Escolar Documentos
Profissional Documentos
Cultura Documentos
Rapidly Blinding Posterior Tubercular Uveitis: Briefreport Open Access
Enviado por
SusPa NarahaTítulo original
Direitos autorais
Formatos disponíveis
Compartilhar este documento
Compartilhar ou incorporar documento
Você considera este documento útil?
Este conteúdo é inapropriado?
Denunciar este documentoDireitos autorais:
Formatos disponíveis
Rapidly Blinding Posterior Tubercular Uveitis: Briefreport Open Access
Enviado por
SusPa NarahaDireitos autorais:
Formatos disponíveis
Agarwal et al.
Journal of Ophthalmic Inflammation and Infection 2014, 4:13
http://www.joii-journal.com/content/4/1/13
BRIEF REPORT
Open Access
Rapidly blinding posterior tubercular uveitis
Manisha Agarwal1*, Vivek Jha2 and Jyotirmay Biswas3
Abstract
Background: A 21-year-old female patient had chorioretinitis in the left eye which relapsed while being on
anti-tubercular treatment and oral corticosteroids leading to blindness and the loss of the left eye.
Findings: Mycobacterium tuberculosis causing chorioretinitis showed a poor response, and the lung lesions
showed a good response to the same anti-tubercular treatment.
Conclusions: Mycobacterium tubercle bacilli in the eye may show a poor response to the anti-tubercular drugs
due to poor ocular penetration of the drugs secondary to early ocular hypoxia.
Keywords: Ocular tuberculosis; Blinding; Posterior
Findings
Introduction
Intraocular tuberculosis represents an extrapulmonary
form of tuberculosis. Posterior uveitis is the most common manifestation of intraocular tuberculosis [1]. The
inflammation predominantly involves the choroid in the
form of choroidal tubercles, tuberculoma, sub-retinal
abscess, chorioretinitis, and serpiginous-like choroiditis.
We report a case of pulmonary and intraocular tuberculosis which showed a good response to the anti-tubercular
drugs in the lungs but not in the eye leading to a blinding
posterior tubercular uveitis.
Case report
A 21-year-old female presented with sudden painless
diminution of vision in the left eye for 10 days. There
was an associated history of low grade fever with evening rise and nonpurulent cough. There was a history of
pulmonary tuberculosis in her brother. On examination,
the best corrected visual acuity (BCVA) was 20/20, N6
in the right eye and counting finger close to face in the
left eye. Slit lamp examination was unremarkable in both
eyes. Fundus examination of the right eye was normal,
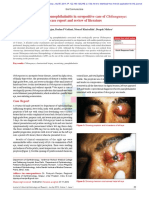
and the left eye showed a granuloma on the optic nerve
head (ONH) with perivascular sheathing and chorioretinitis patch with overlying retinal hemorrhages in the
macula (Figure 1).
* Correspondence: agarwalmannii@yahoo.co.in
1
Vitreoretina Services, Dr. Shroffs Charity Eye Hospital, 5027-Kedar Nath Road,
Daryaganj, New Delhi 110002, India
Full list of author information is available at the end of the article
Blood investigation showed hemoglobin 7.6 gm%, raised
erythrocyte sedimentation rate (ESR) 65 mm in the first
hour, and Mantoux test 26 26 mm. Sputum test was
negative for acid fast bacilli. Chest X-ray was normal and
a high-resolution computed tomography (HRCT)-thorax
scan showed enlarged mediastinal lymph nodes with
necrosis in the center and patches of infiltration in the left
apical region and right lower lobe. She was evaluated by
the pulmonologist and started on four-drug regimen of
anti-tubercular therapy (ATT) comprising of rifampicin
600 mg/day, ethambutol, pyrazinamide and isoniazid,
and systemic corticosteroids 1 mg/kg body weight.
Topical prednisolone 1% eye drops and atropine 1%
were also started. There was evidence of mild vitritis
after 1 week on treatment.
After 1 month follow-up, the BCVA of the left eye was
counting fingers at 2 meters and fundus examination
showed a decrease in the size of the chorioretinitis
patch in the macula with a decrease in the paerivasculitis and the granuloma on the ONH (Figure 2).
