Escolar Documentos
Profissional Documentos
Cultura Documentos
Fotografia 1
Enviado por
Ana Maria Olivo Ulloa0 notas0% acharam este documento útil (0 voto)
22 visualizações9 páginasClinical photography is an essential facility to support the work of cranio-maxillo-facial surgical departments. This paper highlights the requirements to ensure the highest quality and consistency of photographs taken. It also provides assistance in the selection of equipment, archival storage and error avoidance.
Descrição original:
Título original
FOTOGRAFIA 1
Direitos autorais
© © All Rights Reserved
Formatos disponíveis
PDF, TXT ou leia online no Scribd
Compartilhar este documento
Compartilhar ou incorporar documento
Você considera este documento útil?
Este conteúdo é inapropriado?
Denunciar este documentoClinical photography is an essential facility to support the work of cranio-maxillo-facial surgical departments. This paper highlights the requirements to ensure the highest quality and consistency of photographs taken. It also provides assistance in the selection of equipment, archival storage and error avoidance.
Direitos autorais:
© All Rights Reserved
Formatos disponíveis
Baixe no formato PDF, TXT ou leia online no Scribd
0 notas0% acharam este documento útil (0 voto)
22 visualizações9 páginasFotografia 1
Enviado por
Ana Maria Olivo UlloaClinical photography is an essential facility to support the work of cranio-maxillo-facial surgical departments. This paper highlights the requirements to ensure the highest quality and consistency of photographs taken. It also provides assistance in the selection of equipment, archival storage and error avoidance.
Direitos autorais:
© All Rights Reserved
Formatos disponíveis
Baixe no formato PDF, TXT ou leia online no Scribd
Você está na página 1de 9
Journal of Cranio-Maxillofacial Surgery (2006) 34, 6573
r 2005 European Association for Cranio-Maxillofacial Surgery
doi:10.1016/j.jcms.2005.11.002, available online at http://www.sciencedirect.com
Standards for digital photography in cranio-maxillo-facial surgery Part I:
Basic views and guidelines
Giovanni ETTORRE
1
, Martina WEBER
1
, Heidrun SCHAAF
1
, John C. LOWRY
2
, Maurice
Y. MOMMAERTS
3
, Hans-Peter HOWALDT
1
1
Department of Oral and Maxillofacial Plastic Surgery (Chairperson: Prof. Dr. Dr. H.-P. Howaldt), Justus
Liebig University, Giessen, Germany;
2
Department of Maxillofacial Surgery (Consultant: Prof. J.C. Lowry,
FRCS, FDSRCS), Royal Bolton Hospital, Bolton, UK;
3
Bruges Cleft & Craniofacial Center (Director: Prof.
M.Y. Mommaerts, MD, DMD, PhD, FEBOMS, FICS), Brugge, Belgium
SUMMARY. Clinical photography is an essential facility to support the work of cranio-maxillo-facial surgical
departments. This paper highlights the requirements to ensure the highest quality and consistency of photographs
taken and provides a standardized set of both facial and intra-oral views that t the needs of accurate digital photo-
documentation in cranio-maxillo-facial surgery. Furthermore it gives assistance in the selection of equipment,
archival storage and error avoidance.
These guidelines have been approved in November 2005 by the Council of the European Association for
Cranio-Maxillo-Facial Surgery and are to be understood as a proposal to all our colleagues in Maxillofacial
Surgery. r 2005 European Association for Cranio-Maxillofacial Surgery
Keywords: digital; photography; standards; clinical; maxillofacial; surgery; guidelines
INTRODUCTION
Complex clinical appearances of patients in cranio-
maxillo-facial surgery and facial plastic surgery are
usually difcult to describe in words. Therefore,
much of our professional time is spent in judging and
discussing pictures and photographs. For that pur-
pose standardized views and high-quality photo-
graphs are fundamental for pre- and postoperative
documentation. Clinical photographs are most com-
monly used to assist accurate planning of a surgical
procedure and to illustrate the purpose of the surgical
intervention for the patient. Consistent documenta-
tion of clinical diagnosis and treatment is also
demanded in medico-legal cases. In addition, photo-
documentation with reliable pre- and postoperative
pictures are invaluable for scientic development,
surgical education and staff training (Shaw et al.,
2001). In the authors view high-quality clinical
photographs should become an integral part of the
patients record just as radiographs and other medical
images.
Although several publications discuss medical
photography, the authors and probably most readers
have had numerous disappointing experiences
when searching clinical les in preparation for a
lecture. Moreover, most manuscripts focus on the
need of documentation in plastic surgery, dermatol-
ogy and orthodontics (Zarem, 1984; Jemec and
Jemec, 1981; DiBernardo et al., 1998; Becker and
Tardy, 1999; Galdino et al., 2001, 2002; Sullivan, 2002;
McKeown et al., 2005). In these publications,
documentation of special features such as the
anatomy of the nose or skin pathology by means of
analogue photography are highlighted, while none of
them explain the particular requirements for digital
photography and the special areas of interest in
cranio-maxillo-facial surgery.
