Escolar Documentos
Profissional Documentos
Cultura Documentos
IJPsy 39 251
Enviado por
Diskta W RonicaTítulo original
Direitos autorais
Formatos disponíveis
Compartilhar este documento
Compartilhar ou incorporar documento
Você considera este documento útil?
Este conteúdo é inapropriado?
Denunciar este documentoDireitos autorais:
Formatos disponíveis
IJPsy 39 251
Enviado por
Diskta W RonicaDireitos autorais:
Formatos disponíveis
Indian J.
Psychiat, 1997, 39 (3), 251-255
INCREASED RISK OF OCCURRENCE OF NEUROLEPTIC MALIGNANT
SYNDROME ON COMBINED TREATMENT WITH
LITHIUM AND NEUROLEPTIC
P. JOHN ALEXANDER & RANJI MATHAI THOMAS
ABSTRACT
Whether there is an increased risk of occurrence of neuroleptic malignant syndrome (NMS)
on combined treatment with lithium and neuroleptic is a controversial issue. Patients seen in a
general psychiatry unit of a university hospital in India were prospectively screened for NMS over
a 2 year period. Diagnosis of NMS was made on operational criteria and the details of treatment at
the time of occurrence of NMS were collected systematically. Eight cases of NMS were identified
during the period of the study, out of which 5 (62.5%). were taking lithium and a neuroleptic together at the time of occurrence of NMS. The high prevalence of patients on lithium and
neuroleptic concomitantly in our sample of NMS, and the similar findings in many of the earlier
prospective studies, makes it possible to speculate whether there is an association between combined use of lithium and neuroleptic and occurrence of NMS. Findings are discussed.
Key words : NMS, lithium, neuroleptics
Neuroleptic malignant syndrome (NMS)
is a rare but potentially lethal condition,
estimated to occur in 0.02% to 3.23% of patients treated with neuroleptics (Addonizio &
Susman, 1991; Carrof & Mann, 1993). Though
a variety of risk factors like use of high
potency neuroleptics, rapid dose escalation,
administration of parenteral neuroleptics, use
of high dose of neuroleptics, organic brain
disorder, affective disorder, agitation etc. have
been reported to increase the risk of NMS,
consensus about aetiopathogenesis is elusive
(Levenson, 1985; Addonizio & Susman,'1991;
Carroff & Mann, 1993;).
The role of lithium (when used concurrently with neuroleptic) in increasing the risk of
NMS is a controversial issue. There are many
case reports of increased neurotoxicity and
NMS occurring with a combination of lithium
and neuroleptics, especially with haloperidol
(Cohen & Cohen, 1974; Loudon & Waring, 1976;
Spring & Frankel, 1991). Retrospective
analysis have found that upto 50% of patients
who developed NMS were on treatment with
lithium and neuroleptics at the time of
occurrence of NMS (Addibuzui et al., 1986;
Kecketal., 1989). Also, Kecketal. (1987) and
Rosebush & Stewart (1988) found on
prospective studies that 50% or more of
patients with NMS w,ere taking lithium along
with a neuroleptic when they developed NMS.
These authors found that NMS can occur when
lithium is used with neuroleptics other than haloperidol also. However, some retrospective
studies didn't find any evidence of neurotoxicity with concurrent use of lithium and neuroleptics (Baastrup et al., 1976; Goldney & Spence,
1986). A variety of methodological factors like
the retrospective design, imprecise diagnosis
of NMS, non-control of other variables etc. could
251
P. JOHN ALEXANDER & RANJI MATHAI THOMAS
have confounded the results of many studies.
In Indian literature there is a paucity of
reports on NMS (Thomas et al., 1993).
Epidemiological studies from various countries
have shown that bipolar disorder has an estimated life time risk of around 1 % (Goodwin &
Jamison, 1990). In view of the large population
of India and enormous number of patients exposed to this treatment combination of litium
and neuroleptic/s, we conducted a prospective
study about the association of combined us'e of
lithium and neuroleptic and the occurrence of
NMS.
