Escolar Documentos
Profissional Documentos
Cultura Documentos
Mild Cognitive Impairment Applicability of Research
Enviado por
IcaroDireitos autorais
Formatos disponíveis
Compartilhar este documento
Compartilhar ou incorporar documento
Você considera este documento útil?
Este conteúdo é inapropriado?
Denunciar este documentoDireitos autorais:
Formatos disponíveis
Mild Cognitive Impairment Applicability of Research
Enviado por
IcaroDireitos autorais:
Formatos disponíveis
Psychological Medicine, 2006, 36, 507515.
f 2006 Cambridge University Press
doi:10.1017/S0033291705006744 First published online 23 January 2006. Printed in the United Kingdom
Mild cognitive impairment : applicability of research
criteria in a memory clinic and characterization of
cognitive prole
S U V A R N A A L L A D I 1 , R O B E R T A R N O L D1 , J O A N N A M I T C H E L L1 ,
P E T E R J. N E S T O R 1 A N D J O H N R. H O D G E S 1 ,2*
1
Department of Clinical Neurosciences, University of Cambridge, UK ; 2 MRC Cognition
and Brain Sciences Unit, Cambridge, UK
ABSTRACT
Background. We explored the applicability of recently proposed research criteria for mild cognitive
impairment (MCI) in a memory clinic and changes in case denition related to which memory tests
are used and the status of general cognitive function in MCI.
Method. A total of 166 consecutive GP referrals to the Cambridge Memory Clinic underwent
comprehensive neuropsychological and psychiatric evaluation.
Results. Of 166 cases, 42 were excluded (signicant depression 8, established dementia 29 and other
disorders 5). Of 124 non-demented, non-depressed patients, 72 fullled Petersens criteria for
amnestic MCI based upon verbal memory performance [the Rey Auditory Verbal Learning Test
(RAVLT)] and 90 met criteria if performance on verbal and/or non-verbal memory tests [the Rey
gure recall or the Paired Associates Learning test (PAL)] was considered. Of the 90 broadly
dened MCI cases, only 25 had pure amnesia: other subtle semantic and/or attention decits were
typically present. A further 12 were classed as non-amnestic MCI and 22 as worried well.
Conclusions. Denition of MCI varies considerably dependent upon the tests used for case
denition. The majority have other cognitive decits despite normal performance on the
Mini-mental State Examination (MMSE) and intact activities of daily living (ADL) and t within
multi-domain MCI. Pure amnesic MCI is rare.
INTRODUCTION
Alzheimers disease (AD) and other neurodegenerative cognitive disorders pass through a
phase characterized by subtle cognitive decits
before onset of frank dementia (Nestor et al.
2004). A number of terms have been used to
describe this early stage, the most widely used
being mild cognitive impairment (MCI). This
term has been used inconsistently at times, but
the recent trend has been to reserve the label for
cases with (i) informant-corroborated history of
* Address for correspondence: Professor John R. Hodges, MRC
Cognition and Brain Sciences Unit, 15 Chaucer Road, Cambridge
CB2 2EF, UK.
(Email : john.hodges@mrc-cbu.cam.ac.uk)
memory symptoms, (ii) objective evidence of
memory impairment (usually worse than 1.5
standard deviations below a demographically
matched control group on a verbal memory
test), (iii) preserved general cognition, (iv) preserved activities of daily living (ADL), and (v)
no dementia (Grundman et al. 2004). Although
undoubtedly a useful concept, controversies
exist regarding the validity of MCI as a cohesive
clinical entity, the applicability of the researchbased concept in clinical practice, the homogeneity of the cognitive decits in MCI and the
prognosis (Ritchie et al. 2001; Chertkow, 2002 ;
Luis et al. 2003 ; Dubois & Albert, 2004).
Reasons for the lack of consensus include
variability in populations studied, criteria used
507
508
S. Alladi et al.
for the diagnosis of MCI, the neuropsychological tests used and duration of follow-up.
Among the various criteria for MCI, those
proposed by Petersen et al. (1999 ; 2001) are the
most widely used and, as listed above, have been
operationalized for use in population-based research trials (Grundman et al. 2004). According
to these criteria, MCI is considered to be an
amnestic state with a very high rate of progression to clinical AD. In this study we focus
on two key issues related to these criteria. The
rst relates to the denition of amnesia and
the memory test(s) that should be used to detect
MCI because the inuence that dierent
memory tests have on MCI case denition is
unknown. The Petersen criteria recommend the
use of verbal recall tests to dene memory
impairment, but verbal recall is known to be
vulnerable to other processes such as performance anxiety and aective disorders (Quraishi &
Frangou, 2002). Some studies have shown
that visual memory tests such as the Paired
Associates Learning test (PAL) from the computerized CANTAB battery are highly predictive of subsequent cognitive decline to probable
AD (Fowler et al. 1995; Swainson et al. 2001 ;
Blackwell et al. 2004). As far as we are aware, no
studies have compared the use of verbal and
non-verbal/visual memory tests in dening
MCI.
The second unresolved and contentious issue
addressed by this study is the extent to which
other cognitive domains, such as semantic
memory and/or attentional-executive function,
are involved in apparently pure amnestic MCI
patients. According to current criteria, other
cognitive decits are excluded on the basis of the
Mini-mental State Examination (MMSE) score
(o24) and clinical judgement, but no specic
tests or cut-os have been specied as exclusion
criteria (Petersen et al. 2001; Grundman et al.
2004). Dierences in interpreting this component of the criteria have given rise to considerable variability in case denition and prognosis
of MCI (Tierney et al. 1996 ; Bowen et al. 1997 ;
Devanand et al. 1997 ; Petersen et al. 1999 ;
Albert et al. 2001; Bozoki et al. 2001; De Jager
et al. 2003 ; Lambon-Ralph et al. 2003).