This paper also aims to provide assistance in the
acquisition of the necessary equipment and denes a
range of standard photographic views for cranio-
maxillo-facial surgery. It is suggested that these
picture sets may now lay the foundation for the
introduction of a European-wide standard in photo-
graphy for cranio-maxillo-facial surgery in order to
ensure greater precision and comparability of results
for treatment planning, clinical records, education
and scientic congresses.
DIGITAL PHOTOGRAPHY
Advantages and disadvantages of digital photography
Several camera manufacturers have invested consid-
erable effort in the development of digital single
lens reex cameras (SLR-cameras) for semi-profes-
sional use and this has resulted in a progressive
decrease in their prices. For example, 10 years ago
a digital SLR-camera with a resolution of 4 Mega-
pixels may have cost 10,000 euros, whereas today a
ARTICLE IN PRESS
65
high-quality SLR-camera with 6 or even 8 Mega-
pixels may be obtained for 10001500 euros.
Although digital SLR-cameras are more expensive
than analogue cameras, this relatively small nancial
disadvantage is now counterbalanced by the signi-
cant advantages of digital photography.
In contrast to the analogue technique where the
photographs are displayed on a 24 35 mm lm,
digital images are stored on an electronic photo-
sensitive digital chip. The size of these photosensitive
chips varies between manufacturers, but is generally
about 1.5 times smaller than a 24 35 mm lm.
Discussion about the resulting elongation of focal
length is complex and can easily be avoided by
increasing the distance between the camera and
patient to obtain the recommended display window.
Digital pictures are immediately available with
neither lms nor processing being required, thereby
economizing on time and costs.
Moreover, direct control of the taken picture is
possible, and if it is not consistent with the photo-
graphers perception of what is required, it can be
retaken without arranging a new appointment with
the patient. This convenience is especially useful for
the documentation of pathology, developmental
anomalies and other diseases in small children.
If necessary close-up views can easily be obtained
by enlargement. This reduces the number of required
pictures. Storage is quick and space saving in digital
archives with the facility for pictures to be tagged
with multiple indices. This facilitates rapid access
when preparing lectures and other presentations.
EQUIPMENT, TECHNIQUE AND
REQUIREMENTS
Camera, card reader, personal computer, monitor and
colour printer
To ensure high-quality photo-documentation, the
standard equipment should include a digital SLR-
camera, a digital memory chip card, a chip card
reader, a personal computer (PC) with a monitor, a
colour printer and a suitable program for storage of
the indexed pictures as patients les.
We recommend the use of a digital SLR-camera as
it provides high-quality pictures combined with the
possibility of variation of lenses. Most digital
cameras offer the possibility of blending a grid with
the viewer, thereby facilitating a more precise and
reproducible presentation of the patients face re-
lative to the peripheral background. If a switch from
the earlier 35 mm camera equipment is planned, the
existing lenses are often compatible with a digital
SLR-camera body from the same manufacturer.
The transfer of pictures from the camera to the PC
can easily be solved by using a card reader or by
direct connection of the camera with the PC and
appropriate software via FireWire or USB connec-
tion. To ensure fast processing and display of the
pictures, the authors recommend a PC with at least
1 GHz processors combined with a 128 MB graphic
card and a 40 GB hard disc to provide sufcient data
space. If the display of colour varies between different
monitors, it is necessary for these to be calibrated.
The different image replication of TFT-displays
(thin-lm transistor or at screen) compared to
standard cathode ray tube monitors should be noted.
For immediate prints of the photographs, a high-
quality colour printer should be available.
Lenses
We suggest a xed focal length (90105 mm) high-
quality macrolens for both facial and intra-oral
pictures. High-quality lenses assure a maximum
depth of eld, with the smallest possible distortion
and minimal alteration of colours. The suggested
focal length (known as portrait) reproduces a
natural anatomy without the bulging that occurs
with wide angle lenses, and provides for an adequate
distance between the camera and patient. Pre- and
postoperative pictures should be taken with the same
lens to avoid the variation of images that occurs with
different focal lengths.
Although the size of the images obtained by
photosensitive chips differs from those of analogue
lms, it is preferred to use a 90105 mm lens to allow
comparison with previously taken pictures using
analogue 35 mm cameras. It is important to mention
that proportions and distortion remain constant if the
subject to object distance is adapted by a factor of
1.51.6 dependent on the chip size in the used digital
camera.
BACKGROUND AND LIGHTING
In the authors opinion, a light blue (sky blue, RAL
5012) background is ideal for medical photography,
as it provides a sufcient contrast to skin colour and
moderates shadows. A white background produces
harsh shadows, while a black background provides
less contrast for dark-skinned subjects.
Lighting is one of the most discussed aspects of
medical photography. Regardless of the high acquisi-
tion costs, a ceiling mounted, multi-ashlight instal-
lation is recommended with at least two soft boxes or
two umbrellas for taking facial pictures, thereby
avoiding cables on the oor. This set-up offers the
possibility of constant lighting conditions (intensity
and angle) with even illumination of the subject when
used correctly.
