Escolar Documentos
Profissional Documentos
Cultura Documentos
Acute Traumatic Posterior Shoulder Dislocation PDF
Enviado por
Muhammad Pringgo ArifiantoTítulo original
Direitos autorais
Formatos disponíveis
Compartilhar este documento
Compartilhar ou incorporar documento
Você considera este documento útil?
Este conteúdo é inapropriado?
Denunciar este documentoDireitos autorais:
Formatos disponíveis
Acute Traumatic Posterior Shoulder Dislocation PDF
Enviado por
Muhammad Pringgo ArifiantoDireitos autorais:
Formatos disponíveis
Review Article
Acute Traumatic Posterior
Shoulder Dislocation
Abstract
Dominique M. Rouleau, MD
Jonah Hebert-Davies, MD
C. Michael Robinson, MD
From the Department of Orthopaedic
Surgery, University of Montreal,
Sacred Heart Hospital of Montreal,
Montreal, ON, Canada (Dr. Rouleau
and Dr. Hebert-Davies), and the Royal
Infirmary of Edinburgh, Edinburgh,
UK (Dr. Robinson).
Dr. Rouleau or an immediate family
member is a member of a speakers
bureau or has made paid presentations
on behalf of Smith & Nephew; has
received research or institutional
support from DePuy, KCI, Smith &
Nephew, Stryker, Synthes, and
Zimmer; and has received nonincome
support (such as equipment or
services), commercially derived
honoraria, or other nonresearchrelated funding (such as paid travel)
from Arthrex. Dr. Robinson or an
immediate family member is a member
of a speakers bureau or has made
paid presentations on behalf of and
serves as a paid consultant to Acumed.
Neither Dr. Hebert-Davies nor any
immediate family member has received
anything of value from or has stock or
stock options held in a commercial
company or institution related directly
or indirectly to the subject of this article.
J Am Acad Orthop Surg 2014;22:
145-152
http://dx.doi.org/10.5435/
JAAOS-22-03-145
Copyright 2014 by the American
Academy of Orthopaedic Surgeons.
March 2014, Vol 22, No 3
Posterior shoulder dislocation occurs rarely and is challenging to
manage. The mechanisms of trauma are varied, which complicates
diagnosis. Missed or delayed diagnosis and treatment can have
serious deleterious effects on shoulder function. All cases of
suspected posterior shoulder dislocation require a high level of
suspicion and appropriate imaging. Identification of associated
injuries, such as fractures and rotator cuff tears, is important to guide
treatment. In the acute setting, most patients are treated with closed or
open reduction with additional soft-tissue or bony procedures.
Patients treated in a delayed fashion for persistent instability may
require additional procedures, including arthroplasty.
irst described in 1838 by Sir Astley
Cooper,1 traumatic posterior
dislocations of the shoulder represent
an unusual and challenging clinical
problem. These injuries account for
2% to 5% of all shoulder dislocations.1-3 Anterior glenohumeral
dislocation is 15.5 to 21.7 times more
common than posterior dislocation.4
Seizures, high-energy trauma, and
electrocution are associated with
a much greater risk of posterior
dislocation.1,2,5 Diagnosis is missed
or delayed in up to 79% of patients.2,3,6 The authors of one study
suggested that systematic evaluation
of AP and Velpeau radiographs in an
emergency department resulted in
dislocation being missed in only 10
of 112 patients.4
In patients who present following
seizure, electric shock, or trauma,
a high index of suspicion for posterior
shoulder dislocation should be maintained, and appropriate physical and
radiologic examinations should be
performed to confirm the diagnosis.7
This is particularly important in the
setting of seizure, in which medical
treatment combined with reduced
nociceptive sensitivity following
convulsions may make it difficult
for the treating physician to detect
the injury.8 Early identification of
these dislocations reduces morbidity
and facilitates treatment.3
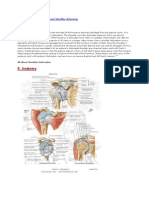
Anatomy of the Shoulder
The shoulder is relatively unconstrained, allowing an extreme range
of motion. Joint stability is provided
by both static and dynamic elements,9 which allows the joint to
maintain a large degree of freedom
while remaining concentric.
Static Stabilizers
Bony congruity is achieved with the
concavity of the glenoid; this is further
increased due to asymmetric deposition
of cartilage, with the peripheral articular surface being thickest.10,11 The glenoid labrum increases the depth and
width of the joint approximately twofold.12 Loss of the labrum decreases
translational resistance by 20%.13
The three glenohumeral ligaments
are discrete capsular fibrous bands
145
Copyright the American Academy of Orthopaedic Surgeons. Unauthorized reproduction of this article is prohibited.
Acute Traumatic Posterior Shoulder Dislocation
pectoralis and latissimus dorsi muscles
overpower the weak external rotators
(ie, infraspinatus, teres minor) and
cause internal rotation of the shoulder,
displacing the humeral head superiorly
and posteriorly against the acromion
and medially against the glenoid fossa,
resulting in posterior dislocation.8,16
Adequate muscle contraction strength
of the infraspinatus and teres minor
and major can cause humeral neck
fracture. In a recent systematic review,
posterior dislocations were found to
occur after trauma in 67% of cases,
after seizure in 31%, and after electrocution in 2%.4
Figure 1
Classifications
Illustration of the dynamic and static stabilizers of the shoulder. IGHL = inferior
glenohumeral ligament, MGHL = middle glenohumeral ligament, SGHL = superior
glenohumeral ligament
that provide stability to the shoulder in
various positions. The coracohumeral
ligament and superior glenohumeral
ligament provide little anterior resistance, but they help prevent posterior
translation in the flexed, adducted,
and internally rotated shoulder.12,14
The inferior glenohumeral ligament
is the main stabilizer against posterior
dislocation. The posterior band of
the inferior glenohumeral ligament
restricts posterior displacement with
the arm in abduction12 (Figure 1).
Dynamic Restraints
Dynamic stabilizers include all shoulder muscles that create a concavity
compression force across the joint.
