Escolar Documentos
Profissional Documentos
Cultura Documentos
Site Preservation Decision Tree
Enviado por
HaoWang0 notas0% acharam este documento útil (0 voto)
147 visualizações8 páginasRidge preservation has been shown to be effective in decreasing alveolar bone resorption after tooth removal. Different types of bone grafts (autograft, allograft, and xenograft) and barrier membranes (resorbable and non-resorbable) have been evaluated in clinical studies.
Descrição original:
Direitos autorais
© © All Rights Reserved
Formatos disponíveis
PDF, TXT ou leia online no Scribd
Compartilhar este documento
Compartilhar ou incorporar documento
Você considera este documento útil?
Este conteúdo é inapropriado?
Denunciar este documentoRidge preservation has been shown to be effective in decreasing alveolar bone resorption after tooth removal. Different types of bone grafts (autograft, allograft, and xenograft) and barrier membranes (resorbable and non-resorbable) have been evaluated in clinical studies.
Direitos autorais:
© All Rights Reserved
Formatos disponíveis
Baixe no formato PDF, TXT ou leia online no Scribd
0 notas0% acharam este documento útil (0 voto)
147 visualizações8 páginasSite Preservation Decision Tree
Enviado por
HaoWangRidge preservation has been shown to be effective in decreasing alveolar bone resorption after tooth removal. Different types of bone grafts (autograft, allograft, and xenograft) and barrier membranes (resorbable and non-resorbable) have been evaluated in clinical studies.
Direitos autorais:
© All Rights Reserved
Formatos disponíveis
Baixe no formato PDF, TXT ou leia online no Scribd
Você está na página 1de 8
PRACTICAL APPLICATIONS
The Decision-Making Process for Ridge Preservation
Procedures After Tooth Extraction
Natalie A. Frost,* Arwa A. Banjar,* Patrick B. Galloway,* Guy Huynh-Ba,* and Brian L. Mealey*
Focused Clinical Question: How should the
extraction socket be managed after tooth removal?
Summary: Resorptive changes that take place af-
ter tooth extraction can result in a significant reduction in
alveolar ridge width and height. This may create a prob-
lem for proper implant placement and fabrication of es-
thetic restorations. Ridge preservation has been shown
to be effective in decreasing alveolar bone resorption af-
ter tooth removal. During ridge preservation, the extrac-
tion socket is filled with graft material, and a barrier is
generally used to contain the graft. Flap reflection is usu-
ally not recommended if the socket walls are intact and
the ridge width is sufficient after tooth removal. However,
if significant breakdown of the buccal bony plate is pres-
ent, mucoperiosteal flap elevation may be required to al-
low proper placement of the bone graft and membrane.
Different types of bone grafts (autograft, allograft, and
xenograft) and barrier membranes (resorbable and non-
resorbable) have been evaluated in clinical studies.
They all are shown to be effective regardless of the ma-
terial or technique used.
Conclusions: Ridge preservation is an effective
procedure for minimizing horizontal and vertical alveolar
ridge resorption after tooth extraction. Current evidence
does not support one technique as being superior to an-
other. The selection of the technique to be used should
be based on the clinical situation. Clin Adv Periodontics
2014;4:56-63.
Key Words: Alveolar bone loss; bone resorption; bone
transplantation; dental implants; tooth extraction.
Background
Understanding the extraction socket repair process is
essential for proper treatment planning after tooth loss.
Extraction initiates a sequence of events that results in
undesirable morphologic changes of alveolar ridge contour.
Anumber of studies in humans and animal models evaluated
extraction socket healing using histologic, clinical, and
radiographic methods.
1-3
They all found a significant re-
duction in alveolar ridge width and height. Schropp et al.
2
reported the resorption after tooth removal may reduce
ridge width by 50% and that most changes take place
within the first 3 months. This study also reported a
significant reduction in ridge height, mainly on the facial
aspect. Subsequent to the remodeling process is relocation of
the center of the alveolar ridge to a more lingual or palatal
position that is unfavorable for implant placement. Ridge
remodeling may be worsened by the presence of severe bone
loss around the tooth from preexisting periodontal disease
or periapical lesions.
The amount of bone resorption that occurs after extrac-
tion is influenced by the thickness of the buccal plate,
which is determined by the size, form, and axial inclination
of the tooth. A thin buccal plate consists mainly of cortical
bundle bone that becomes more susceptible to resorption
after extraction.
1
In a study by Spray et al.,
4
the facial mar-
ginal bone loss around implants was evaluated in relation
to bone thickness. The study reported a significant reduc-
tion in bone loss when the facial bone thickness was 1.8 to
2 mm compared with thinner facial bone. Almost 85% of
maxillary anterior teeth have a buccal plate thickness <1
mm, which makes preservation of ridge dimension criti-
cal for optimal implant placement and construction of
esthetic restorations.
5,6
Ridge preservation is a clinical procedure that is per-
formed at the time of tooth extraction to minimize bone
resorption of the socket walls. Ridge preservation involves
placing a bone graft material into the socket immediately
after extraction. The bone graft material may be an auto-
graft, allograft, xenograft, or alloplastic material. The se-
lection of a barrier membrane to cover the graft material
may depend on the shape of the defect created after tooth
removal.
7
Several studies show that using ridge preserva-
tion techniques limits the resorptive changes that take
place after extraction.
