Escolar Documentos
Profissional Documentos
Cultura Documentos
Cystometry "Cystometrogram" (CMG)
Enviado por
Wendy EscalanteDescrição original:
Título original
Direitos autorais
Formatos disponíveis
Compartilhar este documento
Compartilhar ou incorporar documento
Você considera este documento útil?
Este conteúdo é inapropriado?
Denunciar este documentoDireitos autorais:
Formatos disponíveis
Cystometry "Cystometrogram" (CMG)
Enviado por
Wendy EscalanteDireitos autorais:
Formatos disponíveis
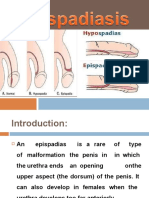
CYSTOMETRY
CYSTOMETROGRAM (CMG)
A test that measures the pressure inside the bladder in order to see how well the urinary
bladder is working.
Done when a muscle or nerve problem may be causing problems with how well the
bladder holds or releases urine.
PURPOSE:
To find the cause of the problem affecting the bladder sphincter or the bladder itself.
To measure how much urine can the bladder store and how much residual volume there is.
To help the physician and the patient she make decisions about the appropriate treatment
regimen.
To see how well the bladder works in people with progressive neurological diseases like
multiple sclerosis.
HOW TO PREPARE FOR THE TEST:
Generally, no special preparations are needed for this test. However, for infants and
children, preparation depends on the child's age, past experiences, and level of trust.
Before the test, patient must tell the healthcare provider if she is taking any medicines
because some meds and herbal supplements can affect bladder function. (e.g.
ANTIHISTAMINE)
Patient should also inform the healthcare provider if she is pregnant or is suspected to be.
HOW THE TEST IS PERFORMED:
1. Patient will be asked to void into a special container (UROFLOWMETER) that is interfaced
with a computer.
It records the (1) time it takes one to begin urinating; (2) the size, force, and
continuity of ones urinary stream; (3) the amount of urine; and (4) how long it
took one to empty ones bladder.
2. Patient will then lie down and a catheter is gently placed in her bladder to drain and
measure the remaining urine.
A smaller catheter is sometimes placed in ones rectum in order to measure the
abdominal pressure. Measuring electrodes, similar to the sticky pads used for
an EKG, are placed near the rectum.
The test usually takes 30 to 60 minutes, but it may take slightly longer if any special tests
are done.
After cystometry, one will need to keep track of how much she drinks and how much she
urinates for the next 24 hours. A burning sensation during urination is a common but
temporary side effect. Drinking lots of fluids will help relieve this sensation. One may be
given an antibiotic to help prevent a urinary tract infection.
One may feel sore after the test though a warm tub bath may be helpful to relieve the
soreness.
RISKS OF CYSTOMETRY:
Cystometry usually does not cause problems though there is always a slight risk of
developing a UTI when a catheter is inserted into the bladder.
If patient has a high spinal cord injury, she may have low heart rate, high blood
pressure, headache, and feel flushed or sweaty during the test. Report these symptoms to
the health professional conducting the test, since further testing may cause complications.
WHAT TO DO AFTER THE TEST:
Patient may need to urinate frequently, with some burning during and after urination for a
day or two. Therefore, patient must drink lots of fluids to help minimize the burning and to
prevent a urinary tract infection.
A pinkish tinge to the urine is common for several days after cystometry. But call the
doctor immediately if:
Urine remains red or you see blood clots after voiding X times
Have not been able to urinate 8 hours after the test.
Have a fever, chills, or severe pain in your flank or abdomen
Have symptoms of a urinary tract infection:
Pain or burning upon urination.
An urge to urinate frequently, but usually passing only small quantities of urine.
Dribbling or leakage of urine.
Urine that is reddish or pinkish, foul-smelling, or cloudy.
Pain or a feeling of heaviness in the lower abdomen.
CAUSES OF ABNORMAL RESULTS:
Enlarged prostate
Multiple sclerosis
Overactive bladder
Reduced bladder capacity
Spinal cord injury
Stroke
Urinary tract infection
CYSTOGRAM
Also known as a bladder scan, is an imaging technique. Doctors use it to diagnose
illnesses or abnormalities of the bladder, such as infection, distension, or incomplete
emptying.
During this exam, small amounts of a radioactive fluid are injected into the bladder
through a thin, flexible tube called a catheter. The fluid can show doctors areas of concern,
such as tumors or structural defects, when highlighted under a specialized scanner.
