Escolar Documentos
Profissional Documentos
Cultura Documentos
Pencitraan Hepar Dan Traktus Biliaris
Enviado por
Imam FahriTítulo original
Direitos autorais
Formatos disponíveis
Compartilhar este documento
Compartilhar ou incorporar documento
Você considera este documento útil?
Este conteúdo é inapropriado?
Denunciar este documentoDireitos autorais:
Formatos disponíveis
Pencitraan Hepar Dan Traktus Biliaris
Enviado por
Imam FahriDireitos autorais:
Formatos disponíveis
ASSESSMENT OF LIVER DISEASE
Imaging the liver and biliary
tract
Whats new?
C
Tom L Kaye
J Ashley Guthrie
Abstract
A variety of modalities is available to image the liver and biliary tract,
many offering complementary information, with a combination of techniques often being required to make the diagnosis or determine optimal
patient management. Ultrasound is commonly used as the primary investigation as it is safe, cheap and widely available. Computed tomography
has a central role for emergency imaging, cancer diagnosis and staging,
and assessment of treatment response. Magnetic resonance imaging is
excellent for interrogating the liver parenchyma, and is the modality of
choice for characterizing a focal liver lesion and non-invasive investigation of the biliary tree. The addition of hepatobiliary contrast agents
and diffusion-weighted imaging has further improved accuracy. This
article describes the role of each of these modalities, highlighting several
common, benign and malignant hepatobiliary disease processes. Other
less commonly used modalities such as PET/CT and cholescintigraphy
are described and various hepatobiliary interventional techniques are
summarized.
shadowing. Adenomyomatosis and chronic cholecystitis are
other common benign causes of mural thickening demonstrated on US. Carcinoma of the gallbladder can present as a
polypoid luminal tumour or as diffuse wall thickening and is
often difficult to differentiate from benign conditions. Gallbladders containing polyps >1 cm are generally resected due
to such difficulties.
US has a major role in identifying biliary dilatation in the
context of jaundice or right upper quadrant pain, which may be
caused by obstructive pathology (duct stones, benign or malignant strictures), but dilatation is also found after cholecystectomy, prolonged fasting or with sphincter of Oddi dysfunction.
The common hepatic duct (CHD) normally measures up to 6 mm
until age 60, with a further allowance of 1 mm per decade
thereafter.3 The double duct sign refers to dilatation of the
pancreatic (>4 mm) and common duct, which is suggestive of a
pancreatic head or ampullary tumour and is usually further
investigated by multiphasic computed tomography (CT).
Keywords Bile ducts; biliary tract diseases; cholangiography; computed
tomography; liver; liver diseases; magnetic resonance imaging; positronemission tomography; ultrasonography
Ultrasonography
Ultrasonography (US) remains the most widely performed primary investigation for suspected hepatobiliary disease, owing to
its wide availability and avoidance of ionizing radiation.
Biliary disease
In the fasted state, the gallbladder appears on US as an oval
hypo-echoic structure with a smooth thin wall. Gallstones
usually appear as mobile echogenic foci with posterior
acoustic shadowing, and are identified with >95% accuracy in
the gallbladder, but less so in the common bile duct due
to adjacent bowel gas.1 The US findings in acute cholecystitis
include mural thickening (>3 mm), pericholecystic fluid and
a positive sonographic Murphys sign (Figure 1).2 Gallbladder
polyps appear as fixed luminal defects without acoustic
Liver disease
The normal liver has a uniform and homogenous echotexture.
Fatty infiltration gives a diffusely echogenic liver, with attenuation of the US beam as it passes deep into the organ. With the
recognition of non-alcoholic fatty liver disease as a cause of
chronic liver disease there is interest in using US attenuation
parameters to quantify steatosis, although this is not established
as a clinical tool at present.
In cirrhosis the liver usually appears coarse and echogenic.
