Escolar Documentos
Profissional Documentos
Cultura Documentos
Zirconia
Enviado por
Ana Massiel NarváezDireitos autorais
Formatos disponíveis
Compartilhar este documento
Compartilhar ou incorporar documento
Você considera este documento útil?
Este conteúdo é inapropriado?
Denunciar este documentoDireitos autorais:
Formatos disponíveis
Zirconia
Enviado por
Ana Massiel NarváezDireitos autorais:
Formatos disponíveis
Review Article
Clinical trials in zirconia: a systematic review
B. AL-AMLEH, K. LYONS & M. SWAI N Department of Oral Rehabilitation, Faculty of Dentistry, University of
Otago, Dunedin, New Zealand
SUMMARY Zirconia is unique in its polymorphic crys-
talline makeup, reported to be sensitive to manu-
facturing and handling processes, and there is debate
about which processing method is least harmful to
the nal product. Currently, zirconia restorations are
manufactured by either soft or hard-milling
processes, with the manufacturer of each claiming
advantages over the other. Chipping of the veneering
porcelain is reported as a common problem and has
been labelled as its main clinical setback. The objec-
tive of this systematic review is to report on the
clinical success of zirconia-based restorations fabri-
cated by both milling processes, in regard to frame-
work fractures and veneering porcelain chipping. A
comprehensive review of the literature was com-
pleted for in vivo trials on zirconia restorations in
MEDLINE and PubMed between 1950 and 2009. A
manual hand search of relevant dental journals was
also completed. Seventeen clinical trials involving
zirconia-based restorations were found, 13 were
conducted on xed partial dentures, two on single
crowns and two on zirconia implant abutments, of
which 11 were based on soft-milled zirconia and six
on hard-milled zirconia. Chipping of the veneering
porcelain was a common occurrence, and framework
fracture was only observed in soft-milled zirconia.
Based on the limited number of short-term in vivo
studies, zirconia appears to be suitable for the
fabrication of single crowns, and xed partial den-
tures and implant abutments providing strict proto-
cols during the manufacturing and delivery process
are adhered to. Further long-term prospective stud-
ies are necessary to establish the best manufacturing
process for zirconia-based restorations.
KEYWORDS: zirconia, fracture, porcelain chipping,
crowns, xed partial dentures, implant abutments
Accepted for publication 13 March 2010
Introduction
In dentistry, gold and metal-alloys have passed the test
of time and are recognized as predictable and well-
established clinical materials for the restoration of
various xed prostheses (1). Indeed, metal-ceramic
systems require relatively little special knowledge for
their routine use which has led to their worldwide
acceptance and use since their inception. Nevertheless,
the increasing aesthetic demand in dentistry has driven
the development of a number of ceramics for their
aesthetic capability, biocompatibility, colour stability,
wear resistance and low thermal conductivity (2). As
far back as 1885, porcelain jacket crowns were rst used
for single crowns for the anterior teeth because of
their aesthetic and natural appearance (3). However,
ceramics cannot withstand deformation strain of more
than 01%03% without fracturing and are susceptible
to fatigue fracture. It is this brittleness, because of the
ionic-covalent atomic bonding, which has limited their
use in dentistry for decades (4).
The most recent introduction to the dental ceramics
family is zirconia, which in its pure form is a polymor-
phic material that occurs in three temperature-depen-
dant forms that are: monoclinic (room temperature to
1170 C), tetragonal (1170 C2370 C) and cubic
(2370 C up to melting point) (5). However, when
stabilizing oxides such as magnesia, ceria, yttria and
calcium are added to zirconia, the tetragonal phase is
retained in a metastable condition at room tempera-
ture, enabling a phenomenon called transformation
toughening to occur. The partially stabilized crystalline
2010 Blackwell Publishing Ltd doi: 10.1111/j.1365-2842.2010.02094.x
Journal of Oral Rehabilitation 2010 37; 641652
J o u r n a l o f
Oral Rehabilitation
tetragonal zirconia, in response to mechanical stimuli,
such as tensile stress at crack tips, transforms to the
more stable monoclinic phase with a local increase in
volume of approximately 4%. This increase in volume
closes the crack tips, effectively blunting crack propa-
gation. It is this transformation-toughening process
which gives zirconia its strength and toughness,
exceeding all currently available sintered ceramics.
Compared to alumina, zirconia has twice the exural
strength, partly because of its grain size and the
transformation-toughening mechanism. (6).
To date, there are three types of zirconia-containing
ceramics which are used in dentistry. Glass-inltrated
zirconia-toughened alumina ceramics, magnesium-
doped partially stabilized zirconia and 3 mol% yttria
containing tetragonal zirconia polycrystalline (Y-TZP),
with the latter being the most utilised form in dentistry
because of its higher exural strength reported to range
from 900 to 1200 MPa (7). Y-TZP has been used in root
canal posts (8), frameworks for all-ceramic posterior
crowns and xed partial dentures (FPDs) (912),
implant abutments (13, 14) and dental implants (15).
Advances in CAD CAM technology has made it
possible to more readily use zirconia in dentistry. This
technology enables complex shapes to be milled out of
pre-made zirconia blanks (or blocks), where the
prepared abutment is rst scanned, then using com-
puter software, the desired framework is designed prior
to milling (16).
There are two types of zirconia milling processes
available: (i) soft-milling and (ii) hard-milling. Soft-
milling involves machining enlarged frameworks out of
pre-sintered blanks of zirconia, also called the green
state. These are then sintered to their full strength,
which is accompanied by shrinkage of the milled
framework by approximately 25% to the desired
dimensions. Hard-milling involves machining the
framework directly to the desired dimension out of
densely sintered (higher strength and more homoge-
nous) zirconia blanks, typically these have been hot
isostatic pressed (HIPed). However, because of the
extreme hardness of sintered zirconia, a robust milling
system is required that needs an extended milling
period compared to the soft-milling process as well as
placing heavy demands on the rigidity of the cutting
instruments. The relative ease and speed of soft-milling
may be why more manufacturers chose this method to
fabricate their dental zirconia products, while only a
smaller number have used HIPed zirconia. Among the
common representative systems utilizing soft-milling
are Lava,* Procera zirconia,
IPS e.max ZirCAD
and
Cercon.
Systems that utilize hard-milling of HIPed
zirconia include DC-Zirkon
and Denzir.**
Supporters of soft-milling claim that hard-milling
may introduce microcracks in the framework during
the milling process. In contrast, hard-milling supporters
claim a superior marginal t because no shrinkage is
involved in their manufacturing process. Nevertheless,
in vitro studies support the use of both HIPed and non-
HIPed zirconia for all-ceramic FPDs, crowns and
implant abutments for the posterior of the mouth
because of their high exural strength and fracture
toughness (17).
The most utilized zirconia in dentistry, Y-TZP, has
been found to withstand cyclic fatigue testing, where
posterior all-ceramic FPDs spanning up to 5-units, had a
lifetime comparable to that achieved with metal-
ceramic restorations (2), and it has been predicted,
based on the results of this study, to have a lifetime
longer than 20 years (18). However, early clinical
ndings show that there are two main drawbacks for
zirconia restorations compared to metal-ceramics. The
rst is a high incidence of veneering porcelain fracture,
manifesting clinically as chipping fractures, and the
other is an inherent accelerated ageing problem that
has been identied to occur in zirconia in the presence
of water. This ageing phenomenon is known as
low-temperature degradation (LTD), which causes a
decrease in physical properties by spontaneous phase
transformation of the zirconia crystals from the tetrag-
onal phase to the weaker monoclinic phase putting
zirconia frameworks at risk of spontaneous catastrophic
failure (19).
The objective of this systematic review is to report
on the clinical success of HIPed and non-HIPed Y-TZP-
based restorations (single crowns, FPDs and implant
abutments), focusing on the incidence of framework
fracture and chipping of the veneering porcelain in
both groups. In addition, recent in vitro studies con-
ducted in an attempt to solve some of the reported
problems in zirconia-based restorations are also dis-
cussed.
*3M ESPE, Seefeld, Germany.
Nobel Biocare AB, Carolinsk, Sweden.
Vivadent-Ivoclar, Ellwangen, Germany.
Dentsply-Degudent, Hanau, Germany.
DCS Dental AG, Allschwil, Germany.
**Decim AB, Skelleftea , Sweden.
B. AL - AML E H et al. 642
2010 Blackwell Publishing Ltd
Materials and methods
A search was performed in MEDLINE and PubMed
for in vivo trials on zirconia restorations published
between 1950 and June 2009. The main keywords
used for the search and the number of articles
produced were:
1 zirconia AND clinical- 329 articles
2 zirconia AND xed partial dentures- 130 articles
3 zirconia AND FPD- 23 articles
4 zirconia AND implant abutments- 61 articles
5 zirconia AND single crowns- 73 articles
In addition, a manual hand search was conducted
through the literature to identify any possible clinical
trials on Y-TZP which may have not been listed on
MEDLINE and PubMed. The articles found were read to
identify ones which satised the following inclusion
and exclusion criteria:
Inclusion Criteria:
1 Human in vivo only
2 Conducted on Y-TZP
3 Fixed prosthetics (single
crowns, FPDs or implant abutments)
4 Study has a set inclusion and exclusion criteria
5 Study has a materials and methods
6 In the English language
Exclusion Criteria:
1 Case reports
2 In vitro trials
3 Animal studies
4 Trials <12 months
The search yielded 19 articles and abstracts involving
Y-TZP restorations in clinical trials which satised the
inclusion criteria. Following this, one nal search was
done by inspecting the bibliographies of the 19
reviewed articles for any additional studies, however,
none were found.