7-10
Iasella et al.
11
evaluated the
use of freeze-dried bone allograft (FDBA) and collagen
membrane versus no treatment and found significantly
less reduction in ridge width, z2 mm less, and evidence
of improvement of ridge height with use of grafting ma-
terials.
11
Other studies have assessed different types of
bone graft materials and barrier membranes for ridge
preservation, and all have proven to be effective in reduc-
ing alveolar ridge resorption.
7-10
The quality of bone formed in grafted sockets has also
been examined. Histologic assessment of biopsies obtained
from grafted sites show residual graft material in addition
to vital bone and connective tissue (CT), with the percent-
ages of each tissue type varying depending on graft material
used and the amount of healing time between grafting
and implant placement.
7,8,10,12
The effect of the residual
* Department of Periodontics, University of Texas Health Science Center
at San Antonio, San Antonio, TX.
Submitted February 15, 2013; accepted for publication March 27, 2013
doi: 10.1902/cap.2013.130013
56 Clinical Advances in Periodontics, Vol. 4, No. 1, February 2014
graft particles on the future osseointegration of the dental
implant has not been determined. The purpose of this pa-
per is to provide clinicians with guidance on the decision-
making process for ridge preservation techniques after
tooth extraction.
Decision Process
Ridge preservation techniques may be necessary if the ulti-
mate goal after extraction is the surgical placement, os-
seointegration, and functional and esthetic success of an
implant (Figs. 1 and 2). Ridge preservation may also be com-
pleted in areas in which implants are not going to be placed,
for example, to support the intaglio surface of a pontic for
esthetic reasons (Fig. 3). The following decision process is
based on the evidence available for howdifferent clinical sce-
narios may be handled. The clinician should analyze a series
of questions to guide the decision-making process (Fig. 4).
The first question is: Will ridge preservation likely result
in sufficient bone width for eventual implant placement,
assuming normal healing? A disease process or trauma
from extraction may result in partial breakdown of the
buccal plate, resulting in a dehiscence or fenestration. Flap
reflection may not be necessary for small fenestrations and
dehiscences. Here, an internal membrane may be adequate
to repair the socket and contain the graft material, separat-
ing the graft material fromthe soft tissue opposite the fenes-
tration or dehiscence
13
(Fig. 3). However, if there has been
significant breakdown of the bony socket walls, it may be
prudent to reflect a flap and perform guided bone regenera-
tion (GBR) at the site to restore appropriate ridge shape
and dimension in which bony walls are missing (Fig. 5).
Flap reflection will allow better access to the defect and
more space for the necessary grafting materials. The au-
thors distinguish between ridge preservation procedures
in which the bony walls of the socket are entirely or almost
entirely intact and GBR procedures in which bony walls are
substantially missing and the ridge form must be re-created
with graft materials and barrier membranes.
If the bony walls of the socket are mainly intact after
tooth extraction, and ridge dimensions would be sufficient
for an implant without having to perform a GBR proce-
dure, the next question is: What is the status of the buccal
plate after tooth removal? If the buccal plate thickness is at
least 2 mm, such as might be found in some molar sites,
FIGURE 1 Anterior extraction and ridge preser-
vation. The patient reported previous trauma to
tooth #9 and was diagnosed with a hopeless
periodontal prognosis. Tooth #9 was extracted
with minimal trauma. The buccal plate was intact
without fenestration or dehiscence. Anorganic
bovine bone was placed into the socket. An
autogenous free gingival graft with CT exten-
sions was harvested and placed under the
buccal and palatal flaps to obtain primary
closure over the grafted site. 1a Preoperative
radiographic evidence of severe bone loss. 1b
Postextraction, buccal view. 1c Immediate post-
operative image. 1d Six-month postoperative
evaluation. 1e Six-month cone-beam computed
tomography (CBCT) image suggests that implant
placement at site #9 is possible without the need
for bone grafting before implant placement.
P R A C T I C A L A P P L I C A T I O N S
Frost, Banjar, Galloway, Huynh-Ba, Mealey Clinical Advances in Periodontics, Vol. 4, No. 1, February 2014 57
ridge preservation may be optional, although most ridge
preservation research has focused on non-molar teeth.
However, ridge preservation techniques may still have
some benefit in preventing sinus pneumatization in
maxillary molar sites.
14
Non-molar sites inherently pose a bigger esthetic risk, be-
cause any loss of ridge dimensionmay affect the final esthetic
outcome (Figs. 1 and 4). The buccal plate is usually thin in
non-molar sites.
5,6,15
Thus, the potential esthetic benefit in
non-molar sites mayoutweighthe costs associatedwithbasic
ridge preservation techniques. When the buccal plate thick-
ness is <2 mm, ridge dimensions are more susceptible to
resorption.
4
Therefore, ridge preservation is recommen-
ded when the buccal plate thickness is <2 mm, regardless
of tooth type (Fig. 4). The clinician may also decide to
include a CT graft if esthetics are a concern.
16
The CT
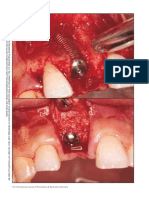
FIGURE 2 Posterior extraction and ridge preservation. Tooth #4 was deemed hopeless as a result of vertical root fracture. The tooth was extracted with
minimal trauma. Although the clinical biotype was average to thick, the buccal plate thickness was <1 mm. The socket was grafted with mineralized FDBA and
covered with a resorbable collagen orifice barrier. The site was sutured with 4-0 chromic gut sutures. 2a Preoperative view. 2b Immediate postoperative image.
