Escolar Documentos
Profissional Documentos
Cultura Documentos
Anal Fissure
Enviado por
Rae02Descrição original:
Direitos autorais
Formatos disponíveis
Compartilhar este documento
Compartilhar ou incorporar documento
Você considera este documento útil?
Este conteúdo é inapropriado?
Denunciar este documentoDireitos autorais:
Formatos disponíveis
Anal Fissure
Enviado por
Rae02Direitos autorais:
Formatos disponíveis
Hemorrhoids
• Hemorrhoids are vascular masses that protrude into the lumen of the lower rectum or perianal area.
• They result when increased intra-abdominal pressure causes engorgement in the vascular tissue lining the anal canal.
• Loosening of vessels from surrounding connective tissue occurs with protrusion or prolapse into the anal canal.
• There are two main types of hemorrhoids: external hemorrhoids appear outside the external sphincter, and internal
hemorrhoids appear above the internal sphincter.
• When blood within the hemorrhoids becomes clotted because of obstruction, the hemorrhoids are referred to as being
thrombosed.
• Predisposing factors include pregnancy, prolonged sitting or standing, straining stool, chronic constipation or diarrhea, anal
infection, rectal surgery or episiotomy, genetic predisposition, alcoholism, portal hypertension (cirrhosis), coughing, sneezing, or
vomiting, loss of muscle tone attributable to old age, and anal intercourse.
• Complications include hemorrhage, anemia, incontinence of stool, and strangulation.
• Hemorrhoids are the most common of a variety of anorectal disorders.
Assessment:
1. Pain (more so with external hemorrhoids), sensation of incomplete fecal evacuation, constipation, and anal itching. Sudden rectal
pain may occur if external hemorrhoids are thrombosed.
2. Bleeding may occur during defecation; bright red blood on stool caused by injury of mucosa covering hemorrhoid.
3. Visible and palpable masses at anal area.
Diagnostic Evaluation:
1. External examination with anoscope or proctoscope shows single or multiple hemorrhoids.
2. Barium edema or colonoscopy rules out more serious colonic lesions causing rectal bleeding such as polyps.
Therapeutic Interventions:
1. High-fiber diet to keep stools soft.
2. Warm sitz baths to ease pain and combat swelling.
3. Reduction of prolapsed external hemorrhoid manually.
Pharmacologic Interventions:
1. Stool softeners to keep stools soft and relieve symptoms.
2. Topical creams, suppositories or other preparation such as Anusol, Preparation H, and witch-hazel compresses to reduce itching
and provide comfort.
3. Oral analgesics may be needed.
Surgical Interventions:
1. Injection of sclerosing solutions to produce scar tissue and decrease prolapse is an
office procedure.
2. Cryodestruction (freezing) of hemorrhoids is an office procedure.
3. Surgery may be indicated in presence of prolonged bleeding, disabling pain,
intolerable itching, and general unrelieved discomfort.
Nursing Interventions:
1. After thrombosis or surgery, assist with frequent repositioning using pillow support for
comfort.
2. Provide analgesics, warm sitz baths, or warm compresses to reduce pain and
inflammation.
3. Apply witch-hazel dressing to perianal area or anal creams or suppositories, if ordered, to relieve discomfort.
4. Observe anal area postoperatively for drainage and bleeding.
5. Administer stool softener or laxative to assist with bowel movements soon after surgery, to reduce risk of stricture.
6. Teach anal hygiene and measures to control moisture to prevent itching.
7. Encourage the patient to exercise regularly, follow a high fiber diet, and have an adequate fluid intake (8 to 10 glasses per day) to
avoid straining and constipation, which predisposes to hemorrhoid formation.
8. Discourage regular use of laxatives; firm, soft stools dilate the anal canal and decrease stricture formation after surgery.
9. Tell patient to expect a foul-smelling discharge for 7 to 10 days after cryodestruction.
10. Determine the patient’s normal bowel habits and identify predisposing factors to educate patient about preventing recurrence of
symptoms.
What is an anal fissure?
An anal fissure is a tear in the lining of the lower rectum (anus) that causes pain during bowel movements. It is a common condition. Anal
fissures do not lead to more serious conditions.
Most anal fissures heal with home treatment after a few days or weeks (acute anal fissures). If you have an anal fissure that has not healed
after 6 weeks, it is considered a long-term problem (chronic). You may need to take medicine to help a chronic anal fissure heal. Surgery
may be necessary for fissures that do not heal with medicine.
Anal fissures affect people of all ages, particularly young and otherwise healthy people. They are equally common in men and women.
Sometimes an anal fissure and a hemorrhoid develop at the same time.
