Escolar Documentos
Profissional Documentos
Cultura Documentos
Nasal Fractures
Enviado por
amitdineshp0 notas0% acharam este documento útil (0 voto)
89 visualizações3 páginasPetersen's nasal fracture
Título original
24. Nasal Fractures
Direitos autorais
© © All Rights Reserved
Formatos disponíveis
DOCX, PDF, TXT ou leia online no Scribd
Compartilhar este documento
Compartilhar ou incorporar documento
Você considera este documento útil?
Este conteúdo é inapropriado?
Denunciar este documentoPetersen's nasal fracture
Direitos autorais:
© All Rights Reserved
Formatos disponíveis
Baixe no formato DOCX, PDF, TXT ou leia online no Scribd
0 notas0% acharam este documento útil (0 voto)
89 visualizações3 páginasNasal Fractures
Enviado por
amitdineshpPetersen's nasal fracture
Direitos autorais:
© All Rights Reserved
Formatos disponíveis
Baixe no formato DOCX, PDF, TXT ou leia online no Scribd
Você está na página 1de 3
Amit Patel OMFS PGY 1
Chapter 24: Nasal Fractures
Most frequently fractured bones of the face.
Less force required to fracture this area than any other facial bone.
Seemingly simple approach to management
Incident of unfavorable results are as high as 62%.
Etiology factors
Motor vehicle collision
interpersonal altercations
Sport-related injury
A. Surgical Anatomy
Nasal mucosa and turbinates
Upper and lower cartilages
Cartilaginous and bony septum in middle
Primary support mechanism of nasal complex
Anterior: cartilage (thicker posteriorly)
Posterior: ethmoid and vomer bones
Paired nasal bones
Cephalically: Nasofrontal suture
Caudally: Upper lateral cartilages
Laterally: Frontal processes of maxilla
Vascular supply
Arteries
Interna carotid branches
Ophthalmic >>> Anterior and posterior Ethmoid arteries
External Carotid branches
Superior labial, angular, sphenopalatine, and greater palatine arteries.
External nose: Facial artery > angular artery
Veins follow arterial pattern. Significant for direct communication with cavernous sinus and lack of
valves.
Innervation
Second division (Maxillary) of the Trigeminal nerve
B. Clinical and Radiographic Diagnostic Tools
Address life threatening and major organ injuries first
Obtain complete history
Mechanism and timing of injury
Force perpendicular to nasal dorsum >>> bony complex fractured laterally
Force lateral to nose (Right handed punch to left side of nose) >>> bony complex will deviate
away from vector of force with one nasal bone medially displaced and other laterally displaced.
Previous nasal trauma or preexisting nasal deviations
Examination
Epistaxis common
Clinical signs of nasal complex fracture
Amit Patel OMFS PGY 1
Periorbital ecchymosis
Nasal swelling
Nasal complex deviation
CSF rhinorrhea
Lack of Nasal projection
Increased intercanthal distance
Mobility or crepitus upon palpation
Anosmia (difficulty smelling) - Late finding occurs if cribriform plate of ethmoid bone is involved
Internal exam with good lighting, speculum and suction
Intranasal laceration
Septal deviation off the nasal crest of maxilla
Nasal septal hematoma
Must be drained to prevent vascular complications associated with devitalized cartilage pre-
disposing to the development of septal perforation.
If cribriform plate of ethmoid bone is fractured >>> perform double-halo test to ascertain presence
of CSF.
Imaging: CT scan without contrast
Clearly delineates nasal bone injuries and septal deviations and fractures
Premorbid photographs are helpful for documentation and comparison purposes.
Classifications
Open vs Closed
Fracture through an external or internal laceration
Deviated vs Non-deviated
Appearance of nasal bones and septum
Comminuted vs Non-comminuted
Status of nasal bones and surrounding bony pyramid (frontal process of maxilla anterior nasal
spine, ethmoidal bones)
C. Surgical Management
Goals
Prevent development of post-traumatic nasal deformity
Restoration of proper nasal air flow
Prevention of cosmetic deformity
Maintenance of proper nasal complex topography and projection
Restoration of sense of smell.