Results
In total, only 17 clinical trials involving Y-TZP-based
restorations were found in the literature, of which only
three are randomized control trials (14, 20, 21). The
majority of studies investigated all-ceramic FPDs in the
posterior mouth (4, 912, 20, 2229), while a small
number investigated single crowns (21, 30), implant
abutments (13, 14, 31), and only one study was
available on implant-supported zirconia FPDs (20).
Eight different brands of Y-TZP were identied among
the 17 studies with Cercon zirconia being the most
investigated brand (Table 1).
Thelongest follow-upperiodfoundwas 5 years, where
two papers reported results on patients restored with
zirconia all-ceramic FPDs (9, 10). Bothstudies involved 3
to5-unit FPDs onnatural teethinthepremolar andmolar
regions, except for one 3-unit FPD that replaced a lateral
incisor (9). The survival rate of Y-TZP FPDs over 5 years
was 100% (9) and 74% (10), and in the latter study, a
5-unit FPD framework fracture occurred, reportedly
because of accidental biting of a stone in a piece of bread.
While the incidence of chipping of the veneering ceramic
was 152%, in this study, secondary caries was found to
be the most common cause of failure (217%). This was
attributed to the poor marginal t produced by a
prototype milling technique usedtofabricatethe zirconia
restorations in this particular study.
Four studies reported data on 1-year follow-up
periods for four different treatment modalities. These
were zirconia FPDs on natural teeth (27), FPDs restored
on titanium implant abutments (20), inlay-retained
FPDs (28) and zirconia implant abutments(31), two of
which are randomized control trials (20, 31). The
highest incidence of framework fracture and chipping
veneering porcelain was both reported in 1-year follow-
up studies (10%(28) and 54%(20), respectively) when
compared to longer follow-up periods.
Zirconia implant abutments
Zirconia implant abutments demonstrated encouraging
early results in the only two studies conducted on
single-tooth implant abutments using both HIPed and
non-HIPed zirconia. Glauser et al. reported no fractures
of the 38 HIPed-based zirconia abutments in the
anterior and premolar regions in 18 patients evaluated
after 4 years (13), and favourable hard and soft tissue
responses were also reported. All abutments were
restored with Empress I (Leucite reinforced) crowns
and cemented with Panavia TC
resin cement. How-
ever, screw loosening of two zirconia abutments at 8
and 27 months was reported, nevertheless no frame-
work fracture occurred during the follow-up period.
In a randomized controlled trial, 20 customized non-
HIPed-based zirconia single-tooth implant abutments
(Procera
) and 20 customized titanium single-tooth
implant abutments (Procera
) were followed for
Kuraray, Okayama, Japan.
C L I NI C AL T R I AL S I N Z I R C ONI A 643
2010 Blackwell Publishing Ltd
3 years, with no fractures or loosening of abutments in
either group, and a 100% survival rate reported (14). In
this study, the abutments were restored in the canine to
molar regions. There was no difference in the soft tissue
health around both abutment groups, nevertheless
using spectrophotometric analysis, both zirconia and
titanium abutments induced similar amount of discol-
ouration of the mucosa when compared to the gingiva
of natural teeth.
Both trials on zirconia implant abutments were
conducted on regular platform, externally hexed
implants (Bra nemark system- RP
)were used for sin-
gle-tooth replacement. The Bra nemark implant system
was the rst titanium dental implant introduced in the
mid 1970s, nevertheless recently introduced internal
type connections have been shown to improve the
fracture resistance and stability of the implant-
abutment system (32). However, so far there are no
published clinical trials using internal type zirconia
implant abutments, so no comparison could be made of
the long-term stability of both systems using zirconia
abutments.
Zirconia single crowns
Single crowns have a small representation in pub-
lished clinical trials on Y-TZP. In a 2-year randomized
control trial, 1 of 15 Cercon zirconia crowns
fractured
in half only 1 month after cementation on a maxillary
second molar (21), so that the success rate for this
study was 93% after 2-years. There was no signicant
difference in soft tissue health adjacent to the Cercon
crowns and the control crowns made with In-Ceram
zirconia (Vita). No chipping of the veneering porcelain
was reported after 2 years. In the mean time, no
framework fracture have been reported after 3 years
in a study with 204 single crowns fabricated with
Procera zirconia
in a private practice setting (30).
However, 16% of the crowns had some type of
complication, and 6% were recorded as a failure. Loss
Table 1. List of in vivo trials conducted in yttria-stabilized tetragonal zirconia polycrystalline
Type of
zirconia Brand Study
Follow-up
periods
Type of
restorations
Sample
size
Framework
fracture, %
Veneering
porcelain
fracture,
%
Non-HIPed Cercon zirconia
(Dentsply)
Sailer et al. 2007 (10) 5 years 35 units FPD 33 8 15
Beuer et al. 2009 (22) 3 years 3 units FPD 21 5 0
Cehreli et al. 2009 (21) 2 years Single crowns 15 7 0
Schimitter et al. 2009 (23) 2 years 47 units FPD 30 3 3
Bornemann et al. 2003 (24) 15 years 34 units FPD 59 0 3
Lava (3M ESPE) Raigrodski et al. 2006 (25) 25 years 3 units FPD 20 0 25
Pospeich et al. 2003 (26) 2 years 3 units FPD 38 0 3
Crisp et al. 2008 (27) 1 year 34 units FPD 38 0 3
Procera zirconia
(Nobel Biocare)
Zembic et al. 2009 (14) 3 years Implant
abutments
18 0
Ortrop et al. 2009 (30) 3 years Single crowns 204 0 2
IPS e.max Zir CAD
(Vivadent-Ivoclar)
Ohlmann et al. 2008 (28) 1 year IRFPD 30 10 13
HIPed Denzir (Cadesthetics
AB)
Molin & Karlsson 2008 (9) 5 years 3 units FPD 19 0 36
Larsson et al. 2006 (20) 1 year 25 units
FPD Ti abut
13 0 54
DC- Zirkon
(DCS Dental AG)
Tinschert et al. 2008 (29) 3 years 310 units
+cantilever
65 0 6
Vult von Steyern et al.
2005 (4)
2 years 35 units FPD 23 0 15
Digizon Edelhoff et al. 2008 (12) 3 years 36 units FPD 21 0 95
Wohlwend Glauser et al. 2004 (13) 4 years Implant
abutments
54 0
HIPed, hot isostatic pressed zirconia; FPD, xed partial denture; IRFPD, inlay-retained xed partial denture; Ti abut, titanium implant
abutment.
B. AL - AML E H et al. 644
2010 Blackwell Publishing Ltd
of retention (12 204 = 6%), extraction of abutment
tooth (5 204 = 25%), persistent pain (10 204 = 5%)
and chipping of veneering porcelain (4 204 = 2%)
were some of the complications reported in this study
which had a cumulative survival rate of 93% at
3 years.
Although zirconia single crowns appear to demon-
strate good short-term success rates of 93% after
2 years and a survival rate of 93% after 3 years, these
must be viewed with caution as they reect data from a
study with a small sample size of 15, and the other
study reported data from a private practice setting that
was mainly based on patients records rather than
clinical evaluation.
Zirconia-xed partial dentures
The most investigated treatment modality are the
zirconia-xed partial dentures, with 13 different clinical
trials reporting data on FPD spans ranging from 3 to
10-units. Except for one study, all FPDs used natural
teeth as abutments; the exception used titanium
implant abutments. Zirconia PFDs demonstrated
favourable results, exhibiting a high success rate in
most studies. A relatively small number of framework
fractures have been reported in the clinical trials and do
not appear to have occurred spontaneously, but rather
an initiating factor was determined to have contributed
to the fractured framework. The longest FPD spanned
10-units (5 pontics on 5 abutments) with the frame-
work made with DC-Zirkon
and the veneering porce-
lain was Vita D (29). This study also included two
cantilever posterior FPDs. No framework fractures were
reported after 3 years of follow-up; however, chipping
of the veneering porcelain was reported in 4 posterior
FPDs of the 65 FPDs placed in the anterior and posterior
regions.
Zirconia framework fracture
Fracture of Y-TZP substructures mostly occurred in
FPDs, nevertheless this was found to be rare, and was
only reported in ve studies on two zirconia brands
(Table 2). The incidence of framework fracture was
directly related to the design of the FPD, where inlay-
retained FPDs (IRFPD) showed the highest failure rate
of 10% after only 12 months. These IRFPDs were made
with IPS e.max ZirCAD
, where debonding of the inlay
pontic has been concluded to be the cause of the
framework fractures. In the review, Cercon zirconia
suffered the majority of frameworks fractures compared
to the other investigated zirconia brands; however, it
must be kept in mind that it is also the most investi-
gated brand (5 of 18 trials), followed by Lava* (3 of 18
trials). Both IPS e.max ZirCAD and Cercon zirconia are
a non-HIPed zirconia manufactured by the soft-milling
process.
