Escolar Documentos
Profissional Documentos
Cultura Documentos
Postgrad Med J 1974 Krikler 447 53
Enviado por
Mochammad Dwiki Rahman SaniDireitos autorais
Formatos disponíveis
Compartilhar este documento
Compartilhar ou incorporar documento
Você considera este documento útil?
Este conteúdo é inapropriado?
Denunciar este documentoDireitos autorais:
Formatos disponíveis
Postgrad Med J 1974 Krikler 447 53
Enviado por
Mochammad Dwiki Rahman SaniDireitos autorais:
Formatos disponíveis
Downloaded from http://pmj.bmj.com/ on September 18, 2016 - Published by group.bmj.
com
Postgraduate Medical Journal (July 1974) 50, 447-453.
Verapamil in the treatment of paroxysmal supraventricular tachycardia
DENNIS M. KRIKLER
ROWORTH A. J. SPURRELL
M.D., F.R.C.P., F.A.C.C.
Cardiovascular Division, Royal Postgraduate
Medical School, London, W. 12
B.Sc., M.B., M.R.C.P.
Department of Cardiology,
Guy's Hospital, London, S.E.1
Summary
Verapamil is a novel antiarrhythmic agent which
appears to act as a calcium-ion antagonist, blocking
calcium transport across the myocardial cell membrane. It was given intravenously, in a dose of 10 mg,
to thirty-two patients suffering from paroxysmal
supraventricular tachycardia, and sinus rhythm was
achieved promptly in all. Identical results were obtained in a further ten patients with supraventricular
tachycardias associated with the Wolff-ParkinsonWhite or other pre-excitation syndromes. In a separate
group of eighteen patients in whom A-V junctional
tachycardias were induced during intracardiac electrography, conversion to sinus rhythm was achieved in
fifteen patients, with prolongation of the cycle length
in the others. Circus-movement tachycardias were induced in eight patients with the Wolff-ParkinsonWhite syndrome, and conversion to sinus rhythm was
achieved in seven. The results were less consistent in
patients with other supraventricular arrhythmias including ectopic atrial tachycardia and atrial flutter,
and, in the single patient with supraventricular and
ventricular tachycardia, only the former was controlled. In the single patient with atrial fibrillation
complicating the Wolff-Parkinson-White syndrome
who received verapamil, sinus rhythm was restored.
Side effects were few and mild, with rare exceptions of
profound hypotension, bradycardia and asystole; their
management is discussed, and reasons are advanced
why their occurrence is likely to be related either to the
concomitant administration of beta-adrenergic blockers
or to the presence of sinoatrial disease. It appears that
verapamil is particularly saitable for the treatment of
supraventricular tachycardias due to a circus movement as calcium antagonism is likely to be most effective in the N region of the atrioventricular node.
VERAPAMIL was originally considered to be a coronary vasodilator (Haas and Hairtfelder, 1962), and
on this basis was introduced for the treatment of
cardiac ischaemia (Tschirdewahn and Klepzig, 1963;
Hoffmann, 1964). Under experimental conditions,
potent antiarrhythmic activity was noted (Melville,
Shister and Huq, 1964; Schmid and Hanna, 1967;
Kaumann and Aramendia, 1968) and it is now recog-
nized that its antiarrhythmic activity and any action
improving cardiac ischaemia is determined by its
ability to prevent calcium inflow across the cell
membrane (Nayler et al., 1968; Fleckenstein, Doring
and Kammermeier, 1968; Nayler and Szeto, 1972;
Singh and Vaughan Williams, 1972). In clinical use
its antiarrhythmic properties have been demonstrated by Bender et al. (1966) and, in anaesthetized
subjects, by Brichard and Zimmerman (1970).
Given intravenously, it has been shown to have a
potent effect in slowing and regularizing the ventricular response in atrial fibrillation (Schamroth,
1971; Schamroth, Krikler and Garrett, 1972).
In the study reported by Schamroth et al. (1972)
twenty patients with paroxysmal supraventricular
tachycardia all responded promptly to intravenous
verapamil. We have now extended the number of
cases treated, and have included a further group in
whom paroxysmal supraventricular tachycardias
were induced during intracardiac electrographic
studies. The response in some other arrhythmias is
also briefly considered.
Methods
Verapamil was administered intravenously as
previously described (Schamroth et al., 1972). A
dose of 10 mg was given over a period of 15-30 sec.
In all cases the patients were in the recumbent position, a 12-lead electrocardiogram was first recorded,
and the arrhythmia was identified. A continuous
electrocardiographic recording was started before
the injection and continued until sinus rhythm had
been restored, or for at least 5 min. The blood pressure was recorded before, immediately after and on
several occasions subsequent to the administration
of the verapamil.