Treatment can be performed under local anesthesia , conscious sedation or general anesthesia
Most efficient and comfortable method: Repair under general endotracheal intubation
Close reduction of nasal complex is most commonly performed procedure
Incidence of patient requiring post-traumatic rhinoplasty >>> 9% - 62%
Procedure:
Intubation
Thorough manual examination of nasal complex
Assess and note crepitus, mobility, depressions, asymmetries, perinasal lacerations, etc
Intranasal exam
Via Endoscopy or nasal speculum and good lighting
Inject local anesthesia and vasoconstrictor into nasal cavity
Amit Patel OMFS PGY 1
Pack nasal cavity with Cottonoid strips soaked in vasoconstrictive solution >>> improves intranasal
visualization
Examination of cavity after 10-15 minutes
Used nasal reduction forceps to reduce nasal ones and septum fractures in appropriate vector
Intranasal packing/splint to maintain reduction
If not successful >>> Perform extensive procedures such as septoplasty (with or without harvest of
cartilage) or bony osteotomies.
Septoplasty
Approached through hemitransfixion incision
Maintain all septal cartilage at initial repair
May be of use in post-traumatic nasal deformity repair
If nasal septum deviates off of ANS, subperichondrial and subperiosteal dissections must be per-
formed in ANS region >>> manually separate septum from ANS >>> reattach septum to ANS using
sutures.
Bony vault deviation not repaired with close reduction may require open reduction or osteotomies.
Callus forms after 10-14 days
Transoral approach to nasomaxillary buttresses, frontal processes of maxilla and nasal bones may
facilitate Open reduction with or without internal fixation
Approaching bones through perinasal lacerations is also acceptable
Use intranasal packing/splint to maintain mobilized bony segments in place5 days
Use external splint: aid in elimination of dead space and maintenance of reduction 7 days
D. Postoperative care and complications
Recommend prolonged antibiotics when internal nasal packings used.
Recommend sinus precautions
Incidence for residual nasal deformity after close reduction: up to 62%
Follow patients progress to ensure acceptable functional and cosmetic outcome
Wait up to 1 year before addressing residual post-traumatic deformity
Grossly deviated nose 1 months s/p repair will remain grossly deviated 1 yr s/p repair.
Post-traumatic rhinoplasty is recommended earlier in such cases.
Você também pode gostar
- Nbde Boards Radiology 14Documento14 páginasNbde Boards Radiology 14amitdineshp100% (6)
- NBDE Dental Boards Ortho 25Documento25 páginasNBDE Dental Boards Ortho 25amitdineshp100% (8)
- NBDE Dental Boards Pedo 21Documento21 páginasNBDE Dental Boards Pedo 21amitdineshp78% (9)
- NBDE Dental Boards Oral Surgery-27Documento27 páginasNBDE Dental Boards Oral Surgery-27amitdineshp100% (11)
- NBDE Dental Boards Operative Dentistry-33Documento33 páginasNBDE Dental Boards Operative Dentistry-33amitdineshp91% (11)
- Mosby Dental Boards Endo 26Documento26 páginasMosby Dental Boards Endo 26amitdineshp100% (7)
- The Yellow House: A Memoir (2019 National Book Award Winner)No EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Nota: 4 de 5 estrelas4/5 (98)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeNo EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeNota: 4 de 5 estrelas4/5 (5795)
- Never Split the Difference: Negotiating As If Your Life Depended On ItNo EverandNever Split the Difference: Negotiating As If Your Life Depended On ItNota: 4.5 de 5 estrelas4.5/5 (838)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceNo EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceNota: 4 de 5 estrelas4/5 (895)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersNo EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersNota: 4.5 de 5 estrelas4.5/5 (345)
- The Little Book of Hygge: Danish Secrets to Happy LivingNo EverandThe Little Book of Hygge: Danish Secrets to Happy LivingNota: 3.5 de 5 estrelas3.5/5 (400)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureNo EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureNota: 4.5 de 5 estrelas4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryNo EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryNota: 3.5 de 5 estrelas3.5/5 (231)
- The Emperor of All Maladies: A Biography of CancerNo EverandThe Emperor of All Maladies: A Biography of CancerNota: 4.5 de 5 estrelas4.5/5 (271)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaNo EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaNota: 4.5 de 5 estrelas4.5/5 (266)