Why the Test Is Performed
Your doctor may recommend this test if youre having problems with your bladder. This
could include incomplete emptying of the bladder, leakage, or difficult urination. It is also
performed to diagnose the cause of urinary tract infections, particularly in children.
Some of the most common reasons a radionuclide cystogram are done include:
Bladder infection
Enlarged prostate gland
Nerve problems
Obstruction in urine flow
Urine refluxbackward flow of urine from bladder to the kidneys
The solution containing radioactive material is injected into the bladder through a catheter
in the urethra (the tube through which urine is expelled from the body). There may be
slight discomfort when the catheter is inserted and removed, but this typically subsides
shortly after the test.
Urine may appear slightly pink after the test due to bleeding from catheter insertion and
removal. Some people experience urinary tract infections as a result of the procedure, but
this is rare.
HOW TO PREPARE:
This requires no special preparation. You will have to remove all jewelry and change into a
hospital gown prior to the test. Your doctor will ask you questions about your medical
history and symptoms. Answering these questions as completely as possible can help your
doctor identify and minimize any other side effects of the procedure.
HOW THE TEST IS PERFORMED:
The test will be performed in a hospitals radiology department or in a specialized testing
facility.
Youll begin by lying down on a scanner table. A nurse will then insert a catheter into your
urethra and up into your bladder. This may cause some discomfort.
A solution containing radioactive tracers, which allows the doctor to view the affected
internal organs using X-ray, will flow through the catheter into your bladder. When your
bladder is full, images will be taken of your bladder using a special camera.
You may also have to urinate while images are taken. You may urinate into a urinal or
bedpan. More images are taken when your bladder is empty.
When the radiologist is finished with the images, the catheter will be removed and the test
terminated. You will be free to leave when the test is complete.
There is no risk of radioactive tracers remaining in your body because your bladder will
completely expel them during normal urination.
URODYNAMICS
A three-fold procedure that involves different tests including:
1. Measured voiding without a catheter
2. Filling phase Test
3. Emptying phase test
For complete urodynamic testing, a much smaller catheter is placed in the bladder so the
patient will be able to urinate around it. Because this special catheter has a sensor on the
tip, the computer can measure the pressure and volumes as the bladder fills and as the
patient empties it. Patient may be asked to cough or push so that the health care provider
can check for urine leakage.
VIDEOURODYNAMICS
Type of urodynamic test wherein x-rays can be taken during the test. In this case, instead of
water, a special fluid that shows up on x-ray is used to fill ones bladder rather than water or air.
HOW TO PREPARE FOR THE TEST:
Healthcare provider should also be notified by the patient if she has symptoms of a urinary
tract infection: pain or burning with urination, foul-smelling or cloudy urine, or an urge to
urinate more often than usual.
KUB ULTRASOUND (KIDNEY URETER BLADDER UTZ)
KUB refers to a diagnostic medical imaging technique of the abdomen and stands for
Kidneys, Ureters, and Bladder, although in fact the Ureters only show if they are
abnormally distended. A KUB ultrasound is an examination requested by your doctor to
evaluate the urinary tract (which includes the kidneys, ureters, and urinary bladder). In
the male patient, the prostate gland is also scanned.
A KUB Ultrasound may be requested:
To look for changes in the bladder wall
To look for changes in the kidney size or structure
To look for stones in the urinary tract
To evaluate reasons why you have recurrent kidney infection
To identify the cause of renal or pelvic pain
What happens during renal or KUB ultrasound?
The urinary bladder can only be properly assessed when full or distended, as bladder
volume measurements are taken whilst the bladder is full.
The bladder and both kidneys are also scanned after the bladder has been emptied to
evaluate the volume of urine retained
In the male patient the prostatic volume is measured.
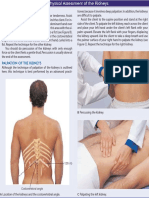
DURING THE ULTRASOUND EXAMINATION:
Health care providers will make a detailed study of the size, shape and condition of
the:
Urinary bladder, both full and immediately after emptying (you will be sent to a lavatory to
empty your bladder)
Both right and left kidneys and their ureters
The prostate gland (males)
What preparation is required for the KUB Ultrasound scan?
A full bladder is required and you will need to drink a pint of water in the hour before your
scan. During this period, please do not empty your bladder.
What will happen during the examination?