Balance between anterior and posterior forces allows the humeral head
to remain centered in the glenoid.9
146
Posterior dynamic restraints of the
shoulder include the rotator cuff, the
biceps tendon, and the deltoid.12 The
subscapularis provides the greatest
opposition to posterior translation.12
The biceps tendon increases posterior
stability, mostly in external rotation.
Mechanisms of Injury
Several different mechanisms have
been proposed for posterior dislocation. Direct high-energy trauma with
the shoulder in adduction, flexion, and
internal rotation is the most frequent
cause of posterior dislocation.2,15
Posterior shoulder dislocation may
also be caused by seizures or electrocution.8 Dislocation due to seizure is
the result of unbalanced contraction of
the shoulder muscles.16 In adduction,
internal rotation, and flexion, the
Several classification systems exist to
describe posterior shoulder dislocations, but none has been established
as a clear standard. Detenbeck17 first
separated dislocations based on type:
acute, chronic (dislocated .3 weeks),
or recurrent (traumatic or atraumatic).
Heller et al18 developed a system
based on an extensive literature review
and included different parameters:
traumatic or atraumatic, acute or
persistent, or recurrent voluntary.
Others have classified dislocations as
acute (,6 weeks) or chronic (.6
months) and have separated pure
dislocations from fracture-dislocations
(ie, any associated humeral fracture
except a reverse Hill-Sachs lesion).19
Robinson and Aderinto19 also classified humeral head defect as small
(,25%), medium (25% to 50%),
and large (.50%). Classification of
the humeral head defect is extremely
important for planning eventual surgical treatment. Classifications of
posterior recurrent instability and
atraumatic posterior instability are
beyond the scope of this article.20
Clinical Evaluation
Physical examination is particularly
important in acute posterior shoulder
Journal of the American Academy of Orthopaedic Surgeons
Copyright the American Academy of Orthopaedic Surgeons. Unauthorized reproduction of this article is prohibited.
Dominique M. Rouleau, MD, et al
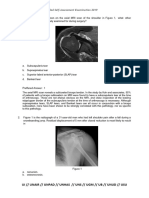
Figure 2
A, AP radiograph of the shoulder with the trough line visible (arrow). This is representative of the anterior humeral head
impaction. B, Axillary radiograph demonstrating posterior dislocation with a significant reverse Hill-Sachs lesion. C, AP
radiograph demonstrating the lightbulb sign (arrows).
dislocations because patients may be
unable to provide an adequate clinical
history. On visual inspection, the
shoulder often is in internal rotation,
with a prominent coracoid process and
posterior fullness in the axilla.1,3,21
Physical examination may reveal
a springy or soft end point or a block
to external rotation,1-3,21,22 as well as
the subtler sign of diminished supination of the forearm.6 Specific instability examinations such as the jerk test,
posterior load-and-shift test, or the
posterior drawer test can be useful
in patients with chronic instability.
However, these tests are rarely useful
in the acute setting.
Imaging
To minimize the risk of missing a posterior glenohumeral dislocation, the
evaluation should include standard
AP and Velpeau radiographs.1-4,21 An
axillary view is useful to evaluate
associated head impaction (ie, reverse
Hill-Sachs lesion) and glenoid rim
fractures.21 A Velpeau view is
acceptable if the patient is unable to
achieve sufficient abduction. Other
indirect signs that can be seen on
standard radiographs include the
lightbulb sign, loss of the half-moon
sign, and the trough line23 (Figure 2).
March 2014, Vol 22, No 3
CT is particularly useful for
preoperative assessment of associated fractures and quantification
of reverse Hill-Sachs impaction1,3,21,24,25 (Figure 3). Thin-slice
axial CT is the best imaging
modality for defining the humeral
head bone defect as part of the
articular surface.24
Capsulolabral and rotator cuff evaluation on MRI is essential in cases
without associated fracture7 (Figure 4).
Posterior labral lesions, such as reverse
Bankart lesions, posterior labrocapsular periosteal sleeve avulsions, and
posterosuperior tears, are found in up
to 58% of patients.26 In cases of
irreducible dislocation, MRI can
identify the responsible structure,
which most commonly is a torn rotator cuff, avulsed capsule, or biceps
tendon.26
Associated Injuries
Isolated posterior dislocations of the
proximal humerus are rare, and associated injuries often are missed or
diagnosed in a delayed fashion.7 Historically, bony and soft-tissue injuries
were thought to occur in 49% of
dislocations,21 but a recent systematic
review indicated that up to 65% of
dislocations had associated bony or
Figure 3
Axial CT scan demonstrating severe
humeral head impaction, that is,
reverse Hill-Sachs lesion. The extent
of glenoid fracture or bone loss
dictates management.
soft-tissue injuries.7 Simple or multiple
fractures were present in 34% of
shoulders, with the most common site
being the neck (55%), followed by
the lesser (42%) and greater (23%)
tuberosities.7 Lesser tuberosity fractures are particularly important
because they influence treatment. In
these cases, it is important to enter the
joint through the fracture rather than
perform a subscapularis tenotomy.
Reverse Hill-Sachs lesions of
varying size are seen in up to 86% of
147
Copyright the American Academy of Orthopaedic Surgeons. Unauthorized reproduction of this article is prohibited.
Acute Traumatic Posterior Shoulder Dislocation
Figure 4
Axial T1-weighted magnetic
resonance arthrogram of a right
shoulder demonstrating a posterior
Bankart lesion. The rotator cuff is
also assessed on this view.
patients.26 Bone defects are common, with significant reverse HillSachs lesions found in 29% of
shoulders7 and posterior rim fracture seen in approximately 5% of
shoulders.4 The frequency and significance of these defects can
increase with delayed or chronic
presentation.5
Rotator cuff tears are found in 13%
of patients evaluated with MRI;
however, the odds ratio of finding
a tear is 4.6 times higher in the
absence of an associated fracture or
reverse Hill-Sachs lesion.7 Thus, in
the patient with a dislocation but
without concomitant fracture on
CT, a focused rotator cuff physical
examination and MRI evaluation
are strongly suggested. Nerve palsy
secondary to posterior glenohumeral
dislocation is rare, occurring in ,1%
of injuries.7 The axillary nerve is the
most commonly injured.