Common features include surface nodularity, atrophy of the right
lobe, hypertrophy of the caudate lobe and enlargement of the
gallbladder fossa and umbilical fissure. Associated findings
related to portal hypertension include reduced, reversed or absent portal vein flow, varices, splenomegaly and ascites.4
Changes in stiffness correlate with fibrosis, currently assessed
by invasive liver biopsy, and can now be quantified using US (or
magnetic resonance imaging; MRI) via techniques such as transient elastography (FibroScan), performed without generating
images, or shear-wave elastography, where stiffness is measured
in a region of interest while imaging the liver.5
Tom L Kaye BMBS BMedSci MSc(Edin) FRCR is a Radiology Registrar at St
Jamess University Hospital, Leeds, UK. Competing interests: none
declared.
J Ashley Guthrie MB BChir FRCR is a Consultant Radiologist at St Jamess
University Hospital, Leeds, UK. Competing interests: Dr Guthrie has
received honoraria for lecturing and chairing sessions for Bayer
HealthCare.
MEDICINE 43:10
Non-invasive quantitative US and MRI techniques are playing an
increasing role in the assessment of fibrosis, fat and iron in
parenchymal liver disease
The combination of liver-specific contrast agents, diffusionweighted imaging, and improved MRI technology has
increased the accuracy of focal liver lesion detection and
characterization, in many cases avoiding the need for biopsy
CT dose-reduction techniques such as iterative reconstruction
have been introduced, which can substantially reduce patient
dose in multi-phase hepatobiliary examinations
Image-guided ablative and endovascular treatments such as
RFA now have an established role in the treatment of hepatocellular carcinoma and unresectable hepatic malignancy
562
2015 Elsevier Ltd. All rights reserved.
ASSESSMENT OF LIVER DISEASE
Figure 1 (a) US image showing normal thin walled gallbladder. (b) acute calculous cholecystitis. The gallbladder wall is diffusely thickened (dashed white
arrows) and contains echogenic bile, with a gallstone impacted in the neck (solid white arrows).
bleeding.11,12 High-quality 3D reformats of hepatobiliary
vascular anatomy are useful for planning endovascular intervention in cases of vascular injury.
CT demonstrates complications of cholecystitis such as necrosis, perforation, or pericholecystic abscess (Figure 3). Intrahepatic or perihepatic fluid collections and abscesses are
accurately depicted and CT can facilitate drainage. In severe
acute pancreatitis CT is widely used for identifying complications
such as necrosis, collections or bleeding.
Doppler ultrasound
The frequency shift of an ultrasonic wave (Doppler effect) that
occurs when it is reflected from a moving target (such as blood)
can be used to create a colour map of blood flow and direction
(colour Doppler) or a targeted waveform of blood flow (spectral
Doppler). This is commonly used to interrogate the major hepatic
vessels in chronic liver disease and after liver transplantation.
Contrast-enhanced ultrasound (CEUS)
Grey-scale US has modest sensitivity (50e65%) for metastatic
disease and hepatocellular carcinoma (HCC).6,7 It can differentiate simple cysts reliably but is limited in the characterization of
solid focal lesions. CEUS improves both lesion detection and
characterization.8 It involves the intravenous injection of
microbubble contrast media. Benign lesions are usually iso- or
hyper-echoic to background liver in the late phase of enhancement (Figure 2). Although comparable to CT and MRI for lesion
detection and characterization in ideal circumstances,9 multiple
lesions and lesions near the diaphragm or obscured by bowel gas
are difficult to evaluate.
Hepatobiliary oncology imaging
Metastases are by far the most common malignant liver lesions,
exceeding primary liver tumours by a factor of at least twenty. CT
is used for staging and to assess response to treatment for the
majority of malignancies that metastasize to the liver and primary tumours arising from the liver, pancreas and biliary tree.