The KUB ultrasound examination is non-invasive and painless.
You will be asked to lie on your back on the examination couch and expose your lower
abdomen.
Your highly qualified and experienced Sonographer will move a transducer lubricated with
warm gel over your lower abdomen to obtain the necessary images
INTRAVENOUS PYELOGRAPHY
DESCRIPTION:
IVP is the commonly performed test to determine urinary tract dysfunction or renal
disease.
Uses IV radiopaque contrast medium to visualize the kidney, ureter, bladder, and renal
pelvis.
The contrast medium concentrates in the blood and is filtered out by the glomeruli; it
passes out through the renal tubule and is concentrated in the urine.
Renal function is reflected by the length of time it takes the contrast medium to appear
and to be excreted by each kidney.
A series of x-rays is performed during a 30-minute period to view passage of the medium
through the kidney and ureter into the bladder.]
A final film is taken after the patient empties the bladder (post voiding film).
CT scan may be employed during examination to permit the examination of an individual
layer or plane of an organ that may be obscured by surrounding overlying structures.
INDICATIONS:
Evaluate known or suspected ureteral obstruction.
Evaluate function of the K/U/B.
Evaluate presence of renal, ureter, and bladder calculi.
Evaluate the cause of blood in the urine.
Aid in the diagnosis of renovascular hypertension
Evaluate space-occupying lesions or congenital anomalies of the urinary system.
Evaluate the effects of urinary system trauma
NORMAL FINDINGS:
Normal size of KUB.
Normal bladder and absence of masses or renal calculi, with prompt visualization of
contrast medium through the urinary system
ABNORMAL FINDINGS:
Absence of kidney (Congenital
Malformation)
Prostatic enlargement
Benign or Malignant kidney tumors.
Pyelonephritis
Renal cysts
Bladder tumors.
Congenital renal or urinary tract
abnormalities.
Renal hematomas
Renal or ureteral calculi
Glomerulonephritis
Soft-tissue masses
Hydronephrosis
Tumors of the collecting system
CONTRAINDICATIONS
Patients who are allergic to shellfish or iodinated dyes.
Patients who are severely dehydrated, because this can cause renal shutdown and failure
(Geriatric patients are particularly vulnerable).
Patients with renal insufficiency, as evidenced by a BUN value greater than 40 mg/dl,
because the iodinated nephrotoxic dye can worsen kidney function.
Patients with Multiple myeloma, because the iodinated nephrotoxic dye can worsen renal
function.
Patients who are pregnant, unless the benefits outweigh the risk of radiation exposure to
the fetus
POTENTIAL COMPLICATIONS
Allergy to dye
Infiltration of contrast dye
Renal failure ( This occurs most often in elderly patients who are dehydrated before the
dye injection)
Hypoglycemia or acidosis may occur in pt. who are taking (Glucophage) and receive iodine
dye
INTERFERING FACTORS
Fecal material, gas, or barium in the bowel may obscure visualization of the renal system.
Abnormal renal function studies may prevent adequate visualization of the urinary tract.
Retained barium from previous studies may obscure visualization. Studies using barium
(e.g., barium enema) should be scheduled after an IVP.
Procedure and Patient Care
Before:
Explain the procedure to the patient. Inform the pt. that several x-ray will be taken over 30
minutes.
Obtain informed consent If required by the institution.
Check the pt. for allergies to iodinated dye and shellfish.
Give the pt. a laxative as ordered, the evening before the test
Inform the pt. of the required food and fluid restrictions. Some institutions prefer
abstinence from solid for 8 hours before testing. Some allow a clear-liquid breakfast on the
test day.
Ensure adequate hydration for the patient before and after the test to avoid dye-induced
renal failure.
Note that pediatric pts. Will have decreased fasting times, as ordered on an individual
basis.
Note that elderly and debilitated pts. should have fasting times specifically for them.
Note the pts. Receiving high rates of IV fluids may have infusion rates decreased several
hours before the study to increase concentration of the dye within the urinary system.
Assess the pts. BUN and CREA levels. Abnormal renal function could deteriorate as a result
of the dye injection.
Schedule any barium studies after completion of the IVP.
Give the pt. an enema or suppository on the morning of the study, if ordered.
DURING:
Note the following procedural steps:
1. The pt. is taken to the radiology department and placed in a supine position.
2. A plain film of the abdomen (KUB) is taken to ensure that no residual stool obscures
visualization of the renal system. This also screens for calculi in the renal collecting
system.
