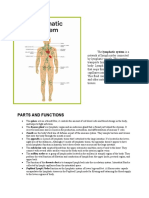
Escolar Documentos
Profissional Documentos
Cultura Documentos
A Computer Model of The Lymphatic System PDF
Enviado por
nnimrodo0 notas0% acharam este documento útil (0 voto)
123 visualizações17 páginasA mathematical model of the whole body lymphatic network is developed using the fundamental conservation laws and current notions of lymphology. The set of mathematical equations are then translated into a series of FORTRAN statements for the purpose of digital computer simulation. The model analysis revealed interesting characteristics of lymphatic contractility at various points along the network.
Descrição original:
Título original
A computer model of the lymphatic system.pdf
Direitos autorais
© © All Rights Reserved
Formatos disponíveis
PDF, TXT ou leia online no Scribd
Compartilhar este documento
Compartilhar ou incorporar documento
Você considera este documento útil?
Este conteúdo é inapropriado?
Denunciar este documentoA mathematical model of the whole body lymphatic network is developed using the fundamental conservation laws and current notions of lymphology. The set of mathematical equations are then translated into a series of FORTRAN statements for the purpose of digital computer simulation. The model analysis revealed interesting characteristics of lymphatic contractility at various points along the network.
Direitos autorais:
© All Rights Reserved
Formatos disponíveis
Baixe no formato PDF, TXT ou leia online no Scribd
0 notas0% acharam este documento útil (0 voto)
123 visualizações17 páginasA Computer Model of The Lymphatic System PDF
Enviado por
nnimrodoA mathematical model of the whole body lymphatic network is developed using the fundamental conservation laws and current notions of lymphology. The set of mathematical equations are then translated into a series of FORTRAN statements for the purpose of digital computer simulation. The model analysis revealed interesting characteristics of lymphatic contractility at various points along the network.
Direitos autorais:
© All Rights Reserved
Formatos disponíveis
Baixe no formato PDF, TXT ou leia online no Scribd
Você está na página 1de 17
(ompsr Bid Med. Pergamon Press 1977 Vol. 7. pp. 1X1-197. Prmted m Great Britain.
A COMPUTER MODEL OF THE LYMPHATIC SYSTEM
NARENDER P. REDDY*, THOMAS A. KROUSKOP and PAUL H. NEWELL, JR.
Rehabilitation Engineering Center, Texas Institute for Rehabilitation and Research. P.O. Box 20095.
Houston, TX 17025. USA
(Received 11 August 1915; in revised form 30 August 1976)
Abstract-A mathematical model of the whole body lymphatic network, which simulates the
lymph propulsion along the network from the periphery through the thoracic duct into the
venous system, is developed using the fundamental conservation laws and current notions of
lymphology. Only the major lymphatic vessels are considered. The set of mathematical equations
are then translated into a series of FORTRAN statements for the purpose of digital computer
simulation of the pressure and flow patterns along the network. The model analysis revealed
interesting characteristics of lymphatic contractility at various points along the network.
Lymph flow and pressure Lymphatic active contractility Lymphangion pump Smooth
muscle Network model Computer simulation
GENERAL NOMENCLATURE
radius of a lymphangion (cm)
capillary filtration coefficients (cm5/dyn)
filtration coefficients for the terminal lymphatics (cm/dyn)
protein concentration (g/ml)
modulus of elasticity in the transeverse direction (dyn/cm)
acceleration due to gravity (cm/se&
thickness of the lymphangion wall (cm)
length of a lymphangion (cm)
pressure (dyn/cm)
external pressure on the lymphangion (dyn/cm*)
flow rate (cm/sec)
rate of flow into the terminal lymphatics (cmj/sec)
valve resistance (dyn/cm)
resting radius of a lymphangion (cm)
radi;ll co-ordinate (cm)
strain
threshold of strain required to initiate an active contraction
tissue pressure (dyn/cm2)
time coordinate (set)
duration of contraction (set)
refractory period (set)
interstitial fluid pressure
pressure head due to gravity (cm)
SplllOlS
I
density gjcm3
p
viscosity [g/(cm-set)]
4
coefficient of active contractility (dyn/cm)
4,,1
stress developed due to an active contraction (dyn/cm)
D huor hoop stress (dyn/cm)
n osmotic pressure (dyn/cxr?) = E,
Subscripts
A arterial end of the capillary
V venous end of the capillary.
INTRODUCTION
The development of transplantation procedures and increased clinical problems involv-
ing edema and cancer have created a growing need for detailed studies of the lymphatic
system due to its role as a component in the circulatory system and as a component
* Present address: Postgraduate Research Physiologist, University of California, Cardiovascular Research
Institute. San Francisco. CA 94143. U.S.A.
182
NARENDER P. REDDY, THOMAS A. KROUSKOP and PAUL H. NEWELL, JR.
in the immunological system Cl]. It is now generally agreed that the lymphocytes which
become sensitized at the site of transplantation travel through the afferent vessels to
the regional lymph node where they initiate an immunological response. Thus resto-
ration of lymph flow from transplanted tissue is important for the survival of a graft;
also restoration of lymph flow between the graft and the host is important in understand-
ing the homograft mechanisms [27. Moreover, the lymphatic system is known to play
a decisive role in the dissemination of cancer. Malignant cells escape the tissue of origin
and enter the blood vessels through the lymphatic system [3).
The lymphatic systems role in the circulation of protein molecules and lymphocytes
throughout the extracellular space also makes it important in several common maladies.
Filariasis, involving lymphatic obstruction which leads to lymphedema in the associated
region, is one of the most common diseases found in tropical countries. The impairment
of lymphatic valve function may also lead to lymph stasis and subsequently to edema.
With the accumulation of edema fluid and protein molecules, the region involved
becomes highly susceptible to infection [4]. Another important pathological condition
which centers on the lymphatic system is the thoracic duct fistula which leads to loss
of protein molecules and fluid [3].
The composition of lymph fluid reflects the composition of interstitial fluid from
which it is derived. There is growing evidence that most of the bodys enzymes are
transported from the tissue of origin into the circulatory system via the lymphatics.
In addition, most of the metabolic waste products are transported through the lym-
phatics. Moreover, as pointed out by Newell et al. [IS] the lymphatics play an important
role in the tissue ulceration and necrosis. Occlusion of the lymphatics leads to the
accumulation of the enzymes and other metabolic waste products in the interstitial
spaces, This accumulation then leads to tissue necrosis and ulceration. Thus, in order
to study the pressure effects on soft tissue, it is imperative to understand the mechanism
of lymph propulsion.
