Escolar Documentos
Profissional Documentos
Cultura Documentos
Jcei 00528
Enviado por
Ginanjar JsDescrição original:
Título original
Direitos autorais
Formatos disponíveis
Compartilhar este documento
Compartilhar ou incorporar documento
Você considera este documento útil?
Este conteúdo é inapropriado?
Denunciar este documentoDireitos autorais:
Formatos disponíveis
Jcei 00528
Enviado por
Ginanjar JsDireitos autorais:
Formatos disponíveis
JCEI /
Cengiz et al. Surgical management of tuboovarian abscess 2012; 3 (4): 463-466 463 Journal of Clinical and Experimental Investigations doi: 10.5799/ahinjs.01.2012.04.0203
RESEARCH ARTICLE
Surgical management of tuboovarian abscess: Results of retrospective case series
Tubaovaryan apsenin cerrahi ynetimi: Olgu serilerinin retrospektif sonular
Hseyin Cengiz, Hediye Dadeviren, Murat Ekin, Cihan Kaya, kr Yldz, Levent Yaar
ABSTRACT Objectives: Tuboovarian abscess (TOA) is a serious and potentially life-threatening condition. Treatment modalities vary as broad spectrum of antibiotherapy, minimallyinvasive drainage procedures, invasive surgery or combinations of these interventions. The objective of this study was to evaluate surgically treated patients for TOA. Materials and methods: The medical records of 57 cases who had surgically treated for TOA at Bakirkoy Dr. Sadi Konuk Education and Research Hospital, Department of Obstetrics and Gynecology from January 2007 to September 2012 were evaluated retrospectively. Results: The average age was 37.2 years and the mean gravidity and parity were 2.9 and 2.1, respectively. The most common presenting symptom was abdominal pain 47.4% (n=27). Twenty eight (49.1%) of the patients had laparotomy and twenty nine (50.9%) of the patients had laparoscopic surgery. 6 patients had a ruptured TOA and 17.9% of the patients had complications. Conclusions: The choice of an open or laparoscopic surgical approach should be largely based on operator skill, experience, and ability to perform the necessary surgical maneuvers. J Clin Exp Invest 2012; 3(4): 463-466 Key words: Complication, laparoscopy, surgery, tuboovarian abscess ZET Ama: Tubaovaryan apse (TOA) ciddi ve hayati tehlikesi bulunan bir durumdur. Tedavi ekilleri olarak geni spektrumlu antibioterapi, minimal invaziv abse drenaj, invaziv cerrahi veya bu tedavi usullerinin kombinasyonunu iermektedir. Bu almann amac cerrahi olarak tedavi edilmi TOA olgularn deerlendirmektir. Gere ve yntem: Ocak 2007-Eyll 2012 tarihleri arasnda Bakrky Dr. Sadi Konuk Eitim ve Aratrma Hastanesi Kadn Hastalklar ve Doum kliniinde yatrlp cerrahi tedavisi yaplan hastalar retrospektif olarak incelendi. Bulgular: TOA olgularnda ortalama ya 37.2 olarak saptand. Ortalama gravida ve parite sras ile 2.9 ve 2.1 olarak bulundu. En sk saptanan semptom olarak %47.4 (n=27) oran ile karn ars izlendi. %49.1(n=28) hasta laparatomik cerrahi ve %50.9 (n=29) hasta laparaskopik cerrahi geirdi. 6 hastada rptre TOA izlendi ve %17.9 hastada komplikasyon geliti. Sonu: Gerekli cerrahi mdahaleleri gerekletirmek iin, ak veya laparoskopik cerrahi yaklamn seimi byk lde operatrn beceri, deneyim ve yeteneine baldr. Anahtar kelimeler: Cerrahi, Komplikasyon, laparoskopi, tubaovaryan apse
INTRODUCTION
A tuboovarian abscess (TOA) is an inflammatory mass involving the fallopian tube, ovary and other adjacent pelvic organs (eg, bowel, bladder) occasionally.1 These abscesses are seen most commonly in reproductive age women and typically originated from upper genital tract infection. TOA is a complication of pelvic inflammatory disease (PID) in 15% of cases, and 33% of patients requiring admission with PID, have a TOA.2 TOAs are polymicrobial infections and E.coli, B.fragilis, peptococci, peptostreptococci and mix flora especially encountered microorganisms in abscess cavity. The pathogen-
