Escolar Documentos
Profissional Documentos
Cultura Documentos
Jurnal Lani 2
Enviado por
Nicky Adi SaputraDireitos autorais
Formatos disponíveis
Compartilhar este documento
Compartilhar ou incorporar documento
Você considera este documento útil?
Este conteúdo é inapropriado?
Denunciar este documentoDireitos autorais:
Formatos disponíveis
Jurnal Lani 2
Enviado por
Nicky Adi SaputraDireitos autorais:
Formatos disponíveis
Indian J Surg Oncol (June 2012) 3(2):154157
DOI 10.1007/s13193-012-0151-5
ORIGINAL ARTICLE
Accuracy of Clinical Examination of Breast Lumps
in Detecting Malignancy: A Retrospective Study
Chandni Ravi & Gabriel Rodrigues
Received: 4 February 2012 / Accepted: 24 April 2012 / Published online: 22 May 2012
# Indian Association of Surgical Oncology 2012
Abstract Clinical examination is a simple method to detect
breast lumps and their nature as it is inexpensive and noninvasive and if found to be accurate, might be of great value
as a diagnostic tool. The aim of this study was to evaluate
the accuracy of clinical examination and its contribution
towards the diagnosis of a palpable breast lump. The study
was record based and conducted at a University Medical
College Hospital and a tertiary referral centre of South India.
Patient files of those women who presented with a breast
lump between January to December 2011 were studied. A
total of 120 patients were obtained following necessary
exclusions. The accuracy of clinical assessment at an outpatient facility was determined by comparing the physicians diagnosis with the final histopathological diagnosis.
The inter-observer agreement (kappa) for diagnosing a
breast lump was 81 % (95 % Confidence Interval071 %
to 92 %) indicating a good agreement between clinical and
pathological diagnoses. McNemar test also indicated a high
degree of concordance between the two diagnoses (4.17 %
discordance). Sensitivity, specificity, positive and negative
predictive values of clinical breast examination in comparison to histopathology were 95, 88, 87, and 95 % respectively, with an overall accuracy of 90.8 %. 11 lumps were
wrongly diagnosed at the time of clinical examination. Clinical examination of breast lumps was found to have a high
sensitivity (94.5 %) and specificity (87.7 %) and can be used
as the diagnostic tool to identify the nature of the lump,
however, its value in diagnosing breast malignancy remains
contributory due to the possibility that malignant lumps
C. Ravi : G. Rodrigues (*)
Department of General Surgery, Kasturba Medical College,
Manipal University,
Manipal 576104 Karnataka, India
e-mail: gabyrodricks@gmail.com
could be overlooked and present as advanced cancer at a
later stage. Histopathology is recommended in all cases
unless clinical examination is supported with strong evidence of benignity based on repeated breast imaging via
ultrasound or mammogram (>35 yrs).
Keywords Breast cancer . Clinical examination . Biopsy .
Surgery
Introduction
Breast cancer is the second most common cancer (10.4 % of
all cancer incidence, both sexes counted) and the fifth most
common cause of cancer death in the world [1]. In 2005,
breast cancer caused 502,000 deaths worldwide (7 % of
cancer deaths; almost 1 % of all deaths) [2]. One-fourth of
women suffer from breast disease in their life time [1, 2].
With the improvement in health care and increasing life
expectancy, more and more women are being exposed to
the risk of developing breast cancer. Majority of women
who come to the surgical OPD complain of either pain or
lump in the breast or discharge from the nipple [3].
There are various modalities for the diagnosis of a breast
lump such as mammography, ultrasonography, fine needle
aspiration cytology (FNAC) but none of them are without
impunity [4]. Clinical evaluation, however, is a simple
method to detect cases as it is inexpensive and noninvasive and if found to be accurate, might be of great value
[5]. Timely and accurate diagnosis of a breast lump with
early intervention can bring down morbidity and mortality
of malignant disease. Clinical evaluation could function as a
valuable diagnostic tool. This would prove to be highly
useful particularly in rural areas where funds and/or facilities may not be available for more sophisticated diagnostic
Indian J Surg Oncol (June 2012) 3(2):154157
methods [6]. The systematic use of the clinical examination
criteria and the organizational platform would allow the
clinicians to select malignant cases and plan inpatient/outpatient surgical treatment so as to avoid unnecessary admissions which will reduce hospital bed occupancy and
expenditures incurred on the part of the patient.
