Escolar Documentos
Profissional Documentos
Cultura Documentos
Function Rpe
Enviado por
Kristine Ramos100%(1)100% acharam este documento útil (1 voto)
48 visualizações4 páginasThe RPE shields the retina from excess incoming light. It supplies omega-3 fatty acids and glucose. It secretes substances to help build and sustain the choroid and retina.
Descrição original:
Direitos autorais
© © All Rights Reserved
Formatos disponíveis
DOCX, PDF, TXT ou leia online no Scribd
Compartilhar este documento
Compartilhar ou incorporar documento
Você considera este documento útil?
Este conteúdo é inapropriado?
Denunciar este documentoThe RPE shields the retina from excess incoming light. It supplies omega-3 fatty acids and glucose. It secretes substances to help build and sustain the choroid and retina.
Direitos autorais:
© All Rights Reserved
Formatos disponíveis
Baixe no formato DOCX, PDF, TXT ou leia online no Scribd
100%(1)100% acharam este documento útil (1 voto)
48 visualizações4 páginasFunction Rpe
Enviado por
Kristine RamosThe RPE shields the retina from excess incoming light. It supplies omega-3 fatty acids and glucose. It secretes substances to help build and sustain the choroid and retina.
Direitos autorais:
© All Rights Reserved
Formatos disponíveis
Baixe no formato DOCX, PDF, TXT ou leia online no Scribd
Você está na página 1de 4
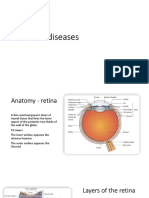
RETINAL PIGMENTED EPITHELIUM
By: Angelic Norefil Padilla
Gross Description
1. Consist of single layer of cells that
extends forward from the margin of the
optic nerve to the ora serrata anteriorly.
2. The cells are narrow and tall in the
posterior pole region and become flattened
near the ora serrata.
3. On tangential section, the cells are
hexagonal.
4. When seen in section, each cell consist of
an outer non-pigmented epithelium part
containing a large oval nucleus and an inner
pigmented portion which extends as a series
of straight thread-like process between the
rods.
Functions:
1. Light absorption - The RPE shields the
retina from excess incoming light. It
supplies omega-3 fatty acids and glucose.
2. Epithelial transport- This epithelial
transport serves to supply nutrients to the
photoreceptors (transport from the blood
to the retinal side), control the ion
homeostasis in the subretinal space and
to eliminate water and metabolites from
retinal tissue (transport from the retinal
to the blood side).
3. Visual cycle- The RPE plays a crucial
role in visual function, in the light
adaptation.
The visual cycle fulfills an essential
task of maintaining visual function
and needs therefore to be adapted to
different visual needs such as vision
in darkness or lightness
4. Phagocytosis- . Has a participation in the
turnover of the outer segments of the
photoreceptors and the formation of the
rhodopsin and iodopsin by storing and
releasing vitamin A.
5. Secretion and immune modulation- It
secretes substances to help build and
sustain the choroid and retina. It secretes
ATP, fibroblast growth factors,
transforming growth factor, insulin-like
growth factor, ciliary neurotrophic factor,
platelet-derived growth factor, vascular
endothelial growth factor, lens
epithelium-derived growth factor, and
pigment epithelium-derived factor.
BLOOD RETINAL BARRIER
By:Patricia Myka Dayap
Blood-Ocular Barrier
The eye has two barriers that prevent the
entry of macromolecules, chiefly proteins,
into the eye:
1. Blood Aqueous Barrier
2. Blood Retinal Barrier
It is a physical barrier between the
local blood vessels and most parts of
the eye itself, and stops many substances
including drugs from traveling across it.
Inflammation can break down this barrier
allowing drugs and large molecules to
penetrate into the eye.
Blood-Retinal Barrier (BRB)
The blood-retina barrier is formed by the
retinal pigment epithelium and the
endothelium of the retinal blood vessels.
Adjacent cells of each are joined by tight
junctions called as zonulae occludentes to
prevent certain substances from entering the
retina.
It consists of non-fenestrated capillaries of
the retinal circulation and tight-
junctions between retinal epithelial
cells preventing passage of large molecules
from choriocapillaris into the retina.
Function:
It regulates fluids and molecular movement
between the ocular vascular beds and retinal
tissues and prevents leakage into the retina
of macromolecules and other potentially
harmful agents.
Structure:
The blood retinal barrier has two components:
Retinal blood vessels maintains the inner
blood-ocular barrier.
