Escolar Documentos
Profissional Documentos
Cultura Documentos
Clinical Pearls in General Internal Medicine 2012 (Mayo Clinic)
Enviado por
Pkern0 notas0% acharam este documento útil (0 voto)
266 visualizações7 páginasClinical Pearls in General Internal Medicine 2012 (Mayo Clinic)
Direitos autorais
© © All Rights Reserved
Formatos disponíveis
PDF, TXT ou leia online no Scribd
Compartilhar este documento
Compartilhar ou incorporar documento
Você considera este documento útil?
Este conteúdo é inapropriado?
Denunciar este documentoClinical Pearls in General Internal Medicine 2012 (Mayo Clinic)
Direitos autorais:
© All Rights Reserved
Formatos disponíveis
Baixe no formato PDF, TXT ou leia online no Scribd
0 notas0% acharam este documento útil (0 voto)
266 visualizações7 páginasClinical Pearls in General Internal Medicine 2012 (Mayo Clinic)
Enviado por
PkernClinical Pearls in General Internal Medicine 2012 (Mayo Clinic)
Direitos autorais:
© All Rights Reserved
Formatos disponíveis
Baixe no formato PDF, TXT ou leia online no Scribd
Você está na página 1de 7
Clinical Pearls in General Internal Medicine 2012
John B. Bundrick, MD, and Scott C. Litin, MD
A
t the 2001 Annual Conference of the
American College of Physicians,
a new teaching format to aid physi-
cian learning, Clinical Pearls, was introduced.
Clinical Pearls is designed with the 3 qualities
of physician-learners in mind. First, we physi-
cians enjoy learning from cases. Second, we
like concise, practical points that we can use
in our practice. Finally, we take pleasure in
problem solving.
In the Clinical Pearls format, speakers pres-
ent a number of short cases in their specialty to
a general internal medicine audience. Each case
is followed by a multiple-choice question an-
swered live by attendees using an audience
response system. The answer distribution is
shown to attendees. The correct answer is then
displayed and the speaker discusses teaching
points, clarifying why one answer is most appro-
priate. Each case presentation ends with a Clin-
ical Pearl, dened as a practical teaching point
that is supported by the literature but generally
not well-known to most internists.
Clinical Pearls is currently one of the most
popular sessions at the American College of
Physicians meeting. As a service to its readers,
Mayo Clinic Proceedings has invited a selected
number of these Clinical Pearl presentations
to be published in our Concise Reviews for
Clinicians section. The following Clinical
Pearls in General Internal Medicine 2012 is
one of them.
CASE 1
A 32-year-old woman presents to your ofce
with 2 days duration of rhinorrhea, nasal
congestion, and a slight dry cough. She denies
any fever, headache, or sore throat and has
otherwise been well. She is not taking any
medications. She works as a nurse in an
outpatient internal medicine clinic, and her
symptoms have been a considerable nuisance
as she interacts with her patients. On examina-
tion, she appears generally well and is afebrile.
She has moderate nasal edema and pale yellow
mucus in both nasal passages. The pharynx
appears normal, and there is no tenderness
over the maxillary sinuses. There is no lymph-
adenopathy. Her lungs are clear.
Question
Which one of the following intranasal
topical therapy combinations would
provide the most effective relief of
her symptoms in the next 7 days?
a. Zinc and oxymetazoline
b. Ipratropium and oxymetazoline
c. Ipratropium and zinc
d. Fluticasone and oxymetazoline
e. Fluticasone and ipratropium
Discussion
The common cold is a viral upper respiratory
tract infection (URTI) for which there is no
known cure, although the nasal symptoms
may be substantially alleviated by topical thera-
pies. The use of nasal ipratropium was assessed
in a recent Cochrane Review that involved 7
randomized controlled trials of 2144 patients
with acute viral URTI.
1
In a representative study
of 943 patients, rhinorrhea scores decreased
from a baseline of 6.5 (on a 1-10 scale) to 3.4
with treatment. In another trial of 410 patients,
global improvement on day 5 was rated 81%
with nasal ipratropium treatment compared
with 65% in the placebo group and only 18%
in a group that received no treatment. Adverse
effects included primarily mild epistaxis and
nasal dryness, both of which were judged toler-
able by the study participants. The dose of ipra-
tropiumusedinmost studies was 2sprays of the
0.06%solutionineachnostril 4 times daily. The
Cochrane reviewers concluded: For people
with the common cold, the existing evidence,
which has some limitations, suggests that ipra-
tropium bromide is likely to be effective in
ameliorating rhinorrhoea.
1
Nasal congestion was not affected by ipra-
tropium treatment and can also be quite
annoying for patients with URTI. A review of
trials of intranasal xylometazoline (which is
equivalent to oxymetazoline) for the common
cold demonstrated a 34%reduction in symptom
scores for nasal congestion (alone and combined
See end of article for
correct answers to
questions.
From the Division of General
Internal Medicine, Mayo
Clinic, Rochester, MN.
106
Mayo Clin Proc. n January 2013;88(1):106-112 n http://dx.doi.org/10.1016/j.mayocp.2012.11.003
www.mayoclinicproceedings.org n 2013 Mayo Foundation for Medical Education and Research
CONCISE REVIEW FOR CLINICIANS
withnasal ipratropium) comparedwithplacebo.
2
Mild epistaxis was the only adverse effect. Treat-
ment was used for up to 10 days, and there was
no evidence of rhinitis medicamentosa in these
trials (although it would be wise to avoid nasal
decongestant use in patients with a history of
rhinitis medicamentosa).
Trials of intranasal uticasone in the
common cold show a lack of benet. Whereas
oral zinc use has been found to modestly
decrease the duration and severity of common
cold symptoms,
3
intranasal zinc use has no
efcacy (and may lead to permanent anosmia).
Clinical Pearl
Intranasal ipratropium and oxymetazoline
treatment reduces the symptoms of rhinorrhea
and nasal congestion (respectively) in the
common cold.
