Escolar Documentos
Profissional Documentos
Cultura Documentos
009003
Enviado por
rulisakaroziDireitos autorais
Formatos disponíveis
Compartilhar este documento
Compartilhar ou incorporar documento
Você considera este documento útil?
Este conteúdo é inapropriado?
Denunciar este documentoDireitos autorais:
Formatos disponíveis
009003
Enviado por
rulisakaroziDireitos autorais:
Formatos disponíveis
4/28/2010
UPDATE & MANAGEMENT
OF
PEDIATRIC SEPTIC SHOCK
Abdul-Rahman Abu-Taleb, MD
Pediatric Intensivist
Chairman, Pediatric Department, KKNGH
KAMCR -Jeddah
INCIDENCE & MORTALITY RATE
Mortality has decreased from 97 % in the mid 60s
to 9% in children before 2002
(better than in adults 9% vs 28%)
Reported outcomes associated with implementation of the
best clinical practices MR 0%-5% in previously healthy
and 10% in chronically ill children
Crit Care Med 2009 Vol. 37, No.2
4/28/2010
INCIDENCE & MORTALITY RATE
Sepsis still is a major killer. It kills more people
than lung cancer, bowel and breast cancer put
together.
Cost over $30 billion.
billion
Br J Nurs. 2008 Jan 1010-23
23;;17(
17(1):16
):16--21
SURVIVING SEPSIS CAMPAIGN
Guidelines for Management of Severe Sepsis
and Septic Shock.
Reduce mortality rates
in severe sepsis
by 25 % in 5 years
Crit Care Med 2004 Vol.32.No.11 (suppl.)
4/28/2010
SURVIVING SEPSIS CAMPAIGN
Randomized clinical trails
in pediatric critical care
are rarely done but
desperately needed
SURVIVING SEPSIS CAMPAIGN
Evidence-based medicine (EBM) is an important strategy
for assessing the vast amount of published data and
applying them appropriately to our patients. However, in
pediatric intensive care, there is a shortage of "gold
standard therapy" randomized controlled trails (RCT) to
support "or not support" therapeutic decisions. This is
because, most of the therapies delivered to patients with
sepsis/severe sepsis and septic shock in the PICU are
life saving (e. g, IV antibiotics, vasopressor agents) and
could not ethically be put to the RCT test.
4/28/2010
Large well conducted RCT in 2001 & 2004 will have impact
on ICU practice
TV for
ALI
Anti-TNF
Antiin sepsis
Activated
protein C
St id
Steroids
in sepsis
Renal dose
dopamine
British Journal of Anesthesia. 2001 Sep; 87(3): 377
Anesth Analg, Volume 99(2). Aug; 2004.566-572
International pediatric sepsis consensus
conference 2005
The definitions for systemic inflammatory response
syndrome (SIRS), sepsis, severe sepsis, and septic
shock, in adults
were recently modified for children
Pediatr Crit Care Med 2005 Vol. 6, No. 1
4/28/2010
International pediatric sepsis consensus
conference 2005
Definitions for sepsis and organ
dysfunction in pediatrics
Brahm Goldstein, MD; Brett Giroir, MD; Adrienne Randolph, MD; and the
Members of the International Consensus Conference on Pediatric Sepsis
Pediatr Crit Care Med 2005 Vol. 6, No. 1
Definitions of SIRS, Infection, Sepsis, Severe Sepsis & Septic Shock
SIRS
(systemic inflammatory response syndrome)
The presence of at least two of the following four criteria, one of which
must be:
Abnormal temperature
or
Leukocyte count
Core temperature of > 38.5 C or < 36 C.
Tachycardia / Bradycardia.
Mean respiratory rate 2 SD above normal for age or mechanical
ventilation.
Leukocyte count elevated or depressed for age. Pediatr Crit Care Med 2005 Vol. 6, No. 1
4/28/2010
DEFINITION OF SEPSIS
Sepsis
SIRS in the presence of or as a
result of suspected or proven
infection.
Age-specific vital signs and laboratory variables
Age Group
Tachyc
Tachyc.
Bradyc
Bradyc.