Management
Nonsurgical
Definitive treatment options for posterior shoulder dislocations are varied,
and the decision must be individualized to each patient. In the elderly
148
low-demand patient, chronic posterior dislocation can be tolerated provided pain is minimal and anterior
elevation is sufficient for activities
of daily living.27,28 This treatment
option has been dubbed supervised
neglect.28,29 Nonsurgical treatment
also may be appropriate in patients
with cognitive impairment or other
severe medical comorbidities.
Closed reduction can be attempted
in the presence of an acute dislocation
in an elderly low-demand patient
with a reverse Hill-Sachs lesion measuring ,20%. Recurrent dislocation
or failed reduction warrants a discussion with the patient and family
about definitive treatment. In an
active and independent patient, the
goal of treatment of acute and
chronic dislocations is to restore
shoulder stability and mobility. Isolated closed reduction is reserved for
acute posterior instability with
a reverse Hill-Sachs lesion of #20%
that is stable after reduction.
Careful imaging evaluation should
be done prior to any reduction
maneuver to avoid displacing a neck
fracture. In the presence of suspected
fracture, an urgent CT scan should be
obtained before reduction. An attempt
at closed reduction of posterior shoulder dislocation requires complete
sedation to allow gentle manipulation.
Forceful manipulations often cause
humeral head fractures, which increases the chance of osteonecrosis and
has an adverse effect on prognosis. In
a series of 112 patients, 33% of
shoulders were successfully reduced
using in-line gentle traction.4
The Stimson technique is a passive
method used to manage acute posterior dislocation without associated
neck fracture or a significantly engaged
reverse Hill-Sachs lesion. The patient is
positioned prone on a table with the
arm in abduction over the side and
with 5 to 10 lb placed in the hand.30
Muscle spasms can eventually be
overcome with the weight to allow for
spontaneous reduction.
Another method of closed reduction involves manipulating the
shoulder into adduction, anterior
flexion, and internal rotation. This is
followed by longitudinal traction
and anteriorly directed pressure on
the humeral head. As the humeral
head is felt to translate anteriorly,
progressive external rotation and
extension is done. Caution is required
at this stage because initiating rotation before humeral head translation
may cause humeral head fracture.
Residual instability following closed
reduction with the arm in the neutral
position warrants surgical management provided the patient is medically
fit to undergo anesthesia.
Surgical
Open Reduction
Following unsuccessful closed reduction, open reduction can be done
through either an anterior or a posterior approach. The approach is determined based on preoperative planning.
Isolated open reduction can be successful in acute dislocations with
reverse Hill-Sachs lesions measuring
,20%.
An anterior approach is done via
a standard deltopectoral incision,
where the humeral head lies deeper than
usual. Initially, the rotator interval is
opened to allow the introduction of
a finger into the glenohumeral joint to
aid in manual reduction of the shoulder.
In cases in which the shoulder is not
reducible through an open rotator
interval alone, a formal arthrotomy is
necessary. Management of the subscapularis is crucial and is dictated by
associated fractures. The two options
are peeling of the subscapularis and
lesser tuberosity osteotomy. In the setting of persistent posterior dislocation,
locked internal rotation limits access to
the subscapularis. The long head of the
biceps is useful in identifying the lateral
margin; frequently, the subscapularis
tendon lies beneath the conjoined
tendon.
Journal of the American Academy of Orthopaedic Surgeons
Copyright the American Academy of Orthopaedic Surgeons. Unauthorized reproduction of this article is prohibited.
Dominique M. Rouleau, MD, et al
mended to prevent contact between
the grafted zone and the glenoid.
Figure 5
formed approximately 1 cm deep to
the bicipital groove in the sagittal
plane. A second cut is made from the
rotator interval in the coronal plane
from the reverse Hill-Sachs lesion
medially to the groove laterally. This
cut is possible only if the rotator
interval is open. Careful manipulation
of the lesser tuberosity is required to
prevent fragmentation.
Posterior Open Bankart Procedure
Irreducible posterior shoulder dislocations or persistent instability after
closed reduction without a significant
reverse Hill-Sachs lesion (#20%) can
be managed with a posterior approach
to achieve reduction, followed by
posterior Bankart repair33 (Figure 7).
A posterior longitudinal incision is
made medial to the deltoid border in
line with the posterior joint. Inferior
dissection must be done carefully to
prevent injury to the axillary nerve.
The deltoid is lifted with a retractor,
after which the infraspinatus is visualized and transverse tenotomy is
performed in line with the capsule.
The posterior labrum and capsule are
repaired in a standard fashion. Alternatively, the approach can be done
through a longitudinal split between
the infraspinatus and teres minor. This
approach allows excellent exposure
of the labrum complex without posterior tendon tenotomy. The interval
between these muscles is not always
obvious. Typically, it can be found
2 cm inferior to the scapular spine. It is
harder to see the separation at the
tendinous portion, and a longitudinal
tenotomy is usually necessary. Alternatively, on palpation, the humeral
head is usually felt deep to the infraspinatus, whereas the inferior portion
of the teres minor feels soft on
palpation.
Anterior Approach and Bone
Grafting
Significant acute reverse Hill-Sachs
lesions (20% to 40%) can also be addressed with disimpaction and bone
grafting or allograft (Figure 6). The
ideal patient for these techniques is
young, with good healing potential.
Following fracture disimpaction, an
iliac crest bone graft can be inserted
under the cartilage for support.32
Postoperative use of an external
rotation splint for 4 weeks is recom-
Arthroscopic Posterior Bankart
Repair
Arthroscopic posterior Bankart repair
is an option for acute reducible dislocations with little or no humeral head
impaction (,20%) and with persistent instability. The arthroscope is
introduced through the anterior portal, and a posterolateral portal is used
for suture anchor placement. A posterosuperior portal is used for suture
management. The posterior portion of
the acromion may prevent vertical
A, Axial (top) and AP (bottom) illustrations of a shoulder with a reverse Hill-Sachs
lesion. The AP view illustrates a modified McLaughlin procedure, which is done
through a transsubscapularis approach. B, Axial (top) and AP (bottom)
illustrations of the shoulder following suture of the subscapularis tendon into the
defect with the help of suture anchors and subsequent repair of that approach
through the tendon.