3. Skin testing for iodine allergy is often done.
4. A peripheral IV line is started and a contrast dye (e.g., Hypaque, Renografin) is given.
5. X-ray films are taken at specific times, usually at 1, 5, 10, 15, 20, and 30 minutes and
sometimes longer, to follow the course of the dye from the cortex of the kidney to the
bladder.
6. Tomography may be performed to identify a mass.
7. The patient is taken on the bathroom and asked to void.
8. A post voiding film is taken to visualize the empty bladder, ureter temporarily to obtain
an better film of the collecting system in the upper part of the ureter. This is done by
compressing the abdomen with an inflatable rubber tube, which is wrapped tightly around
the abdomen slightly below the umbilicus.
Note that this test is performed by a radiologist in approximately 45 minutes.
Inform the pt. that the dye injection often causes a transitory flushing of the face, a feeling
of warmth, a salty taste in the mouth, or even transient nausea. Initial IV needle
placement and lying on a hard x-ray table are the only other discomforts associated with
IVP.
After:
Maintain the pt. on adequate oral or IV hydration for several hours after the IVP to
counteract fluid depletion caused by test preparation. Encourage fluid intake.
Assess the pt. urinary output. A decreased output may be an indication of renal failure.
Evaluate elderly and debilitated pts. For weakness because fasting necessary for test
preparation. Instruct these pts. to ambulate only with assistance.
Você também pode gostar
- Blood SpecimenDocumento41 páginasBlood SpecimenPooja Hardiya100% (1)
- Nasogastric Aspiration: Preparation of ArticlesDocumento2 páginasNasogastric Aspiration: Preparation of ArticlesVarun ToshniwalAinda não há avaliações
- Gastrostomy Feeding ProcedureDocumento5 páginasGastrostomy Feeding ProcedureRohini RaiAinda não há avaliações
- Abdominal ParacentesisDocumento5 páginasAbdominal ParacentesisSivaprasad S100% (1)
- Gastric LavageDocumento15 páginasGastric LavageEm BelandoAinda não há avaliações
- Bladder IrrigationDocumento14 páginasBladder IrrigationsandhyaAinda não há avaliações
- Urine Specimen Collection Procedure PDFDocumento3 páginasUrine Specimen Collection Procedure PDFtincho9Ainda não há avaliações
- Esophageal ObstructionDocumento18 páginasEsophageal ObstructionArun Murali50% (2)
- Tracheostomy CareDocumento37 páginasTracheostomy Carepreet kaurAinda não há avaliações
- Eye Irrigation ChecklistDocumento3 páginasEye Irrigation ChecklistAlma Janella TOSINOAinda não há avaliações
- Angiography: Presented By: Mulituba, Nairah DDocumento9 páginasAngiography: Presented By: Mulituba, Nairah DAkazukin AineAinda não há avaliações
- Bone Marrow Aspiration and BiopsyDocumento7 páginasBone Marrow Aspiration and BiopsyPriyanjali SainiAinda não há avaliações
- Bladder TraumaDocumento13 páginasBladder TraumaBernardAinda não há avaliações
- Intravenous UROGRAMDocumento14 páginasIntravenous UROGRAMvijendrakumarsahuAinda não há avaliações
- Tracheostomy CareDocumento40 páginasTracheostomy CareSreelekhaAinda não há avaliações
- Peritoneal DialysisDocumento3 páginasPeritoneal DialysisSumit YadavAinda não há avaliações
- Renal CalculiDocumento11 páginasRenal CalculiAaqashh MasseyAinda não há avaliações
- Gastrostomy FeedingDocumento9 páginasGastrostomy FeedingJamie Luz Tongco0% (1)
- Caring For Your Jejunostomy Feeding Tube - Feb22Documento6 páginasCaring For Your Jejunostomy Feeding Tube - Feb22Buvana VigneshAinda não há avaliações
- Surgical CP ParotidDocumento43 páginasSurgical CP ParotidValarmathiAinda não há avaliações