2c Healed edentulous ridge 4 months after ridge preservation. 2d Flap reflection of edentulous site z4 months after ridge preservation. 2e Implant placement
possible with adequate buccal and palatal bone remaining. 2f Final crown delivery.
P R A C T I C A L A P P L I C A T I O N S
58 Clinical Advances in Periodontics, Vol. 4, No. 1, February 2014 Decision Making for Ridge Preservation After Extraction
graft will provide a bulk of soft tissue to better simulate
a physiologic gingival architecture.
Many different resorbable and non-resorbable mem-
branes, allografts, autografts, xenografts, and alloplasts
have been used successfully for ridge preservation. There
is no evidence at this time to support superiority for any
particular materials. The process to determine which type
of grafting material, orifice barrier, and membrane mate-
rial to be used is beyond the scope of this article.
Discussion
The scenarios presented above demonstrate a variety of
clinical situations possible at the time of tooth extraction.
Each circumstance may require a modification in the
approach to ridge preservation techniques. The follow-
ing offers additional explanations and supporting evidence
for the clinical management relating to each scenario.
Posterior Versus Anterior (Biotype and Buccal
Plate)
Periodontal biotype is often categorized as thick, thin, or
average.
15,17
Assessment of periodontal biotype may be ac-
complished by inserting a periodontal probe into the facial
sulcus and evaluating for probe visibility.
15,17
Cook et al.
15
demonstrated that periodontal biotype is related to buccal
plate thickness; a thinbiotype was associatedwitha thinner
buccal plate. As stated previously, a thin buccal plate is more
susceptible to resorption, compromising esthetics and gingi-
val margin stability after implant placement. Therefore, it
may not be necessary to perform ridge preservation in areas
with a thick buccal plate, such as the molar region.
Sinus Pneumatization
Although ridge preservation may not be needed in poste-
rior sites with a thick buccal plate, maxillary posterior tooth
extraction may be followed by sinus pneumatization.
18
This decreases vertical bone height inferior to the sinus
floor, possibly complicating future implant placement.
Greater pneumatization of the sinus may occur when the si-
nus floor curves superiorly above the root apices of the teeth
to be extracted, when multiple adjacent maxillary teeth are
extracted, and after extraction of second molars compared
with first molars.
18
Evaluating the patient and identifying
any of the above characteristics may support use of ridge
preservation procedures. In a small study, Rasperini et al.
14
examined the need for sinus augmentation after maxillary
first or second molar extraction. Test sites received ridge
preservation with anorganic bovine bone in a collagen
FIGURE 3 Multiple adjacent ridge preserva-
tions. Patient presented with multiple maxillary
anterior teeth with endodontic and restorative
failure. All maxillary incisors were extracted and
ridge preservation was completed at each
socket site. A 5-mm-deep buccal dehiscence
was noted at tooth #8. A resorbable collagen
socket repair membrane was placed in the
internal aspect of the socket to replace the
missing buccal bony dimension. After membrane
placement, mineralized FDBA and resorbable
collagen barriers were used in all sites for ridge
preservation. 3a Preoperative periapical radio-
graph. 3b Use of resorbable collagen socket
repair membrane placed inside socket to replace
missing buccal bony dimension. 3c Immediate
postoperative image showing collagen orifice
barriers. 3d Five-month postoperative CBCT
image at site #8 verifying sufficient ridge di-
mensions for future implant placement. 3e Five-
month postoperative clinical image.
P R A C T I C A L A P P L I C A T I O N S
Frost, Banjar, Galloway, Huynh-Ba, Mealey Clinical Advances in Periodontics, Vol. 4, No. 1, February 2014 59
sponge, whereas control sites received no ridge preserva-
tion. Only one of six sites treated with ridge preservation
required sinus augmentation before implant placement
compared to three of eight sites in the control group.
Internal Membrane Versus External Membrane
Extraction sites with small fenestrations or dehiscences may
not require reflection of a full-thickness mucoperiosteal
flap. Here, the use of an internal socket repair membrane
may be adequate for graft containment
13
(Fig. 3). Larger
fenestrations or dehiscences may require a full-thickness
flap for access to extend the membrane beyond the margins
of the bony defect (Fig. 5). There is currently no evidence to
support which technique, interior versus exterior membrane
placement, is superior.
Flap Versus Flapless
It has been suggested that greater alveolar resorption oc-
curs after elevation of a mucoperiosteal flap at the time
of extraction. In beagle dogs, Fickl et al.
19
investigated
soft- and hard-tissue volumetric changes that can be attrib-
uted to flap elevation at the time of extraction. In sites in
which a flap was elevated, there was 0.7-mm greater vol-
umetric hard- and soft-tissue loss compared with flapless
procedures. However, other authors have demonstrated
histologically that similar amounts of buccal and lingual
bone loss at the coronal extent of the socket occurs after 6
months of healing with or without flap reflection.
1
A re-
cent meta-analysis concluded that surgical procedures in-
volving flap reflection had significantly less horizontal
resorption of the socket when compared with flapless sur-
geries.