Two weeks later, she presented with severe pain in the
left eye. BCVA in the left eye was counting fingers at 2
meters and fundus examination of the left eye showed
appearance of new patches of chorioretinitis in the macula
between the ONH and previous patch of chorioretinitis
(Figure 3). Systemic evaluation and repeat HRCT-thorax
showed resolution of the chest infiltrates. The systemic
corticosteroids were increased to 1.5 mg/kg/body weight
and oral ofloxacin 400 mg twice daily was added to the
ongoing four-drug ATT.
2014 Agarwal et al.; licensee Springer. This is an Open Access article distributed under the terms of the Creative Commons
Attribution License (http://creativecommons.org/licenses/by/2.0), which permits unrestricted use, distribution, and reproduction
in any medium, provided the original work is properly credited.
Agarwal et al. Journal of Ophthalmic Inflammation and Infection 2014, 4:13
http://www.joii-journal.com/content/4/1/13
Page 2 of 4
Figure 3 Appearance of new patches of chorioretinitis in
the macula.
Figure 1 Granuloma on the ONH with perivascular sheathing and
chorioretnitis patch with retinal hemorrhages in the macula.
Follow-up after 2 weeks showed a decrease of vision
in the left eye to perception of light with extensive neovascularization of the iris (NVI), posterior synechiae formation, and early lenticular changes. The intraocular
pressure (IOP) by Goldmann applanation tonometer was
28 mm of Hg. Ultrasound B-scan showed exudative retinal
detachment with evidence of choroidal thickening. She
was treated with off-label use of intravitreal injections of
bevacizumab (Avastin, Genentech, South San Francisco,
CA, USA). The left eye subsequently became a painful
blind eye which was digitally soft with a decreased axial
length on ultrasound B-scan.
Figure 2 The chorioretinitis patch in the macula decreased with
a decrease in the granuloma on the disc and perivasculitis.
Enucleation with ball implant was done for the left eye
after an informed consent. Gross histopathology of the
left eyeball showed total retinal detachment with choroidal
thickening. Microscopic examination of the sub-retinal
areas showed extensive caseation necrosis with intraretinal
inflammation and dense collections of lymphocytes and
plasma cells, choroidal inflammation with lymphocytic
cells, chronic inflammation of the ciliary body, and
inflammation of the scleral fibers (Figure 4a,b,c).
On microbiological examination, acid fast bacilli (AFB)
stain was negative for mycobacterium tubercle bacilli.
Grams stain was negative for fungal filaments. Polymerase chain reaction (PCR) for mycobacterium tuberculosis was positive with both the primers IS6110 and
MPb 64 (Figure 5).
She was subsequently dispensed with a prosthetic shell
for the left socket.
Discussion
Tuberculosis is a clinical disease caused by infection
with Mycobacterium tuberculosis and is characterized
pathologically by the formation of granulomas [2]. It is
commonly described as a systemic disease of protean
manifestations that mainly involves the lungs. Extrapulmonary involvement, including lesions of the gastrointestinal tract, genito-urinary tract, cardiovascular
system, skin, central nervous system, and eyes, may occur
either in association with clinically apparent pulmonary
tuberculosis or in isolation, with no clinical or laboratory
evidence of pulmonary infection. In India, where pulmonary tuberculosis is endemic, the incidence of ocular
involvement is variable [3].
In our patient, there was initially a response to the oral
corticosteroids and four-drug ATT; however, this was
2 weeks later followed by a deterioration in the left eye
and improvement in the lung lesions while being on
treatment. We got different response in the lungs and in
the eye even though it is presumed that the strain of
Agarwal et al. Journal of Ophthalmic Inflammation and Infection 2014, 4:13
http://www.joii-journal.com/content/4/1/13
Page 3 of 4
Figure 4 Microscopic examination of the sub-retinal areas (a,b,c).
mycobacterium tubercle bacilli causing infection in the
lungs would also be the causative bacilli in the left eye.
This excludes the fact that our case was of a multidrugresistant tuberculosis as then neither lungs or the eye
would have responded to the treatment. There was a resistance to start second line anti-tubercular drugs seeing to
the resolution of the chest lesions; however, oral ofloxacin
was added which failed to provide any additional benefit.
We were unable to see the antibiotic sensitivity of the
mycobacterium tubercle bacilli as the microbiology testing
showed no growth though the polymerase chain reaction
confirmed the same.
Figure 5 Positive polymerase chain reaction for mycobacterium tuberculosis.