Furthermore, as the general public may use
memory problems as a generic term to
describe cognitive impairment, it is possible that
the cognitive decits in non-memory domains
such as naming and executive function may be
the most prominent decits in some patients.
The frequency of non-amnestic MCI relative to
amnestic MCI in a memory clinic is not known.
The Cambridge MCI longitudinal study aims
to follow up a large cohort of people with
memory complaints who do not full criteria for
dementia. All patients undergo a comprehensive
assessment of their symptoms, mood state and
performance on a range of neuropsychological
tests. Patients are followed up annually for repeat neuropsychological and clinical evaluation.
We present the preliminary baseline results.
The primary aim of this study was to assess
the applicability of research criteria for MCI in
a memory clinic setting. We also aimed to assess
how dierent episodic memory tests categorized
MCI and to study the pattern of general cognitive dysfunction within amnestic MCI as dened
by the Petersen criteria.
METHOD
Subjects
A total of 166 participants were included in the
study, consisting of consecutive referrals to the
Cambridge Memory Clinic between June 2003
and March 2005 from general practitioners in
the Cambridge area in whom the referral letter
suggested the possibility of early dementia. Over
the same time period 150 referrals from other
consultants were received who were not included in the study as these patients had (in
general) established dementia syndromes and a
wide range of neuropsychiatric syndromes. All
were aged 50 or over and had an informant,
typically a spouse. All patients were examined
by an experienced behavioural neurologist
(P. J. N. or J. R. H.). The MMSE (Folstein
et al. 1975) and Addenbrookess Cognitive Examination (ACE) (Mathuranath et al. 2000;
Bak et al. 2005; Dudas et al. 2005) were used
to assess general cognitive status. Impact on
everyday activities was evaluated using the
Clinical Dementia Rating Scale (CDR ; Morris,
1993). Depression and anxiety were scored using
the Hospital Anxiety and Depression Scale
(HADS) and the Geriatric Depression Scale
(GDS; Snaith, 1994). Patients were investigated
with a standard battery of screening blood tests
and brain imaging [computed tomography (CT)
or magnetic resonance imaging (MRI) scan].
509
Mild cognitive impairment
166
GP Referrals
Mild memory complaints
42 Excluded
Depression, Medical disorders,
Dementia
124
Non-demented, nondepressed
72 MCI
Petersens criteria
90 Amnestic MCI
26
Pure amnestic MCI
FIG. 1.
30 MCI
Non-Petersens
18 Amnestic MCI
Visual memory
64
Multiple domain MCI
12
Non-amnestic MCI
22
Worried well
Cognitive characteristics of elderly people with mild memory complaints referred to a memory clinic.
Patients with established dementia (DSM-IV),
signicant depression (clinical judgement or
HADS>14) or other medical conditions such as
alcoholism, stroke, epilepsy or head injury that
could account for memory problems were
excluded. Forty-two patients were excluded because of signicant depression (8), other medical
causes for amnesia (5) and established dementia
(29). The dementia cases comprised 20 with AD
and nine non-AD [frontotemporal dementia (5),
dementia with Lewy bodies (2), corticobasal
degeneration (1) and vascular dementia (1)].
The nal study cohort therefore comprised 124
subjects (Fig. 1). The study was approved by the
Local Research Ethics Committee. Control data
were obtained from 30 age- and educationmatched normal volunteers drawn from the
MRC Cognition and Brain Sciences Unit subject panel.
Neuropsychological assessment
All patients underwent neuropsychological
assessment covering a range of cognitive
domains. Pre-morbid IQ was determined by the
National Adult Reading Test (NART) (Nelson
& Willison, 1991). Four cognitive domains
were assessed : episodic memory, language and
semantic memory, attentional-executive functioning, and visuospatial skills. We selected tests
that are widely used in routine neuropsychological practice and are sensitive to early decits
in these cognitive domains.
Episodic memory
Rey Auditory Verbal Learning Test (RAVLT ;
Schmidt, 1996). The RAVLT was administered
in the standard manner, which consists of ve
learning trials of a 15-word list (with the subject
asked to repeat back as many items as possible
after each trial). A distracter list is then presented once, after which the subject is asked to
recall as many items as possible from the
original list (immediate recall). Delayed recall of
the same list is assessed after 30 min, and then
recognition is measured through identication
of the 15 original target words from a list
containing 35 foils.
Rey complex gure test (Rey, 1941). Subjects
were asked to copy this gure freehand, and
without time restriction. After an interval of
30 min, subjects were asked (without warning)
to reproduce from memory the gure that they
had copied.
510
S. Alladi et al.
Paired Associates Learning (PAL). Subjects
were administered a modied and shortened
version of the PAL from the CANTAB battery
(Swainson et al. 2001 ; Blackwell et al. 2004).
This test is given in two phases. In the rst,
introductory phase, six white boxes appear on
a touch-sensitive computer screen. Each box
opens and closes in a random sequence,
revealing in three of them three dierent simple
coloured patterns. Once all boxes have opened
and closed, the patterns are presented in random order in the centre of the screen and the
subject touches the box in which he or she
remembers each pattern appearing. Up to 10
attempts are allowed to achieve all three correct.
As soon as success is achieved, the main test
phase starts in which all six boxes have dierent
patterns and again the subject has up to 10
attempts to remember which pattern appeared
in which box. The nal scores include number
of trials to success in each phase and number
of pattern-position errors in each and both
phases.
Semantic memory
Category uency. Subjects were asked to produce as many dierent category exemplars
as possible in 1 minute, from the category
animals .