What causes an anal fissure?
Anal fissures are caused by injury (trauma) to the anal canal. Injury can happen if:
• You pass a large stool that stretches the anal canal.
• You are constipated and try to pass a hard stool.
• You have repeated diarrhea.
Childbirth can also cause trauma to the anal canal. During childbirth, some women develop anal fissures. Fissures can also be caused by
digital insertion (as during an examination), foreign body insertion, or anal intercourse.
Because many people get constipated or have diarrhea without getting anal fissures, many experts believe there is some other cause of
anal fissures. Some people may have excessive tension in the two muscular rings (sphincters) controlling the anus. The external anal
sphincter is under your conscious control. But the internal anal sphincter is not under your control. This muscle remains under pressure, or
tension, all of the time. A fissure may develop if the internal sphincter's resting pressure becomes too high, causing spasm and reducing
blood flow to the anus. This high resting pressure can also keep a fissure from healing.
In some cases, an anal fissure may be caused by Crohn's disease, an inflammatory bowel disease (IBD) that causes bloody diarrhea,
abdominal (belly) pain, fever, weight loss, and fissures or fistulas near the anus.
Crohn's disease is a form of inflammatory bowel disease that causes inflammation and ulcers that may affect the deepest layers of the
lining of the digestive tract. It can also cause abnormal openings or connections (fistulas) in the diseased intestine. Symptoms of Crohn's
disease include episodes of diarrhea, abdominal pain, fever, nausea, loss of appetite, and weight loss.
What are the symptoms?
An anal fissure causes a sharp, stinging, or burning pain during a bowel movement. The pain, which can be severe, may last for a few
hours.
Fissures may itch. They often bleed lightly or cause a yellowish discharge. You may see a small spot of bright red blood on toilet tissue or a
few drops in the toilet bowl. The blood is separate from the stool. Very dark, tarry stools or dark red blood mixed with stool indicates some
other condition, possibly inflammatory bowel disease (IBD) or colon cancer. You should contact a doctor if you have any bleeding with
bowel movements.
Sometimes an anal fissure may be a painless wound that won't heal and that bleeds intermittently but causes no other symptoms.
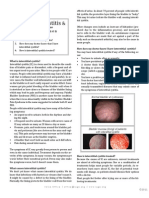
How is an anal fissure diagnosed?
Most doctors can diagnose an anal fissure from symptoms and by looking at the anus. Usually, the doctor can see the fissure by gently
separating the buttocks.
A doctor may use a gloved finger (digital rectal examination) or a lighted instrument (anoscope) to examine the fissure. But if the fissure is
extremely painful, the doctor will usually wait until it has begun to heal before performing a rectal exam or using an anoscope (anoscopy)
to rule out other problems. A topical anesthetic may be used if an immediate examination is necessary.
During an exam, a doctor can also find out whether another condition may be causing the fissure. If you have several fissures or have one
or more in an area of the anus where fissures usually do not occur, you may have another condition such as inflammatory bowel disease,
syphilis, a suppressed immune system, tuberculosis, HIV infection, or anal cancer. Most fissures occur along the midline—the top or bottom
—of the anus.
How is it treated?
Most acute fissures need some home treatment, including soaking in a shallow tub of warm water (sitz bath) 2 or 3 times a day, increasing
fiber in the diet, and taking stool softeners or laxatives. Some people find relief within a day or two of home treatment. Although your pain
may go away, it may take several weeks for the fissure to heal completely. Sometimes fissures heal without treatment.
Try to prevent constipation, because it can keep a fissure from healing. The pain of a fissure may make you anxious about having bowel
movements. But trying not to have bowel movements will only increase constipation and create a cycle that keeps the fissure open and
painful.
Drinking lots of water or other fluids also will make stools softer and easier to pass.
You may want to use a nonprescription ointment such as zinc oxide, Preparation H, Anusol, or 1% hydrocortisone to soothe anal tissues.
But evidence suggests that fiber and sitz baths help symptoms better than nonprescription creams.1 Talk with your doctor about whether
you should use these medicines for a short period of time.
If a fissure lasts a long time, prescription medicine may help. Prescription medicines used to treat anal fissure include nitroglycerin, high
blood pressure medicines, and botulinum toxin (Botox).
You may need to consider surgery if medicines do not stop your symptoms. The most commonly used surgery is lateral internal
sphincterotomy. In this procedure, a doctor cuts into part of the internal sphincter to relax the spasm that is causing the fissure.
