Escolar Documentos
Profissional Documentos
Cultura Documentos
A 100 Year Update On Diagnosis of Tuberculosis Infection PDF
Enviado por
Rahmiati LaoDescrição original:
Título original
Direitos autorais
Formatos disponíveis
Compartilhar este documento
Compartilhar ou incorporar documento
Você considera este documento útil?
Este conteúdo é inapropriado?
Denunciar este documentoDireitos autorais:
Formatos disponíveis
A 100 Year Update On Diagnosis of Tuberculosis Infection PDF
Enviado por
Rahmiati LaoDireitos autorais:
Formatos disponíveis
Published Online November 18, 2009
A 100 year update on diagnosis of tuberculosis
infection
Ajit Lalvani* and Manish Pareek
Tuberculosis Research Unit, Department of Respiratory Medicine, National Heart and Lung
Institute, Imperial College London, London, UK, and Department of Infectious Disease
Epidemiology, Imperial College London, London, UK
Areas of agreement: IGRAs are more specific than TST for diagnosis of LTBI as
they are not confounded by previous bacille Calmette-Guerin (BCG) vaccination.
Assessing IGRA sensitivity in the absence of a gold standard for LTBI is
challenging. Studies have therefore used surrogate markers such as active TB
and correlation with degree of TB exposure in contact investigations. These
studies suggest that sensitivity of ELISpot is higher than TST while whole-blood
ELISA has similar sensitivity to TST. Recent longitudinal studies demonstrating
the prognostic power of these tests for development of active TB provide
definitive evidence that positive IGRA results reflect infection with dormant yet
viable bacilli.
Areas of controversy: Is the prognostic power of IGRAs greater than the TST?
What are the false-negative rates in immunocompromised individuals with LTBI
at high risk of progressing to active TB?
Accepted: October 7,
2009
*Correspondence to: Ajit
Lalvani, Tuberculosis
Research Unit,
Department of
Respiratory Medicine,
National Heart and Lung
Institute, Imperial College
London, London, UK.
E-mail: a.lalvani@imperial.
ac.uk
Growing points: IGRAs have been incorporated into national guidelines,
although their optimal deployment in diagnostic algorithms is evolving. The
health economic benefits of utilizing IGRAs are increasingly recognized, partly
because their high specificity avoids unnecessary chemoprophylaxis in BCGvaccinated persons with false-positive TST results.
Areas timely for developing research: Current IGRAs are being improved and
next-generation tests, with improved sensitivity, could enable the reliable
exclusion of LTBI in immunocompromised individuals.
Keywords: latent tuberculosis/interferon-gamma release assays/tuberculosis
infection/review
British Medical Bulletin 2010; 93: 6984
DOI:10.1093/bmb/ldp039
& The Author 2009. Published by Oxford University Press. All rights reserved.
For Permissions, please e-mail: journals.permissions@oxfordjournals.org
Downloaded from http://bmb.oxfordjournals.org/ at Gadjah Mada University on December 4, 2014
Background: Diagnosis and treatment of latent tuberculosis infection (LTBI) is a
cornerstone of tuberculosis (TB) control in the developed world. In the last
century, the tuberculin skin test (TST) was the only means of diagnosing LTBI.
ELISpot and whole-blood ELISA, collectively known as interferon-gamma release
assays (IGRAs), are promising new tools.
A. Lalvani and M. Pareek
Introduction
The global epidemiology of latent TB infection
With an estimated one-third of the worlds population latently infected
with TB (LTBI),3 and therefore potentially at future risk of developing
active disease, increasing importance is being accorded to the effective
identification and treatment of individuals with LTBI, particularly in
low TB burden countries where latently infected migrants and recently
infected contacts of smear-positive cases account for the bulk of the TB
case-load.4
Data on TB natural history suggest that in the first 2 years following
initial infection with tubercle bacilli 5% of infected individuals will
progress to active disease;5 if the bacilli are brought under immune
control they may lie dormant for several decades with only a further
5 10% of infected immunocompetent people eventually going on to
develop active disease over their lifetime.5 As a result, the diagnosis
and treatment of LTBI will be most effective if it is specifically targeted
at those individuals with the highest risk of progression from LTBI to
active disease including: recently infected individuals and all those with
underlying immunosuppression.6
Methods of diagnosing LTBI
Making the diagnosis of LTBI is constrained by a low bacteria load
that makes it impossible to directly detect Mycobacterium tuberculosis
and a weak humoral response that makes serological testing unreliable.
As a consequence, for much of the previous century, diagnosis of LTBI
has been defined as a positive tuberculin skin test (TST) in an asymptomatic person exposed to tuberculosis with no other evidence of active
disease. The utility of the TST is that it detects a cutaneous delayedtyped hypersensitivity response to purified protein derivative (PPD),
70
British Medical Bulletin 2010;93
Downloaded from http://bmb.oxfordjournals.org/ at Gadjah Mada University on December 4, 2014
Globally, tuberculosis (TB) continues to be one of the leading infectious causes of morbidity and mortality accounting for an estimated
9 million cases and 2 million deaths per year.1 This failure to adequately control the global epidemic may partly reflect the slow progress
that has been made, over the last century, in developing innovative
diagnostic tools for TB.2 However, the potential to significantly
advance TB control now exists with the development of novel diagnostic modalities for latent TB infection (LTBI).
A 100 year update on diagnosis of tuberculosis infection
a mixture of over 200 M. tuberculosis proteins. However, the TST is
neither specific, as the antigens present in PPD cross-react with bacille
Calmette-Guerin (BCG) and environmental mycobacteria, nor sensitive, due to anergy in those individuals with a compromised immune
system (such as HIV, iatrogenic immunosuppression and children).
T-cell interferon gamma release assays
Performance of IGRAs in the diagnosis of LTBI
Objectively comparing the diagnostic performance of the IGRAs and the
TST is hindered by the lack of a gold standard reference test for LTBI
that makes it impossible to directly measure sensitivity and specificity. As
a result, investigators have utilized proxy markers of LTBI including:1
degrees of exposure to infectious cases,2 active TB as a surrogate for
LTBI and, to assess specificity,3 the presence of IGRA negativity in
healthy BCG-vaccinated individuals at low risk of TB infection due to the
absence of epidemiologic risk factors for tuberculosis exposure.