The blood supply to the liver is via the hepatic artery (25%) and
portal vein (75%), with most tumours taking their blood supply
from the hepatic artery and displaying a varying degree of
vascularity. Hypervascular tumours such as hepatocellular carcinoma (HCC) or neuroendocrine malignancy should be imaged
in the arterial phase to maximize contrast enhancement between
tumour and background liver.
The majority of metastases from other sources (such as
colorectal cancer) are hypovascular and best depicted on the
portal venous phase scan. Triple-phase CT (unenhanced, arterial
and portal venous phase) is used to clarify the cause of biliary
obstruction identified on US (when stones are not suspected) and
to stage pancreatic malignancy.13
Computed tomography
Modern multi-detector CT is widely used and versatile, allowing
rapid imaging of a large volume with high spatial resolution,
facilitating accurate multi-phase imaging of the liver and biliary
tree. Iodinated contrast is used for most examinations; it is
contra-indicated in those with severe renal impairment or a
history of anaphylactic reaction. The high-radiation dose of CT
should be considered (especially with multiphase imaging), but
can be reduced by decreasing scanning dose parameters, peak
kVp and mA. Increased computing power has enabled iterative
reconstruction techniques to further reduce dose.10
Characterization of liver lesions
In cases where MRI is contraindicated or unsuitable, multi-phase
CT may be used to characterize liver lesions. European and
American Liver Associations allow multiphasic CT to be used as
a non-invasive means of diagnosing HCC in patients with
cirrhosis. Key diagnostic criteria include arterial hypervascularity
with washout demonstrated on a portal venous or 3minute delayed acquisition.14,15 Benign lesions, such as
Imaging the acute abdomen
CT retains an important role for imaging in the emergency
situation. In major trauma, dual phase imaging or a military
protocol with a single biphasic contrast injection has a high accuracy for traumatic liver injuries and active arterial
MEDICINE 43:10
563
2015 Elsevier Ltd. All rights reserved.
ASSESSMENT OF LIVER DISEASE
Figure 2 (a) Grey scale US image in a 24-year-old female shows a well-defined isoechoic mass adjacent to the gallbladder fossa. (b) CEUS images shows
avid homogenous arterial enhancement within the lesion, (c) which is near isointense in the delayed phase with a faint central scar visible. (d) Subsequent coronal hepatobiliary phase MRI image shows persisting uptake of contrast with a central scar, confirming focal nodular hyperplasia (FNH).
interpretation. Both benign (iatrogenic, post-inflammatory or
secondary to primary sclerosing cholangitis (PSC)) and malignant strictures can be identified (Figure 4b). Malignant biliary
strictures tend to be longer, with wall thickening and an irregular
margin.19
Variant biliary anatomy is well demonstrated and MRCP can
identify the relationship between the pancreatic duct and cystic
pancreatic tumours. More recently, functional assessment of
biliary excretion and pancreatic exocrine function has become
possible using hepatobiliary contrast media and secretinstimulated MRCP, respectively. Direct cholangiography (ERCP)
has now been largely replaced as a diagnostic test, being reserved
for tissue biopsy, stone extraction or stent insertion.
haemangiomas, focal nodular hyperplasia (FNH) and adenomas,
can be identified although contrast resolution is inferior to MRI
and characterization of lesions smaller than 1 cm is poor.16
Magnetic resonance imaging
MRI is a versatile imaging technique, allowing manipulation of
sequence parameters to vary soft tissue contrast or obtain
structural data. It is the examination of choice for imaging
complex biliary disease and characterizing liver lesions in both
the normal and cirrhotic liver. MRI has excellent liver-to-lesion
contrast resolution and incurs no ionizing radiation. The addition of hepatocyte-specific contrast agents and diffusionweighted images (DWI) has further improved sensitivity and
specificity.17 Limitations include cost, length of examination
(particularly for unwell patients who cannot lie still), and contraindications such as pacemakers and implants.