Breast lump is a very sensitive issue for the patient so a
reliable, non-invasive and prompt diagnosis helps to lessen
the associated anxiety and leads to early definitive
treatment.
Review of Literature
Early work by Magarey CJ et al. [7] was concerned with the
development of a management plan for the outpatient diagnosis of breast symptoms and they concluded that in the
majority of patients the presence or absence of malignancy
can be established with a high degree of certainty before
biopsy. Several groups of researchers have evaluated the
diagnostic efficacy of what is known as the triple test score,
or the clinical-radiologic-cytological triad [812]. Majority
of them advocate this system of diagnosis and suggest that it
should be followed by definitive treatment, based on the
high accuracy values obtained by the studies. However,
Crone P et al. [9] found that while the diagnostic sensitivity
of clinical examination was high, around 98 %, the specificity was rather low, averaging 48 %. In addition, the study
disclosed a statistical possibility of overlooking a few malignant tumors when using these three procedures and they
recommended excision of all palpable breast lumps.
Reeves MJ et al. [13] developed a clinical decision rule
for triage of women with palpable breast masses into open
biopsy or follow-up and concluded that it reduced the number of open biopsies performed. There is an overall consensus that clinical breast examination (CBE) is useful in
screening as well as in evaluation of a lump. About 3 % to
45 % of cancer diagnoses missed by mammography were
reported as having been detected by CBE. Although the
sensitivity of mammography is greater than that of CBE,
there is a residual diagnostic value of CBE that favors its
continued use in screening [14].
Patients and Methods
The study design was record based. The records of women
who presented with a breast lump or referred for breast
examination to this University Medical College Hospital
and a tertiary referral centre of South India, during the time
period January to December 2011 were studied. Structured
performas were filled based on the information obtained
from the individual patient files. Out of a total of 207
155
women who presented to our outpatient department with a
breast lump, 87 exclusions were made when the diagnosis
was known prior to examination (For example, if they were
diagnosed elsewhere and had come for a second opinion),
when patients who were admitted for treatment or follow-up
and if the clinical impression following examination was not
documented, or where pathological confirmation of the diagnosis was absent. Information was obtained regarding the
clinical impression and differential diagnosis as recorded by
the physician at the time of examination, following which
histopathology lab reports of those were patients were
accessed to obtain the final/confirmatory diagnosis.
Collected data were analyzed using SPSS 16.0. The
sensitivity, specificity, positive predictive value, negative
predictive values were calculated. An inter-observer reliability analysis using the Kappa statistic was performed to
determine consistency between clinical and pathological
findings. McNemar test was performed to test the degree
of discordance between the findings. Sensitivity, specificity,
predictive values and accuracy were calculated by using
standard formulae on the 22 table.
Results
A total of 120 patients fulfilled the inclusion criteria of
whom clinically, 60 (50 %) were benign and 60 (50 %) were
suspicious for malignancy. Of the 23 patients that underwent
mammography, 9 (39 %) were benign and 14 (61 %) were
suspicious for malignancy. Histopathology revealed 65
(54.2 %) to be benign and 55 (45.8 %) to be malignant.