Veneering porcelain fracture
The most common complication observed in zirconia-
based restorations was fracture of the veneering porce-
lain, manifesting clinically as chipping fractures of the
veneering ceramic with or without exposing the
underlying Y-TZP framework. All eight of the investi-
gated zirconia brands exhibited chipping fractures, even
when using specically manufactured veneering
porcelains with modied coefcients of thermal
expansions compatible with zirconia (>11 10
)6
K
)1
)
(10, 25). These chipping fractures were found to occur
in non-load-bearing areas, such as the mesio-lingual
cusps on a mandibular second molars (23), and the
lingual aspect of FPD pontics (10). Possible trends in the
location of the chipping have been identied by some
authors and included the premolar and molar regions
Table 2. In vivo studies which reported Y-TZP framework fracture and the time until fracture
Study Brand of Zirconia
Type of
restoration
Follow-up
periods
Time until
fracture
Number of units
fractured
Incidence,
%
Sailer et al. 2007 (10) Cercon zirconia 35 unit FPD 5 years 38 months 1 out of 13 8
Beuer et al. 2009 (22) Cercon zirconia 3 unit FPD 3 years 30 months 1 out of 21 5
Schimitter et al. 2009 (23) Cercon zirconia 47 unit FPD 2 years 1 month 1 out of 30 3
Cehreli et al. 2009 (21) Cercon zirconia Single crowns 2 years 1 month 1 out of 15 7
Ohlmann et al. 2008 (28) IPS e.max ZirCAD IR FPD 1 year Not specied
(<12months)
3 out of 30 10
C L I NI C AL T R I AL S I N Z I R C ONI A 645
2010 Blackwell Publishing Ltd
(30), particularly the second molars on FPDs (25) and
the connector area in mandibular posterior FPDs (29).
Denzir zirconia
frameworks veneered with Espri-
dent Triceram,
demonstrated the highest incidence of
veneering porcelain fracture at 1 year of 54% when
FPDs were using titanium implant abutments (20). In
addition, there was a 36% incidence of roughness pit-
ting on occlusal surfaces of 3-unit FPDs on natural teeth
after 5 years with Denzir zirconia frameworks veneered
with either a feldspathic porcelain Vita Veneering
Ceramic D (Vita) or leucite reinforced pressed ceramic
IPS Empress
(9).
Cementation and bonding
Because of its high exural strength, zirconia can be
conventionally cemented, just like metal-ceramic res-
torations, without the need for any pretreatment;
although bonding of zirconia is possible provided
special conditioning, treatment of the zirconia is carried
out rst because zirconia is not etchable. Indeed,
cementation of zirconia all-ceramic restorations is a
simpler process compared to other all-ceramic systems
which require added steps for bonding. This was
evident in the range of cements used by the various
authors in the published clinical trials; zinc phosphate
cement (4, 9, 20, 24, 29, 30), glassionomer cements
(GIC) (2123, 26), resin-modied GIC (12, 25) and
resin cements (913, 2730).
Loss of retention was seen in 7 of 16 studies involving
the cementation of zirconia restorations. One 3-unit
FPD cemented with Panavia F lost retention after
12 months (9), a 4-unit FPD cemented with Variolink
lost retention after 333 months in service (10), while
two 3-unit FPDs in the molar region cemented with
zinc phosphate lost retention at 17 and 32 months (29).
Ketac Cem* glassionomer cement had one posterior 3-
unit FPD decemented after 38 months (22), in addition
to two long-span FPDs at 88 and 142 months in service
(23). All debonded zirconia restorations were rece-
mented successfully for the duration of the follow-up
period in each of the studies.
In contrast, six cases of debonded inlay-retained
zirconia FPDs were seen with Panavia F (dual-cured
resin cement) and Multilink (automix self-curing resin
cement), despite the pretreatment of the zirconia with
tribochemical air abrasion (Rocatec*). Fracture of the
framework occurred in three of the six debonded
restorations (28). Similarly, in a study on single Procera
zirconia crowns, 12 of 204 crowns lost retention of
which 4 could not be recemented (30). Unfortunately,
the type of cement used for the crowns which lost
retention was not reported, as both zinc phosphate and
resin cement (Rely-X Unicem*) where used.
Despite the encouraging retentive capacity of zinc
phosphate-cemented zirconia restorations, after 5-years
follow-up of 3-unit FPDs that were cemented with
either resin cement (Panavia F) or zinc phosphate
(De Trey Zinc
), visible evidence of ditching along the
margins was only seen in the zinc phosphate-cemented
group. Ditching was reported in 5% of mesial abut-
ments and 26% in distal abutments in this study,
however, this problem was not reported in the other
trials using zinc phosphate cement.
Discussion
With the limited number of published clinical trials, one
can conclude that Y-TZP has the potential for being
accepted as a suitable material for xed prosthodontic
dental treatment; however, larger sample sizes and
longer in vivo studies are needed. The majority of
published studies are prospective clinical trials, with the
longest follow-up period being 5 years. In addition,
only three randomized control trials exist, with 1 to
3-year follow-up periods. Long-span multi-unit FPDs
have also been included in a number of studies
demonstrating condence in the structural potential
of zirconia frameworks (4, 10, 12, 20, 23, 29).
Certainly, the published clinical trials demonstrate a
careful and meticulous approach in their treatments,
with steps taken to insure that the zirconia frameworks
are delivered at their best possible condition before nal
cementation. Furthermore, it was interesting to note
that all 17 studies included bruxism in their exclusion
criteria, and therefore this should alert a potential
limitation of this all-ceramic system that is not being
investigated clinically.
Zirconia framework fracture
The probability of fracture of zirconia FPDs has been
estimated to be almost 0% after a simulated 10-year
clinical service study (33), however, framework fracture
has been reported in several in vivo trials of less than
Cadesthetics AB, Skelleftae, Sweden.
Dentaurum, Ispringen, Germany.
B. AL - AML E H et al. 646
2010 Blackwell Publishing Ltd
5-years (10, 2123, 28). Four of 5 studies involving
Cercon zirconia reported framework fractures both in
single crowns and FPDs. Inanin vitro trial, it was reported
that a force of 379 to 501 MPa was needed to load Cercon
zirconia 4-unit FPDs to failure which is higher than the
average human bite, conrming its suitability as a
substructure framework for FPDs (34). Cercon zirconia
is a non-HIPed Y-TZP, and it is too early to say whether it
is a weaker brand of zirconia compared to others because
of the limited number of trials published so far, and
keeping in mind that Cercon zirconia has been the most
clinically investigated brand of Y-TZP so far.
A 5-unit Cercon zirconia maxillary FPD fractured at
theconnector betweentwopontics at the rst andsecond
premolars after 38 months in service (10). The dimen-
sion of the fractured connector was 1928 mm
2
, well
above the recommended connector area of 916 mm
2
by
Raigrodski (2004) (35). Accidental biting on a stone was
reported to be the primary reason for failure. Scanning
electron microscopy (SEM) analysis revealed the pri-
mary crack initiation site on a Cercon zirconia FPD that
failed 29 days after insertion to be from the gingival
aspect of the connector that was around 105 mm
2
in
surface area (23). It was claimed by the authors to be
because of inappropriate alteration performed by a
dental technician during the veneering of the FPD. This
conrms reports that the most susceptible part of fracture
inall-ceramic FPDs is the connector area (36, 37). In fact,
fractographic analyses of ve failed 4-unit Cercon zirco-
nia FPDs conrmed all the connector failures were
initiated fromthe gingival surface; where tensile stresses
were the greatest (34). In contrast, lithium disilicate-
based FPDs were found to fracture from the occlusal
surface of the failing connector (38).
As for single crowns, one Cercon zirconia crown
restoring a non-vital maxillary second molar fractured
in half after 1 month in service (21). This tooth did not
have a post, and although bruxism was part of their
exclusion criteria, the patient reportedly had nocturnal
bruxism, for which he had been undertaking muscle-
relaxation splint therapy.
Despite the promising results reported in vitro (39),
IRFPDs made with IPS e.max ZirCAD
also a non-HIPed
Y-TZP, demonstrated the highest incidence of fractured
frameworks in just 1-year, with a survival rate of 57%
(28). These FPDs had inlays, partial and full-crowns as
retainers with at least one retainer being an inlay.
Debonding of 20% of the retainers resulted in a 10%
framework fracture primarily when one retainer
debonded, which subsequently overloaded the connec-
tors to failure. Bonding procedures in the study used
the generally recommended bonding method for Y-TZP,
namely using tribochemical silica-coating air abrasion
(Rocatec*) pretreatment of the inner surface of the
copings, followed by silanization and cementation using
phosphate monomer resin cements, Panavia F
and
Multilink Automix
. Debonding was explained by the
reduced area of adhesion, either because of the small
surface area of the inlay retainers or because of voids in
the resin cement. No other in vivo study investigated the
longevity of inlay-retained FPDs, and furthermore, it is
the only in vivo study conducted on IPS e.max ZirCAD.
The physical properties of IPS e.max ZirCAD are no
lower than the average Y-TZP (40), hence the high
failure rate seen could only be explained by the design
of the inlay-retained framework. Wolfart & Kern
reported two case studies on IRFPDs. These IRFPDs
had modied wrap-around wing retainers resembling
metal winged resin-bonded retainers to increase the
bonding surface area that also had full thickness
zirconia that omitted any veneering ceramic for max-
imum strength (41). Nevertheless, in contrast to other
treatment modalities, Y-TZP IRFPDs cannot yet be
recommended and should not be clinically prescribed
until improvements in bonding of zirconia is achieved
and further long-term clinical trials are published.
An in vitro study of ve framework-designed canti-
lever zirconia FPDs made of Lava* showed poor fracture
resistance, where most fractures occurred at the distal
wall of the terminal abutment (42). As a consequence,
cantilever FPDs made of zirconia were not recom-
mended by the authors; nevertheless, a 3-unit and a
4-unit cantilever Y-TZP FPDs survived 3 years in
function in the posterior region of the mouth (29).
These cantilever FPDs were made from DC-Zirkon
HIPed densely sintered blanks and cemented with zinc
phosphate cement. Further larger sample sizes and
longer follow-up periods are necessary before zirconia
cantilever FPDs can be recommended.