In the patients studied in the laboratory, intracardiac electrographic recordings were made and
stimulation carried out as previously described
(Spurrell, Krikler and Sowton, 1973). Catheters were
passed from the femoral veins and positioned in the
right atrium, the right ventricle, and across the tricuspid valve in apposition to the bundle of His; in
some patients, transseptal puncture was performed
and recordings made from the left atrium. In all
Downloaded from http://pmj.bmj.com/ on September 18, 2016 - Published by group.bmj.com
D. M. Krikler and R. A. J.
448
Vi
-
1I
III l,I [I/]z
:l,--
1'
iA" , [
Spurrell
i TTIi
It-
FIG. 1. ECG, showing paroxysmal supraventricular tachycardia at
rhythm (100 beats a minute) 40 sec after injection of verapamil.
160 beats a minute, with
abrupt conversion to sinus
V2
-I
iI
.
- -
J' ,
l-
. --- -Ir-----
- -
'Li I
I- I
I I I
Al!
lail
.1 I I
1,AILL1
Jar
rltr
lJI
J
.- .--
I L!
A I I I
FIG. 2. ECG, showing paroxysmal supraventricular tachycardia with conversion to sinus rhythm 30 sec after verapamil,
with ventricular extrasystole at transition.
'l
244
24
II
TTT r r
Trrnl
48
....
E.w14tfl1ml-tX11
11f1
.....-9-
1161
*I
TT
alRl
60
E t77
SSS
;TXii;BEii---$-
;;n
I EM
AII
1 1
IV
T1 lTSITI
Xt1
I
7 11i,
..
.I
IIL
..1
1 1111
I I-IIIIs
FIG. 3. ECG (lead II) showing paroxysmal supraventricular tachycardia (160 beats a minute) in upper panel (0 = prior
to injection of verapamil). The middle two panels start 24 and 48 sec after verapamil, respectively, and show persistence of tachycardia pattern with progressive slowing of heart rate down to 84 beats a minute. Note the progressive PR
lengthening to 0-48 sec. In the bottom panel (60 sec) sinus rhythm has been restored at a rate of 78 beats a minute, with
a normal PR interval of 0-16 sec.
patients the procedure was essential to obtain information in the interests of their health; they were fully
informed of what was to be done, and consented to
the study. Verapamil was administered in the same
dose and tracings recorded as appropriate both from
intracardiac electrodes and surface leads, and the
response to verapamil noted.
Results
Clinical cases
Thirty-two patients suffered from paroxysmal
supraventricular tachycardia due to a circus movement affecting the atrioventricular node, and all
responded promptly to the verapamil. Typical responses are shown in Figs. 1 and 2, and consisted
either of an abrupt change to sinus rhythm, or one
punctuated by the occurrence of one or more ventricular extrasystoles; there was often a brief period of
sinus bradycardia, lasting for 30-60 sec. There was
occasional evidence of antero-grade A-V nodal conduction delay prior to restoration of sinus rhythm,
as is demonstrated in Fig. 3, where progressive PR
lengthening occurred with persistence of the tachycardia, until abrupt restoration of sinus rhythm with
a normal PR interval.
Mild transient hypotension, with a drop in the
Downloaded from http://pmj.bmj.com/ on September 18, 2016 - Published by group.bmj.com
Verapamil and tachycardia
,
=,
'I-
i. IT
' |'
T i
..
.:...
.1. .1.
449
IT
77
I.
VI
FIG. 4. ECG, showing paroxysmal supraventricular tachycardia (rate 200 beats a minute with alternating intranodal
conduction pathways or dissipation of intraventricular conduction disturbance affecting every third beat), with runs
of broad complexes due to paroxysmal ventricular tachycardia at 135 beats a minute. Note fusion beats (X) at interface
of dual tachycardias.
VI
35
ni .It1
ITTrm-1
L .1
lrrIl-t.
FIG. 5. ECG, lead VI: 35 sec after verapamil, paroxysmal supraventricular tachycardia is completely suppressed, unmasking ventricular tachycardia which persisted until DC cardioversion used.
systolic pressure to 80-100 mmHg for 2-3 min, was This is similar to our further experience with atrial
noted in four patients, but recovery was spontaflutter, which has proved less promising than the
neous. However, in a further three patients, more
original findings (Schamroth et al., 1972). We have
administered verapamil to twenty patients, achieving
marked hypotension, of the order of 60-40 mmHg,
sinus rhythm in five and a transient increase in the
was noted, and all these patients were then found to
have received oral beta-blocking agents (propranolol
degree of atrioventricular block in the remaining
or practolol) in normal therapeutic doses on the same
fifteen, without altering the cycle length of the flutter
day.
