Escolar Documentos
Profissional Documentos
Cultura Documentos
Research Papers
Enviado por
Cassie E. Zerna0 notas0% acharam este documento útil (0 voto)
36 visualizações21 páginas:)
Título original
Research papers
Direitos autorais
© © All Rights Reserved
Formatos disponíveis
DOCX, PDF, TXT ou leia online no Scribd
Compartilhar este documento
Compartilhar ou incorporar documento
Você considera este documento útil?
Este conteúdo é inapropriado?
Denunciar este documento:)
Direitos autorais:
© All Rights Reserved
Formatos disponíveis
Baixe no formato DOCX, PDF, TXT ou leia online no Scribd
0 notas0% acharam este documento útil (0 voto)
36 visualizações21 páginasResearch Papers
Enviado por
Cassie E. Zerna:)
Direitos autorais:
© All Rights Reserved
Formatos disponíveis
Baixe no formato DOCX, PDF, TXT ou leia online no Scribd
Você está na página 1de 21
Lung Cancer: How does it develop, attack and affect humans?
Mark Anthony C. Dizon
Content
Organization
Technicalities
Total 100%
Mrs. Lilia P. Angub
English IV-Del Pilar
Dizon, 2
Dizon, 3
Dizon, 4
Dizon, 5
Lung cancer is the uncontrolled growth of abnormal cells that start off in one or both
lungs; usually in the cells that line the air passages. The abnormal cells do not develop into
healthy lung tissue, they divide rapidly and form tumors. As tumors become larger and more
numerous, they undermine the lungs ability to provide the bloodstream with oxygen.
(medicalnewstoday.com)
Lung cancer was uncommon before the advent of cigarette smoking; it was not even
recognized as a distinct disease until 1761. Different aspects of lung cancer were described
further in 1810. Malignant lung tumors made up only 1% of all cancers seen at autopsy in 1878,
but had risen to 1015% by the early 1900s. Case reports in the medical literature numbered only
374 worldwide in 1912, but a review of autopsies showed the incidence of lung cancer had
increased from 0.3% in 1852 to 5.66% in 1952. In Germany in 1929, physician Fritz Lickint
recognized the link between smoking and lung cancer, which led to an aggressive antismoking
campaign. The British Doctors Study, published in the 1950s, was the first solid epidemiological
evidence of the link between lung cancer and smoking.As a result, in 1964 the Surgeon General
of the United States recommended smokers should stop smoking. The connection with radon gas
was first recognized among miners in the Ore Mountains near Schneeberg, Saxony. Silver has
been mined there since 1470, and these mines are rich in uranium, with its accompanying radium
and radon gas. Miners developed a disproportionate amount of lung disease, eventually
recognized as lung cancer in the 1870s. Despite this discovery, mining continued into the 1950s,
due to the USSR's demand for uranium. Radon was confirmed as a cause of lung cancer in the
1960s. The first successful pneumonectomy for lung cancer was performed in 1933.
Palliative
radiotherapy has been used since the 1940s. Radical radiotherapy, initially used in the 1950s,
Dizon, 6
was an attempt to use larger radiation doses in patients with relatively early-stage lung cancer,
but who were otherwise unfit for surgery. In 1997, continuous hyperfractionated accelerated
radiotherapy was seen as an improvement over conventional radical radiotherapy. With small
cell lung carcinoma, initial attempts in the 1960s at surgical resection and radical radiotherapy
were unsuccessful. In the 1970s, successful chemotherapy regimens were developed.