Chipping of veneering porcelain
Zirconia has a white opaque colour, which needs
masking by veneering it with a more translucent, and
aesthetic porcelain to achieve an acceptable aesthetic
result, as with porcelain-fused-to-metal restorations
(PFM). The most striking nding which has been
reported in the literature is the high incidence of
C L I NI C AL T R I AL S I N Z I R C ONI A 647
2010 Blackwell Publishing Ltd
cohesive failure of the veneering porcelain, manifesting
clinically as chipping of the veneering ceramic with or
without exposing the underlying Y-TZP framework.
The incidence of chipping fractures ranged from 0% in
two studies, both on Cercon zirconia at 2 years (21) and
3 years(22), to as high as 54% in just 1 year (20). No
brand of Y-TZP has escaped this problem, and it has
been reported in all seven brands of zirconia investi-
gated for crowns and bridges as follows: Cercon [15% in
5 years (10), 3% in 2 years (23), 3% in 15 years (24)];
Lava [25% in 25 years (25), 3% in 1 year (27) and 3%
in 2 years (26)]; IPS e.max ZirCAD [13% in 1 year
(28)]; Procera [2% in 3 years (30)]; DC-Zirkon [6% in
3 years(29), 15% in 2 years (4)]; Denzir [36% in
5 years (9), 54% in 1 year (20)] and Digizon [95% in
3 years (12)]. In some occasions, they occur at non-
load-bearing areas, and no set pattern has been iden-
tied so far, although the second molars have been
reported to have a higher incidence than the rest of the
dentition because of higher forces found at the posterior
of the mouth (25, 29).
It is important to appreciate that a large number of
chip fractures reported were undetected by the patients
and were an incidental nding during review appoint-
ments (4, 20, 27), and some patients were satised with
simply polishing the rough margins (23, 27), or repair-
ing the fracture with composite resin (12), while in
some cases, the patients chose not to have them
polished at all (25). Nevertheless, some restorations
did require total replacement because of major chipping
fractures which could not be polished or because they
posed aesthetic concerns (10, 30).
Chipping fractures can be a disappointment to both
the clinician and patient, and it has been noted in the
literature as a serious problem (43), instigating a large
number of studies investigating this phenomenon in
an attempt to solve it. Numerous reasons have been
suggested, such as mismatch of the CTE between the
veneering porcelain and the zirconia substructure
(44), mechanically defective micro-structural regions
in the porcelain, areas of porosities (28), surface
defects or improper support by the framework (43),
overloading and fatigue (45), low fracture toughness
of the veneering porcelain (46) and nally the low
thermal conductivity of zirconia (47). Delamination,
as opposed to chip fractures, has also been proposed as
a cause of failure. Delamination is the adhesive failure
between the veneering ceramic and zirconia, mani-
festing clinically as the complete loss of porcelain
partially exposing the substructure, although Ohl-
mann et al. (2008) argued that delamination can only
be conrmed after microscopic examination, which is
impossible if the restoration remains in situ, and
therefore it is quite possible that many fractures that
have been classied as delamination may in fact be
chipping fractures. This speculation is supported by
the evidence that the bond strength between zirconia
and a large number of veneering porcelains with
varying CTEs was higher than the cohesive strength of
the porcelain itself (44, 48, 49). Consequently, it has
been concluded that the veneering porcelain is the
weakest link, and improving its strength could reduce
the incidence of veneering porcelain chipping (44,
50). This was attempted by using high-strength heat-
pressed ceramics which have shown to have better
bond strengths to zirconia frameworks compared to
traditional layering ceramics and have been receiving
support in the literature (51). Aboushelib et al.(52)
described a double veneering technique which
combines the high bond strength of heat-pressed
ceramics with the superior aesthetics of layered
porcelain in an effort to improve the overall strength
and aesthetics of the veneering porcelain. Unfortu-
nately, chipping fractures have also been reported in
pressed porcelain in clinical trials on zirconia FPDs
and do not appear to have solved this chipping
problem (9, 28).
Swain (2009) (47) proposed that tempering residual
stress was the basis for the preponderance of chipping of
porcelain bonded to zirconia. He concluded that there
are three factors which contribute these residual
stresses and the unstable chipping fractures in zirconia:
mismatch of the higher thermal expansion coefcient
of porcelains bonded to zirconia; thickness of the
veneering porcelain and cooling rate. The cooling rate
after the removal of the sintered restoration from the
furnace, while the restoration is still at elevated
temperatures, generates signicant thermal gradients
within the porcelain and is directly related to the low
thermal conductivity of zirconia, which is much lower
than that of metal-alloys and even alumina ceramic,
which has not experienced similar incidences of chip-
ping fractures. He suggests that by more slowly cooling
the restoration above the glass transition temperature
of the porcelain, it is possible to prevent the develop-
ment of high tensile subsurface residual stresses in the
porcelain which may result in unstable cracking or
chipping. This approach of a reduced cooling rate after
B. AL - AML E H et al. 648
2010 Blackwell Publishing Ltd
the nal ring or glazing procedure is now recom-
mended by most dental material producers.
Improper design of the zirconia framework has also
been suggested to be a contributing factor in chipping
fractures, because of the inadequate support provided
by the thin zirconia copings commonly milled. Re-
cently, an improved customised zirconia-coping design
has been recommended by bulking out the substructure
to provide adequate support to the veneering porcelain.
This was demonstrated in a case report by Marchack
and colleagues (43), where the design of their zirconia
crowns was taken from the conventional PFM tech-
nique of a full contour wax-up which was then cut back
to allow for the veneering porcelain. An aesthetic
drawback would be the visible opaque white zirconia
along the palatal or lingual surfaces; however, the
authors argue that patient acceptance is high as soon as
they are given the choice between the appearance of a
metal margin or a white ceramic. Tinschert et al. (29)
adopted this modied framework design in their FPDs,
however, chipping fractures still occurred in 4 of 65
FPDs in their clinical trial spanning 3 years. Alteration
of the zirconia crystalline structures during sandblasting
prior to the veneering process was suggested by the
authors to be a possible reason why they had chipping
fractures, however, if that was the case, then complete
delamination of the porcelain would be expected rather
than chipping fracture of the supercial porcelain.
A novel approach in veneering zirconia copings has
been described by Beuer and colleagues (46) by
sintering a CAD CAM-milled lithium disilicate veneer
cap onto the zirconia coping signicantly increasing the
mechanical strength of the restoration. Other than
improved strength, they claimed this method to be a
cost-effective way of fabricating all-ceramic restora-
tions. To date, there are no clinical trials that have
adopted this method, and further in vitro studies are
needed before they can be clinically trialed.
Low-temperature degradation
Catastrophic failure of zirconia restorations has been a
major concern because of the inherent spontaneous
ageing problem of zirconia in the presence of water.
Low-temperature degradation (LTD) was rst described
by Kobayashi in 1981 (53), where in a humid envi-
ronment, spontaneous slow transformation from the
tetragonal phase to the more stable monoclinic phase
occurred in zirconia grains at relatively low tempera-
tures of 150400
C. This ageing process initiates at
surface grains and then later progresses towards the
bulk material causing a reduction in exural strength of
the material, putting it at risk of spontaneous cata-
strophic failure. How great a problem this ageing
process is going to be for zirconia restorations is
currently unknown. The vulnerability of zirconia to
ageing is exacerbated by the fact that its severity has
been shown to differ between different zirconias from
different manufacturers, and even in zirconia from the
same manufacturer but which have been processed
differently (54). This may be reected clinically, for
example, in the fractured zirconia frameworks reported
with Cercon zirconia, suggesting a possible weakness of
this brand compared to others, however, before this can
be conrmed, further studies with larger sample sizes
and following a longer review period must be com-
pleted; especially that each case of framework fracture
was caused by an initiating factor, such as accidentally
biting a stone, improper laboratory technique, insuf-
cient thickness of the zirconia coping and poor design,
which if avoided, a longer restoration life-time may
have been expected.
HIPed vs. non-Hiped zirconia
The type of blanks with which the zirconia restorations
are milled from have been suggested to have a direct
affect on the nal outcome of the restoration. Support-
ers of soft-milling using the non-HIPed zirconia claim
that hard-milling of HIPed zirconia could introduce
microcracks to the framework during the milling pro-
cess, reducing its overall physical strength and longevity
of the prosthesis (16). This was not evident in the
published clinical trials; in contrast, zirconia cata-
strophic fractures have only been reported in non-
HIPed zirconia and not in HIPed zirconia. On the other
hand, HIPed zirconia supporters claimsuperior marginal
t because no shrinkage is involved in the manufactur-
ing process, and precise margins are not possible with
non-HIPed zirconia, giving rise to recurrent caries,
periodontal conditions and unaesthetic margins. Sailer
et al. (2007) reported the highest incidence of secondary
caries (22%) in a non-HIPed zirconia
FPDs after a 5-
year follow-up, suggested to be because of using a
prototype soft-milling method which has since been
improved. Notably, no other study reported a high
Cercon zirconia, Dentsply Degudent, Hanau, Germany.
C L I NI C AL T R I AL S I N Z I R C ONI A 649
2010 Blackwell Publishing Ltd
incidence of caries, even when using non-HIPed zirco-
nia. Reich and colleagues (55) examined the clinical t
of 4-unit posterior FPDs made by non-HIPed zirconia
and found a median marginal gap of 77 lm in 24 FPDs,
well within the clinically acceptable marginal gap limit
of 100120 lm (56). Further, in vivo studies with larger
sample sizes and longer follow-up periods are needed to
establish any signicant differences between HIPed and
non-HIPed zirconia restorations; and although more
dental zirconia manufacturers supply non-HIPed Y-
TZP, so far clinical results are in favour of HIPed
zirconia because of the absence of any framework failures
in the short-term.
