Escolar Documentos
Profissional Documentos
Cultura Documentos
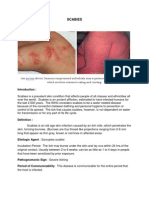
Paederus Dermatitis
Enviado por
ErynaDireitos autorais
Formatos disponíveis
Compartilhar este documento
Compartilhar ou incorporar documento
Você considera este documento útil?
Este conteúdo é inapropriado?
Denunciar este documentoDireitos autorais:
Formatos disponíveis
Paederus Dermatitis
Enviado por
ErynaDireitos autorais:
Formatos disponíveis
CMYK13
T
h
i
s
P
D
F
i
s
a
v
a
i
l
a
b
l
e
f
o
r
f
r
e
e
d
o
w
n
l
o
a
d
f
r
o
m
a
s
i
t
e
h
o
s
t
e
d
b
y
M
e
d
k
n
o
w
P
u
b
l
i
c
a
t
i
o
n
s
(
w
w
w
.
m
e
d
k
n
o
w
.
c
o
m
)
.
ReviewArticle
Paederus dermatitis Paederus dermatitis Paederus dermatitis Paederus dermatitis Paederus dermatitis
Gurcharan Si ngh, Syed Yousuf Al i Gurcharan Si ngh, Syed Yousuf Al i Gurcharan Si ngh, Syed Yousuf Al i Gurcharan Si ngh, Syed Yousuf Al i Gurcharan Si ngh, Syed Yousuf Al i
Department of Dermatology and STD, Sri Devaraj Urs Medical College, Kolar, Karnataka, India.
Address for correspondence: Dr. Gurcharan Singh, 108-A, Jal Vayu Vihar, Kammanhalli, Bangalore - 560043, India.
E-mail: drsinghgs@gmail.com
days to larvae and adults. Paederus beetles are beneficial to
agriculture because they eat crop pests.
[9]
Paederus dermatitis, also known as dermatitis linearis
[
]
or
blister beetle dermatitis
[
]
is a peculiar irritant contact
The species commonly causing Paederus dermatitis are Paederus
dermatitis characterized by erythematous and bullous lesions
melampus in India, Paederus brasilensis in South America,
of sudden onset on exposed areas of the body. The disease is
commonly known as podo, Paederus colombius in Venezuela,
provoked by an insect belonging to the genus Paederus. This
Paederus fusipes in Taiwan and Paederus peregrinus in Indonesia.
[13]
beetle does not bite or sting, but accidental brushing against
or crushing the beetle over the skin provokes the release of its
Paederus are nocturnal and attracted by incandescent and
coelomic fluid which contains paederin, a potent vesicant.
[3]
fluorescent lights and as a result, inadvertently come into contact
with humans.
[9]
Hemolymph of the beetle contains paederine
ETIOPATHOGENESIS
(latigaza)
[14]
which is released on crushing of the insect onto the
skin due to the reflex of brushing away the insect. Paederin
The genus Paederus belongs to family Staphyllinidae, order
(C
25
H
45
O
9
N) is an amide with two tetrahydropyran rings and makes
Coleoptae, class Insecta and consists of over 622 species which
up approximately 0.025% of an insects weight (for P. fusipes).
are distributed worldwide.
[2,4]
Paederus beetles have been
associated with outbreaks of dermatitis in various countries
Recently, it has been demonstrated that the production of
including Australia,
[5]
Malaysia,
[6]
Sri Lanka,
[7]
Nigeria,
[8]
Kenya,
paederin relies on the activities of an endosymbiont (Pseudomonas
Iran,
[2]
Central Africa, Uganda, Okinawa, Sierra Leone,
[9]
species) within Paederus. The manufacture of paederin is largely
Argentina, Brazil, France, Venezuela, Ecuador and India.
[10-12]
confined to adult female beetles. Larvae and males only store
paederin acquired maternally (i.e., through eggs) or by
Adults of these beetles are usually 7-10 mm long and 0.5 mm
ingestion.
[15]
It is a vesicant and blocks mitosis at levels as low as
wide, having the size around one and half times that of a
1 ng/ml apparently by inhibiting protein and DNA synthesis
INTRODUCTION
mosquito. They have a black head, lower abdomen and elytral
(this structure covers the wings and first three abdominal
segments) and a red thorax and upper abdomen.