(Wikipedia.org)
What are the symptoms of lung cancer? Symptoms of lung cancer are varied depending
upon where and how widespread the tumor is. Warning signs of lung cancer are not always
present or easy to identify. Lung cancer may not cause pain or even any symptoms at all in some
cases. A person with lung cancer may have the following kinds of symptoms: 1) No symptoms:
In up to 25% of people who get lung cancer, the cancer is first discovered on a routine chest X
ray or CT scan as a solitary small mass sometimes called a coin lesion, since on a two-
dimensional X-ray or CT scan, the round tumor looks like a coin. These patients with small,
single masses often report no symptoms at the time the cancer is discovered. 2) Symptoms
related to the cancer: The growth of the cancer and invasion of lung tissues and surrounding
tissue may interfere with breathing, leading to symptoms such as cough, shortness of breath,
wheezing, chest pain, and coughing up blood. If the cancer has invaded nerves, for example, it
may cause shoulder pain that travels down the outside of the arm or paralysis of the vocal cords
leading to hoarseness. Invasion of the esophagus may lead to difficulty swallowing. If a large
airway is obstructed, collapse of a portion of the lung may occur and cause infections (abscesses,
pneumonia) in the obstructed area. 3) Symptoms related to metastasis: Lung cancer that has
spread to the bones may produce excruciating pain at the sites of bone involvement. Cancer that
Dizon, 7
has spread to the brain may cause a number of neurologic symptoms that may include blurred
vision, headaches, seizures, or symptoms of stroke such as weakness or loss of sensation in parts
of the body. 4) Paraneoplastic symptoms: Lung cancers frequently are accompanied by
symptoms that result from production of hormone-like substances by the tumor cells. These
paraneoplastic syndromes occur most commonly with SCLC but may be seen with any tumor
type. A common paraneoplastic syndrome associated with SCLC is the production of a hormone
called adrenocorticotrophic hormone by the cancer cells, leading to oversecretion of the hormone
cortisol by the adrenal glands. The most frequent paraneoplastic syndrome seen with NSCLC is
the production of a substance similar to parathyroid hormone, resulting in elevated levels of
calcium in the bloodstream. 5) Nonspecific symptoms: Nonspecific symptoms seen with many
cancers, including lung cancers, include weight loss, weakness, and fatigue. Psychological
symptoms such as depression and mood changes are also common. One should consult a health
care professional if he or she develops the symptoms associated with lung cancer, in particular, if
they have a new persistent cough or worsening of an existing cough, blood in the sputum,
persistent bronchitis or repeated respiratory infections, chest pain, unexplained weight loss
and/or fatigue, breathing difficulties such as shortness of breath or wheezing. (medicinenet.com)
How is lung cancer diagnosed? Physicians use information revealed by symptoms as well
as several other procedures in order to diagnose lung cancer. Common imaging techniques
include chest X-rays, bronchoscopy, CT scans, MRI scans, and PET scans. Physicians will also
conduct a physical examination, a chest examination, and an analysis of blood in the sputum. All
of these procedures are designed to detect where the tumor is located and what additional organs
may be affected by it. Although the above diagnostic techniques provided important information,
Dizon, 8
extracting cancer cells and looking at them under a microscope is the only absolute way to
diagnose lung cancer. This procedure is called a biopsy. If the biopsy confirms lung cancer, a
pathologist will determine whether it is non-small cell lung cancer or small cell lung cancer.
(medicalnewstoday.com)
A chest x-ray is usually the first test performed to evaluate any concerns based on a
careful history and physical. (about.com) The majority of lung cancers are discovered after a
patient goes to see their family physician with one or more of the symptoms mentioned. In the
presence of such symptoms, particularly in smokers, a chest X-ray is mandatory. If the X-rays
show either as an abnormal shadowing or an obvious mass that is regarded non-specific but
needs further investigation. You may be referred to a chest specialist, who may use a
bronchoscope to look for cancerous growths in your bronchi. (Manila Bulletin, 7) This may show
a mass in the lungs or enlarged lymph nodes. Sometimes the chest x-ray is normal, and further
tests are needed look for a suspected lung cancer. Even if a mass is found, these are not always
cancerous and further studies are needed. (about.com)
A CT scan is frequently the second step either to follow up on an abnormal chest x-ray
finding, or to evaluate troublesome symptoms in those with a normal chest x-ray. CT scanning
involves a series of x-rays that create a 3-dimensional view of the lungs. If the CT is abnormal,
the diagnosis of lung cancer still needs confirmation through a sample of tissue by one of the
procedures below. (about.com)
In some patients, MRI will be used to evaluate the possibility of lung cancer. This
procedure uses magnetism and does not involve radiation. Certain individuals, such as those
with metal implants should not have MRI scans. The technician will ask questions to make sure
Dizon, 9
these are not present. (about.com)
A PET scan uses radioactive material to create colorful 3-dimensional images of a region
of the body. This type of scan differs from the others in that it defines tumors that are actively
growing. As an addition to the other procedures, some researchers suggest that PET scanning
may detect tumors earlier, even before they are visible anatomically through other studies. After
a lung cancer is suspected based on imaging, a sample of tissue is required to confirm the
diagnosis and determine the type of cancer. Sputum cytology is the easiest way to do this, but its
use is limited to those tumors that extend into the airways. Sputum cytology is not always
accurate and can miss some cancer cells. In a bronchoscopy, a lung specialist inserts a tube into
the airways to visualize and take a sample of the tumor. This procedure is used when the tumor is
found in the large airways and can be reached by the scope. Patients are given anesthesia during
this procedure to minimize discomfort. With this procedure, a hollow needle is inserted through
the chest wall, usually guided by CT visualization, to take a sample of the tumor. This can be
performed for tumors that cannot be reached by bronchoscopy. Endobronchial ultrasound is a
relatively new technique for diagnosing lung cancer. During a bronchoscopy, physicians use an
ultrasound probe within the airway to examine the lungs and area between the lungs. When lung
cancer affects the periphery of the lungs, it can create a fluid builds up between the lungs and
the lung lining.With local anesthesia, a larger needle is inserted into the pleural space from
which either a diagnostic amount of fluid or a therapeutic amount of fluid is removed. This
procedure is done in the operating room under general anesthesia. A scope is inserted just above
the sternum, the region between the lungs to take tissue samples from lymph nodes. Lung cancer
most commonly spreads to the liver, the adrenal glands, the brain, and the bones. (about.com)
How is lung cancer classified? Lung cancers are classified according to histological type.