The future of zirconia
Case reports of large multi-unit tooth and implant FPDs
suggest that the dental community may have some
condence in zirconia as a restorative material, with
some authors restoring full mouth rehabilitations using
zirconia abutments and frameworks despite limited
scientic evidence (5759).
The issue of porcelain chipping appears to be germane
to zirconia frameworks despite their intrinsic superior
mechanical properties and that porcelain mechanical
properties are almost framework independent. Despite
this apparent anomaly methods of strengthening the
veneering porcelain are being developed to control the
unstable chipping fractures. These include novel con-
cepts that are being reported in the literature, such as
the high-strength CAD CAM-fabrication of the veneer-
ing porcelain (46) and the double veneering tech-
nique (52). Other approaches include bulking out the
zirconia framework and omitting veneering porcelain at
non-aesthetic areas such as the lingual and palatal
aspects of the restoration.
At this time, investigations appear to have been
directed towards zirconia materials with stabilisers
other than yttria which are less prone to LTD, such as
magnesia partially stabilized zirconia (Mg-PSZ) (60) and
ceria-stabilized zirconia alumina nanocomposites
(Ce-TZP A) (61). These non-yttria-stabilized zirconia
materials may be less susceptible to LTD and spontane-
ous phase transformation, however, their fracture
toughness and exural strengths are not as high as Y-
TZP and so they may not be suitable for medium to
long-span FPDs. Therefore, long-term in vivo studies
must be carefully evaluated before non-yttria-stabilized
zirconia materials could be recommended.
Conclusion
1 Based on the limited short-term studies available,
zirconia can be said to be suitable for the fabrication
of all-ceramic posterior single crowns, long-span
FPDs and implant abutments.
2 Inlay-retained FPDs cannot be recommended in light
of published in vivo trials.
3 Chipping of the veneering porcelain is conrmed to
be an ongoing problem with zirconia all-ceramic-
based restorations.
4 Zirconia framework fractures have only been reported
in soft-milled non-HIPed zirconia, with a possible
advantage being seen in hard-milling HIPed zirconia.
5 Zirconia-based all-ceramic restorations can be
cemented with conventional luting cements, how-
ever, bonding to tooth structure is also possible but
with limited success.
Conicts of interest
The authors declare no conicts of interests.
References
1. Spear F. The metal-free practice: myth? Reality desirable goal?
J Esthet Restor Dent. 2001;13:5967.
2. Studart AR, Filser F, Kocher P, Gauckler LJ. In vitro lifetime of
dental ceramics under cyclic loading in water. Biomaterials.
2007;28:26952705.
3. McLean JW, Hughes TH. The reinforcement of dental
porcelain with ceramic oxides. Br Dent J. 1965;119:
251267.
4. Vult von Steyern P, Carlson P, Nilner K. All-ceramic xed
partial dentures designed according to the DC-Zirkon
technique. A -year clinical study. J Oral Rehabil. 2005;32:
180187.
5. Denry I, Kelly J. State of the art zirconia for dental applica-
tions. Dent Mater. 2008;24:299307.
6. Piconi C, Maccauro G. Zirconia as a ceramic biomaterial.
Biomaterials. 1999;20:125.
7. Christel P, Meunier A, Heller M, Torre J, Peille C. Mechanical
properties and short-term in vivo evaluation of yttrium-oxide-
partially-stabilized zirconia. J Biomed Mater Res. 1989;23:
4561.
8. Meyenberg K, Luthy H, Scharer P. Zirconia posts: a new all-
ceramic concept for nonvital abutment teeth. J Esthet Dent.
1995;7:7380.
9. Molin MK, Karlsson SL. Five-year clinical prospective evalu-
ation of zirconia-based Denzir 3-unit FPDs. Int J Prosthodont.
2008;21:223227.
10. Sailer I, Feher A, Filser F, Gauckler LJ, Luthy H, Hammerle
CH. Five-year clinical results of zirconia frameworks for
B. AL - AML E H et al. 650
2010 Blackwell Publishing Ltd
posterior xed partial dentures. Int J Prosthodont.
2007;20:383388.
11. Sailer I, Feher A, Filser F, Luthy H, Gauckler LJ, Scharer P
et al. Prospective clinical study of zirconia posterior xed
partial dentures: 3-year follow-up. Quintessence Int.
2006;37:685693.
12. Edelhoff D, Florian B, Florian W, Johnen C. HIP zirconia xed
partial denturesclinical results after 3 years of clinical service.
Quintessence Int. 2008;39:459471.
13. Glauser R, Sailer I, Wohlwend A, Studer S, Schibli M, Scharer
P. Experimental zirconia abutments for implant-supported
single-tooth restorations in esthetically demanding regions: 4-
year results of a prospective clinical study. Int J Prosthodont.
2004;17:285290.
14. Zembic A, Sailer I, Jung R, Ha mmerle C. Randomized-
controlled clinical trial of customized zirconia and titanium
implant abutments for single-tooth implants in canine and
posterior regions: 3-year results. Clin Oral Implants Res.
2009;20:802808.
15. Wenz H, Bartsch J, Wolfart S, Kern M. Osseointegration and
clinical success of zirconia dental implants: a systematic
review. Int J Prosthodont. 2008;21:2736.
16. Raigrodski AJ. Contemporary all-ceramic xed partial den-
tures: a review. Dent Clin North Am. 2004;48:531544.
17. Guazzato M, Albakry M, Ringer SP, Swain MV. Strength,
fracture toughness and microstructure of a selection of all-
ceramic materials. Part II. Zirconia-based dental ceramics.
Dent Mater. 2004;20:449456.
18. Studart AR, Filser F, Kocher P, Luthy H, Gauckler LJ. Cyclic
fatigue in water of veneer-framework composites for
all-ceramic dental bridges. Dent Mater. 2007;23:177185.
19. Kelly J, Denry I. Stabilized zirconia as a structural ceramic: an
overview. Dent Mater. 2008;24:289298.
20. Larsson C, Vult von Steyern P, Sunzel B, Nilner K. All-ceramic
two- to ve-unit implant-supported reconstructions. A
randomized, prospective clinical trial. Swed Dent J. 2006;30:
4553.
21. C ehreli M, Ko kat A, Akca K. CAD CAM Zirconia vs. slip-cast
glass-inltrated Alumina Zirconia all-ceramic crowns: 2-year
results of a randomized controlled clinical trial. J Appl Oral
Sci. 2009;17:4955.
22. Beuer F, Edelhoff D, Gernet W, Sorensen J. Three-year
clinical prospective evaluation of zirconia-based posterior
xed dental prostheses (FDPs). Clin Oral Investig.
2009;13:445451.
23. Schmitter M, Mussotter K, Rammelsberg P, Stober T, Ohl-
mann B, Gabbert O. Clinical performance of extended zirconia
frameworks for xed dental prostheses: two-year results.
J Oral Rehabil. 2009;36:610615.
24. Bornemann G. Prospective Clinical Trial with Conventionally
Luted Zirconia-based Fixed Partial Dentures18-month Re-
sults. J Dent Res. 2003;82:117 (Sp issue B).
25. Raigrodski AJ, Chiche GJ, Potiket N, Hochstedler JL, Moham-
ed SE, Billiot S et al. The efcacy of posterior three-unit
zirconium-oxide-based ceramic xed partial dental prosthe-
ses: a prospective clinical pilot study. J Prosthet Dent.
2006;96:237244.
26. Pospiech P, Rountree P, Nothdurft F. Clinical evaluation of
zirconia-based all-ceramic posterior bridges: two-year results.
J Dent Res. 2003;82:114.
27. Crisp RJ, Cowan AJ, Lamb J, Thompson O, Tulloch N, Burke
FJ. A clinical evaluation of all-ceramic bridges placed in UK
general dental practices: rst-year results. Br Dent J.
2008;205:477482.
28. Ohlmann B, Rammelsberg P, Schmitter M, Schwarz S,
Gabbert O. All-ceramic inlay-retained xed partial dentures:
preliminary results from a clinical study. J Dent. 2008;36:
692696.
29. Tinschert J, Schulze KA, Natt G, Latzke P, Heussen N,
Spiekermann H. Clinical behavior of zirconia-based xed
partial dentures made of DC-Zirkon: 3-year results. Int J
Prosthodont. 2008;21:217222.
30. O
rtorp A, Kihl M, Carlsson G. A 3-year retrospective and
clinical follow-up study of zirconia single crowns performed in
a private practice. J Dent. 2009;37:731736.
31. Sailer I, Zembic A, Jung R, Siegenthaler D, Holderegger C,
Hammerle C. Randomized controlled clinical trial of custom-
ized zirconia and titanium implant abutments for canine and
posterior single-tooth implant reconstructions: preliminary
results at 1 year of function. Clin Oral Implants Res.
2009;20:219225.
32. Norton MR. An in vitro evaluation of the strength of an
internal conical interface compared to a butt joint interface
in implant design. Clin Oral Implants Res. 1997;8:
290298.
33. Fischer H, Weber M, Marx R. Lifetime prediction of all-
ceramic bridges by computational methods. J Dent Res.
2003;82:238242.
34. Taskonak B, Yan J, Mecholsky JJ Jr, Sertgoz A, Kocak A.
Fractographic analyses of zirconia-based xed partial den-
tures. Dent Mater. 2008;24:10771082.
35. Raigrodski A. Contemporary materials and technologies for
all-ceramic xed partial dentures: a review of the literature.
J Prosthet Dent. 2004;92:557562.
36. Kelly JR, Tesk JA, Sorensen JA. Failure of all-ceramic xed
partial dentures in vitro and in vivo: analysis and modeling.
J Dent Res. 1995;74:12531258.
37. Oh W, Gotzen N, Anusavice KJ. Inuence of connector design
on fracture probability of ceramic xed-partial dentures.
