Escolar Documentos
Profissional Documentos
Cultura Documentos
A Surprising Cause of Chronic Cough
Enviado por
Jhonnathan RodriguezDireitos autorais
Formatos disponíveis
Compartilhar este documento
Compartilhar ou incorporar documento
Você considera este documento útil?
Este conteúdo é inapropriado?
Denunciar este documentoDireitos autorais:
Formatos disponíveis
A Surprising Cause of Chronic Cough
Enviado por
Jhonnathan RodriguezDireitos autorais:
Formatos disponíveis
The
n e w e ng l a n d j o u r na l
of
m e dic i n e
Clinical Problem-Solving
CarenG. Solomon, M.D., M.P.H., Editor
A Surprising Cause of Chronic Cough
Deepti Damaraju, M.D., Ted Steiner, M.D., John Wade, M.D., Kenneth Gin, M.D.,
and J.Mark FitzGerald, M.B., M.D.
In this Journal feature, information about a real patient is presented in stages (boldface type) to an expert
clinician, who responds to the information, sharing his or her reasoning with the reader (regular type).
The authors commentary follows.
A 63-year-old nonsmoking white man presented to the clinic with a 2-year history of
cough. The cough was dry, and it was worse at night. The cough had begun after an
upper respiratory tract infection and a trip to South America. The patient was prescribed antibiotics by a family physician but had no improvement; he was then given
a combination inhaler (salmeterol and fluticasone) and had minimal improvement.
This patient has chronic cough, which is defined as a cough lasting more than
8 weeks. In a nonsmoker, the most common causes are the upper-airway cough
syndrome (allergic, nonallergic, or infectious), asthma, and gastroesophageal reflux disease (GERD). This patient has features suggestive of GERD or the upperairway cough syndrome after an upper respiratory tract infection. Although the
long duration of cough may suggest mild asthma, this condition should have
improved substantially with the correct use of a combination inhaler.
From the Department of Medicine, University of British Columbia, Vancouver,
Canada. Address reprint requests to Dr.
Damaraju at 5288 Melbourne St., Apt. 1702,
Vancouver, BC V5R 6E6, Canada, or at
deepti.damaraju@gmail.com.
N Engl J Med 2015;373:561-6.
DOI: 10.1056/NEJMcps1303787
Copyright 2015 Massachusetts Medical Society.
The patients medical history included at least 5 years of intermittent arthralgias and
myalgias and a 2-year history of night sweats (now resolved) before this presentation.
The arthralgias occurred in his neck, shoulders, wrists, hands, hips, and ankles;
episodes would last 2 weeks on average, followed by complete recovery. He was assessed by a rheumatologist during the first 2 years after the onset of these symptoms
and had negative results on tests for antinuclear antibody (rheumatoid factor, extractable nuclear antigens, and anticyclic citrullinated peptide antibodies) and
HLA-B27. A tuberculin skin test, chest radiography, and ultrasonography of the abdomen were also negative. Additional medical history included pitting edema in the
lower limbs bilaterally for the past 2 years (attributed to venous stasis), for which the
patient used compression stockings. There was no other clinically significant medical history. The patient had never smoked, and he drank minimal amounts of alcohol.
He had no pets. His only medications were the inhaler and ibuprofen (as needed).
Given the absence of allergies or history of rhinitis, the upper-airway cough syndrome is less likely. Ibuprofen may be a risk factor for bronchospasm or nasal
congestion in a patient with asthma and rhinosinusitis with nasal polyps. This
patients history of night sweats and arthralgias may relate to his current presentation, but this remains unclear. He does not have additional findings to suggest
sarcoidosis, such as a history of erythema nodosum or hilar adenopathy.
Asthma or GERD remains a likely cause of his cough, although imaging is
warranted to assess for parenchymal lung disease. If the patient has asthma, it
n engl j med 373;6nejm.org August 6, 2015
The New England Journal of Medicine
Downloaded from nejm.org on August 8, 2015. For personal use only. No other uses without permission.
Copyright 2015 Massachusetts Medical Society. All rights reserved.
561
The
n e w e ng l a n d j o u r na l
may be incompletely responsive to inhaled medication for several reasons (incorrect inhaler technique, inadequate adherence to therapy, poor
avoidance of triggers, the presence of vocalcord dysfunction, or untreated nasal symptoms).
