Escolar Documentos
Profissional Documentos
Cultura Documentos
Basic Pathology Repair. Cell Growth and Regeneration. Wound Healing
Enviado por
armin5090 notas0% acharam este documento útil (0 voto)
21 visualizações4 páginasrepair
Título original
Repair
Direitos autorais
© © All Rights Reserved
Formatos disponíveis
DOC, PDF, TXT ou leia online no Scribd
Compartilhar este documento
Compartilhar ou incorporar documento
Você considera este documento útil?
Este conteúdo é inapropriado?
Denunciar este documentorepair
Direitos autorais:
© All Rights Reserved
Formatos disponíveis
Baixe no formato DOC, PDF, TXT ou leia online no Scribd
0 notas0% acharam este documento útil (0 voto)
21 visualizações4 páginasBasic Pathology Repair. Cell Growth and Regeneration. Wound Healing
Enviado por
armin509repair
Direitos autorais:
© All Rights Reserved
Formatos disponíveis
Baixe no formato DOC, PDF, TXT ou leia online no Scribd
Você está na página 1de 4
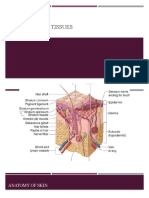
BASIC PATHOLOGY
REPAIR. CELL GROWTH AND REGENERATION. WOUND HEALING.
-proper healing needs previous removal of inflammatory and necrotic
cell debris
resolution -removal of debris associated with a complete restoration of the
tissue to preinjury state
regeneration - complete replacement of necrotic parenchymal cells by new
parenchymal cells of the same quality
-resolution and regeneration- ideal outcome of healing- is possible only in the
tissues with prevailing labile cells (cells capable of mitotic division- complete
regeneration)
-if complete resolution and regeneration is not possible, necrotic foci may be
replaced by collagen, this process is termed organisation repair by scar
formation
- mechanism of healing depends on the type of inflammation, the extent of
necrosis, regenerative capacity of damaged cells, rate of lymphatic flow,
amount of fibrin in the inflammatory exudate etc.
REGENERATION
-replacement of lost parenchymal cells is dependent on
1-regenerative capacity of the cells
2-number of surviving cells
3-maintenance of basement membranes or presence of stem cell layer
The cells of the body can be divided into 3 groups on the basis of their
regenerative capacity and their relation to the cell cycle:
1.- Labile cell (intermitotic)
2.- Stable cell (reversible postmitotic )
3.- Permanent cell (irreversible postmitotic)
1.- Labile cells- continuously dividing cells- they continue to proliferate,
remain all the time in cell cycle
-Healing in tissues with many labile cells:
-injury is followed by rapid and complete regeneration
-surgical removal of endometrium by curettage is followed by
complete regeneration from the basal germinative layer within short
time
-or destruction of erythrocytes stimulates rapid erythroid hyperplasia in
bone marrow which results in complete regeneration of erythropoesis
2.-Stable cells-quiescent- they are considered to be in G0 phase, may
undergo rapid proliferation after appropriate stimuli, they may be recruited
back to the cell cycle
Healing in tissues with prevailing stable cells:
-regeneration in tissues with most stable cell is possible but the following
conditions must be fulfilled:
-sufficient amount of viable tissue must remain
- intact fibrous interstitial network and original basement membranes
preserved
-if complete necrosis involves both parenchyma and interstitium- no
regeneration is possible and necrosis heals by scar formation
3.- Permanent cells- non-dividing. cells have no regenerative capacity
Healing in tissues with permanent cells:
-injury to tissue with permanent cells is always followed by scar formation,
no regeneration is possible.
REPAIR BY SCAR FORMATION.
scar=mass of collagen that is the final result of the process of organization
repair by scar occurs:
- if resolution fails
- if the injurious agent continuously causes injury in chronic
inflammation
- if parenchymal necrosis cannot be repaired by regeneration because
of prevalence of permanent cells
Process of repair by scar formation has several steps:
1- Preparation - the tissue is prepared by removal of the inflammatory
exudate. Debris is liquefied by lysosomal enzymes derived of neutrophil
leukocytes, liquefied material is removed by lymphatics, residual particle are
phagocytosed by macrophages
2- Ingrowth of granulation tissue
-granulation tissue is highly vascularized connective tissue composed of
newly formed capillaries, proliferating fibroblasts and myofibroblasts, cell
debris and residual inflammatory cells
-major role of the granulation tissue is to occupy the tissue defects lost
by injury
grossly- granulation tissue is deeply red (because of numerous capillaries)
and soft, with granularity of the surface
3- Collagenization
-collagens are the major fibrillary extracellular proteins.