Beats/min
RR
Breaths/min
Leukocyte C
Leucosytes x 103
>34
Sys
Sys. BP
mm HG
0 days to 1 wk
> 180
< 100
> 50
< 65
1 wk to 1 mo
> 180
< 100
> 40
>19.5 or < 5
< 75
1 mo to 1 yr
> 180
< 90
> 34
>17.5 or < 5
<100
5 yrs
y
25
> 140
0
NA
> 22
>15.5
5 5 or
o <6
< 94
9
612 yrs
> 130
NA
> 18
>13.5 or < 4.5
<105
13 to 18 yrs
> 110
NA
> 14
>11 or < 4.5
<117
Lower values for heart rate, leukocyte count, and systolic blood pressure are for the 5th
and upper values for heart rate, respiration rate, or leukocyte count for the 95th percentile.
Pediatr Crit Care Med 2005 Vol. 6, No. 1
4/28/2010
PEDIATRIC CONSIDERATIONS
Goal directed Endpoints in the management of sepsis are based on
evidence-based adult studies and the extrapolation to the pediatric
patient remains unvalidated.
1.
3.
5.
7.
8.
9.
10.
11.
12.
Mechanical Ventilation
2.
Fluid Resuscitation
Vasopressors / Inotropes
4.
Steroids
Blood/ and blood products
6.
Sedation / Analgesia
prophylaxis
p y
Stress ulcer p
Renal replacement therapy
Extracorporeal membrane oxygenation (ECMO)
Glycemic control
DVT
Protein C & activated protein C
Pediatr Crit Care Med 2005 Vol. 6, No. 1
MECHANICAL VENTILATION
Mechanical Ventilation:
Due to low functional residual capacity (FRC) in
neonates and young infants with severe sepsis early
intubation and mechanical ventilation may be required.
Lung protective strategies are applied to children as
th are tto adults.
they
d lt
Avoiding hyperoxemia in premature infants to prevent
retinopathy.
4/28/2010
MECHANICAL VENTILATION
Max O2
extraction
VO2
Max O2
extraction
VO2
Critical DO2
DO2
Normal
VO2 = DO2 x O2ER
Critical DO2
DO2
Septic Shock/ARDS
ScvO2 < 70%
70%
ScvO2 > 70%
70%
OXYGEN DELIVERY (DO
DO2)
OXYGEN CONSUMPTION (VO2)
OXYGEN EXTRACTION RATIO (O2ER)
INTIAL RESUSCITATION
The initial resuscitation of septic
patients is of utmost importance and
should start in the ED or wards prior
t ttransfer
to
f tto th
the PICU
PICU.
4/28/2010
Early Goal-Directed Therapy (EGDT) for Sepsis Induced
Hypoperfusion
Standard therapy N=133
EGDT N=130
Mortality %
60
P=0.009
50
40
30
56.9
49.2
46.5
44.3
35.1
30.5
20
10
0
In-hospital mortality
(all ptients)
28-day mortality
60-day mortality
Rivers E, et al. Early goal-directed therapy in the treatment of severe sepsis and septic shock. N Engl J Med 2001;
345:1368-1377
The new recommendation 2007 indicate
the following:
g
proportionally larger quantities of fluid than in
adult
first hour fluid resuscitation and inotrope therapy
directed to goals of threshold heart rates, normal
blood pressure, and capillary refill < 2 secs.
Crit Care Med 2009 Vol. 37, No.2
4/28/2010
FLUID RESUSCITATION DURING
INITIAL MANAGEMENT
Aggressive fluid resuscitation with boluses of 20 ml/kg
over 5-10 min
Initial resuscitation usually requires up to 60 ml/kg,
but more may be required
Blood pressure by itself is not a reliable endpoint for
resuscitation
Physical exam, urine output, and pulse response are
the primary response monitors.
HEMODYNAMIC SUPPORT
H
Hemodynamic
d
i profile
fil may be
b variable
i bl
1.
CO and
SVR
22%
2.
CO and
SVR
58%
3.
CO and
SVR
Vasopressors/Inotrops:
Shock
Ceneviva et al: Hemodynamic support in
fluid refractory pediatric septic shock.
Pediatrics 1998; 102:e19
Should only be used after appropriate volume Resuscitation.