Spirometry and chest imaging should be ordered
to assess for parenchymal lung disease.
m e dic i n e
The normal flow-volume loop rules out clinical
ly significant fixed obstruction (from vocal-cord
dysfunction or a mass). A methacholine challenge in this context, with the use of a cutoff
value of 8 to 16 mg per milliliter for the concentration of methacholine required to reduce the
FEV1 by 20%, has a high negative predictive
value; the negative results (i.e., fall in FEV1 of
<20% with maximal challenge) makes a diagnosis of asthma highly unlikely.
In this patient, GERD appears to be the next
most likely cause. A 24-hour pH monitor could be
considered. Alternatively, a trial of therapy with
a proton-pump inhibitor would be reasonable.
headache developed that lasted for 2 days, and the
patient had transient binocular vision loss, for
which he was evaluated at an outside emergency
department. He had an elevated C-reactive protein
level (44.7 mg per liter; normal value, <3.0 mg per
liter) and erythrocyte sedimentation rate (69 mm
per hour; normal value, <25 mm per hour). His
hemoglobin level was 13.5 g per deciliter, and
the white-cell count was 8.7103 per cubic millimeter (neutrophils 7.3103 per cubic millimeter,
lymphocytes 0.9103 per cubic millimeter, monocytes 0.3103 per cubic millimeter, and eosinophils
0.2103 per cubic millimeter). Electrolyte and creatinine levels were normal. A CT scan of the head
was normal. A presumptive diagnosis of temporal
arteritis and polymyalgia rheumatica was made.
The patient began taking prednisone (at a dose of
60 mg daily) and was referred to a rheumatologist.
The headache resolved in 2 days, and the visual
loss did not recur. A temporal-artery biopsy several weeks later was negative for vasculitis. Given
the rapid resolution of his neurologic symptoms
while he was taking prednisone, the patient continued taking this medication and was followed
for several months. He noted a marked reduction
in his chronic arthralgias and myalgias and slight
abatement of his cough and long-standing peripheral edema. With tapering to a dose of 10 mg
per day, however, his cough and arthralgias worsened (with no recurrence of neurologic symptoms). He was again referred to his original pulmonologist.
The patient declined pH monitoring but agreed to
try a proton-pump inhibitor. However, he did not
return for follow-up.
Three years later, he returned and reported new
symptoms that had been present for 6 months.
These symptoms began with intense gas pain,
bloating, and small-volume diarrhea; the diarrhea
decreased spontaneously over a period of 6 weeks,
and the gas and bloating decreased after several
months, which he attributed to increased dietary
fiber intake. Two months after the initial development of gastrointestinal symptoms, he had sudden severe leg pain and difficulty walking. Although the severe pain resolved within days, he
continued to have myalgias and arthralgias as well
as intermittent cough, which he noted had not
abated with the use of a proton-pump inhibitor.
One month after the episode of leg pain, a severe
Patients with giant-cell arteritis can have a nonproductive cough that is caused by vasculitic
involvement of airways. This patients cough
worsened as prednisone was tapered, which suggested a possible underlying inflammatory cause
(such as eosinophilic bronchitis, a pulmonary vas
culitis, or, less likely, an interstitial pneumonitis).
False negative results on biopsies may occur in
patients with temporal arteritis. In cases in which
the biopsy is negative, the clinical suspicion for
temporal arteritis must be weighed against the
risks of glucocorticoid use (e.g., worsening of occult infection, impaired glucose tolerance, bone
loss, and avascular necrosis). Alternative diagnoses should continue to be considered, with the
understanding that patients without temporal
arteritis may also report improvement while taking prednisone.
Spirometry, including the flow-volume loop, was
normal. A methacholine challenge was negative;
with sequential inhalations up to 16 mg per milliliter, the fall in the forced expiratory volume in
1 second (FEV1) was 9% (final FEV1, 3.60 liters,
which was 89% of the predicted level). A computed tomographic (CT) scan of the chest showed
mild bronchiectasis and no other clinically significant abnormality.
562
of
n engl j med 373;6nejm.org August 6, 2015
The New England Journal of Medicine
Downloaded from nejm.org on August 8, 2015. For personal use only. No other uses without permission.