Clinical examination was found to have a sensitivity of
94.5 %, i.e., 52 out of 55 malignant lumps were detected
clinically, and a specificity of 87.7 %, i.e., 57 out of 65
benign lumps were clinically diagnosed to be benign. The
predictive value of a positive was 86.7 %, the predictive
value of a negative test was 95 % (Table 1). 109 out of 120
lumps were diagnosed correctly (overall accuracy of
90.8 %). The inter-observer agreement (Kappa) was 0.817
Table 1 Accuracy of clinical diagnosis (when compared to histopathological diagnosis)
Histopathology
Clinical impression
Malignant
Benign
Total
Malignant
Benign
Total
52
3
55
8
57
65
60
60
120
a) Sensitivity052/55100094.5 % b) Specificity057/65100087.7 %
c) Positive predictive value052/60100086.7 % d) Negative predictive
value057/60100095 %
e) Accuracy052+57/120090.8 %
156
Indian J Surg Oncol (June 2012) 3(2):154157
(81 %) with p<0.001, 95 % confidence interval (71 %,
92 %) indicating a strong agreement existed between the
clinical examination and histopathological impressions.
McNemar test: The difference between clinical diagnosis
and histopathological diagnosis was 4.17 % with 95 %
confidence interval from -2.01 % to 8.06 %, (P00.226, not
statistically significant).
Discussion
In our study, retrospective analysis of clinical examination
of 120 patients and confirmation of the results with the
histopathological findings showed CBE to have a high
sensitivity and specificity. However, despite an overall accuracy of 90.8 %, in 11 patients, the nature of the breast
lump was not detected clinically. 3 patients with malignant
breast lumps were clinically diagnosed to be benign and
8 women with benign lumps were diagnosed clinically to
have breast cancer.
Peak incidence of malignancy was seen in the 4150 age
group. The mean age of diagnosis of a benign lump was
34.8 years and of a malignant lump was 47.7 years. 14 of
the malignant lumps were in women under 40, and 18 of the
benign lumps were in women over 40, therefore age cannot be
used as a reliable indicator of the nature of the lump (Table 2).
The most common location of any breast lump was
the upper outer quadrant (29.2 %). 11 % of malignant
lumps were soft in consistency while 8 % of benign
lumps were hard in consistency. Majority of the lumps
examined were mobile (82.5 %). Of the malignant
lumps, 65.5 % were mobile and 34.5 % were fixed to
the chest wall. 27.5 % of the lumps had an ill-defined
margin, out of which 84.8 % were found to be malignant (Table 3). Thus, while these factors are contributory to the clinical diagnosis, they are imprecise and
cannot alone decide the nature of the breast lump.
The sensitivity, specificity, positive predictive value and
negative predictive values obtained on comparison of clinical examination with mammogram were 100 %, 77.8 %,
87.5 % and 100 % respectively. Out of 15 malignant patients
Table 3 Chart indicating the characteristics of the breast lumps
examined
Examination finding
Location
-Upper Outer Quadrant
-Upper Inner Quadrant
-Lower Outer Quadrant
-Lower Inner Quadrant
-Central
Consistency
-Soft
-Firm
-Hard
Mobility
-Mobile
-Fixed
Margins
-Regular
-Irregular
Benign (65)
Malignant (55) Total (120)
19
13
14
7
12
16
11
8
13
7
35 (29.2
24 (20.0
22 (18.3
20 (16.7
19 (15.8
40
20
5
6
16
33
46 (38.3 %)
36 (30.0 %)
38 (31.7 %)
63
2
36
19
99 (82.5 %)
21 (17.5 %)
60
5
27
28
87 (72.5 %)
33 (27.5 %)
%)
%)
%)
%)
%)
that had undergone both mammogram and confirmatory
histopathology, clinical examination detected a case of malignancy that was missed by mammogram. Clinical examination, used in conjunction with mammogram may be used
for early screening since they would have an additive value.
The quality of clinical breast examination needs to be increased by standardizing examination procedures. Careful,
systematic palpation has been shown to increase detection
of breast lumps. Patient position, palpation of breast boundaries, and examination pattern and technique are important
variables in CBE [14].
9 % of lumps were misdiagnosed clinically. Considering
the prevalence of breast cancer, in a large population that
would amount to too many missed cases that could have
been avoided by use of improved diagnostic techniques that
are available, such as mammogram, ultrasound, FNAC and
biopsy.