- Assessment of GI SystemDocumento40 páginasAssessment of GI SystemJeffRy SinyOe100% (1)
- Nursing Management of The Critically Ill PatientDocumento28 páginasNursing Management of The Critically Ill PatientAtinder Sran100% (2)
- Care of A Bedridden Patient: Prepared by Jannet Reena PuraniDocumento25 páginasCare of A Bedridden Patient: Prepared by Jannet Reena PuraniAnn Merlin Jobin100% (1)
- Institute of Nursing and Allied Health SciencesDocumento2 páginasInstitute of Nursing and Allied Health Sciencesshadow gonzalezAinda não há avaliações
- Stomal TherapyDocumento2 páginasStomal Therapyসায়ন্তন দত্ত100% (1)
- Colostomy Care: Sital B Sharma MSC Nursing Part I Con, NBMCDocumento39 páginasColostomy Care: Sital B Sharma MSC Nursing Part I Con, NBMCShetal Sharma100% (1)
- Pulse OximetryDocumento3 páginasPulse OximetryJanna Favila100% (3)
- Anatomy and Physiology of GallbladderDocumento15 páginasAnatomy and Physiology of GallbladderIkea Balhon100% (1)
- PeritonitisDocumento22 páginasPeritonitisBobby Faisyal Rakhman100% (1)
- Thoracocentasis: INTRODUCTION:-Thoracentasis Also Known As The Thoracocentasis or Plural Tap Is AnDocumento7 páginasThoracocentasis: INTRODUCTION:-Thoracentasis Also Known As The Thoracocentasis or Plural Tap Is AnaparnaAinda não há avaliações
- Care of Chest Drainage: Articles RationaleDocumento7 páginasCare of Chest Drainage: Articles Rationalepreeti sharmaAinda não há avaliações
- Tracheostomy CareDocumento14 páginasTracheostomy Caresourabh mehraAinda não há avaliações
- ColostomyDocumento11 páginasColostomyRiddhi Mehta0% (1)
- Ateneo de Zamboanga University College of Nursing NCM 112j RLEDocumento3 páginasAteneo de Zamboanga University College of Nursing NCM 112j RLEsenyorakath0% (1)
- Care of Patient With DrainsDocumento49 páginasCare of Patient With DrainsAnusha Verghese100% (3)
- EpispadiasisDocumento12 páginasEpispadiasisvishnuAinda não há avaliações
- Burns DressingDocumento4 páginasBurns DressingBalaMuruganAinda não há avaliações
- IV Cannulation and Fixation Infusion PumpDocumento23 páginasIV Cannulation and Fixation Infusion PumpUday Kumar0% (1)
- Cystoscopy WordDocumento4 páginasCystoscopy WordMon ManguilinAinda não há avaliações
- NG TubeDocumento3 páginasNG TubeKenny JosefAinda não há avaliações
- Abdominal Paracentesis, AP, Abdominal TapDocumento32 páginasAbdominal Paracentesis, AP, Abdominal TapMeraflor BahonsuaAinda não há avaliações
- Assisting With Arterial Puncture For Blood Gas Analysis EquipmentDocumento7 páginasAssisting With Arterial Puncture For Blood Gas Analysis EquipmentPoova RagavanAinda não há avaliações
- ETT IntubationDocumento10 páginasETT IntubationPoova RagavanAinda não há avaliações
- Assisting With Lumbar PunctureDocumento4 páginasAssisting With Lumbar PuncturePhelanCoy100% (1)
- Gastric LavageDocumento13 páginasGastric Lavagetibinj67Ainda não há avaliações
- Neurological AssessmentDocumento5 páginasNeurological AssessmentVIDYAAinda não há avaliações
- Cardiac MonitoringDocumento19 páginasCardiac MonitoringYaska Musa100% (1)
- LESSON PLAN ON. Lung AbscessDocumento12 páginasLESSON PLAN ON. Lung AbscessFriends ForeverAinda não há avaliações
- Colostomy CareDocumento8 páginasColostomy CareAhmed Hamed100% (2)
- Coronary Care Unit/ Cardiac Care Unit: Patient MonitorsDocumento3 páginasCoronary Care Unit/ Cardiac Care Unit: Patient MonitorsPhoebe Kyles Camma100% (1)
- TracheostomyDocumento1 páginaTracheostomyDudil GoatAinda não há avaliações
- Colostomy Dressing ProcedureDocumento2 páginasColostomy Dressing Procedurejoel david knda mj100% (1)
- Assignment On Radiation TherapyDocumento16 páginasAssignment On Radiation TherapyAxsa AlexAinda não há avaliações