Copyright 2015 Massachusetts Medical Society. All rights reserved.
Clinical Problem-Solving
13.0 mm
9.8 mm
8.2 mm
16.1 mm
10.7 mm
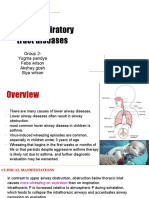
Figure 1. Computed Tomographic Scan of the Abdomen.
Coronal sections show enlarged and borderline mesenteric lymph nodes, with indicated measurements.
phoma, was referred for exploratory laparotomy
and excisional lymph-node biopsy. Microbiologic
testing of the sample revealed gram-positive bacilli, which prompted the laboratory to investigate
for possible Whipples disease. Direct 16S gene
sequencing detected Tropheryma whipplei DNA.
Pathological findings from the lymph-node biopsy
showed granulomatous inflammation with numerous foamy histiocytes (Fig. 2). Organisms that
were positive on periodic acidSchiff staining
The findings on the CT scan of the abdomen may were present and had morphologic features consuggest a lymphoproliferative disease or other sistent with those of T. whipplei. Blood cultures
cancer involving the jejunum. Lymphadenopathy were negative.
may also be explained by infection, including
tuberculosis; the prior negative tuberculin skin Whipples disease provides a unifying diagnosis
test does not rule out tuberculosis, because this for this patients presentation, including the
testing is often negative in patients with dis- chronic arthropathy, cough, lymphadenopathy,
seminated tuberculosis. The patient should be and lymphopenia. The diagnosis could have
examined for peripheral adenopathy to identify been made by less invasive means (i.e., smallnodes that would be amenable to biopsy. The bowel endoscopy) had it been suspected preopfindings on the CT scan of the chest may indi- eratively. The absence of chronic diarrhea in this
cate heart failure and warrant further evaluation, case is atypical for Whipples disease.
including assessment for cardiomyopathy or
The infectious disease service was consulted, and
valvular disease.
it was recommended that the patient receive intraThe patient had no palpable peripheral adenopa- venous ceftriaxone for 2 weeks, followed by oral
thy and, given a high clinical suspicion of lym- trimethoprimsulfamethoxazole at a dose of one
A CT scan of the chest and abdomen showed mild
interstitial pulmonary edema and small bilateral
pleural effusions. The main pulmonary artery
was enlarged at 30.9 mm in diameter, and there
was a small pericardial effusion. There was extensive abdominal lymphadenopathy, which was
considered to be a potential marker of lymphoma,
as well as a region of poorly distended proximal
jejunum that appeared to be thickened (Fig. 1).
n engl j med 373;6
nejm.org
August 6, 2015
The New England Journal of Medicine
Downloaded from nejm.org on August 8, 2015. For personal use only. No other uses without permission.
Copyright 2015 Massachusetts Medical Society. All rights reserved.
563
The
n e w e ng l a n d j o u r na l
of
m e dic i n e
Figure 2. Pathological Findings.
The low-power photomicrograph in Panel A shows a markedly abnormal intraabdominal lymph node in which the
normal architecture has been replaced by numerous macrophages, many of which are foamy, and occasional giant
cells (hematoxylin and eosin). The high-power photomicrograph in Panel B shows foamy macrophages with granular
eosinophilic cytoplasm (hematoxylin and eosin). Panel C (periodic acidSchiff stain) and Panel D (WarthinStarry
silver stain) show numerous intracytoplasmic organisms, with morphologic features consistent with those of Tropheryma whipplei.
Videos showing
echocardiograms
are available at
NEJM.org
564
double-strength tablet (160 mg of trimethoprim
and 800 mg of sulfamethoxazole) twice daily. The
prednisone was tapered and subsequently discontinued. At follow-up 2 weeks later, the patient was
found to have a systolic murmur, which had not
been noted previously. An echocardiogram showed
a mobile mass measuring 7 mm in length by 6 mm
in width on the left ventricular surface of a bicuspid aortic valve, with mild aortic stenosis and
moderate aortic insufficiency; systolic pulmonary-artery pressures could not be estimated
(Fig. 3 and Video 1). He had no fevers, cardiac
symptoms, or embolic phenomena of endocarditis. Three blood cultures were negative.