Four patients with ectopic atrial tachycardia
received verapamil. In one patient, there was conversion to sinus rhythm, preceded by A-V nodal
Wenckebach periods (see Fig. 7 in the report by
Schamroth et al., 1972). In another patient, in whom
the aetiology was congestive cardiomyopathy, the
tachycardia was converted to atrial fibrillation which
spontaneously changed to sinus rhythm 1 day later;
in the other patients, in whom the arrhythmia was
believed to be due to thyroxine overdose in one and
to cardiac ischaemia in the other, there was a transient increase in the degree of atrioventricular block.
waves in any.
A 61-year-old man who suffered from a dual
paroxysmal tachycardia of both supraventricular
and ventricular origin (Fig. 4), possibly due to
digitalis intoxication, responded promptly to intravenous verapamil in that the supraventricular tachycardia was completely controlled, but the ventricular
tachycardia persisted (Fig. 5), with consequent
haemodynamic deterioration and the need for DC
shock.
Ten patients who had reciprocating tachycardias
associated with pre-excitation syndromes all responded promptly to intravenous verapamil, with
Downloaded from http://pmj.bmj.com/ on September 18, 2016 - Published by group.bmj.com
450
D. M. Krikler and R. A. J.
I'[
1rlIq
iI
]I[
~I
III
t1
]I'
JI TI]
I'T
it
Splrrell
IrLm ]rT 71
II
4
IJff[~ii1 !.. 1il
[t
illlU
i!
!i
!.J
iIl tI
I1
I I Il II
[;J .m
.II lJ
r
JJI]
l Il
fl
I IIIL
I
i]L]
I
II
Iii'
r
........
..............
6
.
.
.
l
jjll ......
I J]IIIIIIIl]ll[]TI'lJ
J 1[IItIJ[I
10
[II
lJII
10
FIG. 6. ECGs, lead II, showing response of patient with atrial fibrillation complicating Wolff-Parkinson-White syndrome. 0 - control tracing, with maximal
pre-excitation pattern and ventricular response of 230 beats a minute. Four
minutes after verapamil, the same pattern persists but the ventricular rate has
fallen to 140. At 6 min, junctional rhythm with retrograde P'-waves, at 80 beats
a minute; at 10 min, restoration of sinus rhythm with Wolff-Parkinson-White
appearances (note negative delta wave), at 72 beats a minute.
;IIi~l]W11\t1-::-t-illi'
I I [Al
I T -l ltlmlililt-
C--,
r l
V2
VI
Iiii
iJ
III T:III'I
IIrI
I
][ i
.T
....
I
-lIlliIIIIItI II1I i11I
iT'I
7 |~~~
111
It
I.....
[ !I~ IT4II*1-1IT]
1111|IIII|Ir-lI
.......
111111
'
~ l TI Il;
i
r - ,U
I I
IrII*III1
I.
.I
Ii
*-
1'1
II
S1-
[
[
Trl gIwIUIIlllllrIIIrT.111*IIil
Lllll
llllllIl
1- 1I III
IJ~[[ I ~ III]-
V5
I:
l
ll'
IIII-I
L
ii
I*
i I
I
I[
I*IIIIn a
FIG. 7. Wolff-Parkinson-White
I1
I.lllllTN
I
Il
II
I I
Il I I Ill
oVF
V6
IIIIIIl
l][l I
^ ':,l: I I-ln--lr-'f11
lllllllll
I
'T., Ill
11l1]1|IIIIsI1-11 11 rrlll21 [1 1 ti
1!trl
r|1TII
lI
I
1-
1
1
Iii1111111IIIII 1
LX|-|E^B|Illll
li!1
TTAT
|x|+||[
wi
IL
I
[I 1J~]ILTT-Ii
TI I- nil
llJJlI I*I I
ITITITrTr1[
lKiB
Ii
db.j..
ILL
ll
V4
ll
V3
tl
aVL
11
1 I
&EjwIL
oVR
II
II i IIIII
!!11 FiIII~llll
t.l
I~
~!
I
IL
111
ii
i!ii
l[ IJ U-I
I11lIJ-I
IJILL
Al I I][
II
I I
I Fl...........1
[ l llll [.-{:I:: I:: L
IlIlZ
T
i1
BfB
l11 ll
||tEt||
nll*1l[liI
-
T..............I
L[I
Il
~III ItJ
I[
syndrome, Type B, with negative delta wave and dominant S in VI.
conversion to sinus rhythm within 2 min. One of
these patients, a 68-year-old woman, appears also to
have sinoatrial disease as judged by marked sinus
bradycardia and sinus arrhythmia and junctional or
ventricular escape beats while not receiving anti-
arrhythmic medications; paroxysmal supraventricular tachycardia occurred despite the prophylactic
oral administration of practolol 400 mg daily. She
received 10 mg verapamil intravenously, which produced prompt control of the arrhythmia, but with
temporary sinus arrest, necessitating temporary
ventricular pacing before sinus rhythm was restored.