Naming. Subjects were asked to name the 30
line drawings from the Graded Naming Test
described by McKenna & Warrington (1983).
Attentional-executive functioning
Trail Making Test, Parts A and B (Reitan,
1985). Subjects were instructed to sequentially
connect 25 circles on a sheet that contained the
numbers 1 to 25 in Part A, and the numbers 1 to
13 and the letters A to L in Part B. Part A required that individuals connect the circles in
ascending sequence from 1 to 25. Part B required that individuals connect the circles in an
ascending sequence that alternated between
numbers and letters (1, A, 2, B, etc.). The total
number of seconds required to complete Parts A
and B was measured separately.
Letter uency. Subjects were asked to produce
as many words as possible in 1 min that begin
with the letter P.
Visuospatial skills
Copy of the Rey complex gure. As described
above.
Statistics
To assess each patients performance on each
test, we calculated z scores. Patients were considered to be impaired on a test if their scores
were below the 10th percentile of control performance. Dierences in frequency of decits
between groups were analysed using the x2 test.
Group means were compared using independent
sample t tests.
RESULTS
Amnestic MCI : case denition
MCI categorized by Petersens verbal memory
criteria
Of 124 non-demented, non-depressed nonmedical patients, 72 fullled the following
criteria (Petersen et al. 2001 ; Grundman et al.
2004) : (1) memory complaint corroborated by
an informant ; (2) abnormal memory function
documented by total learning across the
ve trials, immediate or delayed recall of the
RAVLT using a 10th percentile cut-o based on
controls ; (3) normal general cognitive function
as determined by the clinician after assessment of the patient and informant interview
plus an MMSE score o24/30 ; (4) minimal
impairment in ADL, as determined by a
clinician interview with the patient and their
informant and CDR score of 0.5 ; (5) not
suciently impaired, cognitively or functionally
to meet NINCDS-ADRDA criteria for probable AD.
MCI categorized by visual memory test
performance
Identical criteria to those applied above were
used, except that performance on the PAL
(six pattern stage) or Rey complex gure was
used to dene amnesia (again based on 10th
percentile scores) rather that the RAVLT.
In total, 50 patients were impaired on the
PAL and 47 patients were impaired on recall
of the Rey gure. Overall, 69 people were
categorized as MCI when performance on
either one of the two visual memory tests was
considered.
Mild cognitive impairment
RAVLT (72)
21
11
16
24
RCF (47)
8
PAL (50)
6
FIG. 2. Overlap in performance on episodic memory tests in mild
cognitive impairment. Numbers in parentheses indicate total number
of patients impaired on the test. RAVLT, Rey Auditory Verbal
Learning Test ; RCF, Rey Complex Figure recall, PAL, Paired
Associates Learning.
MCI categorized by performance any of the
episodic memory tests : verbal/non-verbal
A broader classication of MCI was then used
to include patients in whom performance was
impaired on any of the episodic memory tests
(verbal or non-verbal/visual) and who also
satised the other components of Petersens
criteria. In addition to the 72 who satised
Petersens criteria, based on the RAVLT, an
additional 18 were impaired only on visual
memory tests. Overall, therefore, 90 persons
could be categorized as MCI based on these
broader criteria.
Overlap in performance on memory tests
The overall performance on the episodic
memory measures is shown in Fig. 2. Of the 90
patients showing impairment on one or more
tests, 24 were impaired on all three tests, 31 on
two tests, and 35 on a single memory test
(RAVLT 21, PAL 6 and Rey complex gure 8).
Of the 72 patients dened by Petersens criteria
(based on the RAVLT) the majority (51/72 or
71 %) were also impaired on one of the visual
memory test(s). Conversely, of the 69 patients
with visual memory impairment, 51 (74 %) also
had poor verbal memory performance. Thus, if
dened in terms of impairment on both a verbal
test (RAVLT) and a visual memory test, 51
(41 %) of the total cohort of non-demented,
non-depressed subjects met criteria for MCI.
511
Non-amnestic MCI : case denition
There were 12 patients (9.7 %) who performed
normally on all episodic memory tests but
showed decits on one or more of the nonmemory cognitive tests : three had isolated
semantic impairment, four had attentionalexecutive impairment, one had a visuospatial
decit and four had impairment in more than
one non-memory cognitive domain (see Fig. 1).
Worried well : case denition
Twenty-two patients performed normally on all
episodic memory and non-memory tests and
were categorized as worried well. The mean age
of this group (64.110 years) was signicantly
lower than that of the broad MCI group (n=90,
age 69.78.8 years, p<0.001).
Other cognitive decits in MCI
To address the question of subtle cognitive
decits beyond episodic memory in amnestic
MCI, we compared the performance of the
broadly dened MCI group (n=90) with the
worried well (n=22) on the MMSE, ACE and
the non-amnestic tests (Table 1). The MCI
patients had signicantly lower mean scores on
MMSE, ACE, Trails A and B, Category
uency, Graded Naming and Rey complex
gure copy tasks (p<0.001 for all). There were
no dierences in performance on Letter uency
(Table 1).
We then determined the frequency of cognitive decits in this group based on individual z
scores compared to normal controls. Overall, 64
(71.1 %) of the 90 MCI subjects were found to
have decits in other domains : 24 had semantic
impairment (Category uency and/or Graded
Naming test), 22 had attentional-executive
function decit (Trails and/or Letter uency)
and ve patients had poor visuospatial function
(Rey copy). Thirteen patients had impairment
of three or more cognitive domains (Fig. 2).
Thus only 26 patients from the overall group of
124 non-demented, non-depressed individuals
met strict criteria for pure amnestic MCI
when their performance on an expanded
neuropsychological battery was included in the
algorithm.
