400)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureNo EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureNota: 4.5 de 5 estrelas4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryNo EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryNota: 3.5 de 5 estrelas3.5/5 (231)
- The Emperor of All Maladies: A Biography of CancerNo EverandThe Emperor of All Maladies: A Biography of CancerNota: 4.5 de 5 estrelas4.5/5 (271)
- The Unwinding: An Inner History of the New AmericaNo EverandThe Unwinding: An Inner History of the New AmericaNota: 4 de 5 estrelas4/5 (45)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersNo EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersNota: 4.5 de 5 estrelas4.5/5 (345)
- Team of Rivals: The Political Genius of Abraham LincolnNo EverandTeam of Rivals: The Political Genius of Abraham LincolnNota: 4.5 de 5 estrelas4.5/5 (234)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreNo EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreNota: 4 de 5 estrelas4/5 (1090)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyNo EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyNota: 3.5 de 5 estrelas3.5/5 (2259)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)No EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Nota: 4.5 de 5 estrelas4.5/5 (121)
- IMMUNE SYSTEM Notes MidtermsDocumento5 páginasIMMUNE SYSTEM Notes MidtermsAdiel Calsa100% (1)
- Immune System Lecture NotesDocumento2 páginasImmune System Lecture NotesPrabin KumarAinda não há avaliações
- Biology Chapter 5 Form 5Documento15 páginasBiology Chapter 5 Form 5Nadiah BorhanAinda não há avaliações
- Hypersensitivity ReactionsDocumento25 páginasHypersensitivity Reactionsbpt2100% (3)
- The Bodys DefenceDocumento106 páginasThe Bodys DefenceKaushikAinda não há avaliações
- Chapter 15 Nonspecific Host Defense MechanismsDocumento7 páginasChapter 15 Nonspecific Host Defense MechanismsmyfilesAinda não há avaliações
- Ilovepdf Merged PDFDocumento171 páginasIlovepdf Merged PDFA-Naeem To'mah Al-sawaieAinda não há avaliações
- 5 Immunological DisordersDocumento22 páginas5 Immunological DisordersPaula CárdenasAinda não há avaliações
- Surgery A 1.1Documento4 páginasSurgery A 1.1Aisha Al JenaibiAinda não há avaliações
- Bsaab2 11 Testing For MastitisDocumento20 páginasBsaab2 11 Testing For MastitisMohamed Ahmed Mohamed DhuxulAinda não há avaliações
- USMLE Road Map Immunology (001-102) PDFDocumento102 páginasUSMLE Road Map Immunology (001-102) PDFJonathan B Gutierrez LeyvaAinda não há avaliações
- MAAP Set 2Documento86 páginasMAAP Set 2AaronMaroonFive100% (1)
- Pathophysiology Test Bank CH 6-9Documento33 páginasPathophysiology Test Bank CH 6-9Joyy86% (7)
- Unit-1 Intro To ImmunologyDocumento49 páginasUnit-1 Intro To ImmunologyRituAinda não há avaliações
- How The Immune System WorksDocumento13 páginasHow The Immune System Worksnishant nagyan100% (2)
- The Body's System of Defenses Against Agents That Cause DiseaseDocumento8 páginasThe Body's System of Defenses Against Agents That Cause Diseasemaya100% (2)
- SBL100-Immunology Lectures 1-3Documento92 páginasSBL100-Immunology Lectures 1-3B.simhachalam100% (1)
- AQA Immunity BookletDocumento7 páginasAQA Immunity Bookletsu966Ainda não há avaliações
- Infection and Host ResistanceDocumento62 páginasInfection and Host ResistanceAndrea Marie T. Artajo-BoheromAinda não há avaliações
- Body Defences, Immunity, ImmunizationDocumento27 páginasBody Defences, Immunity, Immunizationenam professorAinda não há avaliações
- Study Guide For Lecture Exam 2 Biol 1407 03.12.2010Documento50 páginasStudy Guide For Lecture Exam 2 Biol 1407 03.12.2010Erica MizzIndependent BubuchuAinda não há avaliações
- Transport in Mammals: The Need For A Transport SystemDocumento2 páginasTransport in Mammals: The Need For A Transport SystemAhmed OmarAinda não há avaliações
- Turgeon Question and AnswersDocumento5 páginasTurgeon Question and AnswersBabylene MamauagAinda não há avaliações
- Human MilDocumento88 páginasHuman MilAmalia Dwi AryantiAinda não há avaliações
- Medicinal Mushrooms C HobbsDocumento38 páginasMedicinal Mushrooms C HobbsAnatole33100% (7)
- Chap 17 Reading WorksheetDocumento5 páginasChap 17 Reading WorksheetSarahAinda não há avaliações
- Infection and Immunity Bacterial, Viral and FungalDocumento30 páginasInfection and Immunity Bacterial, Viral and FungalCharrieBognotRagadiAinda não há avaliações
- Module 9: Lymphatic System & Immunity: InnateDocumento5 páginasModule 9: Lymphatic System & Immunity: InnatejunquelalaAinda não há avaliações
- The Health Consequences of Smoking - ARRT 24+ Cat. A Credits Test QuestionsDocumento14 páginasThe Health Consequences of Smoking - ARRT 24+ Cat. A Credits Test QuestionsTake CEAinda não há avaliações
- Role of The Circulatory System in The Body's Defence MechanismsDocumento15 páginasRole of The Circulatory System in The Body's Defence MechanismsArash Halim67% (3)