J Dent Res. 2002;81:623627.
38. Taskonak B, Mecholsky JJ Jr, Anusavice KJ. Fracture surface
analysis of clinically failed xed partial dentures. J Dent Res.
2006;85:277281.
39. Ohlmann B, Gabbert O, Schmitter M, Gilde H, Rammelsberg
P. Fracture resistance of the veneering on inlay-retained
zirconia ceramic xed partial dentures. Acta Odontol Scand.
2005;63:335342.
40. Giordano R. Materials for chairside CAD CAM-produced
restorations. J Am Dent Assoc. 2006;137:14S21S.
41. Wolfart S, Kern M. A new design for all-ceramic inlay-
retained xed partial dentures: a report of 2 cases. Quintes-
sence Int. 2006;37:2733.
42. Ohlmann B, Marienburg K, Gabbert O, Hassel A, Gilde H,
Rammelsberg P. Fracture-load values of all-ceramic cantile-
C L I NI C AL T R I AL S I N Z I R C ONI A 651
2010 Blackwell Publishing Ltd
vered FPDs with different framework designs. Int J Prosth-
odont. 2009;22:4952.
43. Marchack BW, Futatsuki Y, Marchack CB, White SN. Cus-
tomization of milled zirconia copings for all-ceramic crowns: a
clinical report. J Prosthet Dent. 2008;99:169173.
44. Fischer J, Stawarzcyk B, Trottmann A, Hammerle CH.
Impact of thermal mist on shear strength of veneering
ceramic zirconia composites. Dent Mater. 2009;25:419423.
45. Coelho PG, Silva NR, Bonfante EA, Guess PC, Rekow ED,
Thompson VP. Fatigue testing of two porcelain-zirconia
all-ceramic crown systems. Dent Mater. 2009;25:11221127.
46. Beuer F, Schweiger J, Eichberger M, Kappert HF, Gernet W,
Edelhoff D. High-strength CAD CAM-fabricated veneering
material sintered to zirconia copingsa new fabrication mode
for all-ceramic restorations. Dent Mater. 2009;25:121128.
47. Swain MV. Unstable cracking (chipping) of veneering porce-
lain on all-ceramic dental crowns and xed partial dentures.
Acta Biomater. 2009;5:16681677.
48. Al-Dohan HM, Yaman P, Dennison JB, Razzoog ME, Lang BR.
Shear strength of core-veneer interface in bi-layered ceramics.
J Prosthet Dent. 2004;91:349355.
49. Tsalouchou E, Cattell MJ, Knowles JC, Pittayachawan P,
McDonald A. Fatigue and fracture properties of yttria partially
stabilized zirconia crown systems. Dent Mater. 2008;24:
308318.
50. Ashkanani HM, Raigrodski AJ, Flinn BD, Heindl H, Mancl LA.
Flexural and shear strengths of ZrO2 and a high-noble alloy
bonded to their corresponding porcelains. J Prosthet Dent.
2008;100:274284.
51. Aboushelib MN, Kleverlaan CJ, Feilzer AJ. Microtensile bond
strength of different components of core veneered all-ceramic
restorations. Part II: Zirconia veneering ceramics. Dent Mater.
2006;22:857863.
52. Aboushelib MN, Kleverlaan CJ, Feilzer AJ. Microtensile bond
strength of different components of core veneered all-ceramic
restorations. Part 3: double veneer technique. J Prosthodont.
2008;17:913.
53. Kobayashi K, Kuwajima H, Masaki T. Phase change and
mechanical properties of ZrO2-Y2O3 solid electrolyte after
aging. Solid State Ionics. 1981;3:489493.
54. Chevalier J. What future for zirconia as a biomaterial?
Biomaterials. 2006;27:535543.
55. Reich S, Kappe K, Teschner H, Schmitt J. Clinical t of four-
unit zirconia posterior xed dental prostheses. Eur J Oral Sci.
2008;116:579584.
56. McLean JW, von Fraunhofer JA. The estimation of cement
lm thickness by an in vivo technique. Br Dent J. 1971;131:
107111.
57. Dunn DB. The use of a zirconia custom implant-supported
xed partial denture prosthesis to treat implant failure in the
anterior maxilla: a clinical report. J Prosthet Dent.
2008;100:415421.
58. Chang PP, Henegbarth EA, Lang LA. Maxillary zirconia
implant xed partial dentures opposing an acrylic resin
implant xed complete denture: a two-year clinical report. J
Prosthet Dent. 2007;97:321330.
59. Nam J, Raigrodski AJ, Heindl H. Utilization of multiple
restorative materials in full-mouth rehabilitation: a clinical
report. J Esthet Restor Dent. 2008;20:251263.
60. Sundh A, Sjogren G. Fracture resistance of all-ceramic
zirconia bridges with differing phase stabilizers and quality
of sintering. Dent Mater. 2006;22:778784.
61. Fischer J, Stawarczyk B, Trottmann A, Hammerle CH. Impact
of thermal properties of veneering ceramics on the fracture
load of layered Ce-TZP A nanocomposite frameworks. Dent
Mater. 2009;25:326330.
Correspondence: Basil Al-Amleh, Department of Oral Rehabilitation,
Faculty of Dentistry, University of Otago, PO Box 647, Dunedin 9054,
New Zealand. E-mail: alamleh@gmail.com
B. AL - AML E H et al. 652
2010 Blackwell Publishing Ltd
Você também pode gostar
- Zirconia-Based Ceramics and VM9 Veneering PorcelainDocumento13 páginasZirconia-Based Ceramics and VM9 Veneering PorcelainJafar SadiqAinda não há avaliações
- Occlusal Adjustment Technique Made Simple: Masticatory System and Occlusion As It Relates to Function and How Occlusal Adjustment Can Help Treat Primary and Secondary Occlusal TraumaNo EverandOcclusal Adjustment Technique Made Simple: Masticatory System and Occlusion As It Relates to Function and How Occlusal Adjustment Can Help Treat Primary and Secondary Occlusal TraumaAinda não há avaliações
- Materiale Ceramice in StomatologieDocumento23 páginasMateriale Ceramice in StomatologieMogos PaulAinda não há avaliações
- Fundamentals of Tooth Preparation PDFDocumento74 páginasFundamentals of Tooth Preparation PDFAyesha AwanAinda não há avaliações
- All Ceramic (Part 1)Documento41 páginasAll Ceramic (Part 1)Faisal Ali BalochAinda não há avaliações
- Metal Ceramic Crown Has Always Been The Most Popular Complete Veneer Restoration in DentistryDocumento3 páginasMetal Ceramic Crown Has Always Been The Most Popular Complete Veneer Restoration in DentistryFlorian LitaAinda não há avaliações
- Dental Ceramics For Restoration and Metal VeneeringDocumento23 páginasDental Ceramics For Restoration and Metal VeneeringMichael XuAinda não há avaliações
- PeekDocumento8 páginasPeeksalmaAinda não há avaliações
- Dental Cements For Definitive LutingDocumento16 páginasDental Cements For Definitive LutingParmod GuliaAinda não há avaliações
- Digitalization in Dentistry CADCAM A ReviewDocumento6 páginasDigitalization in Dentistry CADCAM A ReviewnabeghAinda não há avaliações
- ZirconiaDocumento8 páginasZirconiaAmitAinda não há avaliações
- All You Need to Know About Zirconium Dental ImplantsDocumento5 páginasAll You Need to Know About Zirconium Dental ImplantsCostin VasilescuAinda não há avaliações
- Difficulties in Complete Denture Construction & Solutions IIDocumento13 páginasDifficulties in Complete Denture Construction & Solutions IIIndrani DasAinda não há avaliações
- Ceramics in Dental RestorationsDocumento11 páginasCeramics in Dental RestorationsDaniel CostinAinda não há avaliações
- Ceramic Inlays A Case Presentation and LessonsDocumento11 páginasCeramic Inlays A Case Presentation and LessonsStef David100% (1)
- Resin Bonded Fixed Dental ProsthesisDocumento48 páginasResin Bonded Fixed Dental ProsthesismanasviAinda não há avaliações
- 1) Introduction To Pre Clinical Complete Denture PDFDocumento56 páginas1) Introduction To Pre Clinical Complete Denture PDFMustafa AhmedAinda não há avaliações
- Cad CamDocumento5 páginasCad CamsauriuaAinda não há avaliações
- Kutler's Thery PDFDocumento10 páginasKutler's Thery PDFSam RoyAinda não há avaliações
- 13 Implant Supported Fixed ProsthesesDocumento52 páginas13 Implant Supported Fixed ProsthesesJúliaJulieAinda não há avaliações
- The Historical Evolution of Dental Impression MaterialsDocumento11 páginasThe Historical Evolution of Dental Impression MaterialsHassanein Al-Hamdani100% (1)
- Dental Ceramics Seminar on All-CeramicsDocumento32 páginasDental Ceramics Seminar on All-CeramicsnjucyAinda não há avaliações
- Tooth Preparation Design and PrinciplesDocumento80 páginasTooth Preparation Design and PrinciplesAnonymous ceYk4p4100% (2)
- Magnification and IlluminationDocumento22 páginasMagnification and Illuminationwhussien7376100% (1)
- Iti ImplantDocumento8 páginasIti ImplantMuaiyed Buzayan AkremyAinda não há avaliações
- Basic Properties and Types of Zirconia: An OverviewDocumento8 páginasBasic Properties and Types of Zirconia: An OverviewAndrea PrestiAinda não há avaliações
- Dental Materials & Prosthodontics ReferencesDocumento5 páginasDental Materials & Prosthodontics ReferencesratiAinda não há avaliações
- Tehnica Bulk FillDocumento6 páginasTehnica Bulk FillVictor MarcautanAinda não há avaliações
