Escolar Documentos
Profissional Documentos
Cultura Documentos
Lect4 Respiratory
Enviado por
Nicolai Babalici0 notas0% acharam este documento útil (0 voto)
12 visualizações55 páginasrespiratory
Direitos autorais
© © All Rights Reserved
Formatos disponíveis
PDF, TXT ou leia online no Scribd
Compartilhar este documento
Compartilhar ou incorporar documento
Você considera este documento útil?
Este conteúdo é inapropriado?
Denunciar este documentorespiratory
Direitos autorais:
© All Rights Reserved
Formatos disponíveis
Baixe no formato PDF, TXT ou leia online no Scribd
0 notas0% acharam este documento útil (0 voto)
12 visualizações55 páginasLect4 Respiratory
Enviado por
Nicolai Babalicirespiratory
Direitos autorais:
© All Rights Reserved
Formatos disponíveis
Baixe no formato PDF, TXT ou leia online no Scribd
Você está na página 1de 55
Lecture 4
RESPIRATORY SYSTEM I The Conducting Portion
I. Major functions of respiratory system:
A. Gas exchange: The respiratory system is responsible for taking in oxygen and
eliminating waste gases like carbon dioxide. But it also:
Moistens air (glandular secretions) to prevent dessication of tissues
Warms air
Filters air
B. Body temperature control in some species (horse: 20% of heat generated
during exercise is exchanged across the lung surface)
1. Phonation (production of sound).
D. Metabolic Functions.
1) Inactivates bradykinin, serotonin, prostaglandins, norepinephrine
2) Angiotensin converting enzyme (Angiotensinase) converts angiotensin
I to angiotensin II (blood pressure regulation).
II. Functional adaptations of respiratory tract:
A. Site of gas exchange must have thin walls (alveoli of lungs are very thin).
B. Moistening of air requires glands; usually simple tubuloalveolar
(tubuloacinar) serous or seromucous glands.
C. Air is warmed by blood (erectile tissue); many vessels with thick walls,
extensive terminal vascular bed found along the conducting portion of the
respiratory tract.
D. Filtering of air is accomplished by hair and cilia (particles
deposited/removed)
2. Phonation is possible due to the presence of vocal apparatus.
III. Major subdivisions of mammalian respiratory tract (see Fig 1 on the next
page):
A. Conducting portion: (~150 ml vol in humans)
1) Involved in moving air.
2) Part of tract from nasal cavity through terminal (tertiary) bronchiole in
lung
3) Specific portions are responsible for olfaction and phonation.
General organization of conducting portion:
1) Lumen
2) Epithelium on a thick basal lamina (lines lumen)
3) Lamina propria
- rich vascular connective tissue (ct)
- glands in places
4) perichondrium (dense ct)
5) cartilage (provides support and maintains an open airway)
Respiratory System
Why Study the Respiratory System?
Respiratory system diseases in the domestic
animals are common and may affect the nose,
throat, trachea, or lungs. They are sometimes
combined with diseases of the heart, as in
heartworm infection. Causes of these
disorders include infections, parasites,
cancer, trauma, and toxins.
I. Major Functions of the Respiratory System
D. Metabolic Functions
1. Inactivation of bradykinin (vasodilation),
serotonin,PGE2, NE
2. ACE in lungs converts angiotensin I to
angiotensin II; Angiotensin (vasoconstrictor).