esis of TOA is due to fallopian tubal necrosis and epithelial damage by bacterial pathogens causing a favorable environment for anaerobic invasion and growth. Also these abscesses have important risk factors. Some of these risk factors are IUD use, age > 40, adoloscence, low socioeconomic status, multiple sex partners and nulliparity. The most important risk factor in tuba ovarian abscess formation is intercourse a partner having infection because of this disease caused by sexually transmitted infections. Malignancies, gynecological surgery, in vitro fertilization, perforated appendicitis and diverticulitis have also shown to cause abscess formation in lit-
Copyright JCEI / Journal of Clinical www.jceionline.org and Experimental Investigations 2012, All rights J Clin Exp Invest Vol 3,reserved No 4, December 2012
Bakrky Dr. Sadi Konuk Education and Research Hospital, Obstetrics and Gynecology stanbul, Turkey Correspondence: Hseyin Cengiz, Bakrky Dr. Sadi Konuk Education and Research Hospital Obstetrics and Gynecology stanbul Email: obstetrik@gmail.com Received: 11.10.2012, Accepted: 30.11.2012
464
Cengiz et al. Surgical management of tuboovarian abscess
erature. Also it is rarely seen in virgins. In literatue a few cases were published about TOA in virgin patients.3 TOAs especially result in irreversible tubal and ovarian damage and this is a potential threat to fertility. Also this disease may be accompanied other complications such as incapacitating abdominal pain, ectopic pregnancy and abscess rupture. Aggressive medical and/or surgical therapy is required and rupture of an abscess may result in sepsis.4,5 Mortality associated with TOA has decreased dramatically over the last 50 years, however the route of management varies. Treatment modalities include broad spectrum antibiotherapy, minimallyinvasive drainage procedures, invasive surgery, or combinations of these interventions. The objective of this study was to evaluate surgically treated patients for TOA.
inflammatory debris.6-8 Complications were defined as factors that could result in prolonged hospitalization as; intensive care unit (ICU) admission, bowel or bladder injury, blood transfusion, blood loss >1000 mL, sepsis or bacteremia, ileus, conversion from laparoscopy to laparotomy, and death. Fever was defined as a temperature greater than 38C. In our series, antibiotics were started all the patients at the admission to the hospital. After 48 to 72 hours of treatment with antibiotics alone, patients who do not respond to the medical therapy or who had a worsen vital findings, required either minimally invasive abscess drainage or surgery. Statistical Analysis was performed by using the SPSS 20.0 Statistical Software Package (SPSS, Chicago, IL, USA).
MATERIALS AND METHODS
The medical records of the patients who had surgically treated for TOA at Bakirkoy Dr. Sadi Konuk Education and Research Hospital, Department of Obstetrics and Gynecology from January 2007 to September 2012 were evaluated retrospectively. Patients were preoperatively diagnosed as TOA relying on laboratory and ultrasonographic findings in the presence of a mass at the pelvic examination. Ultrasonographic images of TOAs were complex multilocular masses that often obliterate the normal adnexal architecture and/or cul-de-sac anatomy, speckled fluid and internal echoes consistent with
RESULTS
57 patients with preoperative diagnosis of TOA were undergone for surgical treatment. The average age was 37.2 years and the mean gravidity and parity were 2.9 and 2.1, respectively. 21.1% of the cases had a history of PID and 17.5% of the patients had smoking habit. The most common symptom was abdominal pain 47.4% (n=27). 29.8% (n=17) of the cases had fever during admission. 49.1% (n=28) of the patients had laparotomy and %50.9 (n=29) had laparoscopic surgery.6 patients had a ruptured TOA and 17.9% of the patients had complications. Clinical characteristics of the study population are noted in Table 1.