In recent years, one of the most important trends of research in the sphere of bioen-
gineering has been the modeling of physiological systems. Models are conceptual con-
structions which allow formulation of hypotheses and in this way stimulate meaningful
research. A mathematical model is a conceptual representation of a real physical system.
Mathematical models are widely used in todays scientific world due to the ease with
which they can be used to analyze real systems. The most prominent value of a model
is its ability to predict as yet unknown properties of the system.
A model can also be used as a powerful education tool since it permits the idealization
of processes. It also allows the study of sub-systems in isolation from the parent system.
Model studies are often inexpensive and less time consuming than the corresponding
experimental study. Models of a physiological system often aid in the specification of
design criteria for the design of procedures aimed at alleviating pathological conditions.
In a recent investigation [6] we have developed a mathematical model of the lym-
phatic vessel using the tools of continuum mechanics together with the currently
accepted notion of lymphology, and have identified the equations governing the lymph
flow in a lymphatic vessel. The lymphatic vessel model is used in the present investiga-
tion to develop a network model of the whole body lymphatic system, considering
the regional lymphatics. The model is then coupled to a previously developed model [7]
used to describe the interstitial fluid dynamics and the resulting composite model is
simulated on a digital computer to yield pressure and flow patterns along the lymphatic
network.
SYNTHESIS OF THE MODEL
The lymphatic system is a complex network of vessels. A lymph vessel consists of
a number of compartments, called lymphangions, which are separated by unidirec-
tional valves (Fig. 2). A growing body of evidence now supports the concept that lymph
propulsion in the lymphatic system is achieved by active and passive contractilities
A computer model of the lymphatic system
Right heart Left hear t
I t
Vena cava Aorta
I I
Thoraclc
duct
I
Lymphatic
vessels
I
Collecting
lymphattcs
I
Lymph
caplllarles
I I
Venous
Arteries
system
I I
Venules Arterioles
I I
Capillaries
1
I I
Interstltlal f lulds
1
Fig. 1. Diagrammatic representation of circulatory and lymphatic systems. The lymph capillaries
and other vessels which absorb lymph from the interstitial spaces are collectively referred to
as the terminal lymphatics. Not shown in the diagram are the lymph nodes which he along
the lymphatics are the centers of immunological response.
of th.e lymphatic walls and lymph nodes. Passive contractility is due to respiratory
movements, rhythmic changes in the volumes of the intestines, spleen and other organs
and also due to movement of the limbs and skeletal muscles. Active contractility is
due .to intrinsic contractions of the smooth muscle in the walls of the lymphatics and
lymph nodes. A number of investigators [8-l 31 have demonstrated active contractility
of the lymph vessels in uiuo and in vitro. The frequency of contractions were found
to be independent of the respiratory, intestinal and cardiac rhythms [8]. Recent findings
suggest that a lymphangion contracts independently and therefore, constitutes an
autonomous functional element. Active contractions in the walls of a lymphangion have
been shown to occur if the diameter of the Iymphangion exceeds certain threshold
values [9]. The terminal iymphatics are free of smooth muscle and therefore they do
not exhibit active contractility [lo].
In a recent investigation [6] it has been shown that a lymphatic vessel can be charac-
terized as a chain of lymphagions and that the adjacent lymphagions can be conceptually
coupled through the continuity and the momentum equations. This analysis can be
extertded to the entire lymphatic system by conceptually coupling the lymphangions
at each branching point to form a network model of the entire lymph system.
Yoffey and Courtice [3] extensively reviewed the literature on regional lymph flows
and noted that under normal conditions, the hepatic and intestinal lymph ducts contrib-
ute ;I. major portion of the lymph found in the thoracic duct. However, during conditions
1,
I
I
I
Fig. 2. A lymph vessel.
84 NARENDER P. REDDY, THOMAS A. KROUSKOP and PAUL H. NEWELL, JR.
Fig. 3. The lymphatic system. [ indicates boundary. The pressure at the arterial and venous
ends of the capillary (P, = 35 mm Hg and PV = I5 mm Hg in the present case) are the boundary
[ conditions. JV Jugular Venous pressure (6 mm Hg) is the proximal boundary condition.
Organs
E
:
e
f
i?
i
:
I
m
n
0
Vessel No
1
2
3
4
5
6
1
8
9
10
11
12
13
14
15
16
17
18
19
20
21
22
23
24
25
26
2-I
28
29
liver
stomach and other portions drained by hepatic duct
small intestine
large intestine
right leg
right part of the trunk
right kidney
left leg
left part of the trunk
left kidney
thoracic wall
heart
lungs
head and neck
left hand
Name
hepatic duct
vessels from the stomach
hepatic duct
intestinal duct
intestinal duct
intestinal duct
intestinal duct
left leg lymphatic
right part of the trunk
right lumbar duct
right kidney lymphatic
right lumbar duct
left leg lymphatic
left part of the kidney
left lumbar duct
left kidney lymphatic
left lumbar duct
cistemal chyli
thoracic duct
intercoastal lymphatics
thoracic duct
heart lymphatic
lung lymphatic
branchio-mediastinal lymphatic
thoracic duct
cerircal duct
hand lymphatics
jugular lymphatic
thoracic duct
jugular vein
Compartments
l-8
9-16
17-26
21-36
37-5 I
52-61
62-66
67-106
107-I 16
117-121
122-131
132-141
142-181
182-191
192-196
197-206
207-2 16
217
217-224
225-232
233-252
253-258
259-266
267-270
271-274
215-279
280-257
288-293
294296
297
A computer model of the lymphatic system 185
such as exercise, the contribution from the other organs increased substantially. In the
present analysis, lymph flows from the limbs, the trunk, the kidneys, the heart, the
lungs, the liver, small and large intestines, the thoracic wall, the cervical vessels and
the thoracic duct are considered. Due to the lack of sufficient quantitative anatomical
data concerning the lymph capillary network, the present investigation considers only
the primary lymphatic vessel from each organ. The second and higher generation lymph
vessels are assumed to be lumped such that they constitute a series of compartments
in the primary vessel. Furthermore, it is assumed that all the terminal lymphatics of
each organ can be lumped into a single compartment of the primary vessel draining
the organ. Unfortunately, there is no information present in the existing literature regard-
ing the microcirculation within a lymph node. This investigation assumes that the flow-
characteristics of a lymph node can be treated as a lymphangion within the primary
vessel. Moreover, the ratio of the number of lymph nodes to the number of lymphan-
gions is very small and the lymph nodes are localized structures.
The lymph vessels considered in this study are shown in Fig. 3. The present model
does not consider the right side of the head, neck, thorax and upper right extremity.
These tissues are drained by the right lymph duct which directly empties into the venous
system. It should be noted that organs, such as the limbs, have superficial and deep
lymphatics; however, they are lumped into a single vessel.