An additional observation, in a single case of
atrial fibrillation complicating the Wolff-ParkinsonWhite syndrome, is instructive. A 36-year-old woman
had suffered one previous attack of palpitations, and
was admitted with an irregular tachycardia with
wide QRS complexes (Fig. 6). This has the appearance of atrial fibrillation complicating the WolffParkinson-White syndrome, most of the impulses
being conducted totally down the anomalous tract.
The response to intravenous verapamil was at first
Downloaded from http://pmj.bmj.com/ on September 18, 2016 - Published by group.bmj.com
451
Verapainil and tachycardia
slowing of the ventricular response (4 min), then
development of junctional rhythm with narrow
QRS complexes (6 min), and, after 10 min, restoration of sinus rhythm with the pre-excitation pattern
(see also Fig. 7).
HAE X
|4
A'
LAE
^/
Intracardiac studies
Eighteen patients with A-V junctional tachycardias were given verapamil while in circus-movement tachycardia, and in fifteen patients the tachycardia was terminated within 2-3 min. In the remaining three cases, the cycle length was prolonged in
both the anterograde and retrograde directions but
reciprocation continued. Cessation of tachycardia
could take place with interruption of the circuit either
in the anterograde pathway (Fig. 8) or in the retrograde pathway (Fig. 9) within the atrioventricular
node. Of these fifteen patients-in whom there was
no reason to suspect pre-excitation-the presence of
a concealed bypass outside the atrioventricular node
was suggested in five by constant ventriculoatrial
conduction times which were not influenced by
verapamil (Spurrell, Krikler and Sowton, 1974a).
Eight patients with Wolff-Parkinson-White syndrome were given verapamil while in circus-movement tachycardia during laboratory studies, and in
seven of these patients the tachycardia was termi-
LAE-L---
A'
---
A^
--
Y--
---
AH
AHV
HBE7r-
ECG
---
390
Atrium
545
360
AV
Ventricle
360
390
A-H 80
H-A 310
H-V 45
360
A-H 85
H-A 275
H-V 46
H-A' 375
545
P-A 29
A-H 72
H-V 52
FIG. 9. Intracardiac electrogram, conventions as in Fig.
8. Tachycardia stops after fourth V wave, i.e. in retrograde conduction within A-V node; the next two complexes are sinus beats with normal atrioventricular
conduction.
nated within 2 min. In the remaining patient, a
suitably-timed extrasystole was injected in order to
disrupt the circuit, as described by Wellens (1971).
Comment
Whether circus-movement tachycardia is due to
a process involving the atrioventricular node alone,
or whether the circuit involves an anomalous pathway as well as the A-V node, verapamil appears to
be a highly effective antiarrhythmic agent, acting
directly on the A-V node. The onset of action is
rapid, and the response prompt. Intracardiac studies
ECG
....
-"
AV.Ventricle
495
H-A' 45
A'-H 450
H-V 45
495
Rate 122/min
P-A 45
A-H 60
HHV 50
H-V
FiG. 8. Intracardiac electrogram showing high right
atrial electrogram (HAE), low right atrial electrogram
(LAE), His bundle electrogram and simultaneous surface
ECG lead. Arrhythmias stopped after third A' wave, i.e.
in anterograde direction within A-V node. The fourth
complex shows a sinus beat with normal atrioventricular
conduction.
show that verapamil has a potent effect in prolonging
A-V nodal conduction (Puech, 1972a; Husaini et al.,
1973; Roy, Spurrell and Sowton, 1974). However,
in a certain number of cases, side effects have been
noted, including hypotension, bradycardia and on
rare occasions, cardiac arrest (Benaim, 1972; Boothby, Garrard and Pickering, 1972; Sacks and Kennelly, 1972). In the majority of such cases, the prior
administration of beta-adrenergic blockers appears
to have been an important factor. As has been shown
by Nayler and Szeto (1972), verapamil and betaadrenergic blockers both have calcium-antagonistic
properties on the cell though working in totally
different ways. Whereas verapamil blocks transport
of calcium across the cell membrane, beta-blockers
interfere with intracellular calcium handling. Separately each has a mild negative inotropic effect; when
given together, this is additive (Nayler, 1974).
Downloaded from http://pmj.bmj.com/ on September 18, 2016 - Published by group.bmj.com
452
D. M. Krikler and R. A. J.
Another possible mode of adverse reaction to
verapamil implies depression of S-A nodal activity.
Under normal circumstances, the administration of
verapamil has very little if any effect on S-A nodal
automaticity (Puech, 1972a; Roy et al., 1974), but
if there is sinoatrial disease, it is to be anticipated
that any slight inherent tendency to depression will
be increased. For this reason verapamil should be
used with caution in patients with the 'sick sinus
syndrome' who present with supraventricular tachycardia (Husaini et al., 1973), as, indeed, should other
drugs. The summation of these effects is well shown
in the patient with Wolff-Parkinson-White syndrome
and sinoatrial disease in whom transient cardiac
standstill was produced after correction of her circusmovement tachycardia.