Figure 1. Anoscope or proctoscope
Você também pode gostar
- A Simple Guide To Anal Disorders, Diagnosis, Treatment And Related ConditionsNo EverandA Simple Guide To Anal Disorders, Diagnosis, Treatment And Related ConditionsAinda não há avaliações
- Hemorrhoids (Piles) : Dr. Sahni BSDocumento7 páginasHemorrhoids (Piles) : Dr. Sahni BSavidmasterAinda não há avaliações
- Fissure SurgeryDocumento26 páginasFissure SurgerylenathorntonAinda não há avaliações
- A Simple Guide to Blood in Stools, Related Diseases and Use in Disease DiagnosisNo EverandA Simple Guide to Blood in Stools, Related Diseases and Use in Disease DiagnosisNota: 3 de 5 estrelas3/5 (1)
- Mixed Internal & External HemorrhoidsDocumento4 páginasMixed Internal & External HemorrhoidsHerne BalberdeAinda não há avaliações
- Hemorrhoids (Piles), A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo EverandHemorrhoids (Piles), A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsAinda não há avaliações
- DD Fissura AniDocumento7 páginasDD Fissura AniAnonymous LoQcj2xEAinda não há avaliações
- Natural Way To Get Rid Of Hemorrhoid In 2 Days: Practical Guide To How Anyone Can Completely Eliminate Hemorrhoid In 48 HoursNo EverandNatural Way To Get Rid Of Hemorrhoid In 2 Days: Practical Guide To How Anyone Can Completely Eliminate Hemorrhoid In 48 HoursNota: 3 de 5 estrelas3/5 (1)
- Diverticulitis Cure: The Ultimate Diverticulitis Diet: Diverticulitis Recipes: Your Ultimate Diverticulitis CookbookNo EverandDiverticulitis Cure: The Ultimate Diverticulitis Diet: Diverticulitis Recipes: Your Ultimate Diverticulitis CookbookAinda não há avaliações
- Fissure Treatment in MumbaiDocumento4 páginasFissure Treatment in MumbaiSambit ClinicAinda não há avaliações
- HemorrhoidsDocumento6 páginasHemorrhoidsfurqon hidayatullohAinda não há avaliações
- Anal Fissure, (Break in the Anus) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo EverandAnal Fissure, (Break in the Anus) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNota: 5 de 5 estrelas5/5 (5)
- Haemorrhoids: Natural Treatments That Really Work!No EverandHaemorrhoids: Natural Treatments That Really Work!Ainda não há avaliações
- The Hemorrhoids Handbook: Hemorrhoids Home Remedies | Hemorrhoids Causes, Symptoms, Therapy for Hemorrhoids no more | Hemorrhoids Pregnancy | Prevention, Diet | Hemorrhoids Bleeding TreatmentNo EverandThe Hemorrhoids Handbook: Hemorrhoids Home Remedies | Hemorrhoids Causes, Symptoms, Therapy for Hemorrhoids no more | Hemorrhoids Pregnancy | Prevention, Diet | Hemorrhoids Bleeding TreatmentAinda não há avaliações
- Treating Hemorrhoids: Using Non-Surgical MethodsDocumento14 páginasTreating Hemorrhoids: Using Non-Surgical MethodsRonald ReaganAinda não há avaliações
- Anal FissureDocumento3 páginasAnal FissureBhaveen ShethAinda não há avaliações
- Diverticulosis, A Simple Guide to the Condition, Treatment and Related DiseasesNo EverandDiverticulosis, A Simple Guide to the Condition, Treatment and Related DiseasesNota: 1 de 5 estrelas1/5 (1)
- Hemorrhoids - Causes, Treatments, and PreventionDocumento5 páginasHemorrhoids - Causes, Treatments, and PreventionSAIFUL ISLAMAinda não há avaliações
- Hemorrhoid: Hemorrhoids (Documento12 páginasHemorrhoid: Hemorrhoids (Dwika Putri MentariAinda não há avaliações
- GCSA HemorrhoidsDocumento3 páginasGCSA HemorrhoidsIka Niswatul ChamidahAinda não há avaliações
- Gastrointestinal DiseasesDocumento9 páginasGastrointestinal DiseasesJeraLdine HÜfanoAinda não há avaliações
- Your Health Choices: Signs, Causes and Treatment of PeritonitisDocumento11 páginasYour Health Choices: Signs, Causes and Treatment of PeritonitisAyu MegasariAinda não há avaliações
- Causes: Hemorrhoids (Documento14 páginasCauses: Hemorrhoids (Stephen S. PadayhagAinda não há avaliações
- 5960 1 Hartmanns ProcedureDocumento8 páginas5960 1 Hartmanns ProcedurecosmicdaeAinda não há avaliações