CASE 2
A 72-year-old woman presents with 4 months
duration of right upper quadrant anterior
abdominal pain. The pain is described as
a deep burning ache that is continuous for
most of the day and is worse as the day pro-
gresses. It is better with lying down and
bothers her only at night if she lies on either
side. It is unaffected by meals. She has no
history of trauma and has not had a rash.
She has no back pain. Her medical history is
remarkable for a remote cholecystectomy and
a diagnosis of osteoporosis. Her medications
include alendronate, 70 mg by mouth once
weekly; vitamin D, 1000 U daily; and a calcium
supplement, 600 mg twice daily. Her exami-
nation reveals moderate kyphosis and tender-
ness in the right lateral abdomen. There is
no mass or organomegaly and no rash.
Question
Which one of the following would be most
likely to yield the diagnosis?
a. Check for the Murphy sign
b. Perform the Carnett maneuver
c. Measure the rib-pelvis distance
d. Thoracic spine lms
e. Computed tomography of the abdomen
Discussion
In patients with osteoporosis, the cumula-
tive effects of vertebral compression fractures
(which are frequently occult) often lead to a nar-
rowing of the distance between the lowest ante-
rior rib (the 10th rib, at its most inferior point,
which is generally the midaxillary line) and the
top of the iliac crest. This narrowing can be
easily measured by ngerbreadths on examina-
tion with the patient in the seated or standing
position. Even in asymptomatic patients, this
measurement may be a helpful diagnostic clue
to the presence of subclinical compression frac-
tures. A distance of 2 ngerbreadths or less
progressively increases the odds of such frac-
tures, and at 4 ngerbreadths they would be
virtually excluded (negative likelihood ratio of
0.1).
4,5
In this case, measurement of the rib-
pelvis distance would provide a further clue
to the mechanism of her abdominal pain. If
the distance were 1 ngerbreadth or less,
and the tenderness could be localized to
the tip of the 10th rib (which is the lowest
anterior rib), then a clinical diagnosis of ilio-
costal syndrome (aka ribs on pelvis
syndrome) may be condently established.
6
Treatment is aimed at postural training (to
avoid contact of the rib with the pelvis)
and other physical therapy modalities. If
these are not effective, then a local injection
of anesthetic and corticosteroid may some-
times be of benet. In all cases, reassurance
as to the benign nature of the diagnosis and
avoidance of further testing is helpful. A
similar syndrome of back and ank pain
may develop in these patients in which the
tip of the 12th rib contacts the top of the
pelvis posteriorly.
7
The Carnett maneuver is a test for abdom-
inal wall pain that involves tensing the abdom-
inal muscles while palpating a tender spot to
see whether the pain increases (which localizes
the pain to the abdominal wall and helps
exclude intra-abdominal causes). Although
generally a useful maneuver, in this case the
pain is farther lateral than in most cases of
abdominal wall pain and the context is
weighted more toward a rib-tip mechanism
of pain. Thoracic spine lms would simply
conrm her kyphosis but would be unlikely
to provide further insight into the cause of
her abdominal pain. Findings on computed
tomography of the abdomen would be ex-
pected to be normal in iliocostal syndrome
and would be unnecessary in this case.
CLINICAL PEARLS IN GENERAL INTERNAL MEDICINE 2012
Mayo Clin Proc. n January 2013;88(1):106-112 n http://dx.doi.org/10.1016/j.mayocp.2012.11.003
www.mayoclinicproceedings.org
107
Clinical Pearl
Patients with osteoporosis may develop
chronic pain over the tip of the 10th rib where
it contacts the pelvis, and this may be strongly
suspected based on features of the clinical
examination.
CASE 3
A 69-year-old man reports a history of nocturia
that has become progressively more bother-
some to him during the past couple of years.
He now gets up 3 times at night to void and
has trouble getting back to sleep each time.
His daytime voiding pattern is normal (about
4 times during the day), and he has no hesi-
tancy, decreased force of stream, urgency, or
sensation of incomplete voiding. His wife has
mentioned that he has snored loudly for many
years, but she has not noticed any apnea. He
has gained approximately 10 lb during the
past year, but his fasting glucose level was
recently only 92 mg/dL (to convert to mmol/L,
multiply by 0.0555). His only medication is
lisinopril, 10 mg/d, for hypertension. His
body mass index is 34 (calculated as weight
in kilograms divided by height in meters
squared), and his blood pressure is 136/76
mm Hg. Heart and lungs are normal. There
is trace pitting edema at the ankles. His pros-
tate is mildly enlarged (1). Laboratory tests
revealed normal serum sodium, potassium,
creatinine, and calcium levels.
Question
Which one of the following diagnoses
best explains his nocturia?
a. Obstructive sleep apnea (OSA)
b. Remobilization of peripheral edema
c. Benign prostatic hypertrophy (BPH)
d. Detrusor instability
e. Supercial bladder cancer
Discussion
Nocturia is a common symptom in older indi-
viduals (especially men) and may be associated
with sleep disruption, poor quality of life, and
falls at night. It generally arises in relation to
reduced bladder capacity, increased nocturnal
urine volume, or some combination of the
two. Bladder causes include BPH, detrusor
instability, and (less often) infection or tumor.
Nocturnal urine volume in healthy individuals
is much less than daytime output owing to
decreased meal-related solute at night and
a natural increase in vasopressin (antidiuretic
hormone). This circadian increase in nocturnal
antidiuretic hormone is blunted in elderly indi-
viduals and is one of many factors predisposing
them to nocturia. Specic diseases may also
increase nocturnal urine volume, including dia-
betes mellitus, congestive heart failure, renal
disease, and hypercalcemia.
8
More recently, OSA has been strongly
linked to nocturia, which may occur in as
many as 50% of patients with OSA.