The soft boxes should be positioned at an angle of
451, with a constant distance of 11.5 meters at either
side in front of the patient. They should be positioned
as close as possible together, as this minimizes
shadows on the patients face.
A manual setting of exposure time and aperture
setting is recommended, as through-the-lens metering
is not always reliable. Under studio light conditions,
ARTICLE IN PRESS
66 Journal of Cranio-Maxillofacial Surgery
high aperture settings (f416) and short exposure
time (o1/125 s) can easily be achieved. This guaran-
tees appropriate depth of eld and prevents loss of
sharpness attributable to shaking of the camera. As a
result of constant quality (almost one light tempera-
ture) and amount of lighting, the white balance of
digital cameras can be set on the provided ashlight
setting. As digital pictures can immediately be
assessed, it is suggested that several pictures be taken
with different aperture settings (e.g. f 16; 18, 20;
trial and error) rather than using a handheld light
meter.
For intra-oral pictures, the ring light ash provides
adequate illumination, while for an adequate depth of
eld, maximal aperture settings (f427) are recom-
mended.
Patient consent form
Patients consent is required if pictures are to be used
for scientic purposes such as congresses, publica-
tions, media presentation and internet-based con-
sultation projects (for example the one on the
Eurofaces website of the European Association for
Cranio-Maxillo-Facial Surgery). The consent form
should be easily understood and should not exceed
one page. The patient should be informed that
pictures are part of the individual le and support
planning of treatment as well as the follow-up. It
should be made clear that the patients permission is
voluntary and withholding consent will be in no way
a disadvantage regarding clinical care. Patients
should have the freedom to restrict the utilization
of pictures for scientic purposes.
A standardized consent form in most European
languages is also available on the home page of the
European Association for Cranio-Maxillo-Facial
Surgery (www.eurofaces.com).
Data storage and presentation
Data should not be stored on a local PC without
backup to prevent loss that may occur in the event of
a system crash. Regular backup copies should be
made to a CD, DVD, external hard disc, ash drive
or by server solutions.
As the pictures are part of the patients le,
maximum security must be assured. The databases
should provide log-in facilities in order to prevent
unauthorized data access. If the pictures are stored in
a hospital-wide network, access for clinicians of other
departments should be discussed to facilitate inter-
disciplinary discussion. However, interdisciplinary
availability must be gauged with sensitivity, and it
is generally thought to be prudent where institution-
wide networks allow individual log-in facilities for
each physician for the separate data bases for each
department.
There are several databases in the market, which t
the needs of clinical picture storage. In general they
should be able to recognize the established image
formats and provide the possibility to create folders
and keywords. There are two general principles for
the organization of clinical image data: one patient-
based and the other on diagnosis or keyword.
A combination of the two has several advantages.
Searching is simplied as retrieval for presentations
may be via special topics or alternatively via patients
name for case reports or discussions with other
physicians. Storage and labelling of pictures should
occur immediately after taking the pictures to prevent
loss of photographs or misling. In addition, doctors
can easily obtain their own pictures after each
program rotation, and this might increase the
motivation to capture accurate photographs.
As many image editing programs cause data loss
when pictures are manipulated, care must be taken
when selecting a suitable software program. Lectures
may be prepared using an appropriate presentations
graphics package such as Microsoft Power Point
R
.
CONVENTIONAL FACIAL PICTURE SET
General notes
In pre- and postoperative photography the results are
only comparable when the patients position is
reproducible. A constant distance from the subject
to camera is preferred, which is achieved by marks on
the oor showing the position of the patient and
photographer. Although this approach produces
inter-individual differences in size due to different
anatomical proportions between patients, it has
several advantages: rst it is time saving to take up
a predened position compared to methods when
orientation is obtained by anatomical structures.
Moreover, mainly intra-individual comparison is
practised, e.g. preoperative vs. postoperative photo-
graphs. Furthermore, standardized positions for the
photographer and patient facilitate comparable
results concerning reproduction ratios. To compen-
sate for inter-individual differences in reproduction
ratios, e.g. for lectures, digital photos can easily be
adjusted in size. It is therefore suggested to obtain
slightly larger image frames to allow cropping if
necessary.
The camera height must be at the same level as the
focus point. The respective focus points are men-
tioned in the detailed picture descriptions in the
related chapter. In order to allow the patient and
camera to be at the same height, it is suggested to use
chairs allowing adjustment of the vertical position.
To reduce the need for height changes for every single
picture, most of the suggested focus points are
aligned to the Frankfort horizontal plane. To ensure
constant positions of the spine and head, the patients
chair should be equipped with a backrest.
Finally, all kinds of jewellery or excessive make-up
should be removed before taking clinical pictures.
Long hair should be held out of the area of clinical
ARTICLE IN PRESS
Standards for digital photography in cranio-maxillo-facial surgery 67
interest with hairpins or hair ties, and clothing should
allow the neck to be clearly seen.
The following pictures are featured with a grid that
resembles the grating provided in digital cameras to
clarify positioning of the patient, while the focus
point is illustrated by the circle in the middle of the
grid.