Agarwal et al. Journal of Ophthalmic Inflammation and Infection 2014, 4:13
http://www.joii-journal.com/content/4/1/13
This case is reported to highlight the fact that it is not
essential that pulmonary and extrapulmonary manifestation
especially ocular involvement of tuberculosis may show the
same response to the ATT. This maybe secondary to the
fact that ocular hypoxia sets in very fast in eyes with inflammation of the choroid secondary to mycobacterium tuberculosis [4-6]. This causes decreased choroidal circulation,
and this may reduce the penetration of the drugs of ATT
into the eye. Early neovascular complications are seen in
these eyes secondary to ocular hypoxia as in our case where
we treated our patient with multiple intravitreal injections
of bevacizumab (Avastin,Genentech) which is a nonselective vascular endothelial growth factor inhibitor providing relief from pain till the eye was enucleated. We need to
be very careful and follow a case of intraocular tuberculosis
at frequent intervals as there maybe a very fast progression
of ocular tuberculosis leading to a complete loss of the eye.
5.
6.
Page 4 of 4
Bansal R, Sharma A, Gupta A (2012) Intraocular tuberculosis. Expert Rev
Ophthalmol 7(4):341349
Thayil SM, Albini TA, Nazari H, Moshfeghi AA, Parel JMA, Rao NA, Karakousis
PC (2011) Local ischemia and increased expression of vascular endothelial
growth factor following ocular dissemination of mycobacterium
tuberculosis. PLoS One 2011:2011
doi:10.1186/1869-5760-4-13
Cite this article as: Agarwal et al.: Rapidly blinding posterior tubercular
uveitis. Journal of Ophthalmic Inflammation and Infection 2014 4:13.
Abbreviations
AFB: acid fast bacilli; ATT: anti-tubercular treatment; BCVA: best corrected
visual acuity; ESR: erythrocyte sedimentation rate; HRCT: high-resolution
computed tomography; IOP: intraocular pressure; NVI: neovascularization of
iris; ONH: optic nerve head; PCR: polymerase chain reaction.
Competing interests
The authors declare that they have no competing interests.
Authors contributions
MA provided ophthalmic care to the patient and drafted the manuscript.
VJ managed the patient systemically and monitored the anti-tubercular
treatment. JB did the histopathological examinations. All the authors read
and approved the final manuscript.
Authors information
Dr. Manisha Agarwal, M.S. (Ophthalmology), is the head of Vitreoretina
Services, Dr.Shroffs Charity Eye Hospital, New Delhi, India. Dr. Vivek Jha, M.D.
(Medicine), is a physician and pulmonologist at Dr. Shroffs Charity Eye
Hospital, New Delhi, India. Dr. Jyotirmay Biswas, M.S. (Ophthalmology) is the
head of Uvea and Ocular Pathology, Sankara Nethralaya, Chennai, India.
Acknowledgements
The authors would like to acknowledge Ms. Renu Verma and
Mr. Brajesh Kumar.
Author details
1
Vitreoretina Services, Dr. Shroffs Charity Eye Hospital, 5027-Kedar Nath Road,
Daryaganj, New Delhi 110002, India. 2Internal Medicine Services, Dr. Shroffs
Charity Eye Hospital, 5027-Kedar Nath Road, Daryaganj, New Delhi 110002,
India. 3Sankara Nethralaya, 18, College Road, Chennai, Tamil Nadu 600006,
India.