Dizon, 10
This classification is important for determining management and predicting outcomes of the
disease. The vast majority of lung cancers are carcinomasmalignancies that arise from
epithelial cells. Lung carcinomas are categorized by the size and appearance of the malignant
cells seen by a histopathologist under a microscope. The two broad classes are non-small-cell
and small-cell lung carcinoma. The three main subtypes of NSCLC are adenocarcinoma,
squamous-cell lung carcinoma, and large-cell lung carcinoma. Nearly 40% of lung cancers are
adenocarcinoma, which usually originates in peripheral lung tissue.
Most cases of
adenocarcinoma are associated with smoking; however, among people who have smoked fewer
than 100 cigarettes in their lifetimes, adenocarcinoma is the most common form of lung cancer.
A subtype of adenocarcinoma, the bronchioloalveolar carcinoma, is more common in female
never-smokers, and may have a better long term survival. Squamous-cell carcinoma accounts for
about 30% of lung cancers. They typically occur close to large airways. A hollow cavity and
associated cell death are commonly found at the center of the tumor.About 9% of lung cancers
are large-cell carcinoma. These are so named because the cancer cells are large, with excess
cytoplasm, large nuclei and conspicuous nucleoli. In small-cell lung carcinoma, the cells
contain dense neurosecretory granules, which give this tumor an endocrine/paraneoplastic
syndrome association. Most cases arise in the larger airways (primary and secondary
bronchi).These cancers grow quickly and spread early in the course of the disease. Sixty to
seventy percent have metastatic disease at presentation. This type of lung cancer is strongly
associated with smoking. (wikipedia.org)
After a diagnosis is made, an oncologist will determine the stage of the cancer by finding
out how far the cancer has spread. Lung cancer staging is an assessment of the degree of spread
of the cancer from its original source. (wikipedia.org) It is one of the factors affecting the
Dizon, 11
prognosis and potential treatment of lung cancer.The stage determines which choices will be
available for treatment and informs prognosis. The most common cancer staging method is
called the TNM system. T (1-4) indicates the size and direct extent of the primary tumor, N (0-3)
indicates the degree to which the cancer has spread to nearby lymph nodes, and M (0-1)
indicates whether the cancer has metastasized to other organs in the body. A small tumor that
has not spread to lymph nodes or distant organs may be staged as (T1, N0, M0), for example.
For non-small cell lung cancer, TNM descriptions lead to a simpler categorization of stages.
These stages are labeled from I to IV, where lower numbers indicate earlier stages where the
cancer has spread less. Stage I is when the tumor is found only in one lung and in no lymph
nodes. Stage II is when the cancer has spread to the lymph nodes surrounding the infected lung.
Stage IIIa is when the cancer has spread to lymph nodes around the trachea, chest wall, and
diaphragm, on the same side as the infected lung. Stage III is when the cancer has spread to
lymph nodes on the other lung or in the neck. Stage IV is when the cancer has spread throughout
the rest of the body and other parts of the lungs. Small cell lung cancer has two stages: limited
or extensive. In the limited stage, the tumor exists in one lung and in nearby lymph nodes. In the
extensive stage, the tumor has infected the other lung as well as other organs in the body.
(medicalnewstoday.com)
What are the causes of lung cancer? Cigarette smoking is the main cause of about 90
percent of lung cancer cases in men and about 70 percent of them in women. The number of
women that are diagnosed with lung cancer is rising. This is due to increasing numbers of
women in smoking. (Manila Bulletin, 4)
As almost everyone knows, cigarette smoking is the major cause of lung cancer being
Dizon, 12
implicated in about 90 per cent of cases. The more a person smokes, and the longer they smoke,
the greater the risk. There is an average lag period of 20 years between exposure to smoke and
the development of lung cancer, which is why it is an uncommon diagnosis in people under 40.
Lung cancer is more common in people over the age of 50. Men are more likely to get lung
cancer than women, which simply reflects the fact that historically, men have smoked more than
women. However, lung cancer rates in women are rising because of higher rates of smoking
amongst women over the past few decades. In addition, there is also an increase in lung cancer in
non-smoking Asian women. The cause for this increase is unclear but may include both genetic
and environmental factors. Smoke in the environment is another cause of lung cancer. Inhaling
carcinogens in a workplace over long periods of time, is another cause; so is repeated exposure
of the lungs to radiation. (abc.net.au)
The incidence of lung cancer is strongly correlated with cigarette smoking, with about
90% of lung cancers arising as a result of tobacco use. The risk of lung cancer increases with the
number of cigarettes smoked and the time over which smoking has occurred; doctors refer to this
risk in terms of pack-years of smoking history. For example, a person who has smoked two
packs of cigarettes per day for 10 years has a 20 pack-year smoking history. While the risk of
lung cancer is increased with even a 10-pack-year smoking history, those with 30-pack-year
histories or more are considered to have the greatest risk for the development of lung cancer.