[8,9]
Paederus
beetles live in moist habitats
[13]
and feed on debris. Although
these insects can fly, they prefer to run and are extremely
agile. They have a characteristic habit of curling up their
abdomen when they run or are disturbed and this habit allows
an on the spot identification on many occasions.
[4]
Eggs are
laid singly on a moist substance and typically develop in 3-19
without affecting RNA synthesis.
[9]
Acantholysis is probably
caused by the release of epidermal proteases.
[2]
CLINICAL FEATURES
The dermatitis may affect persons of either sex, all ages,
races or social conditions, since it depends on the patients
activities and insect habitat. The exposed areas are affected
with a greater frequency. The incidence of cases is reported to
How to cite this article: Singh G, Ali SY. Paederus dermatitis. Indian J Dermatol Venereol Leprol 2007;73:13-5.
Received: April, 2006. Accepted: September, 2006. Source of Support: Nil. Conflict of interest: None declared.
Indian J Dermatol Venereol Leprol|Januar y-Februar y 2007|Vol 73|Issue 1 13
14 CMYK
T
h
i
s
P
D
F
i
s
a
v
a
i
l
a
b
l
e
f
o
r
f
r
e
e
d
o
w
n
l
o
a
d
f
r
o
m
a
s
i
t
e
h
o
s
t
e
d
b
y
M
e
d
k
n
o
w
P
u
b
l
i
c
a
t
i
o
n
s
(
w
w
w
.
m
e
d
k
n
o
w
.
c
o
m
)
.
Singh G, et al.: Paederus dermatitis
be greater during the last quarter of the year, the period that
immediately follows the rainy season.
[4]
The lesions are
erythematous and edematous which may be linear, giving a
whiplash appearance. The vesicles generally appear towards
the center of the plaque. The vesicles turn into pustules quite
frequently. The signs appear after 24 to 48h of contact and
take a week or more to disappear.
[4,8]
A striking feature is the
presence of kissing lesions that occur whenever apposition
of damaged areas to previously intact skin is possible, e.g.,
flexure of the elbow, adjacent surfaces of the thighs.
[4]
Diffuse erythematous and desquamative lesions which
floor consists of the basal cell layer and sometimes one or
more strata of the malpighian layer. Inside the vesicle there
is fluid and a weft, formed by degenerated epithelial cells
( ghosts) . There i s al ways some admi xture of
polymorphonuclear cells. The basal cell layer may be intact
or indistinct and there may even be destruction of the
dermo-epidermal junction.
In the dermis there is a perivascular infiltrate, more marked in
the papillae and the upper reticular dermis. It consists mainly
of mononuclear cells, but some polymorphonuclear cells are
also present. There may be edema, more marked at the papillae.
predominantly occur on the upper body and face have been In the full blown pustular stage, the histopathological
reported and several possible causes for this atypical variant characteristics mentioned above are exaggerated. The vesicles
of paederus dermatitis
[2]
are: change into pustules, full of neutrophils, which are seen
Contact with a different species of Paederus. migrating through the neighboring areas of the epidermis as
Recurrent contact during a short period of time. well as the papillae. The perivascular infiltrate and the edema
The existence of underlying disorders such as atopic are more intense. The papillary edema may give a false
dermatitis. impression of a subepidermal vesicle.
The use of heavily infested natural source of water for
washing. During healing, the pustule is pushed upwards by maturing
An immunologic phenomenon resulting in an eczematized new keratinocytes and then may resemble the spongiform
reaction pattern. pustule of Kogoj. Finally, all that remain are crust, some
acanthosis and mild perivascular infiltrate.
[4]
Complications include postinflammatory hyperpigmentation,
secondary infections, and extensive exfoliating and ulcerating Direct immunofluorescence is negative for deposition of
dermatitis requiring hospitalization.
[2,5,9]
immunoglobulins (IgG, IgM and IgA) and C3.
[2]
Ocular and genital involvement is relatively common; it occurs DIFFERENTIAL DIAGNOSIS
secondary to transfer of the toxic chemical from elsewhere on
the skin by fingers. However, ocular area may be the only site Clinical appearance of paederus dermatitis may be confused with
of involvement. Ocular involvement usually presents with herpes simplex, herpes zoster, liquid burns, acute allergic or irritant
unilateral periorbital dermatitis, or keratoconjunctivitis, which contact dermatitis, millipede
has been named the Nairobi eye.
[2]
phytophotodermatitis.