Received: 15 January 2014 Accepted: 25 April 2014
Published: 9 June 2014
References
1. Gupta V, Gupta A, Rao NA (2007) Intraocular tuberculosis-an update.
Surv Ophthalmol 52(6):561586
2. Centers for Disease Control and Prevention (1997) Case definitions for
infectious conditions under public health surveillance. MMWR Morb Mortal
Wkly Rep 46:155
3. Glassroth J, Robins AG, Snider DE (1980) Tuberculosis in the 1980s. N Engl J
Med 302:14411450
4. Steven Y, Sen HN, Colyer M, Zapor M, Wroblewski K (2012) Curr Opin
Ophthalmol 23(6):551556
Submit your manuscript to a
journal and benet from:
7 Convenient online submission
7 Rigorous peer review
7 Immediate publication on acceptance
7 Open access: articles freely available online
7 High visibility within the eld
7 Retaining the copyright to your article
Submit your next manuscript at 7 springeropen.com
Você também pode gostar
- Culturing of Microbiology Specimens in LaboratoriesDocumento100 páginasCulturing of Microbiology Specimens in Laboratoriestummalapalli venkateswara raoAinda não há avaliações
- Nip Mop Booklet 2Documento42 páginasNip Mop Booklet 2Arlo Winston De GuzmanAinda não há avaliações
- Laws Affecting Community Health Nursing PracticeDocumento3 páginasLaws Affecting Community Health Nursing PracticeRakesh Ladjahasan75% (4)
- Labor Advisory No. 21-23 Supplemental Guidelines On The Implementation of Safety and Health Measures For The Prevention and Control of Tuberculosis in The WorkplaceDocumento2 páginasLabor Advisory No. 21-23 Supplemental Guidelines On The Implementation of Safety and Health Measures For The Prevention and Control of Tuberculosis in The WorkplaceRaymond Cruzin100% (1)
- Continue: Sharma Mohan Textbook of Tuberculosis PDFDocumento2 páginasContinue: Sharma Mohan Textbook of Tuberculosis PDFAbdul JalilAinda não há avaliações
- Tubercular Posterior SchleritisDocumento6 páginasTubercular Posterior SchleritisInayatul muthmainnahAinda não há avaliações
- Imprimir 2Documento3 páginasImprimir 2Gino VitteriAinda não há avaliações
- Presumed TB Choroiditis 2015Documento3 páginasPresumed TB Choroiditis 2015TrinitaAinda não há avaliações
- 2014 Article 33Documento5 páginas2014 Article 33SusPa NarahaAinda não há avaliações
- Orbital Apex Syndrome Secondary To Herpes Zoster OphthalmicusDocumento4 páginasOrbital Apex Syndrome Secondary To Herpes Zoster OphthalmicusYosiita KartinaaAinda não há avaliações
- Leg Tuberculosis Presenting As Hypopion UveitisDocumento3 páginasLeg Tuberculosis Presenting As Hypopion UveitisIJAR JOURNALAinda não há avaliações
- Case Report: Tuberculous Scleritis A Challenging DiagnosticDocumento10 páginasCase Report: Tuberculous Scleritis A Challenging DiagnosticIJAR JOURNALAinda não há avaliações
- Iaet 12 I 2 P 135Documento2 páginasIaet 12 I 2 P 135leonjunchan_66965707Ainda não há avaliações
- Jurding Mata EndophthalamitisDocumento24 páginasJurding Mata EndophthalamitisBenk Setsuna F. SeieiAinda não há avaliações
- Challenging Treatment of Bilateral Multiple Infection Panuveitis in HIV/AIDS PatientsDocumento5 páginasChallenging Treatment of Bilateral Multiple Infection Panuveitis in HIV/AIDS PatientsRosyid PrasetyoAinda não há avaliações
- Acute Necrotizing Panophthalmitis in Seropositive Case of ChikungunyaDocumento3 páginasAcute Necrotizing Panophthalmitis in Seropositive Case of ChikungunyaPratyushAinda não há avaliações
- Case Report Bacterial Conjunctivitis WengDocumento9 páginasCase Report Bacterial Conjunctivitis WengIka NovitaAinda não há avaliações
- A Case Series of Ocular Manifestations in TuberculosisDocumento4 páginasA Case Series of Ocular Manifestations in TuberculosisInternational Journal of Innovative Science and Research TechnologyAinda não há avaliações
- Clinical Profile of Tubercular Uveitis in A Tertiary Care Ophthalmic CentreDocumento3 páginasClinical Profile of Tubercular Uveitis in A Tertiary Care Ophthalmic CentreArif BudimanAinda não há avaliações