To explore whether MCI patients with combined verbal and non-verbal memory impairment had a higher frequency of non-amnestic
cognitive decits, we compared MCI patients
512
S. Alladi et al.
Table 1. Demographic data and performance of worried well and MCI groups on the
neuropsychological test battery
Age (years)
Years of education
NART
MMSE (30)
ACE (100)
Rey Copy (36)
Rey Complex Figure Recall (36)
RAVLT Total Recall (75)
RAVLT Immediate Recall (15)
RAVLT Delayed Recall (15)
PAL 6 errors
Trails A (seconds)
Trails B (seconds)
Category uency
Letter uency
Graded Naming test
Worried well (n=22)
MCI (n=90)
p value
64.1 (10)
12.2 (2.8)
109.6
29.1 (1.2)
92.8 (4.4)
34.7 (1.5)
19.9 (5.1)
46.2 (8.5)
9.0 (2.4)
9.5 (2.8)
4.2 (3.9)
35.7 (10)
96.0 (37)
18.9 (3.9)
15.0 (3.2)
24.3 (3.2)
69.7 (8.8)
12.0 (3.1)
110.7
27.7(1.9)
86.1 (7.4)
31.4 (4.4)
8.6 (6.3)
31.8 (8.4)
4.1 (2.9)
3.9 (3.4)
18.9 (14.6)
51.2 (17.4)
146.9 (87.8)
15.0 (4.8)
14.1 (4.6)
20.1 (2.4)
<0.001
N.S.
N.S.
<0.0001
<0.0001
<0.0001
<0.0001
<0.0001
<0.0001
<0.0001
<0.0001
<0.0001
0.0001
<0.0001
0.33
<0.0001
Values are mean (S.D.). Maximum scores are given in parentheses following the name of each test. The p values are from independent sample
t tests comparing the groups.
MCI, mild cognitive impairment ; NART, National Adult Reading Test ; MMSE, Mini-mental State Examination ; ACE, Addenbrookes
Cognitive Examination; RAVLT, Rey Auditory Verbal Learning Test; PAL, Paired Associates Learning test.
Table 2. Performance of isolated amnesia MCI
and multiple domain MCI groups on memory
tests
RAVLT Total Recall (75)
RAVLT Immediate Recall (15)
RAVLT Delayed Recall (15)
Rey Complex Figure Recall (36)*
PAL 6 errors
MCI
Isolated
amnesia
(n=26)
MCI
Multiple
domains
(n=64)
34.8 (10.7)
5.2 (3.3)
4.9 (3.4)
10.4 (6.4)
14.8 (13.7)
30.4 (8.9)
4.1 (3)
3.5 (3.2)
7.1 (6.1)
20.8 (14.7)
Values are mean (S.D.). Maximum scores are given in parentheses
following the name of each test.
MCI, Mild cognitive impairment ; RAVLT, Rey Auditory Verbal
Learning Test ; PAL, Paired Associates Learning test.
* Independent sample t test, p<0.05.
who only had a single (either verbal or visual)
modality with those who had combined memory
impairment : 23 (59 %) of 39 patients with
single-modality memory impairment (verbal or
visual) and 41 (80 %) of 51 with both verbal and
visual memory impairment had non-amnestic
decits. This dierence was statistically signicant (p=0.016).
To explore the hypothesis that those with
multi-domain MCI have more advanced disease, and hence a greater degree of amnesia, we
compared memory performance in those with
isolated amnesia (n=26) and multi-domain
MCI (n=64) (Table 2). Although there was a
trend for worse memory in the multi-domain
group, this dierence reached signicance for
only the Rey gure recall (p<0.05), and not the
other four measures.
DISCUSSION
In this study we have shown that a large proportion (72 of 124, 60%) of non-depressed, nondemented older individuals with mild memory
complaints fullled MCI research criteria, suggesting that the criteria proposed by Petersen
et al. (1999, 2001) have broad applicability in
clinical practice. The actual number of people
categorized as MCI varied considerably depending upon the choice and combination of
memory tests used. In addition, using standard
neuropsychological tests, we were able to
demonstrate cognitive decits beyond episodic
memory in the majority of MCI subjects. Of note
was the nding that only 26 (21 %) had pure
amnestic MCI if all those with additional, albeit
subtle, non-memory decits were excluded. A
small group (n=12, 10%) with non-amnestic
cognitive impairment was also identied.
Although almost 60 % of cases met Petersens
MCI criteria, it should be noted that tertiary
referrals (from other consultants) were excluded
Mild cognitive impairment
from the study and that the memory clinic is
neurology led, so that older patients with more
established cognitive decits tend not to be
referred. When performance on either verbal or
visual memory tests was considered in dening
amnesia, the inclusion rate of MCI went up to
73 % (90/124). If impairment on both a verbal
and a visual test was used to classify cases, the
detection rate fell to 41% (51/124). Diagnosis of
MCI has conventionally been based on performance on verbal memory tests in view of their
proposed accuracy in predicting conversion to
AD in the pre-clinical phase (Flicker et al. 1991;
Tierney et al. 1996 ; Petersen et al. 1999 ; Albert
et al. 2001; De Jager et al. 2003 ; EstevezGonzalez et al. 2003). However, although visual
memory impairment can pre-date clinical AD
by a long period (Kawas et al. 2003), this aspect
has received comparatively less attention.
Results from a longitudinal study of questionable dementia suggested that the pattern-spatial
PAL test, from the computerized CANTAB
battery, predicts patients who will convert to
AD with a very high degree of accuracy
(Swainson et al. 2001 ; Blackwell et al. 2004). We
identied 50 patients with impairment on the
shortened version of the PAL test, of whom 40
(80 %) also had verbal memory decits. We also
identied 49 patients who were impaired on delayed recall of the Rey complex gure, of whom
40 (89 %) also had verbal memory decits.