The McLaughlin Procedure
For patients with reverse Hill-Sachs
lesions of #20% and with persistent
instability following reduction, the
subscapularis can be either lifted off
the lesser tuberosity and transposed
into the defect with transosseous sutures after reduction as originally
described by McLaughlin2 or sutured
into the bed of the defect.31 The circumflex vessels are preserved inferiorly by maintaining a small sleeve of
tendon attached to its original site.
Modified McLaughlin Procedure
In the presence of a significant reverse
Hill-Sachs lesion (20% to 40%), the
lesser tuberosity can be osteotomized
to access the joint and eventually
transposed to the bone defect after
joint reduction.21 This is known as
the modified McLaughlin procedure
(Figure 5). The osteotomy is perMarch 2014, Vol 22, No 3
149
Copyright the American Academy of Orthopaedic Surgeons. Unauthorized reproduction of this article is prohibited.
Acute Traumatic Posterior Shoulder Dislocation
Figure 6
A, Axial CT scan of a left shoulder with significant humeral head impaction. B, Axial CT scan of the same patient 3 months
after an allograft was implanted into the deficit. C, Axial CT scan of a different patient with a similar injury 3 months after
fracture disimpaction.
Figure 7
Illustration of the skin landmarks
used in the posterior approach
(represented by the dashed line)
used to manage irreducible posterior
shoulder dislocation or persistent
instability after closed reduction in
the absence of a significant reverse
Hill-Sachs lesion. Access to the joint
is achieved either through
infraspinatus tenotomy or between
the infraspinatus and the teres minor.
positioning of suture anchors, and the
surgeon must have at the ready
a variety of suture passers to accommodate the anatomy in this area.
Arthroplasty
In the presence of massive humeral head
impaction (.40%) in patients aged
150
,55 years or in patients who are
not good candidates for graft incorporation, hemiarthroplasty is a good
option to address both instability
and the articular surface deficit.33
In order to prevent postoperative
dislocation, the humeral head must
be positioned in normal retroversion (#20). In more severe cases
of residual instability, the posterior
labrum can be repaired before
prosthesis implantation. Through
an anterior approach, the humeral
head is excised and the humeral cut
is oriented parallel to the glenoid,
leaving 1 to 2 cm of joint space to
visualize the posterior labrum. Use
of a laminar spreader and gentle
lateral traction can improve visualization. In a right shoulder, the
first glenoid anchor is positioned at
the 7-oclock position and the second at the 9-oclock position.
The anchor is placed at the edge of
the cartilage at a 45 angle to the
joint surface. A free 2/3 circular
needle is usually sufficient to pass
the anchor suture through the posterior labrum and capsule. Following repair of the labrum, the
hemiarthroplasty can be performed
as usual. A treatment algorithm is
shown in Figure 8.
Rehabilitation
Regardless of management type, the
shoulder is braced in 20 of external
rotation and abduction for 4 weeks to
aid healing of the posterior capsule.
Pendulum exercises and elbow range
of motion three times per day are
encouraged. At 4 weeks, unlimited
progressive range of motion is initiated
as well as isometric posterior rotator
cuff strengthening. Noncontact sports
are allowed 3 months after reduction or
surgery, and contact sports are permitted 4 to 6 months postoperatively.
Results
Approximately 18% of patients experience recurrent instability in the first
year following acute posterior dislocation.4 Risk factors for recurrence are
age ,40 years, seizure, and large
reverse Hill-Sachs lesion (.1.5 cm3).
Persistent functional impairment has
been noted 2 years after the initial
trauma, even without recurrent instability.4 Activities that require significant internal rotation may be
particularly difficult.
Typically, patients with persistent symptoms present with either
Journal of the American Academy of Orthopaedic Surgeons
Copyright the American Academy of Orthopaedic Surgeons. Unauthorized reproduction of this article is prohibited.
Dominique M. Rouleau, MD, et al
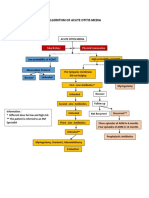
Figure 8
Treatment algorithm for the surgical management of acute posterior shoulder dislocation.
subjective or objective posterior
instability and a painful shoulder.
On physical examination, apprehension is seen with the shoulder in
adduction and forward elevation.
Most patients will present additional
symptoms with a posteriorly directed
translational force of the humerus.
Compensatory scapular winging can
be seen with anterior shoulder elevation.9 For these patients, imaging
should include magnetic resonance
arthrography of the shoulder. Treatments include all modalities of nonsurgical treatment as well as surgical
management of refractory cases. PosMarch 2014, Vol 22, No 3
terior capsular plication and posterior
Bankart repair have been reported to
improve both function and pain.34
Summary
Posterior shoulder dislocation is a relatively uncommon pathology, with
several typical modes of presentation.
Dislocation often goes undiagnosed in
the acute setting in patients who present following seizure, electric shock, or
high-energy trauma. Thus, particular
attention is required to diagnose the
injury in these patients. Imaging stud-
ies should always include an axillary
or equivalent radiograph. CT and
MRI are both useful to diagnose
associated injuries, which are much
more frequent than previously
thought. Treatment is individualized
to each patient based on timing
of presentation, size of the reverse
Hill-Sachs lesion, and the presence of
associated injuries (ie, fracture, rotator
cuff tear, glenoid bone loss). Younger
patients are treated with soft-tissue
management with or without a bony
procedure, whereas older patients
may require arthroplasty to maintain
stability.
151
Copyright the American Academy of Orthopaedic Surgeons. Unauthorized reproduction of this article is prohibited.