Full face front view
Fig. 1A shows the full face front view. For the full
face frontal view, the patients head should be aligned
to the Frankfort horizontal line. Focus point and
centre of the picture is the intersection between the
Frankfort horizontal line and the midline of the face.
The patient should look straight ahead into the lens
and the interpupillary line should be horizontal. No
rotation in the vertical axis should occur. Lips should
be relaxed with a visible interlabial gap if existing.
The lower margin is the uncovered sterno-clavicular
joint and the background should be visible around
the face.
By enlargement, the following close-up views can
be achieved of the full face front view: front view of
eyes, front view of lower face and jaw, front view of
nose, front view of auricles.
The oblique view
Fig. 1B shows the right oblique view. The patients
head is positioned in a similar way as for the full face
view, but rotated 451 to either side. This position is
preferred as it is independent of the size of the nose in
contrast to the alignment of the nose with the cheek.
This might affect the postoperative position when
nose correction has been performed. Constant patient
position can easily be obtained by a mark xed on the
wall at a 451 position on either side. Focus point and
centre of the picture is on the Frankfort horizontal
line at the junction with the lateral canthus. The
lower margin is the sterno-clavicular joint.
By enlargement, the following close-up views can
be achieved from the oblique view: oblique view of
eyes, oblique view of the lower face and jaw, oblique
view of the nose.
Prole view
Fig. 1C shows the right prole view. The patients
head is positioned in a similar way as for the frontal
view, but rotated at 901 to either side. The
contralateral eyebrow should not be visible. Lips
should be relaxed and an interlabial gap should be
visible. The focus point and centre of the picture is on
the Frankfort horizontal line in the midline between
the tragus and lateral canthus. The lower margin is
the sterno-clavicular joint.
By enlargement, the following close-up views can
be achieved of the prole view: prole view of eyes,
prole view of the lower face and jaw, prole view of
the nose, lateral aspect of auricles.
ADDITIONAL FACIAL PICTURES
Front view, closed eyes
Fig. 2A shows the front view with closed eyes. The
patients head is positioned in a similar way as for the
full face view with relaxed eyelid closure. This picture
is felt to be useful for planning surgery on eyelids (e.g.
blepharoplasty) and documentation and evaluation
of facial palsy.
By enlargement, close-up views can be achieved of
the full face with closed eyes.
Front view, smiling
Fig. 2B shows the front view with smile. The patients
head is positioned in a similar way as for the full face
front view. Full smiling is accomplished when the
eyelids are slightly narrowed, compared to the
ARTICLE IN PRESS
Fig. 1 Full face front, oblique, and prole views.
68 Journal of Cranio-Maxillofacial Surgery
relaxed position, and patients should show a small
part of maxillary gingival tissue, provided that there
is a normal cranial conguration. This picture is
helpful for planning orthognathic and cleft surgery,
as well as documentation and evaluation of facial
palsy.
By enlargement, close-up views can be achieved of
the full face view with smile and frontal view of the
lower face with smile.
Back view, with ears
Fig. 2C shows the back view with ears. Reference for
the patients head position is the full face front view
with a 1801 turn. It is important to note that the ears
should not be covered by the patients hair. This
picture is thought to be useful for planning surgery
on prominent or hypoplastic auricles.
By enlargement, the following close-up view can be
achieved of the back view with ears: back view of ears
and of the neck.
Front view, lip retractor
Fig. 3A shows the front view with lip retractor.
Reference for patients head position is the full face
front view. The picture of the patient should be taken
in relaxed rest position with a slightly open mouth
(incisal edge distance about 5 mm) so that the
occlusal plane can be seen. This picture is useful for
evaluating the occlusal plane in relation to the
interpupillary line when orthognathic surgery is
planned. Furthermore, complex facial skull deformi-
ties can be documented (e.g. hemifacial microsomia).
Front view, spatula in occlusion plane
Fig. 3B shows the front view with the spatula in
occlusal plane. The spatula should be placed between
the canine teeth. Although the display of the occlusal
plane is not always accurate because of dental
anomalies (e.g. asymmetrical abrasion, asymmetrical
dental hypoplasia), the front view with the spatula in
ARTICLE IN PRESS
Fig. 3 (A) Front view with lip retractor; (B) front view with spatula in occlusal plane and (C) submental oblique view.
Fig. 2 Front views with closed eyes (A), smiling (B); back view with ears visible (C).
Standards for digital photography in cranio-maxillo-facial surgery 69
occlusion together with the front view with lip
retractor provides a valuable tool for planning
orthognathic surgery and the documentation of
complex facial skull deformities.
Submental oblique view
Fig. 3C shows the submental oblique view. As in the
frontal view, the interpupillary line should be ar-
ranged parallel to the horizontal axis, and no rotation
to the occipito-mental axis should occur. The focus
point and the centre of the picture is the junction
between the lip-line and the midline of the columella.
The head is retroclined until an imaginary line joining
both corners of the mouth reaches the level of the
upper edges of the ears. The patient should x a point
on the ceiling. The lower margin is the sterno-
clavicular joint. This view is useful for documentation
and evaluation of enophthalmos or exophthalmos
and the planning of rhinoplasty.