A. Gas exchange and condition the air:
Moisten, warm & filter air
B. Body temperature control (lower body temp - horse
20% heat loss via lung surface during exercise)
C. Phonation (vocalization); olfaction
II. Functional adaptations
Gas exchange - thin walls
Moistening of air - tubuloacinar glands
Warming air - extensive vascular bed
Filtering air - hair and cilia
Larynx for phonation
Components of the Respiratory System
III. Major Subdivisions of Resp. Tract (3):
A. Conducting Portion: nares to terminal
bronchiole in lung
B. Respiratory Portion- Gas Exchange
C. Transitional Portion=Resp. Bronchioles
(conducts & exchanges: carnivores & monkeys
Conducting
Respiratory Portion
Nasopharynx
Transitional
C
o
n
d
u
c
t
i
n
g
Transitional
IV. Respiratory Epithelium (3 main types):
1. Pseudostratified Ciliated Columnar
2.Simple Cuboidal
3. Simple
Squamous
Found
through most
of the
Conducting
portion
V. Functional morphology of conducting region
Nasal cavity
Vestibule-rostral nasal cavity-stratified squamous
Respiratory-PSC
Olfactory
1. Basal cells
2. Olfactory Cells
3. Supporting Cells
Paranasal sinuses
Vomeronasal organ
Nasopharynx
Larynx
Trachea
Bronchi
A. NASAL CAVITY
1. Vestibule:
- rostral- stratified
squamous epithelium
- site of transition from
integument to mucous
membrane of nasal
cavity.
- resembles the skin
- melanocytes
- hairs
- sweat glands
- sebaceous glands
A. NASAL CAVITY
2. Respiratory portion
Most of nasal cavity
Area of conchae (turbinates) -
Epithelium: pseudostratified ciliated columnar
epithelium with goblet cells
Also specialized cells like brush cells (sensory), nonciliated cells
with SER, basal cells
Lamina Propria: Connective tissue containing -
Mixed, mainly serous, glands to moisten & Erectile
tissue to warm the air
Thin Shelf of Bone (cartilage)- forms core of Conchae
Inhaled particles removed in nasal passages
2. Respiratory Portion
e) Nasal conchae:
- bony shelves of tissue
extending from the
lateral walls of the
nasal cavity
- increase surface area
for conditioning inspired
air. Ethmoidal Labyrinth
Ventral
conchae
(Olfactory Epithelium)
Dorsal Conchae
2. Concave surface:
- unexposed (less exposed)
- respiratory epithelium
- more cilia
- less extensive glandular
development.
e. Conchae:
1. Convex Surface
-PSC with cilia (i.e,
respiratory epithelium)
- exposed to air and
subject to drying (many
serous glands)
- richly vascular
(conditioning of air)
-Olfactory: Ethmoturbinates - olfactory mucosa on one side and
-Respiratory epithelium on the other side (core of bone-center)
Nerves
3. Olfactory Portion
A. Nasal Cavity
- caudal nasal cavity
- thick PSC epith. (appears to
have many layers but all
cells reach the basal lamina)
- few goblet cells
- bipolar neurons
- unmyelinated axons
(3) Olfactory
Surface:
epithelium
Handout:Figure 2
V. Functional Morphology of Conducting Portion
B. Paranasal Sinuses
- spaces in maxillary, frontal, ethmoid and sphenoid
bones that are continuous with nasal cavity
- thin respiratory epithelium (PSC with cilia)
- continuous with nasal cavity
- few nasal glands and goblet cells; adhered to bone
- no erectile tissue
Frontal Sinus
Mouse
Snout
Embryo:
Vomeronasal
Organ
C. Vomeronasal organ
- more important
to some species.
- opens into duct
that connects oral
and nasal cavities.
- permits sampling
of volatilized
substances (pheromones).
Diseases of the Nasal Cavity: Chronic diseases of
the Nasal Cavity are typically due to inflammation
or neoplasm.
Rhinitis is the term applied to an infection or
inflammation of the nose. If the sinuses are
also involved, it is called sinusitis. There are
many bacteria, fungi, and viruses capable of
infecting the noses of dogs & cats. These
infections behave very similarly to common
colds in people.
Distemper virus can affect many systems of the body.
The most common signs related to the respiratory
system are nasal discharge and coughing
V. Functional Morphology
of the Conducting Portion
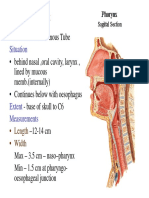
D. Nasopharynx:
- located dorsal to the soft
palate.