The patient was referred for assessment to a
cardiologist, who considered the vegetation to be
a likely complication of Whipples disease and
n engl j med 373;6
Left atrium
Mitral valve
Vegetation
Left ventricle
Aorta
Aortic valve
Figure 3. Transesophageal Echocardiogram.
A mobile vegetative mass is seen on the noncoronary
cusp of the aortic valve.
nejm.org
August 6, 2015
The New England Journal of Medicine
Downloaded from nejm.org on August 8, 2015. For personal use only. No other uses without permission.
Copyright 2015 Massachusetts Medical Society. All rights reserved.
Clinical Problem-Solving
who recommended follow-up with antibiotic therapy. The patient reported resolution of his cough,
peripheral edema, arthralgias, myalgias, and fatigue in the 2 months after the initiation of antibiotic therapy. Serial echocardiograms showed
resolution of the vegetation by the sixth month of
therapy, with stable valvular regurgitation (Fig.4
and Video 2).
It is possible that the transient vision loss earlier
may have been embolic in nature in association
with endocarditis (although vision loss in this
context would be much less likely to be bilateral
than unilateral). The resolution of the patients
cough and other symptoms, as well as the valvular vegetation, with antibiotic therapy supports
the conclusion that these were attributable to
Whipples disease.
C om men ta r y
Chronic cough lasting more than 8 weeks is
common and most often caused by bronchospasm, GERD, eosinophilic bronchitis, or the
upper-airway cough syndrome (postnasal drip).1,2
These were not the culprits in our patient, and
the presence of other symptoms (edema, arthralgias, myalgias, night sweats, diarrhea, and headache) suggested that a systemic condition was
responsible for his cough and other symptoms.
In this patient, Whipples disease was the
underlying cause. Whipples disease is a chronic
infectious disease that affects multiple organ
systems; it is a rare disease, with a reported annual incidence of less than 1 case per 1,000,000
people.3 It is caused by T. whipplei, a ubiquitous
environmental organism. T. whipplei is thought
to be acquired by fecaloral transmission and is
found in sewage-plant effluxes.4 The organism
is dependent on host cells for growth and is one
of the slowest-growing pathogenic bacteria in
humans, with a generation time of 18 days.5 The
disease appears to occur more frequently in persons of European ancestry than in persons of
other ancestries and more frequently in men
than in women (male:female ratio, 4:1). It most
often manifests in middle age, although cases
occur across the age spectrum.6
Whipples disease has a broad spectrum of
symptoms and signs; typical manifestations (and
their frequency in case series) include weight
loss (in 92% of patients), diarrhea (in 76%), arthralgia (in 67%), abdominal pain (in 55%), fever
(in 38%), supranuclear ophthalmoplegia (in 32%),
headache (in 10%), anemia (in 85%), lymphadenopathy (in 60%), endocarditis (in 30%, and
usually culture-negative), and pulmonary involvement (in 30 to 40%, approximately half of whom
have cough).3,7 The typical presentation is a
prodrome of arthritis, followed by persistent
diarrhea and weight loss; arthritis can precede
the gastrointestinal symptoms by many years.
Neurologic manifestations may be irreversible
despite treatment.
Whipples disease is a rare cause of chronic
cough, although cough is well described in patients with Whipples disease. In our patient,
cough was a central feature. In a small case series of patients who had Whipples disease with
pulmonary involvement,7 common symptoms included dyspnea and dry cough, and findings on
chest imaging included interstitial patterns, pleural effusions, and mediastinal lymphadenopathy.
Whereas the diagnosis in our patient was
made serendipitously owing to the lymph-node
biopsy (for suspicion of lymphoma), the diagnostic test of choice is upper gastrointestinal
endoscopy with biopsies (although other tissue
sites may be sampled). Macroscopic features
may include pale yellow duodenal mucosa and
ectatic lymph vessels. Immunohistochemical testing can improve the yield of histologic diagnosis. Identification of the 16S ribosomal RNA gene
Left ventricle
Aortic valve
Mitral valve
Left atrium
Figure 4. Transthoracic Echocardiogram.