By enlargement, the following close-up views of the
submental oblique view can be achieved: close-up of
the nose in submental oblique view, close-up of the
zygomatic complexes and eyes in the submental
oblique view, close-up of the neck.
Submental vertical view
Fig. 4A shows the submental vertical view. Like in
the submental oblique view, the interpupillary line
should be horizontal and no rotation in the occipito-
mental axis should occur. The focus point and the
centre of the picture is the junction between the lip-
line and the midline of the columella. The head is
retroclined until the nasal tip reaches the edge of the
forehead. The patient should x a point on the ceiling
and must not try to look into the camera. The lower
margin of the display window is the posterior edge of
the ears, and the picture is arranged in landscape
view.
Together with the submental view, this picture
provides an excellent tool for the documentation and
evaluation of enophthalmos or exophthalmos, sym-
metry of the zygomatic complexes, and the planning
of rhinoplasty.
By enlargement, the following close-up views of the
submental vertical view can be achieved: close-up of
the nose in submental vertical view, close up of the
eyes and zygomatic complexes in the submental
vertical view.
Supracranial oblique
Fig. 4B shows the supracranial oblique view. In the
same way as for the submental oblique view the
interpupillary line should be horizontal and no
rotation in an occipito-mental axis should occur.
The focus point and the centre of the photograph is
the junction between the midline of the nose bridge
and the centre of the glabella. Like the submental
vertical view, the picture is arranged in landscape
view. The patient inclines the head backwards until
the nasal tip is aligned with the chin. The forehead
should act as the base of the picture. It is suggested
that this view is for the evaluation of the shape of the
zygoma, although it may also serve as an additional
tool for planning and evaluation of rhinoplasty.
By enlargement, the following close-up view can be
achieved of the submental vertical view: close-up of
the nose in supracranial oblique view.
INTRA-ORAL PICTURES
General notes
The oral cavity is hard to access for accurate clinical
photography. Therefore, several measures have to be
taken to achieve satisfactory results. To obtain a full
view of the dentition or the alveolar ridge, lip
retractors should be used to keep the lips out of
focus. There are different types of lip retractors on
the market, for example one that is single-piece self-
retaining (Lip and Cheek Retractor (SDI), adult size
and child size, Hager & Werken, Duisburg, Ger-
many) or alternatively two separate retractors for
each side (Cheek Retractor Mirahold, adult size and
child size, Hager & Werken, Duisburg, Germany).
The disadvantage of the latter is that an additional
person is needed for positioning. However, the
patient may hold the instruments, although this
may lack precision. To avoid excessive tissue covering
by the retractor itself, the authors advise the usage of
clear lucent self-holding retractors.
Additionally, a black spatula is necessary to
prevent coverage of the front teeth by the lips.
ARTICLE IN PRESS
Fig. 4 (A) Submental vertical view and (B) supracranial oblique.
70 Journal of Cranio-Maxillofacial Surgery
To obtain high-quality intra-oral pictures the use
of mirrors is essential. The authors use mirrors of the
following brands Rocky Mountain, Dent Care,
Brunntal, Germany and Spiegel Dental-Fotograe,
Dent-o-care, Ho henkirchen, Germany.
Sometimes long-handle mirrors can be recom-
mended (Long-handle mirror, Aesculap, Melsungen,
Germany). Although signicantly more expensive,
the use of front-silvered glass mirrors is preferred to
polished metal mirrors because of their superior
optical properties and higher resistance to scratches.
To prevent fogging, the mirrors should be warmed
before use. Cleaning with a surface tension reducer,
such as Neo-Sabenyl
R
(Qualifar), or suction near the
mirror immediately before taking the picture is a
useful alternative.
As mirrors are known to absorb light, accurate
light adaptation is necessary. It is therefore advisable
to adjust local-aperture settings by at least one step.
Due to the small distance between the lens and the
photographed object and high magnication, accu-
rate setting of the focus point and maximal focal
depth are required to prevent bluntness. Aperture
settings of f422 are suitable for intra-oral pictures
and can easily be reached if a ring light ash is used.
Compared to all point ash solutions, a ring light
ash ensures even illumination of all areas of interest.
LED lights might cause a bluish cast, and they should
be used with care.
As auto-focus is not reliable in the oral cavity, we
consider manual focus as the best way to reach
adequate focus point setting. It is important to note
that the depth of eld is distributed about one-third
in front of and two-thirds behind the focal plane.
Therefore, the centre of the picture will not match the
focus point in intra-oral photography. All intra-oral
pictures should be taken in landscape view, and the
image window should be slightly larger than compar-
able facial pictures to allow cropping if needed.
When mirrors are used, they should be positioned
at an angle of 451 to the occlusal plane, as this
provides a 901 view of the area of interest.
Finally, saliva should be carefully aspirated before
taking the pictures.
The following pictures show the intra-oral views.
In a similar way as for the facial photographs, a grid
is inserted, and the circle represents the centre of the
picture. The asterisks indicate the focus point.
