Escolar Documentos
Profissional Documentos
Cultura Documentos
142 531 1 PB
Enviado por
ayuandraniTítulo original
Direitos autorais
Formatos disponíveis
Compartilhar este documento
Compartilhar ou incorporar documento
Você considera este documento útil?
Este conteúdo é inapropriado?
Denunciar este documentoDireitos autorais:
Formatos disponíveis
142 531 1 PB
Enviado por
ayuandraniDireitos autorais:
Formatos disponíveis
Journal of Dentistry Indonesia 2012, Vol. 19, No.
1, 20-26
CASE REPORT
Biomechanics Strategies for Space Closure in Deep Overbite
Harryanto Wijaya, Isnani Jenie, Himawan Halim
Department of Orthodontics, Faculty of Dentistry, Trisakti University Jakarta 11440, Indonesia
Correspondence e-mail to: harryantowijaya@yahoo.com
ABSTRACT
Space closure is an interesting aspect of orthodontic treatment related to principles of biomechanics. It should be
tailored individually based on patients diagnosis and treatment plan. Understanding the space closure biomechanics
basis leads to achieve the desired treatment objective. Overbite deepening and losing posterior anchorage are the
two most common unwanted side effects in space closure. Conventionally, correction of overbite must be done
before space closure resulted in longer treatment. Application of proper space closure biomechanics strategies is
necessary to achieve the desired treatment outcome. This cases report aimed to show the space closure biomechanics
strategies that effectively control the overbite as well as posterior anchorage in deep overbite patients without
increasing treatment time. Two patients who presented with class II division 1 malocclusion were treated with fixed
orthodontic appliance. The primary strategies included extraction space closure on segmented arch that employed
two-step space closure, namely single canine retraction simultaneously with incisors intrusion followed by enmasse retraction of four incisors by using differential moment concept. These strategies successfully closed the
space, corrected deep overbite and controlled posterior anchorage simultaneously so that the treatment time was
shortened. Biomechanics strategies that utilized were effective to achieve the desired treatment outcome
ABSTRAK
Strategi biomekanika penutupan ruang pada tumpang gigit dalam. Penutupan ruang dalam perawatan ortodonti
merupakan aspek yang menarik berkenaan dengan prinsip-prinsip biomekanika. Dibuat khusus secara individu
berdasarkan diagnosis dan rencana perawatan. Pemahaman dasar-dasar biomekanika penutupan ruang akan
meningkatkan kemampuan operator untuk mencapai tujuan perawatan yang diinginkan. Efek samping yang paling
sering terjadi dalam penutupan ruang adalah bertambah dalamnya tumpang gigit dan hilangnya penjangkaran
posterior. Umumnya tumpang gigit dikoreksi sebelum penutupan ruang, sehingga waktu perawatan menjadi lebih
lama. Untuk mengatasi masalah-masalah tersebut, diperlukan penerapan strategi biomekanika penutupan ruang
yang tepat untuk memperoleh hasil perawatan yang sesuai harapan. Tujuan laporan kasus-kasus ini adalah untuk
menunjukkan penerapan strategi biomekanika yang efektif untuk mengontrol tumpang gigit dan penjangkaran
posterior pada pasien dengan tumpang gigit dalam, tanpa memperpanjang waktu perawatan. Dilaporkan dua kasus
maloklusi kelas II divisi 1 yang dilakukan perawatan alat ortodonti cekat. Strategi utama meliputi penutupan ruang
pencabutan di lengkung segmental dalam dua tahapan yaitu retraksi kaninus secara individu dengan intrusi insisivus
secara simultan, diikuti dengan retraksi empat insisivus dengan menggunakan konsep momen diferensial. Dengan
strategi ini, dapat dilakukan penutupan ruang, perbaikan tumpang gigit dalam, dan pengendalian penjangkaran
posterior dalam waktu bersamaan, sehingga diperlukan waktu perawatan yang lebih singkat. Strategi biomekanika
yang digunakan pada kasus-kasus ini efektif mencapai hasil perawatan yang diharapkan.
Keywords: anchorage, biomechanics, deep overbite, differential moment, intrusion, space closure
INTRODUCTION
closure have a tendency to generate detrimental effect particularly deepening the overbite and losing
the posterior anchorage. Deep overbite correction is
necessary to properly reduce overjet, especially in
class II division 1 extraction case. If the correction
During orthodontic treatment, closure of extraction
space in deep overbite patients is biomechanically
a difficult task. In many extraction cases, space
20
Journal of Dentistry Indonesia 2012, Vol. 19, No. 1, 20-26
of deep overbite is not considered during retraction
period, the palatal aspects of the maxilla incisors
could interfere with the mandibular incisor, causing
lingual tipping, loss of anchorage, and temporomandibular joint dysfunction. In growing individuals, it
is imperative to correct deep overbite to allow the
mandible to grow and develop normally.1 In most
orthodontic treatment for deep overbite extraction
case, correction of overbite must be done before
space closure and therefore, treatment time will be
longer.2
To control the deep overbite and posterior anchorage,
various methods have been proposed. Those methods
are ranged from traditional headgear to contemporary
TADs (Temporary Anchorage Devices) with their
shortcomings such as patient compliance; invasive
procedures; and additional treatment cost.1 The
biomechanics strategies that are presented in this
cases report will be used to overcome those problems.