Table 1. Clinical characteristics of the patients with tubo-ovarian abscess Mean SD/ n Age Gravidity Parity Smoking Previous PID Contraception Pain Abnormal uterine bleeding Abnormal discharge Fever Rebound Guarding Uterine tenderness Adnexal tenderness Cervical motion tenderness Treatment laparatomy Treatment laparoscopy 37,29,1 2,91,7 2,11,2 10 12 21 27 12 17 17 18 19 24 24 21 28 29 % WBC, /mm WBC 17,5% 21,1% 36,8% 47,4% 21,1% 29,8% 29,8% 31,6% 33,3% 42,1% 42,1% 36,8% 49,1% Abscess location
3
Mean SD/n <10000 10000 to 15000 >15000 Right Left Bilateral 0-4 cm 5-8 cm >8 cm 0 1 2 3 142544554 13 19 25 15 29 13 15 28 14 44 4 8 1 10 6 6,33,8
% 22,8% 33,3% 43,9% 26,3% 50,9% 22,8% 26,3% 49,1% 24,6% 77,2% 7,0% 14,0% 1,8% 17,9% 10,5%
Abscess size
Febrile days
Complication Rupture
50,9% Hospitalization (Days)
PID, Pelvic inflammatory disease; WBC, White blood cells, SD= standard deviation
J Clin Exp Invest
www.jceionline.org
Vol 3, No 4, December 2012
Cengiz et al. Surgical management of tuboovarian abscess
Table 2. Comparison of some variables according to existence of fever in tubo-ovarian abscess patients Febrile Negative MeanSD/n WBC WBC <10000 10000 to 15000 >15000 Complication Hospitalization (Days) Negative Positive 132504157 13 14 17 36 7 6,54,1 29,5% 31,8% 38,6% 83,7% 16,3% % Positive MeanSD/n 176504318 0 5 8 10 3 5,52,3 0,0% 38,5% 61,5% 76,9% 23,1% % p
465
0,002 0,075
0,575 0,075
Chi-square test / I.S t test, WBC, White blood cells, SD= standard deviation
DISCUSSION
Tuboovarian abscesses are usually found among reproductive age women. Abdominal pain, vaginal discharge and fever are usually seen in TOA patients.9 In our series, we found abdominal pain as the most common presenting symptom. Ginsburg et al10 reported previous PID in TOA patients as %49. Our patients had a 21.1% previous PID rate. Diagnosing and managing adnexal masses can be problematic for physicians. A preoperative disease classification for patients with adnexal masses, in particular discrimination between benign and malignant ovarian tumors, is important for optimal patient management.11 It is unclear whether a subjective evaluation of a US image (i.e., pattern recognition) of an adnexal mass. In one study the sensitivity of ultrasonography in the diagnosis of TOA was found as 93%, while specificity was 98.6%.12 In our daily practice we also use ultrasonography as a major diagnostic tool. Medical management with broad spectrum antibiotics is now generally considered as the initial management for unruptured Tubaovarian abscess.13 TOAs are polymicrobial infections and E.coli, B.fragilis, peptococci, peptostreptococci, A. israeli and mix flora especially encountered microorganisms in abscess cavity. The 2010 Center for Disease Control and Prevention Sexually Transmitted Diseases Treatment Guidelines recommends inpatient intravenous antibiotics for at least 24 hours. No specific inpatient antibiotic regimen is suggested. Upon discontinuation of parenteral therapy, the CDC recommends that clindamycin or metronidazole be used with doxycycline for a total of 14 days of treatment. Treatment of TOA was thought to require bilateral oophorectomy and hysterectomy. However, optimal treatment of TOA remains unclear. Doganay M. et al14 aimed to find out the optimal therapauJ Clin Exp Invest