Dopamine for hypotension
Epinephrine or norepinephrine for dopaminerefractory shock
Dobutamine for low cardiac output state
10
4/28/2010
HEMODYNAMIC SUPPORT
In cases were epinephrine-resistant low CO & high SVR shock is present
management should include as first-line therapy:
Nitrosovasodilators (nitroprusside & nitroglycerin)
When pat remain in a low CO & high SVR resistant state,
despite of epi. + nitros. therapy
use of
phosphodiesterase inhibitor (milrinone) should be
strongly considered.
MR 1985 vs 1998 was reduced from 58% down to 18% in fluid-refractory, dopamine
resistant septic shock since aggressive volume resuscitation & goal-directed therapy
(CI 3.3-6.0 L/min/m2) were applied.
HEMODYNAMIC SUPPORT
Catecholamine-resistant shock
Draw baseline cortisol level
At risk of adrenal insufficiency
Give hydrocortisone (50mg/kg)
Normal BP
Cold shock
CV O2 sat < 70 %
Add vasodilator or
type III PDE inhibitor
with volume loading
Not at risk
dont give hydrocortisone
Low BP
Cold shock
CV O2 sat < 70 %
Titrate volume
and
Epinephrine
Low BP
Warm shock
CV O2 sat 70 %
Titrate volume
and
Norepinephrine
11
4/28/2010
Hemodynamic support guidelines by ACCM/PALS
for pediatric septic shock with & without monitoring ScvO2
(End point 70%)
Parameter
n
28 days MR
Crystalloid (ml/kg)
Inotrops in first 6
hours
With
ScvO2
51
11.8%
28 (20-40)
(20 40)
Without
ScvO2
51
39.2%
5 (0-20)
(0 20)
29.4%
7.8%
P - Value
0.002
< 0.001
0 001
0.01
Resulted in significant & additive impact on the outcome.
Intensive Care Med. 2008 Jun;
Jun;34
34((6):991
):991--3.
Early and Late stage of septic shock
Early Stage (hyperdynamic)
Hyperthermia
Tachycardic
Tachypnea
Warm extremities
Bounding pulse
Normal capillary refill time
Hypertensive / Normotensive
Hypoxia
Polyuria
Increased cardiac output
Decreased SVR
Normal CNS
Respiratory alkalosis
Hyperglycemia
Normal coagulation
Late Stage (cardiogenic)
Hypothermia
Tachycardic
Bradypnea
Cold mottled extremities
Weak, thready pulse
Prolonged capillary refill time
Hypotensive
Hypoxia
Oliguria / anuria
Decreased cardiac output
Increased SVR
Obtunded, comatose
Metabolic acidosis
Hypoglycemia
Disseminated intravascular
coagulopathy (DIC)
12
4/28/2010
Historical informations and clinical signs in different shock forms
Cardiogenic
shock
Hypovolemic
shock
History:
Trauma, Vomiting
and /or Diarrhea
CHD, Cardiac surgery,
poor feeding and
respiratory distress
Distributive
shock
Fever, Lethargic,
poor skin color
and irritability
Clinical signs :
Increased
Increased
Increased
1 Heart size
1-
S ll
Small
Large
Small
2- Lungs
Clear
Wet
Clear
(in the early stage)
Gallop rhythm
Not present
Present
Not present
Capillary refill
Prolonged
Prolonged
Normal (in the early stage)
Heart rate
Chest x-ray :
time
Clinical practice parameters for hemodynamic support of pediatric and
neonatal septic shock
2007 update from the American College of Critical Care Medicine
The updated 2007 guidelines continue to recognize an increased
likelihood that children with septic shock, compared with adults, require:
proportionally larger quantities of fluid
inotrope and vasodilator therapies
hydrocortisone for absolute adrenal insufficiency
(ECMO for refractory shock).
The major new recommendation in the 2007 update is earlier use
of inotrope support through peripheral access until central
access is attained.
13
4/28/2010
Clinical practice parameters for hemodynamic support of pediatric and
neonatal septic shock
2007 update from the American College of Critical Care Medicine
CONCLUSIONS
1. first hour fluid resuscitation and inotrope therapy
directed to goals of threshold heart rates, normal blood
pressure, and capillary refill < 2 secs.