The mobile vegetative mass resolved by the sixth
month of therapy and is no longer seen on the noncoronary cusp of the aortic valve.
n engl j med 373;6nejm.org August 6, 2015
The New England Journal of Medicine
Downloaded from nejm.org on August 8, 2015. For personal use only. No other uses without permission.
Copyright 2015 Massachusetts Medical Society. All rights reserved.
565
Clinical Problem-Solving
with the use of a polymerase-chain-reaction assay (e.g., from feces or saliva) has high sensitivity
and specificity for the organism but should not
be used in isolation for diagnosis. Culture is not
useful in diagnosis, because it may take months
for the organism to grow and requires special
techniques; serologic testing is nonspecific.3
In the absence of randomized trials, treatment recommendations are guided largely by
case series. First-line treatment typically involves
2 weeks of ceftriaxone, followed by at least 1 year
of trimethoprimsulfamethoxazole.3 In one case
series, 92% of patients receiving this regimen
had a remission; the remission rate was higher
than with tetracycline, especially with respect to
relapse involving the central nervous system.8
For patients who have a sulfa allergy or desire
only oral therapy, doxycycline plus hydroxychloroquine may be substituted for either or both
ceftriaxone and trimethoprimsulfamethoxazole3
(with response rates in case series similar to
those reported with standard therapy). Antibiotic treatment alone has been effective in curing
culture-negative endocarditis related to Whipples disease.9,10
Whipples disease is notorious for masquerading as other inflammatory conditions (e.g.,
sarcoidosis), and many cases have been treated
References
1. Chung KF, Pavord ID. Prevalence,
pathogenesis, and causes of chronic
cough. Lancet 2008;371:1364-74.
2. Pavord ID, Chung KF. Management
of chronic cough. Lancet 2008;371:137584.
3. Schneider T, Moos V, Loddenkemper C,
Marth T, Fenollar F, Raoult D. Whipples
disease: new aspects of pathogenesis and
treatment. Lancet Infect Dis 2008;8:17990.
4. Schniger-Hekele M, Petermann D,
Weber B, Mller C. Tropheryma whipplei
in the environment: survey of sewage
plant influxes and sewage plant workers.
Appl Environ Microbiol 2007;73:2033-5.
empirically with glucocorticoids. Although some
reports have described improvement in association with glucocorticoid therapy, the improvement was rarely sustained, and there are numerous reports of symptoms worsening with this
medication.11
The present case shows the difficulty in recognizing Whipples disease; its rarity and nonspecific clinical features (overlapping with those
of many chronic inflammatory diseases) often
result in delayed diagnosis (up to 2 to 6 years
after the onset of symptoms, according to some
case series).10 Although Whipples disease is uncommon, chronic infection with T. whipplei should
be considered in any patient with persistent unexplained arthralgias or gastrointestinal or systemic symptoms.
Dr. Gin reports receiving fees for serving on advisory boards
from Bayer, Forest, Boehringer Ingelheim, and Pfizer. No other potential conflict of interest relevant to this article was reported.
Disclosure forms provided by the authors are available with
the full text of this article at NEJM.org.
We thank the staff of the microbiology laboratory; Drs. Patrick Doyle and Elizabeth Bryce (University of British Columbia)
and Dr. Linda Hoang (British Columbia Centre for Disease Control) for making the microbiologic diagnosis of Whipples disease with the direct 16S gene-sequencing technique; and Dr.
Valerie A. White (University of British Columbia) for making the
histopathological diagnosis of Whipples disease and providing
the photomicrographs.
5. Raoult D, Birg ML, La Scola B, et al.
Cultivation of the bacillus of Whipples
disease. N Engl J Med 2000;342:620-5.
6. Dobbins WI. Whipples disease. Springfield, IL:Charles C Thomas, 1985.
7. Urbanski G, Rivereau P, Artru L,
Fenollar F, Raoult D, Puchal X. Whipple
disease revealed by lung involvement:
a case report and literature review. Chest
2012;141:1595-8.
8. Feurle GE, Marth T. An evaluation of
antimicrobial treatment for Whipples
disease: tetracycline versus trimethoprimsulfamethoxazole. Dig Dis Sci 1994;
39:
1642-8.