Diffuse and focal liver disease
MRI can characterize both diffuse liver disease and focal liver
lesions, in certain cases obviating the need for biopsy. A standard
liver protocol usually includes T2-weighted sequences that provide an overview of anatomy and can help identify simple cysts
or haemangiomas. In- and out-of-phase T1 imaging is used to
identify cellular fat within a lesion (such as in adenomas, HCC or
areas of focal fatty infiltration), or to detect iron deposition in
haemochromatosis or haemosiderosis. Various contrast agents
can be used to achieve imaging in the arterial, portal venous and
delayed phases. MRI can be used accurately to quantify fat and
Biliary disease
Magnetic resonance cholangiopancreatography (MRCP) uses
heavily weighted T2 sequences to display static or slow-moving
fluid within the biliary tree and pancreatic duct. MRCP can
identify ductal stones as small as 2 mm with comparable accuracy to endoscopic retrograde cholangiopancreatography
(ERCP)18 (Figure 4a). Flow artefacts, intra-ductal gas and adjacent pulsatile vascular compression can lead to false-positive
MEDICINE 43:10
564
2015 Elsevier Ltd. All rights reserved.
ASSESSMENT OF LIVER DISEASE
Figure 3 Perforated cholecystitis with hepatic abscess. Coronal (a) and axial (b) contrast enhanced CT images show irregular thick walled gallbladder
containing a large stone (solid white arrows), with extensive multi-loculated hepatic abscess (dashed white arrows).
from primary and secondary malignant lesions. In both the
cirrhotic and non-cirrhotic liver, MRI is the investigation choice
for demonstrating the anatomical distribution of disease with
high accuracy before liver resection and transplantation.
iron, and MR elastography is under evaluation as a means of
measuring fibrosis.
Gadolinium chelates are commonly used and are confined to
the extracellular space, behaving in a similar way to iodinated
contrast used in CT. Hepatocyte-specific contrast agents (such as
gadobenate dimeglamine and gadoxetic acid) show a degree of
active uptake by lesions with hepatocyte function and are
excreted into the bile, providing additional information about the
cellular constituents of a focal lesion.
The use of DWI gives unique information about the movement of water molecules at the cellular level. Malignant lesions
have a significantly lower apparent diffusion co-efficient (ADC)
and display greater diffusion restriction than benign lesions
(Figure 5).20 DWI is particularly useful in the detection of malignant lesions in the non-cirrhotic liver.
MRI allows accurate characterization of benign liver lesions,
such as haemangiomas, adenomas and FNH, differentiating them
Positron emission tomography e CT
FDG (2-[fluorine-18]fluoro-2-deoxy-D-glucose) positron emission
tomography with CT (PET/CT) is a functional imaging technique
using a glucose analogue that is taken up by metabolically active
tissues and tumour cells. PET/CT is frequently used for demonstrating disseminated malignant disease and may identify occult
primary tumours in patients with metastatic liver disease from an
unknown primary. It is unreliable for the identification of HCC
(although a high standardized uptake value (SUV) correlates
with poor differentiation21) and is inferior to MRI for identification of liver metastases. It may improve the detection rate of
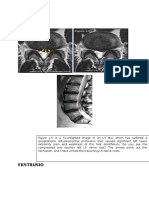
Figure 4 (a) Reconstructed MRCP maximum intensity projection (MIP) showing proximal biliary dilatation with a 9 mm calculus in the common bile duct
(solid white arrow). (b) Reconstructed MRCP MIP showing the classic findings of primary sclerosing cholangitis (PSC) with beading, stricturing and
diverticula affecting the intrahepatic ducts. A dominant CBD stricture (dashed white arrow) was investigated for cholangiocarcinoma but was found to be
inflammatory.