20
The authors suggested that this finding is the re-
sult of achieving primary intention healing after ridge
preservation with flapped procedures. However, many
clinicians do not attempt primary closure for simple ridge
preservation procedures. In light of conflicting study de-
signs and results, it seems prudent to minimize surgical
trauma to decrease healing time and postoperative com-
plications. This is generally done by minimizing flap re-
flection for extraction and ridge preservation. Of course,
FIGURE 4 Decision tree: selection of treatment strategy. Proper management of an extraction socket should be based on careful analysis of the clinical
presentation and restorative treatment plan. Also, the clinician should consider intraoperative surgical findings, including thickness of the buccal plate and
clinical biotype, presence of buccal fenestrations or dehiscences, and molar versus non-molar sites. Depending on the graft material used, the clinician may or
may not choose to cover the graft with an orifice barrier in some cases. Adjunctive CT grafts may be indicated in areas with thin biotype, gingival recession, or
other potential esthetic compromise.
P R A C T I C A L A P P L I C A T I O N S
60 Clinical Advances in Periodontics, Vol. 4, No. 1, February 2014 Decision Making for Ridge Preservation After Extraction
flap elevation still may be justified for adequate tooth re-
moval and extraction site management.
What Material/Technique Is Superior?
Numerous studies have shownthat ridge preservation tech-
niques reduce alveolar resorption compared with extraction
alone.
2,3,21
There are a variety of techniques and materials
available, and no study has demonstrated a clear superi-
ority for technique or choice of grafting material.
22
Unless
and until such time a given material or technique shows
superiority to others, clinicians generally choose mate-
rials for ridge preservation based on experience with those
materials or techniques when used for other purposes,
such as guided tissue regeneration or GBR; material costs;
handling characteristics; and patient concerns about use
of materials from other humans or different species.
22,23
Primary Closure Versus No Primary Closure
There are many methods of closure over grafted sockets,
including complete flap advancement over the socket,
placement of a resorbable or non-resorbable membrane,
and CTor free soft-tissue autografts (Fig. 1). Some prac-
titioners also leave their grafts exposed and allowhealing
by secondary intention. One meta-analysis showed a small
tendency toward less horizontal resorption when sockets
healed by primary intention.
20
However, another meta-anal-
ysis found that, given the variety of techniques and materials
used, it appears that there is no superior method of closure
for ridge preservation.
22
Healing Time Between Ridge Preservation and
Implant Placement
How long after ridge preservation is the graft adequately
incorporated, and when will the grafted site be ready for
implant placement? Studies of ridge preservation have var-
ied widely in healing time between socket grafting and im-
plant placement, from several weeks to >1 year.
22
A study
by Beck and Mealey
7
investigated the use of mineralized
bone allograft combined with a resorbable collagen barrier
dressing. Their results indicated that similar percentages of
vital bone were present in the former socket region after 3
and 6 months of healing: 45.8%versus 45.0%, respectively.
However, even if one completes ridge preservation at the
time of extraction, it may be necessary to performadditional
bone augmentation before or even at the time of implant
placement because some horizontal loss of ridge width often
FIGURE 5 Anterior ridge preservation with large
buccal defect. Teeth #7 and #8 presented with
internal root resorption and were deemed end-
odontically hopeless. After extraction of these
teeth, a fracture of the buccal plate occurred that
necessitated aborting ridge preservation tech-
niques and proceeding with GBR instead. A full-
thickness flap was elevated to reveal large
buccal deformities at both sites #7 and #8.
Mineralized FDBA was used to graft both sites
and was covered with a resorbable collagen
membrane. 5a Preoperative view. 5b Preopera-
tive CBCT image, site #8. 5c Preoperative CBCT
image, site #7. 5d Intraoperative view of buccal
deformity existing after tooth extraction. 5e
Intraoperative view of GBR technique with
particulate bone graft and overlying resorbable
membrane.
P R A C T I C A L A P P L I C A T I O N S
Frost, Banjar, Galloway, Huynh-Ba, Mealey Clinical Advances in Periodontics, Vol. 4, No. 1, February 2014 61
occurs even with ridge preservation procedures.
7,10-12,21,22
The need for additional bone grafting during implant place-
ment can be determined by clinical and radiographic evalu-
ation of the future implant site (Figs. 1 and 2).
Success and Survival Rates of Implants at
Ridge-Preserved Sites
What are the success and survival rates for implants
placed in grafted sites? A systematic review found a lim-
ited number of studies reporting success/survival of im-
plants placed into ridge-preserved sites; however, the
survival rates ranged from 90% to 97%.
22
Future long-
termstudies are needed regarding the dimensional stability
of sites that have previously undergone ridge preservation.
Important questions remain to be answered regarding im-
plant placement in augmented sites. Does it really matter
how much vital bone there is at the time of implant place-
ment? Is there any clinical benefit for a higher percentage of
vital bone? Does ridge preservation affect the quality of the
bone supporting the dental implant? If implant placement
is not performed for an extended period of time after ridge
preservation procedures, is the dimensional stability of the
ridge maintained or does ridge loss occur in the absence of
an implant? Future studies should focus on these inquiries.
Conclusions
Ridge preservation is commonly recommended after tooth
extraction, especially in sites having thin remaining bony
walls. Evidence suggests that ridge preservationis generally
effective in decreasing the loss of horizontal and vertical
ridge dimensions, with some variability between sites or pa-
tients. Ridge preservation may allowplacement of dental im-
plants at sites that might otherwise require GBR procedures
before or in conjunction with implant placement. Future re-
search should improve the current knowledge as to which
specific techniques and materials may best preserve ridge
dimensions after extraction. n
Acknowledgment
The authors report noconflicts of interest relatedtothis study.