The purpose of this cases report was to show the
space closure biomechanics strategies that effectively
control the deep overbite as well as posterior
anchorage in deep overbite extraction cases.
CASE OPERATION PROCEDURE 1
Diagnosis and etiology
Patient was an 11 years 3 months old girl with
forward position of her front teeth and unable to
close the lips when resting as her chief complaint.
Past and present medical history was negligible. The
conditions of dentition and other intra oral structure
were partially erupted lower second molars; adequate
periodontal health; amalgam filling on 16 and 26,
and no other past dental history. Upon examination,
temporomandibular joint revealed normal finding
with a normal range of motion and no joint sounds.
She had symmetrical mesofacial face and convex
facial profile. When resting, incisors display was
excessive and lips were strain upon closure. Facial
and upper dental midlines were coincided. The patient
was in early permanent dentition stage which molar
along with canine relationships were 75% class II in
both sides. Overjet was 8mm and deep overbite in
such case, the incisal edges of lower incisors nearly
impinge palatal mucosa. The lower dental midline
was shifted 2mm to the right. Moderate crowding
could be seen in the upper and lower arches (Figure
1). The pretreatment cephalometric analysis (Table 1)
revealed that the patient had a mild class II skeletal
pattern with slightly high mandible plane angle. Upper
incisors were protruded and proclined. Interincisal
and nasolabial angle were acute.
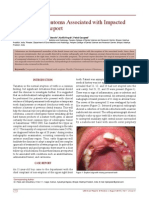
Figure 1. Pretreatment facial and intraoral photographs.
Facial photographs showed the view at rest, smile, and
lateral profile, respectively. Intraoral photographs showed the
condition of occlusion, dentition and other intra oral structure
Table 1. Pretreatment cephalometric measurement
Parameters
Norm -SD +SD
SNA (degree)
84.6 82.6 86.6
SNB (degree)
81.0 79.0 83.0
Facial angle (degree)
86.1 83.4 88.8
Convexity (mm)
4.80 2.80 6.80
Mandible Plane (degree)
25.0 20.7 29.3
Lower Incisors - A Pog (mm)
4.10 2.40 5.80
Lower Incisors A Pog (degree) 25.3 19.9 30.7
Upper Incisors A Pog (mm)
6.40 4.90 7.90
Upper Incisors A Pog (degree) 35.5 31.9 39.1
Interincisal (degree)
119.6 112.1 127.1
Nasolabial (degree)
98.5 85.2 111.8
Lower Lip - E Line (mm)
4.10 3.00 5.20
Upper Lip - E Line (mm)
3.20 1.60 4.80
Pretreatment
76.0
72.0
81.0
3.00
29.0
4.50
31.0
14.0
48.0
102.0
93.0
5.00
4.00
Lower and upper lips were protruded relative to esthetic
line. The patient had passed the peak of mandibular
growth period. Panoramic radiograph confirmed
that there was no pathology existed (Figure 2). This
malocclusion was diagnosed as class II division 1. The
suspected etiology was probably combination of genetic
and environment factors.
Treatment Objective
The treatment objectives were established to relieve
upper and lower arches crowding, relieve upper incisors
protrusion proclination, achieve adequate overbite and
overjet, maintain lower incisor inclination, achieve
adequate intercuspal relationship, and improve facial
esthetic.
21
Journal of Dentistry Indonesia 2012, Vol. 19, No. 1, 20-26
Treatment Plan
The treatment plans were determined as follows: (1) Removing upper first premolars; (2) Leveling and aligning
upper and lower dental arches; (3) Intruding the upper
incisors and simultaneously retracting the canines to
class I relationship on three-piece segmented arch;
(4) Retracting the previously intruded upper incisors
in group A anchorage by using differential moment
concept; (5) Coordinating upper and lower arches;
(6) Retention to achieve stabilization of the treatment
result. The 0.018 slot preadjusted appliance with Roths
prescription (Minisprint, Forestadent, Pforzheim, Germany) and molar bands with auxiliary tube were used.
Treatment Progress
After upper first premolars had been extracted, leveling
and aligning were started by using 0.014 and 0.016
martensitic active nickel titanium archwire (Copper
Ni-Ti, Ormco, Glendora, Calif) to relieve crowding.