The retinal pigment epithelium maintains the
outer bloodretinal barrier
Blood-Retinal Barrier Breakdown
Diabetic retinopathy
- An eye damage that frequently occurs as a result
of diabetes, is related to the breakdown of the
bloodretinal barrier.
- The barrier becomes more leaky in patients with
diabetic retinopathy
Signs and Symptoms:
First stage which is called non-proliferative diabetic
retinopathy (NPDR) there are no symptoms, it is not
visible to the naked eye and patients will have 20/20
vision. The only way to detect NPDR is by fundus
photography.
second stage, as abnormal new blood vessels
(neovascularisation) form at the back of the eye as a
part of proliferative diabetic retinopathy (PDR), they
can burst and bleed (vitreous hemorrhage) and blur
vision, because the new blood vessels are weak.
Treatment:
Scatter (pan-retinal) photocoagulation. Scatter
treatment is used to slow the growth of new abnormal
blood vessels that have developed over a wider area
of the retina.
Diabetic macular edema (DME)
occurs when blood vessels in the retina of
patients with diabetes begin to leak into the
macula, the part of the eye responsible for
detailed central vision.
These leaks cause the macula to thicken and
swell, progressively distorting acute vision.
While the swelling may not lead to
blindness, the effect can cause a severe loss
in central vision.
DME is the major cause of vision loss in
people with diabetic retinopathy.
People with diabetes have a 10 percent risk
of developing the condition during their
lifetime.
Treatment
Laser photocoagulation is a retinal
procedure in which a laser is used to
cauterize leaky blood vessels or to apply a
pattern of burns to reduce edema.
AGE RELATED MACULAR
DEGENERATION (ARMD)
By: Kristine Nicole Ramos
Mainly affects the older generation. It can
affect people over 50years of age.
It is a deterioration or breakdown of the
eye's macula. The macula is a small area in
the retina the light-sensitive tissue lining
the back of the eye.
The macula is the part of the retina that is
responsible for your central vision, allowing
you to see fine details clearly.
2 Types of ARMD:
Dry AMD
The "dry" form of macular degeneration is
characterized by the presence of yellow deposits,
called drusen, in the macula. A few small drusen
may not cause changes in vision; however, as they
grow in size and increase in number, they may lead
to a dimming or distortion of vision that people find
most noticeable when they read.
Wet AMD
In the 'wet' form, abnormal blood vessel growth in
the eye leads to the leaking of blood and proteins
into the sensitive cells (called photoreceptors) in the
macula, damaging them and causing vision loss.
The wet form is the condition in its advanced stage.
Role of RPE in ARMD:
o The RPE is responsible for maintaining the
extracellular matrix and the activity of the
photoreceptors.
o The primary cause of AMD is thought to be
the degeneration of a layer of specialised
cells called retinal pigment epithelium
(RPE)
o The RPE, melanin granules diminish, and
lipofuscin granules form.
o As we age, Bruchs membrane tends to
accumulate debris in the elastin lamina and
also drusen between the collagen layer and
RPE basal lamina.
o This debris accumulation causes a reduction
in the permeability of Bruchs membrane.
o This will hinder the pumping of waste from
inside to outside of the eye by the RPE and
may cause pigment epithelial detachments.
PARTS OF RETINAL PIGMENTED
EPITHELIUM
By: Aaron Jake De Leon & Charisse Visca
1. Base- adjacent to the curricular portion of
Bruchs Membrane to which its basement
membrane is firmly attached. The base contains
prominent infolding of the basal plasma membrane,
many mitochondria, and a little or no pigment.
It contains:
(Plasma membrane and mitochondria)
2. Body- contains the cell nucleus, many organelles
and lipofuscin. The lipofuscin become prominent in
the retinal pigment epithelium underlying the
central retina in individuals older than 30 years.
It contains:
(Nucleus, endoplasmic reticulum, lipofuscin)
3. Apices-are topped with microvilli in which the
outer segments of the rods and cones are imbedded
in the interphotoreceptor matrix.
There are no specialized attachments
between the photoreceptors and the retinal
pigment epithelium.
The lateral surfaces of the apices of
adjacent cells (but not the microvilli) are
bound together by terminal bars that are
composed of a basilar portion and an apical
portion.
There is no Intracellular space at the level of
these junctions, and together with the non-
fenestrated retinal blood vessels they
constitute the blood-retinal barrier.
Apical portion: It makes contact loosely
with sensory retina through numerous
Microvillus and concentrated with melanin
granules.
Apex(pigmented, ingested outer segment)
It contains:
1. Microvilli
2. Lateral terminal bars
( Zonula Adherens and zonula occludens )
The zonula occludens (ZO) (Tight Junction)
occupied very large, macular gap junctions
occur within the region.