[2]
The characteristic linear appearance of
the lesions, their predilection for exposed areas, the presence of
HISTOPATHOLOGY kissing lesions, the histopathology, appropriate patch test and
finally epidemiological features (occurrence of similar cases in a
1.
2.
3.
4.
5.
dermatitis and
Early lesions show neutrophilic spongiosis leading to vesiculation
and eventual reticular degeneration of the epidermis. This is
followed by confluent epidermal necrosis, usually with a
surviving layer of suprabasal cells. Scattered acantholytic cells
may be present. The large number of intraepidermal neutrophils,
combined with areas of confluent necrosis and reticular
degeneration, are characteristic. Older lesions show irregular
acanthosis and pallor of superficial keratinocytes, with overlying
parakeratotic scale containing a neutrophilic exudate.
[16]
In the early vesicular stage, there are intraepidermal
vesicles. The top of the vesicle is usually formed by the
horny layer or by one or two rows of flattened cells. The
given area, the seasonal incidence and identification of the insect)
should enable the clinician to arrive at the right diagnosis.
[4]
TREATMENT
The cases should be managed as irritant contact dermatitis
removal of irritant, initial washing with soap and water,
application of cold wet compresses followed by topical steroid
and antibiotic, if secondarily infected.
[9]
PREVENTION
Preventing human-beetle contact is the primary method of
Indian J Dermatol Venereol Leprol|Januar y-Februar y 2007|Vol 73|Issue 1 14
CMYK15
T
h
i
s
P
D
F
i
s
a
v
a
i
l
a
b
l
e
f
o
r
f
r
e
e
d
o
w
n
l
o
a
d
f
r
o
m
a
s
i
t
e
h
o
s
t
e
d
b
y
M
e
d
k
n
o
w
P
u
b
l
i
c
a
t
i
o
n
s
(
w
w
w
.
m
e
d
k
n
o
w
.
c
o
m
)
.
Singh G, et al.: Paederus dermatitis
preventing paederin-based trauma. Tactics that can be
employed to achieve this
[2,7]
include:
1. Learn to recognize paederus beetles and avoid handling
or crushing these insects against exposed areas of skin.
2. Keep doors closed and put screens on doors. Both doors
and windows should be kept in good repair to reduce the
entry of beetles into buildings.
3. Sleeping under a bed net, preferably permethrin-treated,
may also reduce the probability of a beetle falling on the
skin during the night.
4. A net or mesh can be tied under the lights to prevent the
beetle from dropping onto humans.
reference to the medical importance. J Egypt Soc Parasitol
1996;26:337-51.
2. Zargari O, Asadi AK, Fathalikhani F, Panahi M. Paederus
dermatitis in northern Iran: A report of 156 cases. Int J Dermatol
2003;42:608-12.
3. Gelmietti C, Grimalt R. Paederus dermatitis: An easy diagnosable
but misdiagnosed eruption. Eur J Pediatr 1993;153:6-8.
4. Vegas FK, Yahr MG, Venezuela C. Paederus dermatitis. Arch
Dermatol 1996;94:175-83.
5. Todd RE, Guthridge SL, Montgomery BL. Evacuation of an
Aboriginal community in response to an outbreak of blistering
dermatitis induced by a beetle (Paederus australis). Med J Aust
1996;164:238-40.
6. Mokhtar N, Singh R, Ghazali W. Paederus dermatitis among
5. Patients should be advised to avoid crushing the beetle on
medical students in USM, Kelatan. Med J Malaysia 1993;48:403-
the skin, manipulating primary lesions or rubbing the eyes
6.
following primary involvement. 7. Kamaladasa SD, Pereea WDH, Weeratunge L. An outbreak of
If a beetle lands on the skin, try to remove it gently (example:
Paederus dermatitis in a suburban hospital in Srilanka. Int J
blow it off, try to get the beetle to walk on to a piece of
Dermatol 1997;36:34-6.
8. George AO, Hart PD. Outbreak of Paederus dermatitis in
paper and then remove it). Wash contact areas of the skin.
southern Nigeria: Epidemiology and dermatology. Int J Dermatol
Check areas for beetles (especially on walls and ceiling
1990;29:500-1.
around the light) before going to bed. Beetle, if present,
9. Frank JH, Kanamitsu K. Paederus, sensu lato (Coleoptera:
should be killed by using insecticide (pyrethroid) followed
Staphylinidae): Natural history and medical importance. J Med
by sweeping up and removal of beetle carcasses. Entomol 1987;24:155-91.