Clinical performance of IGRAs in immunocompetent
individuals
Correlation with TB exposure of IGRA results
An important facet of TB transmission is that the risk of acquiring
M. tuberculosis is primarily determined by the frequency, duration and
British Medical Bulletin 2010;93
71
Downloaded from http://bmb.oxfordjournals.org/ at Gadjah Mada University on December 4, 2014
T-cell interferon gamma release assays (IGRAs) have been developed as
an alternative immunodiagnostic approach to the TST for detecting
M. tuberculosis infection.7 Currently 2 ex vivo assays are available: the
ELISpot that directly counts the number of IFN-g secreting T-cells and
the whole-blood ELISA that measures the concentration of IFN-g
secretion. Commercially, the ELISpot assay is available as the
T-SPOTTM.TB (Oxford Immunotec, Abingdon, UK) and the ELISA as
the QuantiFERONTM -TB Gold In-Tube (Cellestis, Carnegie, Australia).
Both IGRAs incorporate two antigensearly secretory antigen target-6
(ESAT-6) and culture filtrate protein-10 (CFP-10)which are strong
targets of Th1 T-cells in M. tuberculosis infection but also deleted
from all strains of BCG and the majority of environmental mycobacteria (except M. Kansasi, M. szulgai, M. marinum, M. flavescens and
M. gastrii).8,9 Therefore, in comparison with the TST, T-cell responses
to these antigens are not confounded by prior BCG vaccination and
hence a more specific marker of TB infection.2
A. Lalvani and M. Pareek
72
British Medical Bulletin 2010;93
Downloaded from http://bmb.oxfordjournals.org/ at Gadjah Mada University on December 4, 2014
proximity of contact with an infectious source case.10 Hence, if a new
test is more sensitive and specific than the TST it should correlate more
closely with the level of exposure to M. tuberculosis and be independent of BCG status.11
Outbreak and contact-tracing investigations have made use of this
theory to compare the diagnostic accuracy of IGRAs and the TST11,12
and concluded that both IGRAs correlate either as well as, or better
than, the TST with levels of exposure to tuberculosis whilst also being
independent of BCG status. In one of the largest, and earliest, studies
of this type the ELISpot was employed in a large school outbreak investigation comprising 535 students.12 ELISpot results, but not TST
results, were independent of the BCG vaccination status, indicating
higher specificity. Overall, ELISpot also correlated better with tuberculosis exposure (based on proximity and duration of exposure to the
index case) than TST suggesting a higher diagnostic sensitivity for
LTBI.12 Other work from varying TB burden settings has also confirmed that the ELISpot significantly correlates with TB exposure.13 17
In a recent study of South African children, positive ELISpot and TST
results were found to be significantly associated with the degree of
exposure to smear-positive index cases.17
Studies have also confirmed that the ELISA significantly correlates
with exposure to TB.18 21 In a recent case control study from Nigeria,
a dose response relationship was found between bacillary load in the
sputum of index cases and ELISA positivity in child contacts;20 children who had been in contact with the most heavily smear-positive
index cases, rather than smear-negative adults, were more likely to be
TST and ELISA positive.20 However, in contrast, a study from a South
African township of children at high risk of LTBI does not find any significant relationship between ELISA positivity and levels of exposure.22
An important outcome of these studies is an assessment of the level
of concordance between the IGRAs and TST. In BCG-vaccinated populations, there are lower levels of agreement between IGRAs and the
TST. This is to be expected as the TST, but not IGRAs, are confounded
by BCG vaccination. Where the ELISpot assay has been studied, generally moderate to high levels of agreement with the TST have been
found.12,13,15,23
On the other hand, the concordance between the ELISA and the TST
appears to be more variable; across a variety of TB burden settings investigators have found agreement between the ELISA and TST ranges from
high to poor.13,18,19,21 Studies in non-BCG vaccinated children from
Australia and Spain, which are low TB burden countries, have found
that the ELISA remained negative in a significant proportion of children
with a positive TST.13,21 These data suggest that the ELISA may have a
lower sensitivity than the TST in diagnosing LTBI in children.
A 100 year update on diagnosis of tuberculosis infection
However, the significance of discordant TST/IGRA results cannot be
reliably elucidated by these cross-sectional studies and will require data
from longitudinal studies.
Active TB as a surrogate marker for LTBI
Clinical performance of IGRAs in immunocompromised
individuals
The strategy for diagnosis and treatment of LTBI is based on targeted
tuberculin testing, which targets persons at highest risk of progression
from LTBI to active tuberculosis. This group particularly includes
HIV-positive individuals and people with immune-mediated inflammatory diseases (such as inflammatory bowel disease and inflammatory
arthritides) who are iatrogenically immunosuppressed or receiving
anti-TNF therapy.25 In these populations with impaired cellular immunity, there is a need to assess the diagnostic performance of IGRAs as an
alternative to the TST, which is well-recognized to have poor sensitivity.
HIV-seropositive individuals
Following the early reports on the diagnostic performance of IGRAs in
HIV-positive individuals26,27 a number of studies have added to the
evidence base to show that the ELISpot has a higher sensitivity than
the TST.26 30 A recent German study of HIV-positive individuals
found that the ELISpot was more sensitive than the TST and also correlated with previous active TB unlike the ELISA or TST.30 Other
studies from high-burden settings in Africa have also found that the
ELISpot has a high sensitivity in both children and adults. Liebeschuetz
et al.27 conducted a prospective study in South African children with a
high prevalence of HIV coinfection, which showed that the sensitivity
British Medical Bulletin 2010;93
73
Downloaded from http://bmb.oxfordjournals.org/ at Gadjah Mada University on December 4, 2014
As infection with M. tuberculosis is a prerequisite for active TB
disease, this principle has been exploited as an alternative surrogate
marker for TB infection by several studies evaluating the diagnostic
sensitivity of IGRAs. Pai et al. 24 have recently systematically reviewed
these studies and concluded that the ELISpot had a pooled sensitivity
of 90% (range 832100%) which was significantly higher than the
pooled sensitivities of the second generation ELISA (78%, range
55288%) and the latest generation ELISA (QuantiFERON-Gold
in-tube, pooled 70%, range 64293%).
A. Lalvani and M. Pareek
Individuals with immune mediated inflammatory diseases
Published experience of the performance of the IGRAs in diagnosing
LTBI in immune mediated inflammatory diseases (IMID) is still fairly
limited and is mainly drawn from small-scale cross-sectional studies that
have concentrated on evaluating the concordance between the TST and
IGRAs rather than correlating IGRA results with risk factors for TB
infection. In general, these studies have found that agreement between
74
British Medical Bulletin 2010;93
Downloaded from http://bmb.oxfordjournals.org/ at Gadjah Mada University on December 4, 2014
of the ELISpot was higher than that for the TST and unaffected by
HIV infection, malnutrition and age under 3 years. Overall sensitivity
of ELISpot in children with culture confirmed, or highly probable, TB
was 83%, rising to 91% when combined with the TST.27 Conversely,
the TST alone had a sensitivity of only 36% in those with HIV infection. In a study looking at HIV-positive Zambian adults coinfected
with sputum smear-positive TB, ELISpot sensitivity was maintained at
92%.26 Subsequent studies with ELISpot have shown that the results
remain robust in HIV infection and independent of CD4 cell
count.27,29 31 Independent work by Clark et al.32 and Dheda et al.31
has found that CD4 cell counts do not affect the ELISpot performance
in HIV-positive individualsboth in terms of positivity and the frequency of indeterminate results.