- Bilateral Radiation Retinopathy 17 Years Following.62Documento3 páginasBilateral Radiation Retinopathy 17 Years Following.62ShivcharanLalChandravanshiAinda não há avaliações
- Spontaneous Closure of Macular Holes Secondary To Posterior Uveitis: Case Series and A Literature ReviewDocumento7 páginasSpontaneous Closure of Macular Holes Secondary To Posterior Uveitis: Case Series and A Literature ReviewJusty GuavaAinda não há avaliações
- Case Study CAPS PDFDocumento5 páginasCase Study CAPS PDFCitra KristiAinda não há avaliações
- A Case of Bilateral Presumed Chikungunya Neuroretinitis: Other Sections Abstractcase ReportdiscussionreferencesabstractDocumento5 páginasA Case of Bilateral Presumed Chikungunya Neuroretinitis: Other Sections Abstractcase Reportdiscussionreferencesabstractsuci nourmalizaAinda não há avaliações
- Granuloma Epididimitisarticle-2Documento4 páginasGranuloma Epididimitisarticle-2Feby Kurnia PutriAinda não há avaliações
- Primary Conjunctival Tuberculosis-2Documento3 páginasPrimary Conjunctival Tuberculosis-2puutieAinda não há avaliações
- Tubercular ScleritisDocumento5 páginasTubercular Scleritismutya yulindaAinda não há avaliações
- Conjunctivitis As A Manifestation of Wegener 'S GranulomatosisDocumento5 páginasConjunctivitis As A Manifestation of Wegener 'S GranulomatosisAsd DsaAinda não há avaliações
- Jaad O: NlineDocumento2 páginasJaad O: NlinepunishAinda não há avaliações
- Jurnal Nirza MataDocumento15 páginasJurnal Nirza MataRozans IdharAinda não há avaliações
- Inflammatory Choroidal NeovascularizationDocumento7 páginasInflammatory Choroidal NeovascularizationMarj MendezAinda não há avaliações
- Orbital Cellulitis As A Complication of Odontogenic InfectionDocumento5 páginasOrbital Cellulitis As A Complication of Odontogenic InfectionCikal Abyan Nur 1417Ainda não há avaliações
- A Painful Red EyeDocumento2 páginasA Painful Red EyeCristhian Agustin ParedesAinda não há avaliações
- Crs LinDocumento4 páginasCrs LinPoolerErAinda não há avaliações
- Sal Agar 2015Documento2 páginasSal Agar 2015occcAinda não há avaliações
- Schechter 2015Documento8 páginasSchechter 2015joseph rivaldoAinda não há avaliações
- The Pathogenesis of Optic Neuritis Caused by Angiostrongylus Cantonensis in BALB/c MiceDocumento12 páginasThe Pathogenesis of Optic Neuritis Caused by Angiostrongylus Cantonensis in BALB/c Miceracut_khansatraAinda não há avaliações
- American Journal of Ophthalmology Case ReportsDocumento3 páginasAmerican Journal of Ophthalmology Case ReportsElison Jaya PanggaloAinda não há avaliações
- Ocular Basidiobolomycosis A Case ReportDocumento7 páginasOcular Basidiobolomycosis A Case ReportYUNA RATNA WULANSARIAinda não há avaliações
- 2016 Article 294 PDFDocumento7 páginas2016 Article 294 PDFChato Haviz DanayomiAinda não há avaliações
- Pink Hypopyon in A Patient With Serratia Marcescens Corneal UlcerationDocumento2 páginasPink Hypopyon in A Patient With Serratia Marcescens Corneal UlcerationRusman Hadi RachmanAinda não há avaliações
- Articulo 2 OftalmoDocumento6 páginasArticulo 2 OftalmoJhonathan Andres Garcia FiallosAinda não há avaliações
- Staphylococcus Epidermidis End PDFDocumento4 páginasStaphylococcus Epidermidis End PDFNisaAinda não há avaliações
- MainDocumento3 páginasMainomidazadmehr1375Ainda não há avaliações
- Ophthal Notes PGDocumento6 páginasOphthal Notes PGSwati TyagiAinda não há avaliações
- OTDCP: Herpes Simplex: Case History and FindingsDocumento4 páginasOTDCP: Herpes Simplex: Case History and FindingsMaggie DuttaAinda não há avaliações
- Seasonal Monthly Variation Amongst Reported Cataract Surgeries in IndiaDocumento92 páginasSeasonal Monthly Variation Amongst Reported Cataract Surgeries in IndiafriendsofindiaAinda não há avaliações