- A Simple Guide to Rectal Disorders, Diagnosis, Treatment and Related ConditionsNo EverandA Simple Guide to Rectal Disorders, Diagnosis, Treatment and Related ConditionsAinda não há avaliações
- Pathophysiology of Anorectal Disease: Presented By: Abegail TolerosoDocumento29 páginasPathophysiology of Anorectal Disease: Presented By: Abegail TolerosoAbby Gill TolerosoAinda não há avaliações
- Case Presentation - Catherine Uy DiazDocumento27 páginasCase Presentation - Catherine Uy DiazCatherine DiazAinda não há avaliações
- Gastrointestinal Bleeding, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo EverandGastrointestinal Bleeding, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsAinda não há avaliações
- Hemorrhoids and Anal ProblemsDocumento64 páginasHemorrhoids and Anal ProblemsAhmed Noureldin Ahmed100% (3)
- HemorrhoidsDocumento2 páginasHemorrhoidsadadanAinda não há avaliações
- 5960 1 Hartmanns ProcedureDocumento8 páginas5960 1 Hartmanns ProcedureZakiAinda não há avaliações
- Hemorrhoids DiseaseDocumento3 páginasHemorrhoids Diseaseto van quyenAinda não há avaliações
- Interstitial Cystitis & Painful Bladder Syndrome: A Guide For WomenDocumento2 páginasInterstitial Cystitis & Painful Bladder Syndrome: A Guide For Womencateterdoblejota100% (1)
- Clinical Study of Gastrointestinal System Diseases and Their MedicationsDocumento63 páginasClinical Study of Gastrointestinal System Diseases and Their MedicationsNajamAliAinda não há avaliações
- Diverticular Disease, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo EverandDiverticular Disease, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsAinda não há avaliações
- What Is A Cystoscopy?Documento3 páginasWhat Is A Cystoscopy?Harley Justiniani Dela Cruz100% (1)
- HemorrhoidsDocumento8 páginasHemorrhoidsArt Christian RamosAinda não há avaliações
- Peptic UlcerDocumento12 páginasPeptic UlcerhaddejAinda não há avaliações
- Peptic UlcerDocumento12 páginasPeptic UlcerhaddejAinda não há avaliações
- Peptic Ulcer Symptoms, Causes, Diagnosis and Treatment (40Documento12 páginasPeptic Ulcer Symptoms, Causes, Diagnosis and Treatment (40haddejAinda não há avaliações
- Lower Gastrointestinal Bleeding: Clinical Science SessionDocumento48 páginasLower Gastrointestinal Bleeding: Clinical Science SessionNissaa IslamiatiAinda não há avaliações
- Understanding Hemorrhoids: Causes, Symptoms, and TreatmentDocumento24 páginasUnderstanding Hemorrhoids: Causes, Symptoms, and TreatmentMonica SorianoAinda não há avaliações
- Polyp DKKDocumento45 páginasPolyp DKKNadya Beatrix Yohanna NapitupuluAinda não há avaliações
- Anal Fissure Guide: Causes, Symptoms and TreatmentsDocumento14 páginasAnal Fissure Guide: Causes, Symptoms and TreatmentsAnonymous LoQcj2xEAinda não há avaliações
- Fecal ImpactionDocumento5 páginasFecal Impactioncharie2Ainda não há avaliações
- Nursing Care Plan for Acute Pain and HemorrhoidsDocumento10 páginasNursing Care Plan for Acute Pain and HemorrhoidsFate Zephyr100% (2)
- Dyspepsia BrochureDocumento5 páginasDyspepsia BrochureJns RamAinda não há avaliações
- Hemoroid PW PointDocumento56 páginasHemoroid PW PointSalamahAinda não há avaliações
- Розлади трав. сист.Documento2 páginasРозлади трав. сист.Дария КоваленкоAinda não há avaliações
- AppendicitisDocumento6 páginasAppendicitisStephanie PeAinda não há avaliações
- Bahan Referat AppendicitisDocumento5 páginasBahan Referat AppendicitisMeidy WerorAinda não há avaliações
- Open Cholecystectomy Inpatient Care GuideDocumento7 páginasOpen Cholecystectomy Inpatient Care GuideMonique CastroAinda não há avaliações
- Gastric Outlet Obstruction, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo EverandGastric Outlet Obstruction, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsAinda não há avaliações
- Naturopathic Treatment of Anal FissureDocumento3 páginasNaturopathic Treatment of Anal FissureSorin VlaicuAinda não há avaliações