Among those who smoke two or more packs of cigarettes per day, one in seven will die of lung
cancer. Pipe and cigar smoking also can cause lung cancer, although the risk is not as high as
with cigarette smoking. Thus, while someone who smokes one pack of cigarettes per day has a
risk for the development of lung cancer that is 25 times higher than a nonsmoker, pipe and cigar
Dizon, 13
smokers have a risk of lung cancer that is about five times that of a nonsmoker. Tobacco smoke
contains over 4,000 chemical compounds, many of which have been shown to be cancer-causing
or carcinogenic. The two primary carcinogens in tobacco smoke are chemicals known as
nitrosamines and polycyclic aromatic hydrocarbons. The risk of developing lung cancer
decreases each year following smoking cessation as normal cells grow and replace damaged cells
in the lung. In former smokers, the risk of developing lung cancer begins to approach that of a
nonsmoker about 15 years after cessation of smoking. Passive smoking or the inhalation of
tobacco smoke by nonsmokers who share living or working quarters with smokers, also is an
established risk factor for the development of lung cancer. Research has shown that nonsmokers
who reside with a smoker have a 24% increase in risk for developing lung cancer when
compared with nonsmokers who do not reside with a smoker. The risk appears to increase with
the degree of exposure, number of years exposed and number of cigarettes smoked by the
household partner. An estimated 3,000 lung cancer deaths that occur each year in the U.S. are
attributable to passive smoking. (webmd.com)
Radon gas is also a cause of lung cancer. It is a natural, chemically inert gas that is a
natural decay product of uranium. It decays to form products that emit a type of ionizing
radiation. Radon gas is a known cause of lung cancer, with an estimated 12% of lung cancer
deaths attributable to radon gas, or 15,000 to 22,000 lung cancer-related deaths annually in the
U.S. As with asbestos exposure, concomitant smoking greatly increases the risk of lung cancer
with radon exposure. Radon gas can travel up through soil and enter homes through gaps in the
foundation, pipes, drains, or other openings. The U.S. Environmental Protection Agency
estimates that one out of every 15 homes in the U.S. contains dangerous levels of radon gas.
Radon gas is invisible and odorless, but can be detected with simple test kits. (webmd.com)
Dizon, 14
Another cause is the Asbestos fibers, which are silicate fibers that can persist for a
lifetime in lung tissue following exposure to asbestos. The workplace is a common source of
exposure to asbestos fibers, as asbestos was widely used in the past for both thermal and acoustic
insulation materials. Today, asbestos use is limited or banned in many countries including the
Unites States. Both lung cancer and mesothelioma which is a type of cancer of the pleura or of
the lining of the abdominal cavity called the peritoneum are associated with exposure to
asbestos. Cigarette smoking drastically increases the chance of developing an asbestos-related
lung cancer in exposed workers. Asbestos workers who do not smoke have a fivefold greater risk
of developing lung cancer than non-smokers, and those asbestos workers who smoke have a risk
that is 50 to 90 times greater than non-smokers. (webmd.com)
While the majority of lung cancers are associated with tobacco smoking, the fact that not
all smokers eventually develop lung cancer suggests that other factors, such as individual genetic
susceptibility, may play a role in the causation of lung cancer. Numerous studies have shown that
lung cancer is more likely to occur in both smoking and non-smoking relatives of those who
have had lung cancer than in the general population. Recent research has localized a region on
the long arm of the human chromosome number 6 that is likely to contain a gene that confers
an increased susceptibility to the development of lung cancer in smokers. The presence of certain
diseases of the lung, notably chronic obstructive pulmonary disease, is associated with a
slightly increased risk for the development of lung cancer even after the effects of concomitant
cigarette smoking are excluded. Survivors of lung cancer have a greater risk than the general
population of developing a second lung cancer. Survivors of non-small cell lung cancers have an
additive risk of 1-2% per year for developing a second lung cancer. In survivors of small cell
Dizon, 15
lung cancers the risk for development of second cancers approaches 6% per year. Air pollution,
from vehicles, industry, and power plants, can raise the likelihood of developing lung cancer in
exposed individuals. Up to 1% of lung cancer deaths are attributable to breathing polluted air,
and experts believe that prolonged exposure to highly polluted air can carry a risk similar to that
of passive smoking for the development of lung cancer. (webmd.com)
The treatment of lung cancer depends upon the type of tumor, the stage of the disease at
diagnosis and the general fitness of the patient. If the tumor is small and there is no evidence of
spread to local lymph nodes, surgical removal of the tumor is usually performed. Chemotherapy
is used in all other stages, and roughly 75 percent of tumors will respond to it. In patients who
decline operation, or who are not fit for surgery but have stage I, II, IIIA disease, high dose
radiotherapy is the treatment of choice. It involves bombarding the lung tumor with high-dose
radiation aiming to kill all the cancer cells. (Manila Bulletin, 9)
The patient and the doctor choose a cancer treatment plan based on a number of factors,
such as your overall health, the type and stage of your cancer, and your preferences. Options
typically include one or more treatments, including surgery, chemotherapy, radiation therapy or
targeted drug therapy. In some cases, the patient may choose not to undergo treatment. For
instance, the patient may feel that the side effects of treatment will outweigh the potential
benefits. When that's the case, the doctor may suggest comfort care to treat only the symptoms
the cancer is causing, such as pain or shortness of breath.