However, the experience gained from using the ELISA in HIV-positive
individuals seems to be more inconsistent. Raby et al. 33 recently evaluated the ELISA in a cross-sectional study of Zambian adults with smearpositive TB, and found that the sensitivity of the ELISA in HIV-positive
individuals was 63%, which was significantly lower than the 84% sensitivity seen in HIV-negative individuals. In a South African study of
HIV-positive individuals comparing the IGRAs and TST in the diagnosis
of TB infection, the sensitivity of the ELISA (28%) was lower than that
for the ELISpot (61%) and the TST (41%).28 On the other hand,
Balcells et al.34 found that in HIV-positive adults the ELISA had a
higher positivity rate than the TST and correlated with TB exposure
whilst the TST did not. In addition, CD4 cell counts did not have an
adverse effect on ELISA results. However, other authors have found that
in advanced HIV where there are low CD4 cell counts, the performance
of the ELISA is compromised. Brock et al. 35 conducted a large crosssectional study of HIV-positive individuals in Denmark and found a significant association between low CD4 cell count and indeterminate
ELISA results. Subsequent studies have also confirmed that with declining CD4 count, false negative and indeterminate results become increasingly common, which may affect the diagnostic utility of the ELISA in
HIV-positive individuals.28,33,35,36
A 100 year update on diagnosis of tuberculosis infection
Specificity of IGRAs
To estimate the diagnostic specificity quantitatively, BCG-vaccinated
individuals at an ultra-low risk of LTBI due to the absence of epidemiologic risk factors for tuberculosis exposure have been studied. The
ELISA has been assessed in larger numbers of individuals in such
studies than the ELISpot. In a recent systematic review the specificity of
the ELISA ranged from 89 to 100% with a pooled specificity of 99%
for the second-generation ELISA and 96% for the latest generation,
in-tube ELISA.24 The pooled specificity of the ELISpot was also high:
93% (range 85 100%).24 On the whole, both IGRAs have consistently
been shown to have a higher specificity than the TST particularly in
BCG-vaccinated populations.
Reliability of the IGRAs in routine clinical use: indeterminate
results
Over the last few years the IGRAs have increasingly been incorporated into routine clinical use, which makes it imperative to evaluate
British Medical Bulletin 2010;93
75
Downloaded from http://bmb.oxfordjournals.org/ at Gadjah Mada University on December 4, 2014
the TST and IGRAs is, at best, fair in individuals with IMID and that
discordant TST-positive, IGRA-negative results are associated with prior
BCG vaccination.37 39 Conversely, recent work from Italy by Bartalesi
et al. 40 where individuals with IMID were screened for LTBI using the
ELISA and TST found a relatively higher concordance (k 0.55) and
less TST-positive, IGRA-negative discordancy, which possibly reflects
the low proportion of BCG-vaccinated individuals in their population.
Fewer studies have correlated IGRA and TST results in individuals
with IMID with risk factors for LTBI. In a study of 142 patients with
IMID, the ELISA was significantly more closely associated with the
presence of risk factors for LTBI than TST. In addition, a positive TST,
but not IGRA, was significantly associated with previous BCG vaccination.37 Martin et al.41 evaluated both IGRAs in individuals with
inflammatory arthritides and found that both the ELISpot and the
ELISA correlated with risk factors for LTBI. Data from a large Italian
study revealed that individuals who had been in close contact with
smear-positive TB patients were significantly more likely to have a
positive ELISA and TST result.40
On the basis of the current evidence, one can conclude that although
false-negative IGRA results may occur, the diagnostic sensitivity of
IGRAs is more robustly maintained than that of the TST in individuals
with IMID on immunosuppressive treatment.
A. Lalvani and M. Pareek
their reliability. Indeterminate results occur for both IGRAs2 and can
arise for many reasons but the most significant cause is a failed positive
control that usually reflects underlying cellular immune suppression.
Studies suggest that indeterminate results are relatively common with
the ELISA occurring in 5240% of cases with the second-generation
ELISA but less frequently with the newer in tube ELISA.42 44
Indeterminate ELISA results seem to be associated with extremes of
age (under 5 and over 80) and immunosuppression, especially HIV
infection.35 In contrast, indeterminate results are rarer with the
ELISpot occurring in 0 5.4% of tests undertaken.45
Clinical benefits from chemoprophylaxis for LTBI can only occur if
IGRA-positive contacts are truly at increased risk of subsequently progressing to active TB compared with IGRA-negative contacts.
Longitudinal data, which can answer this important question, have
recently begun to appear from studies that aim to assess the predictive
value of IGRAs (see Table 1).46 50 Aichelberg et al.50 explored the
prognostic power of a positive ELISA result in TB uninfected
HIV-positive individuals. Over a median follow-up period of 19
months, 3/37 individuals with a positive ELISA at baseline went on to
develop active TB whereas 0/738 with a negative ELISA subsequently
developed TB. A German study in 601 contacts found that a significantly higher proportion of untreated household contacts with a positive ELISA progressed to TB disease as compared with contacts with a
5 mm positive TST; all six incident cases were ELISA positive at
recruitment.46
Bakir et al.47 conducted a large study of 908 child contacts in
Turkey. During the follow-up period of 1.3 years, 15 incident cases
occurred and the investigators found that contacts with a positive
ELISpot had a significantly increased risk of developing active TB as
compared with those contacts with a negative ELISpot. In this study,
TB incidence in the ELISpot positive contacts was similar to that in
TST positive contacts though the ELISpot predicted these from fewer
contacts tested.47 However, a high proportion of the children received
chemoprophylaxis which is likely to have resulted in the incidence rate
ratios being underestimated.
Hill et al. 48 followed up 2348 household contacts in the Gambia for
2 years. 11/649 ELISpot-positive individuals developed active disease
as compared with 14/843 TST-positive individuals; 10/1087 ELISpot
76
British Medical Bulletin 2010;93
Downloaded from http://bmb.oxfordjournals.org/ at Gadjah Mada University on December 4, 2014
Longitudinal data quantifying the prognostic value of IGRAs
for progression to active TB
British Medical Bulletin 2010;93
Table 1: Currently published studies that have evaluated the prognostic value of the IGRAs.