- Hemorrhoids: What Are Hemorrhoids? What Are The Symptoms of Hemorrhoids?Documento6 páginasHemorrhoids: What Are Hemorrhoids? What Are The Symptoms of Hemorrhoids?Devina NugrohoAinda não há avaliações
- HEMORRHOID (Case Study)Documento45 páginasHEMORRHOID (Case Study)enny92% (24)
- Ohio Prison Suicide ReportDocumento26 páginasOhio Prison Suicide ReportPBS NewsHourAinda não há avaliações
- Human Resources Manager or Human Resources Director or Sr. HR BuDocumento2 páginasHuman Resources Manager or Human Resources Director or Sr. HR Buapi-77982767Ainda não há avaliações
- The Lord of Lost Heart PDFDocumento44 páginasThe Lord of Lost Heart PDFCouteron LaurentAinda não há avaliações
- Unit 4 BacteriologyDocumento51 páginasUnit 4 BacteriologySharmila LamisharAinda não há avaliações
- People Pleasing Patterns Are Learned When Needs Are Not Met PDFDocumento10 páginasPeople Pleasing Patterns Are Learned When Needs Are Not Met PDFPamela RodriguezAinda não há avaliações
- Surya Namaskar BenefitsDocumento16 páginasSurya Namaskar BenefitsMillion Dollar KnowledgeAinda não há avaliações
- Managing Mental Health and Stress Online CourseDocumento2 páginasManaging Mental Health and Stress Online CourseDakota624Ainda não há avaliações
- Annual Report 2013-14Documento198 páginasAnnual Report 2013-14shahabAinda não há avaliações
- Slide PPT PrismaDocumento31 páginasSlide PPT PrismaUlul Azmi AdnanAinda não há avaliações
- Manuale Advantage 350Documento50 páginasManuale Advantage 350PaulmankeAinda não há avaliações
- Jordan Belliveau DocumentsDocumento2 páginasJordan Belliveau DocumentsLeigh Egan100% (1)
- Invega Sustenna PIDocumento13 páginasInvega Sustenna PIAisha SyedAinda não há avaliações
- Serial number verification formDocumento1 páginaSerial number verification formArjelyAinda não há avaliações
- MRNA Vaccines - Day - 04.14.20 PDFDocumento259 páginasMRNA Vaccines - Day - 04.14.20 PDFTammy G100% (1)
- Hematology Lecture - AnemiaDocumento10 páginasHematology Lecture - AnemiaKimberly EspaldonAinda não há avaliações
- LAS For Summative Assessment (Written Work Performance Task)Documento2 páginasLAS For Summative Assessment (Written Work Performance Task)Angel Dela CruzAinda não há avaliações
- Sport Science and Sports Medicine Framework 2017 v1Documento31 páginasSport Science and Sports Medicine Framework 2017 v1api-443327549Ainda não há avaliações
- Learning Kit - Q3W3 CeslDocumento10 páginasLearning Kit - Q3W3 CeslJoselle Batas MagbanuaAinda não há avaliações
- OD-PRO-HSE-032 Safety To Work at Height - Rev.01Documento31 páginasOD-PRO-HSE-032 Safety To Work at Height - Rev.01aymenmoataz100% (1)
- GRADE 5 - WEEK 6 Catch UpDocumento8 páginasGRADE 5 - WEEK 6 Catch Upbutchabdon1992Ainda não há avaliações
- Gene TherapyDocumento15 páginasGene TherapyRose Mary GeorgeAinda não há avaliações
- Single/ Exam Zone Centre DetailsDocumento5 páginasSingle/ Exam Zone Centre DetailsHarsh AroraAinda não há avaliações
- Summary of key provisions in the Domestic Workers ActDocumento46 páginasSummary of key provisions in the Domestic Workers ActPaul Christopher PinedaAinda não há avaliações
- Laparoscopic Appendectomy ReportDocumento1 páginaLaparoscopic Appendectomy ReportAjit AJAinda não há avaliações
- Nutrition Counseling And Dietary InstructionDocumento5 páginasNutrition Counseling And Dietary Instructionnicoleangela ubasroselloAinda não há avaliações
- Đề số 10Documento4 páginasĐề số 10Duong Nguyen Trieu100% (1)
- Edgar Allen Poe, The Tell-Tale HeartDocumento6 páginasEdgar Allen Poe, The Tell-Tale HeartAdinanCDAinda não há avaliações
- ImplantsDocumento11 páginasImplantsraheelAinda não há avaliações
- Cancer Lesson Plan For High SchoolDocumento7 páginasCancer Lesson Plan For High SchoolUm IbrahimAinda não há avaliações
- Commissioning Federal Facilities Chiller (PQ)Documento19 páginasCommissioning Federal Facilities Chiller (PQ)Yu-Chih PuAinda não há avaliações