In order to facilitate the conceptual handling of the system of vessels and the lymphan-
gion:s, each vessel considered in this investigation, and each lymphangion are assigned
specific numbers. The numbers assigned to vessels are shown in Fig. 3. Columns 3
and 4 of Table 1 indicate the numbers assigned to the lymphangions which comprise
each lymphatic vessel. The lymphangions listed in column 4 empty into the respective
lymphangions listed in column 6. The last compartment of the thoracic duct is coupled
to the venous system. To further facilitate the mathematical handling, each of the organs
is identified with a serial number. Table 2 shows the number of the compartment drain-
ing #::ach organ. The compartments representing the terminal lymphatics are coupled
to the respective tissue spaces through the equations expressing the flow of fluid into
Table 1
j N, B(j-l)+ 1
B(j) mj
B(m,-l)+l mj
B(mj)
1 8
2 8
3 IO
4 10
5 15
6 10
7 5
8 40
9 IO
10 5
II IO
12 10
13 40
14 IO
I5 5
16 10
17 10
18 8
19 8
20 20
21 6
22 8
23 4
24 4
25 5
26 8
27 6
28 3
9
17
27
37
52
62
67
107
117
122
132
142
182
192
197
207
217
225
233
253
259
267
271
275
280
288
294
8 3
16 3
26 7
36 6
51 6
61 7
66 18
106 10
116 10
121 12
131 12
141 18
181 15
191 I5
196 17
206 17
216 18
224 20
232 20
252 24
258 23
266 23
270 24
274 28
279 27
287 27
293 28
296 29
17
17
62
52
52
62
217
117
117
132
132
217
192
192
207
207
217
233
233
271
267
267
271
294
288
288
294
297
4
8 106
10 121
I3
15
12
18
21 258
20 252
25 219
24 274
8
36
26
181
171
141
224
186 NARENDER P. REDDY, THOMAS A. KROUSKOP and PAUL H. NEWELL, JR.
Table 2
Compt. draining Vessel draining
Organ no. the organ organ
k
D(k)
1 1
2
3
4
5
6
7
8
9
10
11
12
13
14
15
9
21
31
67
107
122
142
182
197
225
253
259
275
280
1
2
4
5
8
9
11
13
14
16
19
21
22
25
26
the terminal lymphatics. Finally, the interstitial spaces are coupled to the blood circula-
tory system through the equations describing the capillary exchange and the interstitial
fluid dynamics. The complete set of equations are given below.
EQUATIONS OF THE NETWORK MODEL
In the development that follows, the following notations apply:
1. Each lymphangion in the network and each vessel are identified with unique numbers.
The words compartment and lymphangion are used interchangeably. All of the com-
partments in a vessel are numbered, consecutively, starting from receiving end to
the emptying end of the vessel.
2. Nj represents the number of compartments in the jth vessel.
n=j
3. B(j) = 1 Nn.
n=l
B(j) represents the compartment located at the emptying end of the J vessel.
B(j - 1) + 1 represents the compartment at the receiving end of vessel j. Compartments
ofjlh vessel are represented by B(j - 1) f 1, B(j - I) + 2 - - - - B(j) - 1, and B(j)
4. jth vessel empties into vessel mj such that compartment B(j) empties into compartments
B(mj - 1) + 1 (Fig. 4).
5. At a converging branch, vessel j is fed by vessels j - 1 and Mj such that compartment
B(j - 1) + 1 receives fluid from B( j - 1) and B(Mj).
6. The tissue spaces of kth organ are drained by the terminal lymphatics represented
by compartment D(k).
The assumptions in derivation and the limitation on the usage of the set of equations
(l-3) (6) and (7) are discussed in detail in Ref. 6.
The rate of change of radius of a lymphangion can be obtained using the law of
mass action.
Rate of change of lymphangion radius =
flowin-flowout
surface area
If lymphangions i - 1 and i are located in the same vessel, i.e. lymphangion i is
not at the receiving end of a vessel, then flow out of lymphangion i - 1 is the same
as flow into lymphangion i. Therefore, for i = B(j - 1) + 2, B( j - 1) + 3, B(j) - 1 and
B(j), and j = 1, 2, 3, . ., 28
c&i_
- 25 CQi- 1 - Qil3
dt I,
where Qi is the flowout of ith compartment.
A computer model of the lymphatic system 187
Fig. 4. Notation at branching points.
AI: a converging branch, two or more vessels feed into a single compartment. In
the present model (Fig. 3), vessels 3, 6, 7, 10, 12, 15, 17, 20, 23, 24, 27 and 28 receive
fluid from two feeding vessels;
For i = B(j - 1) + 1, b = B(Mj) and
j = 3, 6, 7, 10, 12, 15, 17, 20, 23, 24, 27 and 28
3_
- .jj CQi- I + Qb - Qil~
df 1,
(lb)
However, vessel 18 has three feeders;
fori=B(j- l)+ l,b=B(Mj) and j= 18
&i_ 1
dt 1,
- 2~ {Qi-1 + Qb + QB[TI - Qi). (lc)
The above equations describe the rates of change of all the lymphangions in the
network except those which represent the terminal lymphatics.
In the case of the lymphangions representing the terminal lymphatics, for i = D(k)
and k = 1, 2, 3,. . . , 15
gi_
- 2& {Qtl, - Qi 1,
dt I,
(14
where Qtlr is the flow into terminal lymphatics from the kth organ.
The rates of change in flow rates can be-determined using Newtons laws of motion
and the constitutive relation for the fluid [6].
Density x Rate of change of flowrate = hydrodynamic force gradient
+ gradient in gravitation forces
-
viscous resistance
-
valve resistance;
for
i = B(j - 1) + l,B(j - 1) + 2...Bcj) -2,&j) - 1, and
j= 1,2,...28
dQi
- = ;-&+pi-pi+l +(q-~~+~)}
dt , if1
(2a)
,111 the case of a lymphangion (i) located at the emptying end of a vessel (j) which
empties into lymphangion B(mJ, the pressure difference between lymphangion i and
lymphangion B(mj) determines the hydrodynamic forces which drive the fluid out of
188 NARENDER P. REDDY, THOMAS A. KROUSKOP and PAUL H. NEWELL, JR.
lymphangion i; therefore,
for
i = B(j), b = B(mj) and j = 1,2,3,. . .28
_ di.
(2b)
The intraluminal pressure of the lymphangions can be determined by using the
momentum balance for the lymphangion wall [14].
Intraluminal pressure = extraluminal pressure + (ratio of wall thickness to
radius) x (hoop stress + stress developed due to active contractility).