9
Levels of
atrial natriuretic factor (ANF) have been docu-
mented to be signicantly elevated in patients
with OSA, and this is thought to be the mech-
anism of the nocturia. The elevated ANF level is
most likely from right atrial stretch related to
either the negative intrathoracic pressure
directly, hypoxia-induced pulmonary vasocon-
striction, or some combination of the two.
Continuous positive airway pressure (CPAP)
therapy has been shown to improve nocturia
in concert with reducing the levels of ANF.
One representative trial of CPAP treatment
resulted in nocturia decreasing from a mean
of 2.5 times per night to 0.7 times per night.
More than 70% of the patients reported good
to excellent relief of their nocturia with CPAP
treatment in that study.
10
Remobilization of edema on assuming the
recumbent position at night is certainly
a common cause of nocturia as well, but the
present patient (even when examined toward
the end of the day) does not have sufcient
edema for that to be the cause. He has no
daytime symptoms to suggest BPH, detrusor
instability, or bladder neoplasm.
Clinical Pearl
Nocturia is a common symptom in OSA and is
substantially improved after initiation of CPAP
therapy.
CASE 4
A 62-year-old woman is bothered by a sensa-
tion of dry eyes. This is more noticeable toward
the end of the day and interferes at times with
her ability to work on her computer. She has
no dry mouth and is otherwise healthy. On
examination, she has perhaps a slight decrease
in tear production, but the eyes otherwise
appear normal.
MAYO CLINIC PROCEEDINGS
108
Mayo Clin Proc. n January 2013;88(1):106-112 n http://dx.doi.org/10.1016/j.mayocp.2012.11.003
www.mayoclinicproceedings.org
Question
In addition to the use of articial tears,
which one of the following is most likely
to help her symptoms?
a. Evening primrose oil
b. Vitamin E
c. Vitamin D
d. Horse chestnut extract
e. Fish oil
Discussion
Dry eyes are a common symptom and occur in
up to 30% of those older than 50 years.
11
Mechanisms include decreased tear production
and increased evaporative loss (often related to
changes in the complex lipid composition of
the outer layer of the tear lm). Several medica-
tions have been implicated, including estrogens,
antihistamines, anticholinergics, and selective
serotonin reuptake inhibitors. The symptoms
can be quite distracting in some cases and
can have a major effect on visual acuity, social
functioning, and workplace productivity. Most
cases will not be related to Sjgren syndrome
or other systemic diseases and may be treated
symptomatically.
The rst line of treatment in all cases is the
use of articial tears. In addition, sh oil may
be benecial. Several studies have established
an association between decreased dietary
intake of omega-3 fatty acids and dry eye
syndrome.
12-14
The mechanism is not entirely
clear but is thought to relate to effects on meibo-
mian gland oils. A recent small, randomized,
double-blind trial of patients with mild to
moderate dry eye syndrome used a daily dose
of sh oil that contained 450 mg of eicosapen-
taenoic acid, 300 mg of docosahexaenoic acid,
and 1000 mg of axseed oil. After 90 days, those
in the treatment group had a notable increase in
tear volume compared with the placebo group.
Furthermore, 70% of the treated group had
become asymptomatic compared with only
37% of those who took placebo.
15
Clinical Pearl
Fish oil seems to be benecial in treating the
symptoms of dry eye syndrome.
CASE 5
Three months ago, a 64-year-old male ac-
countant experienced an episode of left arm
weakness lasting 15 minutes that was diag-
nosed as a transient ischemic attack (TIA).
He was found to be in atrial brillation at
that time. Findings on carotid ultrasonography
were normal, and his echocardiogram showed
normal left ventricular function and no
valvular disease. He has no cardiac symptoms
and no additional remarkable medical history
apart from hypertension. He takes lisinopril,
10 mg/d, and warfarin, 5 mg/d. His interna-
tional normalized ratio has been consistently
in the 2 to 3 range on his current dose of
warfarin. His examination ndings are normal
except for an irregular heart rhythm at a rate of
84 beats/min. His blood pressure is 130/82
mm Hg. His father died of intracranial
bleeding while taking warfarin, and the patient
worries that he may be at risk for the same
outcome. He has also been troubled by
epistaxis and easy bruising and wonders just
how important it is for him to continue taking
anticoagulants.
Question
If the patient were to stop taking warfarin,
what would be his risk of a stroke within
the next year?
a. 4%
b. 6%
c. 7.5%
d. 12%
e. 18%
Discussion
The CHADS
2
score is a well-validated method
of estimating the risk of stroke in patients with
atrial brillation
16,17
and is enormously help-
ful in making decisions as to who should be
undergoing long-term anticoagulation. It is
also easy to use and remember, as patients
are assigned 1 point each for congestive heart
failure, hypertension, age 75 years and older,
and diabetes mellitus and 2 points for stroke
or TIA. However, there are currently 2 com-
monly used versions of the CHADS
2
score,
each derived from different populations with
considerable interstudy variation in risk of
stroke. This is illustrated in Table 1, which
shows rates of stroke in patients with atrial
brillation not undergoing anticoagulation
from the 2 studies.
CLINICAL PEARLS IN GENERAL INTERNAL MEDICINE 2012
Mayo Clin Proc. n January 2013;88(1):106-112 n http://dx.doi.org/10.1016/j.mayocp.2012.11.003
www.mayoclinicproceedings.org
109
The lower-risk cohort involved ambulatory
patients with a mean age of 71 years,
17
and the
original study (the higher-risk cohort) validating
the index involved Medicare patients with
a mean age of 81 years who had been hospital-
ized in the past year.
18
Although either index
may be used in the appropriate setting, the
higher-risk cohort is likely better matched to
a substantial proportion of the frail elderly
patients seen by many physicians.
The CHA
2
DS
2
-VASc score adds another
layer of precision by giving 1 point for age
65 to 74 years (and an additional point for
age 75 years) and adding 1 point for
vascular disease and female sex. This predic-
tion rule has particular utility in identifying
patients who are truly at low risk for stroke
and for whom warfarin therapy may be safely
withheld.