Conclusion
Table 2 Chart indicating the characteristics of the study population
Age
Number of lumps
Benign
Malignant
<20
2130
3140
4150
5160
6170
7180
10
23
28
40
11
4
4
9
22
16
15
3
0
0
1
1
12
25
8
4
4
While we found the sensitivity and specificity of clinical
examination to be high, with an overall accuracy of 90.8 %,
it cannot be used as a stand-alone diagnostic tool when tools
with higher diagnostic value are at our disposal. It is, however, a reasonable assessment tool to determine how to
proceed from the point of presentation. If the clinical
examination of the breast lump points towards malignancy, a biopsy must be arranged. In case of a clinically
benign lump, an ultrasound and a mammogram (in
women above 35 years) must be arranged. If the breast
Indian J Surg Oncol (June 2012) 3(2):154157
imaging suggests benign nature - cyst or clear cut fibroadenoma with BIRADS 2 lesion, a biopsy may be avoided
and patient called for six monthly follow up by repeat
breast imaging. In case of BIRADS 3, 4 or 5 lesions a biopsy
is mandatory.
Conflict of interest Nil
Sources of funding
Nil
References
1. Curado MP (2011) Breast cancer in the world: incidence and
mortality. Salud Publ Mex 53:372384
2. Meads C, Ahmed I, Riley RD (2011) A systematic review of breast
cancer incidence risk prediction models with meta-analysis of their
performance. Breast Cancer Res Treat Oct 22 [Epub ahead of print]
3. Nederend J, Duijm LE, Voogd AC, Groenewoud JH, Jansen FH,
Louwman MW (2012) Trends in incidence and detection of advanced breast cancer at biennial screening mammography in The
Netherlands: a population based study. Breast Cancer Res 14:R10
4. Prasad SN, Houserkova D (2007) A comparison of mammography
and ultrasonography in the evaluation of breast masses. Biomed
Pap Med Fac Univ Palacky Olomouc Czech Repub 151:315322
157
5. Hampton T (2012) Breast cancer symposium highlights risk, recurrence, and research trials. JAMA 307:348350
6. Magarey CJ (1976) Detection and diagnosis of early breast cancer.
Med J Aust 2:834837
7. Magarey CJ, Watson WJ (1976) The outpatient diagnosis of breast
lumps. 46:344-349
8. Thomas JM, Fitzharris BM, Redding WH et al (1978) Clinical
examination, xeromammography, and fine-needle aspiration
cytology in diagnosis of breast tumours. Br Med J 2:1139
1141
9. Crone P, Hertz J, Nilsson T et al (1984) The predictive value of
three diagnostic procedures in the evaluation of palpable breast
tumours. Ann Chir Gynaecol 7:273276
10. Di Pietro S, Fariselli G, Bandieramonte G et al (1987) Diagnostic
efficacy of the clinical-radiological-cytological triad in solid breast
lumps: results of a second prospective study on 631 patients. Eur J
Surg Oncol 13:335340
11. Martelli G, Pilotti S, Coopmans de Yoldi G et al (1990) Diagnostic
efficacy of physical examination, mammography, fine needle aspiration cytology (triple-test) in solid breast lumps: an analysis of
1708 consecutive cases. Tumori 76:476479
12. Ghimire B, Khan MI, Bibhusal T, Singh Y, Sayami P (2008)
Accuracy of triple test score in the diagnosis of palpable breast
lump. JNMA J Nepal Med Assoc 47:189192
13. Reeves MJ, Osuch JR, Pathak DR (2003) Development of a
clinical decision rule for triage of women with palpable breast
masses. Clin Epidemiol 25:636645
14. Barton MB, Harris R, Fletcher SW (1999) Does this patient have
breast cancer? The screening clinical breast examination: Should it
be done? How? JAMA 282:12701280
Você também pode gostar