- connects nasal cavity with
the oropharynx.
- pseudostratified columnar
epithelium (some stratified
squamous caudodorsally)
- pharyngeal tonsil:
organized lymphoid tissue
located above the soft
palate and it has PSC
epithelium
Nasopharynx
E. Larynx:
- First solely respiratory
structure.
- Cartilage framework
-striated musculature
-May contain taste buds
-Intrinsic: respiration and
- phonation
- lined by PSC (stratified
squamous lines epiglottis
vestibule and vocal fold)
- Functions:
1) air conduit
2) phonation
- branched tubuloalveolar glands (gl)- mucoid or mixed
(lubrication).
Nonkeratinized
stratified squamous
Respiratory
Lumen
2
Lumen
Image 1
Image 2
Vocal Fold-Larnyx
Tunica
Muscularis
Ventricle
Lumen
Larynx
Conducting Portion: Trachea to Terminal
Bronchioles
F. Trachea: Provides
passage from larynx to
bronchi
Layers:
1) Tunica mucosa-
submucosa
- ciliated PSC with goblet
cells
- lamina propria (ct)
- elastic fibers (mm)
- submucosa of ct. and
tubuloalvelar glands
(mucous or mixed).
2) Tunica muscularis
- C-shaped cartilage rings
- smooth tracheal muscle
which can narrow lumen
to increase air velocity
(cough)
3) Tunica adventitia
- loose vascular ct.
Lamina propria
Tunica Muscularis
Tunica Mucosa/submucosa
Tunica Adventitia
Lumen
Dog Trachea: Low Magnification
Trachea
Trachea,
High Mag
Scanning Electron
Micrograph of the
Trachea
Clinical Note: A disorder known as Tracheal
Collapse is commonly seen in toy and
miniature breeds, especially the Yorkshire
terrier, pomeranian, and toy poodle. It is
characterized by a narrowing of the inner
diameter of the trachea, that fluctuates with the
stage of the respiratory cycle. Affected dogs
typically have a harsh, dry "honking" cough that
is paroxysmal in nature and gradually becomes
worse over time. Either the cervical, or both
cervical and thoracic trachea may be involved.
If both, then inspiratory radiographs usually
show collapse of the cervical and dilation of the
thoracic segments, and essentially the reverse
on expiration. Fluoroscopy may be necessary to
confirm the diagnosis, as sometimes collapse is
only evident during forced expiration of
coughing. Most cases can be treated
successfully medically, with the use of
bronchodilators, nebulizers or vaporizers, and
occasional use of corticosteroids or sedatives.
G. Bronchi: Note - If its got cartilage, its a
bronchus not a bronchiole!
Divided into: Primary (outside lung), secondary and tertiary (inside lung):
Primary-structurally similar to trachea
1.PSC epithelium; decreased goblet cells distally
2. Lamina propria-thin layer of conn tiss with many leukocytes; Lymphoid
nodules present (especially at the branching sites)
3. Muscularis mucosa is distinct, separates lamina propria/submuc; this muscle
contracts in asthma and reduces lumen of bronchus
4. Tunica Submucosa: loose CT with elastic fibers and glands. Highly elastic for
expansion and recoilation of lung during respiration
5. Cartilage Plates: Cartilage plates diminish in size distally (toward bronchioles)
Bronchial fluid--mucin, serum proteins, lactoferrin, immunoglobulins-IgA,
glycoproteins
Primary bronchi:-
extra pulmonary
-structure as in trachea
-except all layers are thinner
( plates of cartilage)
Secondary bronchi:
- intrapulmonary
more distal:
- ciliate PSC becomes
ciliated simple columnar
- decrease in #- goblet cells
- cartilage begins to be
replaced by smooth
muscle
lamina propria- thin layer of conn. tiss. with lymphoid elements
- smooth muscle layer- contracts to narrow lumen (asthma).