Study population
Aichelburg
HIV adults
Country
Austria
Number
Progression
Progression
Progression
IGRA
follow up
of
to ATB of
to ATB of
to ATB of
prognostic
(years)
incident
cases
IGRA
contacts
TST
(5 mm)
TST
(10 mm)
contacts
contacts
3/36 (8)
Not
Not done
Yes
Period of
1.6
IGRA used
QFT-G in-tube
IGRA positive
44/783
TST (5 mm)
31/42 (74)
TST (10 mm)
Not done
et al.50
reported
Household contacts:
adults
Germany
QFT-G in-tube
66/601 (11)
243/601 (40)
110/601 (18)
6/41 (15)
5/219 (2)
5/90 (6)
Yes
Bakir
Household contacts:
Turkey
1.3
ELISpot
381/908 (42)
550/908 (61)
462/908 (51)
15
11/381 (3)
12/550 (2)
6/462 (1)
Yes
et al.47
children
Hill et al.48
Household contacts:
children & adults
Gambia
ELISpot
649/1736 (37)
Not done
843/2230 (38)
26
11/649
(1.7%)
Not done
14/843 (1.7)
No
Doherty
Household contacts:
Ethiopia
ELISA (ESAT6
9/24 (38)
Not done
Not done
6/9 (67)
Not done
Not done
Yes
et al.49
adults
only)
Values in parenthesis represent percentage values.
77
A 100 year update on diagnosis of tuberculosis infection
Diel et al.46
Downloaded from http://bmb.oxfordjournals.org/ at Gadjah Mada University on December 4, 2014
A. Lalvani and M. Pareek
Summary of clinical data
As the evidence base for the performance of IGRAs expands, one can
conclude that both IGRAs are not confounded by BCG vaccination
and are therefore more specific than the TST in the diagnosis of LTBI.
In LTBI, both tests are more sensitive than the TST, with the ELISpot
having a higher sensitivity than the ELISA.24 In children, the ELISpot
seems to be superior to the TST whilst the sensitivity of the ELISA
appears to be comparable to the TST although the data are inconsistent. Whilst both tests are relatively robust in HIV infection, the
ELISpot seems to perform better than the ELISA with a higher sensitivity and a lower proportion of indeterminate results, particularly
when CD4 counts are low. In individuals with IMID undergoing
immunosuppressive therapy, the performance of the ELISpot and
ELISA seem to be equivalent.
Impact of IGRAs on public health policy
As the experience with IGRAs has increased, they have become an integral part of national guidelines that recommend their use in the diagnosis of LTBI. European guidelines advise that the IGRA should be used
in individuals with a positive TST to confirm the diagnosis of LTBI
and as a direct replacement for the TST in persons in whom TST is
unreliable, e.g. in those with suppressed cellular immunity (see
Fig. 1).52 Conversely, in the US and Japan, it is recommended that the
IGRAs should completely replace the TST as the standard investigation
for LTBI in all individuals.53
Economics have been an important determinant in the diverse final
recommendations framed by different countries. Although the IGRAs
78
British Medical Bulletin 2010;93
Downloaded from http://bmb.oxfordjournals.org/ at Gadjah Mada University on December 4, 2014
negative and 11/1387 TST negative contacts developed TB.48 The
investigators concluded that neither the TST nor the ELISpot was prognostic of subsequent progression to tuberculosis. The reason for the
lack of prognostic power of both TST and ELISpot in the African study
is unclear but may relate to the highly endemic setting, in which de
novo community transmission outside the household may account for a
significant proportion of cases of tuberculosis.51
Longitudinal, predictive, data from these studies provide the initial
evidence to support the use of IGRAs in targeting chemoprophylaxis
for recent IGRA-positive contacts. This is promising as it may potentially prevent a similar number of cases as when the TST is used but
requiring the treatment of fewer contacts.
A 100 year update on diagnosis of tuberculosis infection
are more expensive than the TST, health economic analyses have found
that they are cost-effective as they reduce the number of individuals
needing unnecessary chemoprophylaxis and monitoring whilst on drug
therapy.54,55 The United Kingdom National Institute of Health and
Clinical Excellence (NICE) economic analysis concluded that the
two-step TST and confirmatory IGRA approach would be the most
cost-effective model and this was the basis of the recommendations
made for the UK and most other European countries.52
One consequence of the European/Canadian recommendations is that
immunocompetent individuals who are TST negative but who may
have been IGRA positive may not be identified as having LTBI and
hence left untreated. In contrast, the US/Japanese guidelines may result
British Medical Bulletin 2010;93
79
Downloaded from http://bmb.oxfordjournals.org/ at Gadjah Mada University on December 4, 2014
Fig. 1 Algorithm of all possible outcomes resulting from parallel IGRA and TST testing.
A. Lalvani and M. Pareek
in overtreatment of individuals who are IGRA positive/TST negative as
the risk of progressing to active TB in this group is not known. This
highlights the importance of prospective data that will quantify the predictive value of a positive IGRA result and the prognosis of contacts
where the IGRA and TST results are discordant.
Future directions for T-cell based TB testing
Conclusions
IGRAs represent a new paradigm with the potential to supersede the
century old TST and, in the process, revolutionize the diagnosis, and
thereby targeted chemoprophylaxis, of LTBI. The evidence base supporting their use has expanded dramatically over the last few years
which has resulted in them becoming an important diagnostic tool in
low prevalence settings. However, guidelines vary between countries,
which is likely to reflect some underlying uncertainty about the prognostic value of a positive IGRA result. As a consequence there is an
urgent need for further large, longitudinal studies to explicitly define
the prognostic value of positive IGRA results for the development of
active TB disease, particularly in high-risk groups and subgroups with
discordant IGRA and TST results. Data of this type would provide
80
British Medical Bulletin 2010;93
Downloaded from http://bmb.oxfordjournals.org/ at Gadjah Mada University on December 4, 2014
IGRAs have revolutionized the diagnosis of LTBI but they remain a
dynamic work in progress with attendant advantages and limitations.
As a diagnostic tool, IGRAs are unable to differentiate between active
and latent TB. In addition, longitudinal studies during treatment of
active and TB and LTBI have shown that serial IGRA testing cannot be
used for treatment monitoring or as test of cure.2 However, simultaneous measurement of IL-2 and IFN-g secretion by M. tuberculosis
specific T-cells correlate with therapeutic response and may allow treatment monitoring and potentially test of cure.56
Studies are also exploring whether measuring alternative, downstream chemokines secreted by IFN-g-activated macrophages such as
inducible protein 10 (IP-10), in combination with IFN-g, may serve as
a more amplified readout than IFN-g alone thereby resulting in higher
sensitivity.57
Although the current IGRAs have superior diagnostic sensitivity than
the TST, research indicates that next-generation assays will have an
even higher sensitivity without compromising specificity. This will be
achieved by including additional, novel, antigens such as RV3879c (in
ELISpotPLUS)58 alongside ESAT-6 and CFP-10.