- Ultrasonics in Endodontics.Documento43 páginasUltrasonics in Endodontics.moatazendo100% (1)
- Dental ImpressionDocumento26 páginasDental ImpressionArthi Ramalingam aAinda não há avaliações
- Classifications of Dental Ceramics (Autosaved)Documento52 páginasClassifications of Dental Ceramics (Autosaved)Muralidharan100% (1)
- Dental CeramicsDocumento26 páginasDental CeramicsDarshilAinda não há avaliações
- Clinical Guide: All Ceramic All You NeedDocumento44 páginasClinical Guide: All Ceramic All You NeedMarcelo EnsigniaAinda não há avaliações
- Modern Endodontic PracticeDocumento335 páginasModern Endodontic PracticeMiguel Jaèn100% (1)
- 3M ESPE Filtek Bulk Fill Technical Profile - LRDocumento24 páginas3M ESPE Filtek Bulk Fill Technical Profile - LRelokfaiqAinda não há avaliações
- Consideratii Clinice Privind Restauratiile ProtetiDocumento5 páginasConsideratii Clinice Privind Restauratiile ProtetivalentinanlAinda não há avaliações
- Richmond CrownDocumento5 páginasRichmond Crownndra16Ainda não há avaliações
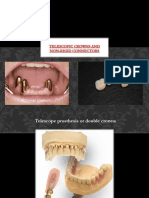
- Telescopic Crowns and Non-Rigid ConnectorsDocumento17 páginasTelescopic Crowns and Non-Rigid ConnectorsCha Xue ChinAinda não há avaliações
- Oral Rehabilitation With Removable Partial Dentures in Advanced Tooth Loss SituationsDocumento7 páginasOral Rehabilitation With Removable Partial Dentures in Advanced Tooth Loss SituationsIoana-NicoletaNicodimAinda não há avaliações
- Application of The Rotational Path Design Concept To A Removable Partial Denture With A Distal-Extension BaseDocumento3 páginasApplication of The Rotational Path Design Concept To A Removable Partial Denture With A Distal-Extension BaseChepe LemusAinda não há avaliações
- CAD/CAM Dental Restorations ReviewedDocumento7 páginasCAD/CAM Dental Restorations ReviewedLjubomirErdoglijaAinda não há avaliações
- Esthetic Rehabilitation of A Worn Dentition With A Minimally Invasive Prost... : EBSCOhostDocumento21 páginasEsthetic Rehabilitation of A Worn Dentition With A Minimally Invasive Prost... : EBSCOhostNaoki Mezarina100% (1)
- InLine PoM Edition GruebelDocumento28 páginasInLine PoM Edition GruebelFabio WenoAinda não há avaliações
- Magnification in EndodonticsDocumento53 páginasMagnification in Endodonticsdurga7100% (1)
- Introd: Venire Ape Piata Si Descoperirea Zirconiului Struc Mat Interact Cu Mat Cu Care Vin in ContactDocumento8 páginasIntrod: Venire Ape Piata Si Descoperirea Zirconiului Struc Mat Interact Cu Mat Cu Care Vin in ContactRusu CosminaAinda não há avaliações
- IPS E-Max Press PDFDocumento40 páginasIPS E-Max Press PDFKianoosh EmamzadehAinda não há avaliações
- IPS E.maxDocumento32 páginasIPS E.maxKhaled ElshabrawyAinda não há avaliações
- Avadent Article Loma LindaDocumento8 páginasAvadent Article Loma LindaRoxana LupuAinda não há avaliações
- Obturation Techniques - CastelucciDocumento7 páginasObturation Techniques - CasteluccikariAinda não há avaliações
- Concepts of Arrangement of Artifical Teeth, SelectiveDocumento7 páginasConcepts of Arrangement of Artifical Teeth, SelectiveAmar BhochhibhoyaAinda não há avaliações
- Variolink+Esthetic LC - Glass Ceramic Restorations - Flow Chart - enDocumento2 páginasVariolink+Esthetic LC - Glass Ceramic Restorations - Flow Chart - engmacaneataAinda não há avaliações
- 1proteza Partiala Mobilizabila, Nevoia Clinica de Inovare 2017 Journal of Prosthetic DentistryDocumento8 páginas1proteza Partiala Mobilizabila, Nevoia Clinica de Inovare 2017 Journal of Prosthetic DentistrydanielaAinda não há avaliações
- Prosthodontics Definition and BranchesDocumento42 páginasProsthodontics Definition and BranchesSangeetha BommineniAinda não há avaliações
- Articulators and facial archesDocumento124 páginasArticulators and facial archesBogdan DumitrachiAinda não há avaliações
- Metal CeramicsDocumento62 páginasMetal CeramicsSai Kumar67% (3)
- Class II Cavity PreperationDocumento44 páginasClass II Cavity Preperationirfanuk69Ainda não há avaliações
- Inlays and Onlays ReportDocumento32 páginasInlays and Onlays ReportAlnielJoManlapigAinda não há avaliações
- All Ceramic Materials Guide for Dental RestorationsDocumento6 páginasAll Ceramic Materials Guide for Dental RestorationsMahaAhmedAinda não há avaliações
- Relining and Rebasing in Complete DenturesDocumento58 páginasRelining and Rebasing in Complete DenturesJASPREETKAUR0410Ainda não há avaliações
- Bonding Performance of Universal Adhesives in Different Etching ModesDocumento9 páginasBonding Performance of Universal Adhesives in Different Etching ModesRitter Adolfo OlivaresAinda não há avaliações
- Utilization of Ethyl Cyanoacrylate and 2-Octyl Cyanoacrylate Adhesives For Autogenous Bone GR Fixation - Histomorphometric StudyDocumento9 páginasUtilization of Ethyl Cyanoacrylate and 2-Octyl Cyanoacrylate Adhesives For Autogenous Bone GR Fixation - Histomorphometric StudyAna Massiel NarváezAinda não há avaliações
- Adhesion To Tooth Structure Mediated by Contemporary Bonding Systems.Documento18 páginasAdhesion To Tooth Structure Mediated by Contemporary Bonding Systems.Sadeer RiyadhAinda não há avaliações
- 2 MICROMORPHOLOGICAL EFFECTS AND THE THICKNESS OF THE HYBRID LAYER Skupien, 2010Documento9 páginas2 MICROMORPHOLOGICAL EFFECTS AND THE THICKNESS OF THE HYBRID LAYER Skupien, 2010Ana Massiel NarváezAinda não há avaliações
- Human Cementum Protein 1 Induces Expression of Bone and Cementum Proteins by Human Gingival FibroblastsDocumento7 páginasHuman Cementum Protein 1 Induces Expression of Bone and Cementum Proteins by Human Gingival FibroblastsAna Massiel NarváezAinda não há avaliações
- Direct and Indirect Restorative Materials PDFDocumento10 páginasDirect and Indirect Restorative Materials PDFAna Massiel NarváezAinda não há avaliações
- Doc-20201220-Wa0 221210 104536Documento10 páginasDoc-20201220-Wa0 221210 104536Ana Massiel NarváezAinda não há avaliações
- An Overview of Dental Adhesive Systems and The Dynamic Tooth-Adhesive InterfaceDocumento19 páginasAn Overview of Dental Adhesive Systems and The Dynamic Tooth-Adhesive InterfaceLynda M. NaranjoAinda não há avaliações
- Cements and Adhesives For All-Ceramic RestorationsDocumento22 páginasCements and Adhesives For All-Ceramic RestorationsViviana Florez PantojaAinda não há avaliações
- Effect of Static and Cyclic Loading On CeramicDocumento10 páginasEffect of Static and Cyclic Loading On CeramicAciih HeHoAinda não há avaliações
- Effect of Self-Curing Activators and Curing Protocols On Adhesive Properties of Universal Adhesives Bonded To Dual-Cured CompositesDocumento13 páginasEffect of Self-Curing Activators and Curing Protocols On Adhesive Properties of Universal Adhesives Bonded To Dual-Cured CompositesAna Massiel NarváezAinda não há avaliações
- Biomechanical Response of Retrodiscal Tissue in The Temporomandibular Joint Under CompressionDocumento6 páginasBiomechanical Response of Retrodiscal Tissue in The Temporomandibular Joint Under CompressionAna Massiel NarváezAinda não há avaliações
- Product News: Practice Overheads Expenses Insurance Touchless Treatment ConsentDocumento1 páginaProduct News: Practice Overheads Expenses Insurance Touchless Treatment ConsentAna Massiel NarváezAinda não há avaliações
- Self-Adhesive Resin Cements - Adhesive Performance To Indirect Restorative CeramicsDocumento7 páginasSelf-Adhesive Resin Cements - Adhesive Performance To Indirect Restorative CeramicsAna Massiel NarváezAinda não há avaliações
- Review of The Mechanism of Tooth WhiteningDocumento19 páginasReview of The Mechanism of Tooth WhiteningAna Massiel Narváez100% (1)
- Effectiveness of Exercise Therapy in Patients With Myofascial Pain Dysfunction SyndromeDocumento8 páginasEffectiveness of Exercise Therapy in Patients With Myofascial Pain Dysfunction SyndromeAna Massiel NarváezAinda não há avaliações
- Dental Adhesion Review-BreschiDocumento12 páginasDental Adhesion Review-BreschiAna Massiel NarváezAinda não há avaliações
- Dental Adhesion Review-BreschiDocumento12 páginasDental Adhesion Review-BreschiAna Massiel NarváezAinda não há avaliações
- Dental Adhesion Review-BreschiDocumento12 páginasDental Adhesion Review-BreschiAna Massiel NarváezAinda não há avaliações
- 05 Goodacre 1994 Review Part 1Documento8 páginas05 Goodacre 1994 Review Part 1Ana Massiel NarváezAinda não há avaliações