For i = B(j - 1) + 2, B(j - 1) + 2, B(j - 1) + 3,. . . , B(j), j = 1, 2,. . . , 28 and for
i = B(j - 1) + 1, j = 3, 6, 7, 10, 12, 15, 17, 18, 20, 23, 24, 27 and 28
pi = Pext,i + 1 {~hoopi
+ ~.act,l. (34
t
Terminal lymphatics do not have smooth muscle on their walls and therefore do
not exhibit active contractility [15].
Flow into terminal lymphatics is due to the instantaneous pressure difference between
the tissue pressure and i&alumina1 pressure of the terminal lymphatics [15].
for i = D(k) and k = 1, 2, 3,. . . , 15
Qt~k = Cl yrnphk {Tk - Pi ) >
(4)
where QIlr is the flow into lymphangion i which represents the terminal lymphatics
of organ k; Tk is the tissue pressure of organ k; Clymphk is the filtration coefficient
of two terminal lymphatics of kth organ.
The tissue pressure is dynamic and is a function of the interstitial fluid volume. The
rate of change of interstitial fluid volume may be expressed as:
Rate of change of interstitial fluid volume = Net rate of filtration into the tissue
across the blood capillary-rate of flow into the terminal lymphatics
for k = 1, 2, 3, .,., 15
d&, _
- - Cfap*PAl, + pvr
dt
- Tk - n,, + fl,,> - Qt~p ( 54
where Ccapk is the capillary filtration coefficient of kth organ; PA* is the pressure at
arterial end of kch organ; Pv, is the pressure at venous end of kfh organ; II,, is the
osmotic pressure in the capillary of kth organ; BT, is the tissue osmotic pressure in kth
organ.
Osmotic pressure is a function of the protein concentration [16].
n = 133.24 210 C,, + 1600 C& + 9000 Cz, dyn/cm, (5b)
where C,, is the protein concentration in g/ml.
The dynamic changes in the tissue protein concentration may be represented by
Rate of change of protein = net rate of leakage into the tissue across the blood
capillary wall - the rate of removal via the lymphatics
d&l, 1
~ =
- WM&~, - C,,,) - Qt~, CprtJ
dt VW,
(5c)
The stress developed in the walls of a vessel due to active contractility is a function
of the strain history. The mathematical representation of the stress due active contracti-
lity, presented in [6], is given below.
A computer model of the lymphatic system
I h9
If,
then
si 2 Sthr,i
and t > (7i + t,)
Ti = t + t,
$i = 4i(l + (Si - Sthr,i)Ka.
Here Ka is a constant.
If t -:s TV, then
(r
= yi
Sitl(Ti - t)
act,,
tP
where
tp = ;.
If
or il:
Si - S,hr,i and (Ti + tp) > t > Ti.
Si < Sthr,i and t > (Ti + t,).
(64
(6b)
(64
the],.
0.& = 0.
(6dl
Where: Si be the engineering strain in the wall of the iIh lymphangion ; Sthr, i be
the threshold of strain required to initiate an active contraction in the lth lymphangion;
I$+ be the amplitude of the stress developed due to an active contraction when initial
filling is such that Si = Sthr,i; pi be a parameter which denotes the amplitude of stress
developed due to an active contraction and is dependent on the initial filing; 7; be
a parameter which denotes the time at which the contraction ceases, t, be the duration
of contraction; and t, be the refractory period. The parameters cbi and Sthr,i depend
on the amount of smooth muscle present in the wall of the ith lymphangion.
In addition, the presence of valves along the lymphatics imposes the constraint that
Qi 2 0 for all i
(74
and
Qtlt 2 0 for all k.
(7b)
In all, there are 296 lymphangions and hence 296 equations each of type 1, 2, 3,
6, 2nd 7. There are 15 organs and 15 equations each of type 4 and 5.
THE BOUNDARY CONDITIONS
The pressure in the jugular vein forms one of the boundary conditions of the present
model. The pressures at the arterial and venous ends of the capillaries of each organ
and the capillary protein concentrations form the second set of boundary conditions.
The third set of boundary conditions include the external pressures on the individual
lymphangions. These boundary conditions are the input parameters to the present
model.
RESULTS
The differential system described above is translated into a FORTRAN program for
the purpose of digital computer simulation. In developing the program reported here,
an effort was made to make the program sufficiently general so that it can be easily
modified when further quantitative anatomical data are available, especially with regard
NARENDER P. REDDY. THOMAS A. KROUSKOP and PAUL H. NEWELL, JR.
Fig. 5. Pressure patterns in the thoracic duct lymphangion 250. Active contractions are super-
posed over the low frequency respiratory rhythm.
to the number of compartments and their arrangement. The model has been simulated.
The parameters, and boundary conditions used in the model together with the listing
of the computer program are documented in [16]. Figures 5-14 depict pressure pat-
terns and flow patterns in intestinal, hepatic, and leg lymphatics, thoracic duct. and
cistera chyli.
Fig. 6. Pattern of flow-out of thoracic duct lymphangion 250.
A computer model of the lymphatic system 191
~~+--_ .
klo 1.m 2. 00 5. w I . 00 5. 00 6. 00
I
7. 00
TI HE IN SECUNDS
D. 00 n.00 10. 03
Fig. 7. Pressure pattern in cisterna Chyli.
DISCUSSION
Il. is extremely difficult to measure pressures and low rates of flow in small collapsible
tubes such as the lymphatics. Consequently, most measurements of flow have been
made with cannulated lymphatics. The cannulation procedure distorts the normal mic-
roanantomy and pressure flow relationships that exist in the intact lymphatics. Hall
et al. [S] recorded pulsatile pressures in the intestinal, hepatic and lumbar lymphatic
ducts and the efferenct lymphatic duct of popliteal lymph nodes of sheep. It should
be noted that the pressure pattern differs from one lymphangion to another in the
Fig. 8. Pattern of flow-out of Cisterna Chyli.
NARENDER P. REDDY, THOMAS A. KROUSKOP and PAUL H. NEWELL, JR.
-_-._--t__-_-t--_-+-__-+
I
a 1.00 2.00 3.uo LOO 5.00 6.00 7.00 e.00 o.orl 111.00
TIWE IN SECBNDS
Fig. 9. Pressure pattern in intestinal duct lymphangion 66.
same lymphatic vessel. Hall and his associates recorded the pressure pattern by cannulat-
ing the lymphatic against the direction of flow. In their experiments they used cannulas
with i.d. ranging from 0.8 to 1.0 mm and outer diameter ranging from 1.20 to 2.00 mm.
The cannulas were tied to the lymphatics. These procedures cause trauma to the vessels.