MATERIAL & METHOD
All the cases seen at psychiatry unit of
Kasturba Hospital, Manipal from January 1994
to December 1995 were carefully assessed for
NMS. This psychiatry unit runs its outpatient
clinic three times a week and on these days
besides outdoor patients attending the section,
the unit also saw all the inpatient referrals from
other departments and the emergency calls.
This is a referral hospital, catering to a geographical area of two southern states of India.
The present report is a part of study to assess
the prevalence and risk factors for NMS.
The diagnosis of NMS was made when
patients exposed in the past 1 week to neuroleptic (4 weeks in case of depot neuroleptic preparation) had fever, rigidity, altered consciousness
and autonomic instability which couldn't be
accounted by any other physical or mental illness (Carroff et al., 1991). All the patients were
also seen by a consultant neurologist and appropriate investigations to rule out neurological
illness to account for these symptoms were
done. When clinically indicated, patients were
referred to other consultants and relevant
investigations tc rule out other physical disorders were carried out. Details of the drug treatment was collected from the close relative/s,
available prescriptions at the time of admission
and from the patients after they recovered from
the episode of NMS. Informed consent was
obtained from all the patients for the use of
clinical records.
RESULTS
Eight cases who met the operational
criteria of NMS were identified. The age, sex,
ICD-10 psychiatric diagnosis (WHO, 1992) and
details of drug treatment of the 8 patients are
shown in table . The age range of the patients
was from 21 to 63 years. Male and female were
equally present in the sample. Seven (87.5%)
of the patients were suffering from affective
disorder. Except one all the other patients were
on treatment from practising psychiatrists or
other doctors. A diagnosis of NMS as a
possibility was mentioned in only 2 of the
referrals by the treating doctor.
Out of the 8 patients, 5 were taking
lithium and a neuroleptic concomitantly when
they developed NMS. Serum lithium level was
within the therapeutic range in all the 5 patients
on lithium (range being 0.4 milliequivalents to
1.2 milliequivalents) which was done at
varying points of time (24 hours to 72 hours
after the last dose of lithium).
DISCUSSION
Our diagnosis of NMS was made on
operational criteria of Caroff et al. (1991) and
also met the research criteria proposed by
DSM-IV (APA, 1994). We have tried to exclude
by careful evaluation other systemic and neuropsychiatric illnesses producing the symptoms
of NMS. It has been observed that NMS be over
diagnosed if broad criteria are applied as other
medical causes may account for the symptoms
necessary for the diagnoses of NMS (Levinson
& Simpson, 1986).
It may be difficult in some cases to distinguish between lithium neurotoxicity and NMS,
since lithium in therapeutic range is known to
produce neurotoxicity (Schou, 1984). In some
patients there can be features of both lithium
toxicity and NMS (Cohen & Cohen, 1984). However, lithium toxicity is not usually associated
with fever and typically its neurotoxicity
252
LITHIUM AND NMS
manifests with weakness, extreme lethargy, cerebellar signs, fasciculations, myoclonic jerKS
and seizure (Schou, 1984; Sansone & Zeigler,
1985; Rosebush & Stewart, 1989). Thus, based
on the symptomatology, in most cases it is possible to distinguish lithium toxicity and NMS. It
is unlikely that any of our patient primarily had
lithium toxicity.
The findings of the present study is in
concordance with observations in literature that
a majority of patients who develop NMS are on
haloperidol. However, this may reflect prescribing practice rather than any specific risk for
haloperidol (Addonizio & Susman, 1991).
Lithium in combination with other neuroleptics
is also known to produce NMS (Addonizio &
Susman, 1991; Carroff & Mann, 1993).
Keck et al. (1987) found 6 cases of NMS,
3 were on lithium and neuroleptic. The authors
opined that lithium might have increased the
frequency of NMS. Similarly, Rosebush et al.