A 100 year update on diagnosis of tuberculosis infection
a clear mandate for basing treatment decisions for LTBI on IGRA
results.
Conflict of interest: Professor Lalvani is inventor for several patents
underpinning T-cell-based diagnosis. The Lalvani ELISpot was commercialized by an Oxford University spin-out company (T-SPOT.TB w,
Oxford Immunotec Ltd, Abingdon, UK) in which Oxford University
and Professor Lalvani have a minority share of equity.
AL is a Wellcome Senior Research Fellow in Clinical Science. MP is
undertaking a Medical Research Council Capacity Building Studentship.
References
1
2
3
4
5
6
7
10
11
12
British Medical Bulletin 2010;93
World Health Organisation (2008) Global Tuberculosis ControlSurveillance, Planning,
Financing. Geneva: WHO.
Lalvani A (2007) Diagnosing tuberculosis infection in the 21st century: new tools to tackle
an old enemy. Chest, 131, 18981906.
Dye C, Scheele S, Dolin P, Pathania V, Raviglione MC (1999) Consensus statement. Global
burden of tuberculosis: estimated incidence, prevalence, and mortality by country. WHO
Global Surveillance and Monitoring Project. JAMA, 282, 677686.
Cain KP, Benoit SR, Winston CA, Mac Kenzie WR (2008) Tuberculosis among foreign-born
persons in the United States. JAMA, 300, 405 412.
Comstock GW, Livesay VT, Woolpert SF (1974) The prognosis of a positive tuberculin reaction in childhood and adolescence. Am J Epidemiol, 99, 131138.
Richeldi L (2006) An update on the diagnosis of tuberculosis infection. Am J Respir Crit
Care Med, 174, 736 742.
Lalvani A, Pathan AA, McShane H et al. (2001) Rapid detection of Mycobacterium tuberculosis infection by enumeration of antigen-specific T cells. Am J Respir Crit Care Med, 163,
824828.
Mahairas GG, Sabo PJ, Hickey MJ, Singh DC, Stover CK (1996) Molecular analysis of
genetic differences between Mycobacterium bovis BCG and virulent M. bovis. J Bacteriol,
178, 1274 1282.
Harboe M, Oettinger T, Wiker HG, Rosenkrands I, Andersen P (1996) Evidence for occurrence of the ESAT-6 protein in Mycobacterium tuberculosis and virulent Mycobacterium
bovis and for its absence in Mycobacterium bovis BCG. Infect Immun, 64, 16 22.
Houk VN, Baker JH, Sorensen K, Kent DC (1968) The epidemiology of tuberculosis infection
in a closed environment. Arch Environ Health, 16, 26 35.
Lalvani A, Pathan AA, Durkan H et al. (2001) Enhanced contact tracing and spatial tracking
of Mycobacterium tuberculosis infection by enumeration of antigen-specific T cells. Lancet,
357, 20172021.
Ewer K, Deeks J, Alvarez L et al. (2003) Comparison of T-cell-based assay with tuberculin
skin test for diagnosis of Mycobacterium tuberculosis infection in a school tuberculosis outbreak. Lancet, 361, 11681173.
81
Downloaded from http://bmb.oxfordjournals.org/ at Gadjah Mada University on December 4, 2014
Funding
A. Lalvani and M. Pareek
82
British Medical Bulletin 2010;93
Downloaded from http://bmb.oxfordjournals.org/ at Gadjah Mada University on December 4, 2014
13 Dominguez J, Ruiz-Manzano J, De Souza-Galvao M et al. (2008) Comparison of two commercially available gamma interferon blood tests for immunodiagnosis of tuberculosis. Clin
Vaccine Immunol, 15, 168 171.
14 Soysal A, Millington KA, Bakir M et al. (2005) Effect of BCG vaccination on risk of
Mycobacterium tuberculosis infection in children with household tuberculosis contact: a prospective community-based study. Lancet, 366, 1443 1451.
15 Connell TG, Ritz N, Paxton GA, Buttery JP, Curtis N, Ranganathan SC (2008) A three-way
comparison of tuberculin skin testing, QuantiFERON-TB Gold and T-SPOT.TB in children.
PLoS ONE, 3, e2624.
16 Diel R, Loddenkemper R, Meywald-Walter K, Gottschalk R, Nienhaus A (2009)
Comparative performance of tuberculin skin test, QuantiFERON-TB-Gold in tube assay, and
T-Spot.TB test in contact investigations for tuberculosis. Chest, 135, 1010 1018.
17 Nicol MP, Davies M-A, Wood K et al. (2009) Comparison of T-SPOT.TB assay and tuberculin skin test for the evaluation of young children at high risk for tuberculosis in a community
setting. Pediatrics, 123, 38 43.
18 Chun JK, Kim CK, Kim HS et al. (2008) The role of a whole blood interferon-gamma assay
for the detection of latent tuberculosis infection in Bacille Calmette-Guerin vaccinated children. Diagn Microbiol Infect Dis, 62, 389394.
19 Okada K, Mao TE, Mori T et al. (2008) Performance of an interferon-gamma release assay
for diagnosing latent tuberculosis infection in children. Epidemiol Infect, 136, 11791187.
20 Nakaoka H, Lawson L, Squire SB et al. (2006) Risk for tuberculosis among children. Emerg
Infect Dis, 12, 13831388.
21 Connell TG, Curtis N, Ranganathan SC, Buttery JP (2006) Performance of a whole blood
interferon gamma assay for detecting latent infection with Mycobacterium tuberculosis in
children. Thorax, 61, 616620.
22 Tsiouris SJ, Austin J, Toro P et al. (2006) Results of a tuberculosis-specific IFN-gamma assay
in children at high risk for tuberculosis infection. Int J Tuberc Lung Dis, 10, 939 941.
23 Hill PC, Brookes RH, Adetifa IM et al. (2006) Comparison of enzyme-linked immunospot
assay and tuberculin skin test in healthy children exposed to Mycobacterium tuberculosis.
Pediatrics, 117, 1542 1548.
24 Pai M, Zwerling A, Menzies D (2008) Systematic review: T-cell-based assays for the diagnosis
of latent tuberculosis infection: an update. Ann Intern Med, 149, 177 184.
25 Lalvani A (2003) Spotting latent infection: the path to better tuberculosis control. Thorax,
58, 916 918.
26 Chapman AL, Munkanta M, Wilkinson KA et al. (2002) Rapid detection of active and latent
tuberculosis infection in HIV-positive individuals by enumeration of Mycobacterium
tuberculosis-specific T cells. AIDS, 16, 2285 2293.