Furthermore, it should be pointed out, from the experiments of Smith [12] and Mis-
lin [9] that when a lymphangion is sufficiently dilated there is an increase in the pressure
due to increased intrinsic contractility. Therefore, the pressure recorded by them may
not be assumed as absolute. Instead, the concepts derived from their recordings and
the pressure patterns are important. Considering the various factors discussed above,
Fig. 10. Pattern of flow-out of intestional duct lymphangion 66.
A computer model of the lymphatic system
Fig. 11. Pressure pattern in leg lymphatic (lymphangion 106).
the pressure patterns in various lymphatic simulated in present investigation are in
accord with the experimental observations by Hall et al. The frequencies observed in
the present investigation are in the neighborhood of those reported. The frequency
of contraction depends on the amount of filling and also on the rate of fluid flow
out of the lymphangion; the insertion of a cannula of the size which is comparable
to the size of the vessel may alter the frequency of the intrinsic contraction.
The flow rates from the intestinal duct are shown in Fig. 9. The average lymph
flops from the vessel (1.48 ml/min), computed in the present analysis, are consistent
with the average flow rates for sheep reported by Hall et al., when their results are
Fig. 12. Flow pattern in leg lymphatic (lymphangion 106).
NARENDER P. REDDY, THOMAS A. KROUSKOP and PAUL H. NEWELL, JR
0 1.00 2.00
4
s.00
TI%?IN !&J&S
6.00 7.00 a.w WJO 1o.m
Fig. 13. Pressure pattern in hepatic duct lymphangion 26.
extrapolated to the human. It should be pointed out that Hall and his associates have
reported the how rates after averaging over a period of hours. In their experiments
the lymph was collected in graduated clyinders. The flow rates recorded by Hall et
al. should by no means be assumed to be the normal physiological flows with the
vessel intact. On the other hand, in the absence of better instrumentation techniques,
their observations should be commended. The average flow rate from the intestinal
duct decreased by 50% when the intestinal motility is removed. This data is in agreement
with the observations of Lee l-171 that intestinal lymph flow increases when the intestinal
motility is established.
Fig. 14. Flow pattern in hepatic duct lymphangion 66
A computer model of the lymphatic system 195
Quantitative anatomical data of the lymphatic system are scarce. In particular, there
is very little information in the present literature regarding the dimensions of various
lymphangions. Moreover, the diameter of a lymphangion varies with intraluminal pres-
sure, and it is difficult to obtain the exact unstressed or the resting diameter of a
vessel. Although, the lymphangion at the proximal end of a vessel may be smaller
in diameter than the lymphangion at the distal end of the vessel, a uniform unstressed
diameter and a uniform length are assumed over the entire length of the vessel in
the present analysis.
The stress developed due to an active muscular contraction is dependent on the
amount of smooth muscle present in the wall of a lymphangion. Nisimaru [13] studied
the relative amounts of smooth muscle, and leg lymphatics have higher muscle quantity.
However, the absolute muscle mass per unit of lumen diameter decreases with the size
of the vessel. High muscle quantity has been reported by Mislin for the intestinal lym-
phatics. Nisimaru further observed that the thoracic duct has higher muscle quantity
in the upper part than in the lower part. These findings suggest that a lymphangion
has lower amount of smooth muscle than the lymphangion into which it empties. Simi-
larly, a lymphangion develops lower stress during active contractility than the lymphan-
gion into which it empties. Mislins experiments reveal that a pressure of 2 mmHg
is necessary in the mesenteric lymphatics to initiate an active contraction. His findings
also suggest that the threshold varies with the vessel. The distribution of smooth muscle
observed [13] suggests that a lymphangion has a lower threshold than the lymphangion
into which it empties. This increase in the threshold from the upstream end to the
down stream end of a vessel further facilitates the contraction co-ordination between
the iymphangions. A parametric study of the present model revealed that the gradients
in thresholds are important for the efficient propulsion of the lymph along the lym-
phat its.
This analysis assumes that the duration of a single contraction and the duration
of the refractory period are the same for all the lymphangions regardless of their location
within the body. In actual case this may not be true for all the lymphangions. Moreover,
thesl.: durations may be significantly altered by several pharmacological agents [ 1 S].
Experiments are in progress in several laboratories which are aimed at studying the
effects of various neurotransmitters. It is further assumed that all the lymphangions
have: the same elastic modulus in the transverse direction. The relative amount of elastic
tissue present in the lymphangion may vary from one lymphangion to another.
Furthermore, a uniform intervalvular distance is assumed for all the lymphangions
in a vessel. We hope that the present analysis would stimulate lymphologists to conduct
experiments aimed at obtaining quantitative anatomical data which would make it poss-
ible for better estimation of the parameters involved in lymph propulsion.
SUMMARY
A computer model of the whole body lymphatic system is developed considering
onl!, the major lymph vessels and using a previously developed model of a lymphatic
vess,el. The terminal lymphatics of each organ are lumped into a single compartment
of the primary vessel draining the organ. In order to facilitate conceptual handling
of the system of lymph vessels, each lymph vessel and each lymphangion (compartment
within the vessel) are identified with specific numbers. A set of differential equations
are presented which describe the flow and pressure patterns along the lymphatic
network. The jugular venous pressure, the pressures at the arterial and venous ends
of the capillaries of each organ and the external pressures on the individual lymphan-
gions form the set of boundary conditions of the present. model. The mathematical
model is then translated into a series of Fortran Statements for the purpose of digital
computer simulation. Simulation results are consistent with the available experimental
data. A parametric study of the model revealed that gradients in thresholds of distention,
along the vessel, are important for efficient lymph propulsion along the network.
I i, NARENDER P. REDDY, THOMAS A. KROUSKOP and PAUL H. NEWELL, JR
Acknowlrdgemenrs-This investigation was partially supported by the Social and Rehabilitation Service
through a Grant (SRS-23-P-55-823-6). This work is a part of a Ph.D. dissertation submitted by the senior
author to Texas A & M University.
REFERENCES
1. P. Malek and J. Vrubel. Lymphatic system and organtransplantation, Lymphology 1. l-22 (1968).
2. P. R. Koehler. Injuries and complications of the lymphatic system following renal transplantation, Lympho-
lo</!. 5. 6 167 f 1972).
3. J. M. Yoffey and F. C. Courtice, Lympharics. Lymph, and Lymphomyebid Complex, Academic Press, New
York (1970).
4. E. Tosatti, The unsolved problem of peripheral lymphedema, Lymphology 6. 167-168 (1973).
5. P. H. Newell, J. D. Thrumunberg and W. C. Flemming. The management of pressures and other external
factors in the prevention of ischemic ulcers, ASME Truns. J. Basic Engng 92, Series D, 3, 59&596 (1970).