18,19
For patients with a history of stroke or
TIA, all of these models may underestimate
the risk of recurrent stroke. The patient in
this case has a CHADS
2
and a CHA
2
DS
2
-
VASc score of 3 (2 points for TIA and 1 point
for hypertension) and would thus be esti-
mated to have an annual stroke risk of
approximately 5% to 6%. However, data
from the placebo arm of the European Atrial
Fibrillation Trial (a randomized trial of
warfarin for secondary prevention after TIA
or minor stroke) indicate that his actual stroke
risk is closer to 12% per year.
20
In that study,
the patients were randomized within 3
months after a TIA or stroke, but the curves
for this increased risk in the placebo arm did
not signicantly atten through up to 3 years
of follow-up.
Clinical Pearl
The CHADS
2
and CHA
2
DS
2
-VASc scores
provide an accurate estimation of stroke risk
in patients with atrial brillation but consider-
ably underestimate the risk in those who have
experienced a TIA or stroke.
CASE 6
A 67-year-old woman undergoes osteoporosis
screening using dual-energy x-ray absorpti-
ometry (DXA) and is found to have osteo-
penia. Her T scores at the femur neck and
total hip are both 1.6. She receives appro-
priate vitamin D and calcium therapy and
has no other osteoporosis risk factors. She
took estrogen for 4 years after menopause at
age 50 years.
TABLE 1. Rates of Stroke in Patients With Atrial Fibrillation Not Undergoing Anticoagulation
CHADS
2
or
CHA
2
DS
2
-VASc score
Annual stroke risk
Annual thromboembolism risk
in the CHA
2
DS
2
-VASc cohort Lower-risk cohort Higher-risk cohort
0 0.49 1.9 0.8
1 1.52 2.8 2.0
2 2.50 4.0 3.7
3 5.27 5.9 5.9
4 6.02 8.5 9.3
5 6.88 (5 or 6 combined) 12.5 15.3
6 6.88 (5 or 6 combined) 18.2 19.7
7 NA NA 21.5
8 NA NA 22.4
9 NA NA 23.6
NA not applicable.
TABLE 2. Time Required for 10% of Women to Transition to a BMD of
Osteoporosis
Baseline
osteopenia level
T score
Interval to reach a BMD
of osteoporosis (y)
Normal 1.00 or better 17.4
Mild 1.01 to e1.49 16.5
Moderate 1.50 to e1.99 4.6
Advanced 2.00 to e2.49 1.0
BMD bone mineral density.
MAYO CLINIC PROCEEDINGS
110
Mayo Clin Proc. n January 2013;88(1):106-112 n http://dx.doi.org/10.1016/j.mayocp.2012.11.003
www.mayoclinicproceedings.org
Question
What is the most appropriate interval to
wait before retesting her bone density?
a. 1 year
b. 2 years
c. 3 years
d. 5 years
e. 10 years
Discussion
Current osteoporosis screening guidelines
advise bone mineral density (BMD) screening
for osteoporosis in women 65 years and older.
However, evidence-based guidance has been
lacking as to the optimal screening interval
for repeating this testing based on the initial
BMD result. This question has now been
addressed by data from a cohort of women
from the Study of Osteoporotic Fractures.
Five thousand women 67 years and older
without osteoporosis on their initial DXA
screening were followed prospectively for up
to 15 years. The DXA screening was repeated
in years 2, 6, 8, 10, and 16. The outcome of
interest was the time required for 10% of
women to transition to a BMD of osteoporosis
(T score e2.5) before incident hip/clinical
vertebral fracture or before receiving treatment
for osteoporosis. Patients were classied
according to their baseline BMD, and the
time required to reach this primary outcome
was found to vary considerably (Table 2).
Age was a factor in determining the
testing intervals. For example, although the
overall testing interval was approximately
5 years for those with moderate osteopenia,
for women 85 years and older it was closer
to 3 years.
21
Although these data provide
useful information to physicians regarding
when to retest with DXA, it is important to
remember that BMD is only one factor in
determining risk of fracture. Treatment and
testing decisions should ultimately be based
on overall risk assessment (eg, Fracture Risk
Assessment score). Women at higher risk
(eg, corticosteroid users) need more frequent
testing.
Clinical Pearl
In most women who are at average risk for
osteoporosis, the decision of when to retest
the BMD may be based on the initial BMD
result. Longer intervals may be appropriate
for many of these women.
Abbreviations and Acronyms: ANF = atrial natriuretic
factor; BMD = bone mineral density; BPH = benign prostatic
hypertrophy; CPAP = continuous positive airway pressure;
DXA = dual-energy x-ray absorptiometry; OSA = obstruc-
tive sleep apnea; TIA = transient ischemic attack; URTI =
upper respiratory tract infection
Correspondence: Address to John B. Bundrick, MD,
Division of General Internal Medicine, Mayo Clinic, 200 First
St SW, Rochester, MN 55905 (bundrick.john@mayo.edu).
REFERENCES
1. Albalawi ZH, Othman SS, Alfaleh K. Intranasal ipratropium
bromide for the common cold. Cochrane Database Syst Rev.
2011;(7):CD008231.
2. Eccles R, Martensson K, Chen SC. Effects of intranasal xylometa-
zoline, alone or in combination with ipratropium, in patients with
common cold. Curr Med Res Opin. 2010;26(4):889-899.
3. Singh M, Das RR. Zinc for the common cold. Cochrane Data-
base Syst Rev. 2011;(2):CD001364.
4. Siminoski K, Warshawski RS, Jen H, Lee KC. Accuracy of
physical examination using the rib-pelvis distance for detection
of lumbar vertebral fractures. Am J Med. 2003;115(3):233-236.
5. Green AD, Colon-Emeric CS, Bastian L, Drake MT, Lyles KW.
Does this woman have osteoporosis? JAMA. 2004;292(23):
2890-2900.