When alignment had been achieved in the upper arch,
three-piece segmented arch (0.016 x 0.022 stainless
steel; Stainless Steel, Ortho Organizer, Carslbad, Calif)
was put on posterior and anterior segment, and then the
upper canines were retracted to class I position. Simultaneously, an intrusion arch (0.016 x 0.022 titanium;
CNA Beta III, Ortho Organizer, Carslbad, Calif) was
included to intrude the four incisors and control posterior
anchorage by tipping molar distally (Figure 3).
In lower arch, leveling and aligning were continued
until full sized (0.016 x 0.022 stainless steel)
archwire could be inserted. Once the upper canines
had been retracted completely, the anterior segment
was retracted by applying differential moment concept.
In this step, titanium continous archwire (0.016 x
0.022) with preactivated, off-centered position, and
gable bent T-loop was utilized (Figure 4). When the
space had already been closed, the finishing phase
would be started. This phase of treatment involved
use of coordinated 0.017 x 0.025 titanium wire.
Intermaxillary elastics were used for coinciding
the midline and settling the occlusion. Minor bends
were placed in these titanium wires for finishing
details. Retention consisted of an upper and lower
circumferential retainer.
Figure 2. Pretreatment panoramic radiograph. No pathology
condition was found
Treatment Result
Crowding in upper and lower dental arch were
relieved. Upper incisors had normal inclination and
position. Canine relationship was class I with 100%
class II molar relationship on both sides. Intercuspal
relationship was settled with adequate overjet and
overbite. The upper and lower dental midlines were
coincided with the facial midline. The upper and lower
arch form were ovoid and symmetric. Facial profile
was improved significantly. Lips strain and excessive
incisal display were disappearing when resting (Figure
5). Posttreatment cephalometric measurement (Table
2) showed some positive changes when compare
to pretreatment measurement. The superimposed
cephalograph tracing illustrates the changes associated
with treatment and growth (Figure 6).
Figure 3. Canine retraction stage. Upper arch: Three-piece
segmented and intrusion arch were used to simultaneously
intrude incisors and enhance posterior anchorage during
canine retraction. The intrusion arch was tied at the distal
wing of the lateral incisor bracket to allow the line of force
passes through the incisors center of resistance. Lower arch:
Continued leveling and aligning with full sized archwire
Overall superimposition showed that there was forward
and particularly downward growth for upper and lower
jaws. Nose and chin soft tissue also showed growth
vector in the same direction. Maxillary superimposition
showed upper incisors were retracted in control tipping
movement approximately 13 degrees. Maxillary
first molars moved forward in translation manner
and downward approximately 2 mm and 1.5 mm,
respectively. Nose and chin soft tissue also showed
growth vector in the same direction.
Figure 4. Four incisors retraction stage. T- loop was used to
retract four incisors on upper arch. The loops which directly
engaged to the molar auxiliary tube bypassing the second
premolars were preactivated, off-centered and gable bent
on distal of T- loop to create differential moments effect. In
the lower arch full sized stainless steel archwire was used
22
Journal of Dentistry Indonesia 2012, Vol. 19, No. 1, 20-26
Mandibular molars and lower incisor were seen moved
upward 2 mm and 3 mm in that order. Mandibular
condyles were grown about 6 mm. Anterior rotation
of maxillary and posterior rotation of mandibular were
seen. At the end of treatment, panoramic radiograph
showed adequate root parallelism and no sign of root
resorption.
CASE OPERATION PROCEDURE 2
Figure 5. Posttreatment facial and intraoral photographs.
After treatment facial and intraoral photographs showed
significantly improvement changes
Figure 6. Overall and regional superimposition. Superimposition of pretreatment (black solid line) and posttreatment
(red dash line) cephalograph tracings illustrated the changes
associated with treatment and growth
Table 2. Comparison of cephalometric measurement between
pre and posttreatment
Pretreatment
SNA (degree)
76.0
SNB (degree)
72.0
Facial angle (degree)
81.0
Convexity (mm)
3.0
Mandible Plane (degree)
29.0
Lower Incisors - A Pog (mm)
4.5
Lower Incisors A Pog
31.0
(degree)
Upper Incisors A Pog (mm)
14.0
Upper Incisors A Pog
48.0
(degree)
Interincisal (degree)
102.0
Nasolabial (degree)
93.0
Lower Lip - E Line (mm)
5.0
Upper Lip - E Line (mm)
4.0
Parameters
Posttreatment
76.0
72.0
83.0
3.0
32.0
6.0
34.0
8.0
35.0
112.0
102.0
2.0
0.0
Diagnosis and Etiology
The patient was a boy, 14 years 6 months old at the
time of consultation. His main complaint was forward
position of her front teeth. He was in good health and
no relavant medical history. The conditions of dentition
and other intra oral structure were central upper diastema, healthy periodontal status with an adequate band
of attached gingival, all permanent teeth were present
except for third molars. He had experienced of upper
right central incisor trauma that causing crown fracture.