Remember that beetles can cause symptoms, alive or dead
10. Handa F, Pradeep S, Sudarshan G. Beetle dermatitis in Punjab.
and hence avoid handling the beetle directly.
Indian J Dermatol Venerol Leprol 1985;51:208-12.
Clear excess vegetations from and around the residence,
11. Kalla G, Ashish B. Blister beetle dermatitis. Indian J Dermatol
Venerol Leprol 1997;62:267-8.
as beetles may rest in these areas.
12. Sujit SR, Koushik L. Blister beetle dermatitis in West Bengal.
Indian J Dermatol Venereol Leprol 1997;63:69-70.
13. Parasitic infestations stings and bites. In: Arnold HL, Odam RB,
James WD, editors. Andrews Diseases of the skin. 8
th
ed. WB
Paederus dermatitis is a common condition. We believe that
Saunders: Philadelphia; 1990. p. 486-533.
increased public awareness of this condition can decrease
14. Davalos AV. Epidemic dermatitis by paederus irritant in piura,
Peru at 1999, related to EI Nino Phenomenon. Rev Soc Bras
mucocutaneous exposure to paederin.
Med Trop 2002;35:23-8.
15. Piel J. Polyketide synthesis-peptide synthetase gene cluster
from an uncultured bacterial symbiont of paederus beetles.
PNAS 2002;99:14002-7.
Morsy TA, Arafa MA, Younis TA, Mahmoud IA. Studies on 16. Banney LA, Wood DJ, Francis GD. Whiplash rove beetle dermatitis
Paederus alfierii Koch (Coleoptera: Staphylinidae) with special in central Queensland. Aust J Dermatol 2000;41:162-7.
6.
7.
8.
CONCLUSION
REFERENCES
1.
Announcement
ContactandOccupationalDermatosesForumofIndia(CODFI)
FellowshipsandMembership
Applications are invited for CODFI fellowships at any one of the centers mentioned Sion Hospital, Mumbai; AIIMS, New
Delhi; PGIMER, Chandigarh; IAISD, Kolkatta. The period of fellowship is 4 weeks (Last date for application - 21
st
April
2007). Application forms and other details can be downloaded from our website www.codfi.org
Applications are also invited from members of IADVL to become members of the Contact and Occupational Dermatoses
Forum of India (CODFI). This membership offers you several advantages besides attending our annual workshop and
biennial conference CODFICON. For application forms and other details visit our website www.codfi.org
Send completed applications for fellowship and membership to Dr. Sanjeev Handa, Secretary CODFI, Department of
Dermatology, PGIMER, Chandigarh.
Indian J Dermatol Venereol Leprol|Januar y-Februar y 2007|Vol 73|Issue 1 15
Você também pode gostar
- Impetigo, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo EverandImpetigo, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNota: 5 de 5 estrelas5/5 (3)
- Cutaneous Larva MigransDocumento4 páginasCutaneous Larva MigransanissabilfaqihAinda não há avaliações
- Paederus Dermatitis An Outbreak On A Medical Mission AmazonDocumento3 páginasPaederus Dermatitis An Outbreak On A Medical Mission AmazonrrrawAinda não há avaliações
- Superficial Mycoses 3Documento8 páginasSuperficial Mycoses 3Mohammad KaifAinda não há avaliações
- Tinea Corporis, Tinea Cruris, Tinea Nigra, and Piedra: Dermatologic Clinics August 2003Documento7 páginasTinea Corporis, Tinea Cruris, Tinea Nigra, and Piedra: Dermatologic Clinics August 2003Dicky KurniawanAinda não há avaliações
- Periorbital Paederus DermatosisDocumento3 páginasPeriorbital Paederus DermatosisWanly SyahrizalAinda não há avaliações
- Ectoparasites and Parasites On Human'S Skin/Body Surface: Parasitology DepartmentDocumento36 páginasEctoparasites and Parasites On Human'S Skin/Body Surface: Parasitology DepartmentmiaraissaAinda não há avaliações
- How to identify and treat DracunculiasisDocumento24 páginasHow to identify and treat DracunculiasisFatemaAinda não há avaliações