6. Simpson C, Greenough WB III. Abdominal pain in an elderly
osteoporotic patient: ribs on pelvis syndrome. J Am Geriatr Soc.
2004;52(6):1039.
7. Wynne AT, Nelson MA, Nordin BE. Costo-iliac impingement
syndrome. J Bone Joint Surg Br. 1985;67(1):124-125.
8. Weiss JP, Blaivas JG. Nocturia. Curr Urol Rep. 2003;4(5):362-366.
9. Krieger J, Petiau C, Sforza E, Delanoe C, Hecht MT,
Chamouard V. Nocturnal pollakiuria is a symptom of
obstructive sleep apnea. Urol Int. 1993;50:93-97.
10. Margel D, Shochat T, Getzler O, Livne PM, Pillar G. Continuous
positive airway pressure reduces nocturia in patients with
obstructive sleep apnea. Urology. 2006;67(5):974-977.
11. The epidemiology of dry eye disease: report of the Epidemi-
ology Subcommittee of the International Dry Eye WorkShop
(2007). Ocul Surf. 2007;5(2):93-107.
12. Miljanovic B, Trivedi KA, Dana MR, Gilbard JP, Buring JE,
Schaumberg DA. Relation between dietary n-3 and n-6 fatty
acids and clinically diagnosed dry eye syndrome in women. Am J
Clin Nutr. 2005;82(4):887-893.
13. Oxholm P, Asmussen K, Wiik A, Horrobin DF. Essential fatty
acid status in cell membranes and plasma of patients with
primary Sjogrens syndrome: correlations to clinical and
immunologic variables using a new model for classication and
assessment of disease manifestations. Prostaglandins Leukot
Essent Fatty Acids. 1998;59(4):239-245.
14. Sullivan BD, Cermak JM, Sullivan RM, et al. Correlations
between nutrient intake and the polar lipid proles of meibo-
mian gland secretions in women with Sjogrens syndrome. Adv
Exp Med Biol. 2002;506(pt A):441-447.
15. Wojtowicz JC, Butovich I, Uchiyama E, Aronowicz J, Agee S,
McCulley JP. Pilot, prospective, randomized, double-masked,
placebo-controlled clinical trial of an omega-3 supplement for
dry eye. Cornea. 2011;30(3):308-314.
16. Go AS, Hylek EM, Chang Y, et al. Anticoagulation therapy for
stroke prevention in atrial brillation: how well do randomized
trials translate into clinical practice? JAMA. 2003;290(20):
2685-2692.
17. Gage BF, Waterman AD, Shannon W, Boechler M, Rich MW,
Radford MJ. Validation of clinical classication schemes for
CLINICAL PEARLS IN GENERAL INTERNAL MEDICINE 2012
Mayo Clin Proc. n January 2013;88(1):106-112 n http://dx.doi.org/10.1016/j.mayocp.2012.11.003
www.mayoclinicproceedings.org
111
predicting stroke: results from the National Registry of Atrial
Fibrillation. JAMA. 2001;285(22):2864-2870.
18. Lip GY, Nieuwlaat R, Pisters R, Lane DA, Crijns HJ. Rening
clinical risk stratication for predicting stroke and thrombo-
embolism in atrial brillation using a novel risk factor-based
approach: the Euro Heart Survey on Atrial Fibrillation. Chest.
2010;137(2):263-272.
19. Olesen JB, Lip GY, Hansen ML, et al. Validation of risk strati-
cation schemes for predicting stroke and thromboembolism in
patients with atrial brillation: nationwide cohort study. BMJ.
2011;342:d124.
20. EAFT (European Atrial Fibrillation Trial) Study Group.
Secondary prevention in non-rheumatic atrial brillation after
transient ischaemic attack or minor stroke. Lancet. 1993;
342(8882):1255-1262.
21. Gourlay ML, Fine JP, Preisser JS, et al. Bone-density testing
interval and transition to osteoporosis in older women. N Engl J
Med. 2012;366(3):225-233.
CORRECT ANSWERS: Case 1: b. Case 2: c. Case 3: a.
Case 4: e. Case 5: d. Case 6: d.
MAYO CLINIC PROCEEDINGS
112
Mayo Clin Proc. n January 2013;88(1):106-112 n http://dx.doi.org/10.1016/j.mayocp.2012.11.003
www.mayoclinicproceedings.org
Você também pode gostar
- 000-Intro To Internal MedicineDocumento6 páginas000-Intro To Internal MedicineRizky KykyAinda não há avaliações
- Diabetes Medication SummaryDocumento1 páginaDiabetes Medication Summarywoody_2512Ainda não há avaliações
- Sources: CardiovascularDocumento117 páginasSources: CardiovascularMohannad AlfadhalAinda não há avaliações
- Clinical Pearls in Pediatric CardiologyDocumento8 páginasClinical Pearls in Pediatric CardiologySunjon JondhleAinda não há avaliações
- The Audio PANCE and PANRE Episode 9Documento4 páginasThe Audio PANCE and PANRE Episode 9The Physician Assistant Life100% (1)
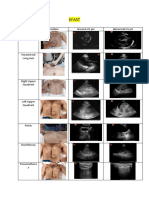
- Efast: Name Position Normal US Pic Abnormal US Pic SubcostalDocumento4 páginasEfast: Name Position Normal US Pic Abnormal US Pic SubcostalMaryam FadahAinda não há avaliações
- Internal Medicine (II) 2011 LogbookDocumento73 páginasInternal Medicine (II) 2011 LogbookQasim HaleimiAinda não há avaliações
- Antibiotic Sensitivity ChartDocumento1 páginaAntibiotic Sensitivity ChartJHAinda não há avaliações
- Common Bacteria by Site of Infection: Mouth Skin/Soft Tissue Bone and JointDocumento72 páginasCommon Bacteria by Site of Infection: Mouth Skin/Soft Tissue Bone and JointMuthia FadhilaAinda não há avaliações