tic approach in patients. They were used a scoring system for defining the beneficial treatment modality. According to their study laparascopy seems to be the optimal treatment modality and medical treatment may be a reasonable alternative in well selected cases since it does not carry a risk of operative complications. Surgery or drainage should be considered when the patient displays a failure to respond to therapy in 48 to 72 hours.15 In our clinic, we use the same algorithm for TOA. Today, the preferable management options are minimally invasive technics with conservative approach. In many clinics laparoscopy has been the gold standard for the diagnosis and treatment of TOA. Henry-Suchet et al carried out laparoscopic adhesiolysis and drainage of abscess in combination with antibiotics in 50 women.16 In 45 patients (90%) the approach was successful, while five patients (10%) required further surgery. Reich et al reported no complications following laparoscopic and organ-preserving management of tubo-ovarian abscess in 25 patients.17 Raiga et al also demonstrated that operative laparoscopy involving drainage of adnexal abscesses is a safe and effective procedure.18 In our study, 29 patients treated laparoscopically. Buchweitz et al reported no complications in the patients who underwent laparoscopic organ-preserving treatment.19 We defined conversion from laparoscopy to laparotomy as a complication and we evaluate these cases within the laparotomy group. 10 patients had complications in our study but 7 of them were laparoscopy to laparatomy conversion. There were two bowel injuries in 28 patients undergoing laparatomy. Only one port side infection occurred with laparoscopy in 29 patients undergoing laparoscopy. The limitations of our study include a relatively small number of TOAs In conclusion, the choice of an open or laparoscopic surgical approach should be largely based
Vol 3, No 4, December 2012
www.jceionline.org
466
Cengiz et al. Surgical management of tuboovarian abscess
10. Ginsburg DS, Stern JL, Hamod KA, Genadry R, Spence MR. Tubo-ovarian abscess: a retrospective review. Am J Obstet Gynecol 1980;138:10558. 11. Yildiz P, Cengiz H, Yildiz G, Sam DA, Yavuzcan A, Celikbas B, Sahin L. Two Unusual Clinical Presentations of Broad Ligament Leimyomas: A Report of Two Cases. Medicina (Kaunas) 2012;48(3):163-5. 12. Taylor KJ, Wasson JF, De Graaff C et al. Accuracy of grey-scale ultrasound diagnosis of abdominal and pelvic abscesses in 220 patients. Lancet 1978;1:8384. 13. R. L. Sweet, Tubo-ovarian abscess, in Pelvic Inflammatory Disease, pp. 101-124, Taylor & Francis, London, UK, 2006. 14. Doganay M, Iskender C, Kilic S, Karayalcin R, Moralioglu O, Mollamahmutoglu L. Treatment approaches in tubo-ovarian abscesses according to scoring system. Bratisl Lek Listy 2011;112(4):200-3. 15. L. A. McNutt, C. Wu, X. Xue, and J. P. Hafner, Estimating the relative risk in cohort studies and clinical trials of common outcomes, Am J Epidemiol 2003;157(10):940-3. 16. Henry-Suchet J, Soler A & Loffredo V. Laparoscopic treatment of tuboovarian abscesses. J Reprod Med 1984;29(8):579-82. 17. Reich H & McGlynn F. Laparoscopic treatment of tuboovarian and pelvic abscess. J Reprod Med 1987;32(10):747-52. 18. Raiga J, Canis M, Le Boue dec G et al. Laparoscopic management of adnexal abscesses: consequences for fertility. Fertil Steril 1996;66(5):712-7. 19. Buchweitz O, Malik E, Kressin P et al. Laparoscopic management of tubo-ovarian abscesses: retrospective analysis of 60 cases. Surg Endosc 2000;14(10):94850.
on operator skill, experience, and ability to perform the necessary surgical maneuvers given the anatomical distortion.