(1989) in their study found that lithium was
being used in 58% of those who developed
NMS, enabling them to raise the question of an
association between concomitant lithium and
neuroleptic use and development of NMS.
These findings make it possible to speculate
that there is an increased risk of occurrence of
NMS when patients are treated with a combination of lithium and antipsychotic/s.
A variety of ways of which lithium can
increase the risk of development of NMS have
been proposed (Rosebush et al., 1989; Addonizio & Susman, 1991). Lithium alone can
cause extrapyramidal (EPS) symptoms
(Shopsin & Gershon, 1975) and it is known that
it enhances the EPS produced by neuroleptics
(Addonizio, 1985). It may also increase the
TABLE
CHARACTERISTICS OF PATIENTS WITH NEUROLEPTC MALIGNANT SYNDROME
No.
Age
Sex
30
Unspecified nonorganic
psychosis (postpartum)
Chlorpromazine - 20mg
21
B A D . Currently Mania
Lithium 900 mg+
Thioridazine 100 mg
24
B.A.D. Currently Mania
Lithium 900 mg+
Haloperidol 15 mg
62
B.A.D. Currently Mania
Lithium 600 mg +
Haloperidol 5mg+
Carbamazepine 600 mg
55
B.A.D. Currently Mania
Lithium 600 mg +
Haloperidol 20 mg
63
B.A.D. Currently Mania
22
Severe
Depressive
(postpartum)
Episode
Amoxa pine 100 mg
26
Severe
Depressive
(postpartum)
Episode
Trifluperazine 20mg +
Chlopromazine 100 mg+
Trihexyphenidyl 4 mg
Psychiatric Diagnosis
B.A.D. Bipolar Affective Disorder
253
Medications Per Day
Lithium 900mg +
Haloperidol 50mg
P. JOHN ALEXANDER & RANJI MATHAI THOMAS
chance of a hypodopaminergic state and this is
implicated in the pathogenesis of NMS (Addonizio &Susman, 1991). Also, these drugs by
interaction may alter intercellular and serum
levels of both the drugs thereby increasing the
risk of NMS. Lithium toxicity can predispose to
the development of NMS by electrolyte
imbalance and renal dysfunction. Even in
nontoxic range lithium by inducing polyuria, can
produce fluid and electrolyte imbalance and
increase the risk for NMS (Addonizio &
Susman, 1991; Carroff & Mann, 1993).
Alternatively, it can be conceptualised
that lithium is likely to be used in
affective disorder and since these patients are
likely to get agitated and excited, all these factors are proposed risks for NMS, the association between lithium and NMS may be spurious. Retrospective studies have found that there
are significantly more patients with affective
disorders in NMS than in controls (Addonizio et
al., 1986; Keck etal., 1989). In the present study
also, 87.5% of patients were of affective
disorder.
However, it can't be concluded definitely
from our study that lithium neuroleptic
combination increases the risk of NMS. In
clinical practice these drugs are often used in
combination with no untoward effects. Two
retrospective studies (Baastrup et al., 1976;
Goldney & Spence, 1986) found no significant
risk of neurotoxicity or NMS with this
combination. Similarly, retrospective studies for
risk factors of NMS using control groups have
found no significantly increased use of lithium
in NMS patients compared to controls who didnt
develop NMS (Addonizio et al., 1986; Keck et
al., 1989). Deng et al. (1990) in a prospective
study of 7 years identified 12 cases of NMS
and found that only 1 was on lithium and thus
concluded that lithium is not a significant risk
factor for NMS.
The confounding effects of risk factor for
NMS need study using multivariate statistical
techniques. Unless large sample size are
collected using collaborative effort from
multiple centres, it may be difficult to precisely
pin point the risk factors for NMS, including that
of lithium.
REFERENCES
Addonizio, G. (1985) Rapid induction of extrapyramidal side effects with combined use of
lithium and neuroleptics. Journal of Clinical
Psychopharmacology, 5, 296-298.