- Progestogen For Treating Threatened Miscarriage (Review) : Wahabi HA, Abed Althagafi NF, Elawad MDocumento16 páginasProgestogen For Treating Threatened Miscarriage (Review) : Wahabi HA, Abed Althagafi NF, Elawad MNicky Adi SaputraAinda não há avaliações
- The Yellow House: A Memoir (2019 National Book Award Winner)No EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Nota: 4 de 5 estrelas4/5 (98)
- Depression and Risk of Stroke in Midaged Women: A Prospective Longitudinal StudyDocumento6 páginasDepression and Risk of Stroke in Midaged Women: A Prospective Longitudinal StudyNicky Adi SaputraAinda não há avaliações
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeNo EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeNota: 4 de 5 estrelas4/5 (5795)
- Posttraumatic Stress Disorder and Adherence To Medications in Survivors of Strokes and Transient Ischemic AttacksDocumento7 páginasPosttraumatic Stress Disorder and Adherence To Medications in Survivors of Strokes and Transient Ischemic AttacksNicky Adi SaputraAinda não há avaliações
- Never Split the Difference: Negotiating As If Your Life Depended On ItNo EverandNever Split the Difference: Negotiating As If Your Life Depended On ItNota: 4.5 de 5 estrelas4.5/5 (838)
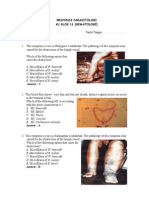
- Responsi Parasitologi Ku Blok 11 (Hematologi)Documento8 páginasResponsi Parasitologi Ku Blok 11 (Hematologi)Nicky Adi SaputraAinda não há avaliações
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceNo EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceNota: 4 de 5 estrelas4/5 (895)
- ?DD R/ T 1 Qussg: Alamat Iido, Go 'Documento1 página?DD R/ T 1 Qussg: Alamat Iido, Go 'Nicky Adi SaputraAinda não há avaliações
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersNo EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersNota: 4.5 de 5 estrelas4.5/5 (345)
- Arthropod-Born VirusesDocumento3 páginasArthropod-Born VirusesNicky Adi SaputraAinda não há avaliações
- Classic Pulse Diagnosis PDFDocumento21 páginasClassic Pulse Diagnosis PDFDani TenaAinda não há avaliações
- NUR 104 Nursing Process MY NOTESDocumento77 páginasNUR 104 Nursing Process MY NOTESmeanne073100% (1)
- The Little Book of Hygge: Danish Secrets to Happy LivingNo EverandThe Little Book of Hygge: Danish Secrets to Happy LivingNota: 3.5 de 5 estrelas3.5/5 (400)
- ResumedieteticinternshipDocumento1 páginaResumedieteticinternshipapi-208833628Ainda não há avaliações
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureNo EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureNota: 4.5 de 5 estrelas4.5/5 (474)
- TBL (Miscarrriage)Documento36 páginasTBL (Miscarrriage)hitsugayat_7100% (1)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryNo EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryNota: 3.5 de 5 estrelas3.5/5 (231)
- Corneal Collagen Cross-Linking: A ReviewDocumento12 páginasCorneal Collagen Cross-Linking: A ReviewHimawan WidyatmikoAinda não há avaliações
- Ureteropelvic Junction Obstruction 0Documento4 páginasUreteropelvic Junction Obstruction 0Dhian Hidayat100% (1)
- The Emperor of All Maladies: A Biography of CancerNo EverandThe Emperor of All Maladies: A Biography of CancerNota: 4.5 de 5 estrelas4.5/5 (271)
- Anatomy: Patellar Tendon TearDocumento11 páginasAnatomy: Patellar Tendon TearrahadianpambudiAinda não há avaliações
- 6.Intra-Arch DistractionDocumento15 páginas6.Intra-Arch DistractionMónica C. BadilloAinda não há avaliações
- Cold InjuryDocumento34 páginasCold Injurydassdeepak69100% (1)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaNo EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaNota: 4.5 de 5 estrelas4.5/5 (266)