- S0733 8635 2803 2900032 920160621 22881 1su0moo With Cover Page v2Documento33 páginasS0733 8635 2803 2900032 920160621 22881 1su0moo With Cover Page v2Alfian DjaafaraAinda não há avaliações
- Guidelines Therapy CLMDocumento6 páginasGuidelines Therapy CLMAgaipAinda não há avaliações
- Bullous Contact Dermatitis Caused by Self-Applied Crushed Paederus Fuscipes For The Treatment of VitiligoDocumento4 páginasBullous Contact Dermatitis Caused by Self-Applied Crushed Paederus Fuscipes For The Treatment of Vitiligosoumalya481Ainda não há avaliações
- Ectoparasites and Parasites On Human'S Skin/Body Surface: Parasitology DepartmentDocumento36 páginasEctoparasites and Parasites On Human'S Skin/Body Surface: Parasitology DepartmentJimmy Fran IIAinda não há avaliações
- Dermatitis Linearis: Vesicating Dermatosis Caused by Series and ReviewDocumento8 páginasDermatitis Linearis: Vesicating Dermatosis Caused by Series and ReviewrositaAinda não há avaliações
- Papular UrticariaDocumento10 páginasPapular UrticariaNuri Sakina SuhartoAinda não há avaliações
- Ccid 11 175Documento11 páginasCcid 11 175Remo Alnovryanda PutraAinda não há avaliações
- Severe DermatoDocumento13 páginasSevere DermatoadriantiariAinda não há avaliações
- Fungal InfectionsDocumento9 páginasFungal InfectionsCoral Srinivasa RamaluAinda não há avaliações
- M13 - Dermatology - Chapter 4Documento11 páginasM13 - Dermatology - Chapter 4Idham BaharudinAinda não há avaliações
- Antifungal DrugsDocumento16 páginasAntifungal DrugsAmrinder SagguAinda não há avaliações
- A Clinico-Epidemiological Study On Palmoplantar DermatosesDocumento8 páginasA Clinico-Epidemiological Study On Palmoplantar DermatosesIJAR JOURNALAinda não há avaliações
- Tinea Cruris Imp Points With ReferencesDocumento35 páginasTinea Cruris Imp Points With ReferencesSyed Saqib AliAinda não há avaliações
- Fungal Infections-MlcDocumento31 páginasFungal Infections-Mlcsamuel gathenyaAinda não há avaliações
- Scabies: Signs and SymptomsDocumento5 páginasScabies: Signs and Symptomsputri intanAinda não há avaliações
- ScabiesDocumento39 páginasScabiesShahzeb KhanAinda não há avaliações
- M13 v2 Dermatology & STI - LO6Documento8 páginasM13 v2 Dermatology & STI - LO6medipro clinicAinda não há avaliações
- Tinea Pedis - An Update: September 2011Documento6 páginasTinea Pedis - An Update: September 2011Disty Aldilla WicaksonoAinda não há avaliações
- D. Diaper 1Documento4 páginasD. Diaper 1Merinda Ajeng Arum PratiwiAinda não há avaliações
- Dyshidrotic Eczema: January 2014Documento4 páginasDyshidrotic Eczema: January 2014Strawberry ShortcakeAinda não há avaliações
- Canine Demodicosis - TPIDocumento3 páginasCanine Demodicosis - TPIDeepak CAinda não há avaliações
- CellulitisDocumento39 páginasCellulitisMary Jhane Villanueva50% (4)
- Trematode Granuloma in Children - JORS - Rathinam SRDocumento5 páginasTrematode Granuloma in Children - JORS - Rathinam SRRathinamAinda não há avaliações
- Dermato Venerology ScienceDocumento11 páginasDermato Venerology ScienceAQis AQishAinda não há avaliações
- Defi Nition and NomenclatureDocumento4 páginasDefi Nition and NomenclatureintanphAinda não há avaliações
- PDF DocumentDocumento4 páginasPDF DocumentAditya Yudha PratamaAinda não há avaliações
- Superficial Mycoses Group 4Documento38 páginasSuperficial Mycoses Group 4prudence azenaborAinda não há avaliações
- Diagnosis, Prevention and Treatment of Scabies: A ReviewDocumento5 páginasDiagnosis, Prevention and Treatment of Scabies: A ReviewSince Ivanna RumbiakAinda não há avaliações