Acute Traumatic Posterior Shoulder Dislocation
References
Evidence-based Medicine: Levels of
evidence are described in the table of
contents. In this article, reference 4 is
a level II study. Reference 7 is a level
III study. References 2, 3, 6, 8, 15,
16, 21, 22, 24, 26, 27, 29, and 31 are
level IV studies. Reference 28 is level
V expert opinion.
References printed in bold type are
those published within the past 5
years.
1. Kowalsky MS, Levine WN: Traumatic
posterior glenohumeral dislocation:
Classification, pathoanatomy, diagnosis,
and treatment. Orthop Clin North Am
2008;39(4):519-533, viii.
2. McLaughlin HL: Posterior dislocation of the
shoulder. J Bone Joint Surg Am 1952;24(3):
584-590.
3. Hatzis N, Kaar TK, Wirth MA,
Rockwood CA Jr: The often overlooked
posterior dislocation of the shoulder. Tex
Med 2001;97(11):62-67.
4. Robinson CM, Seah M, Akhtar MA: The
epidemiology, risk of recurrence, and
functional outcome after an acute traumatic
posterior dislocation of the shoulder. J Bone
Joint Surg Am 2011;93(17):1605-1613.
5. Hawkins RJ: Unrecognized dislocations of
the shoulder. Instr Course Lect 1985;34:
258-263.
6. Rowe CR, Zarins B: Chronic unreduced
dislocations of the shoulder. J Bone Joint
Surg Am 1982;64(4):494-505.
7. Rouleau DM, Hebert-Davies J: Incidence of
associated injury in posterior shoulder
dislocation: Systematic review of the literature.
J Orthop Trauma 2012;26(4):246-251.
8. Goudie EB, Murray IR, Robinson CM:
Instability of the shoulder following
seizures. J Bone Joint Surg Br 2012;94(6):
721-728.
9. Tjoumakaris FP, Bradley JP: Posterior shoulder
instability, in Galatz LM, ed: Orthopaedic
Knowledge Update: Shoulder and Elbow 3.
Rosemont, IL, American Academy of
Orthopaedic Surgeons, 2008, pp 313-320.
152
10. Matsen FA III: Letter: The biomechanics of
glenohumeral stability. J Bone Joint Surg
Am 2002;84(3):495-496.
11. Halder AM, Kuhl SG, Zobitz ME, Larson D,
An KN: Effects of the glenoid labrum and
glenohumeral abduction on stability of the
shoulder joint through concavitycompression: An in vitro study. J Bone Joint
Surg Am 2001;83(7):1062-1069.
12. Levine WN, Flatow EL: The
pathophysiology of shoulder instability.
Am J Sports Med 2000;28(6):910-917.
13. Lippitt S, Matsen F: Mechanisms of
glenohumeral joint stability. Clin Orthop
Relat Res 1993;(291):20-28.
14. Curl LA, Warren RF: Glenohumeral joint
stability: Selective cutting studies on the
static capsular restraints. Clin Orthop Relat
Res 1996;(330):54-65.
15. Robinson CM, Akhtar A, Mitchell M,
Beavis C: Complex posterior fracturedislocation of the shoulder: Epidemiology,
injury patterns, and results of operative
treatment. J Bone Joint Surg Am 2007;89(7):
1454-1466.
16. Shaw JL: Bilateral posterior fracturedislocation of the shoulder and other trauma
caused by convulsive seizures. J Bone Joint
Surg Am 1971;53(7):1437-1440.
17. Detenbeck LC: Posterior dislocations of the
shoulder. J Trauma 1972;12(3):183-192.
18. Heller KD, Forst J, Forst R, Cohen B:
Posterior dislocation of the shoulder:
Recommendations for a classification. Arch
Orthop Trauma Surg 1994;113(4):228-231.
19. Robinson CM, Aderinto J: Posterior
shoulder dislocations and fracturedislocations. J Bone Joint Surg Am
2005;87(3):639-650.
20. Millett PJ, Clavert P, Hatch GF III, Warner JJ:
Recurrent posterior shoulder instability. J Am
Acad Orthop Surg 2006;14(8):464-476.
21. Hawkins RJ, Neer CS II, Pianta RM,
Mendoza FX: Locked posterior dislocation
of the shoulder. J Bone Joint Surg Am 1987;
69(1):9-18.
22. Walch G, Boileau P, Martin B, Dejour H:
Unreduced posterior luxations and fracturesluxations of the shoulder: Apropos of 30
cases [French]. Rev Chir Orthop Reparatrice
Appar Mot 1990;76(8):546-558.
23. Cisternino SJ, Rogers LF, Stufflebam BC,
Kruglik GD: The trough line: A
radiographic sign of posterior shoulder
dislocation. AJR Am J Roentgenol 1978;
130(5):951-954.
24. Wadlington VR, Hendrix RW, Rogers LF:
Computed tomography of posterior
fracture-dislocations of the shoulder: Case
reports. J Trauma 1992;32(1):113-115.
25. Zissin R, Morag B, Apter S, Rubinstein Z:
Bilateral posterior glenohumeral fracturedislocation: CT appearance. Isr J Med Sci
1990;26(1):55-57.
26. Saupe N, White LM, Bleakney R, et al:
Acute traumatic posterior shoulder
dislocation: MR findings. Radiology 2008;
248(1):185-193.
27. Loebenberg MI, Cuomo F: The treatment
of chronic anterior and posterior
dislocations of the glenohumeral joint and
associated articular surface defects. Orthop
Clin North Am 2000;31(1):23-34.
28. Cicak N: Posterior dislocation of the
shoulder. J Bone Joint Surg Br 2004;86(3):
324-332.
29. Bhler M, Gerber C: Shoulder instability
related to epileptic seizures. J Shoulder
Elbow Surg 2002;11(4):339-344.
30. Court-Brown CM, McQueen MM,
Tornetta P III: Shoulder girdle, in
Tornetta P III, Einhorn TA, eds:
Orthopaedic Surgery Essentials: Trauma.
Philadelphia, PA, Lippincott, Williams
and Wilkins, 2006, pp 68-88.