Although these results illustrate that there is
reasonable concordance between verbal and
visual memory impairment, they also indicate
that a sizeable minority of cases with objective
evidence of memory impairment would not be
captured when this evidence is only sought from
a verbal memory test. Furthermore, there is no
evidence at present to suggest that visual memory impairment is a less ominous predictor of
decline to AD than is verbal memory impairment. As such, the results suggest that approximately 20% of cases may be inappropriately
excluded from the category of amnestic MCI,
where episodic memory sampling is restricted to
the verbal domain. This result conrms, in a
larger sample, the nding of a previous study
that found isolated visual memory impairment
in 9/29 MCI subjects (De Jager et al 2003).
Addressing further the issue of overlap in
performance on memory tests, a signicant
proportion of subjects (55/90) were impaired on
513
more than one memory test : 31 performed
poorly on two tests and 24 on all three episodic
memory tests. A similar prole was found in
a community-based study assessing cognitive
performance among older people (De Jager
& Budge, 2005). Because isolated impairment
on a single memory test may be due to nonspecic processes such as mood disturbance or
performance anxiety, it is likely that subjects
with a poor performance on more than one test
have more stable memory impairment. The
other possibility is that people with impairment
conned to one memory domain have earlier
stage disease than those with combined decits
a hypothesis supported by the observation that
impairment across multiple memory tests is
typical of established AD (De Jager et al. 2003).
Regarding the purity of amnesia in MCI as
dened by Petersens criteria our study demonstrated that MCI is frequently associated
with more general cognitive impairment. Furthermore, these decits were readily detectable
on standard clinical neuropsychological tests.
Among those with additional decits we identied three distinct sub-groups : a group with
attentional-executive dysfunction, another that
had semantic impairment, and a third, smaller
group, with visuospatial involvement. A proportion showed impairment in three or
more domains. This pattern resembles wellrecognized cognitive variants described in early
AD (Perry & Hodges, 2000; Perry et al. 2000 ;
Lambon-Ralph et al. 2003). Furthermore, multiple domain MCI was more common in
patients with combined visual and verbal memory impairment. It is likely that these cases in
whom the cognitive decit prole was qualitatively, though not quantitatively, consistent was
AD will be the rst to meet clinical criteria for
dementia. Longitudinal follow-up is under way
to test this hypothesis.
Petersens criteria recommend that general
cognitive impairment be excluded on the basis
of the MMSE and the clinicians judgement. It is
clear from our study that these criteria are insuciently robust to identify a purely amnestic
group and that most subjects have multiple
cognitive decits when non-amnestic cognitive
abilities are formally examined. If we exclude
people with other cognitive decits on the basis
of neuropsychological tests, the number of
patients categorized as MCI is radically reduced
514
S. Alladi et al.
(from 90 to 25 in the current sample). It is unclear whether this pure sub-group represents an
earlier disease stage or a more unstable group
with a lower risk of later developing dementia.
The group of patients in our study who have
normal performance on memory tests while
being impaired in other cognitive domains
(non-amnestic MCI) is of particular interest. At
present, considerably less is known of the longterm signicance of non-amnestic, compared to
amnestic, MCI. Our results indicate that it is an
important group for further study, in that cases
were readily identiable in this clinic-based
sample, occurring in a ratio of 1 : 6 compared
to those who met Petersen criteria. This ratio,
in itself, provides an interesting contrast to
population-based cohorts in which the ratio
may be biased in the opposite direction. Using
neuropsychological cut-os of >1.5 S.D. below
controls, Busse et al. (2003) reported a population-based prevalence of 2.5 % for amnestic
MCI and 4.2% for non-amnestic MCI. They
also reported that the latter group had a better
long-term prognosis. This may suggest that the
bias towards amnestic MCI in a symptomatic
clinic-based cohort is indicative of this prole
being more likely in cases with incipient AD.
Nevertheless, atypical AD syndromes with nonamnestic presentations are well recognized,
although their prevalence compared to typical
AD is uncertain (Galton et al. 2000). The nonamnestic MCI group may progress to atypical
AD or, alternatively, be in the early stages of a
non-AD dementia syndrome. The commonest
non-amnestic decit identied in these cases was
in the domain of attention and executive function, suggesting that depression or test performance anxiety may also be a contributing
factor. Depression was an exclusion criterion in
the present study, although as executive dysfunction can be a feature of minor depression in
elderly individuals (Elderkin-Thompson et al.
2003), it is possible that sub-clinical depressive
illness may also be a contributing factor.
In conclusion, when Petersens criteria for
MCI were applied to a memory clinic cohort,
several potentially important issues in case denition were identied. First, when the objective
measure of memory impairment was changed
from a verbal to a non-verbal measure, a signicant minority of cases were captured that
were not identied by a verbal memory test.
Many cases exhibited both verbal and nonverbal memory impairment, suggesting a more
pervasive and possibly a more sinister decit.
However, when a single test is used, the results
indicate that a non-verbal homologue to the
verbal memory impairment proposed in a literal
application of the Petersen criteria also exists.
Second, when non-amnestic decits are formally
examined, the number of cases with pure
amnestic MCI was radically attenuated. The
corollary of this nding was that many cases
classied as MCI by Petersens criteria exhibit a
neuropsychological prole that, although subtle, is consistent with that seen in probable AD.