MEDICINE 43:10
565
2015 Elsevier Ltd. All rights reserved.
ASSESSMENT OF LIVER DISEASE
Figure 5 Typical MRI appearances of a HCC. (a) T2 axial image shows mildly hyperintense lesion in the left lobe. (b)e(d) Arterial, hepatobiliary phase and
DWI axial images after gadoxetate disodium show arterial enhancement, reduced uptake of hepatobiliary contrast and diffusion restriction.
evaluated. EUS is more sensitive than US or CT for detecting
early chronic pancreatitis, biliary microlithiasis and small
pancreatic or ampullary masses. Fine-needle aspiration of lymph
nodes and solid and cystic pancreatic lesions can be performed.22
occult metastatic disease in HCC (as these tend to be less well
differentiated tumours), cholangiocarcinoma and gallbladder
cancer but is not in widespread use for detecting these tumours.
It can differentiate benign from malignant liver lesions, the latter
usually having an SUV of greater than 3.5.21 PET/CT is
commonly used to identify occult metastatic disease in patients
with colorectal liver metastases being assessed for liver resection. Limitations include cost, low spatial resolution, large radiation burden and lack of specificity.
Hepatic interventional oncology
Percutaneous radio-frequency ablation (RFA) is an accepted
treatment modality for unresectable HCC and liver metastases.
A needle is introduced into the tumour under US or CT guidance and rapidly alternating current produces frictional heat
leading to liquefactive necrosis. Local disease control is achieved in up to 98% of patients with colorectal liver metastases
<3e4 cm and for HCC <5 cm 4-year survival is comparable to
surgery.23 Alternative ablative therapies include cryotherapy,
microwave and laser therapy and high-intensity focused US.
These may be combined with endovascular treatments such as
trans-arterial chemoembolization (TACE) or Yttrium-90 radioembolization in which microspheres are delivered to the
tumour and emit beta radiation. Successfully ablated lesions
followed up with CT show no residual internal enhancement,
sometimes with intra-lesional air bubbles and a surrounding
hypervascular rim.24
A
Cholescintigraphy
This technique involves an intravenous injection of a
technetium-99 labelled hepatobiliary iminodiacetic acid (99m TcHIDA), which is taken up by the liver and excreted in the bile.
The technique retains an important role in the paediatric setting,
differentiating between biliary atresia and neonatal hepatitis. In
biliary atresia there is good hepatic uptake but no excretion into
the bowel 24 hours after injection. It is rarely used as a first-line
investigation in the diagnosis of acute cholecystitis, although it is
highly accurate. Absence of activity in the gallbladder after
4 hours is diagnostic as HIDA cannot enter through an inflamed
and oedematous cystic duct. False positives can occur due to
underlying liver disease or after a prolonged fast.
REFERENCES
1 Cronan JJ. US diagnosis of choledocolithiasis: a re-appraisal. Radiology 1986; 161: 133e4.
2 Trowbridge RL, Rutkowski NK, Shojania KG. Does this patient have
acute cholecystitis. JAMA 2009; 289: 80e6.
Endoscopic US (EUS)
EUS is an invasive technique in which a high-frequency transducer is attached to the tip of an endoscope. The left lobe of the
liver, pancreas, biliary tree, and associated nodal chains can be
MEDICINE 43:10
566
2015 Elsevier Ltd. All rights reserved.
ASSESSMENT OF LIVER DISEASE
3 Wu CC, Ho YH, Chen CY. Effect of aging on common bile duct diameter: a real-time ultrasonographic study. J Clin Ultrasound 1984; 12:
473e8.
4 Murakami T, Mochizuki K, Nakamura H. Imaging evaluation of the
cirrhotic liver. Semin Liver Dis 2001; 21: 213e24.
5 Frulio N, Trillaud H. Ultrasound elastography in liver. Diagn Interv
Imaging 2013; 94: 515e34.
6 Schima W, Kulinna C, Langenberger H, et al. Liver metastases of
colorectal cancer: US, CT or MR. Cancer Imaging 2005; 5: 149e56.