CORRESPONDENCE:
Dr. Brian L. Mealey, Department of Periodontics, University of Texas
Health Science Center at San Antonio, MSC 7894, 7703 Floyd Curl Dr.,
San Antonio, TX 78229-3900. E-mail: mealey@uthscsa.edu.
P R A C T I C A L A P P L I C A T I O N S
62 Clinical Advances in Periodontics, Vol. 4, No. 1, February 2014 Decision Making for Ridge Preservation After Extraction
References
1. Arau jo MG, Lindhe J. Ridge alterations following tooth extraction with
and without flap elevation. An experimental study in the dog. Clin Oral
Implants Res 2009;20:545-549.
2. Schropp L, Wenzel A, Kostopoulos L, Karring T. Bone healing and soft
tissue contour changes following single-tooth extraction: A clinical and
radiographic 12-month prospective study. Int J Periodontics Restorative
Dent 2003;23:313-323.
3. Van der Weijden F, DellAcqua F, Slot DE. Alveolar bone dimensional
changes of post-extraction sockets in humans: A systematic review.
J Clin Periodontol 2009;36:1048-1058.
4. Spray JR, Black CG, Morris HF, Ochi S. The influence of bone thickness
on facial marginal bone response: Stage 1 placement through stage 2
uncovering. Ann Periodontol 2000;5:119-128.
5. Janua rio AL, Duarte WR, Barriviera M, Mesti JC, Arau jo MG, Lindhe J.
Dimension of the facial bone wall in the anterior maxilla: A cone-beam
computed tomography study. Clin Oral Implants Res 2011;22:1168-
1171.
6. Huynh-Ba G, Pjetursson BE, Sanz M, et al. Analysis of the socket bone
wall dimensions in the upper maxilla in relation to immediate implant
placement. Clin Oral Implants Res 2010;21:37-42.
7. Beck TM, Mealey BL. Histologic analysis of healing after tooth
extraction with ridge preservation using mineralized human bone
allograft. J Periodontol 2010;81:1765-1772.
8. Cardaropoli D, Tamagnone L, Roffredo A, Gaveglio L, Cardaropoli G.
Socket preservation using bovine bone mineral and collagen membrane:
A randomized controlled clinical trial with histologic analysis. Int
J Periodontics Restorative Dent 2012;32:421-430.
9. Nevins M, Camelo M, De Paoli S, et al. A study of the fate of the buccal
wall of extraction sockets of teeth with prominent roots. Int J
Periodontics Restorative Dent 2006;26:19-29.
10. Wood RA, Mealey BL. Histologic comparison of healing after tooth
extraction with ridge preservation using mineralized versus demineral-
ized freeze-dried bone allograft. J Periodontol 2012;83:329-336.
11. Iasella JM, Greenwell H, Miller RL, et al. Ridge preservation with
freeze-dried bone allograft and a collagen membrane compared to
extraction alone for implant site development: A clinical and histologic
study in humans. J Periodontol 2003;74:990-999.
12. Hoang TN, Mealey BL. Histologic comparison of healing following
ridge preservation using human demineralized bone matrix putty with
one versus two different-sized bone particles. J Periodontol 2012;83:
174-181.
13. Elian N, Cho SC, Froum S, Smith RB, Tarnow DP. A simplified socket
classification and repair technique. Pract Proced Aesthet Dent 2007;19:
99-104, quiz 106.
14. Rasperini G, Canullo L, Dellavia C, Pellegrini G, Simion M. Socket
grafting in the posterior maxilla reduces the need for sinus augmenta-
tion. Int J Periodontics Restorative Dent 2010;30:265-273.
15. Cook DR, Mealey BL, Verrett RG, et al. Relationship between clinical
periodontal biotype and labial plate thickness: An in vivo study. Int J
Periodontics Restorative Dent 2011;31:345-354.
16. Tsuda H, Rungcharassaeng K, Kan JY, Roe P, Lozada JL, Zimmerman
G. Peri-implant tissue response following connective tissue and bone
grafting in conjunction with immediate single-tooth replacement in
the esthetic zone: A case series. Int J Oral Maxillofac Implants 2011;
26:427-436.
17. De Rouck T, Eghbali R, Collys K, De Bruyn H, Cosyn J. The gingival
biotype revisited: Transparency of the periodontal probe through the
gingival margin as a method to discriminate thin from thick gingiva.
J Clin Periodontol 2009;36:428-433.
18. Sharan A, Madjar D. Maxillary sinus pneumatization following extrac-
tions: A radiographic study. Int J Oral Maxillofac Implants 2008;23:
48-56.
19. Fickl S, Zuhr O, Wachtel H, Bolz W, Huerzeler M. Tissue alterations
after tooth extraction with and without surgical trauma: A volumetric
study in the beagle dog. J Clin Periodontol 2008;35:356-363.
20. Vignoletti F, Matesanz P, Rodrigo D, Figuero E, Martin C, Sanz M.
Surgical protocols for ridge preservation after tooth extraction. A
systematic review. Clin Oral Implants Res 2012;23(Suppl. 5):22-38.