This raises the question of whether such cases
already exhibit sucient evidence for a diagnosis of probable AD a proposition that needs
testing with longitudinal follow-up. Finally, the
study identied a group with non-amnestic MCI
whose signicance is particularly uncertain at
this time. Overall, the present results illustrate
that, without straying from the boundaries of
the MCI operational criteria, varying the neuropsychological parameters can have a signicant
impact on case denition. It is likely that this
variability has implications for the long-term
fate of individual subjects.
DECLARATION OF INTEREST
None.
REFERENCES
Albert, M. S., Moss, M. B., Tanzi, R. & Jones, K. (2001). Preclinical
prediction of AD using neuropsychological tests. Journal of the
International Neuropsychological Society 7, 631639.
Bak, T. H., Rogers, T. T., Crawford, L. M., Hearn, V. C.,
Mathuranath, P. S. & Hodges, J. R. (2005). Cognitive bedside
assessment in atypical parkinsonian syndromes. Journal of
Neurology, Neurosurgery, and Psychiatry 76, 420422.
Blackwell, A. D., Sahakian, B. J., Vesey, R., Semple, J. M., Robbins,
T. W. & Hodges, J. R. (2004). Detecting dementia : novel neuropsychological markers of pre-clinical Alzheimers disease.
Dementia and Geriatric Cognitive Disorders 17, 4248.
Bowen, J., Teri, L., Kukull, W., McCormick, W., McCurry, S. M. &
Larson, E. B. (1997). Progression to dementia in patients with
isolated memory loss. Lancet 349, 763765.
Bozoki, A., Giordani, B., Heidebrink, J. L., Berent, S. & Foster, N. L.
(2001). Mild cognitive impairments predict dementia in nondemented elderly patients with memory loss. Archives of Neurology
58, 411416.
Busse, A., Bischkopf, J., Reidel-Heller, S. G. & Angermeyer, M. C.
(2003). Subclassications for mild cognitive impairment : prevalence and predictive validity. Psychological Medicine 33,
10291038.
Chertkow, H. (2002). Mild cognitive impairment. Current Opinion in
Neurology 15, 401407.
Mild cognitive impairment
De Jager, C. A. & Budge, M. M. (2005). Stability and predictability
of the classication of mild cognitive impairment as assessed by
episodic memory test performance over time. Neurocase 11, 7279.
De Jager, C. A., Hogervorst, E., Combrinck, M. & Budge, M. M.
(2003). Sensitivity and specicity of neuropsychological tests for
mild cognitive impairment, vascular cognitive impairment and
Alzheimers disease. Psychological Medicine 33, 10391050.
Devanand, D. P., Folz, M., Gorlyn, M., Moeller, J. R. & Stern, Y.
(1997). Questionable dementia : clinical course and predictors of
outcome. Journal of the American Geriatrics Society 45, 321328.
Dubois, B. & Albert, M. L. (2004). Amnestic MCI or prodromal
Alzheimers disease ? Lancet Neurology 3, 246248.
Dudas, R. B., Berrios, G. E. & Hodges, J. R. (2005). The
Addenbrookes Cognitive Examination (ACE) in the dierential
diagnosis of early organic dementias from aective disorder.
American Journal of Geriatric Psychiatry 13, 218226.
Elderkin-Thompson, V., Kumar, V., Bilker, W. B., Dunkin, J. J.,
Mintz, J., Moberg, P. J., Mesholam, R. I. & Gure, R. E. (2003).
Neuropsychological decits among patients with late-onset minor
and major depression. Archives of Clinical Neuropsychology
18, 529549.
Estevez-Gonzalez, A., Kulisevsky, J., Boltes, A., Otermin, P. &
Garcia-Sanchez, C. (2003). Rey verbal learning test is a useful
tool for dierential diagnosis in the preclinical phase of
Alzheimers disease : comparison with mild cognitive impairment
and normal aging. International Journal of Geriatric Psychiatry
18, 10211028.
Flicker, C., Feris, S. & Reisberg, B. (1991). Mild cognitive impairment in the elderly : predictors of dementia. Neurology 41, 1006
1009.
Folstein, M. F., Folstein, S. E. & McHugh, P. R. (1975). Minimental state. A practical method for grading the cognitive state
of patients for the clinician. Journal of Psychiatric Research 12,
189198.
Fowler, K. S., Saling, M. M., Conway, E. L., Semple, J. M. & Louis,
W. J. (1995). Computerized delayed matching to sample and
paired associate performance in the early detection of dementia.
Applied Neuropsychology 2, 7278.
Galton, C. J., Patterson, K., Xuereb, J. H. & Hodges, J. R. (2000).
Atypical and typical presentations of Alzheimers disease: a clinical, neuropsychological, neuroimaging and pathological study of
13 cases. Brain 123, 484498.
Grundman, M., Petersen, R. C., Ferris, S. H., Thomas, R. G., Aisen,
P. S., Bennett, D. A., Foster, N. L., Jack, C. R. J., Galasko, D. R.,
Doody, R. S., Kaye, J., Sano, M., Mohs, R., Gauthier, S., Kim,
H. T., Jin, S., Schultz, A. N., Schafer, K., Mulnard, R., van Dyck,
C. H., Mintzer, J., Zamrini, E. Y., Cahn-Weiner, D. & Thal, L. J.
(2004). Mild cognitive impairment can be distinguished from
Alzheimer disease and normal aging for clinical trials. Archives of
Neurology 61, 5966.
Kawas, C. H., Corrada, M. M., Brookmeyer, R., Morrison, A.,
Resnick, S. M., Zonderman, A. B. & Arenberg, D. (2003). Visual
memory predicts Alzheimers disease more than a decade before
diagnosis. Neurology 60, 10891093.