The temporomandibular joints were clinically normal.
The facial photographs showed a symmetrical
dolichofacial face, convex facial profile with marked lip
protrusion and an everted upper and lower lips Facial
and upper dental midlines were coincided. Molars and
canines relationship were 50 % class II on both sides.
Overjet was 12.5 mm with an impinging deep overbite.
The lower dental midline was shifted to the left 2 mm.
Moderate to severe crowding could be seen in lower arch
(Figure 7). patient had a mild class II skeletal pattern
with the Cephalometric analysis (Table 3) revealed that
the slightly high mandible plane angle. Upper incisors
were protruded and proclined. Nasolabial angle were
acute. Lower and upper lips were protruded relative
to E-line. The patient had passed the peak of growth
period. Panoramic radiograph confirmed that there was
no pathology existed (Figure 8). This patient can also be
classified as class II division 1 malocclusion. Persistent
sucking habit until the age of eight was suspected as
the etiology of his malocclusion.
Treatment Objective
The treatment objectives were established to relieve
upper incisors protrusion and proclination, achieve
adequate overbite and overjet, relieve lower arch
crowding, achieve adequate intercuspal relationship,
and improve facial esthetics.
Treatment Plan
The treatment were planned as follows: (1) Removing
upper and lower first bicuspids; (2) Leveling and
aligning upper and lower dental arch; (3) Intruding the
upper incisors and simultaneously retracting the canines
to class I relationship on three-piece segmented arch;
(4) Retracting the previously intruded upper incisors
in group A anchorage by using differential moment
concept; (5) Closing the extraction space on lower
arch in group B anchorage; (6) Coordinating upper
23
Journal of Dentistry Indonesia 2012, Vol. 19, No. 1, 20-26
aligning. In the mandibular arch, 0.012 austenitic
active nickel titanium archwire (BioStarter, Forestadent,
Pforzheim, Germany) was employed to unravel. In the
canine retraction stage, for upper arch, three-piece
segmented arch (0.016 x .022 stainless steel; Stainless
Steel, Ortho Organizer, Carslbad, Calif) was put on
buccal and anterior segment and an intrusion arch (0.016
x 0.022 titanium; CNA Beta III, Ortho Organizer,
Carslbad, Calif) was included to intrude the four incisors
as well as to enhance posterior anchorage (Figure 9).
Canine retraction in lower arch was performed to relieve
anterior crowding. Once the upper canines had been
distalized completely and the class I relationship with
lower canines had been achieved, the anterior retraction
phase would be started. Differential moment concept
was applied in the upper arch as part of space closure
strategies to attain group A anchorage.
Figure 7. Pretreatment facial and intraoral photographs.
Photographs before treatment showed the severity of
malocclusion with the impact on facial appearance
The remaining space in lower arch was closed by utilizing sliding mechanics on 0.016 x 0.022 stainles steel
archwire (Figure 10). After retraction, the coordinated
finishing archwires (0.017 x 0.025 titanium) with
detailing bending were used in upper and lower arch.
Retention was provided by maxillary and mandibular
circumferential retainer.
Figure 8. Pretreatment panoramic radiograph. This
radiograph confirmed adequate condition of dentition and
periodontal tissue for orthodontic treatment
Treatment Result
Following treatment, the teeth were aligned. A class I
molar and canine relationship with coincident midlines,
proper interdigitation, adequate overjet and overbite were
also obtained. The post-treatment facial photographs
showed distinctly improvement of facial esthetics since
significant dental protrusion was corrected (Figure 11).
Table 3. Pretreatment cephalometric measurement
Parameters
Norm -SD +SD
SNA (degree)
84.6
SNB (degree)
81.0
Facial angle (degree)
87.8
Convexity (mm)
3.8
Mandible Plane (degree)
25.0
Lower Incisors - A Pog (mm) 3.0
Lower Incisors A Pog
23.2
(degree)
Upper Incisors A Pog (mm) 5.5
Upper Incisors A Pog
34.9
(degree)
Interincisal (degree)
121.9
Nasolabial (degree)
100.6
Lower Lip - E Line (mm)
1.6
Upper Lip - E Line (mm)
3.0
82.6
79.0
85.2
0.9
20.6
0.7
19.1
Pretreatment
86.6
82.5
83.0
75.0
90.4
86.5
6.7
8.5
29.4
31.0
5.3
4.5
27.3
25.0
3.5 7.5
30.5 39.3
15.0
49.0
114.5 129.3
87.0 114.2
-2.1 5.2
1.4 4.6
106.5
97.0
9.0
8.0
The superimposed cephalometric tracing illustrates
the changes achieved with treatment and growth process (Figure 12). Overall superimposition showed that
there was slightly downward growth of upper jaw; significantly forward and downward growth of lower jaw.