The zonula adherens (ZA) (Intermediate
Junction) in adult chicken retinal pigment
epithelium was examined with cryo-electron
microscopic methods.
Deep-etching of the cross-fractured ZA showed
globules in the intercellular space
Você também pode gostar
- OCAPDocumento24 páginasOCAPKristine RamosAinda não há avaliações
- Pemicu 1 Pengindraan c2Documento113 páginasPemicu 1 Pengindraan c2CcAinda não há avaliações
- Pemicu 1 PENGINDRAAN C2Documento113 páginasPemicu 1 PENGINDRAAN C2CcAinda não há avaliações
- Retinal AnatomyDocumento86 páginasRetinal AnatomySean ScogginsAinda não há avaliações
- Paper MataDocumento18 páginasPaper Matairawaty purbaAinda não há avaliações
- Diabetic ThesisDocumento13 páginasDiabetic ThesisRemiAinda não há avaliações
- Vitreo Retinal DisordersDocumento47 páginasVitreo Retinal DisordersTabreez KhanAinda não há avaliações
- Cet 5Documento4 páginasCet 5jumi26Ainda não há avaliações
- UntitledDocumento45 páginasUntitledc/risaaq yuusuf ColoowAinda não há avaliações
- AVICENNIA LBM 4 Mata SGD 20Documento28 páginasAVICENNIA LBM 4 Mata SGD 20Maylinda Putri100% (1)
- Understanding Vitreous Humour and Retinal AnatomyDocumento28 páginasUnderstanding Vitreous Humour and Retinal AnatomyMaylinda PutriAinda não há avaliações
- Retinal Diseases 230210 210855Documento108 páginasRetinal Diseases 230210 210855RgdAinda não há avaliações
- Referat Retinopathy of PrematurityDocumento24 páginasReferat Retinopathy of Prematurityromzanr97Ainda não há avaliações
- Mechanisms of Macular Edema Beyond The SurfaceDocumento49 páginasMechanisms of Macular Edema Beyond The SurfaceGustavo RiveraAinda não há avaliações
- Giai-Phau-Sinh-Ly EnglishDocumento29 páginasGiai-Phau-Sinh-Ly EnglishTrang BuiAinda não há avaliações
- Diabetic RetinopathyDocumento18 páginasDiabetic Retinopathymohelshiekh100% (3)
- Desease of The Retina 09Documento30 páginasDesease of The Retina 09somebody_maAinda não há avaliações
- Occular Drug Delivery System - Unit V - NotesDocumento17 páginasOccular Drug Delivery System - Unit V - NotesVaishnavi SinghAinda não há avaliações
- Blindness: Introduction:-Low Vision Is A General Term Describing Visual Impairment That Requires Patients To UseDocumento12 páginasBlindness: Introduction:-Low Vision Is A General Term Describing Visual Impairment That Requires Patients To UseaparnaAinda não há avaliações
- Histology of The EyeDocumento91 páginasHistology of The EyeFazira EkmaAinda não há avaliações
- Optic Nerve: Applied AnatomyDocumento10 páginasOptic Nerve: Applied AnatomyMariam QaisAinda não há avaliações
- Orbital ExenterationDocumento9 páginasOrbital ExenterationJoji Dela pPeñaAinda não há avaliações
- Topic Presentation CataractDocumento11 páginasTopic Presentation Cataractjyoti singhAinda não há avaliações
- COATS DISEASEDocumento24 páginasCOATS DISEASEAnggie Imaniah SitompulAinda não há avaliações
- Anatomy of RetinaDocumento39 páginasAnatomy of Retinadr_dev100% (1)
- Chronic Visual LossDocumento7 páginasChronic Visual LossJim Jose AntonyAinda não há avaliações
- RetinaDocumento76 páginasRetinaSarahAinda não há avaliações
- Eye and AdnexaDocumento22 páginasEye and AdnexaWadabiAinda não há avaliações
- Li LBM 4 Mata 2Documento30 páginasLi LBM 4 Mata 2Salma SavitaAinda não há avaliações
- Meza-Rios Et Al-2020-Ophthalmology and TherapyDocumento14 páginasMeza-Rios Et Al-2020-Ophthalmology and TherapyMaría Patricia FereiraAinda não há avaliações
- Retinal Disorders Med VDocumento66 páginasRetinal Disorders Med Vhenok birukAinda não há avaliações
- Diabetic RetinopathyDocumento67 páginasDiabetic RetinopathyFirstyIlminovia0% (1)
- Final TouchDocumento49 páginasFinal TouchmalathiAinda não há avaliações