Lambon-Ralph, M. A., Patterson, K., Graham, N., Dawson, K. &
Hodges, J. R. (2003). Homogeneity and heterogeneity in mild
515
cognitive impairment and Alzheimers disease : a cross-sectional
and longitudinal study of 55 cases. Brain 126, 23502362.
Luis, C. A., Loewenstein, D. A., Acevedo, A., Barker, W. W. &
Duara, R. (2003). Mild cognitive impairment : directions for future
research. Neurology 61, 438444.
Mathuranath, P. S., Nestor, P., Berrios, G. E., Rakowicz, W. &
Hodges, J. R. (2000). A brief cognitive test battery to dierentiate
Alzheimers disease and frontotemporal dementia. Neurology
55, 16131620.
McKenna, P. & Warrington, E. K. (1983). Graded Naming Test.
NFER-Nelson: Windsor.
Morris, J. C. (1993). The Clinical Dementia Rating (CDR) : current
version and scoring rules. Neurology 43, 24122414.
Nelson, H. & Willison, J. (1991). The National Adult Reading Test
(NART). NFER-Nelson: Windsor.
Nestor, P. J., Scheltens, P. & Hodges, J. R. (2004). Advances in the
early detection of Alzheimers disease. Nature Medicine 10, S34
S41.
Perry, R. J. & Hodges, J. R. (2000). Fate of patients with questionable (very mild) Alzheimers disease: longitudinal proles of
individual subjects decline. Dementia and Geriatric Cognitive
Disorders 11, 342349.
Perry, R. J., Watson, P. & Hodges, J. R. (2000). The nature and
staging of attention dysfunction in early (minimal and mild)
Alzheimers disease : relationship to episodic and semantic memory impairment. Neuropsychologia 38, 252271.
Petersen, R. C., Doody, R., Kurz, A., Mohs, R. C., Morris, J. C.,
Rabins, P. V., Ritchie, K., Rossor, M., Thal, L. & Winblad, B.
(2001). Current concepts in mild cognitive impairment. Archives of
Neurology 58, 19851992.
Petersen, R. C., Smith, G. E., Waring, S. C., Ivnik, R. J., Tangalos,
E. G. & Kokmen, E. (1999). Mild cognitive impairment : clinical
characterization and outcome. Archives of Neurology 56, 303308.
Quraishi, S. & Frangou, S. (2002). Neuropsychology of bipolar
disorder : a review. Journal of Aective Disorders 72, 209226.
Reitan, R. M. (1985). HalsteadReitan Neuropsychological Test
Battery. Reitan Neuropsychology Laboratory/Press : Tuscon.
Rey, A. (1941). Psychological examination of a case of posttraumatic encephalopathy [in French]. Archives de Psychologie 28,
286340.
Ritchie, K., Artero, S. & Touchon, J. (2001). Classication criteria for
mild cognitive impairment a population-based validation study.
Neurology 56, 3742.
Schmidt, M. (1996). Rey Auditory Verbal Learning Test : A Handbook. Western Psychological Services : Los Angeles.
Snaith, R. P. (1994). HADS : Hospital Anxiety and Depression Scale.
NFER-Nelson: Windsor.
Swainson, R., Hodges, J. R., Galton, C. J., Semple, J., Michael, A.,
Dunn, B. D., Iddon, J. L., Robbins, T. W. & Sahakian, B. J. (2001).
Early detection and dierential diagnosis of Alzheimers disease
and depression with neuropsychological tasks. Dementia and
Geriatric Cognitive Disorders 12, 265280.
Tierney, M. C., Szalai, J. P., Snow, W. G., Fisher, R. H., Nores, A.,
Nadon, G., Dunn, E. & St George Hyslop, P. H. (1996). Prediction
of probable Alzheimers disease in memory-impaired patients a
prospective longitudinal study. Neurology 46, 661665.
Você também pode gostar
- Neuropsychology and Neuropsychiatry of Neurodegenerative DisordersDocumento192 páginasNeuropsychology and Neuropsychiatry of Neurodegenerative DisordersIcaroAinda não há avaliações
- Kos Toulas 2017Documento11 páginasKos Toulas 2017IcaroAinda não há avaliações
- Luria's Three-Step Test: What Is It and What Does It Tell Us?Documento5 páginasLuria's Three-Step Test: What Is It and What Does It Tell Us?IcaroAinda não há avaliações
- Using Latent Class Analysis To Model Prescription Medications in The Measurement of Falling Among A Community Elderly PopulationDocumento7 páginasUsing Latent Class Analysis To Model Prescription Medications in The Measurement of Falling Among A Community Elderly PopulationIcaroAinda não há avaliações
- Indications For NeuropsychologicalDocumento5 páginasIndications For NeuropsychologicalIcaroAinda não há avaliações
- Informed Consent in Clinical Neuropsychology Practice Official Statement of The National Academy of NeuropsychologyDocumento6 páginasInformed Consent in Clinical Neuropsychology Practice Official Statement of The National Academy of NeuropsychologyIcaroAinda não há avaliações
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceNo EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceNota: 4 de 5 estrelas4/5 (895)
- Never Split the Difference: Negotiating As If Your Life Depended On ItNo EverandNever Split the Difference: Negotiating As If Your Life Depended On ItNota: 4.5 de 5 estrelas4.5/5 (838)
- The Yellow House: A Memoir (2019 National Book Award Winner)No EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Nota: 4 de 5 estrelas4/5 (98)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeNo EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeNota: 4 de 5 estrelas4/5 (5794)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaNo EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaNota: 4.5 de 5 estrelas4.5/5 (266)