- Colostomy CareDocumento7 páginasColostomy CareChrismon Arek KeneAinda não há avaliações
- Defibrillation TypedDocumento8 páginasDefibrillation TypedValarmathiAinda não há avaliações
- Hyperpyrexia: Definition: Fever Is Any Abnormal Elevation of The Body Temperature. Temperature 40c Is Called .Documento5 páginasHyperpyrexia: Definition: Fever Is Any Abnormal Elevation of The Body Temperature. Temperature 40c Is Called .Jenish Panchal100% (1)
- Rahman Institute of Nursing and Paramedical Sciences, Radhanagar, Guwahati Demonstration ON Peritoneal DialysisDocumento7 páginasRahman Institute of Nursing and Paramedical Sciences, Radhanagar, Guwahati Demonstration ON Peritoneal DialysisPuy Puy ChhangteAinda não há avaliações
- Portal HypertensionDocumento23 páginasPortal HypertensionSumathi GopinathAinda não há avaliações
- Skills LabDocumento20 páginasSkills LabJei JayAinda não há avaliações
- Urodynamic Testing ReportDocumento25 páginasUrodynamic Testing Reportzharah180% (1)
- Assessment of Kidneys PDFDocumento1 páginaAssessment of Kidneys PDFWendy EscalanteAinda não há avaliações
- Drug StudyDocumento14 páginasDrug StudyWendy EscalanteAinda não há avaliações
- PATHODocumento2 páginasPATHOWendy EscalanteAinda não há avaliações
- NCPDocumento3 páginasNCPWendy EscalanteAinda não há avaliações
- NCP 2 MiDocumento16 páginasNCP 2 MiWendy EscalanteAinda não há avaliações
- Modifiable Risk Factors Non - Modifiable Risk Factors: LegendDocumento2 páginasModifiable Risk Factors Non - Modifiable Risk Factors: LegendWendy Escalante100% (1)
- Nasogastric Tube Management and CareDocumento21 páginasNasogastric Tube Management and CareWendy EscalanteAinda não há avaliações
- Acid-Ash DietDocumento10 páginasAcid-Ash DietWendy Escalante0% (1)
- Concept Map of Carotid Artery DiseaseDocumento2 páginasConcept Map of Carotid Artery DiseaseWendy EscalanteAinda não há avaliações
- 02 Orig Art 02 PDFDocumento3 páginas02 Orig Art 02 PDFWendy EscalanteAinda não há avaliações
- Case Presentation: Group 2Documento30 páginasCase Presentation: Group 2Wendy EscalanteAinda não há avaliações
- Caring For The Bedridden PatientDocumento1 páginaCaring For The Bedridden PatientWendy EscalanteAinda não há avaliações
- Assessment of KidneysDocumento1 páginaAssessment of KidneysWendy EscalanteAinda não há avaliações
- Concept Map of CKD Gastrointestinal SymptomsDocumento4 páginasConcept Map of CKD Gastrointestinal SymptomsWendy Escalante0% (1)
- At DietDocumento8 páginasAt DietWendy EscalanteAinda não há avaliações
- Degenerative Joint DiseaseDocumento35 páginasDegenerative Joint DiseaseWendy EscalanteAinda não há avaliações
- Fundamentals in NursingDocumento9 páginasFundamentals in NursingWendy EscalanteAinda não há avaliações
- Brat DietDocumento8 páginasBrat DietWendy EscalanteAinda não há avaliações
- Pediatric NursingDocumento16 páginasPediatric NursingWendy Escalante100% (1)
- DM Report1Documento16 páginasDM Report1Wendy EscalanteAinda não há avaliações
- Therapeutic DietDocumento3 páginasTherapeutic DietWendy EscalanteAinda não há avaliações
- Drug Study FinalDocumento8 páginasDrug Study FinalWendy EscalanteAinda não há avaliações
- FNCP CommunityDocumento4 páginasFNCP CommunityWendy EscalanteAinda não há avaliações
- Nursing Care For Patient With Neurological DiseaseDocumento8 páginasNursing Care For Patient With Neurological DiseaseWendy EscalanteAinda não há avaliações
- Integrated Management of Childhood Illness: Sick Child Age 2 Months Up To 5 YearsDocumento78 páginasIntegrated Management of Childhood Illness: Sick Child Age 2 Months Up To 5 YearsWendy EscalanteAinda não há avaliações