27 Liebeschuetz S, Bamber S, Ewer K, Deeks J, Pathan AA, Lalvani A (2004) Diagnosis of tuberculosis in South African children with a T-cell-based assay: a prospective cohort study.
Lancet, 364, 2196 2203.
28 Mandalakas AM, Hesseling AC, Chegou NN et al. (2008) High level of discordant IGRA
results in HIV-infected adults and children. Int J Tuberc Lung Dis, 12, 417423.
29 Rangaka MX, Diwakar L, Seldon R et al. (2007) Clinical, Immunological, and epidemiological importance of antituberculosis T cell responses in HIV-infected Africans. Clin Infect Dis,
44, 16391646.
30 Stephan C, Wolf T, Goetsch U et al. (2008) Comparing QuantiFERON-tuberculosis gold,
T-SPOT tuberculosis and tuberculin skin test in HIV-infected individuals from a low prevalence tuberculosis country. AIDS, 22, 2471 2479.
31 Dheda K, Lalvani A, Miller RF et al. (2005) Performance of a T-cell-based diagnostic test for
tuberculosis infection in HIV-infected individuals is independent of CD4 cell count. AIDS,
19, 20382041.
32 Clark SA, Martin SL, Pozniak A et al. (2007) Tuberculosis antigen-specific immune responses
can be detected using enzyme-linked immunospot technology in human immunodeficiency
virus (HIV)-1 patients with advanced disease. Clin Exp Immunol, 150, 238244.
33 Raby E, Moyo M, Devendra A et al. (2008) The effects of HIV on the sensitivity of a whole
blood IFN-g release assay in Zambian adults with active tuberculosis. PLoS ONE, 3, e2489.
A 100 year update on diagnosis of tuberculosis infection
British Medical Bulletin 2010;93
83
Downloaded from http://bmb.oxfordjournals.org/ at Gadjah Mada University on December 4, 2014
34 Balcells ME, Perez CM, Chanqueo L et al. (2008) A comparative study of two different
methods for the detection of latent tuberculosis in HIV-positive individuals in Chile. Int J
Infect Dis, 12, 645 652.
35 Brock I, Ruhwald M, Lundgren B, Westh H, Mathiesen LR, Ravn P (2006) Latent tuberculosis in HIV positive, diagnosed by the M. tuberculosis specific interferon-gamma test. Respir
Res, 7, 56.
36 Luetkemeyer AF, Charlebois ED, Flores LL et al. (2007) Comparison of an
interferon-lcub;gammarcub; release assay with tuberculin skin testing in HIV-infected individuals. Am J Respir Crit Care Med, 175, 737742.
37 Matulis G, Juni P, Villiger PM, Gadola SD (2008) Detection of latent tuberculosis in immunosuppressed patients with autoimmune diseases: performance of a Mycobacterium tuberculosis antigen-specific interferon gamma assay. Ann Rheum Dis, 67, 84 90.
38 Ponce de Leon D, Acevedo-Vasquez E, Alvizuri S, Cucho M et al. (2008) Comparison of an
interferon-gamma assay with tuberculin skin testing for detection of tuberculosis (TB) infection in patients with rheumatoid arthritis in a TB-endemic population. J Rheumatol, 35,
776781.
39 Sellam J, Hamdi H, Roy C et al. (2007) Comparison of in vitro-specific blood tests with
tuberculin skin test for diagnosis of latent tuberculosis before anti-TNF therapy. Ann Rheum
Dis, 66, 16101615.
40 Bartalesi F, Vicidomini S, Goletti D et al. (2009) QuantiFERON-TB Gold and the TST are
both useful for latent tuberculosis infection screening in autoimmune diseases. Eur Respir J,
33, 586 593.
41 Martin J, Walsh C, Gibbs A et al. (2009) Comparison of interferon-lcub;gammarcub;-release
assays and conventional screening tests before tumour necrosis factor-lcub;alpharcub; blockade in patients with inflammatory arthritis. Ann Rheum Dis, ard.2008.101857.
42 Arend SM, Thijsen SF, Leyten EM et al. (2007) Comparison of two interferon-gamma assays
and tuberculin skin test for tracing tuberculosis contacts. Am J Respir Crit Care Med, 175,
618627.
43 Ferrara G, Losi M, DAmico R et al. (2006) Use in routine clinical practice of two commercial blood tests for diagnosis of infection with Mycobacterium tuberculosis: a prospective
study. Lancet, 367, 13281334.
44 Lee JY, Choi HJ, Park IN et al. (2006) Comparison of two commercial interferon-gamma
assays for diagnosing Mycobacterium tuberculosis infection. Eur Respir J, 28, 24 30.
45 Beffa P, Zellweger A, Janssens JP, Wrighton-Smith P, Zellweger JP (2008) Indeterminate test
results of T-SPOT.TB performed under routine field conditions. Eur Respir J, 31, 842846.
46 Diel R, Loddenkemper R, Meywald-Walter K, Niemann S, Nienhaus A (2008) Predictive
value of a whole blood IFN-gamma assay for the development of active tuberculosis disease
after recent infection with Mycobacterium tuberculosis. Am J Respir Crit Care Med, 177,
11641170.
47 Bakir M, Millington KA, Soysal A et al. (2008) Prognostic value of a T-cell-based, interferongamma biomarker in children with tuberculosis contact. Ann Intern Med, 149, 777787.
48 Hill PC, Jackson-Sillah DJ, Fox A et al. (2008) Incidence of tuberculosis and the predictive
value of ELISPOT and Mantoux tests in Gambian case contacts. PLoS ONE, 3, e1379.
49 Doherty TM, Demissie A, Olobo J et al. (2002) Immune responses to the Mycobacterium
tuberculosis-specific antigen ESAT-6 signal subclinical infection among contacts of tuberculosis patients. J Clin Microbiol, 40, 704706.
50 Aichelburg MC, Rieger A, Breitenecker F et al. (2009) Detection and prediction of active
tuberculosis disease by a whole-blood interferon-gamma release assay in HIV-1-infected individuals. Clin Infect Dis, 48, 954 962.
51 Verver S, Warren RM, Munch Z et al. (2004) Proportion of tuberculosis transmission that
takes place in households in a high-incidence area. Lancet, 363, 212 214.
52 National Collaborating Centre for Chronic Conditions (2006) Tuberculosis: clinical diagnosis
and management of tuberculosis, and measures for its prevention and control. London: Royal
College of Physicians.
53 Mazurek GH, Jereb J, Lobue P et al. (2005) Guidelines for using the QuantiFERON-TB
Gold test for detecting Mycobacterium tuberculosis infection, United States. MMWR
Recomm Rep, 54, 49 55.