31. Spencer EE Jr, Brems JJ: A simple technique
for management of locked posterior shoulder
dislocations: Report of two cases. J Shoulder
Elbow Surg 2005;14(6):650-652.
32.
Begin M, Gagey O, Soubeyrand M: Acute
bilateral posterior dislocation of the
shoulder: One-stage reconstruction of both
humeral heads with cancellous autograft
and cartilage preservation. Chir Main
2012;31(1):34-37.
33. Matsen FA III, Titelman RM, Lippitt SB,
Rockwood CA Jr, Wirth MA:
Glenohumeral instability, in
Rockwood CA Jr, Matsen FA III,
Wirth MA, Lippitt SB, eds: The Shoulder,
ed 3. Philadelphia, PA, Saunders Elsevier,
2004, vol 2, pp 655-794.
34. Bottoni CR, Franks BR, Moore JH,
DeBerardino TM, Taylor DC, Arciero RA:
Operative stabilization of posterior
shoulder instability. Am J Sports Med 2005;
33(7):996-1002.
Journal of the American Academy of Orthopaedic Surgeons
Copyright the American Academy of Orthopaedic Surgeons. Unauthorized reproduction of this article is prohibited.
Você também pode gostar
- Anterior Shoulder Instability in Sport Current Management RecommendationsDocumento12 páginasAnterior Shoulder Instability in Sport Current Management RecommendationsAlexie GlóriaAinda não há avaliações
- Posterior Shoulder Fracture-Dislocation: An Update With Treatment AlgorithmDocumento10 páginasPosterior Shoulder Fracture-Dislocation: An Update With Treatment AlgorithmAghnia NafilaAinda não há avaliações
- Shoulder DislocationDocumento44 páginasShoulder DislocationMazvita Maz MatipiraAinda não há avaliações
- Shoulder-Acromioclavicular Separation PDFDocumento13 páginasShoulder-Acromioclavicular Separation PDFFebrian ParuraAinda não há avaliações
- Shoulder Dislocation in The Older Patient: Review ArticleDocumento8 páginasShoulder Dislocation in The Older Patient: Review ArticleFadhli Aufar KasyfiAinda não há avaliações
- Shoulder Dislocation Background: Shoulder Dislocations Traumatic InjuryDocumento7 páginasShoulder Dislocation Background: Shoulder Dislocations Traumatic Injuryanastasiaanggita_265Ainda não há avaliações
- Acute and Chronic Instability of The Elbow: Bernard F. Morrey, MDDocumento12 páginasAcute and Chronic Instability of The Elbow: Bernard F. Morrey, MDFadhli Aufar KasyfiAinda não há avaliações
- Aaos 2002Documento120 páginasAaos 2002Yusufa ArdyAinda não há avaliações
- D.M. Rouleau - Incidence of Associated Injury in Posterior Shoulder Dislocation (2012)Documento6 páginasD.M. Rouleau - Incidence of Associated Injury in Posterior Shoulder Dislocation (2012)João Pedro ZenattoAinda não há avaliações
- Clinical Tests of The Shoulder: Accuracy and Extension Using Dynamic UltrasoundDocumento9 páginasClinical Tests of The Shoulder: Accuracy and Extension Using Dynamic UltrasoundMohammad Al AbdullaAinda não há avaliações
- Shoulder Injures and Management 2Documento94 páginasShoulder Injures and Management 2Khushboo IkramAinda não há avaliações
- The Terrible Triad of The ElbowDocumento5 páginasThe Terrible Triad of The Elbowapi-250084607Ainda não há avaliações
- Complete - Medullacervical - Spinal - Cord - Transection - A Case ReportDocumento8 páginasComplete - Medullacervical - Spinal - Cord - Transection - A Case Reportkarisman kadirAinda não há avaliações
- Whiplash Associated DisordersDocumento12 páginasWhiplash Associated DisorderspuchioAinda não há avaliações
- IOM in Scoliosis TMHDocumento75 páginasIOM in Scoliosis TMHtuanemgAinda não há avaliações
- Manejo Via Aérea Trauma CervicalDocumento26 páginasManejo Via Aérea Trauma CervicalOdlanier Erwin Castro OlivaresAinda não há avaliações
- Posterior Shoulder Fracture-Dislocation A SystematDocumento7 páginasPosterior Shoulder Fracture-Dislocation A SystematMarcos Burón100% (1)
- William C. Cottrell, MD AbstractDocumento4 páginasWilliam C. Cottrell, MD AbstractmalaAinda não há avaliações
- Principles of Spine Trauma and Spinal Deformities PDFDocumento34 páginasPrinciples of Spine Trauma and Spinal Deformities PDFVirlan Vasile CatalinAinda não há avaliações
- Pelvic Injury (Autosaved)Documento44 páginasPelvic Injury (Autosaved)abhishek chaudharyAinda não há avaliações
- Scapular Fracture in A Professional Boxer: Nashville, TennDocumento4 páginasScapular Fracture in A Professional Boxer: Nashville, TennLuis Guillermo Buitrago BuitragoAinda não há avaliações
- Reversetotalshoulder Arthroplasty: Early Results of Forty-One Cases and A Review of The LiteratureDocumento11 páginasReversetotalshoulder Arthroplasty: Early Results of Forty-One Cases and A Review of The LiteratureBruno FellipeAinda não há avaliações
- Return To Play Following Anterior Shoulder Dislocation and Stabilization SurgeryDocumento17 páginasReturn To Play Following Anterior Shoulder Dislocation and Stabilization SurgerydrjorgewtorresAinda não há avaliações
- Rotator CuffDocumento46 páginasRotator CuffLiza Perez- Pagatpatan100% (2)
- Dislocation Shoulder GoodDocumento7 páginasDislocation Shoulder GoodZahiera NajibAinda não há avaliações
- Anterior Shoulder Instability A Review of PathoanatomyDocumento8 páginasAnterior Shoulder Instability A Review of PathoanatomyNikita TripthiAinda não há avaliações