Addonizio, G., Susman, V.L & Roth, S.D.
(1986) Symptoms of neuroleptic malignant syndrome in 82 consecutive inpatients. American
Journal of Psychiatry, 143, 1587-1590.
Addonizio, G. & Susman, V.L. (1991) Neuroleptic malignant syndrome. New York: Mosby year
Book Inc.
American Psychiatric Association (1994)
Diagnostic and statistical manual of mental
disorders. Fourth edition, Washington, DC.
Baastrup, P.C., Hollangel, P., Sorensen, R.
& Schou, M. (1976) Adverse reactions in treatment
with lithium carbonate and haloperidol. Journal of
American Medical Association, 236, 2645-2646.
Carroff, S.N. & Mann, S.C. (1993) Neuroleptic Malignant syndrome. Medical Clinics of North
America, 77, 185-202.
Carroff. S.N., Mann, S.C. & Lazarus, A.
(1991) Neuroleptic malignant syndrome: diagnostic issues. Psychiatric Annals 21, 130-147.
Cohen, W.J. & Cohen, N.H. (1974) Lithium
carbonate, haloperidol and irreversible brain
damage. Journal of American Medical Association,
230, 1283-1287.
Deng, M.Z., Chen, G.Q. & Phillips, M.R.
(1990) Neuroleptic malignant syndrome in 12 of 9,
792 Chinese inpatients exposed to neuroleptic: a
prospective study. American Journal of Psychiatry,
147, 1149-1155.
Goldney, R.D. & Spence, N.D. (1986) Safety
of the combination of lithium and neuroleptic drugs.
American Journal of Psychiatry, 143, 882-884.
254
Goodwin, F.K. & Jamison, K.R. (1990)
Manic Depressive Illness. New York : Oxford
University Press.
Keck, RE. Jr., Pope, H.G. Jr.; & McElroy,
LITHIUM AND NMS
S.L. (1987) Frequency and presentation of neuroleptic malignant syndrome: a prospective study.
American Journal of Psychiatry, 144, 1344-1346.
Lithium toxicity: a review of neurologic
complications. Clinical
Neuropharmacology,
8, 242-248.
Keck. P.E. Jr., Pope, H.E. Jr., Cohen, B.M.,
McElroy, S.L. & Neirenberg, A.A. (1989) Risk factors for neuroleptic malignant syndrome.
Archives of General Psychiatry, 46, 914-918.
Schou, M. (1984) Long-lasting neurological sequale after lithium intoxication. Acta
Psychiatrica Scandinavica, 70 594-602.
Shopsin, B. & Gershon, S. (1975) Cogwheel rigidity related to lithium maintenance.
American Journal of Psychiatry, 132, 536-538.
Levenson, J.L. (1985) Neuroleptic malignant syndrome. American Journal of Psychiatry, 142,
1137-1145.
Spring, G. & Frankel, M. (1981) New data
on lithium and haloperidol incompatibility.
American Journal of Psychiatry, 138, 818-821.
Levinson, D.F. & Simpson, G.M. (1986)
Neuroleptic induced extrapyramidal symptoms with
fever. Archives of General Psychiatry, 43, 839-848.
Thomas, K., Rajeev, K.K., Abraham, O.C.,
Sud, A. & Cherian, A.M. (1993) Management of
neuroleptic malignant syndrome- a series of 8 cases.
Journal of Association of Physicians of India, 41,
91-93.
Loudon, J.B. & Waring, H. (1976) Toxic reactions to lithium and haloperidol. Lancet, 11, 1088.
Rosebush, P. & Stewart, T. (1989) A prospective analysis of 25 episodes of neuroleptic malignant syndrome. American Journal of Psychiatry,
146, 717-725.
World Health Organisation (1992) The ICD10 classification of mental and behavioural disorders, clinical description and diagnostic guidelines,
Geneva: World Health Organisation.