We have encountered seven other patients in
whom there were adverse effects after intravenous
verapamil. In four, verapamil had been administered
to patients who were already receiving beta-blockers.
A 64-year-old patient with the Wolff-ParkinsonWhite syndrome who had received repeated intravenous injections of practolol and propranolol and
who had needed DC cardioversions and triple-beat
ventricular pacing, suffered from repeated bouts of
tachycardia with rates up to 300 a minute, and episodes of ventricular fibrillation, for 4 days: verapamil
produced conversion to sinus rhythm but she collapsed with asystole.
While Puech (1972a) has found atropine regularly
to reverse the effect of verapamil on the A-V node,
others have found the response to be incomplete
(Roy et al., 1974). Atropine 1 mg intravenously
should, however, be given if a reaction occurs,
followed by intravenous calcium (10-20 ml of 10%
solution); an intravenous infusion of isoprenaline
may be needed and, rarely, temporary ventricular
pacing. The chance of an adverse reaction can be
minimized if it can be ensured that the patient has
not been receiving a beta-blocker for at least 6 hr
prior to the administration of verapamil. Suspicion
of sinoatrial disease merits especial caution in the
use of verapamil. However, perspective must be
maintained, as adverse reactions occur to other antiarrhythmic agents, e.g. beta-adrenergic blockers
(Szekely, 1972), and G. C. Sutton (personal communication) has observed hypotension and pulmonary
oedema in a patient with paroxysmal supraventricular tachycardia treated with intravenous practolol
who failed to return to sinus rhythm. Furthermore,
ill patients who have suffered from arrhythmias for
a protracted period are likely to have catecholamine
depletion, and may well react adversely both to betaadrenergic blockers and to verapamil, or indeed any
substance that decreases the amount of calcium
entering or available within the myocardial cell.
The response in atrial fibrillation complicating the
Spurrell
Wolff-Parkinson-White syndrome (Fig. 8) was positive but difficult to understand unless it can be inferred that the initial decrease in ventricular rate was
due to a blocking action at the atrio-bypass junction
and a subsequent antifibrillatory effect on the atrium,
restoring sinus rhythm via a phase of junctional
rhythm. Verapamil does not lengthen the refractory
period of the bypass, tending not to influence it or
produce slight shortening (Spurrell et al., 1974b).
In the vast majority of published reports, results
of treatment have been excellent (Abaza et al., 1972;
Gotsman et al., 1972; Filias and Zanoni, 1972;
Puech, 1972b). Verapamil has been shown to have
an important place in the treatment of paroxysmal
A-V nodal tachycardia. Our experience has been confined to its intravenous use and we have not made
any systematic assessment of its efficacy when given
by mouth for treatment or prophylaxis, though
others have reported satisfactory results (Bender.
1970; Abaza et al., 1972; Filias and Zanoni, 1972;
Puech, 1972b). Its preferential action on the A-V
node may be due to the fact that its potent calcium
antagonism is most sensitively felt in the N region of
the node, where a slow Na+-Ca++ channel determines conduction (Zipes, 1973). Provided precautions are taken in the selection of patients and in the
exclusion of those who have recently received betaadrenergic blockers, use of verapamil in supraventricular tachycardias provides an important and useful
form of therapy. Whether the mechanism involves
the A-V node alone or the A-V node plus an extranodal bypass, verapamil has been shown to be a
safe and effective primary agent for the treatment of
to
circus-movement supraventricular tachycardias.
References
ABAZA, A., BODINIER, C., AZIZA, CL. & GARNIER, J.C. (1972)
Etude clinique d'un nouvel antiarythmique. Coeur et Medecine Interne, 11, 757.
BENAIM, M.E. (1972) Asystole after verapamil. British
Medical Journal, 2, 169.
BENDER, F. (1970) Die Behandlung der tachycarden Arrhythmien und der arteriellen Hypertonie mit Verapamil.
Arzneimittel-Forschung, 20, 1310.
BENDER, F., KOJIMA, N., REPLOH, H.D. & OELMANN, G.
(1966) Behandlung von Rhythmusstorungen des Herzens
durch Beta-Rezeptorenblockade des Atrioventrikulargewebes. Medizinische Welt, 17, 1120.
BRICHARD, G. & ZIMMERMANN, P.E. (1970) Verapamil in
cardiac dysrhythmias during anaesthesia. British Journal
of Anaesthesia, 42, 1005.
BOOTHBY, C.B., GARRARD, C.S. & PICKERING, D. (1972)
Intravenous verapamil in cardiac arrhythmias. British
Medical Journal, 2, 349.