- NCP Rheum 0268Documento9 páginasNCP Rheum 0268drheriAinda não há avaliações
- Anatomy and Physiology of the EyeDocumento37 páginasAnatomy and Physiology of the EyeRajakannan60% (5)
- Assessment of The EyeDocumento4 páginasAssessment of The EyeAira Nicole ROMASAinda não há avaliações
- The Physics of Light and Color - Human Vision and Color Perception - Olympus LSDocumento14 páginasThe Physics of Light and Color - Human Vision and Color Perception - Olympus LSmarialopezmartinez424Ainda não há avaliações
- Diabetic Retinopathy - Aetiopathogenesis, Clinical Presentation andDocumento83 páginasDiabetic Retinopathy - Aetiopathogenesis, Clinical Presentation andOlayemi Olorundare0% (1)
- Pathology - Chapter 29 (Partial)Documento3 páginasPathology - Chapter 29 (Partial)Cory GrayAinda não há avaliações
- Fluorescein AngiographyDocumento81 páginasFluorescein Angiographyeng_25122147100% (4)
- Ocular Drug Delivery SystemDocumento67 páginasOcular Drug Delivery Systemmskhatri3Ainda não há avaliações
- Diabetic Retinopathy Symptoms Causes RisDocumento7 páginasDiabetic Retinopathy Symptoms Causes Riskenneth MoragaAinda não há avaliações
- Med2 Xing HannahDocumento6 páginasMed2 Xing HannahCharlotte YeoAinda não há avaliações
- Vitreoretina: DR - Reinne Natali Christine, SPM Dept. Ilmu Penyakit Mata FK Uki / Rsu FK UkiDocumento45 páginasVitreoretina: DR - Reinne Natali Christine, SPM Dept. Ilmu Penyakit Mata FK Uki / Rsu FK UkitusuksedotanAinda não há avaliações
- Eyes and Vision PresentationDocumento142 páginasEyes and Vision Presentationrhimineecat71100% (1)
- Ignacio - 6TH Paper SGD OphthaDocumento4 páginasIgnacio - 6TH Paper SGD OphthaRichelle IgnacioAinda não há avaliações
- Far Eastern University - Posterior Segment Evaluation TechniquesDocumento13 páginasFar Eastern University - Posterior Segment Evaluation TechniquesCzara DyAinda não há avaliações
- Classification of Retinal Images For Diabetic Retinopathy at Non-Proliferative Stage Using ANFISDocumento7 páginasClassification of Retinal Images For Diabetic Retinopathy at Non-Proliferative Stage Using ANFISIIR indiaAinda não há avaliações
- Stem Cell Therapy For AMD (Paper)Documento12 páginasStem Cell Therapy For AMD (Paper)Febriani MuldiatiAinda não há avaliações
- Retinal Detachment: Causes, Symptoms and Treatment Options Under 40 CharactersDocumento32 páginasRetinal Detachment: Causes, Symptoms and Treatment Options Under 40 Charactersc/risaaq yuusuf ColoowAinda não há avaliações
- Retina Anatomy and PhysiologyDocumento37 páginasRetina Anatomy and PhysiologyAbdisamed AllaaleAinda não há avaliações
- Diabetic RetinopathyDocumento73 páginasDiabetic RetinopathyGetLyricsAinda não há avaliações
- Spirovital Therapy Option For Macular DegenerationDocumento6 páginasSpirovital Therapy Option For Macular DegenerationtavlarAinda não há avaliações
- Special Sense EYEDocumento74 páginasSpecial Sense EYEprekshya shresthaAinda não há avaliações
- Course 7 I, IIDocumento17 páginasCourse 7 I, IItaliya. shvetzAinda não há avaliações
- ANATOMY & PHYSIOLOGY OF THE EYEDocumento70 páginasANATOMY & PHYSIOLOGY OF THE EYEArif MohammadAinda não há avaliações
- Macular Degeneration: From Diagnosis to TreatmentNo EverandMacular Degeneration: From Diagnosis to TreatmentNota: 4 de 5 estrelas4/5 (2)
- Low Vision: Assessment and Educational Needs: A Guide to Teachers and ParentsNo EverandLow Vision: Assessment and Educational Needs: A Guide to Teachers and ParentsAinda não há avaliações
- Diabetic Retinopathy: Causes, Tests, and Treatment OptionsNo EverandDiabetic Retinopathy: Causes, Tests, and Treatment OptionsAinda não há avaliações
- Class 10 Physics Lecture Planner for Light and ElectricityDocumento2 páginasClass 10 Physics Lecture Planner for Light and ElectricityTech AnuragAinda não há avaliações