6. N. P. Reddy, T. A. Krouskop and P. H. Newell, Jr., Biomechanics of a lymphatic vessel, Blood Vessels
12. 261-278 (1975).
7. J. I. Leonard and P. H. Abbrecht, Dynamics of plasma-interstitial fluid distribution following intravenous
infusions in dogs--an experimental and computer simulation study, Circulation Res. pp. 734-747 (1973).
8. J. G. Hall, B. Morris and G. Wolley, Intrinsic rhythmic propulsion of lymph in the unanaesthetized
sheep, J. Physiol. Lond. 180, 336349 (1965).
9. H. Mislin. Structural and functional relations of the mesenteric lymph vessels, In Progress in Lymphlogy,
Hafner NY (1967).
10. B. W. Zweifach. Micromanipulation of pressure in terminal lymphatics in the mesentery. Am. J. Physiol.
228, 1326-1335 (1975).
11. T. Campbell and T. Heath, Intrinsic contractility of lymphatics in sheep and in dogs, J. Ewp. Pkysio/.
207-217 (1973).
12. R. 0. Smith, Lymphatic contractility, a possible intrinsic mechanism of lymphatic vessels for the transport
of lymph, J. Eqi. Med. 90. 497-509 (1949).
13. Y. Nisimaru, Lymphatics and lymph flow, Hiroshima J. Med. Sci. 17. 53-76 (1968).
14. N. P. Reddy. T. A. Krouskop and P. H. Newell, Jr.. Developments of lymph hypertension in lymphatic
occlusion, Lymphology 8. 105- 109 (1975).
15. N. P. Reddy. T. A. Krouskop and P. H. Newell, Jr., A note on the mechanisms of lymph flow through
the terminal lymphatics, Microuasc. Res. 10. 214-216 (1975).
16. N. P. Reddy. A discrete model of the lymphatic system. Ph.D. dissertation, Texas A & M University
(1974).
17. J. S. Lee. Motility, lymphatic contractility and distention pressure in intestinal absorption, Am. J. Physiok
208. 621627 (1965).
18. P. Tinone. P. Schianterelli and G. Rosati. Pharmacological activity of some neurotransmitters in the
isolated thoracic duct of dogs. Qrnphology 6. 65-68 (1973).
About the Author-NAaENDER PABBATHI REDDY. after receiving the B.E. degree in M.E. from
Osmania University in 1969, and M.S. degree from University of Mississippi in 1971, joined
the bioengineering program at Texas A & M University, where he developed a strong interest
in the physiological sciences, and received the Ph.D. in 1974. In addition, he took a special
summer course in Classical Physiology with Modern Instrumentation at Baylor College of
Medicine in 1972. He was a research assistant throughout the period of his graduate education.
Dr. Reddy served Texas A & M University as a research associate in the bioengineering
program, during 7v75, before joining Baylor College of Medicine where he is presently
employed as a research associate in the department of Rehabilitation. During the 1976 summer,
Dr. Reddy visited the laboratory of Autonomic Pharmacology at the University of Ottawa.
Dr. Reddys research interests fill the entire domain of physiological engineering. Dr. Reddy
is member of the International Society of Lymphology, Biomedical Engineering Society, ASME,
Society of Engineering Science, Association of Professional Engineers of Ontario and Sigma
Xi. Dr. Reddy has been credited with several publications.
About the Author--THOMAS A. KROUSKOP. Associate Professor in industrial engineering (bioen-
gineering). came to Texas A & M University in 1971 as an assistant professor from the Carnegie-
Mellon University where he earned his B.S., MS. and Ph.D. degrees. He is also an adjunct
assistant professor of bioengineering in the departments of physical medicine and rehabilitation
and the associate director of Rehabilitation Engineering Center at Baylor College of Medicine.
He has been a consultant to the Texas Heart Association, the Samson Corp. of Pittsburgh
(PA) and worked for the DAppolonia consulting engineers, also of Pittsburgh. In 1975 he
was named young engineer of the year by the Sam Houston chapter, Texas Society of Profes-
sional Engineers. He is listed in American Men & Women of Science (1975) is a Registered
Professional Engineer (Texas) and is a member of the American Association for the Advancement
of Science, American Society of Civil Engineers, Texas Society of Professional Engineers and
the American Society for Engineering Education. Dr. Krouskop has been credited with more
than 30 publications and significant reports.
About the Author-PAuL H. NEWELL, JR., after receiving the Ph.D. in mechanical engineering
from MIT in 1966, started bioengineering programs at the university of Alabama and Texas
A computer model of the lymphatic system
A & M University. Dr. Newell has served Texas A & M University as associate dean of engineer-
ing and as head of Biological and Industrial engineering. was also a professor of bioengineering
in the departments of Physiology, Physical Medicine and Rehabilitation at Baylor College of
Medicine. He is currently the president of New Jersey Institute of Technology.
Dr. Newell is a member of many professional organizations and heads a number of technical
committees. He has received a number of awards for excellence in engineering education and
has been credited with numerous publications.