- Các Trường Hợp Lóc Da CLB Y KHOA TRẺ Y KHOA VINHDocumento84 páginasCác Trường Hợp Lóc Da CLB Y KHOA TRẺ Y KHOA VINHVmu ShareAinda não há avaliações
- Background: FrequencyDocumento15 páginasBackground: FrequencyRandi SukmanaAinda não há avaliações
- Manejo Inicial Trauma EspinalDocumento7 páginasManejo Inicial Trauma EspinalJuan MVAinda não há avaliações
- Brachial Plexus NeuropathyDocumento4 páginasBrachial Plexus NeuropathyKim Torreliza EjeAinda não há avaliações
- The Painful Shoulder: Part I. Clinical Evaluation - AAFPDocumento18 páginasThe Painful Shoulder: Part I. Clinical Evaluation - AAFPMelvin Florens Tania GongaAinda não há avaliações
- Oite 2006Documento823 páginasOite 2006dastroh100% (1)
- Intrathoracic Fracture-Dislocation of The Humeral Head: A Case ReportDocumento4 páginasIntrathoracic Fracture-Dislocation of The Humeral Head: A Case ReportRachmawan WijayaAinda não há avaliações
- Shoulder Bankart Lesion With Posterior Instability A Case Report of Ultrasound DetectionDocumento5 páginasShoulder Bankart Lesion With Posterior Instability A Case Report of Ultrasound DetectionSheila Setiawati TanzilAinda não há avaliações
- Upper Extremity Weightlifting Injuries: Diagnosis and ManagementDocumento6 páginasUpper Extremity Weightlifting Injuries: Diagnosis and ManagementsinduAinda não há avaliações
- The Classification of Shoulder Instability. New Light Through Old Windows!Documento12 páginasThe Classification of Shoulder Instability. New Light Through Old Windows!Christian Tobar FredesAinda não há avaliações
- Posterior Dislocation of The Hip JointDocumento25 páginasPosterior Dislocation of The Hip JointadibahAinda não há avaliações
- Bilateral Inter-Faceted Dislocation of Cervical Spine: Closed Reduction With Traction Weights - Small and Slow or Lose It All (Neurology)Documento10 páginasBilateral Inter-Faceted Dislocation of Cervical Spine: Closed Reduction With Traction Weights - Small and Slow or Lose It All (Neurology)ICAinda não há avaliações
- Broken Neck (Hangman's Fracture) : DescriptionDocumento5 páginasBroken Neck (Hangman's Fracture) : DescriptionFatima RizwanAinda não há avaliações
- SLAP Lesions of The ShoulderDocumento6 páginasSLAP Lesions of The ShoulderPaula Valeria González MarchantAinda não há avaliações
- Sever Inferior Humeral Head Subluxation For 3 Months in Proximal Humerus Fracture DislocationDocumento4 páginasSever Inferior Humeral Head Subluxation For 3 Months in Proximal Humerus Fracture DislocationIJAR JOURNALAinda não há avaliações
- Dislocations: Diagnosis, Management, and Complications: Marvin H. Meyers, M.D.Documento12 páginasDislocations: Diagnosis, Management, and Complications: Marvin H. Meyers, M.D.Unoscientris StupaAinda não há avaliações
- June1997 CC WilkDocumento10 páginasJune1997 CC WilkwesleythompsonAinda não há avaliações
- The Painful Shoulder - Part I. Clinical Evaluation PDFDocumento17 páginasThe Painful Shoulder - Part I. Clinical Evaluation PDFOscar FrizziAinda não há avaliações
- JAAOS-Management of Hemorrhage in Life-Threatening Pelvic Fracture 162Documento11 páginasJAAOS-Management of Hemorrhage in Life-Threatening Pelvic Fracture 162Enny Yunita HariantiAinda não há avaliações
- CR - RamirezDocumento4 páginasCR - RamirezTommysAinda não há avaliações
- Spinal Cord InjuryDocumento9 páginasSpinal Cord Injuryta CAinda não há avaliações
- Adhesive CapsulitisDocumento20 páginasAdhesive Capsulitisvenkata ramakrishnaiahAinda não há avaliações
- SHOULDER INSTABILITY ManagDocumento18 páginasSHOULDER INSTABILITY ManagFarhan JustisiaAinda não há avaliações
- Rehabilitation of Shoulder Impingement Syndrome and Rotator Cuff Injuries: An Evidence-Based ReviewDocumento10 páginasRehabilitation of Shoulder Impingement Syndrome and Rotator Cuff Injuries: An Evidence-Based ReviewEduardo Santana SuárezAinda não há avaliações
- Aaos 2019Documento283 páginasAaos 2019alealer2708Ainda não há avaliações
- Shoulder Pain EvaluationDocumento8 páginasShoulder Pain EvaluationAnonymous 9lmlWQoDm8Ainda não há avaliações
- Lower Extremity TraumaDocumento72 páginasLower Extremity TraumaMariamAinda não há avaliações
- Scapulothoracic Dissociation 2165 7548.1000142Documento2 páginasScapulothoracic Dissociation 2165 7548.1000142Fadlu ManafAinda não há avaliações
- AAOS2014 Shoulder and ElbowDocumento83 páginasAAOS2014 Shoulder and ElbowAmmar HilliAinda não há avaliações
- Brachial Plexus InjuryDocumento20 páginasBrachial Plexus InjurySuci PramadianiAinda não há avaliações
- Clinical Manifestation of Acute Spinal Cord Injury, Chapter-4Documento6 páginasClinical Manifestation of Acute Spinal Cord Injury, Chapter-4cpradheepAinda não há avaliações
- Facet DislocationDocumento33 páginasFacet Dislocationgumi9Ainda não há avaliações
- Update On Traumatic Acute Spinal Cord Injury.: DOI: 10.1016/j.medine.2016.11.007Documento38 páginasUpdate On Traumatic Acute Spinal Cord Injury.: DOI: 10.1016/j.medine.2016.11.007witwiiwAinda não há avaliações