- On Seeing in The Dark - Remarks On The Evolution of The EyeDocumento5 páginasOn Seeing in The Dark - Remarks On The Evolution of The EyeabbraxasAinda não há avaliações
- Light and Optics Unit PlanDocumento13 páginasLight and Optics Unit Planapi-486627052Ainda não há avaliações
- Diseases, Diagnosis and Management of Ocular FundusDocumento111 páginasDiseases, Diagnosis and Management of Ocular FundusThakur Abhishek SinghAinda não há avaliações
- 2 - Sudden and Gradual Vision LossDocumento31 páginas2 - Sudden and Gradual Vision Losstemp001bunnAinda não há avaliações
- Simmel On FaceDocumento15 páginasSimmel On FacemangsilvaAinda não há avaliações
- OptiVisum LLC Releases Plant Based OptiVisum Drops For Restoring Visual AcuityDocumento2 páginasOptiVisum LLC Releases Plant Based OptiVisum Drops For Restoring Visual AcuityPR.comAinda não há avaliações
- MataDocumento16 páginasMataIslah NadilaAinda não há avaliações
- Solution Manual For Transportation A Global Supply Chain Perspective 8th Edition John J Coyle Robert A Novack Brian Gibson Edward J BardiDocumento34 páginasSolution Manual For Transportation A Global Supply Chain Perspective 8th Edition John J Coyle Robert A Novack Brian Gibson Edward J BardimeilbyouxbAinda não há avaliações
- Science Form 3 CHAPTER 1Documento8 páginasScience Form 3 CHAPTER 1loga yuthrashreeAinda não há avaliações
- Hci 2 Mark Question Bank Unit 1Documento10 páginasHci 2 Mark Question Bank Unit 1Sathya MAinda não há avaliações
- Blue Collar Billing CodingDocumento18 páginasBlue Collar Billing CodingShell VenkatAinda não há avaliações
- Eye Disorder PeadsDocumento51 páginasEye Disorder PeadsGrashiaAinda não há avaliações
- Says: "In The Square Inch Field of The Square Foot House, LifeDocumento26 páginasSays: "In The Square Inch Field of The Square Foot House, LifezpdjadazkpAinda não há avaliações
- Topic 14 (2) - Ocular Correction of AmetropiaDocumento13 páginasTopic 14 (2) - Ocular Correction of AmetropiashadowosAinda não há avaliações
- 15 Stimuli, Receptors and Responses: Check Your ProgressDocumento6 páginas15 Stimuli, Receptors and Responses: Check Your Progresssteve LAinda não há avaliações
- Fundus evaluation techniquesDocumento42 páginasFundus evaluation techniqueskeshavAinda não há avaliações
- Individual Movement TechniqueDocumento22 páginasIndividual Movement TechniqueJohn Joshua RemultaAinda não há avaliações
- CC3 Eyesight Test Certificate PDFDocumento3 páginasCC3 Eyesight Test Certificate PDFharrp3000Ainda não há avaliações
- Vol 2 Retinal AtlasDocumento252 páginasVol 2 Retinal AtlasDra. Mitzy Torres - RetinólogaAinda não há avaliações
- Atlas OCTDocumento322 páginasAtlas OCTMacarena Alvarez100% (1)
- Week 8Documento18 páginasWeek 8Jeng JengAinda não há avaliações
- M - Cee-2: C, E, AkeleyDocumento7 páginasM - Cee-2: C, E, AkeleywjzabalaAinda não há avaliações
- Binocular Vision TestsDocumento100 páginasBinocular Vision TestsANDREW OMAKAAinda não há avaliações
- A Scan BiometryDocumento28 páginasA Scan Biometrysolex_Ainda não há avaliações
- PROGRESSIVE LENS GUIDEDocumento6 páginasPROGRESSIVE LENS GUIDEAmyCheahAinda não há avaliações
- Medpor ImplantsDocumento19 páginasMedpor ImplantsAnalyzer FaceAinda não há avaliações
- Ophtha Quiz - Ocular Manifestations of SystemicDocumento3 páginasOphtha Quiz - Ocular Manifestations of SystemicAsif MohammedAinda não há avaliações
- Al Hoota CaveDocumento15 páginasAl Hoota CaveJosep Manuel VictòriaAinda não há avaliações
- The Swinging Flashlight Test: Learning Objective: Facts About The PupilDocumento3 páginasThe Swinging Flashlight Test: Learning Objective: Facts About The Pupilsiti hazard aldinaAinda não há avaliações