Nose and chin soft tissue also showed growth vector
in forward and downward direction. Maxillary superimposition showed that upper and lower incisors were
retracted in bodily movement approximately 7 mm and 2
mm, respectively. Maxillary incisors were also intruded
about 2 mm.
Posttreatment cephalometric measurement (Table 4)
confirmed the changes due to treatment effect as well
as remaining growth when compare to pretreatment
measurement. Maxillary first molars moved forward
and downward approximately 1 mm and 1.5 mm,
respectively. Mandibular first molars were seen moved
forward and upward approximately 3 mm and 2 mm,
respectively. Mandibular condyles were grown about 5
mm. Maxillary rotation were seen in anterior direction
and no significantly posterior rotation of mandibular.
Prior to debonding panoramic radiograph showed no
sign of root resorption. However, minor adjustment of
root position was needed.
and lower arches; (7) Retention to achieve stabilization
of the treatment result. The Roths prescription 0.018
slot preadjusted appliance (Minisprint, Forestadent,
Pforzheim, Germany) and molar bands with auxiliary
tube were used.
Treatment Progress
Extraction of four bicuspids had done before appliance
were placed. An initial 0.016 martensitic active nickel
titanium archwire (Copper Ni-Ti, Ormco, Glendora,
Calif) was placed in the maxillar arch for leveling and
24
Journal of Dentistry Indonesia 2012, Vol. 19, No. 1, 20-26
Figure 9. Canine retraction stage. In upper arch, three-piece
segmented arch in conjunction with intrusion arch was
used in canine retraction stage. In lower arch, canines were
distalized to alleviate anterior crowding
Figure 10. Differential moment concept in incisors retraction
stage. This concept was applied in upper arch to retract
four incisors for achieving group A anchorage. With this
concept, the proper force system is created. Four incisors
will be intruded and retracted appropriately. Molars will
undergo tip back moment and extrusion force. As the space
was closed, the deep overbite was corrected. The remaining
space in lower arch was closed by utilizing sliding mechanics
Table 4. Comparison of cephalometric measurement between
pre and posttreatment
SNA (degree)
Pretreatment
82.5
Posttreatment
81.0
SNB (degree)
75.0
75.0
Facial angle (degree)
86.5
84.5
Parameters
Convexity (mm)
8.5
7.0
31.0
32.0
4.5
3.5
Lower Incisors A Pog (degree)
25.0
25.0
Upper Incisors A Pog (mm)
15.0
8.0
Upper Incisors A Pog (degree)
49.0
32.0
Interincisal (degree)
106.5
122.0
Nasolabial (degree)
97.0
95.0
Lower Lip - E Line (mm)
9.0
4.0
Upper Lip - E Line (mm)
8.0
4.5
Mandible Plane (degree)
Lower Incisors - A Pog (mm)
Figure 11. Posttreatment facial and intraoral photographs.
Improvement of facial appearance was obviously seen. Adequate occlusal relationship with proper overjet and overbite
were evidenced
Figure 12. Overall and regional superimposition between pretreatment (black solid line) and posttreatment (red dash line)
illustrated the changes associated with treatment and growth
DISCUSSION
Space closure is one of the most important steps in orthodontic extraction case. The strategy of space closure
should be based on a careful diagnosis and treatment
plan made according to the specific needs of the individual.1 During space closure, controlling the overbite
and posterior anchorage are a difficult biomechanical
challenge. In extraction deep overbite cases, leveling and
alignment of the anterior teeth do not correct the deep
overbite, and therefore, it must be corrected to ensure
that full space closure is possible.2 The deep overbite
can also be worsening due to iatrogenic factors during
canines or incisors retraction. Canine retraction on light
continuous wire will generate extrusive effect on incisors
and deepening the bite due to wire deflection which creates by changing the canine inclination.3 Furthermore,
during extensive retraction on incisors, aggravation of
deep overbite is common because of uprighting of the
proclined incisors.4 Excessive force overpowers the
incisor torque control and deflects the archwire causing
distal tipping and bite deepening which is also known
as the roller coaster effect.5
The problem of anchorage control is rooted in Newtons
third law of motion, for every action there is an equal and
opposite reaction. Thus, the distal forces acting to retract
anterior teeth must be opposed by equal forces acting on
25
Journal of Dentistry Indonesia 2012, Vol. 19, No. 1, 20-26
the posterior anchorage units in the mesial direction.6 It
is often desirable to maintain posterior units from any
mesial movement, designated as group A anchorage
which is at least 75 % of the extraction space needs to
be closed by anterior teeth retraction.7
Headgear which is used to control anchorage and overbite is a device that has been used in orthodontic for at
least a hundred years, unfortunately, the use of headgear
depends on patient compliance for success. In recent
years, with the introduction of temporary anchorage
devices, a paradigm shift has occurred in the overall
perspective toward patient compliance, preservation of
anchorage and correct of deep overbite.
movement of retracted incisors. All of these outcomes
were due to proper moment to force ratio that generate
by applying differential moment concept during
incisors retraction. Growing of the nose and soft tissue
chin were also contributed for improving soft tissue
profile. There were no significant maxillary growth
in both patients, however, considerable mandibular
growth that partly responsible for overjet and overbite
reduction were evidence.