2. subsequent intensive care unit hemodynamic support
directed to goals of central venous oxygen saturation
>70% and cardiac index 3.36.0 L/min/m2
CONCLUSIONS
THERAPEUTIC ENDPOINTS
Physical exam findings indicating successful
resuscitation include:
Capillary refill < 2 sec
Warm extremities
N
Normal
l mental
t l status
t t
Urine output >1 ml/kg/hr
Central venous O2 sat 70 % (as in adult)
Normalization of lactate (more in adult)
14
4/28/2010
THANK YOU
HEMODYNAMIC SUPPORT
Inhaled NO useful in neonates with persistent
pulmonary hypertension (PPHN) and sepsis.
Pentoxifylline (an immunomodeliating agent)
improved outcome in premature neonates with sepsis
when
h given
i
for
f 6 hrs/day
h /d for
f 5 days
d
in
i a randomized
d i d
controlled trail.
15
4/28/2010
OTHER THERAPIES
Steroids: Recommended for children with catecholamine
resistant shock and suspected or proven adrenal insufficiency
(as in adults).
Activated protein C: Not studied adequately in pediatric
severe sepsis yet.
G M - C S F : Shown to be of benefit in neonates with sepsis
and neutropenia (unlike adults).
adults)
DVT: Most DVTs in young children are associated with CVL,
around 25% of children with a femoral CVL will develop DVT.
There are no data on use of heparin prophylaxis to prevent
DVT in children.
OTHER THERAPIES
Stress ulcer p
prophylaxis:
p y
Commonlyy used in mechanicallyy
ventilated children, usually with H2 blockers. No studies
analyzing the effect of stress ulcer prophylaxis in children.
Renal replacement therapy: Continuous venovenous
hemofiltration (CVVH) may be clinically useful in children with
anuria/severe oliguria and fluid overload, but no large RCTs
have been performed.
Glycemic control: There are no studies in pediatric patients
analyzing the effect of rigid glycemic control using insulin.
Sedation/Analgesia: Appropriate sedation and analgesia
for children who are mechanically ventilated is the standard
care, although there are no data supporting any particular
drugs or drug regimens.
16
4/28/2010
OTHER THERAPIES
Blood p
products: In the absence of data,, it is reasonable to
maintain Hb at 10 g/dl in children with severe sepsis and
septic shock.
Intravenous immunoglobulin (IVIG): Therapy with
monoclonal IVIGs in children remains experimental. All trails
have been small to support strong conclusion of benefit.
Extracorporeal membrane oxygenation (ECMO): May be
considered
id d in
i children
hild
with
ith refractory
f t
shock
h k or respiratory
i t
failure (not recommended in adults).
ECMO for refractory shock in children.
Pediatr Crit Care Med 2007 Vol. 8, No. 5
ECMO rescue for CPR in pediatric patient.
Crit Care Med 2008 Vol.36, No. 5
Crit Care Med 2009 Vol. 37, No.2
ECMO-CPR
Huang, et al Crit Care Med. 2008
In a retrospective study from the year 1999-2006.
Included all p
patients <18 yyears old how received ECMO during
g active
CPR.
17
4/28/2010
ECMO-CPR
Morris and Nadkarni reported 66 children who
were placed on ECMO during CPR over 7
years period
Median time of CPR prior to ECMO was 50
min
23/66 (35%) survived to hospital discharge
These children had a brief period of no flow
phase and excellent CPR during the low flow
phase
ECMO-CPR
How dose this ECMO-CPR experience relate to
post-resuscitation care?
Potential advantage of ECMO come from its
ability to maintain tight control of physiologic
parameters
t
after
ft resuscitation
it ti (e.g.
(
flow
fl
rate,
t
oxygenation, temperature control)
If not available may be we could imitate
ECMO goals by maintaining adequate SvO2?