Treatment options for non-small cell lung cancers
Stage Common options
I Surgery, sometimes chemotherapy
Dizon, 16
II Surgery, chemotherapy, radiation
III
Combined chemotherapy and radiation, chemotherapy alone, sometimes surgery based on
results of other treatments
IV Chemotherapy, targeted drug therapy, clinical trials, supportive care
Treatment options for small cell lung cancers
Stage Common options
I Surgery when possible, but usually combined chemotherapy and radiation
II Combined chemotherapy and radiation
III Combined chemotherapy and radiation, clinical trials, supportive care
IV Chemotherapy, clinical trials, supportive care
During surgery, the surgeon works to remove the lung cancer and a margin of healthy
tissue. Procedures to remove lung cancer include wedge resection to remove a small section of
lung that contains the tumor along with a margin of healthy tissue; segmental resection to
remove a larger portion of lung, but not an entire lobe; lobectomy to remove the entire lobe of
one lung; pneumonectomy to remove an entire lung. If one undergoes surgery, the urgeon may
also remove lymph nodes from the patients chest in order to check them for signs of cancer.
Lung cancer surgery carries risks, including bleeding and infection. Expect to feel short of breath
after lung surgery. If a portion of the lung is removed, the remaining lung tissue will expand over
time and make it easier to breathe. The doctor may recommend a respiratory therapist who can
guide the patients through breathing exercises to aid in your recovery. (mayoclinic.com)
Chemotherapy uses drugs to kill cancer cells. One or more chemotherapy drugs may be
given through a vein in ones arm or taken orally. A combination of drugs usually is given in a
series of treatments over a period of weeks or months, with breaks in between so that the patient
can recover. Chemotherapy can be used as a first line treatment for lung cancer or as additional
treatment after surgery. In some cases, chemotherapy can be used to lessen side effects of cancer.
Dizon, 17
(mayoclinic.com)
Radiation therapy uses high-powered energy beams, such as X-rays, to kill cancer cells.
Radiation therapy can be directed at your lung cancer from outside your body or it can be put
inside needles, seeds or catheters and placed inside your body near the cancer. Radiation therapy
can be used alone or with other lung cancer treatments. Sometimes it's administered at the same
time as chemotherapy. For people with lung cancers that are very small, one option may be
stereotactic body radiotherapy. This form of radiation aims many beams of radiation from
different angles at the lung cancer. Stereotactic body radiotherapy treatment is typically
completed in one or a few treatments. In certain cases, it may be used in place of surgery for
small tumors. (mayoclinic.com)
Cancer survival rates or survival statistics tell you the percentage of people who survive a
certain type of cancer for a specific amount of time. Cancer statistics often use an overall five-
year survival rate. For instance, the overall five-year survival rate for bladder cancer is 80
percent. That means that of all people diagnosed with bladder cancer, 80 of every 100 were
living five years after diagnosis. Conversely, 20 out of every 100 died within five years of a
bladder cancer diagnosis. Cancer survival rates are based on research that comes from
information gathered on hundreds or thousands of people with a specific cancer. An overall
survival rate includes people of all ages and health conditions who have been diagnosed with
your cancer, including those diagnosed very early and those diagnosed very late.