CONCLUSION
Biomechanics strategies that utilized in these cases
report were effective to achieve the desired treatment
outcome. It is recommended to provide more evidence
in the efficacy of this treatment strategies via well
controlled clinical studies.
However, temporary anchorage devices are invasive as
well as expensive appliances and have anatomy restriction in their application.1,8 One of the cardinal rules in
orthodontics is to treat the overbite before the overjet,
however, this approach will cause the longer treatment
time.9 In the light of these problems, it is needed to use
the extraordinary strategies in space closure that can
correct deep overbite as well as preserve the posterior
anchorage. To meet these goals, three-piece segmented
arch in conjunction with intrusion arch was used to
retract the canine and reduce deep overbite simultaneously so that while the canines were retracted, the deep
overbite would be corrected.
ACKNOWLEDGEMENT
We thank the patients and their parents for the agreement
to allow their photographs and cases to be presented.
REFERENCES
1. Nanda RS, Tosun YS. Biomechanics in orthodontics: principle and practice. Chicago: Quintessence
publishing; 2010.
2. Shroff B, Lindauer SJ, Burstone CJ, Leiss JB.
Segmented approach to simultaneous intrusion and
space closure: Biomechanics of the three-piece base
arch appliance. Am J Orthod Dentofacial Orthop.
1995;107:136-43.
3. Nanda R, Uribe F. Treatment of class II division 2
malocclusion in adults: biomechanical consideration.
J Clin Orthod. 2003;37:599-606.
4. Upadhyay M, Nanda R, 2010. Etiology, diagnosis, and
treatment of deep bite. In. Nanda R, Kapila S, editors.
Current therapy in orthodontics. St.Louis: Mosby;
2010. p. 186-98.
5. McLaughlin RP, Bennet JC, Trevisi HJ. Systemized orthodontic treatment mechanics. Edinburgh:
Mosby; 2001.
6. Kuhlberg AJ, Priebe DN. Space closure and anchorage control. Semin Orthod. 2001;7:42-9.
7. Rajcich MM, Sadowsky C. Efficacy of intraarch
mechanics using differential moments for achieving
anchorage control in extraction cases. Am J Orthod
Dentofacial Orthop. 1997;112: 441-8.
8. Nanda R, Uribe F. Temporary anchorage devices in
orthodontics. St.Louis: Mosby; 2009.
9. Ricketts RM, Bench RW, Gugino CF, Hilgers JJ,
Schulhof RJ. Bioprgressive therapy. Rocky mountain
orthodontic; 1979.
10. Nanda R, Kuhlberg AJ, Uribe F. Biomechanic basis of
extraction space closure. In: Nanda R, editor. Biomechanics and esthetic strategies in clinical orthodontics.
St.Louis: Elsevier Saunders; 2005. p. 194-210.
11. Proffit WR, Fields HW Jr, Sarver DM. Contemporary
Orthodontics. 4th ed. St.Louis: Mosby; 2007.
The segmented arch diminish the possibility of overbite
deepening that causing by canine retraction process. By
breaking up the arches into various segments during
treatment, we are able to evaluate the tooth movement in
all three plane of space and apply proper force application, both in direction and amount.9 The intrusion arch
not only creates vertical forces but also delivers distal
tip back moments on the molars to effectively control
the loss of anchorage that often associated with canine
retraction. After canine retraction and deep overbite
correction, the next stage is to retract four incisors. In
this stage, a method that can retract and maintain the
previously intruded incisors was required. Differential
moment was the method of choice due to force systems
that create not only intrusive force but also tip forward
moment on four incisors during retraction movement.
Tip forward moment (alpha moment) is important to
produce control tipping or bodily movement of retracted
incisors. In the posterior segment, differential moment
concept will produce tip back moments (beta moment)
to enhance posterior anchorage and extrusive force to
reduce deep overbite.10
From these two cases treatment result, we can see that
the treatment objective were accomplished. Although
deep overbite was corrected mainly by extrusive of
posterior teeth, fortunately, the remaining vertical
growth of the ramus compensated for the extrusive of
posterior teeth so that the mandibular did not significant
rotate posteriorly.11 Lips protrusion were improved
significantly since the proclined upper incisors were
retracted successfully with adequate type of movement.