- Atypical Case of Presumed Ocular Tuberculosis Presenting As Unilateral Occlusive VasculitisDocumento4 páginasAtypical Case of Presumed Ocular Tuberculosis Presenting As Unilateral Occlusive VasculitisInternational Journal of Innovative Science and Research TechnologyAinda não há avaliações
- Jceh 12 30 021Documento3 páginasJceh 12 30 021Tatik HandayaniAinda não há avaliações
- Bilateral Endogenous Endophthalmitis Secondary To Group B Streptococcal SepsisDocumento1 páginaBilateral Endogenous Endophthalmitis Secondary To Group B Streptococcal SepsisRatih Kusuma DewiAinda não há avaliações
- A Case of Choroidal Neovascularization Secondary To Unilateral Retinal Pigment Epithelium DysgenesisDocumento4 páginasA Case of Choroidal Neovascularization Secondary To Unilateral Retinal Pigment Epithelium DysgenesisdedypurnamaAinda não há avaliações
- BR J Ophthalmol 1999 Das 1050 5Documento7 páginasBR J Ophthalmol 1999 Das 1050 5xoxotheAinda não há avaliações
- Journal OphtalmologyDocumento3 páginasJournal OphtalmologyFaza KeumalasariAinda não há avaliações
- Acknowledgement: Aniridia Associated With Congenital Aphakia and Secondary GlaucomaDocumento3 páginasAcknowledgement: Aniridia Associated With Congenital Aphakia and Secondary GlaucomaNisrina FarihaAinda não há avaliações
- Annals of Medicine and SurgeryDocumento3 páginasAnnals of Medicine and SurgeryAfifah Siti NurAinda não há avaliações
- MUCORMYCOSISDocumento4 páginasMUCORMYCOSISipe.jacobAinda não há avaliações
- JurnalDocumento5 páginasJurnalYazid Eriansyah PradantaAinda não há avaliações
- Parapharingeal AbsesDocumento5 páginasParapharingeal AbsesEping St WindahAinda não há avaliações
- DOI: 10.5281/zenodo.4382252: Annals of Mechnikov Institute, N 4, 2020Documento5 páginasDOI: 10.5281/zenodo.4382252: Annals of Mechnikov Institute, N 4, 2020nitaAinda não há avaliações
- Retinal Tear: An Unusual Complication of Ocular ToxoplasmosisDocumento5 páginasRetinal Tear: An Unusual Complication of Ocular ToxoplasmosisMuhammad Irfan FaizAinda não há avaliações
- The Association of Carotid Cavernous Fistula With Graves' Ophthalmopathy Brief CommunicationsDocumento3 páginasThe Association of Carotid Cavernous Fistula With Graves' Ophthalmopathy Brief CommunicationsRiris SihotangAinda não há avaliações
- Conjunctival Folliculosis Presenting As HemolacriaDocumento5 páginasConjunctival Folliculosis Presenting As HemolacriaAthenaeum Scientific PublishersAinda não há avaliações
- Fungal Keratitis and Ocular Surface Squamous Neoplasia in A HIV Positive PatientDocumento4 páginasFungal Keratitis and Ocular Surface Squamous Neoplasia in A HIV Positive PatientSherly AsrianiAinda não há avaliações
- EED Uveitis 4 Get - FileDocumento3 páginasEED Uveitis 4 Get - FileAmirahShalehaAinda não há avaliações
- Ocular Lesions in 1,000 Consecutive HIV-positive Patients in India: A Long-Term StudyDocumento7 páginasOcular Lesions in 1,000 Consecutive HIV-positive Patients in India: A Long-Term StudyresearchashrafAinda não há avaliações
- Complications in UveitisNo EverandComplications in UveitisFrancesco PichiAinda não há avaliações
- Endophthalmitis After Open Globe Injuries: Changes in Microbiological Spectrum and Isolate Susceptibility Patterns Over 14 YearsDocumento4 páginasEndophthalmitis After Open Globe Injuries: Changes in Microbiological Spectrum and Isolate Susceptibility Patterns Over 14 YearsSusPa NarahaAinda não há avaliações
- 2014 Article 21Documento10 páginas2014 Article 21SusPa NarahaAinda não há avaliações
- Intraocular Lens Subluxation in Marfan SyndromeDocumento3 páginasIntraocular Lens Subluxation in Marfan SyndromeSusPa NarahaAinda não há avaliações
- Toophtj 8 1Documento2 páginasToophtj 8 1SusPa NarahaAinda não há avaliações
- Case Report: Periorbital Edema Secondary To Positive Airway Pressure TherapyDocumento3 páginasCase Report: Periorbital Edema Secondary To Positive Airway Pressure TherapySusPa NarahaAinda não há avaliações