- Paederus Dermatitis: Environmental Risk Factors, Clinical Features, and ManagementDocumento7 páginasPaederus Dermatitis: Environmental Risk Factors, Clinical Features, and ManagementInryuu ZenAinda não há avaliações
- ScabiesDocumento8 páginasScabiesJessica Dumayas Dela RosaAinda não há avaliações
- Pemphigus GuideDocumento8 páginasPemphigus Guidezuqiri ChanelAinda não há avaliações
- Role of Homoeopathic Medicines in Tinea Corporis: A Case StudyDocumento4 páginasRole of Homoeopathic Medicines in Tinea Corporis: A Case StudySandip VaghelaAinda não há avaliações
- Irritant Dermatitis To Staphylinid Beetle in Indian Troops in CongoDocumento4 páginasIrritant Dermatitis To Staphylinid Beetle in Indian Troops in CongorositaAinda não há avaliações
- Ectoparasites and Parasites On Human'S Skin/Body Surface: Parasitology DepartmentDocumento38 páginasEctoparasites and Parasites On Human'S Skin/Body Surface: Parasitology DepartmentArifin MuhammadAinda não há avaliações
- (K6) Ectoparasites and Parasites On Human's Skinbody SurfaceDocumento38 páginas(K6) Ectoparasites and Parasites On Human's Skinbody SurfaceArifin MuhammadAinda não há avaliações
- Case Study On Pemphigus VulgarisDocumento2 páginasCase Study On Pemphigus VulgarisRanindya PutriAinda não há avaliações
- Tinea Corporis, Tinea Cruris, Tinea Nigra, and PiedraDocumento6 páginasTinea Corporis, Tinea Cruris, Tinea Nigra, and PiedraIsni KhoirunisaAinda não há avaliações
- KAYE ROJAS Skin Infection BSN 1 Y2 3Documento10 páginasKAYE ROJAS Skin Infection BSN 1 Y2 3HERLIN HOBAYANAinda não há avaliações
- Dyshidrotic Eczema PDFDocumento3 páginasDyshidrotic Eczema PDFblacklist16Ainda não há avaliações
- Karin Cao Glu 2008Documento3 páginasKarin Cao Glu 2008La la landAinda não há avaliações
- Bacterial Skin Infections GuideDocumento37 páginasBacterial Skin Infections GuideAngelie PedregosaAinda não há avaliações
- Fungal Skin Infections-1Documento27 páginasFungal Skin Infections-1Fabb Nelson100% (1)
- Intertrigo and Secondary Skin InfectionsDocumento5 páginasIntertrigo and Secondary Skin Infectionskhalizamaulina100% (1)
- Todj 3 103Documento8 páginasTodj 3 103Nafiatul MuasyarahAinda não há avaliações
- I - Paederus - I - DermatitisDocumento8 páginasI - Paederus - I - DermatitisresmiAinda não há avaliações
- Tinea Pedis - An Update: September 2011Documento6 páginasTinea Pedis - An Update: September 2011Amara PutraAinda não há avaliações
- Darmstadt 1994Documento15 páginasDarmstadt 1994rismahAinda não há avaliações
- ErytrasmaDocumento17 páginasErytrasmaAndrean LinataAinda não há avaliações
- Super Ficial Fungal Infections: Key PointsDocumento4 páginasSuper Ficial Fungal Infections: Key PointsBagus Putra KurniawanAinda não há avaliações
- DemodexDocumento5 páginasDemodexmigas1996Ainda não há avaliações
- Complete Medical Guide for Disease Volume VII; Atopic DermatitisNo EverandComplete Medical Guide for Disease Volume VII; Atopic DermatitisAinda não há avaliações
- Mycobacterium Leprae Bacillus.: ARYANTI AMBARSARI 20090310019Documento2 páginasMycobacterium Leprae Bacillus.: ARYANTI AMBARSARI 20090310019Minozu AryantiAinda não há avaliações
- A Fat BoyDocumento1 páginaA Fat BoyMinozu AryantiAinda não há avaliações
- Nida PunyaDocumento1 páginaNida PunyaMinozu AryantiAinda não há avaliações
- Data MinireserchDocumento2 páginasData MinireserchMinozu AryantiAinda não há avaliações
- Mental Health Screening ToolsDocumento2 páginasMental Health Screening ToolsMinozu AryantiAinda não há avaliações
- Icd 10Documento6 páginasIcd 10Minozu AryantiAinda não há avaliações
- Diagnosis WorksheetDocumento2 páginasDiagnosis Worksheetnurul ramadhanyAinda não há avaliações