(mayoclinic.com)
Dizon, 18
Lung cancer survival rates are a measure of how many people remain alive with lung
cancer after a certain amount of time. For example, a 5-year survival rate of 40% for a condition,
would mean that 40% of people, or 40 out of 100 people, would be alive after 5 years. When
talking about lung cancer, physicians often use the term median survival as well. Median
survival is the amount of time at which 50% of people with a condition will have died, and 50%
are still alive. Lung cancer survival rates are statistics and don't necessarily give an accurate
estimate of how long an individual will survive with a certain disease. There are many factors
that affect lung cancer survival rates, including general health, sex, race, treatments used, and in
the case of people who smoke, if they are able to quit. (about.com)
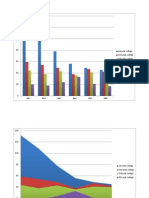
Survival rates for lung cancer vary depending on the type of cancer diagnosed and how
early in progression the illness is diagnosed. Estimated overall survival rate for all lung cancer
patients (regardless of cancer type and cancer stage) are estimated at:
Survival Time after Diagnosis
Years after Diagnosis Survival Rates
5 15%
10 5%
By the stage of cancer at diagnosis, survival rates are estimated at:
Survival Rate by Stage of Cancer at Diagnosis
Stage Survival Rates
Stage 0 70-80%
Stage I 50%
Dizon, 19
Stage II 30%
Stage III 15%
Stage IV Less than 2%
In general, patients diagnosed with non-small cell lung cancer have a better prognosis
than those diagnosed with the more aggressive small cell lung cancer. NSCLC accounts
for roughly 85 percent of all lung cancer cases. The 5-year survival rates for NSCLC are
estimated at:
Five Year Survival Rates for NSCLC Patients
Stage Survival Rates
Stage IA 49%
Stage IB 45%
Stage IIA 30%
Stage IIB 31%
Stage IIIA 14%
Stage IIIB 5% (median survival of 13 months)
Stage IV 1% (median survival of eight months)
In comparison, the overall 5-year survival rate for individuals diagnosed with small cell lung
cancer is estimated at about six percent. With treatment, the median survival time for SCLC
patients is listed at six to 12 months. Patients diagnosed in the earlier limited stage tend to have a
better prognosis. (lung-cancer.com)
The overall 5-year survival rate for small cell lung cancer (limited and extensive) is only
about 6%. The overall 5-year survival rate for non-small cell lung cancer is roughly 15%. The
survival rate with BAC is significantly better than with other forms of non-small cell lung
Dizon, 20
cancer, especially when it is caught early and only one tumor is present. In one study, those who
were diagnosed with BAC and had tumors less than 3 centimeters in diameter, had a 5-year
survival rate of 100% with surgery. The 5-year survival rate for stage 3 and 4 disease is roughly
60%. As mentioned above, survival rates do not reflect differences in individuals. In addition,
keep in mind that not everyone with a particular stage of lung cancer has the same prognosis.
Staging lung cancer can help guide treatment, but there is a wide spectrum of cancers within
each stage. The overall 5-year survival rate for stage 1 lung cancer is 60-80%. The overall
survival rate with stage 2 lung cancer is 40-50%. The overall survival rate for stage 3A lung
cancer is 23%, but this varies widely among different cancers that are classified as stage 3A. The
5-year survival rate with stage 3B lung cancer is only 10%. The median survival time with
treatment is 13 months. The overall 5-year survival rate with stage 4 lung cancer is sadly less
than 10%. The median survival time is about 8 months. The overall 5-year survival rate for both
stages of small cell lung cancer combined is only about 6%. The overall 5-year survival rate for
both stages of small cell lung cancer combined is about 6%. Without treatment, the average life
expectancy for extensive disease is 2 to 4 months, and with treatment is 6 to 12 months.
(about.com)
Dizon, 21
http://www.medicalnewstoday.com/info/lung-cancer/
http://en.wikipedia.org/wiki/Lung_cancer
http://lungcancer.about.com/od/diagnosisoflungcancer/a/diagnosislungca.htm
http://www.medicinenet.com/lung_cancer/page4.htm#what_are_lung_cancer_symptoms_and_signs
http://www.webmd.com/lung-cancer/guide/lung-cancer-causes?page=2
http://www.mayoclinic.com/health/lung-cancer/DS00038/DSECTION=treatments-and-drugs
http://lungcancer.about.com/od/whatislungcancer/a/lungcancersurvivalrates.htm
http://www.lung-cancer.com/lung-cancer-survival-rate.html
http://www.mayoclinic.com/health/cancer/CA00049
http://www.abc.net.au/health/library/stories/2010/07/29/2967396.htm
Você também pode gostar