FILIAS, N. & ZANONI, G. (1972) Klinische Analyse der antiarrhythmischen Wirkung des Verapamils. Schweizerischer
Medizinische Wochenschrift, 102, 406.
FLECKENSTEIN, A., DORING, H.J. & KAMMERMEIER, H. (1968)
Einfluss von Beta-Receptorenblockern und verwandten
Substanzen auf Erregung, Kontraktion und Energiestoffwechsel der Myokardfaser. Klinische Wochenschrift, 46,
343.
Downloaded from http://pmj.bmj.com/ on September 18, 2016 - Published by group.bmj.com
Verapamil and tachycardia
GOTSMAN, M.S., LEWIS, B.S., BAKST, A. & MITHA, A.S.
(1972) Verapamil in life-threatening tachyarrhythmias.
South African Medical Journal, 46, 2017.
HAAS, H. & HARTFELDER, G. (1962) a-lsopropyl-a-[(Nmethyl - N - homoveratryl) - y - amino - propyl] - 3,4 - dimethoxyphenylacetonitril, eine Substanz mit koronargefasserweiternden Eigenschaften. Arzneimittel-Forschung,
12, 549.
HOFFMANN, P. (1964) Behandlung koronarer Durchblutungsstorungen mit Isoptin in der Praxis. Medizinische Klinik,
59, 1387.
HUSAINI, M.H., KVASNICKA, J., RYDEN, L. & HOLMBERG, S.
(1973) Action of verapamil in sinus node, atrioventricular,
and intraventricular conduction. British Heart Journal,
35, 734.
KAUMANN, A.J. & ARAMENDIA, P. (1968) Prevention of ventricular fibrillation induced by coronary ligation. Journal
of Pharmacology and Experimental Therapeutics, 164,
326.
MELVILLE, K.I., SHISTER, H.E. & HUQ, S. (1964) Iproveratril:
Experimental data on coronary dilation and antiarrhythmic action. Canadian Medical Association Journal, 90, 761.
NAYLER, W.G. (1974) The sub-cellular regulation of myocardial function. American Heart Journal. (In press.)
NAYLER, W.G., MCINNES, I., SWANN, J.B., PRICE, J.M.,
CARSON, V., RACE, D. & LOWE, T.E. (1968) Some effects
of iproveratril (isoptin) on the cardiovascular system.
Journal of Pharmacology and Experimental Therapeutics,
161, 247.
NAYLER, W.G. & SZETO, J. (1972) Effect of verapamil on
contractibility, oxygen utilization, and calcium exchangeability on mammalian heart muscle. Cardiovascular Research, 6, 120.
PUECH, P. (1972a) Dissection de la Conduction Sinoventriculaire pour l'Etude du Verapamil Injectable (circulated
privately).
PUECH, P. (1972b) Experimentation Clinique de l'lsoptine Injectable et par Voie Orale dans les Troubles du Rythme
Cardiaque (circulated privately).
RoY, P.R., SPURRELL, R.A.J. & SOWTON, E. (1974) The effect
of verapamil on the conduction system in man. Postgraduate
Medical Journal, 50, 270.
SACKS, H. & KENNELLY, B.M. (1972) Verapamil in cardiac
arrhythmias. British Medical Journal, 2, 716.
453
SCHAMROTH, L. (1971) Immediate effects of intravenous verapamil on atrial fibrillation. Cardiovascular Research, 5,
419.
SCHAMROTH, L., KRIKLER, D.M. & GARRETT, C. (1972)
Immediate effects of intravenous verapamil in cardiac
arrhythmias. British Medical Journal, 1, 660.
SCHMID, J.R. & HANNA, C. (1967) A comparison of the antiarrhythmic actions of two new synthetic compounds,
iproveratril and MJ 1999, with quinidine and pronethalol.
Journal of Parmacology and Experimental Therapeutics,
156, 331.
SINGH, B.N. & VAUGHAN WILLIAMS, E.M. (1972) A fourth
class of anti-dysrhythmic action? Effect of verapamil on
ouabain toxicity, on atrial and ventricular intracellular
potentials, and on other features of cardiac function.
Cardiovascular Research, 6, 109.
SPURRELL, R.A.J., KRIKLER, D.M. & SOWTON, E. (1973)
Two or more intra AV nodal pathways in association with
either a James or Kent extranodal bypass in 3 patients
with paroxysmal supraventricular tachycardia. British
Heart Journal, 35, 113.
SPURRELL, R.A.J., KRIKLER, D.M. & SOWTON, E. (1974a)
Concealed bypass of the AV node in patients with paroxysmal supraventricular tachycardia revealed by intracardiac
electrical stimulation and intravenous verapamil. American
Journal of Cardiology (in press).