Structure of a secondary bronchus
Smooth muscle
Cartilage
Epithelium
Lamina propria
Submucosa
T. Mucosa
Lumen
Clinical Note: Canine infectious
tracheobronchitis (kennel cough) is one of the
most prevalent infectious diseases in dogs.
Fortunately, the majority of cases are not serious
resolving on their own in 1 to 2 weeks. The main
cause of kennel cough is the airborne bacteria,
Bordetella bronchiseptica, but it can also be
caused by a number of viruses. Clinical cases of
Kennel Cough are usually caused by several
infectious agents working together to damage
and irritate the lining of the dog's trachea and
upper bronchi. The damage to the tracheal lining
is fairly superficial, but exposes nerve endings
that become irritated simply by the passage of
air over the damaged tracheal lining. Once the
organisms are eliminated the tracheal lining will
heal rapidly
Respiratory system
LAB Introduction
Concave
Convex
Convex (outer) surface of the turbinate:
Pseudostratified columnar epithelium, goblet cells,
serous/mixed glands, vascular bed-erectile tissue for
heat exchange
Epithelium
Cartilage
Vessels
Concave (inner) surface of the turbinate: PSC epithelium
with goblet cells, relatively thin epithelium, mixed glands-
primarily serous, large blood vessels, scattered lymphocytes in
the lamina propria, decreased # of nerve bundles
Epithelium
Glands
Outer Conchae/Horse Nasal Cavity
Olfactory epithelium: olfactory receptor neurons,
sustentacular cells, basal cells, seromucous glands,
nerve bundles
Olfactory
Epithelium
Nerve
bundle
Larynx: connects pharynx and trachea.
Image 1
Image 2
Mucous Glands
Larynx components--Epiglottis:
- leaf-like valve (prevents material from entering the larynx).
- core - elastic cartilage
- stratified squamous epithelium
- taste buds may be present on oral side (carnivores, swine & ruminants)
Elastic Cartilage
Stratified
Squamous Ep.
Trachea
Muscle Attaches to
Outside of Cartilage
In Carnivores
Pseudostratified Columnar
Goblet cells
Lamina
Propria
Tracheal wall:PS
columnar epithelium
+ Goblet Cells
LP: elastic fibers
Submucosa: Glands
Connective tissue
PSC
Submucosa
Branching pattern
Secondary bronchus of cat
Bronchial wall: PS columnar epithelium
Elastic fiber
GC
Simple columnar
LP: seromucus glands seen less as the bronchi become smaller
Smooth
Muscle
submucosa
Lumen
Muscularis
Mucosae
Lamina propria
Clara cell
Bronchiole: simple columnar epithelium, less # GC,
more clara cells. As bronchioles become smaller,
columnar epithelium becomes cuboidal epithelium.
LP; elastic fibers (lymphocytes present)