- The Little Book of Hygge: Danish Secrets to Happy LivingNo EverandThe Little Book of Hygge: Danish Secrets to Happy LivingNota: 3.5 de 5 estrelas3.5/5 (400)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureNo EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureNota: 4.5 de 5 estrelas4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryNo EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryNota: 3.5 de 5 estrelas3.5/5 (231)
- The Emperor of All Maladies: A Biography of CancerNo EverandThe Emperor of All Maladies: A Biography of CancerNota: 4.5 de 5 estrelas4.5/5 (271)
- The Unwinding: An Inner History of the New AmericaNo EverandThe Unwinding: An Inner History of the New AmericaNota: 4 de 5 estrelas4/5 (45)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersNo EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersNota: 4.5 de 5 estrelas4.5/5 (345)
- Team of Rivals: The Political Genius of Abraham LincolnNo EverandTeam of Rivals: The Political Genius of Abraham LincolnNota: 4.5 de 5 estrelas4.5/5 (234)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreNo EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreNota: 4 de 5 estrelas4/5 (1090)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyNo EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyNota: 3.5 de 5 estrelas3.5/5 (2259)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)No EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Nota: 4.5 de 5 estrelas4.5/5 (121)
- Basal Cell Carcinoma With Lymph Node Metastasis A Case Report and Review of LiteratureDocumento5 páginasBasal Cell Carcinoma With Lymph Node Metastasis A Case Report and Review of LiteratureIJAR JOURNALAinda não há avaliações
- Case Study On RDS - NicuDocumento32 páginasCase Study On RDS - NicuGandimarei89% (19)
- 358 Muhammad Zul SikkDocumento3 páginas358 Muhammad Zul SikkMar Yana MamehAinda não há avaliações
- Antimicrobial FinalDocumento227 páginasAntimicrobial FinalAbdulrhman MekawyAinda não há avaliações
- Group 6 Part 1 Review of The Aging of Physiological System Notes Part 1Documento7 páginasGroup 6 Part 1 Review of The Aging of Physiological System Notes Part 1Crissan Jejomar AbanesAinda não há avaliações
- Nikki CV FormatedDocumento2 páginasNikki CV FormatedSaif AlamAinda não há avaliações
- Lesi Prakanker & Tumor Ginekologi (Versi 2003)Documento71 páginasLesi Prakanker & Tumor Ginekologi (Versi 2003)Satwika EkanandaAinda não há avaliações
- Hand Foot & Mouth DiseaseDocumento23 páginasHand Foot & Mouth DiseaseKabang Moa100% (1)
- 3.4-Behar Anorexia y MadurezDocumento10 páginas3.4-Behar Anorexia y MadurezAlejandra CarmonaAinda não há avaliações
- Sample Sba Questions GynaecologyDocumento6 páginasSample Sba Questions GynaecologyIshola Segun SamuelAinda não há avaliações
- Regine Choe PDFDocumento248 páginasRegine Choe PDFdavoodibrahimAinda não há avaliações
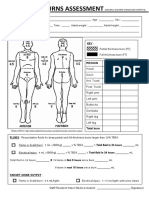
- Burn Assessment CMU PDFDocumento2 páginasBurn Assessment CMU PDFmegamindAinda não há avaliações
- The Study of Drug Resistance in Bacteria Using Antibiotics: June 2019Documento6 páginasThe Study of Drug Resistance in Bacteria Using Antibiotics: June 20197'A'06Aditya BeheraAinda não há avaliações
- Complete DenturesDocumento68 páginasComplete DenturesRaja Rahaizat100% (2)
- CV For FellowshipDocumento3 páginasCV For Fellowshipapi-568710214Ainda não há avaliações
- Drug StudyDocumento7 páginasDrug Studyanne009Ainda não há avaliações
- Things To Read: A. Trauma: Fractures and DislocationsDocumento4 páginasThings To Read: A. Trauma: Fractures and DislocationsHanien YeeAinda não há avaliações
- 345-Article Text-1032-1-10-20180629Documento4 páginas345-Article Text-1032-1-10-20180629Regina AyediaAinda não há avaliações
- 04 Tetanus BDocumento12 páginas04 Tetanus BRahmatul YasiroAinda não há avaliações
- 5 Amiodarona ArticlesDocumento36 páginas5 Amiodarona ArticlesSacrificiuPopescuAinda não há avaliações
- Bahasa Inggris - NurfadilahDocumento6 páginasBahasa Inggris - NurfadilahHardianiAinda não há avaliações
- Skin Assessment FormDocumento2 páginasSkin Assessment FormOng KarlAinda não há avaliações
- Safe Sedation For All Practitioners A Practical GuideDocumento190 páginasSafe Sedation For All Practitioners A Practical Guidemonir61Ainda não há avaliações
- Treatment of Dengue Joe de LiveraDocumento11 páginasTreatment of Dengue Joe de Liverakrishna2205100% (1)
- Nclex PointersDocumento4 páginasNclex PointersCarl Michael de Guzman75% (12)
- Pharma - 2020 General Principles of Drug ActionDocumento163 páginasPharma - 2020 General Principles of Drug Actiongelean payodAinda não há avaliações
- Mycoplasma GallicepticumDocumento18 páginasMycoplasma GallicepticumRoni FaturrahmanAinda não há avaliações
- Bacterial Sinusitis in Children: AcuteDocumento11 páginasBacterial Sinusitis in Children: AcutefriscahalimAinda não há avaliações
- Bhs InggrisDocumento4 páginasBhs InggrisNUR WULAN SARIAinda não há avaliações
- Ajor Epressive Isorder: Marshall Cates, Angela Passero, and Jacqueline FeldmanDocumento16 páginasAjor Epressive Isorder: Marshall Cates, Angela Passero, and Jacqueline FeldmanbencleeseAinda não há avaliações