- FomaDocumento1.218 páginasFomaosamaeAinda não há avaliações
- Mock Record B-1-2-Well Child VisitsDocumento4 páginasMock Record B-1-2-Well Child VisitsaelteeAinda não há avaliações
- Nephrology Guide for Medical StudentsDocumento20 páginasNephrology Guide for Medical StudentsAhmed El AlfyAinda não há avaliações
- NCCPA Exam Blueprint OverviewDocumento5 páginasNCCPA Exam Blueprint Overviewalren258Ainda não há avaliações
- NBME 12 - AnswersDocumento286 páginasNBME 12 - Answers1140271Ainda não há avaliações
- (Libribook - Com) Graber and Wilburs Family Medicine Examination and Board Review 5th EditionDocumento882 páginas(Libribook - Com) Graber and Wilburs Family Medicine Examination and Board Review 5th EditionPunnaphat Tinnaphop DaraswangAinda não há avaliações
- Nephrology Certification Examination Blueprint - American Board of Internal MedicineDocumento4 páginasNephrology Certification Examination Blueprint - American Board of Internal MedicineabimorgAinda não há avaliações
- Diabetes Management GuideDocumento20 páginasDiabetes Management GuideLeelanRamphalAinda não há avaliações
- Pediatrics Slides 23C 2020 8 Banvir 1aDocumento344 páginasPediatrics Slides 23C 2020 8 Banvir 1aBanvir SinghAinda não há avaliações
- JAUNDICE Internal Medicine PresentationDocumento34 páginasJAUNDICE Internal Medicine PresentationNano BaddourAinda não há avaliações
- Rama Id ConceptDocumento49 páginasRama Id ConceptpiangpornAinda não há avaliações
- Canadian Screening GuidelinesDocumento8 páginasCanadian Screening GuidelinesaayceeAinda não há avaliações
- OSCE Final 1 PDFDocumento204 páginasOSCE Final 1 PDFamalAinda não há avaliações
- Test CentreDocumento178 páginasTest CentreShaik Nizam Uddin100% (1)
- Cardiology IDocumento112 páginasCardiology IAhmad Makhlouf100% (1)
- Football Emergency Medicine Manual 2 EditionDocumento152 páginasFootball Emergency Medicine Manual 2 EditionNicolás Alvarez VidelaAinda não há avaliações
- Guide To Revising SceDocumento6 páginasGuide To Revising Scepratim deyAinda não há avaliações
- CCFP Certification Exam GuideDocumento24 páginasCCFP Certification Exam GuidePeterbb HelmanAinda não há avaliações
- Casebook Book: Famil yDocumento24 páginasCasebook Book: Famil ylentini@maltanet.net100% (1)
- Orientation ResidenecyDocumento18 páginasOrientation ResidenecyReeMii AngeLa100% (1)
- 2011 Understanding Pharmacology Essentials For Medication SafetyDocumento1 página2011 Understanding Pharmacology Essentials For Medication SafetygloriyaAinda não há avaliações
- Ospe Ophthalmology CorrectedDocumento55 páginasOspe Ophthalmology CorrectedGgah Vgggagagsg100% (1)
- Docslide - Us Family Medicine Shelf Reviewpptx Read OnlyDocumento142 páginasDocslide - Us Family Medicine Shelf Reviewpptx Read OnlyDavid DengAinda não há avaliações
- 1 4927329208029413644 PDFDocumento578 páginas1 4927329208029413644 PDFWaseem UllahAinda não há avaliações
- Case History and Data Interpretation in Medical PracticeDocumento563 páginasCase History and Data Interpretation in Medical PracticesaifabaasAinda não há avaliações
- Managing Common Infections Summary TablesDocumento8 páginasManaging Common Infections Summary TablesAlessandro ZadraAinda não há avaliações
- Intern Survival Guide (UIC)Documento51 páginasIntern Survival Guide (UIC)medstick100% (1)
- Kaplan Pharmacology FlashcardsDocumento2 páginasKaplan Pharmacology Flashcardsoussama dieselAinda não há avaliações
- Guide to Cardiac Exam Findings and DiagnosesDocumento58 páginasGuide to Cardiac Exam Findings and Diagnoseseliaszavaleta100% (1)
- (Ruth Ballweg, MPA, PA-C, Edward M. Sullivan, MS, (B-Ok - Xyz) PDFDocumento939 páginas(Ruth Ballweg, MPA, PA-C, Edward M. Sullivan, MS, (B-Ok - Xyz) PDFJim Velasquez100% (1)
- Common Genetic Diseases-2548Documento52 páginasCommon Genetic Diseases-2548Veerapong VattanavanitAinda não há avaliações
- Tropical Medicine & Infectious Disease BooksDocumento2 páginasTropical Medicine & Infectious Disease BooksIbrahimFikryAinda não há avaliações
- Mood Disorders: Advanced Practice Education AssociatesDocumento11 páginasMood Disorders: Advanced Practice Education AssociatesAndrea100% (1)
- Neet PG 2021 Q&A Medical JunctionDocumento144 páginasNeet PG 2021 Q&A Medical JunctionKk bhaiAinda não há avaliações
- The Audio PANCE and PANRE Episode 13Documento4 páginasThe Audio PANCE and PANRE Episode 13The Physician Assistant LifeAinda não há avaliações
- Durham Maths Mysteries ( (PDF)Documento16 páginasDurham Maths Mysteries ( (PDF)Stephanie HillAinda não há avaliações
- Banco Kap. - CK 2Documento1.099 páginasBanco Kap. - CK 2Lucas OrtizAinda não há avaliações
- Nurse Practitioner Wound Management Clinical ProtocolsDocumento29 páginasNurse Practitioner Wound Management Clinical ProtocolsBrian HarrisAinda não há avaliações