REFERENCES
1. Granberg S, Gjelland K, Ekerhovd E. The management of pelvic abscess. Best Pract Res Clin Obstet Gynaecol 2009;23(5):667. 2. D. V. L anders and R. L. Sweet, Tubo-ovarian abscess: contemporary approach to management, Reviews of Infectious Diseases, vol. 5, no. 5, pp. 876-884, 1983. 3. Tuncer SZ, Boyraz G, Ycel S, Seluk I, Yazcoglu A. Tuboovarian abscess due to colonic diverticulitis in a virgin patient with morbid obesity: A case report. Case Report Med 2012;2012: 413185 4. Pedowitz P, Bloomfield Rd. Ruptured adnexal abscess (tuboovarian) with generalized peritonitis. Am J Obstet Gynecol 1964;88: 721. 5. Vermeeren J, Te Linde Rw. Intraabdominal rupture of pelvic abscesses. Am J Obstet Gynecol 1954; 68(1):402. 6. Landers DV, Sweet RL. Tubo-ovarian abscess: contemporary approach to management. Rev Infect Dis 1983;5(5):876. 7. Wiesenfeld HC, Sweet RL. Progress in the management of tuboovarian abscesses. Clin Obstet Gynecol 1993;36(2):433. 8. Gagliardi PD, Hoffer PB, Rosenfield AT. Correlative imaging in abdominal infection: an algorithmic approach using nuclear medicine, ultrasound, and computed tomography. Semin Nucl Med 1988;18(4):320. 9. Martens MG. Pelvic inflammatory Disease. In: Rock JA, Jones HW, editors. 9th ed. TeLindes Operative Gynecology 2003. P. 675-704.
J Clin Exp Invest
www.jceionline.org
Vol 3, No 4, December 2012
Você também pode gostar
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceNo EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceNota: 4 de 5 estrelas4/5 (890)
- The Yellow House: A Memoir (2019 National Book Award Winner)No EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Nota: 4 de 5 estrelas4/5 (98)
- The Little Book of Hygge: Danish Secrets to Happy LivingNo EverandThe Little Book of Hygge: Danish Secrets to Happy LivingNota: 3.5 de 5 estrelas3.5/5 (399)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeNo EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeNota: 4 de 5 estrelas4/5 (5794)
- Never Split the Difference: Negotiating As If Your Life Depended On ItNo EverandNever Split the Difference: Negotiating As If Your Life Depended On ItNota: 4.5 de 5 estrelas4.5/5 (838)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureNo EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureNota: 4.5 de 5 estrelas4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryNo EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryNota: 3.5 de 5 estrelas3.5/5 (231)
- The Emperor of All Maladies: A Biography of CancerNo EverandThe Emperor of All Maladies: A Biography of CancerNota: 4.5 de 5 estrelas4.5/5 (271)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreNo EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreNota: 4 de 5 estrelas4/5 (1090)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyNo EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyNota: 3.5 de 5 estrelas3.5/5 (2219)
- Team of Rivals: The Political Genius of Abraham LincolnNo EverandTeam of Rivals: The Political Genius of Abraham LincolnNota: 4.5 de 5 estrelas4.5/5 (234)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersNo EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersNota: 4.5 de 5 estrelas4.5/5 (344)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaNo EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaNota: 4.5 de 5 estrelas4.5/5 (265)
- The Unwinding: An Inner History of the New AmericaNo EverandThe Unwinding: An Inner History of the New AmericaNota: 4 de 5 estrelas4/5 (45)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)No EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Nota: 4.5 de 5 estrelas4.5/5 (119)
- Case Study PneumoniaDocumento14 páginasCase Study PneumoniaJester GalayAinda não há avaliações