Você também pode gostar
- Breslin 2018Documento93 páginasBreslin 2018Rizky RayyanAinda não há avaliações
- MR Lymphangiography Reveals Central Lymphatic PathwaysDocumento14 páginasMR Lymphangiography Reveals Central Lymphatic PathwaysHector Hernandez-SoriaAinda não há avaliações
- Kejang NeonatusDocumento12 páginasKejang NeonatustriAinda não há avaliações
- Lymphotropic Therapy For Diseases of The Maxillofacial Region Review of The LiteratureDocumento6 páginasLymphotropic Therapy For Diseases of The Maxillofacial Region Review of The LiteratureEditor IJTSRDAinda não há avaliações
- The lymphatic system's role in collecting and transporting tissue fluidsDocumento3 páginasThe lymphatic system's role in collecting and transporting tissue fluidsTania Louise Pioquinto AbuanAinda não há avaliações
- Fisiologia LinfedemaDocumento8 páginasFisiologia LinfedemaSAKAI69Ainda não há avaliações
- 15 Lymphatic SystemDocumento4 páginas15 Lymphatic SystemOribello, Athenna Jae W.Ainda não há avaliações
- Jennings 2008 ImagingHemodynamicsDocumento25 páginasJennings 2008 ImagingHemodynamicsAhmed El KaffasAinda não há avaliações
- Lymph SystemDocumento7 páginasLymph SystemghaiathAinda não há avaliações
- Sample Essay BiologyDocumento7 páginasSample Essay Biologyapi-336421734Ainda não há avaliações
- The Lymphatics in Kidney Health and Disease: Michael D. Donnan, Yael Kenig-Kozlovsky and Susan E. QuagginDocumento21 páginasThe Lymphatics in Kidney Health and Disease: Michael D. Donnan, Yael Kenig-Kozlovsky and Susan E. QuagginsilviaAinda não há avaliações
- Cardiovascular LymphaticDocumento17 páginasCardiovascular LymphaticFaisal Ridho SaktiAinda não há avaliações
- Department of Histology, Cytology and EmbryologyDocumento8 páginasDepartment of Histology, Cytology and Embryologysubmen81Ainda não há avaliações
- Anatomyand Physiologyofthe Thoraciclymphatic SystemDocumento15 páginasAnatomyand Physiologyofthe Thoraciclymphatic SystemLis Borda MuñozAinda não há avaliações
- Lec. 1 Selected TopicsDocumento30 páginasLec. 1 Selected TopicsMustafa KamelAinda não há avaliações
- Modeling and Analysis of Blood Flow in Human Circulatory SystemDocumento3 páginasModeling and Analysis of Blood Flow in Human Circulatory SystemPradeep K SinghAinda não há avaliações
- Anatomy of Lymphatics SystemDocumento9 páginasAnatomy of Lymphatics Systemtg856qr4mwAinda não há avaliações
- 24circulation Part 2Documento11 páginas24circulation Part 2Jaydave PatelAinda não há avaliações
- Chapter 16Documento9 páginasChapter 16g_komolafeAinda não há avaliações
- The Lymphatic SystemDocumento7 páginasThe Lymphatic SystemPreeti ChouhanAinda não há avaliações
- Microcirculation & Lymphatics - New-1Documento23 páginasMicrocirculation & Lymphatics - New-1Danial HaiderAinda não há avaliações
- TanisDocumento11 páginasTanisZULMA MADELINE LIBNY GUTARRA TICAAinda não há avaliações
- Anatomy of The Lymphatic SystemDocumento27 páginasAnatomy of The Lymphatic SystemAntonio Lima Filho100% (2)
- Tumor Cell Interaction with Lymphatic Vessels in Cancer Progression and MetastasisDocumento10 páginasTumor Cell Interaction with Lymphatic Vessels in Cancer Progression and MetastasisChetan PatilAinda não há avaliações
- Anatomy of The Lymphatic and Immune Systems - NoteDocumento18 páginasAnatomy of The Lymphatic and Immune Systems - NoteRashini FernandoAinda não há avaliações
- Anatomy and Physiology MidtermsDocumento39 páginasAnatomy and Physiology MidtermsJingky AntonioAinda não há avaliações
- Physical Review Letters Volume 117 issue 13 2016 [doi 10.1103%2FPhysRevLett.117.138301] Ronellenfitsch, Henrik_ Katifori, Eleni -- Global Optimization, Local Adaptation, and the Role of Growth in Dist (1).pdfDocumento5 páginasPhysical Review Letters Volume 117 issue 13 2016 [doi 10.1103%2FPhysRevLett.117.138301] Ronellenfitsch, Henrik_ Katifori, Eleni -- Global Optimization, Local Adaptation, and the Role of Growth in Dist (1).pdfMichele HosackAinda não há avaliações
- Lymphoid Organs ReviewDocumento9 páginasLymphoid Organs Reviewshko noshaAinda não há avaliações
- Chapter 8 - Circulation and ImmunityDocumento94 páginasChapter 8 - Circulation and Immunitychloe06muller.mAinda não há avaliações
- Diuretics: Dr. Ashley M. StokesDocumento26 páginasDiuretics: Dr. Ashley M. StokesDhaif dhaifAinda não há avaliações
- Gashev 2006Documento15 páginasGashev 2006yalocim666Ainda não há avaliações
- tjp0540 1023Documento15 páginastjp0540 1023hjakamjAinda não há avaliações
- Yearly Plan Bio Form5Documento30 páginasYearly Plan Bio Form5maieyAinda não há avaliações
- Comparing Transport in Plants & AnimalsDocumento2 páginasComparing Transport in Plants & AnimalsBio SciencesAinda não há avaliações
- Parts and FunctionsDocumento4 páginasParts and FunctionsGerwin SilvestreAinda não há avaliações
- Notes 20Documento3 páginasNotes 20Paris ShaShaAinda não há avaliações
- Lymphatic System Stu.Documento4 páginasLymphatic System Stu.Rinopro 555Ainda não há avaliações
- 4 Circulatory SystemDocumento23 páginas4 Circulatory SystemSundari D'yojapa NonemAinda não há avaliações
- Lymphatic System: Roles, Functions, and Differences from Blood CirculationDocumento18 páginasLymphatic System: Roles, Functions, and Differences from Blood CirculationNorJannah RAinda não há avaliações
- The Anatomy of The Immune System (Lymphatic SystemDocumento4 páginasThe Anatomy of The Immune System (Lymphatic SystemMohammed R.HusseinAinda não há avaliações
- Lymphatic System ReportDocumento6 páginasLymphatic System ReportcrtgyhujikAinda não há avaliações
- Lymphatic System and Immunity ChapterDocumento18 páginasLymphatic System and Immunity ChapterElvin MoletaAinda não há avaliações
- Nihms 1585884Documento17 páginasNihms 1585884CT DAMAinda não há avaliações
- Cardiovascular and Respiratory Lecture Handout 2023-24Documento40 páginasCardiovascular and Respiratory Lecture Handout 2023-24extreme fattypunchAinda não há avaliações
- Lymphatic SystemDocumento70 páginasLymphatic SystemNang Maizana Megat Yahya100% (1)
- Llymphatic SystemDocumento14 páginasLlymphatic SystemfauziharunAinda não há avaliações
- Anatomy and Physiology of The Circulatory and Ventilatory Systems, ThirietDocumento594 páginasAnatomy and Physiology of The Circulatory and Ventilatory Systems, ThirietSubhajit Chakraborty100% (1)