18
4/28/2010
THANK YOU
19
Você também pode gostar
- Never Split the Difference: Negotiating As If Your Life Depended On ItNo EverandNever Split the Difference: Negotiating As If Your Life Depended On ItNota: 4.5 de 5 estrelas4.5/5 (838)
- Selektive MutismDocumento27 páginasSelektive MutismrulisakaroziAinda não há avaliações
- Current Treatment of Pediatric SepsisDocumento3 páginasCurrent Treatment of Pediatric SepsisrulisakaroziAinda não há avaliações
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeNo EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeNota: 4 de 5 estrelas4/5 (5794)
- Nejmcp0910236 BaruDocumento335 páginasNejmcp0910236 BarurulisakaroziAinda não há avaliações
- The Yellow House: A Memoir (2019 National Book Award Winner)No EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Nota: 4 de 5 estrelas4/5 (98)
- Substance Abuse Slides WebDocumento25 páginasSubstance Abuse Slides WebrulisakaroziAinda não há avaliações
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceNo EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceNota: 4 de 5 estrelas4/5 (894)
- Daftar Pustaka PDFDocumento6 páginasDaftar Pustaka PDFAditya Dwi PradiptaAinda não há avaliações
- The Little Book of Hygge: Danish Secrets to Happy LivingNo EverandThe Little Book of Hygge: Danish Secrets to Happy LivingNota: 3.5 de 5 estrelas3.5/5 (399)
- Hubungan Sanitasi Dan Budaya DNG Diare PDFDocumento7 páginasHubungan Sanitasi Dan Budaya DNG Diare PDFRiskha Febriani HapsariAinda não há avaliações
- Workshop in Pain Management 2015 FlyerDocumento2 páginasWorkshop in Pain Management 2015 FlyerrulisakaroziAinda não há avaliações
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureNo EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureNota: 4.5 de 5 estrelas4.5/5 (474)
- Children PsychiatryDocumento265 páginasChildren PsychiatryrulisakaroziAinda não há avaliações
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryNo EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryNota: 3.5 de 5 estrelas3.5/5 (231)
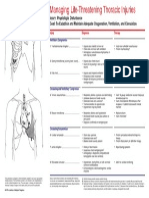
- Managing LT-Thoracic Injuries ACSDocumento1 páginaManaging LT-Thoracic Injuries ACSipsegAinda não há avaliações
- 10 Chest TraumaDocumento59 páginas10 Chest TraumarulisakaroziAinda não há avaliações
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaNo EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaNota: 4.5 de 5 estrelas4.5/5 (265)
- Pediatric Abdominal Emergencies: Loren G. Yamamoto, MD, MPH, MBA, FAAP, FACEPDocumento22 páginasPediatric Abdominal Emergencies: Loren G. Yamamoto, MD, MPH, MBA, FAAP, FACEPrulisakaroziAinda não há avaliações
- Nursing Grand Rounds Reviewer PDFDocumento17 páginasNursing Grand Rounds Reviewer PDFAlyssa Jade GolezAinda não há avaliações
- Demand For Beauty by Society (FINAL)Documento10 páginasDemand For Beauty by Society (FINAL)Maryhan MukhalalatiAinda não há avaliações
- The Emperor of All Maladies: A Biography of CancerNo EverandThe Emperor of All Maladies: A Biography of CancerNota: 4.5 de 5 estrelas4.5/5 (271)
- BarlingFrone 2004 ThePsychologyofWorkplaceSafteyDocumento336 páginasBarlingFrone 2004 ThePsychologyofWorkplaceSafteyfitrianiAinda não há avaliações
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersNo EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersNota: 4.5 de 5 estrelas4.5/5 (344)
- PhysioEx Exercise 4 Activity 2Documento3 páginasPhysioEx Exercise 4 Activity 2Milenka SalcedoAinda não há avaliações
- The Unwinding: An Inner History of the New AmericaNo EverandThe Unwinding: An Inner History of the New AmericaNota: 4 de 5 estrelas4/5 (45)
- Psychoeducation: 19 July 2018 Unit VI Topic DiscussionDocumento26 páginasPsychoeducation: 19 July 2018 Unit VI Topic DiscussionDana Franklin100% (1)
- Team of Rivals: The Political Genius of Abraham LincolnNo EverandTeam of Rivals: The Political Genius of Abraham LincolnNota: 4.5 de 5 estrelas4.5/5 (234)