In the upper arches, seventy-five percent or more of
the extraction space were effectively used for incisors
retraction. Both cases do not show any extrusion
26
Você também pode gostar
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeNo EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeNota: 4 de 5 estrelas4/5 (5794)
- Jurnal Fisure 3 PDFDocumento12 páginasJurnal Fisure 3 PDFayuandraniAinda não há avaliações
- The Little Book of Hygge: Danish Secrets to Happy LivingNo EverandThe Little Book of Hygge: Danish Secrets to Happy LivingNota: 3.5 de 5 estrelas3.5/5 (399)
- Mini ReviewDocumento7 páginasMini ReviewayuandraniAinda não há avaliações
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryNo EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryNota: 3.5 de 5 estrelas3.5/5 (231)
- PedodonsiaDocumento5 páginasPedodonsiaayuandraniAinda não há avaliações
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceNo EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceNota: 4 de 5 estrelas4/5 (894)
- PedodonsiaDocumento5 páginasPedodonsiaayuandraniAinda não há avaliações
- The Yellow House: A Memoir (2019 National Book Award Winner)No EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Nota: 4 de 5 estrelas4/5 (98)
- PedodonsiaDocumento5 páginasPedodonsiaayuandraniAinda não há avaliações
- Jurnal Os 2 GetDocumento7 páginasJurnal Os 2 GetayuandraniAinda não há avaliações
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureNo EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureNota: 4.5 de 5 estrelas4.5/5 (474)
- OrthodonsiaDocumento9 páginasOrthodonsiaayuandraniAinda não há avaliações
- Never Split the Difference: Negotiating As If Your Life Depended On ItNo EverandNever Split the Difference: Negotiating As If Your Life Depended On ItNota: 4.5 de 5 estrelas4.5/5 (838)
- Jurnal PDGIDocumento7 páginasJurnal PDGIayuandraniAinda não há avaliações
- Paresthesia Pasca EndoDocumento5 páginasParesthesia Pasca EndoayuandraniAinda não há avaliações
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaNo EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaNota: 4.5 de 5 estrelas4.5/5 (265)
- Poster Sikat Gigi PuskesDocumento2 páginasPoster Sikat Gigi PuskesayuandraniAinda não há avaliações
- 21582809Documento5 páginas21582809ayuandraniAinda não há avaliações
- Jurnal Os GetDocumento5 páginasJurnal Os GetayuandraniAinda não há avaliações
- The Emperor of All Maladies: A Biography of CancerNo EverandThe Emperor of All Maladies: A Biography of CancerNota: 4.5 de 5 estrelas4.5/5 (271)
- Dental Management of A Patient With Rubinstein-Taybi SyndromeDocumento4 páginasDental Management of A Patient With Rubinstein-Taybi SyndromeayuandraniAinda não há avaliações
- Dental Management of A Patient With Rubinstein-Taybi SyndromeDocumento4 páginasDental Management of A Patient With Rubinstein-Taybi SyndromeayuandraniAinda não há avaliações
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersNo EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersNota: 4.5 de 5 estrelas4.5/5 (344)
- PedodonsiaDocumento5 páginasPedodonsiaayuandraniAinda não há avaliações
- Team of Rivals: The Political Genius of Abraham LincolnNo EverandTeam of Rivals: The Political Genius of Abraham LincolnNota: 4.5 de 5 estrelas4.5/5 (234)
- PedodonsiaDocumento5 páginasPedodonsiaayuandraniAinda não há avaliações
- Jurnal Os 3 Get PDFDocumento3 páginasJurnal Os 3 Get PDFayuandraniAinda não há avaliações
- Dentigerous Cyst Associated With Multiple Complex Composite OdontomasDocumento3 páginasDentigerous Cyst Associated With Multiple Complex Composite OdontomasayuandraniAinda não há avaliações
- Compound Odontoma Associated With Impacted Teeth: A Case ReportDocumento4 páginasCompound Odontoma Associated With Impacted Teeth: A Case ReportayuandraniAinda não há avaliações
- Odontogenic TumorsDocumento14 páginasOdontogenic Tumorskavin_sandhuAinda não há avaliações
- The Unwinding: An Inner History of the New AmericaNo EverandThe Unwinding: An Inner History of the New AmericaNota: 4 de 5 estrelas4/5 (45)
- PedodonsiaDocumento5 páginasPedodonsiaayuandraniAinda não há avaliações
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyNo EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyNota: 3.5 de 5 estrelas3.5/5 (2219)
- The Dog Boy of WestminsterDocumento12 páginasThe Dog Boy of WestminsterKurt GarwoodAinda não há avaliações