- Symptom Conductive Hearing Loss.3Documento3 páginasSymptom Conductive Hearing Loss.3Muhammad Pringgo ArifiantoAinda não há avaliações
- Algorithm Acute Otitis MediaDocumento1 páginaAlgorithm Acute Otitis MediaMuhammad Pringgo ArifiantoAinda não há avaliações
- Algorithm Acute Otitis MediaDocumento1 páginaAlgorithm Acute Otitis MediaMuhammad Pringgo ArifiantoAinda não há avaliações
- System Policy Manual: Facility NameDocumento14 páginasSystem Policy Manual: Facility NameMuhammad Pringgo ArifiantoAinda não há avaliações
- Problem Hypotesis Mechanism More Info Learning Issue Problem SolvingDocumento2 páginasProblem Hypotesis Mechanism More Info Learning Issue Problem SolvingMuhammad Pringgo ArifiantoAinda não há avaliações
- Ogexamination 110401040414 Phpapp02 PDFDocumento26 páginasOgexamination 110401040414 Phpapp02 PDFDika RizkiardiAinda não há avaliações
- JURNALDocumento12 páginasJURNALAsMiraaaaAinda não há avaliações
- Vertical Humeral Osteotomy For Stem Revision in Total Shoulder ArthroplastyDocumento5 páginasVertical Humeral Osteotomy For Stem Revision in Total Shoulder ArthroplastyngoyalnAinda não há avaliações
- Shoulder Function, Exercise Modifications, Strategies For Trainers (NSCA 2005)Documento10 páginasShoulder Function, Exercise Modifications, Strategies For Trainers (NSCA 2005)Fitness Tutor for the ACE & NSCA Exams100% (1)
- Surgical Approaches To JointsDocumento39 páginasSurgical Approaches To JointsJD46Ainda não há avaliações
- UntitledDocumento8 páginasUntitledTulkas el fuerteAinda não há avaliações
- Rehab Guidelines For Reverse Shoulder ArthroplastyDocumento7 páginasRehab Guidelines For Reverse Shoulder Arthroplastydeepak100% (1)
- Management of Rotator Cufftears in The Elderly PopulationDocumento6 páginasManagement of Rotator Cufftears in The Elderly PopulationdrjorgewtorresAinda não há avaliações
- BCS 1 Dan BCS 2Documento5 páginasBCS 1 Dan BCS 2Aisyah SyahidahAinda não há avaliações
- Upper Limb 0809 PDFDocumento59 páginasUpper Limb 0809 PDFasdaAinda não há avaliações
- MRCS Upper Limb Till Forearm - IoDocumento3 páginasMRCS Upper Limb Till Forearm - IoZaeem KhalidAinda não há avaliações
- The Disabled Throwing Shoulder: Spectrum of Pathologyd10-Year UpdateDocumento47 páginasThe Disabled Throwing Shoulder: Spectrum of Pathologyd10-Year UpdateSandro RolimAinda não há avaliações
- Ortho Notes by Joachim & Liyana - Edited by Waiwai (FINAL) - Pdf-Notes - 201409021158Documento142 páginasOrtho Notes by Joachim & Liyana - Edited by Waiwai (FINAL) - Pdf-Notes - 201409021158Yiu Jean LAinda não há avaliações
- Rehabilitation Exercises To Induce Balanced Scapular Muscle Activity in An Anti-Gravity PostureDocumento4 páginasRehabilitation Exercises To Induce Balanced Scapular Muscle Activity in An Anti-Gravity PostureSAMAinda não há avaliações
- Treatment Strategyfor Irreparable Rotator Cuff TearsDocumento16 páginasTreatment Strategyfor Irreparable Rotator Cuff TearshawkjohnAinda não há avaliações
- Orthopedics Toronto NotesDocumento47 páginasOrthopedics Toronto Noteskyliever78% (9)
- HANDBALL: Conditioning For PlayersDocumento120 páginasHANDBALL: Conditioning For PlayersAdriano VretarosAinda não há avaliações
- Intro To Biomech Mid-1Documento122 páginasIntro To Biomech Mid-1reyanahmed7290Ainda não há avaliações
- Applied Anatomy of The ShoulderDocumento11 páginasApplied Anatomy of The ShoulderSamantha HohAinda não há avaliações
- Physical Therapy Management in Shoulder InstabilitiesDocumento7 páginasPhysical Therapy Management in Shoulder InstabilitiesYeshvi sAinda não há avaliações
- Toronto+Notes+2011+ +21.+orthopaedicsDocumento46 páginasToronto+Notes+2011+ +21.+orthopaedicsChanique Cousins100% (1)
- Anatomy Imporatant Points by Dr. Asif AliDocumento31 páginasAnatomy Imporatant Points by Dr. Asif AliSyed imran AbbasAinda não há avaliações
- DislocationDocumento46 páginasDislocationShaa ShawalishaAinda não há avaliações
- Stem Cell Therapy For Rotator Cuff InjuriesDocumento12 páginasStem Cell Therapy For Rotator Cuff InjuriesAthenaeum Scientific PublishersAinda não há avaliações
- Ana BibleDocumento19 páginasAna BibleRamses DagoyAinda não há avaliações
- Scapular Syndromes HODocumento25 páginasScapular Syndromes HOsnbtx7y79sAinda não há avaliações
- Get Fit For TennisDocumento4 páginasGet Fit For TennisCaroline Sandry100% (38)
- HandsOn Muscle TherapyDocumento38 páginasHandsOn Muscle TherapyPhoenixRising61100% (2)
- Current Diagnosis Treatment in Rheumatology 4Th Edition John A Stone Full ChapterDocumento51 páginasCurrent Diagnosis Treatment in Rheumatology 4Th Edition John A Stone Full Chaptercindy.turner467100% (2)
- Manual Therapy Techniques For The ShoulderDocumento12 páginasManual Therapy Techniques For The Shoulderubiktrash1492100% (1)
- Subacromial Impingement SyndromeDocumento14 páginasSubacromial Impingement SyndromeJbarrianAinda não há avaliações
- The Painful Shoulder: Part I. Clinical Evaluation - AAFPDocumento18 páginasThe Painful Shoulder: Part I. Clinical Evaluation - AAFPMelvin Florens Tania GongaAinda não há avaliações