Muscularis Mucosa
Terminal bronchi; simple cuboidal epithelium, large
# of clara cells present, no GC.
LP: No glands present
Terminal respiratory pathway:Alveoli open into
respiratory bronchiole (RB). Alveoli (A) open
into alveolar duct (AD), AS-space around a group of alveoli
Você também pode gostar
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryNo EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryNota: 3.5 de 5 estrelas3.5/5 (231)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)No EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Nota: 4.5 de 5 estrelas4.5/5 (119)
- Never Split the Difference: Negotiating As If Your Life Depended On ItNo EverandNever Split the Difference: Negotiating As If Your Life Depended On ItNota: 4.5 de 5 estrelas4.5/5 (838)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaNo EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaNota: 4.5 de 5 estrelas4.5/5 (265)
- The Little Book of Hygge: Danish Secrets to Happy LivingNo EverandThe Little Book of Hygge: Danish Secrets to Happy LivingNota: 3.5 de 5 estrelas3.5/5 (399)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyNo EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyNota: 3.5 de 5 estrelas3.5/5 (2219)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeNo EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeNota: 4 de 5 estrelas4/5 (5794)
- Team of Rivals: The Political Genius of Abraham LincolnNo EverandTeam of Rivals: The Political Genius of Abraham LincolnNota: 4.5 de 5 estrelas4.5/5 (234)
- The Emperor of All Maladies: A Biography of CancerNo EverandThe Emperor of All Maladies: A Biography of CancerNota: 4.5 de 5 estrelas4.5/5 (271)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreNo EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreNota: 4 de 5 estrelas4/5 (1090)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersNo EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersNota: 4.5 de 5 estrelas4.5/5 (344)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceNo EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceNota: 4 de 5 estrelas4/5 (890)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureNo EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureNota: 4.5 de 5 estrelas4.5/5 (474)
- The Unwinding: An Inner History of the New AmericaNo EverandThe Unwinding: An Inner History of the New AmericaNota: 4 de 5 estrelas4/5 (45)
- The Yellow House: A Memoir (2019 National Book Award Winner)No EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Nota: 4 de 5 estrelas4/5 (98)
- Assessment of The Lower LimbDocumento496 páginasAssessment of The Lower Limbkacheren100% (4)
- Melee Weapons GuideDocumento36 páginasMelee Weapons GuideKim100% (1)
- Volume 15, Number 5 May 2011Documento188 páginasVolume 15, Number 5 May 2011Nicolai BabaliciAinda não há avaliações
- ECA1 Tests Language Test 7C New2018Documento6 páginasECA1 Tests Language Test 7C New2018Kamila RoguzińskaAinda não há avaliações
- CT Mbbs by DR ShamolDocumento197 páginasCT Mbbs by DR ShamolSiva Sandeep Chennimalai50% (2)
- Punctuation Quiz AnswersDocumento9 páginasPunctuation Quiz AnswersFirda Isran NafisahAinda não há avaliações
- High Resolution CT of The Lung Patterns of Disease and Differential DiagnosesDocumento30 páginasHigh Resolution CT of The Lung Patterns of Disease and Differential DiagnosesNicolai Babalici100% (1)
- Create Races in 20 MinutesDocumento8 páginasCreate Races in 20 MinutesRennik McCaigAinda não há avaliações
- Lymphangioleiomyomatosis A Clinical Update ChestDocumento12 páginasLymphangioleiomyomatosis A Clinical Update ChestNicolai BabaliciAinda não há avaliações
- Chronic Respiratory DiseasesDocumento25 páginasChronic Respiratory DiseasesNicolai BabaliciAinda não há avaliações
- Volume 15, Number 3 March 2011Documento152 páginasVolume 15, Number 3 March 2011Nicolai BabaliciAinda não há avaliações
- Volume 15, Number 6 June 2011Documento183 páginasVolume 15, Number 6 June 2011Nicolai BabaliciAinda não há avaliações