7 Memon WA, Haider Z, Beg MA, et al. Diagnosis of hepatoma using
greyscale and Doppler ultrasound in patients with chronic liver disease. Int J Gen Med 2011; 4: 751e4.
8 National Institute for Health and Care Excellence. SonoVue ( sulphur
hexafluoride microbubbles) contrast agent for contrast-enhanced
ultrasound imaging of the liver. London (UK): NICE diagnostics
guidance (DG5), 2012.
9 Ryu SW, Bok GH, Jang JY, et al. Clinically useful diagnostic tool of
contrast enhanced ultrasonography for focal liver masses: comparison to computed tomography and magnetic resonance imaging. Gut
Liver 2014; 8: 292e7.
10 Silva AC, Lawder HJ, Hara A, et al. Innovations in CT dose reduction
strategy: application of the adaptive statistical iterative reconstruction algorithm. AJR Am J Roentgenol 2010; 194: 191e9.
11 Yoon W, Jeong YY, Kim JK, et al. CT in blunt liver trauma. Radiographics 2005; 25: 87e104.
12 Graham RNJ. Battlefield radiology. Br J Radiol 2012; 85: 1556e65.
13 Guthrie AJ, Sheridan MB. Investigation of abdominal pain to detect
pancreatic cancer. BMJ 2008; 336: 1067e9.
14 European Association For The Study Of The Liver, European Organisation For Research And Treatment Of Cancer. EASL-EORTC clinical
practice guidelines: management of hepatocellular carcinoma.
J Hepatol 2012; 56: 908e43.
MEDICINE 43:10
15 Bruix J, Sherman M, American Association for the Study of Liver
Diseases. Management of hepatocellular carcinoma: an update.
Hepatology 2011; 53: 1020e2.
16 Semelka RC, Martin DR, Balci C, et al. Focal liver lesions: comparison
of dual-phase CT and multisequence multiplanar MR imaging
including dynamic gadolinium enhancement. J Magn Reson Imaging
2001; 13: 397e401.
17 Frydrychowicz A, Lubner MG, Brown JJ, et al. Hepatobiliary MR imaging with gadolinium-based contrast agents. J Magn Reson Imaging
2012; 35: 492e511.
18 Griffin N, Charles-Edwards G, Grant LA. Magnetic resonance cholangiopancreatography: the ABC or MRCP. Insights Imaging 2012; 3:
11e21.
19 Shanbhogue AKP, Tirumani SH, Prasad SR, et al. Benign biliary
strictures: a current comprehensive clinical and imaging review. AJR
2011; 197: 295e306.
20 Parikh T, Drew SJ, Lee VS, et al. Focal liver lesion detection and
characterization with diffusion-weighted MR imaging: comparison
with standard breath-hold T2-weighted imaging. Radiology 2008;
246: 812e22.
21 Sacks A, Peller PJ, Surasi DS, et al. Value of PET/CT in the management of primary hepatobiliary tumors, part 2. AJR 2011; 197: 260e5.
22 Schwartz DA, Wiersema MJ. The role of endoscopic ultrasound in
hepatobiliary disease. Curr Gastroenterol Rep 2002; 4: 72e8.
23 Gervais DA, Goldberg SN, Brown DB, et al. Society of interventional
radiology position statement on percutaneous radiofrequency ablation for the treatment of liver tumors. J Vasc Interv Radiol 2009; 20:
342e7.
24 Park MH, Rhim H, Kim YS. Spectrum of CT findings after radiofrequency ablation of hepatic tumors. Radiographics 2008; 28:
379e90.