SPURRELL, R.A.J., KRIKLER, D.M. & SOWTON, E. (1974b)
The effects of verapamil on the electrophysiological properties of the anomalous atrioventricular connexions in
Wolff-Parkinson-White syndrome. British Heart Journal,
36, 256.
SZEKELY, P. (1972) In: Proceedings of United KingdozmScandinavian Cardiology Meeting (Ed. by J. L. Kennedy).
Watford, Astra Chemicals Limited.
TSCHIRDEWAHN, B. & KLEPZIG, H. (1963) Klinische Untersuchung fiber die Wirkung von Isoptin und Isoptin S bei
Patienten mit Koronarinsuffizienz. Deutsche Medizinische
Wochenschrift, 88, 1702.
WELLENS, H.J.J. (1971) Electric Stimulation of the Heart in
the Study and Treatment of Tachycardias. (Ed. by H. E.
Stenfert Kroese, N.V.). Leiden.
ZIPES, D.P. (1973) In: Cardiac Arrhythmias (Ed. by L. S.
Dreifus and W. Likoff), p. 55. New York, Grune and
Stratton.
Downloaded from http://pmj.bmj.com/ on September 18, 2016 - Published by group.bmj.com
Verapamil in the treatment of
paroxysmal supraventricular
tachycardia
Dennis M. Krikler and Roworth A. J. Spurrell
Postgrad Med J 1974 50: 447-453
doi: 10.1136/pgmj.50.585.447
Updated information and services can be found at:
http://pmj.bmj.com/content/50/585/447
These include:
Email alerting
service
Receive free email alerts when new articles cite this
article. Sign up in the box at the top right corner of
the online article.
Notes
To request permissions go to:
http://group.bmj.com/group/rights-licensing/permissions
To order reprints go to:
http://journals.bmj.com/cgi/reprintform
To subscribe to BMJ go to:
http://group.bmj.com/subscribe/
Você também pode gostar
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryNo EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryNota: 3.5 de 5 estrelas3.5/5 (231)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)No EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Nota: 4.5 de 5 estrelas4.5/5 (120)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaNo EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaNota: 4.5 de 5 estrelas4.5/5 (266)
- The Little Book of Hygge: Danish Secrets to Happy LivingNo EverandThe Little Book of Hygge: Danish Secrets to Happy LivingNota: 3.5 de 5 estrelas3.5/5 (399)
- Never Split the Difference: Negotiating As If Your Life Depended On ItNo EverandNever Split the Difference: Negotiating As If Your Life Depended On ItNota: 4.5 de 5 estrelas4.5/5 (838)
- The Emperor of All Maladies: A Biography of CancerNo EverandThe Emperor of All Maladies: A Biography of CancerNota: 4.5 de 5 estrelas4.5/5 (271)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeNo EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeNota: 4 de 5 estrelas4/5 (5794)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyNo EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyNota: 3.5 de 5 estrelas3.5/5 (2259)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersNo EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersNota: 4.5 de 5 estrelas4.5/5 (344)
- Team of Rivals: The Political Genius of Abraham LincolnNo EverandTeam of Rivals: The Political Genius of Abraham LincolnNota: 4.5 de 5 estrelas4.5/5 (234)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreNo EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreNota: 4 de 5 estrelas4/5 (1090)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceNo EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceNota: 4 de 5 estrelas4/5 (895)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureNo EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureNota: 4.5 de 5 estrelas4.5/5 (474)
- The Unwinding: An Inner History of the New AmericaNo EverandThe Unwinding: An Inner History of the New AmericaNota: 4 de 5 estrelas4/5 (45)
- The Yellow House: A Memoir (2019 National Book Award Winner)No EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Nota: 4 de 5 estrelas4/5 (98)
- Dubai Healthcare Professional Licensing Guide - Final - 2Documento141 páginasDubai Healthcare Professional Licensing Guide - Final - 2Fahad IqbalAinda não há avaliações
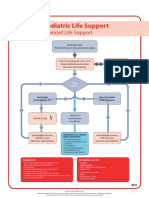
- Poster 10 PALS 01 01 ENG V20100927 PDFDocumento1 páginaPoster 10 PALS 01 01 ENG V20100927 PDFAndy XiaoAinda não há avaliações
- Congestive Heart FailureDocumento86 páginasCongestive Heart FailureNabeel ShahzadAinda não há avaliações