9. Algin A, Wegdam-Blans M, Verduin K,
Janssen H, van Dantzig JM. Tropheryma
whipplei aortic valve endocarditis, cured
without surgical treatment. BMC Res
Notes 2012;5:600.
10. Durand DV, Lecomte C, Cathbras P,
Rousset H, Godeau P. Whipple disease:
clinical review of 52 cases. Medicine (Baltimore) 1997;76:170-84.
11. Berent R, Auer J, Lassnig E, et al.
Whipples disease: misdiagnosed as sarcoidosis with further tricuspid valve endocarditis and pulmonary embolism
a case report. BMJ Case Rep 2009
bcr07.2008.0441.
Copyright 2015 Massachusetts Medical Society.
clinical problem-solving series
The Journal welcomes submissions of manuscripts for the Clinical Problem-Solving
series. This regular feature considers the step-by-step process of clinical decision
making. For more information, please see authors.NEJM.org.
566
n engl j med 373;6nejm.org August 6, 2015
The New England Journal of Medicine
Downloaded from nejm.org on August 8, 2015. For personal use only. No other uses without permission.
Copyright 2015 Massachusetts Medical Society. All rights reserved.
Você também pode gostar
- The Yellow House: A Memoir (2019 National Book Award Winner)No EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Nota: 4 de 5 estrelas4/5 (98)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeNo EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeNota: 4 de 5 estrelas4/5 (5795)
- Merkel Cell CarcinomaDocumento15 páginasMerkel Cell CarcinomaJhonnathan Rodriguez100% (1)
- Vitamin and Mineral Supplements What Clinicians Need To KnowDocumento2 páginasVitamin and Mineral Supplements What Clinicians Need To KnowJhonnathan RodriguezAinda não há avaliações
- Alien Hand SyndromeDocumento2 páginasAlien Hand SyndromeJhonnathan RodriguezAinda não há avaliações
- Endocrinology Meet TeacherDocumento374 páginasEndocrinology Meet TeacherJhonnathan Rodriguez100% (2)
- Anatomy VivaDocumento126 páginasAnatomy VivaBayar A. AhmedAinda não há avaliações
- Porphyrias: M. F. M. James and R. J. HiftDocumento11 páginasPorphyrias: M. F. M. James and R. J. HiftJhonnathan RodriguezAinda não há avaliações
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureNo EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureNota: 4.5 de 5 estrelas4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryNo EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryNota: 3.5 de 5 estrelas3.5/5 (231)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceNo EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceNota: 4 de 5 estrelas4/5 (895)
- Never Split the Difference: Negotiating As If Your Life Depended On ItNo EverandNever Split the Difference: Negotiating As If Your Life Depended On ItNota: 4.5 de 5 estrelas4.5/5 (838)
- The Little Book of Hygge: Danish Secrets to Happy LivingNo EverandThe Little Book of Hygge: Danish Secrets to Happy LivingNota: 3.5 de 5 estrelas3.5/5 (400)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersNo EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersNota: 4.5 de 5 estrelas4.5/5 (345)
- The Unwinding: An Inner History of the New AmericaNo EverandThe Unwinding: An Inner History of the New AmericaNota: 4 de 5 estrelas4/5 (45)
- Team of Rivals: The Political Genius of Abraham LincolnNo EverandTeam of Rivals: The Political Genius of Abraham LincolnNota: 4.5 de 5 estrelas4.5/5 (234)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyNo EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyNota: 3.5 de 5 estrelas3.5/5 (2259)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaNo EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaNota: 4.5 de 5 estrelas4.5/5 (266)
- The Emperor of All Maladies: A Biography of CancerNo EverandThe Emperor of All Maladies: A Biography of CancerNota: 4.5 de 5 estrelas4.5/5 (271)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreNo EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreNota: 4 de 5 estrelas4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)No EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Nota: 4.5 de 5 estrelas4.5/5 (121)