- The Unwinding: An Inner History of the New AmericaNo EverandThe Unwinding: An Inner History of the New AmericaNota: 4 de 5 estrelas4/5 (45)
- Team of Rivals: The Political Genius of Abraham LincolnNo EverandTeam of Rivals: The Political Genius of Abraham LincolnNota: 4.5 de 5 estrelas4.5/5 (234)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyNo EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyNota: 3.5 de 5 estrelas3.5/5 (2259)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreNo EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreNota: 4 de 5 estrelas4/5 (1091)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)No EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Nota: 4.5 de 5 estrelas4.5/5 (121)
- The Effect of The Methanol Extract of Haloxylon Salicornicum (Moq.) Bunge Ex Bioss. On Alleviating in AmmationsDocumento8 páginasThe Effect of The Methanol Extract of Haloxylon Salicornicum (Moq.) Bunge Ex Bioss. On Alleviating in AmmationszzakieAinda não há avaliações
- Drug StudyDocumento21 páginasDrug StudyShyla Garnace JavillonarAinda não há avaliações
- Fcps IMMDocumento22 páginasFcps IMMHaseeb Rasool0% (1)
- Fall RiskDocumento2 páginasFall Riskd_anto781063Ainda não há avaliações
- Treatment For ESRDDocumento9 páginasTreatment For ESRDpunpen ngorsakun100% (1)
- Fundus Examination PDFDocumento125 páginasFundus Examination PDFAravind Kumar100% (5)
- Urinary System Text BookDocumento24 páginasUrinary System Text Bookapi-209542414Ainda não há avaliações
- VoacangaDocumento12 páginasVoacangaLarry Selorm Amekuse100% (1)
- V 11.0 Breakpoint TablesDocumento116 páginasV 11.0 Breakpoint TablesRuth RachitaAinda não há avaliações
- Journal On Threpetical Study On MutraDocumento6 páginasJournal On Threpetical Study On MutraVijay DawarAinda não há avaliações
- PneumoconiosisDocumento19 páginasPneumoconiosisgabriela.was.gabbbieAinda não há avaliações
- Housekeeping Check Lists-UpdatedDocumento26 páginasHousekeeping Check Lists-UpdatedtanishaAinda não há avaliações
- Mental or Intellectual ChangesDocumento18 páginasMental or Intellectual ChangesJonh Edwel Alloc50% (2)
- Gastrointestinal DrugsDocumento27 páginasGastrointestinal DrugsKer YehunAinda não há avaliações
- Cues Nursing Diagnosis Goal Nursing Interventions Rationale EvaluationDocumento3 páginasCues Nursing Diagnosis Goal Nursing Interventions Rationale EvaluationVher SisonAinda não há avaliações
- Clinical Case Scenarios PDF Version PDF 181726381 PDFDocumento85 páginasClinical Case Scenarios PDF Version PDF 181726381 PDFStarr NewmanAinda não há avaliações
- Copia Di Drugs That Cause or Prolong Delirium - UpToDateDocumento2 páginasCopia Di Drugs That Cause or Prolong Delirium - UpToDateAFA.BLSAinda não há avaliações
- Effect of Tooth Type and Ferrule On The Survival of Pulpless Teeth Restored With Fiber Posts - A 3-Year Clinical Study PDFDocumento6 páginasEffect of Tooth Type and Ferrule On The Survival of Pulpless Teeth Restored With Fiber Posts - A 3-Year Clinical Study PDFDan MPAinda não há avaliações
- Niosome Final...Documento9 páginasNiosome Final...Ajma LineAinda não há avaliações
- Stock Count 01ST July 2021Documento4 páginasStock Count 01ST July 2021Williams Lucky ElvisAinda não há avaliações
- Astro Case StudyDocumento3 páginasAstro Case StudyAstrodita Adya SetaAinda não há avaliações
- The Client With Chronic Renal FailureDocumento4 páginasThe Client With Chronic Renal FailureMarisol Jane JomayaAinda não há avaliações
- Schizoid ProcessDocumento17 páginasSchizoid Processdigidevil100% (1)
- Msds F34avturfsiiDocumento10 páginasMsds F34avturfsiiAyat TullahAinda não há avaliações
- JBDS 02 Nursing Management For DKA v1 20122022Documento10 páginasJBDS 02 Nursing Management For DKA v1 20122022olazbt2000Ainda não há avaliações
- Dialysis Technician ExamsDocumento1 páginaDialysis Technician ExamstapanidepuAinda não há avaliações
- BaidyanathDocumento5 páginasBaidyanathRishikesh KumarAinda não há avaliações
- Waukboard Sellsheet v13Documento1 páginaWaukboard Sellsheet v13Forum PompieriiAinda não há avaliações
- Movement Disorders - 2022 - Deuschl - European Academy of Neurology Movement Disorder Society European Section Guideline OnDocumento15 páginasMovement Disorders - 2022 - Deuschl - European Academy of Neurology Movement Disorder Society European Section Guideline OnAnali Durán CorderoAinda não há avaliações
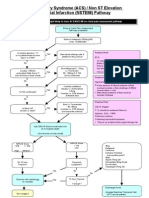
- ACS NSTEMI Clinical PathwayDocumento3 páginasACS NSTEMI Clinical PathwayXtiaRAinda não há avaliações