- Recall of Frozen Mixed BerriesDocumento2 páginasRecall of Frozen Mixed BerriesEmad KhattabAinda não há avaliações
- Abnormal PuerperiumDocumento23 páginasAbnormal Puerperiumseema pundirAinda não há avaliações
- Cleaning For Health in The ClassroomDocumento5 páginasCleaning For Health in The ClassroomCarol WestinghouseAinda não há avaliações
- BronchiectasisDocumento17 páginasBronchiectasisBharat GaikwadAinda não há avaliações
- Anopheles Gambiae S.S. Plasmodium FalciparumDocumento9 páginasAnopheles Gambiae S.S. Plasmodium Falciparumibrahima1968Ainda não há avaliações
- Chapter 5 Normal Flora of The Human BodyDocumento15 páginasChapter 5 Normal Flora of The Human BodyPrincess Angie GonzalesAinda não há avaliações
- Bio ShieldDocumento3 páginasBio ShieldVimal GopalakrishnanAinda não há avaliações
- Viral HepatitisDocumento12 páginasViral HepatitisHeart Of Ayurveda Beatrice DAinda não há avaliações
- Comparative Analysis of Pipe Borne Water and Other Sources of Water in Gwagwalada Area Council, Federal Capital Territory, Abuja, NigeriaDocumento10 páginasComparative Analysis of Pipe Borne Water and Other Sources of Water in Gwagwalada Area Council, Federal Capital Territory, Abuja, NigeriaEsaenwi ThankGodAinda não há avaliações
- Bacte Lesson - 1 Prelim - 1 1Documento22 páginasBacte Lesson - 1 Prelim - 1 1Yormae QuezonAinda não há avaliações
- Fungal Infections in IcuDocumento195 páginasFungal Infections in IcubhumikaAinda não há avaliações
- Viral Infections: Presented By: Fatimah Zahraa Ahmed Supervised By: DR - RafilDocumento31 páginasViral Infections: Presented By: Fatimah Zahraa Ahmed Supervised By: DR - Rafilfatimah zahraaAinda não há avaliações
- Infectious DiseasesDocumento3 páginasInfectious Diseasesshreyavjha2020Ainda não há avaliações
- Main 2Documento5 páginasMain 2monica trifitrianaAinda não há avaliações
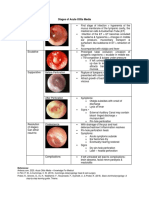
- Stages of Acute Otitis MediaDocumento1 páginaStages of Acute Otitis MediaNicole Marie NicolasAinda não há avaliações
- IN - AJA - Dazel Kit - Plan - V1 - 19042016Documento16 páginasIN - AJA - Dazel Kit - Plan - V1 - 19042016nagaraj2675Ainda não há avaliações
- Term 2 Examination Pointers For MCN LectureDocumento11 páginasTerm 2 Examination Pointers For MCN Lecturezyyw.abello.uiAinda não há avaliações
- Bero 2009 2Documento33 páginasBero 2009 2Shalie VhiantyAinda não há avaliações
- SyncytiumDocumento87 páginasSyncytiumjustin sAinda não há avaliações
- Occupational and Environmental Health: Prepared by Ms Yasmeen Bibi MR Asif ShahDocumento67 páginasOccupational and Environmental Health: Prepared by Ms Yasmeen Bibi MR Asif ShahAamirAinda não há avaliações
- Wuhan Laboratories, Bat Research and BiosafetyDocumento143 páginasWuhan Laboratories, Bat Research and BiosafetyDrastic ResearchAinda não há avaliações
- Betty Knight's "6F S": FluidsDocumento1 páginaBetty Knight's "6F S": FluidsESTHER OGODOAinda não há avaliações
- What is an infectious diseaseDocumento14 páginasWhat is an infectious diseaseLucky Radita Alma100% (1)
- Dental Laboratory Infection ControlDocumento6 páginasDental Laboratory Infection ControlDrShweta SainiAinda não há avaliações
- WIDALDocumento17 páginasWIDALNasti YL HardiansyahAinda não há avaliações
- Answer Key: ComprehensionDocumento5 páginasAnswer Key: ComprehensionPriyanka GandhiAinda não há avaliações
- Food Quality, Food-Borne Diseases, and Food Safety in The Brazilian Food IndustryDocumento15 páginasFood Quality, Food-Borne Diseases, and Food Safety in The Brazilian Food IndustryAnil BhattiAinda não há avaliações
- Visiting Scholar ChecklistDocumento9 páginasVisiting Scholar Checklistসোমনাথ মহাপাত্রAinda não há avaliações
- ACTINOMYCESDocumento47 páginasACTINOMYCESSushant KumarAinda não há avaliações