- Anorexia Nerviosa y Trastornos Del Espectro Autista Investigacion Guiada de Endofenotipos Cognitivos SocialesDocumento31 páginasAnorexia Nerviosa y Trastornos Del Espectro Autista Investigacion Guiada de Endofenotipos Cognitivos SocialesCarito Hernandez RodriguezAinda não há avaliações
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyNo EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyNota: 3.5 de 5 estrelas3.5/5 (2219)
- Antibiotics Nursing ImplicationsDocumento4 páginasAntibiotics Nursing ImplicationsMichael Longs100% (1)
- EHAQ 4th Cycle Audit Tool Final Feb.10-2022Documento51 páginasEHAQ 4th Cycle Audit Tool Final Feb.10-2022Michael Gebreamlak100% (1)
- Sonuplus 492 Operator ManualDocumento72 páginasSonuplus 492 Operator ManualShoaib KhanAinda não há avaliações
- Atrium MedicalDocumento12 páginasAtrium MedicalBo TaoAinda não há avaliações
- Nephrotic Syndrome and Hypertension Nahla I. A L. Gabban Essam Ahmed Abdullah Haider Nadhim Abd FicmsDocumento6 páginasNephrotic Syndrome and Hypertension Nahla I. A L. Gabban Essam Ahmed Abdullah Haider Nadhim Abd FicmsMarcelita DuwiriAinda não há avaliações
- Fall Risk Factors and Fall Risk Assessment of InpatientsDocumento9 páginasFall Risk Factors and Fall Risk Assessment of Inpatientskang soon cheolAinda não há avaliações
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreNo EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreNota: 4 de 5 estrelas4/5 (1090)
- Brain Health Assessment by Dr. Daniel Amen #1 Brain Type QuizDocumento1 páginaBrain Health Assessment by Dr. Daniel Amen #1 Brain Type Quiz03.wizenedwasterAinda não há avaliações
- Tuberculosis and NutritionDocumento14 páginasTuberculosis and NutritionYenny PangaribuanAinda não há avaliações
- PPM Action Plan - 13 - 01 - 2022Documento128 páginasPPM Action Plan - 13 - 01 - 2022whoosh2008Ainda não há avaliações
- Article. Neoadjuvant Treatment Response As An Early Response Indicator For Patients With Rectal CancerDocumento7 páginasArticle. Neoadjuvant Treatment Response As An Early Response Indicator For Patients With Rectal CancerTrí Cương NguyễnAinda não há avaliações
- India Immunization Chart 2010Documento1 páginaIndia Immunization Chart 2010Sarath Nageshwaran SujathaAinda não há avaliações
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)No EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Nota: 4.5 de 5 estrelas4.5/5 (119)
- MEDUMAT Standard 2 83700-ENDocumento16 páginasMEDUMAT Standard 2 83700-ENJagath PrasangaAinda não há avaliações
- Option Volume Ventilation Pi 9066364 en 1506 3Documento2 páginasOption Volume Ventilation Pi 9066364 en 1506 3Abdullah AlsafiAinda não há avaliações
- Tugas Jurnal AppraisalDocumento2 páginasTugas Jurnal Appraisalshabrina nur imaninaAinda não há avaliações
- Lina Marulanda - Nursing Resume FinalDocumento2 páginasLina Marulanda - Nursing Resume Finalapi-490969182Ainda não há avaliações
- The Rubik's Cube Approach To Clinical MedicineDocumento2 páginasThe Rubik's Cube Approach To Clinical Medicinehenrygoldstein100% (1)
- Schedule FinalDocumento2 páginasSchedule Finalapi-360816970Ainda não há avaliações
- Petition To Remove James Wiley Conservator of The Estate of Henry C.MunozDocumento2 páginasPetition To Remove James Wiley Conservator of The Estate of Henry C.MunozpropertylenderAinda não há avaliações
- Medication Instructions Prior To SurgeryDocumento11 páginasMedication Instructions Prior To Surgeryhohj100% (1)
- Nursing Case Study - With Final Slides.Documento77 páginasNursing Case Study - With Final Slides.veejai_kumar100% (2)
- NycoCard Brochure 01Documento2 páginasNycoCard Brochure 01TimAinda não há avaliações
- Sports Injuries ManagementDocumento94 páginasSports Injuries ManagementSaha DirllahAinda não há avaliações
- Case Presentation Hepatitis A LuluDocumento28 páginasCase Presentation Hepatitis A LuluBrenda KarinaAinda não há avaliações
- Dialog Roleplay Bahasa Inggris: Disusun Oleh Kelompok 3Documento4 páginasDialog Roleplay Bahasa Inggris: Disusun Oleh Kelompok 3Desma LindaAinda não há avaliações