- He Effect of 2-Butyl-Cyanoacrylate Adhesive in Osteotomies and Bone Grafts in Rabbits - Macroscopic and Radiographic CharacteristicsDocumento8 páginasHe Effect of 2-Butyl-Cyanoacrylate Adhesive in Osteotomies and Bone Grafts in Rabbits - Macroscopic and Radiographic CharacteristicsAna Massiel NarváezAinda não há avaliações
- Dental Adhesion Review-BreschiDocumento12 páginasDental Adhesion Review-BreschiAna Massiel NarváezAinda não há avaliações
- Dentine HypersensitivityDocumento9 páginasDentine HypersensitivityAna Massiel NarváezAinda não há avaliações
- Dentine HypersensitivityDocumento9 páginasDentine HypersensitivityAna Massiel NarváezAinda não há avaliações
- Orthodontic Extrusionforimplantsite Development Revisited-Anewclassification Determined ByanatomyandclinicaloutcomesDocumento20 páginasOrthodontic Extrusionforimplantsite Development Revisited-Anewclassification Determined ByanatomyandclinicaloutcomesAna Massiel NarváezAinda não há avaliações
- Prosthetic Rehabilitation and Treatment Outcome of Partially Edentulous Patients With Severe Tooth Wear - 3-Years ResultsDocumento10 páginasProsthetic Rehabilitation and Treatment Outcome of Partially Edentulous Patients With Severe Tooth Wear - 3-Years ResultsAna Massiel NarváezAinda não há avaliações
- Dentine HypersensitivityDocumento9 páginasDentine HypersensitivityAna Massiel NarváezAinda não há avaliações
- Recubrimiento TitanioDocumento2 páginasRecubrimiento TitanioAna Massiel NarváezAinda não há avaliações
- Single Distal Implant RestorationDocumento10 páginasSingle Distal Implant RestorationAna Massiel NarváezAinda não há avaliações
- The Septuagint A Critical AnalysisDocumento76 páginasThe Septuagint A Critical AnalysisscaunasAinda não há avaliações
- Laertes' Temper: Definition of DiacopeDocumento27 páginasLaertes' Temper: Definition of DiacopeAhmad Abdellah ElsheemiAinda não há avaliações
- Research Planning: Content, Steps, and Structural ComponentsDocumento18 páginasResearch Planning: Content, Steps, and Structural ComponentsAndrei GS ZapshaAinda não há avaliações
- RepigmentationDocumento4 páginasRepigmentationMariyaAinda não há avaliações
- CMT 565:waste and Wastewater Technology: Experiment No: 5 Title: Biochemical Oxygen Demand (Bod)Documento4 páginasCMT 565:waste and Wastewater Technology: Experiment No: 5 Title: Biochemical Oxygen Demand (Bod)kuekAinda não há avaliações
- Factors Affecting Customer Loyalty to Indosat OoredooDocumento13 páginasFactors Affecting Customer Loyalty to Indosat OoredooDede BhubaraAinda não há avaliações
- Professional Teaching ResumeDocumento2 páginasProfessional Teaching Resumeapi-535361896Ainda não há avaliações
- The Oikos in Athenian LawDocumento13 páginasThe Oikos in Athenian LawTúlio CarvalhoAinda não há avaliações
- Seduction As A Manipulation TacticDocumento6 páginasSeduction As A Manipulation TacticByrlyne Van DykeDowersAinda não há avaliações
- Management Review, 32: 794-816.: Daftar PustakaDocumento8 páginasManagement Review, 32: 794-816.: Daftar PustakaNurulsalamah28Ainda não há avaliações
- Module 1 Sociological PerspectivesDocumento39 páginasModule 1 Sociological PerspectivesCristine BalocaAinda não há avaliações
- Transportasi Kelembagaan PengantarDocumento26 páginasTransportasi Kelembagaan Pengantarade wiraAinda não há avaliações
- Case - 1 Marketing and Distribution of MushroomDocumento2 páginasCase - 1 Marketing and Distribution of MushroomKetan BohraAinda não há avaliações
- Flowera, Fruits and SeedsDocumento66 páginasFlowera, Fruits and SeedsNikkaMontil100% (1)
- Ethics Module 1-7Documento57 páginasEthics Module 1-7Maey RoledaAinda não há avaliações
- Training MaterialDocumento151 páginasTraining MaterialNarendrareddy RamireddyAinda não há avaliações
- English March 3Documento7 páginasEnglish March 3Richard ManongsongAinda não há avaliações
- Nokia CaseDocumento28 páginasNokia CaseErykah Faith PerezAinda não há avaliações
- 1000arepas Maythuna Aceituna Una YogaDocumento164 páginas1000arepas Maythuna Aceituna Una YogaDaniel Medvedov - ELKENOS ABE100% (1)
- Treasures Book 1 Unit 1Documento33 páginasTreasures Book 1 Unit 1Janinne AbuegAinda não há avaliações
- Case Epidural HematomaDocumento16 páginasCase Epidural HematomaBahRunAinda não há avaliações
- United States v. Calvin Antonio Spencer, 68 F.3d 462, 4th Cir. (1995)Documento4 páginasUnited States v. Calvin Antonio Spencer, 68 F.3d 462, 4th Cir. (1995)Scribd Government DocsAinda não há avaliações
- Bio 140 Exam 4 ReviewDocumento7 páginasBio 140 Exam 4 Reviewlp_blackoutAinda não há avaliações
- Assessing The NeckDocumento3 páginasAssessing The NeckAnne Joyce Lara AlbiosAinda não há avaliações
- TGT EnglishDocumento3 páginasTGT EnglishKatta SrinivasAinda não há avaliações
- Function Point and Cocomo ModelDocumento31 páginasFunction Point and Cocomo ModelParinyas SinghAinda não há avaliações
- Clinical Mental Health Counseling in Community and Agency Settings 5Th Edition Full ChapterDocumento41 páginasClinical Mental Health Counseling in Community and Agency Settings 5Th Edition Full Chapterwilliam.kellar832100% (24)
- (13-14) - Modeling of Thermal SystemsDocumento33 páginas(13-14) - Modeling of Thermal SystemsmawooaAinda não há avaliações
- SSC 146G Summer 2016 Human Sexuality SyllabusDocumento1 páginaSSC 146G Summer 2016 Human Sexuality SyllabusJames SmithAinda não há avaliações
- Magnolia Residences Tower D Promo - 20% Downpayment OptionDocumento1 páginaMagnolia Residences Tower D Promo - 20% Downpayment OptionLiv ValdezAinda não há avaliações
- Piping and Pipeline Calculations Manual: Construction, Design Fabrication and ExaminationNo EverandPiping and Pipeline Calculations Manual: Construction, Design Fabrication and ExaminationNota: 4 de 5 estrelas4/5 (18)
- Transportation Engineering: Theory, Practice, and ModelingNo EverandTransportation Engineering: Theory, Practice, and ModelingAinda não há avaliações
- The Things We Make: The Unknown History of Invention from Cathedrals to Soda CansNo EverandThe Things We Make: The Unknown History of Invention from Cathedrals to Soda CansAinda não há avaliações
- To Engineer Is Human: The Role of Failure in Successful DesignNo EverandTo Engineer Is Human: The Role of Failure in Successful DesignNota: 4 de 5 estrelas4/5 (137)
- Methodology for Estimating Carbon Footprint of Road Projects: Case Study: IndiaNo EverandMethodology for Estimating Carbon Footprint of Road Projects: Case Study: IndiaAinda não há avaliações
- Crossings: How Road Ecology Is Shaping the Future of Our PlanetNo EverandCrossings: How Road Ecology Is Shaping the Future of Our PlanetNota: 4.5 de 5 estrelas4.5/5 (10)
- The Great Bridge: The Epic Story of the Building of the Brooklyn BridgeNo EverandThe Great Bridge: The Epic Story of the Building of the Brooklyn BridgeNota: 4.5 de 5 estrelas4.5/5 (59)
- Principles of Forensic Engineering Applied to Industrial AccidentsNo EverandPrinciples of Forensic Engineering Applied to Industrial AccidentsAinda não há avaliações
- The Things We Make: The Unknown History of Invention from Cathedrals to Soda CansNo EverandThe Things We Make: The Unknown History of Invention from Cathedrals to Soda CansNota: 4.5 de 5 estrelas4.5/5 (21)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureNo EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureNota: 4.5 de 5 estrelas4.5/5 (474)
- Shallow Foundations: Discussions and Problem SolvingNo EverandShallow Foundations: Discussions and Problem SolvingNota: 5 de 5 estrelas5/5 (1)
- Introducing Structures: A Textbook for Students of Civil and Structural Engineering, Building and ArchitectureNo EverandIntroducing Structures: A Textbook for Students of Civil and Structural Engineering, Building and ArchitectureNota: 4.5 de 5 estrelas4.5/5 (11)
- Climate Adaptation Engineering: Risks and Economics for Infrastructure Decision-MakingNo EverandClimate Adaptation Engineering: Risks and Economics for Infrastructure Decision-MakingAinda não há avaliações
- Field Book for Quality Control in Earthwork Operations: Project Construction Management BookNo EverandField Book for Quality Control in Earthwork Operations: Project Construction Management BookAinda não há avaliações
- Professional Surveyors and Real Property Descriptions: Composition, Construction, and ComprehensionNo EverandProfessional Surveyors and Real Property Descriptions: Composition, Construction, and ComprehensionAinda não há avaliações