21. Tan WL, Wong TL, Wong MC, Lang NP. A systematic review of post-
extractional alveolar hard and soft tissue dimensional changes in
humans. Clin Oral Implants Res 2012;23(Suppl. 5):1-21.
22. Darby I, Chen ST, Buser D. Ridge preservation techniques for implant
therapy. Int J Oral Maxillofac Implants 2009;24(Suppl.):260-271.
23. Toloue SM, Chesnoiu-Matei I, Blanchard SB. A clinical and histomor-
phometric study of calcium sulfate compared with freeze-dried bone
allograft for alveolar ridge preservation. J Periodontol 2012;83:847-855.
P R A C T I C A L A P P L I C A T I O N S
Frost, Banjar, Galloway, Huynh-Ba, Mealey Clinical Advances in Periodontics, Vol. 4, No. 1, February 2014 63
Você também pode gostar
- Dental Assistant Sample TestDocumento10 páginasDental Assistant Sample TestFaye Nervanna Alecha Alferez100% (2)
- Fixed Orthodontic Appliances: A Practical GuideNo EverandFixed Orthodontic Appliances: A Practical GuideNota: 1 de 5 estrelas1/5 (1)
- Altering Gingival Levels: The Restorative Connection Biologic VariablesDocumento7 páginasAltering Gingival Levels: The Restorative Connection Biologic Variablespooja100% (1)
- Prosthetic Aspects of Dental Implants - IIDocumento73 páginasProsthetic Aspects of Dental Implants - IIKomal TalrejaAinda não há avaliações
- 11-Impacted Third MolarDocumento117 páginas11-Impacted Third MolarAhmed aljumailiAinda não há avaliações
- CasesDocumento49 páginasCasesYasmin Ismaiel100% (13)
- Single Maxillary Complete Denture: Carl F. Driscoll, DMD, Radi M. Masri, BDS, MSDocumento17 páginasSingle Maxillary Complete Denture: Carl F. Driscoll, DMD, Radi M. Masri, BDS, MSSahana RangarajanAinda não há avaliações
- Immediate Implant Placement PDFDocumento11 páginasImmediate Implant Placement PDFFerdinan PasaribuAinda não há avaliações
- Use of Implants in The Pterygoid Region For Prosthodontic TreatmentDocumento4 páginasUse of Implants in The Pterygoid Region For Prosthodontic TreatmentSidhartha KumarAinda não há avaliações
- Implant Complications and Failures - The Complete OverdentureDocumento5 páginasImplant Complications and Failures - The Complete OverdentureAdina UlaruAinda não há avaliações
- Implant ResearchDocumento8 páginasImplant ResearchFBI LUC1FeRAinda não há avaliações
- Horizontal Alveolar Ridge Augmentation in Implant Dentistry: A Surgical ManualNo EverandHorizontal Alveolar Ridge Augmentation in Implant Dentistry: A Surgical ManualNota: 4.5 de 5 estrelas4.5/5 (2)
- Clinical Maxillary Sinus Elevation SurgeryNo EverandClinical Maxillary Sinus Elevation SurgeryDaniel W. K. KaoAinda não há avaliações
- Treatment Planning Single Maxillary Anterior Implants for DentistsNo EverandTreatment Planning Single Maxillary Anterior Implants for DentistsAinda não há avaliações
- Avoiding and Treating Dental Complications: Best Practices in DentistryNo EverandAvoiding and Treating Dental Complications: Best Practices in DentistryDeborah A. TermeieAinda não há avaliações
- Case Selection in Dental Implant TherapyDocumento4 páginasCase Selection in Dental Implant Therapymichealraj rousseauAinda não há avaliações
- A Guide To Implant Dentistry Part 2 Surgical and Prosthodontic ConsiderationsDocumento7 páginasA Guide To Implant Dentistry Part 2 Surgical and Prosthodontic ConsiderationsPhú VinhAinda não há avaliações
- Practice: Failures in Implant DentistryDocumento7 páginasPractice: Failures in Implant DentistryhmsatAinda não há avaliações
- Management of Peri-Implant Mucositis and Peri-Implantitis PDFDocumento19 páginasManagement of Peri-Implant Mucositis and Peri-Implantitis PDFgirl33Ainda não há avaliações
- 3.factors and Techniques Influencing Peri-Implant Papillae - PDFDocumento12 páginas3.factors and Techniques Influencing Peri-Implant Papillae - PDFMargarita María Blanco LópezAinda não há avaliações
- Maxillofacial Prosthetics: Kamolphob Phasuk,, Steven P. HaugDocumento11 páginasMaxillofacial Prosthetics: Kamolphob Phasuk,, Steven P. Hauglaura sanchez avilaAinda não há avaliações
- Biologic WidthDocumento39 páginasBiologic Widthsharanya chekkarrajAinda não há avaliações
- Managing The Unstable CDDocumento8 páginasManaging The Unstable CDNajeeb UllahAinda não há avaliações
- IRTDocumento2 páginasIRTIgnacioAinda não há avaliações
- 2 Nonsurgical Periodontal Therapy - Pocket DentistryDocumento14 páginas2 Nonsurgical Periodontal Therapy - Pocket DentistryRizki OktavianiAinda não há avaliações