A. Lalvani and M. Pareek
54 Diel
R,
Nienhaus
A,
Loddenkemper
R
(2007)
Cost-effectiveness
of
Interferon-lcub;gammarcub; release assay screening for latent tuberculosis infection treatment
in Germany. Chest, 131, 14241434.
55 Wrighton-Smith P, Zellweger JP (2006) Direct costs of three models for the screening of
latent tuberculosis infection. Eur Respir J, 28, 4550.
56 Lalvani A, Millington KA (2008) T cells and tuberculosis: beyond interferon-gamma. J Infect
Dis, 197, 941943.
57 Ruhwald M, Bodmer T, Maier C et al. (2008) Evaluating the potential of IP-10 and MCP-2
as biomarkers for the diagnosis of tuberculosis. Eur Respir J, 32, 16071615.
58 Dosanjh DP, Hinks TS, Innes JA et al. (2008) Improved diagnostic evaluation of suspected
tuberculosis. Ann Intern Med, 148, 325336.
Downloaded from http://bmb.oxfordjournals.org/ at Gadjah Mada University on December 4, 2014
84
British Medical Bulletin 2010;93
Você também pode gostar
- Guide To Infection Control in The HospitalDocumento16 páginasGuide To Infection Control in The HospitalpsikubAinda não há avaliações
- Analysis of Hepatitis in Murine Herpesvirus 68-Infected Mice Used As Epstein-Barr Virus Hepatitis ModelDocumento9 páginasAnalysis of Hepatitis in Murine Herpesvirus 68-Infected Mice Used As Epstein-Barr Virus Hepatitis ModelRahmiati LaoAinda não há avaliações
- Infection Prevention and Control Workbook Final Version Sept 2019 PDFDocumento113 páginasInfection Prevention and Control Workbook Final Version Sept 2019 PDFRahmiati LaoAinda não há avaliações
- CDC Policy Analytical FrameworkDocumento9 páginasCDC Policy Analytical FrameworkRahmiati LaoAinda não há avaliações
- Infection Prevention and Control (IPC) For COVID-19: 3 April 2020Documento89 páginasInfection Prevention and Control (IPC) For COVID-19: 3 April 2020Rahmiati LaoAinda não há avaliações
- File S1 Survey Questionnaire For Antibiotic Use and Antimicrobial ResistanceDocumento18 páginasFile S1 Survey Questionnaire For Antibiotic Use and Antimicrobial ResistancePitua IvaanAinda não há avaliações
- 16 Chapter 42 RabiesDocumento10 páginas16 Chapter 42 Rabiesbeny bungaAinda não há avaliações
- Contoh Antibiogram - Stanford Hospital & Clinics - AntibiogramDocumento2 páginasContoh Antibiogram - Stanford Hospital & Clinics - AntibiogramRahmiati LaoAinda não há avaliações
- File571 PDFDocumento65 páginasFile571 PDFSri KishoreAinda não há avaliações
- Zika Virus Pandemic A Human and Public Health CrisisDocumento3 páginasZika Virus Pandemic A Human and Public Health CrisisRahmiati LaoAinda não há avaliações
- 16 Chapter 42 RabiesDocumento10 páginas16 Chapter 42 Rabiesbeny bungaAinda não há avaliações
- HepatitisDocumento39 páginasHepatitisRahmiati LaoAinda não há avaliações
- Infection Control It S Everyone S Business PDFDocumento60 páginasInfection Control It S Everyone S Business PDFRahmiati LaoAinda não há avaliações
- Grant Manual 2016: Application GuideDocumento32 páginasGrant Manual 2016: Application GuidewibAinda não há avaliações
- Viruses 07 02857Documento22 páginasViruses 07 02857Rahmiati LaoAinda não há avaliações
- 02 Aseptic Technique May 2015 Version 1.01Documento10 páginas02 Aseptic Technique May 2015 Version 1.01Rahmiati LaoAinda não há avaliações
- 23 Appendix G Nutritional Status of Children NCHS StandardDocumento1 página23 Appendix G Nutritional Status of Children NCHS StandardRahmiati LaoAinda não há avaliações
- Eng PDFDocumento214 páginasEng PDFafriantoAinda não há avaliações
- 16 Chapter 42 RabiesDocumento10 páginas16 Chapter 42 Rabiesbeny bungaAinda não há avaliações
- Declining Malaria, Rising of Dengue and Zika Virus Insights PDFDocumento8 páginasDeclining Malaria, Rising of Dengue and Zika Virus Insights PDFRahmiati LaoAinda não há avaliações
- Modul TBDocumento3 páginasModul TBRahmiati LaoAinda não há avaliações
- OnCo VirusesDocumento33 páginasOnCo VirusesSwathi GururajAinda não há avaliações
- Sep14indonesia Inventory Studies GlaziouDocumento25 páginasSep14indonesia Inventory Studies GlaziouRahmiati LaoAinda não há avaliações
- Zika Virus History, Emergence, Biology, and Prospects For ControlDocumento12 páginasZika Virus History, Emergence, Biology, and Prospects For ControlRahmiati LaoAinda não há avaliações
- 26 M Leprae PDFDocumento32 páginas26 M Leprae PDFZigganDEJordanAinda não há avaliações
- 156 FullDocumento10 páginas156 FullRahmiati LaoAinda não há avaliações
- 147 Full PDFDocumento34 páginas147 Full PDFRahmiati LaoAinda não há avaliações
- Cholera Outbreak AssessmentDocumento26 páginasCholera Outbreak AssessmentRahmiati LaoAinda não há avaliações
- 2016 Article 1668Documento7 páginas2016 Article 1668Rahmiati LaoAinda não há avaliações
- Dengue and Dengue Haemorrhagic Fever: Implications of Host GeneticsDocumento12 páginasDengue and Dengue Haemorrhagic Fever: Implications of Host GeneticsRahmiati LaoAinda não há avaliações
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeNo EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeNota: 4 de 5 estrelas4/5 (5794)
- The Yellow House: A Memoir (2019 National Book Award Winner)No EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Nota: 4 de 5 estrelas4/5 (98)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceNo EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceNota: 4 de 5 estrelas4/5 (895)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersNo EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersNota: 4.5 de 5 estrelas4.5/5 (344)
- The Little Book of Hygge: Danish Secrets to Happy LivingNo EverandThe Little Book of Hygge: Danish Secrets to Happy LivingNota: 3.5 de 5 estrelas3.5/5 (399)
- The Emperor of All Maladies: A Biography of CancerNo EverandThe Emperor of All Maladies: A Biography of CancerNota: 4.5 de 5 estrelas4.5/5 (271)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaNo EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaNota: 4.5 de 5 estrelas4.5/5 (266)