- PMR Poster TBI Takotsubo AAP 2010 PosterDocumento1 páginaPMR Poster TBI Takotsubo AAP 2010 PosterjuanvelasquezAinda não há avaliações
- The Unwinding: An Inner History of the New AmericaNo EverandThe Unwinding: An Inner History of the New AmericaNota: 4 de 5 estrelas4/5 (45)
- ABG Algorithm PDFDocumento2 páginasABG Algorithm PDFamin2014Ainda não há avaliações
- Team of Rivals: The Political Genius of Abraham LincolnNo EverandTeam of Rivals: The Political Genius of Abraham LincolnNota: 4.5 de 5 estrelas4.5/5 (234)
- PFPS Is Mainly Due To Changes in The Normal Patella Alignments. The Factors That CanDocumento21 páginasPFPS Is Mainly Due To Changes in The Normal Patella Alignments. The Factors That CanviikkaassAinda não há avaliações
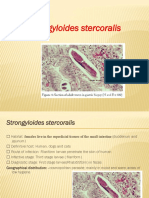
- Strongyloides StercoralisDocumento30 páginasStrongyloides StercoralisEllagEsz100% (1)
- Iptec Teaching LogDocumento2 páginasIptec Teaching Logapi-508924243Ainda não há avaliações
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyNo EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyNota: 3.5 de 5 estrelas3.5/5 (2259)
- Haloperidol: Brand Name: HaldolDocumento15 páginasHaloperidol: Brand Name: Haldolteguh aminAinda não há avaliações
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreNo EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreNota: 4 de 5 estrelas4/5 (1090)
- Neo Launch .Rand 6ifp79iaori5qDocumento2 páginasNeo Launch .Rand 6ifp79iaori5qAnonymous sfkedkymAinda não há avaliações
- Bulacan: Socio-Economic and Health ProfileDocumento29 páginasBulacan: Socio-Economic and Health ProfileHazel Acidre100% (1)
- Clinical LadderDocumento7 páginasClinical LadderAna LusiyanaAinda não há avaliações
- Written Exam Sample 6 With AnswersDocumento5 páginasWritten Exam Sample 6 With AnswersOrtega IanAinda não há avaliações
- Cancer Industry, The Classic Expose of The - Moss, Ralph WDocumento546 páginasCancer Industry, The Classic Expose of The - Moss, Ralph Wpdf ebook free download80% (5)
- Verbal (Non Verbal) Therapeutic Communication Technique Used Rationale and Feelings of Nurse EvaluationDocumento13 páginasVerbal (Non Verbal) Therapeutic Communication Technique Used Rationale and Feelings of Nurse EvaluationLei Ortega80% (10)
- Toxic and Metabolic Disorders of The Nervous SystemDocumento7 páginasToxic and Metabolic Disorders of The Nervous SystemBenj Ricafrente IIIAinda não há avaliações
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)No EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Nota: 4.5 de 5 estrelas4.5/5 (121)
- High Alert MedicationsDocumento1 páginaHigh Alert MedicationsrsdsAinda não há avaliações
- Chronic Gastritis Is Autoimmune or EnvironmentalDocumento4 páginasChronic Gastritis Is Autoimmune or EnvironmentalovidiuticaAinda não há avaliações
- PreOperative & PremedicationDocumento9 páginasPreOperative & PremedicationMastering Archangel SchneiderAinda não há avaliações
- Cardiovascular Ultrasound Supervisor/sonographerDocumento4 páginasCardiovascular Ultrasound Supervisor/sonographerapi-121663384Ainda não há avaliações
- MonitorDocumento3 páginasMonitorestebanAinda não há avaliações
- Humidified High Flow Nasal Cannula Oxygen Guideline PDFDocumento27 páginasHumidified High Flow Nasal Cannula Oxygen Guideline PDFjoaoalmeida_1955Ainda não há avaliações
- Burch-Schneider Reinforcement Cage: Product Information Surgical TechniqueDocumento36 páginasBurch-Schneider Reinforcement Cage: Product Information Surgical TechniquePetru Caraja100% (1)
- Funda 25Documento10 páginasFunda 25Mar OrdanzaAinda não há avaliações