- Periodontology 2000 - 2023 - Urban - Minimal Invasiveness in Vertical Ridge AugmentationDocumento19 páginasPeriodontology 2000 - 2023 - Urban - Minimal Invasiveness in Vertical Ridge AugmentationLEONARDO ALBERTO CRESPIN ZEPEDAAinda não há avaliações
- Ke Principles of Implant Dentistr in The Esthetic Zone: Michael Sonick, DMD Debb Hwang, DMDDocumento6 páginasKe Principles of Implant Dentistr in The Esthetic Zone: Michael Sonick, DMD Debb Hwang, DMDVikas Aggarwal100% (1)
- Crown Lenghtening - Gummy Smile PDFDocumento13 páginasCrown Lenghtening - Gummy Smile PDFVladislava GanevaAinda não há avaliações
- Surgical Vs Non-Surgical Approach in PeriodonticsDocumento13 páginasSurgical Vs Non-Surgical Approach in PeriodonticsBea DominguezAinda não há avaliações
- Bonnick - 2011 - Dental Clinics of North America PDFDocumento14 páginasBonnick - 2011 - Dental Clinics of North America PDFKranti PrajapatiAinda não há avaliações
- Prolonged Retention, Ankylosis and Infraocclusion of Deciduous Teeth Ok OkDocumento5 páginasProlonged Retention, Ankylosis and Infraocclusion of Deciduous Teeth Ok OkRahulLife'sAinda não há avaliações
- RecessionsDocumento68 páginasRecessionsmaryamAinda não há avaliações
- AI Systematic ReviewDocumento15 páginasAI Systematic Reviewsunk86Ainda não há avaliações
- Jung 2018Documento11 páginasJung 2018Sebastien MelloulAinda não há avaliações
- Advances in Extraction TechniquesDocumento13 páginasAdvances in Extraction TechniquesashajangamAinda não há avaliações
- Single Flap Approach With and Without Guided TissueDocumento21 páginasSingle Flap Approach With and Without Guided TissuekarthikAinda não há avaliações
- Mucogingival Conditions in The Natural DentitionDocumento10 páginasMucogingival Conditions in The Natural DentitionMartty BaAinda não há avaliações
- 2015 Kin JIACD - Sticky Bone - Sohn Et Al PDFDocumento20 páginas2015 Kin JIACD - Sticky Bone - Sohn Et Al PDFOscar CabreraAinda não há avaliações
- ImplantDocumento4 páginasImplantSaraAinda não há avaliações
- Tooth Wear An Authoritative Reference For Dental Professionals and Students (Andrew Eder, Maurice Faigenblum, (Eds.) ) (Z-Library)Documento313 páginasTooth Wear An Authoritative Reference For Dental Professionals and Students (Andrew Eder, Maurice Faigenblum, (Eds.) ) (Z-Library)Diego DuranAinda não há avaliações
- Sling and Tag Suturing Technique For Coronally Advanced FlapDocumento7 páginasSling and Tag Suturing Technique For Coronally Advanced FlapFerdinan Pasaribu0% (1)
- The International Journal of Periodontics & Restorative DentistryDocumento10 páginasThe International Journal of Periodontics & Restorative DentistryViorel FaneaAinda não há avaliações
- Implant Occlusion Articles AbstractDocumento4 páginasImplant Occlusion Articles AbstractMrunal DoiphodeAinda não há avaliações
- Implant Thread Designs: An Overview: July 2017Documento10 páginasImplant Thread Designs: An Overview: July 2017Seno FauziAinda não há avaliações
- "Sandwich" Bone Augmentation Technique-Rationale and Report of Pilot Cases PDFDocumento14 páginas"Sandwich" Bone Augmentation Technique-Rationale and Report of Pilot Cases PDFHector MurilloAinda não há avaliações
- Splinting Journal PDFDocumento7 páginasSplinting Journal PDFhanataniarAinda não há avaliações
- Advanced Zygomatic Implants - The ZAGA Concept222222222222Documento354 páginasAdvanced Zygomatic Implants - The ZAGA Concept222222222222Софія БунчужнаAinda não há avaliações
- Catherine A. Hebert, D.D.S .: Internal Vs External ResorptionDocumento2 páginasCatherine A. Hebert, D.D.S .: Internal Vs External ResorptionJames OnealAinda não há avaliações
- 2 Extracted Pages From Anna B. Fuks, Benjamin Peretz Eds. Pediatric Endodontics Current Concepts in Pulp Therapy For Primary and Young Permanent TeethDocumento22 páginas2 Extracted Pages From Anna B. Fuks, Benjamin Peretz Eds. Pediatric Endodontics Current Concepts in Pulp Therapy For Primary and Young Permanent TeethMona CameliaAinda não há avaliações
- Preprosthetic and Reconstructive SurgeryDocumento32 páginasPreprosthetic and Reconstructive Surgeryruoiconmapu100% (1)
- Cairo Clasificaion ResecionDocumento7 páginasCairo Clasificaion ResecionMartty BaAinda não há avaliações
- Classification of Periodontal Diseases and Conditions 2018Documento15 páginasClassification of Periodontal Diseases and Conditions 2018Jean DatorAinda não há avaliações
- Guidelines BookDocumento16 páginasGuidelines BookAdel ElaroudAinda não há avaliações