- Never Split the Difference: Negotiating As If Your Life Depended On ItNo EverandNever Split the Difference: Negotiating As If Your Life Depended On ItNota: 4.5 de 5 estrelas4.5/5 (838)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryNo EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryNota: 3.5 de 5 estrelas3.5/5 (231)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureNo EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureNota: 4.5 de 5 estrelas4.5/5 (474)
- Team of Rivals: The Political Genius of Abraham LincolnNo EverandTeam of Rivals: The Political Genius of Abraham LincolnNota: 4.5 de 5 estrelas4.5/5 (234)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyNo EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyNota: 3.5 de 5 estrelas3.5/5 (2259)
- The Unwinding: An Inner History of the New AmericaNo EverandThe Unwinding: An Inner History of the New AmericaNota: 4 de 5 estrelas4/5 (45)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreNo EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreNota: 4 de 5 estrelas4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)No EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Nota: 4.5 de 5 estrelas4.5/5 (120)
- National Leprosy Eradication ProgrammeDocumento4 páginasNational Leprosy Eradication ProgrammeSaiyan VegetaAinda não há avaliações
- Gambaran Faktor-Faktor Yang Terkait Dengan Kinerja Petugas Dalam Penemuan Kasus Pada Program Tuberkulosis Paru Di Kabupaten GroboganDocumento10 páginasGambaran Faktor-Faktor Yang Terkait Dengan Kinerja Petugas Dalam Penemuan Kasus Pada Program Tuberkulosis Paru Di Kabupaten GroboganNurse AdhyAinda não há avaliações
- Pemeriksaan Bakteriologis Lab TBDocumento49 páginasPemeriksaan Bakteriologis Lab TBTugas HeinzAinda não há avaliações
- WHO Consolidated On Tuberculosis: GuidelinesDocumento134 páginasWHO Consolidated On Tuberculosis: GuidelinesRamesh Karki - SarozzAinda não há avaliações
- Clinical Microbiology Reviews-2018-Forbes-e00038-17.fullDocumento66 páginasClinical Microbiology Reviews-2018-Forbes-e00038-17.fullSharwan KumawatAinda não há avaliações
- Tuberculosis For Dec 1Documento23 páginasTuberculosis For Dec 1Tony Rose Reataza-BaylonAinda não há avaliações
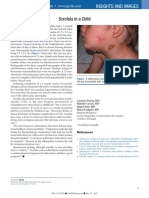
- Scrofula in A Child: Insights and ImagesDocumento1 páginaScrofula in A Child: Insights and Imagesmawarni siahaanAinda não há avaliações
- RNTCPDocumento24 páginasRNTCParunjv1234100% (1)
- PreventionDocumento1 páginaPreventionAshpreetAinda não há avaliações
- ELI AlgorithmDocumento40 páginasELI AlgorithmFitri Nurussani AuliaAinda não há avaliações
- Deteksi Mycobacterium Tuberculosis Pada Sampel Sputum Menggunakan Teknik Loop-Mediated Isothermal Amplification (LAMP-TB)Documento7 páginasDeteksi Mycobacterium Tuberculosis Pada Sampel Sputum Menggunakan Teknik Loop-Mediated Isothermal Amplification (LAMP-TB)Setiaty PandiaAinda não há avaliações
- The Paleopathology of Specific Infectious Diseases From Southeastern Hungary: A Brief OverviewDocumento6 páginasThe Paleopathology of Specific Infectious Diseases From Southeastern Hungary: A Brief OverviewLucía Chavarría RíosAinda não há avaliações
- Lad RefDocumento4 páginasLad RefnurulAinda não há avaliações
- Republic of The Philippines Province of Batangas Municipality of San JoseDocumento3 páginasRepublic of The Philippines Province of Batangas Municipality of San JoseSample BakeshopAinda não há avaliações
- Peran Pengawas Minum Obat (Pmo) Dalam Keberhasilan Pengobatan Tuberculosis Paru Di Masyarakat (The Role of Direct Observed Treatment in Tuberculosis Treatment Successful at Comm...Documento7 páginasPeran Pengawas Minum Obat (Pmo) Dalam Keberhasilan Pengobatan Tuberculosis Paru Di Masyarakat (The Role of Direct Observed Treatment in Tuberculosis Treatment Successful at Comm...petrayohanaAinda não há avaliações
- Skripsi KustaDocumento61 páginasSkripsi Kustaandre yuindartantoAinda não há avaliações
- Recent TB Treatment GuidelinesDocumento28 páginasRecent TB Treatment GuidelinesDr venkatesh jalluAinda não há avaliações
- English AssigmentDocumento15 páginasEnglish AssigmentDhimas YogaAinda não há avaliações
- Beli ObatDocumento54 páginasBeli ObatReynaldi AristaAinda não há avaliações
- BibliographyDocumento2 páginasBibliographyapi-197414643Ainda não há avaliações
- Kadar Asam Urat Pada Pasien Tuberkulosis Dengan Terapi Obat Anti Tuberkulosis (Oat) Di Puskesmas Cempaka Maret 2017Documento5 páginasKadar Asam Urat Pada Pasien Tuberkulosis Dengan Terapi Obat Anti Tuberkulosis (Oat) Di Puskesmas Cempaka Maret 2017Kimitshu Foreverma SakuraAinda não há avaliações
- Specific Information DPT Vaccine: This Vaccine Gives ProtectionDocumento1 páginaSpecific Information DPT Vaccine: This Vaccine Gives ProtectionHarish N VAinda não há avaliações
- Tuberculosis - Wikipedia, The Free EncyclopediaDocumento15 páginasTuberculosis - Wikipedia, The Free EncyclopediaitsmepranielAinda não há avaliações
- Proposal FiadetaDocumento4 páginasProposal Fiadetajose suni100% (1)
- National Immunization ScheduleDocumento3 páginasNational Immunization SchedulescribdscribdtestAinda não há avaliações
- TuberculosisDocumento187 páginasTuberculosisNgọc BảoAinda não há avaliações
- Baby Vaccination Price List & Schedule Chart in India - Indian Beauty HubDocumento2 páginasBaby Vaccination Price List & Schedule Chart in India - Indian Beauty HubsareenckAinda não há avaliações
- Jurnal Ilmiah Maksitek ISSN. 2655-4399 Vol. 5 No. 4 Desember 2020Documento6 páginasJurnal Ilmiah Maksitek ISSN. 2655-4399 Vol. 5 No. 4 Desember 2020MasithaAinda não há avaliações
- BY Dr. Tahmina AzharDocumento71 páginasBY Dr. Tahmina Azharscribdnotes123Ainda não há avaliações
- .PHEM Weekly Reporting Format - 1646640158000Documento17 páginas.PHEM Weekly Reporting Format - 1646640158000Getachew DemissieAinda não há avaliações