- OnchiectasisDocumento33 páginasOnchiectasisNicolai BabaliciAinda não há avaliações
- Volume 15, Number 4 April 2011Documento162 páginasVolume 15, Number 4 April 2011Nicolai BabaliciAinda não há avaliações
- Volume 15, Number 1 January 2011Documento233 páginasVolume 15, Number 1 January 2011Nicolai BabaliciAinda não há avaliações
- Volume 15, Number 2 February 2011Documento154 páginasVolume 15, Number 2 February 2011Nicolai BabaliciAinda não há avaliações
- Vascular Physiology 3Documento39 páginasVascular Physiology 3Nicolai BabaliciAinda não há avaliações
- Volume 15, Number 2 February 2011Documento154 páginasVolume 15, Number 2 February 2011Nicolai BabaliciAinda não há avaliações
- Volume 15, Number 1 January 2011Documento233 páginasVolume 15, Number 1 January 2011Nicolai BabaliciAinda não há avaliações
- Tale of 12 Chinese ZodiacDocumento32 páginasTale of 12 Chinese ZodiacAiman HassanAinda não há avaliações
- NROSCI 1012 - Lecture 1Documento3 páginasNROSCI 1012 - Lecture 1HonzaAinda não há avaliações
- Catclass NotesDocumento3 páginasCatclass NotesIssac CaldwellAinda não há avaliações
- AVMA Guidelines On EutthanasiaDocumento98 páginasAVMA Guidelines On EutthanasiatenguayacoAinda não há avaliações
- 5thsem (FP) Atk Menu 6 10Documento11 páginas5thsem (FP) Atk Menu 6 10Deepak Billa67% (3)
- Find The Temperature Using CricketsDocumento2 páginasFind The Temperature Using CricketsMoreMoseySpeedAinda não há avaliações
- Answers & Solutions: NEET (UG) - 2019Documento35 páginasAnswers & Solutions: NEET (UG) - 2019Gowri ShankarAinda não há avaliações
- Organization of Nervous System: Anatomic DivisionsDocumento2 páginasOrganization of Nervous System: Anatomic DivisionsDr P N N ReddyAinda não há avaliações
- Geo World CatalogDocumento192 páginasGeo World Catalogthinewill_bedone8055Ainda não há avaliações
- About TractorDocumento28 páginasAbout TractorCristy DaylagAinda não há avaliações
- Science Notes Sem1 PDFDocumento31 páginasScience Notes Sem1 PDFWolfie Saraswathi Santhosham100% (1)
- Arthropod ParasiteDocumento3 páginasArthropod ParasiteJayson Tafalla LopezAinda não há avaliações
- Dissecting Pig and Chicken's Heart - Plant vs Animal CellsDocumento3 páginasDissecting Pig and Chicken's Heart - Plant vs Animal CellsRosemarie R. ReyesAinda não há avaliações
- How To Be A Genius Your Brain and How To Train ItDocumento28 páginasHow To Be A Genius Your Brain and How To Train ItmathieuAinda não há avaliações
- Reducing Excess Fluid Volume in a Patient with Chronic Kidney DiseaseDocumento10 páginasReducing Excess Fluid Volume in a Patient with Chronic Kidney DiseasePerrilyn PereyAinda não há avaliações
- Simple Present Tense 11Documento6 páginasSimple Present Tense 11priscila_espinoza_50% (1)
- Animal Farm: George Orwell's Critique of StalinismDocumento55 páginasAnimal Farm: George Orwell's Critique of StalinismQuang Anh LuuAinda não há avaliações
- Consonant VowelDocumento8 páginasConsonant Vowelabc_teacher100% (1)
- Eduardo Serrão - Potential Business For Chickens and Pigs and Their Products in Timor-LesteDocumento6 páginasEduardo Serrão - Potential Business For Chickens and Pigs and Their Products in Timor-LestePapers and Powerpoints from UNTL-VU Joint Conferenes in DiliAinda não há avaliações
- H & N - Pharynx& Deglutition PDFDocumento17 páginasH & N - Pharynx& Deglutition PDFRamin AmirkhiziAinda não há avaliações
- Infectios DiseasesDocumento183 páginasInfectios DiseasesAnonymous eson90Ainda não há avaliações
- Animal Science HandoutDocumento5 páginasAnimal Science Handoutromnickatchecoso14Ainda não há avaliações
- Histology AssignmentDocumento4 páginasHistology AssignmentNico LokoAinda não há avaliações
- Unit 15: at The Dining Table.: Exercise 1: W Rite The Words: Egg Bread Milk Rice Juice Water Meat Fish Bean ChickenDocumento13 páginasUnit 15: at The Dining Table.: Exercise 1: W Rite The Words: Egg Bread Milk Rice Juice Water Meat Fish Bean ChickenThảo TrangAinda não há avaliações
- Animal Identification Systems: Dr. FarooqDocumento15 páginasAnimal Identification Systems: Dr. FarooqmfmalikAinda não há avaliações