- EVIDENCE-BASED MEDICINE GUIDEDocumento34 páginasEVIDENCE-BASED MEDICINE GUIDEMuhamad Ghifari Azhar100% (1)
- Pharmacology Quick HitsDocumento6 páginasPharmacology Quick HitsHuma Hameed DogarAinda não há avaliações
- Finished Ekg Study GuideDocumento4 páginasFinished Ekg Study Guideapi-652914452Ainda não há avaliações
- Diabetes and Complications: When Documenting Diabetes, It's Important To Note The FollowingDocumento2 páginasDiabetes and Complications: When Documenting Diabetes, It's Important To Note The Followingmeikaizen100% (1)
- High Yield Internal MedicineDocumento100 páginasHigh Yield Internal Medicinedubblewalker100% (1)
- Quiz Question 1 - MKSAP 17Documento3 páginasQuiz Question 1 - MKSAP 17alaaAinda não há avaliações
- HandbookDocumento505 páginasHandbookWCLAinda não há avaliações
- Medical School Companion Obstetrics and Gynecology Practice Question BookNo EverandMedical School Companion Obstetrics and Gynecology Practice Question BookAinda não há avaliações
- Painless Evidence-Based MedicineNo EverandPainless Evidence-Based MedicineAntonio L. DansAinda não há avaliações
- 6th Central Pay Commission Salary CalculatorDocumento15 páginas6th Central Pay Commission Salary Calculatorrakhonde100% (436)
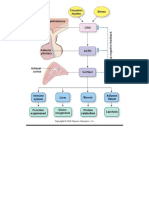
- Simple Adrenal Synthesis PathwayDocumento1 páginaSimple Adrenal Synthesis PathwayPkernAinda não há avaliações
- Selecting The Right' Positive End-Expiratory Pressure Level (Luciano Gattinoni, Current Opinion, 2016)Documento8 páginasSelecting The Right' Positive End-Expiratory Pressure Level (Luciano Gattinoni, Current Opinion, 2016)PkernAinda não há avaliações
- Rule of 4 Illustration Brainstem (LITFL)Documento1 páginaRule of 4 Illustration Brainstem (LITFL)PkernAinda não há avaliações
- Primary FRCA Pharmacology EquationsDocumento11 páginasPrimary FRCA Pharmacology EquationsMustafa SharkawyAinda não há avaliações
- The Crashing Ventilated Patient Ch.3 (Jairo I. Santanilla, ACEP, 2011) PDFDocumento10 páginasThe Crashing Ventilated Patient Ch.3 (Jairo I. Santanilla, ACEP, 2011) PDFPkernAinda não há avaliações
- The Crashing Ventilated Patient Ch.3 (Jairo I. Santanilla, ACEP, 2011) PDFDocumento10 páginasThe Crashing Ventilated Patient Ch.3 (Jairo I. Santanilla, ACEP, 2011) PDFPkernAinda não há avaliações
- Spinning Dials - How To Dominate The Ventilator - Handout (EMCRIT, ARDSnet) PDFDocumento5 páginasSpinning Dials - How To Dominate The Ventilator - Handout (EMCRIT, ARDSnet) PDFPkernAinda não há avaliações
- The Crashing Ventilated Patient Ch.3 (Jairo I. Santanilla, ACEP, 2011) PDFDocumento10 páginasThe Crashing Ventilated Patient Ch.3 (Jairo I. Santanilla, ACEP, 2011) PDFPkernAinda não há avaliações
- The Crashing Ventilated Patient Algorthm (Jairo I. Santanilla, ACEP, 2011)Documento1 páginaThe Crashing Ventilated Patient Algorthm (Jairo I. Santanilla, ACEP, 2011)PkernAinda não há avaliações
- Surgical Procedures in The Intensive Care Unit - A Critical Review. (BM Dennis, OL Gunter OA CC 2013)Documento7 páginasSurgical Procedures in The Intensive Care Unit - A Critical Review. (BM Dennis, OL Gunter OA CC 2013)PkernAinda não há avaliações
- Respiratory-Equations (Adam Hollingworth)Documento4 páginasRespiratory-Equations (Adam Hollingworth)PkernAinda não há avaliações
- Emergency Department Drug Card - For ALIEM - Sep 2013Documento1 páginaEmergency Department Drug Card - For ALIEM - Sep 2013PkernAinda não há avaliações
- Heart Failure PDFDocumento9 páginasHeart Failure PDFPkernAinda não há avaliações
- Primary FRCA Pharmacology EquationsDocumento11 páginasPrimary FRCA Pharmacology EquationsMustafa SharkawyAinda não há avaliações
- Respiratory Notes (Chris Andersen, ICUPrimaryPrep - Com)Documento14 páginasRespiratory Notes (Chris Andersen, ICUPrimaryPrep - Com)PkernAinda não há avaliações
- Diuretics and Renal HormonesDocumento3 páginasDiuretics and Renal HormonesPkernAinda não há avaliações
- Heart FailureDocumento9 páginasHeart FailurePkernAinda não há avaliações
- Neurology Notesc (Chris Andersen, ICUPrimaryPrep - Com)Documento11 páginasNeurology Notesc (Chris Andersen, ICUPrimaryPrep - Com)Pkern100% (1)
- Cardiac Murmurs and Maneuvers GuideDocumento1 páginaCardiac Murmurs and Maneuvers GuidePkernAinda não há avaliações
- ED Drug Treatment Cheat Sheet ANZICSDocumento1 páginaED Drug Treatment Cheat Sheet ANZICSPkernAinda não há avaliações
- Human Metabolism MapDocumento1 páginaHuman Metabolism MapPkern83% (6)
- Pharmacodynamics and Receptor TheoryDocumento8 páginasPharmacodynamics and Receptor TheoryPkernAinda não há avaliações
- STRUCTURE AND FUNCTION OF THE HEARTDocumento16 páginasSTRUCTURE AND FUNCTION OF THE HEARTPkernAinda não há avaliações