- Athraa A. Mahmood M.Sc. of Periodontics: Prepared byDocumento22 páginasAthraa A. Mahmood M.Sc. of Periodontics: Prepared byheycoolalexAinda não há avaliações
- 7 Principles of Uncomplicated ExodontiaDocumento43 páginas7 Principles of Uncomplicated Exodontiaray774432Ainda não há avaliações
- Nine Steps To Occlusal Harmony FamdentDocumento5 páginasNine Steps To Occlusal Harmony FamdentGhenciu Violeta100% (1)
- The Key To Profound Local Anesthesia: NeuroanatomyDocumento8 páginasThe Key To Profound Local Anesthesia: NeuroanatomyRavik FidayatikaAinda não há avaliações
- Article 009Documento9 páginasArticle 009MedstudAinda não há avaliações
- Open Drainage or NotDocumento6 páginasOpen Drainage or Notjesuscomingsoon2005_Ainda não há avaliações
- New Microsoft Office Word DocumentDocumento3 páginasNew Microsoft Office Word DocumentAtulsanapAinda não há avaliações
- Implant-Related Complications and FailuresDocumento91 páginasImplant-Related Complications and FailuresSaman MohammadzadehAinda não há avaliações
- Beggs HocevarDocumento11 páginasBeggs HocevarAmanjot Bajwa100% (1)
- Zygoma ImplantDocumento63 páginasZygoma ImplantKristina Robles100% (2)
- CM 89 279Documento8 páginasCM 89 279Rebin AliAinda não há avaliações
- Analysis of Lingual en Masse Retraction CombiningDocumento9 páginasAnalysis of Lingual en Masse Retraction Combiningandres belloAinda não há avaliações
- Esthetic in Complete DentureDocumento14 páginasEsthetic in Complete DentureNidhi KatochAinda não há avaliações
- Intaglio JPDDocumento7 páginasIntaglio JPDEddie Ojeda HoffmannAinda não há avaliações
- Historical Interest of Denture Base Materials: Dr.M.Vasantha Kumar, DR - Swati Bhagath, Dr.J.Brintha JeiDocumento3 páginasHistorical Interest of Denture Base Materials: Dr.M.Vasantha Kumar, DR - Swati Bhagath, Dr.J.Brintha Jeiஹரி ராமச்சந்திரன்Ainda não há avaliações
- Clinical EndodonticsDocumento30 páginasClinical EndodonticsJemmy WendyAinda não há avaliações
- Daftar Pustaka - 66Documento2 páginasDaftar Pustaka - 66Rosa DelimaAinda não há avaliações
- Case Presentation: Department of Pediatric Dentistry Ziauddin UniversityDocumento10 páginasCase Presentation: Department of Pediatric Dentistry Ziauddin UniversitySaadia ShaikhAinda não há avaliações
- Knowledge and Awareness of Orthodontic Mini Screws Among Dental Students in Saudi Arabia: A Cross Sectional StudyDocumento11 páginasKnowledge and Awareness of Orthodontic Mini Screws Among Dental Students in Saudi Arabia: A Cross Sectional Studybefiyiw478Ainda não há avaliações
- Temporary Splinting.: Accomplished: Leonte Daniela, S1904Documento15 páginasTemporary Splinting.: Accomplished: Leonte Daniela, S1904Daniela LeonteAinda não há avaliações
- Smile Characteristics in Orthodontics: A Concept ReviewDocumento4 páginasSmile Characteristics in Orthodontics: A Concept Reviewjaganath venkatAinda não há avaliações
- Relacion Linea de Terminacion y Ajuste Marginal.Documento7 páginasRelacion Linea de Terminacion y Ajuste Marginal.Emmanuel Doroteo NuñezAinda não há avaliações
- Hawley With Anterior Bite PlateDocumento3 páginasHawley With Anterior Bite PlateClaudia Gamboa FerrerAinda não há avaliações
- Ricketts Visual Treatment Objective & Superimposition - ViksDocumento25 páginasRicketts Visual Treatment Objective & Superimposition - ViksAnonymous kqVtRS100% (1)
- Topical FluorideDocumento106 páginasTopical FluorideSanthoshi Reddy100% (1)
- DENT - 336 SyllabusDocumento7 páginasDENT - 336 Syllabusبراءة أحمد السلاماتAinda não há avaliações
- Syllabus JKSSB Junior Dental TechnicianDocumento6 páginasSyllabus JKSSB Junior Dental TechnicianAshyana SaeedAinda não há avaliações
- Pricelist Dentistry Mei'2018Documento26 páginasPricelist Dentistry Mei'2018Mirza AryantoAinda não há avaliações
- Smartclip SystemDocumento32 páginasSmartclip SystemSandeep NayakAinda não há avaliações
- Precision AttachmentsDocumento92 páginasPrecision AttachmentsRohan Grover100% (3)
- Condylar SagDocumento8 páginasCondylar Sagshreya dasAinda não há avaliações
- Bleaching: Bleaching and Its Relevance To Esthetic DentistryDocumento64 páginasBleaching: Bleaching and Its Relevance To Esthetic DentistryValentina BadiuAinda não há avaliações
- Subiecte An V OrtoDocumento70 páginasSubiecte An V OrtoTanya HernandezAinda não há avaliações
- Assignment 1 - PicoDocumento12 páginasAssignment 1 - Picoapi-596913754Ainda não há avaliações
- Natal Teeth: Case Report and Review of LiteratureDocumento7 páginasNatal Teeth: Case Report and Review of LiteratureElisabeth FransiskaAinda não há avaliações