- Lymphatic SystemDocumento5 páginasLymphatic SystemEmmanuel A. GalvanAinda não há avaliações
- (Robert H Harris) Textbook of Dr. Vodder's ManualDocumento116 páginas(Robert H Harris) Textbook of Dr. Vodder's Manualmitroisergiu100% (10)
- Lymphatic SystemDocumento28 páginasLymphatic SystemRozi Reviana PratiwiAinda não há avaliações
- Anatomy of the Lymphatic and Immune Systems ExplainedDocumento8 páginasAnatomy of the Lymphatic and Immune Systems ExplainedAbdallah AlasalAinda não há avaliações
- Regulation of Tissue Oxygenation: Second EditionDocumento114 páginasRegulation of Tissue Oxygenation: Second EditionrezqAinda não há avaliações
- PLEURAL EFFUSIONS CAUSES AND DIAGNOSISDocumento5 páginasPLEURAL EFFUSIONS CAUSES AND DIAGNOSISnfacmaAinda não há avaliações
- Lymphatic SystemDocumento13 páginasLymphatic SystemCharli ParachinniAinda não há avaliações
- The Lymphatic Fluid: Formation, Circulation, and Immunological RoleDocumento23 páginasThe Lymphatic Fluid: Formation, Circulation, and Immunological RolektorooAinda não há avaliações
- Fisiopatologia Linfedema 1997Documento6 páginasFisiopatologia Linfedema 1997ktorooAinda não há avaliações
- Intrahepatic Cholangiocarcinoma Surgery The ImpactDocumento10 páginasIntrahepatic Cholangiocarcinoma Surgery The Impactraplyhollow_68780740Ainda não há avaliações
- Anatomy of The Human Lymphatic System: Department of Surgery, University of Sao Paulo, BrazilDocumento22 páginasAnatomy of The Human Lymphatic System: Department of Surgery, University of Sao Paulo, BrazilAprodita Permata YulianaAinda não há avaliações
- Importance of lymph in human balanceDocumento1 páginaImportance of lymph in human balanceZaid Bin salmanAinda não há avaliações
- Computational Models in Biomedical Engineering: Finite Element Models Based on Smeared Physical Fields: Theory, Solutions, and SoftwareNo EverandComputational Models in Biomedical Engineering: Finite Element Models Based on Smeared Physical Fields: Theory, Solutions, and SoftwareAinda não há avaliações
- Semiologia UrológicaDocumento137 páginasSemiologia UrológicaAntonio Fernandes Neto100% (3)
- HelloDocumento1 páginaHellonnimrodoAinda não há avaliações
- HelloDocumento1 páginaHellonnimrodoAinda não há avaliações
- HelloDocumento1 páginaHellonnimrodoAinda não há avaliações
- Anhidrosis in EquineDocumento3 páginasAnhidrosis in EquineZain AsifAinda não há avaliações
- Language and BrainDocumento23 páginasLanguage and Brainalbino100% (1)
- Bac ToxinDocumento9 páginasBac ToxinJawairia KhawarAinda não há avaliações
- Nursing Care Plans for Acute Pain, Hyperthermia, Activity Intolerance, and Infection RiskDocumento20 páginasNursing Care Plans for Acute Pain, Hyperthermia, Activity Intolerance, and Infection RiskNursidar Pascual Mukattil80% (5)
- Bio 320 Practical 7Documento12 páginasBio 320 Practical 7MuhammadAsyraf50% (2)
- Enteral NutritionDocumento11 páginasEnteral NutritionEso Soso0% (1)
- Motility Disorders of EsophagusDocumento44 páginasMotility Disorders of EsophagusmackieccAinda não há avaliações
- Zoology Practical Exam Tips 2024Documento62 páginasZoology Practical Exam Tips 2024sureshsooraj426Ainda não há avaliações
- Neuroparasitology PDFDocumento62 páginasNeuroparasitology PDFpsetoAinda não há avaliações
- Snakes in India - Tradition and The Truth PDFDocumento5 páginasSnakes in India - Tradition and The Truth PDFhoticeforuAinda não há avaliações
- 1 - OB 1 (Maternal Anatomy)Documento13 páginas1 - OB 1 (Maternal Anatomy)Gen XAinda não há avaliações
- A Presentation On Pantothenic Acid or b5Documento28 páginasA Presentation On Pantothenic Acid or b5jainsaketAinda não há avaliações
- Throwing RehabDocumento16 páginasThrowing RehabSean GlynnAinda não há avaliações
- Assessment of Fluid and ElectrolyteDocumento15 páginasAssessment of Fluid and ElectrolyteDip Ayan MAinda não há avaliações
- Health Benefits of Running and JoggingDocumento2 páginasHealth Benefits of Running and JoggingOsamaAinda não há avaliações
- Pregnant woman with painful swollen legDocumento12 páginasPregnant woman with painful swollen legjimmojonesAinda não há avaliações
- Hyperosmolar Hyperglycemic Nonketotic Syndrome: Presented by DR MoosallyDocumento10 páginasHyperosmolar Hyperglycemic Nonketotic Syndrome: Presented by DR MoosallyDrsarfaraz SiddiquiAinda não há avaliações
- Brewing Technology (2017)Documento190 páginasBrewing Technology (2017)Јован АдамовAinda não há avaliações
- Yellow Belt Level 01 - Solution - 0Documento2 páginasYellow Belt Level 01 - Solution - 0Jo Marie LeeAinda não há avaliações
- The Ionization of Amino Acids at Physiological pHDocumento4 páginasThe Ionization of Amino Acids at Physiological pHNatasha MahatantilaAinda não há avaliações
- Fluid Volume DeficitDocumento2 páginasFluid Volume DeficitpeternohibiAinda não há avaliações
- NCPDocumento10 páginasNCPbabycheska08Ainda não há avaliações
- Newborn Care PDFDocumento8 páginasNewborn Care PDFZedrake CaraanAinda não há avaliações
- Analgesia AvesDocumento16 páginasAnalgesia AvesJESSICA ZAPATAAinda não há avaliações
- Pediatric DehydrationDocumento27 páginasPediatric DehydrationAbraham ChiuAinda não há avaliações
- ANS & CVS Response To Exercise v2Documento18 páginasANS & CVS Response To Exercise v2chow wing yin amandaAinda não há avaliações
- Prokaryotic Cells: Eukaryotes Vs Prokaryotes: What's The Difference?Documento8 páginasProkaryotic Cells: Eukaryotes Vs Prokaryotes: What's The Difference?Anggun Teh PamegetAinda não há avaliações
- Week 006 Animal-Immune-SystemDocumento13 páginasWeek 006 Animal-Immune-SystemMark Lorens StaanaAinda não há avaliações
- Liver Cirrhosis NCP 1Documento6 páginasLiver Cirrhosis NCP 1Paolo Rafael D EsguerraAinda não há avaliações
- Change Your Life NowDocumento18 páginasChange Your Life NowAbdul Lateef Khan0% (1)


























![Physical Review Letters Volume 117 issue 13 2016 [doi 10.1103%2FPhysRevLett.117.138301] Ronellenfitsch, Henrik_ Katifori, Eleni -- Global Optimization, Local Adaptation, and the Role of Growth in Dist (1).pdf](https://imgv2-1-f.scribdassets.com/img/document/335024555/149x198/c2af002bd6/1482684538?v=1)