567
2015 Elsevier Ltd. All rights reserved.
Você também pode gostar
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeNo EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeNota: 4 de 5 estrelas4/5 (5794)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreNo EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreNota: 4 de 5 estrelas4/5 (1090)
- Never Split the Difference: Negotiating As If Your Life Depended On ItNo EverandNever Split the Difference: Negotiating As If Your Life Depended On ItNota: 4.5 de 5 estrelas4.5/5 (838)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceNo EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceNota: 4 de 5 estrelas4/5 (894)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureNo EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureNota: 4.5 de 5 estrelas4.5/5 (474)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersNo EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersNota: 4.5 de 5 estrelas4.5/5 (344)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)No EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Nota: 4.5 de 5 estrelas4.5/5 (119)
- The Emperor of All Maladies: A Biography of CancerNo EverandThe Emperor of All Maladies: A Biography of CancerNota: 4.5 de 5 estrelas4.5/5 (271)
- The Little Book of Hygge: Danish Secrets to Happy LivingNo EverandThe Little Book of Hygge: Danish Secrets to Happy LivingNota: 3.5 de 5 estrelas3.5/5 (399)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyNo EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyNota: 3.5 de 5 estrelas3.5/5 (2219)
- The Yellow House: A Memoir (2019 National Book Award Winner)No EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Nota: 4 de 5 estrelas4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaNo EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaNota: 4.5 de 5 estrelas4.5/5 (265)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryNo EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryNota: 3.5 de 5 estrelas3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnNo EverandTeam of Rivals: The Political Genius of Abraham LincolnNota: 4.5 de 5 estrelas4.5/5 (234)
- Dynamic Approach To Discounting Patient ShareDocumento11 páginasDynamic Approach To Discounting Patient SharemaleticjAinda não há avaliações
- The Unwinding: An Inner History of the New AmericaNo EverandThe Unwinding: An Inner History of the New AmericaNota: 4 de 5 estrelas4/5 (45)
- Respiratory Physiology AnswersDocumento4 páginasRespiratory Physiology AnswersRamya100% (2)
- AMBROKSOLDocumento1 páginaAMBROKSOLImam FahriAinda não há avaliações
- Background Information On The ProcedureDocumento3 páginasBackground Information On The ProcedureImam FahriAinda não há avaliações
- Daftar PustakaDocumento3 páginasDaftar PustakaImam FahriAinda não há avaliações
- AMBROKSOLDocumento1 páginaAMBROKSOLImam FahriAinda não há avaliações
- Irritable Bowel Syndrome: Nur Safira AnanditaDocumento9 páginasIrritable Bowel Syndrome: Nur Safira AnanditaLestiaAinda não há avaliações
- Background Information On The ProcedureDocumento3 páginasBackground Information On The ProcedureImam FahriAinda não há avaliações
- Background Information On The ProcedureDocumento3 páginasBackground Information On The ProcedureImam FahriAinda não há avaliações
- Background Information On The ProcedureDocumento3 páginasBackground Information On The ProcedureImam FahriAinda não há avaliações
- Requirement RRDocumento2 páginasRequirement RRImam FahriAinda não há avaliações
- PROTUSIODocumento6 páginasPROTUSIOImam FahriAinda não há avaliações
- Nomer 12 FarmakologiDocumento9 páginasNomer 12 FarmakologiAyuagung Chandra Maha DewiAinda não há avaliações
- Pharmacology: Drugs That Affect The: Nervous SystemDocumento84 páginasPharmacology: Drugs That Affect The: Nervous SystemSameh Saber100% (1)