Sansone, M.E. & Ziegler, D.K. (1985)
P JOHN ALEXANDER, M.D., Associate Professor, RANJI MATHAI THOMAS, M.B.B.S., Resident,
Psychiatry. Kasturba Medical College, Manipal 576 119, Kamataka.
'Correspondence
255
Department of
Você também pode gostar
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeNo EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeNota: 4 de 5 estrelas4/5 (5795)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreNo EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreNota: 4 de 5 estrelas4/5 (1090)
- Never Split the Difference: Negotiating As If Your Life Depended On ItNo EverandNever Split the Difference: Negotiating As If Your Life Depended On ItNota: 4.5 de 5 estrelas4.5/5 (838)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceNo EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceNota: 4 de 5 estrelas4/5 (895)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersNo EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersNota: 4.5 de 5 estrelas4.5/5 (345)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureNo EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureNota: 4.5 de 5 estrelas4.5/5 (474)
- The Emperor of All Maladies: A Biography of CancerNo EverandThe Emperor of All Maladies: A Biography of CancerNota: 4.5 de 5 estrelas4.5/5 (271)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)No EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Nota: 4.5 de 5 estrelas4.5/5 (121)
- The Little Book of Hygge: Danish Secrets to Happy LivingNo EverandThe Little Book of Hygge: Danish Secrets to Happy LivingNota: 3.5 de 5 estrelas3.5/5 (400)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyNo EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyNota: 3.5 de 5 estrelas3.5/5 (2259)
- The Yellow House: A Memoir (2019 National Book Award Winner)No EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Nota: 4 de 5 estrelas4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaNo EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaNota: 4.5 de 5 estrelas4.5/5 (266)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryNo EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryNota: 3.5 de 5 estrelas3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnNo EverandTeam of Rivals: The Political Genius of Abraham LincolnNota: 4.5 de 5 estrelas4.5/5 (234)
- The Unwinding: An Inner History of the New AmericaNo EverandThe Unwinding: An Inner History of the New AmericaNota: 4 de 5 estrelas4/5 (45)
- Battery Exam 2017 Level 4Documento202 páginasBattery Exam 2017 Level 4Mevelle Laranjo AsuncionAinda não há avaliações
- A Travel Medicine CaseDocumento65 páginasA Travel Medicine CaseDiskta W RonicaAinda não há avaliações
- Paediatrica Indonesiana: M. Sholeh Kosim, N.P. Noerpramana, Asril Aminullah, Suharyo HadisaputroDocumento6 páginasPaediatrica Indonesiana: M. Sholeh Kosim, N.P. Noerpramana, Asril Aminullah, Suharyo HadisaputroDiskta W RonicaAinda não há avaliações
- Catatonia, Neuroleptic Malignant Syndrome, and Cotard Syndrome in A 22-Year-Old Woman - A Case ReportDocumento3 páginasCatatonia, Neuroleptic Malignant Syndrome, and Cotard Syndrome in A 22-Year-Old Woman - A Case ReportDiskta W RonicaAinda não há avaliações
- Diagnosis of Scabies With DermosDocumento2 páginasDiagnosis of Scabies With DermosDiskta W RonicaAinda não há avaliações
- Diagnosis and Management of Gastroesophageal Reflux Disease (GERD) : An Indian PerspectiveDocumento8 páginasDiagnosis and Management of Gastroesophageal Reflux Disease (GERD) : An Indian PerspectiveDiskta W RonicaAinda não há avaliações