- ECG QuizDocumento6 páginasECG QuizIsland Rae100% (1)
- ECG at A GlanceDocumento53 páginasECG at A GlancePetrus TjiangAinda não há avaliações
- London Core Review Course - (Thurs 18 May - Sun 21 May 2017) - TimetableDocumento5 páginasLondon Core Review Course - (Thurs 18 May - Sun 21 May 2017) - Timetablelondon_core_reviewAinda não há avaliações
- Agipio BingDocumento3 páginasAgipio BingMochammad Dwiki Rahman SaniAinda não há avaliações
- Postgrad Med J 1974 Krikler 447 53Documento8 páginasPostgrad Med J 1974 Krikler 447 53Mochammad Dwiki Rahman SaniAinda não há avaliações
- Find The Passive Structures and Translate ItDocumento3 páginasFind The Passive Structures and Translate ItMochammad Dwiki Rahman SaniAinda não há avaliações
- FootballDocumento1 páginaFootballMochammad Dwiki Rahman SaniAinda não há avaliações
- Congestive Cardiac FailureDocumento61 páginasCongestive Cardiac FailureYAMINIPRIYANAinda não há avaliações
- CKDDocumento54 páginasCKDAnonymous UHnQSkxLBDAinda não há avaliações
- 1... Tell Me Something About Itself... ?: AnswerDocumento12 páginas1... Tell Me Something About Itself... ?: AnswerMuhammad BilalAinda não há avaliações
- EchocardiographyDocumento3 páginasEchocardiographyJanine Alicia VargasAinda não há avaliações
- Cardiovascular DisordersDocumento20 páginasCardiovascular DisordersHampson MalekanoAinda não há avaliações
- Diagnostic Tests in CardiologyDocumento38 páginasDiagnostic Tests in CardiologyDea Amelia YolandaAinda não há avaliações
- Cardiologist-Level Arrhythmia Detection With Convolutional Neural Networks Stanford ML Group Pranav Rakpurkar, Awni Hannun, Codie Bourn, Andrew NGDocumento9 páginasCardiologist-Level Arrhythmia Detection With Convolutional Neural Networks Stanford ML Group Pranav Rakpurkar, Awni Hannun, Codie Bourn, Andrew NGAdvaitAinda não há avaliações
- 2020 - PADUA CriteriaDocumento9 páginas2020 - PADUA CriteriaSeanglaw SituAinda não há avaliações
- Cardioversion For Atrial Fibrillation - ClinicalKeyDocumento27 páginasCardioversion For Atrial Fibrillation - ClinicalKeyAnthony Martin Corrales ParedesAinda não há avaliações
- Anti Arrhythmic DrugsDocumento22 páginasAnti Arrhythmic DrugsHarsheethaAinda não há avaliações
- Curriculum Vitae MMM 1Documento14 páginasCurriculum Vitae MMM 1sonyzanAinda não há avaliações
- Supraventricular Tachycardia NotesDocumento59 páginasSupraventricular Tachycardia NotesShadi TabbarahAinda não há avaliações
- National ECG Workshop AIMST MMA 2015Documento217 páginasNational ECG Workshop AIMST MMA 2015Sara100% (1)
- Differential Diagnosis of Elevated Troponins: Susanne Korff, Hugo A Katus, Evangelos GiannitsisDocumento7 páginasDifferential Diagnosis of Elevated Troponins: Susanne Korff, Hugo A Katus, Evangelos GiannitsisRashad AlarikyAinda não há avaliações
- NCM 118 CARDIO LECTURE LIFE THREATENING EMERGENCY CONGESTIVE HEART FAILURE MVIMMACULATA 2021 For Canvas-1Documento46 páginasNCM 118 CARDIO LECTURE LIFE THREATENING EMERGENCY CONGESTIVE HEART FAILURE MVIMMACULATA 2021 For Canvas-1Pollen Siega BunalAinda não há avaliações
- American College of PhysiciansDocumento4 páginasAmerican College of PhysiciansabimorgAinda não há avaliações
- Wenzhou People's HospitalDocumento14 páginasWenzhou People's HospitalOmega SonnadaraAinda não há avaliações
- Acc Aha Stemi 2004Documento212 páginasAcc Aha Stemi 2004NikosKosmasAinda não há avaliações
- Interpretation Cheat Sheet: VT SVTDocumento1 páginaInterpretation Cheat Sheet: VT SVTTracy Pope100% (1)
- QT Quick Guide PIIC 453564119791Documento2 páginasQT Quick Guide PIIC 453564119791mante sasmAinda não há avaliações
- Congenital Heart DiseaseDocumento57 páginasCongenital Heart DiseaseAparna RawatAinda não há avaliações
- Syndroms Suggestive of Ischemia or Infarction: EMS Assessment and Care and Hospital PrepartionDocumento8 páginasSyndroms Suggestive of Ischemia or Infarction: EMS Assessment and Care and Hospital PrepartionNugroho TeguhAinda não há avaliações
- Ebook Cardiology Secrets 6Th Edition PDF Full Chapter PDFDocumento67 páginasEbook Cardiology Secrets 6Th Edition PDF Full Chapter PDFjohn.eastman290100% (22)
- Resident/Fellow Member Application: CodeDocumento2 páginasResident/Fellow Member Application: CodeKavya ShreeAinda não há avaliações