- Diabetes MellitusDocumento5 páginasDiabetes MellitusWendy EscalanteAinda não há avaliações
- Science 9 First Quarter Exam SY 2021-2022Documento5 páginasScience 9 First Quarter Exam SY 2021-2022Encluna Lindon JayAinda não há avaliações
- Hammer StrengthDocumento5 páginasHammer Strengthrobokop5602Ainda não há avaliações
- Thyroid and Antithyroid Agent-VDocumento60 páginasThyroid and Antithyroid Agent-VVine100% (1)
- Anatomy Mcqs (2) - 1Documento13 páginasAnatomy Mcqs (2) - 1Yashfa Yasin - PharmDAinda não há avaliações
- Cranial Nerves-Anatomy and Clinical Comments Wilson-PauwelsDocumento189 páginasCranial Nerves-Anatomy and Clinical Comments Wilson-PauwelsAlina Elena Tudorache100% (6)
- 01lowback PDFDocumento2 páginas01lowback PDFkotza100% (1)
- Nephron CompressDocumento91 páginasNephron CompressAlligator ZAinda não há avaliações
- Basics of Steps AerobicsDocumento7 páginasBasics of Steps AerobicsJohn Marlo Catibog100% (2)
- Spiderman ExercisesDocumento2 páginasSpiderman ExercisesTerry Zachary100% (1)
- Introduction To Anatomical Terms Organizations of The Human BodyDocumento5 páginasIntroduction To Anatomical Terms Organizations of The Human BodyAnonymous 0C4OZmRAinda não há avaliações
- Basic Anatomical TerminologyDocumento30 páginasBasic Anatomical TerminologyanatomyhqAinda não há avaliações
- Naik, S. - Biomechanics of Knee ComplexDocumento25 páginasNaik, S. - Biomechanics of Knee ComplexKyle Bois100% (4)
- Physical Examination & Review of SystemsDocumento4 páginasPhysical Examination & Review of SystemsDexie James Ventenilla DizonAinda não há avaliações
- Guasha 50 PatologiiDocumento55 páginasGuasha 50 PatologiiDan Alex100% (2)
- Rhythms of The Body, Rhythms of The BrainDocumento14 páginasRhythms of The Body, Rhythms of The BrainManel Piqué100% (1)
- Toaz - Info Imaginefx Presents How To Draw and Paint Anatomy Uk PR 55f8581af53dc57Documento95 páginasToaz - Info Imaginefx Presents How To Draw and Paint Anatomy Uk PR 55f8581af53dc57numero 5Ainda não há avaliações
- Week 1Documento2 páginasWeek 1RexAinda não há avaliações
- Nephron ColoringDocumento3 páginasNephron ColoringkishoreddiAinda não há avaliações
- The Refracting Media - Human AnatomyDocumento4 páginasThe Refracting Media - Human AnatomyanggastavasthiAinda não há avaliações
- Neurological AssessmentDocumento53 páginasNeurological AssessmentAlbert B. BalaceAinda não há avaliações
- Putting It All Together: Introduction To Clinical MedicineDocumento8 páginasPutting It All Together: Introduction To Clinical MedicineZedrake CaraanAinda não há avaliações
- Soccer Specific Strength Conditioning Program PPT FinalDocumento31 páginasSoccer Specific Strength Conditioning Program PPT FinalAbdullah Yazıcı100% (1)
- Y Yyyy: Yyyy Y Yyyyyyyyyyy Y Yyy Yyyyyyy Yyyy Y YyyDocumento18 páginasY Yyyy: Yyyy Y Yyyyyyyyyyy Y Yyy Yyyyyyy Yyyy Y Yyykcc2012Ainda não há avaliações
- 13 Principles of Sterile TechniqueDocumento3 páginas13 Principles of Sterile TechniqueOlive Keithy Ascaño ReyesAinda não há avaliações
- Open BiteDocumento36 páginasOpen BiteWasiAliMemon67% (3)
- 5 Reqs For Occlusal StabilityDocumento2 páginas5 Reqs For Occlusal StabilityNirav MehtaAinda não há avaliações
- Dentistry Semester 1 SAQDocumento4 páginasDentistry Semester 1 SAQKan Chang YuAinda não há avaliações
- Callanetics PhysicalDocumento17 páginasCallanetics PhysicalASAP teleAinda não há avaliações
- Spinningbabies Daily Pelvic Floor ExercisesDocumento1 páginaSpinningbabies Daily Pelvic Floor ExercisesFederica FarfallaAinda não há avaliações
- PMRDocumento17 páginasPMRJoy SinghAinda não há avaliações