INTRA-ORAL PICTURE SET
Front view
To obtain reproducible results, the camera is posi-
tioned parallel to the occlusal plane. The centre of the
picture is the junction between the occlusal plane and
the midline between the rst upper incisors (Fig. 5
centre). The focus point should be set on the cusps of
the canines. If the retractors are placed well, all front
teeth and at least the rst molars should be visible on
the intra-oral front view.
Buccal right and left
The lateral views (Fig. 5 second row) show the upper
and lower jaws with the teeth in full occlusion, and
the picture is extended from the second molar as far
as to the canine of the opposite side.
In order to achieve a complete photograph, it is
recommended to use a narrow mirror in the buccal
corridor combined with a single ended cheek
retractor. The centre of the picture is the cusp of
the upper canine, and the focus point should lay on
the cusps of the rst premolar.
Occlusal upper and lower
In order to obtain symmetrical views of the upper
and lower occlusal surface, it is vital to use intra-oral
mirrors. The camera should be positioned perpendi-
cular to the occlusal plane so that the front teeth are
viewed at their incisal edges. At least the rst molar
should be visible on the picture and ideally all erupted
teeth should be visible. To full these requirements,
maximal mouth opening by the patient is essential.
For the pictures of the lower jaw, the tongue should
be elevated to the hard palate and gently pushed back
out of view with the mirror.
The centre of the picture of the upper jaw is the
junction of a horizontal line between the second
premolars and the middle of the palate (or the
midline between the rst incisors in the lower jaw).
The focus point is on the occlusal surface of the
second premolars in both lower and upper jaws
(Fig. 5 top and bottom).
DISCUSSION
Photographic standards are well dened and dis-
cussed for several medical elds, for example, plastic
surgery and orthodontics (Zarem, 1984; DiBernardo
et al., 1998; Sandler and Murray, 2001), and also
topics including anatomy of the nose and skin lesions
(Galdino et al., 2002; Sullivan, 2002; Ikeda et al., 2003;
McKeown et al., 2005). However, there is no
publication available emphazising the special aspects
of digital photography in cranio-maxillo-facial sur-
gery. This paper demonstrates the important issues of
digital photography, provides assistance in the
selection of suitable software and hardware and
offers dened picture sets for both intra-oral and
facial photographs. It might therefore serve as a
guide for the development of a Europe-wide standard
for digital patient documentation in cranio-maxillo-
facial surgery. Nevertheless, the authors recognize
that there are several previous publications describing
ways to obtain high-quality clinical photographs.
The previously discussed advantages of digital
photography have led to its broad acceptance and
ARTICLE IN PRESS
Standards for digital photography in cranio-maxillo-facial surgery 71
widespread use in clinical documentation. However,
some problems could arise by switching from
analogue to digital photography. If digital pictures
are not accurately tagged with patients personal les
and the database is not maintained regularly, the
search for the required pictures might become
difcult or impossible. One should be aware of the
fact that, for example, the habitual search for slides in
the familiar slide collection by ipping through the
slide panels could become signicantly more difcult
in a database containing thousands of digital photo-
graphs. Moreover, if a complete switch to digital
technology is intended, all analogue les should be
digitized, for example, by scanning, and this can be
very time consuming.
While there is a general agreement about the image
frame and set-up for intra-oral pictures, including the
use of cheek retractors, mirrors and ring light ash
(Zarem, 1984; Bengel, 1985; Sandler and Murray,
2002), a number of alternative set-ups for facial
pictures have been advocated. For example, Mene-
ghini (2001) suggests that high-quality pictures can be
taken with a single ashlight (mono light) in a small
ofce, and Zarem (1984) recommends constant
reproduction ratios by deriving the display window
from anatomical borders. For highly trained and
experienced practitioners this might be an issue, but
this is generally not the case for the novice. The
authors favour a multi-ash-light solution in a
separate room, with constant positions for the
photographer and patient. This guarantees unchan-
ging ambience and is both time saving and reliable.
However, for certain purposes, such as planning of
rhinoplasty and documentation of scars or skin
lesions, the even illumination with little shadowing
might affect the evaluation of the object of interest,
and therefore illumination by spot lights or point
ash, both of which produce harsh shadows, may be
advisable (Galdino et al., 2002; Ikeda et al., 2003).
This approach might also reduce the light reexes on
the patients cornea produced by the soft boxes.
Furthermore, a number of clinical situations might
require different approaches. For example, handi-
capped or immobilized patients will not always be
able to take up every suggested position.
CONCLUSION
The authors consider a clearly arranged picture set
for routine purposes. It consists of three dened facial
views, ve intra-oral views and an additional set of
six facial views for special topics that are sufcient
and helpful in the majority of patients for cranio-
maxillo-facial surgery.
This emphazises the important issues of consis-
tency of illumination, reproduction ratios and patient
positioning for pre- and postoperative pictures to
allow both reproducibility and the possibility of
integration into daily routine.
Many may have observed during presentations a
remarkable correlation between the speakers surgical
competence and the quality of clinical pictures
shown. This should encourage all colleagues to pay
signicant attention to the quality of clinical photo-
graphs, which should ideally be taken personally by
the responsible surgeon.