- B2B MARKETING DURING DOWNTURNSDocumento5 páginasB2B MARKETING DURING DOWNTURNSRicha Mittal100% (1)
- Y1 Module Pet ShowDocumento13 páginasY1 Module Pet ShowJayne Frances EngelbertAinda não há avaliações
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreNo EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreNota: 4 de 5 estrelas4/5 (1090)
- TSR 1142 - The NorthDocumento238 páginasTSR 1142 - The NorthPanagiotisVourtzoumis100% (6)
- The Noun - Number&Concord-1Documento5 páginasThe Noun - Number&Concord-1Minuța Ioana BrătășanuAinda não há avaliações
- Unit 15: at The Dining Table.: Exercise 1: W Rite The Words: Egg Bread Milk Rice Juice Water Meat Fish Bean ChickenDocumento13 páginasUnit 15: at The Dining Table.: Exercise 1: W Rite The Words: Egg Bread Milk Rice Juice Water Meat Fish Bean ChickenThảo TrangAinda não há avaliações
- SeductionDocumento223 páginasSeductionarun151577% (13)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)No EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Nota: 4.5 de 5 estrelas4.5/5 (119)
- ECG BasicsDocumento15 páginasECG Basicsrohitmeena2889Ainda não há avaliações
- Animals Vocabulary Esl Word Search Puzzle Worksheets For KidsDocumento12 páginasAnimals Vocabulary Esl Word Search Puzzle Worksheets For KidsАлёна Кириченко100% (1)
- Science Notes Sem1 PDFDocumento31 páginasScience Notes Sem1 PDFWolfie Saraswathi Santhosham100% (1)
- Punctuation Quiz AnswersDocumento9 páginasPunctuation Quiz AnswersFirda Isran NafisahAinda não há avaliações
- Nursery RhymesDocumento10 páginasNursery RhymesDegee O. GonzalesAinda não há avaliações
- 2003, Vol.21, Issues 1, Oral Medicine and Oral DermatologyDocumento212 páginas2003, Vol.21, Issues 1, Oral Medicine and Oral DermatologyRizweta DestinAinda não há avaliações
- 27 of The Best Ever Sex Positions To Play DirtyDocumento1 página27 of The Best Ever Sex Positions To Play DirtyFrankie CulbertsonAinda não há avaliações
- Crochet Plush Bunny Neon Amigurumi Free PatternDocumento4 páginasCrochet Plush Bunny Neon Amigurumi Free PatternflechedestructriceAinda não há avaliações
- Chapter 14 - Lymph and ImmunityDocumento13 páginasChapter 14 - Lymph and Immunityapi-220531452Ainda não há avaliações
- Tale of 12 Chinese ZodiacDocumento32 páginasTale of 12 Chinese ZodiacAiman HassanAinda não há avaliações
- Meat Quality Evaluation by Computer VisionDocumento9 páginasMeat Quality Evaluation by Computer Visionaleksandar.haAinda não há avaliações
- Donald M. Johnson - Essentials of PsychologyDocumento519 páginasDonald M. Johnson - Essentials of PsychologyPhilippe AblonAinda não há avaliações
- Disney - Ice Age - The Movie Novel (KT) PDFDocumento125 páginasDisney - Ice Age - The Movie Novel (KT) PDFMoyeen Uddin HasanAinda não há avaliações
- The Growing FetusDocumento68 páginasThe Growing Fetusjean thereseAinda não há avaliações
- Acute Respiratory InfectionDocumento32 páginasAcute Respiratory InfectionRinnaAyuNovitaSary100% (1)
- Advanced Ocean Animals Activity BookDocumento5 páginasAdvanced Ocean Animals Activity BookRetno MaharaniAinda não há avaliações
- March P2 (Q & A) Sem Paper BioDocumento13 páginasMarch P2 (Q & A) Sem Paper BioDineish MurugaiahAinda não há avaliações
- Ex Situ Conservation: R.R.Bharathi 2 Yr BiochemistryDocumento20 páginasEx Situ Conservation: R.R.Bharathi 2 Yr BiochemistryVishal TakerAinda não há avaliações
- 0610 s18 QP 23 PDFDocumento16 páginas0610 s18 QP 23 PDFTesterAinda não há avaliações
- Kitchen tools and utensils identification guideDocumento3 páginasKitchen tools and utensils identification guideescabosa.ermelynAinda não há avaliações
- Journal Writing PromptsDocumento6 páginasJournal Writing Promptscombination_soupAinda não há avaliações
- Ghid Utilizare Cuptor ElectricDocumento76 páginasGhid Utilizare Cuptor ElectricRamona RadulescuAinda não há avaliações
- Antiprotozoal Agents 6Documento29 páginasAntiprotozoal Agents 6EinsteenAinda não há avaliações
- The Things We Make: The Unknown History of Invention from Cathedrals to Soda CansNo EverandThe Things We Make: The Unknown History of Invention from Cathedrals to Soda CansAinda não há avaliações
- To Engineer Is Human: The Role of Failure in Successful DesignNo EverandTo Engineer Is Human: The Role of Failure in Successful DesignNota: 4 de 5 estrelas4/5 (137)