- Glycolysis in Patients With Age-Related Macular DegenerationDocumento9 páginasGlycolysis in Patients With Age-Related Macular DegenerationSusPa NarahaAinda não há avaliações
- CapsDocumento1 páginaCapsSusPa NarahaAinda não há avaliações
- 2015 Article 36Documento8 páginas2015 Article 36SUSPAAinda não há avaliações
- Experimental Study On Cryotherapy For Fungal Corneal Ulcer: Researcharticle Open AccessDocumento9 páginasExperimental Study On Cryotherapy For Fungal Corneal Ulcer: Researcharticle Open AccessSusPa NarahaAinda não há avaliações
- Acute Management of Open Fractures An Evidence Based Review PDFDocumento9 páginasAcute Management of Open Fractures An Evidence Based Review PDFSusPa Naraha100% (1)
- Are BCG Vaccination, Population Density, Median Age and Poverty Important Determinants of COVID-19 Pandemic Spread, Morbidity and Mortality?Documento15 páginasAre BCG Vaccination, Population Density, Median Age and Poverty Important Determinants of COVID-19 Pandemic Spread, Morbidity and Mortality?laserdog97Ainda não há avaliações
- CausalityDocumento47 páginasCausalityyeabsraAinda não há avaliações
- TuberculosisDocumento9 páginasTuberculosisIdasari DewiAinda não há avaliações
- TuberculosisDocumento41 páginasTuberculosisMeena Devi100% (1)
- Cobb Research Lab News: A Quarterly Newsletter of The W. Montague Cobb Research Laboratory, Howard UniversityDocumento9 páginasCobb Research Lab News: A Quarterly Newsletter of The W. Montague Cobb Research Laboratory, Howard UniversityW Montague Cobb LabAinda não há avaliações
- Pathology TutorialDocumento12 páginasPathology TutorialjessbunkerAinda não há avaliações
- TB India 2012 - Annual ReportDocumento185 páginasTB India 2012 - Annual ReportdsoorajdAinda não há avaliações
- Kelebihan Kekurangan FixDocumento4 páginasKelebihan Kekurangan FixIffah AfallahAinda não há avaliações
- FC Paed (SA) Part II Past Papers - 2011 Sept 8-4-2014Documento5 páginasFC Paed (SA) Part II Past Papers - 2011 Sept 8-4-2014matentenAinda não há avaliações
- Mycobacterium Tuberculosis and Tuberculosis - TodarDocumento18 páginasMycobacterium Tuberculosis and Tuberculosis - TodarTanti Dewi WulantikaAinda não há avaliações
- Costing Ranap Jan-JunDocumento32 páginasCosting Ranap Jan-Jungalih wicaksonoAinda não há avaliações
- National Tuberculosis ProgramDocumento18 páginasNational Tuberculosis ProgramJhon LapuzAinda não há avaliações
- General Pathology of Infectious DiseasesDocumento47 páginasGeneral Pathology of Infectious DiseasesAbdullah EmadAinda não há avaliações
- English Assigmentt .Documento12 páginasEnglish Assigmentt .Fareza AkbarAinda não há avaliações
- Moxifloxacin: What Is Moxifloxacin? What Are Some Possible Side Effects?Documento1 páginaMoxifloxacin: What Is Moxifloxacin? What Are Some Possible Side Effects?kitsilcAinda não há avaliações
- Pediatric PneumoniaDocumento12 páginasPediatric PneumoniaKrystal Migo Denolo ContrerasAinda não há avaliações
- How To Take Sputum Suitable For TB - InspectionDocumento1 páginaHow To Take Sputum Suitable For TB - InspectionGeneXpert Lab LCPAinda não há avaliações
- Basics of TB, TBDocumento24 páginasBasics of TB, TBzinabu tesfayeAinda não há avaliações
- The Lancet Microbe.: Priya VenkatesanDocumento1 páginaThe Lancet Microbe.: Priya Venkatesankayegi8666Ainda não há avaliações
- 2022 ART Revised Kenyan GuidelinesDocumento39 páginas2022 ART Revised Kenyan GuidelinesJOHN KAMAUAinda não há avaliações
- Philhealth TB PDFDocumento35 páginasPhilhealth TB PDFO.r. CadzAinda não há avaliações
- Part III Internal Medicine Examination AnswersDocumento91 páginasPart III Internal Medicine Examination AnswersFırat GüllüAinda não há avaliações
- TB Lab Report - DR JainDocumento5 páginasTB Lab Report - DR JainDavinder SinghAinda não há avaliações
- Final Manuscript For RecDocumento53 páginasFinal Manuscript For RecAngelica Guinapon DaowagAinda não há avaliações
- Nursing Test IDocumento10 páginasNursing Test IClarenz CanlasAinda não há avaliações