Addresses for supply of cheek retractors and
mirrors:
Masel Orthodontics, 2701 Bartram Road, Bristol,
PA 19007, UK http://www.maselortho.com/
Ortho Organizers, 58-60 Ashley Road, Hampton,
TW12 2HU, UK http://www.orthoorganizers.co.uk/
Hager & Werken GmbH & Co. KG, AckerstraXe
1, 47269 Duisburg, Germany http://www.hagerwer
ken.de
ARTICLE IN PRESS
Fig. 5 Intraoral views. Asterisk (
*
) indicates focus point: Top: upper occlusal surface, 2nd row (from left): buccal left, frontal, and buccal
right views, Bottom: lower occlusal surface.
72 Journal of Cranio-Maxillofacial Surgery
HAGER Worldwide, Inc., 13322 Byrd Drive,
Odessa, FL 33556, USA www.hagerworldwide.com
ACKNOWLEDGEMENTS
The authors wish to thank Mr. John Carr, Dr. H.
Kerkmann, Mr. H. Meyer and The Department of
Medical Photography at the Royal Bolton Hospital
for the excellent technical support.
References
Becker DG, Tardy Jr ME: Standardized photography in facial
plastic surgery: pearls and pitfalls. Facial Plast Surg 15: 9399,
1999
Bengel W: Standardization in dental photography. Int Dent J 35:
210217, 1985
DiBernardo BE, Adams RL, Krause J, Fiorillo MA, Gheradini G:
Photographic standards in plastic surgery. Plast Reconstr Surg
102: 559568, 1998
Galdino GM, Vogel JE, Vander Kolk CA: Standardizing digital
photography: its not all in the eye of the beholder. Plast
Reconstr Surg 108: 13341344, 2001
Galdino GM, DaSilva AD, Gunter JP: Digital photography for
rhinoplasty. Plast Reconstr Surg 109: 14211434, 2002
Ikeda I, Urushihara K, Ono T: A pitfall in clinical photography:
the appearance of skin lesions depends upon the illumination
device. Arch Dermatol Res 294: 438443, 2003
Jemec BI, Jemec GB: Suggestions for standardized clinical
photography in plastic surgery. J Audiov Media Med 4: 99102,
1981
McKeown HF, Murray AM, Sandler PJ: How to avoid common
errors in clinical photography. J Orthod 32: 4354,
2005
Meneghini F: Clinical facial photography in a small ofce: lighting
equipment and technique. Aesthetic Plast Surg 25: 299306,
2001
Sandler J, Murray A: Digital photography in orthodontics.
J Orthod 28: 197201, 2001
Sandler J, Murray A: Clinical photographsthe gold standard.
J Orthod 29: 158161, 2002
Shaw WC, Semb G, Nelson P, Brattstrom V, Molsted K,
Prahl-Andersen B, Gundlach KKH: The Eurocleft Project
19962000: overview. J Cranio Maxillofac Surg 29: 131140,
2001
Sullivan MJ: Rhinoplasty: planning photo documentation and
imaging. Aesthetic Plast Surg 26: S7, 2002
Zarem HA: Standards of photography. Plast Reconstr Surg 74:
137146, 1984
Prof. Dr. Dr. H.-P. HOWALDT
Klinik und Poliklinik fu r Mund-, Kiefer-
und Gesichtschirurgie - Plastische Operationen
Klinikstrasse 29, D-35385 Giessen, Germany
E-mail: HP.Howaldt@uniklinikum-giessen.de
Accepted 21 November 2005
ARTICLE IN PRESS
Standards for digital photography in cranio-maxillo-facial surgery 73
Você também pode gostar
- The Yellow House: A Memoir (2019 National Book Award Winner)No EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Nota: 4 de 5 estrelas4/5 (98)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeNo EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeNota: 4 de 5 estrelas4/5 (5795)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureNo EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureNota: 4.5 de 5 estrelas4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryNo EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryNota: 3.5 de 5 estrelas3.5/5 (231)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceNo EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceNota: 4 de 5 estrelas4/5 (895)
- Never Split the Difference: Negotiating As If Your Life Depended On ItNo EverandNever Split the Difference: Negotiating As If Your Life Depended On ItNota: 4.5 de 5 estrelas4.5/5 (838)
- The Little Book of Hygge: Danish Secrets to Happy LivingNo EverandThe Little Book of Hygge: Danish Secrets to Happy LivingNota: 3.5 de 5 estrelas3.5/5 (400)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersNo EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersNota: 4.5 de 5 estrelas4.5/5 (345)
- The Unwinding: An Inner History of the New AmericaNo EverandThe Unwinding: An Inner History of the New AmericaNota: 4 de 5 estrelas4/5 (45)