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryNo EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryNota: 3.5 de 5 estrelas3.5/5 (231)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)No EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Nota: 4.5 de 5 estrelas4.5/5 (121)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaNo EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaNota: 4.5 de 5 estrelas4.5/5 (266)
- The Little Book of Hygge: Danish Secrets to Happy LivingNo EverandThe Little Book of Hygge: Danish Secrets to Happy LivingNota: 3.5 de 5 estrelas3.5/5 (399)
- Never Split the Difference: Negotiating As If Your Life Depended On ItNo EverandNever Split the Difference: Negotiating As If Your Life Depended On ItNota: 4.5 de 5 estrelas4.5/5 (838)
- The Emperor of All Maladies: A Biography of CancerNo EverandThe Emperor of All Maladies: A Biography of CancerNota: 4.5 de 5 estrelas4.5/5 (271)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeNo EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeNota: 4 de 5 estrelas4/5 (5794)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyNo EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyNota: 3.5 de 5 estrelas3.5/5 (2259)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersNo EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersNota: 4.5 de 5 estrelas4.5/5 (344)
- Team of Rivals: The Political Genius of Abraham LincolnNo EverandTeam of Rivals: The Political Genius of Abraham LincolnNota: 4.5 de 5 estrelas4.5/5 (234)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreNo EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreNota: 4 de 5 estrelas4/5 (1090)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceNo EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceNota: 4 de 5 estrelas4/5 (895)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureNo EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureNota: 4.5 de 5 estrelas4.5/5 (474)
- The Unwinding: An Inner History of the New AmericaNo EverandThe Unwinding: An Inner History of the New AmericaNota: 4 de 5 estrelas4/5 (45)
- The Yellow House: A Memoir (2019 National Book Award Winner)No EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Nota: 4 de 5 estrelas4/5 (98)
- Australian TaxationDocumento45 páginasAustralian TaxationEhtesham HaqueAinda não há avaliações
- Sales Order Process - Key Steps, Attributes and Concepts - v7Documento25 páginasSales Order Process - Key Steps, Attributes and Concepts - v7bob bluhmAinda não há avaliações
- Primary Health Care: Mr. John Michael M. Pitoy, B.S.N., R.NDocumento44 páginasPrimary Health Care: Mr. John Michael M. Pitoy, B.S.N., R.NJohn Michael Manlupig Pitoy100% (9)
- Northern NVProvider DirectoryDocumento82 páginasNorthern NVProvider DirectoryGuru NandeshwarAinda não há avaliações
- Comparitive Study of Pile Foundations With Foundations On Stone Column Treated Ground 170704090313Documento23 páginasComparitive Study of Pile Foundations With Foundations On Stone Column Treated Ground 170704090313anurag hazarikaAinda não há avaliações
- FPC Manual PreviewDocumento5 páginasFPC Manual PreviewIbrahim Levent AkkoyunluAinda não há avaliações
- Master Handover Rev 4-2013Documento8 páginasMaster Handover Rev 4-2013MeysamGholizadehAinda não há avaliações
- The Noble Cars (TNC), San Juan ST., Dumaguete City, Negros Oriental, PhilippinesDocumento3 páginasThe Noble Cars (TNC), San Juan ST., Dumaguete City, Negros Oriental, PhilippinesCassie E. ZernaAinda não há avaliações
- Autocad Interface Overview: The Ribbon The Menu Browser Steeringwheels InfocenterDocumento2 páginasAutocad Interface Overview: The Ribbon The Menu Browser Steeringwheels InfocenterCassie E. ZernaAinda não há avaliações
- Against The Death PenaltyDocumento3 páginasAgainst The Death PenaltyCassie E. ZernaAinda não há avaliações
- February 10Documento2 páginasFebruary 10Vanessa RamosAinda não há avaliações
- Acct. 121 (Tourism)Documento1 páginaAcct. 121 (Tourism)Cassie E. ZernaAinda não há avaliações
- Name: Job Title: Division / Unit: Start Date: Separation Date: Total Length of ServiceDocumento3 páginasName: Job Title: Division / Unit: Start Date: Separation Date: Total Length of ServiceCassie E. ZernaAinda não há avaliações
- Multi-Pressure SystemDocumento10 páginasMulti-Pressure SystemCassie E. ZernaAinda não há avaliações
- Factors of Disease CausationDocumento1 páginaFactors of Disease CausationCassie E. ZernaAinda não há avaliações
- Uniform Sizes For Scuaa 7 NorsuDocumento3 páginasUniform Sizes For Scuaa 7 NorsuCassie E. ZernaAinda não há avaliações
- PrintDocumento9 páginasPrintCassie E. ZernaAinda não há avaliações
- Against The Death PenaltyDocumento3 páginasAgainst The Death PenaltyCassie E. ZernaAinda não há avaliações
- P1-40 Combined Balance SheetDocumento4 páginasP1-40 Combined Balance SheetCassie E. ZernaAinda não há avaliações
- Factors of Disease CausationDocumento1 páginaFactors of Disease CausationCassie E. ZernaAinda não há avaliações