- Renal, Fluids and Acid-Base Notes (Chris Andersen, ICUPrimaryPrep - Com)Documento8 páginasRenal, Fluids and Acid-Base Notes (Chris Andersen, ICUPrimaryPrep - Com)PkernAinda não há avaliações
- 2014 CCM Review Notes Jon-Emile S. Kenny M.D, 2014Documento142 páginas2014 CCM Review Notes Jon-Emile S. Kenny M.D, 2014PkernAinda não há avaliações
- Neurology Notesc (Chris Andersen, ICUPrimaryPrep - Com)Documento11 páginasNeurology Notesc (Chris Andersen, ICUPrimaryPrep - Com)Pkern100% (1)
- Chapter 4 Pathophysiology of Edema FormationDocumento8 páginasChapter 4 Pathophysiology of Edema FormationPkernAinda não há avaliações
- Anaesthetic Drugs Cheat SheetsDocumento2 páginasAnaesthetic Drugs Cheat SheetsPkern100% (3)
- Chapter 3 The Lymphatic VasculatureDocumento8 páginasChapter 3 The Lymphatic VasculaturePkernAinda não há avaliações
- Board 2Documento1 páginaBoard 2kristine_nilsen_2Ainda não há avaliações
- Desert Power India 2050Documento231 páginasDesert Power India 2050suraj jhaAinda não há avaliações
- Reinvestment Allowance (RA) : SCH 7ADocumento39 páginasReinvestment Allowance (RA) : SCH 7AchukanchukanchukanAinda não há avaliações
- Amana PLE8317W2 Service ManualDocumento113 páginasAmana PLE8317W2 Service ManualSchneksAinda não há avaliações
- Digital Communication Quantization OverviewDocumento5 páginasDigital Communication Quantization OverviewNiharika KorukondaAinda não há avaliações
- Ryerson EthicsDocumento20 páginasRyerson EthicssinghbabaAinda não há avaliações
- Operation Manual: Auto Lensmeter Plm-8000Documento39 páginasOperation Manual: Auto Lensmeter Plm-8000Wilson CepedaAinda não há avaliações
- Identifying The TopicDocumento2 páginasIdentifying The TopicrioAinda não há avaliações
- Advantages and Disadvantages of The DronesDocumento43 páginasAdvantages and Disadvantages of The DronesVysual ScapeAinda não há avaliações
- Programming Manual Magic 308/616-CLI Quick ReferenceDocumento16 páginasProgramming Manual Magic 308/616-CLI Quick ReferencekrishnamarajublrAinda não há avaliações
- Control SystemsDocumento269 páginasControl SystemsAntonis SiderisAinda não há avaliações
- IMM Indian Oil Case Group 3Documento13 páginasIMM Indian Oil Case Group 3Soniya AgnihotriAinda não há avaliações
- Finance at Iim Kashipur: Group 9Documento8 páginasFinance at Iim Kashipur: Group 9Rajat SinghAinda não há avaliações
- Vehicle Registration Renewal Form DetailsDocumento1 páginaVehicle Registration Renewal Form Detailsabe lincolnAinda não há avaliações
- Individual Sports Prelim ExamDocumento13 páginasIndividual Sports Prelim ExamTommy MarcelinoAinda não há avaliações
- Put The Items From Exercise 1 in The Correct ColumnDocumento8 páginasPut The Items From Exercise 1 in The Correct ColumnDylan Alejandro Guzman Gomez100% (1)
- Exor EPF-1032 DatasheetDocumento2 páginasExor EPF-1032 DatasheetElectromateAinda não há avaliações
- VEGA MX CMP12HP Data SheetDocumento2 páginasVEGA MX CMP12HP Data SheetLuis Diaz ArroyoAinda não há avaliações
- Ana White - PLANS - A Murphy Bed YOU Can Build, and Afford To Build - 2011-03-03Documento20 páginasAna White - PLANS - A Murphy Bed YOU Can Build, and Afford To Build - 2011-03-03Ahmad KamilAinda não há avaliações
- Introduction To OpmDocumento30 páginasIntroduction To OpmNaeem Ul HassanAinda não há avaliações
- Micropolar Fluid Flow Near The Stagnation On A Vertical Plate With Prescribed Wall Heat Flux in Presence of Magnetic FieldDocumento8 páginasMicropolar Fluid Flow Near The Stagnation On A Vertical Plate With Prescribed Wall Heat Flux in Presence of Magnetic FieldIJBSS,ISSN:2319-2968Ainda não há avaliações
- Colour Ring Labels for Wireless BTS IdentificationDocumento3 páginasColour Ring Labels for Wireless BTS Identificationehab-engAinda não há avaliações
- SQL Server 2008 Failover ClusteringDocumento176 páginasSQL Server 2008 Failover ClusteringbiplobusaAinda não há avaliações
- Tatoo Java Themes PDFDocumento5 páginasTatoo Java Themes PDFMk DirAinda não há avaliações
- Neuropathology of Epilepsy: Epilepsy-Related Deaths and SUDEPDocumento11 páginasNeuropathology of Epilepsy: Epilepsy-Related Deaths and SUDEPTeuku AvicennaAinda não há avaliações
- SiBRAIN For PIC PIC18F57Q43 SchematicDocumento1 páginaSiBRAIN For PIC PIC18F57Q43 Schematicivanfco11Ainda não há avaliações
- Conceptual FrameworkDocumento24 páginasConceptual Frameworkmarons inigoAinda não há avaliações
- The Online Medical Booking Store Project ReportDocumento4 páginasThe Online Medical Booking Store Project Reportharshal chogle100% (2)
- Lesson 2 Mathematics Curriculum in The Intermediate GradesDocumento15 páginasLesson 2 Mathematics Curriculum in The Intermediate GradesRose Angel Manaog100% (1)
- Gi 007 Gerund InfinitiveDocumento2 páginasGi 007 Gerund Infinitiveprince husainAinda não há avaliações