- Team of Rivals: The Political Genius of Abraham LincolnNo EverandTeam of Rivals: The Political Genius of Abraham LincolnNota: 4.5 de 5 estrelas4.5/5 (234)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyNo EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyNota: 3.5 de 5 estrelas3.5/5 (2259)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaNo EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaNota: 4.5 de 5 estrelas4.5/5 (266)
- The Emperor of All Maladies: A Biography of CancerNo EverandThe Emperor of All Maladies: A Biography of CancerNota: 4.5 de 5 estrelas4.5/5 (271)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreNo EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreNota: 4 de 5 estrelas4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)No EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Nota: 4.5 de 5 estrelas4.5/5 (121)
- Photoshop Retouching Cookbook For Digital PhotographerDocumento87 páginasPhotoshop Retouching Cookbook For Digital Photographerchananphorn100% (5)
- Types of Beam-Restricting Devices: 1. Aperture DiaphragmsDocumento5 páginasTypes of Beam-Restricting Devices: 1. Aperture DiaphragmsRachelle Dela Rosa100% (2)
- WhiBalUserGuide V10 PDFDocumento31 páginasWhiBalUserGuide V10 PDFAnonymous Wyb8Y1Ainda não há avaliações
- Nikon F90 PDFDocumento148 páginasNikon F90 PDFEnrico Huarag Guerrero100% (1)
- Night Photography - From Snapshots To Great ShotsDocumento346 páginasNight Photography - From Snapshots To Great ShotsEan VelayoAinda não há avaliações
- Thingiverse - Digital Designs For Physical Objects - Thingiverse 2Documento1 páginaThingiverse - Digital Designs For Physical Objects - Thingiverse 2Nih CalAinda não há avaliações
- ArgonManoukian ZERO IN SRDocumento2 páginasArgonManoukian ZERO IN SRzoranboskovicAinda não há avaliações
- XRS3 - 20V Operators Manual 082017Documento16 páginasXRS3 - 20V Operators Manual 082017PP043Ainda não há avaliações
- Uvp FotodocumentadorDocumento10 páginasUvp Fotodocumentadoradriana_obrAinda não há avaliações
- Fujifilm X-Series Film Recipes - 2022-10-15Documento131 páginasFujifilm X-Series Film Recipes - 2022-10-15hpchavazAinda não há avaliações
- D300s Advanced - Shooting Custom Menu Banks 12-09-8pDocumento8 páginasD300s Advanced - Shooting Custom Menu Banks 12-09-8ptelmopAinda não há avaliações
- GE OEC 9800 Installation ProcedureDocumento37 páginasGE OEC 9800 Installation ProcedureJimena Lopez Cardenas100% (1)
- Beginning Arduino Ov7670 Camera Development - Robert Chin PDFDocumento203 páginasBeginning Arduino Ov7670 Camera Development - Robert Chin PDFedscott66100% (4)
- 15 Tips For Great Candlelight PhotographyDocumento11 páginas15 Tips For Great Candlelight PhotographySuresh BarathanAinda não há avaliações
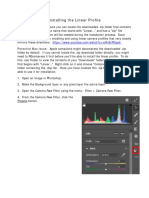
- Installing and Using Linear ProfilesDocumento7 páginasInstalling and Using Linear ProfilesbilbilaAinda não há avaliações
- A Photographers Guide To Ohio (Photography Art Ebook)Documento225 páginasA Photographers Guide To Ohio (Photography Art Ebook)regue100% (1)
- Different Types of LightingDocumento37 páginasDifferent Types of LightingAmbika SivakumarAinda não há avaliações
- 334-500 334 Sensitometer Operation Manual enDocumento30 páginas334-500 334 Sensitometer Operation Manual enKjdfsh DhksjAinda não há avaliações
- Digital CameraDocumento7 páginasDigital CameraMxplatform Mx PlatformAinda não há avaliações
- English Language An Literature: Contemporary PerspectivesDocumento214 páginasEnglish Language An Literature: Contemporary PerspectivesValerijaAinda não há avaliações
- Godox TT350S 20190123Documento13 páginasGodox TT350S 20190123Chris CheungAinda não há avaliações
- Life in The Fast Lane Shoot The Rapids!: Free!Documento132 páginasLife in The Fast Lane Shoot The Rapids!: Free!Ristretto Ardenza100% (1)
- Pentax 6x7 Extension TubesDocumento18 páginasPentax 6x7 Extension TubespeppinhoodAinda não há avaliações
- Reading Passage 3Documento20 páginasReading Passage 3Preet SharmaAinda não há avaliações
- PMAC Fall Progam 2012 - For WebDocumento28 páginasPMAC Fall Progam 2012 - For WebLiana StepanAinda não há avaliações
- Burbank Adult School Spring 2015 Course CatalogDocumento8 páginasBurbank Adult School Spring 2015 Course CatalogburbankadultschoolAinda não há avaliações
- IEC TestDocumento31 páginasIEC Testwazi nisa100% (1)
- Canon IXUS 132 Specification Sheet PDFDocumento3 páginasCanon IXUS 132 Specification Sheet PDFmoscone78Ainda não há avaliações
- Astronomy Lab ReportDocumento6 páginasAstronomy Lab ReportAbhishek PanchalAinda não há avaliações
- plx101 PDFDocumento2 páginasplx101 PDFTulus ArisonoAinda não há avaliações