- AriaDocumento57 páginasAriamushroom bestAinda não há avaliações
- M6 Case StudyDocumento5 páginasM6 Case StudylorrieAinda não há avaliações
- Pediatric Respiratory HandoutsDocumento5 páginasPediatric Respiratory HandoutsBrittanyAinda não há avaliações
- Underwriting Field ManualDocumento76 páginasUnderwriting Field ManualobanAinda não há avaliações
- Worksheet On Obstruction and AsthmaDocumento14 páginasWorksheet On Obstruction and AsthmaKaye CorAinda não há avaliações
- July 21 2022 HDFC - Securities - Retail - Research - Initiation - Supriya - LifescienceDocumento17 páginasJuly 21 2022 HDFC - Securities - Retail - Research - Initiation - Supriya - LifescienceHarish SubramaniamAinda não há avaliações
- DIPROSPAN Sterile Aqueous Suspension: DescriptionDocumento6 páginasDIPROSPAN Sterile Aqueous Suspension: DescriptionAbet AtienzaAinda não há avaliações
- Rational Drug Prescribing Training CourseDocumento78 páginasRational Drug Prescribing Training CourseAhmadu Shehu MohammedAinda não há avaliações
- Asthma Reading Task Text A and B Oet Reading NotesDocumento16 páginasAsthma Reading Task Text A and B Oet Reading NotesSakshi RanbhiseAinda não há avaliações
- Franklyn'Smedi Cal English: PrefaceDocumento68 páginasFranklyn'Smedi Cal English: Prefacesuprnd100% (2)
- OET Reading Sub-Test Practice 1: Time Limit 15 MinutesDocumento7 páginasOET Reading Sub-Test Practice 1: Time Limit 15 Minutesastor toAinda não há avaliações
- Guaifenesin Sample Package InsertDocumento2 páginasGuaifenesin Sample Package InsertCyAinda não há avaliações
- Subjective: "Nahihirapan Ako Huminga" As Verbalized by The Patient. ObjectiveDocumento4 páginasSubjective: "Nahihirapan Ako Huminga" As Verbalized by The Patient. Objectivechaoz09Ainda não há avaliações
- Group 8 Oxygenation AtionDocumento46 páginasGroup 8 Oxygenation AtionPrince Masroor Ali AbroAinda não há avaliações
- 13 Suppl1Documento31 páginas13 Suppl1VinodAinda não há avaliações
- Health Assessment On Asthma ANPDocumento7 páginasHealth Assessment On Asthma ANPSam TullyAinda não há avaliações
- Therapeutic Strategies in CopdDocumento378 páginasTherapeutic Strategies in Copdgermany23Ainda não há avaliações
- Asthma Patient Education: Check ListDocumento2 páginasAsthma Patient Education: Check ListZiyad AlrajhiAinda não há avaliações
- Common OSCE CasesDocumento6 páginasCommon OSCE CasesRosa AlersAinda não há avaliações
- Grila de Lectura A Unui Articol de Studiu TerapeuticDocumento3 páginasGrila de Lectura A Unui Articol de Studiu TerapeuticlacatisAinda não há avaliações
- Case Study 1 - Environmental HealthDocumento2 páginasCase Study 1 - Environmental HealthMohammed Fakhouri50% (4)
- What Causes COPD?Documento4 páginasWhat Causes COPD?Adi PutraAinda não há avaliações
- Asthma by DR Adel MansurDocumento52 páginasAsthma by DR Adel MansurCalvin PintoAinda não há avaliações
- Obesity and AsthmaDocumento26 páginasObesity and AsthmaDumitru BiniucAinda não há avaliações
- OSCE: Respiratory History and ExaminationDocumento10 páginasOSCE: Respiratory History and ExaminationShahin KazemzadehAinda não há avaliações
- Clerkship Handbook: Family MedicineDocumento51 páginasClerkship Handbook: Family MedicineKen WonAinda não há avaliações
- Long Term:: Iloilo Doctors' College College of NursingDocumento7 páginasLong Term:: Iloilo Doctors' College College of NursingAbie Jean BalbontinAinda não há avaliações
- Lower Respiratory Tract Diseases - KeyDocumento45 páginasLower Respiratory Tract Diseases - KeyYugmaPandyaAinda não há avaliações
- COPD Case PresentationDocumento50 páginasCOPD Case PresentationSarah Ann Jamilla FaciolanAinda não há avaliações
- Concise Clinical Review: Role of Biologics in AsthmaDocumento13 páginasConcise Clinical Review: Role of Biologics in AsthmaHossam HamzaAinda não há avaliações