- MISC64 L2 Diabetesand Nutrition 1Documento40 páginasMISC64 L2 Diabetesand Nutrition 1Imam FahriAinda não há avaliações
- Biliary Duct ImagingDocumento7 páginasBiliary Duct ImagingImam FahriAinda não há avaliações
- Lecture 16-17 - Opioids AnalgesicsDocumento20 páginasLecture 16-17 - Opioids AnalgesicsJedoAinda não há avaliações
- Iron Deficiency Anemia and Megaloblastic Anemia - Samson-Cruz MDDocumento47 páginasIron Deficiency Anemia and Megaloblastic Anemia - Samson-Cruz MDMiguel Cuevas DolotAinda não há avaliações
- Types of White Blood CellsDocumento2 páginasTypes of White Blood CellsPRINTDESK by DanAinda não há avaliações
- JMDH 400734 Application Benefits and Limitations of Telepharmacy For PDocumento9 páginasJMDH 400734 Application Benefits and Limitations of Telepharmacy For PIrma RahmawatiAinda não há avaliações
- Mandibular Molar Protraction With Temporary Anchorage DevicesDocumento5 páginasMandibular Molar Protraction With Temporary Anchorage Devicescarlosasd15Ainda não há avaliações
- CS HF Directory 2018 Print PDFDocumento80 páginasCS HF Directory 2018 Print PDFAt Day's WardAinda não há avaliações
- Mental RetardationDocumento11 páginasMental RetardationTherese Tee-DizonAinda não há avaliações
- Askin TumorDocumento6 páginasAskin TumorGaluh Kresna BayuAinda não há avaliações
- Case Study - MyomaDocumento54 páginasCase Study - Myomauvinr100% (1)
- Free Gingival Graft Procedure OverviewDocumento1 páginaFree Gingival Graft Procedure OverviewTenzin WangyalAinda não há avaliações
- TEMPLATE-B-Master-list-of-Learners-for-the-Pilot-Implementation-of-F2F-Classes-for-S.Y.-2021-2022Documento7 páginasTEMPLATE-B-Master-list-of-Learners-for-the-Pilot-Implementation-of-F2F-Classes-for-S.Y.-2021-2022Resa Consigna MagusaraAinda não há avaliações
- CapstoneDocumento40 páginasCapstoneDevanshi GoswamiAinda não há avaliações
- Treating Gout Uric Acid Tibb e NabwiDocumento11 páginasTreating Gout Uric Acid Tibb e Nabwinadeem uddinAinda não há avaliações
- MInTFM Programme Brochure 2019Documento12 páginasMInTFM Programme Brochure 2019Shoban RajAinda não há avaliações
- A New Drug-Shelf Arrangement For Reducing MedicatiDocumento9 páginasA New Drug-Shelf Arrangement For Reducing MedicatiEmmanuel LawerAinda não há avaliações
- Tabel Obat ObatanDocumento7 páginasTabel Obat ObatanMega Suciati100% (1)
- ProspectusDocumento52 páginasProspectusRabinder BakhshiAinda não há avaliações
- Mental Health Personal Statement - Docx'Documento2 páginasMental Health Personal Statement - Docx'delson2206Ainda não há avaliações
- Safe AnalgesicsDocumento3 páginasSafe AnalgesicsJohn SolisAinda não há avaliações
- Student study on family health and pregnancy in rural ZimbabweDocumento3 páginasStudent study on family health and pregnancy in rural ZimbabweTubocurareAinda não há avaliações
- Science Chapter on ReproductionDocumento4 páginasScience Chapter on ReproductionAnita GargAinda não há avaliações
- Symposiumbooklet CareerDocumento36 páginasSymposiumbooklet Careerroh009Ainda não há avaliações
- To Compare Rosuvastatin With Atorvastatin in Terms of Mean Change in LDL C in Patient With Diabetes PDFDocumento7 páginasTo Compare Rosuvastatin With Atorvastatin in Terms of Mean Change in LDL C in Patient With Diabetes PDFJez RarangAinda não há avaliações
- Healing Stories of People Final EditingDocumento53 páginasHealing Stories of People Final Editinggabyk6867% (3)
- Tilapia 4Documento69 páginasTilapia 4Annisa MeilaniAinda não há avaliações
- EEG ArtifactsDocumento18 páginasEEG ArtifactsNazwan Hassa100% (1)
- About Critical Care NursingDocumento7 páginasAbout Critical Care NursingaivynAinda não há avaliações
- Community Acquired PneumoniaDocumento63 páginasCommunity Acquired PneumoniaLet BorlagdanAinda não há avaliações