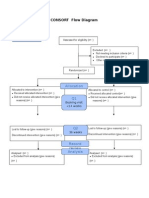
- Additional File 1: CONSORT Flow Diagram: EnrollmentDocumento1 páginaAdditional File 1: CONSORT Flow Diagram: EnrollmentDiskta W RonicaAinda não há avaliações
- Discharge Summary PDFDocumento2 páginasDischarge Summary PDFbalab2311Ainda não há avaliações
- Dental Practice ManagementDocumento5 páginasDental Practice ManagementTavi HeroiuAinda não há avaliações
- Euros Core OrgDocumento6 páginasEuros Core OrgClaudio Walter VidelaAinda não há avaliações
- TelemedicineDocumento39 páginasTelemedicineraju raj100% (1)
- Agencies WebsitesDocumento4 páginasAgencies WebsitesWWMTAinda não há avaliações
- Hemothorax HandoutsDocumento2 páginasHemothorax HandoutsJunathan L. DelgadoAinda não há avaliações
- Complex RestorationDocumento59 páginasComplex Restorationsamar yousif mohamed100% (1)
- Proximal Stripping PDFDocumento11 páginasProximal Stripping PDFsmilecarekkmAinda não há avaliações
- Bioethics Unit IiiDocumento4 páginasBioethics Unit IiiShannel J. DabalosAinda não há avaliações
- About Critical Care NursingDocumento7 páginasAbout Critical Care NursingaivynAinda não há avaliações
- Risk For InjuryDocumento3 páginasRisk For InjuryAvery SandsAinda não há avaliações
- Sebaceous CystDocumento6 páginasSebaceous CystGillarhymes100% (1)
- Critical Care PowerpointDocumento63 páginasCritical Care PowerpointtikoAinda não há avaliações
- Evaluation of Senior Nursing Students' Performance With High Fidelity SimulationDocumento4 páginasEvaluation of Senior Nursing Students' Performance With High Fidelity SimulationJessa BorreAinda não há avaliações
- Protocol - Aminoglycoside DosingDocumento5 páginasProtocol - Aminoglycoside DosingThomasAinda não há avaliações
- Emergency Trolly Lecture 2Documento28 páginasEmergency Trolly Lecture 2Eggy Pascual100% (1)
- Crit Care Nurse 2011 Grossbach 30 44Documento18 páginasCrit Care Nurse 2011 Grossbach 30 44Hanik FiriaAinda não há avaliações
- FNCP FormatDocumento12 páginasFNCP FormatChristi MilanAinda não há avaliações
- Reyes Vs Sisters of Mercy HospitalDocumento9 páginasReyes Vs Sisters of Mercy HospitalMico Maagma CarpioAinda não há avaliações
- 10-Effect of Chest Physical Therapy On Pediatrics Hospitalized With Pneumonia PDFDocumento8 páginas10-Effect of Chest Physical Therapy On Pediatrics Hospitalized With Pneumonia PDFandina100% (1)
- Necrotizing Facitis ReviewDocumento16 páginasNecrotizing Facitis ReviewHadi Firmansyah SidiqAinda não há avaliações
- Hazards of IV TherapyDocumento21 páginasHazards of IV TherapyFaraz Qurban RajperAinda não há avaliações
- ST LukesDocumento14 páginasST LukesJhe VersaceAinda não há avaliações
- Vitamin K Administration in The Newborn GuidelineDocumento10 páginasVitamin K Administration in The Newborn GuidelineAna Sarah KurniaAinda não há avaliações
- Antepartum Haemorrhage - Placenta Previa, Abruption 2Documento78 páginasAntepartum Haemorrhage - Placenta Previa, Abruption 2Sivakumar Kathuu KarthikeyanAinda não há avaliações
- Nursing InformaticsDocumento16 páginasNursing InformaticsSherina W. Edding100% (2)
- Cardio DrillDocumento24 páginasCardio DrillDemuel Dee L. BertoAinda não há avaliações
- 10 Rights in Drug AdministrationDocumento25 páginas10 Rights in Drug AdministrationNathaniel PulidoAinda não há avaliações
- The Nursing Diagnosis Body Image Disturbance Is Most Likely To Be Written For Which of The Following PersonsDocumento3 páginasThe Nursing Diagnosis Body Image Disturbance Is Most Likely To Be Written For Which of The Following PersonsenzoAinda não há avaliações