- GSISDocumento2 páginasGSISCassie E. ZernaAinda não há avaliações
- Bcs ResumeDocumento1 páginaBcs ResumeCassie E. ZernaAinda não há avaliações
- Letter OneDocumento1 páginaLetter OneCassie E. ZernaAinda não há avaliações
- PapiDocumento3 páginasPapiCassie E. ZernaAinda não há avaliações
- Nora'S Laundry Shop: DAILY TIME RECORD For The Month of August 2015Documento15 páginasNora'S Laundry Shop: DAILY TIME RECORD For The Month of August 2015Cassie E. ZernaAinda não há avaliações
- AutobiographyDocumento1 páginaAutobiographyCassie E. ZernaAinda não há avaliações
- Jikni J. Noble: Position Desired: Service CrewDocumento2 páginasJikni J. Noble: Position Desired: Service CrewCassie E. ZernaAinda não há avaliações
- GraphsDocumento5 páginasGraphsCassie E. ZernaAinda não há avaliações
- Diana Kristina Casandra E. Zerna: Presented ToDocumento1 páginaDiana Kristina Casandra E. Zerna: Presented ToCassie E. ZernaAinda não há avaliações
- Nora'S Laundry Shop: DAILY TIME RECORD For The Month of August 2015Documento15 páginasNora'S Laundry Shop: DAILY TIME RECORD For The Month of August 2015Cassie E. ZernaAinda não há avaliações
- GraphsDocumento5 páginasGraphsCassie E. ZernaAinda não há avaliações
- InsuranceDocumento2 páginasInsuranceCassie E. ZernaAinda não há avaliações
- Diana Kristina Casandra E. ZernaDocumento1 páginaDiana Kristina Casandra E. ZernaCassie E. ZernaAinda não há avaliações
- Jikni J. Noble: Submitted byDocumento1 páginaJikni J. Noble: Submitted byCassie E. ZernaAinda não há avaliações
- PolsciDocumento11 páginasPolsciCassie E. ZernaAinda não há avaliações
- The Following Are The Balances of Hercules Insurance CoDocumento1 páginaThe Following Are The Balances of Hercules Insurance CoCassie E. ZernaAinda não há avaliações
- Maria Janette Susan May Erames Zerna: Basic InformationDocumento1 páginaMaria Janette Susan May Erames Zerna: Basic InformationCassie E. ZernaAinda não há avaliações
- Acute GastroenteritisDocumento7 páginasAcute GastroenteritisCherr NollAinda não há avaliações
- Civil EngineeringDocumento13 páginasCivil EngineeringMahmoud OuryemchiAinda não há avaliações
- Measurement of Poverty and Poverty of Measurement: Martin GreeleyDocumento15 páginasMeasurement of Poverty and Poverty of Measurement: Martin GreeleyKule89Ainda não há avaliações
- HC-33 Maximum Moisture Hair Styling Gel PDFDocumento2 páginasHC-33 Maximum Moisture Hair Styling Gel PDFdianaAinda não há avaliações
- 2015 English Grade 7Documento16 páginas2015 English Grade 7AyushAinda não há avaliações
- 4 26 12Documento9 páginas4 26 12stevenscreekAinda não há avaliações
- Start A Quick Budget Start A Budget by MonthDocumento13 páginasStart A Quick Budget Start A Budget by MonthMichelle PadillaAinda não há avaliações
- Synergic Antiobesity Effects of Bitter Melon Water Extract and Platycodin-D in Genetically Obese MiceDocumento9 páginasSynergic Antiobesity Effects of Bitter Melon Water Extract and Platycodin-D in Genetically Obese Micegege wpAinda não há avaliações
- English The RainDocumento2 páginasEnglish The RainsmitaAinda não há avaliações
- Aigen Zhao, PHD, Pe, Gse Environmental, LLC, Usa Mark Harris, Gse Environmental, LLC, UsaDocumento41 páginasAigen Zhao, PHD, Pe, Gse Environmental, LLC, Usa Mark Harris, Gse Environmental, LLC, UsaCarlos Ttito TorresAinda não há avaliações
- Diesel Generator 350-To-500-Kw-Specs-SheetDocumento9 páginasDiesel Generator 350-To-500-Kw-Specs-SheetamrAinda não há avaliações
- Screw Take-Up Device Ur1 Ur7: Conveyor ComponentsDocumento1 páginaScrew Take-Up Device Ur1 Ur7: Conveyor ComponentsDxFxAinda não há avaliações
- Benign Prostate Hyperplasia 2Documento125 páginasBenign Prostate Hyperplasia 2Danieal NeymarAinda não há avaliações
- The Power of Urine PDFDocumento61 páginasThe Power of Urine PDFJohnSmith0488Ainda não há avaliações
- DeethanizeranalysisDocumento7 páginasDeethanizeranalysismindunder36Ainda não há avaliações
- Kf22Qt Sec4 FRDDocumento21 páginasKf22Qt Sec4 FRDMauro PerezAinda não há avaliações
- CH - 3 DrainageDocumento3 páginasCH - 3 DrainageVeena VermaAinda não há avaliações
- Hoja Tecnica IS 320.1 Zona 1Documento2 páginasHoja Tecnica IS 320.1 Zona 1susanivar adrianoAinda não há avaliações
- Hindustan Coca-Cola Beverages PVT LTD B-91 Mayapuri Industrial Area Phase-I New DelhiDocumento2 páginasHindustan Coca-Cola Beverages PVT LTD B-91 Mayapuri Industrial Area Phase-I New DelhiUtkarsh KadamAinda não há avaliações
- RNA and Protein Synthesis Problem SetDocumento6 páginasRNA and Protein Synthesis Problem Setpalms thatshatterAinda não há avaliações
- Cde-Class II Amalgam Restorations-31!12!14Documento36 páginasCde-Class II Amalgam Restorations-31!12!14Archita KureelAinda não há avaliações
- SWT Nedelka Cartagena enDocumento2 páginasSWT Nedelka Cartagena enChristian Lazo FerreyraAinda não há avaliações