Classification of collagens:
-types I and III collagens - interstitial types of collagen, ubiquitous,
most common in connective tissues, scars, stroma of tumours, stroma of
normal organs
-type II collagen - major collagen of cartilage
-type IV collagen - one of major constituents of BMs ( in addition to
laminin, entactin and heparan sulphate )
type V collagen - collagen of so called anchoring fibrils of BMs of
epithelia
-collagens types VI- XIII - are minor constituents of either connective
soft tissues or cartilage
The most important in scar formation are interstitial collagens type III
and I- type III composed of thin fibers, synthesised by young fibroblasts and
myofibroblast in granulation tissue, on the other hand, type I collagen
prevails in mature scar.
4- Maturation of the scar
-collagen content of granulation tissue progressively increases with the time,
particularly the amount of type I collagen increases
-the scar becomes less cellular and less vascular
-the mature scar is composed of hypovascular poorly cellular collagenous
mass- composed mostly of collagen type I
5- Contraction and strengthening
-contraction decreases the size of scar- allows optimal function of the
remaining tissue
HEALING OF SKIN WOUNDS.
1-Healing by first intention (primary union)healing of clean
uninfected surgical incision joined by surgical sutures
-limited number of dead cells, minor discontinuity of basement membrane
-the incisional space immediately fills with clotted blood containing fibrin
-within 24 hrs-neutrophils appear, there is an increased proliferation in basal
layer of epidermis at the margins of the wound - epithelial cells migrate and
synthesise basement membrane
-day 3- leukocytes disappear and the are replaced by macrophages granulation tissue progressively invades the incision space, collagen fibres
are already present but do not cross completely the incision space, and the
epithelial cells continue to proliferate
-day 5- the incision space is filled with granulation tissue, collagen fibres are
abundant and begin to bridge the incision, epidermis recovers to normal
thickness, there is a maturation of the epidermis
-2nd week- accumulation of collagen continues, but proliferation of
fibroblasts and leukocytes slow down,
- oedema, fluid, and necrotic cells mostly have disappeared, and there is a
regression of vascular channels
-end of the 1st month- scar covered by intact epidermis is finished
-the scar is composed of mature collagenous connective tissue devoid of
inflammatory infiltrate
2- Healing by second intention ( secondary union )
healing by second intention differs from primary healing in several aspects:
-large tissue defects, such as large infarctions, ulcerations, abscesses,
large wounds- have always more fibrin in exudate, thus more intense
inflammatory reaction
-much greater amount of granulation tissue is formed
-final scar is much smaller than original wound due to wound
contraction (mostly results of activities of myofibroblasts ) - tissue retraction
PATHOLOGIC ASPECTS OF REPAIR.
-Cell growth and fibroplasia are the most important aspects in healing-these processes of healing may be modified by pathologic state:
The factors that modify the quality of tissue repair include:
-nutrition deficiency, particularly vitamin C deficiency decreases the
ability to heal wounds
-glucocorticoids have anti-inflammatory effect
-persistent infection is the most important cause of delayed healing
-mechanical factors, as wound dehiscence
-low blood supply, presence of foreign bodies
-disorders of lymphatic flow may slow down the removal of necrotic
cells and cause delayed healing
-the presence or absence of diabetes mellitus and other underlying
diseases
-adequate levels of circulating white blood cells
-type of injured tissue - perfect repair may occur only in tissues built
up of labile and stable cells, while injuries to permanent cells results in
scarring, such case is myocardial infarction ( no regeneration of specialised
heart muscle elements )
-large amounts of exudate slows down a healing healing of exudate include:
-digestion of the exudate initiated by proteolytic enzymes of leukocytesresorption of dissolved exudate= process called resolution
-the presence of extensive necrosis or large amounts of fibrin in the exudate
or low blood and lymphatic rate -the process of resolution cannot occur and
the exudate is replaced by granulation tissue and transformed into fibrous
tissue (organization of exudate )- for example lung carnification in pathologic
healing of pneumonia
-aberration of growth -hyperplastic scarring- if excessive amounts of
collagen accumulate within the scar= keloid
-keloid formation appears to an individual predisposition of unknown
reasons or excessive formation of granulation tissue= exuberant granulation
- granulation tissue protrudes over the surface of the wound and in fact
blocks the reepithelization- granulation tissue must be removed surgically.
Você também pode gostar
- Med Bed Info From Skye PrinceDocumento9 páginasMed Bed Info From Skye PrinceTim0% (1)
- Tissue RepairDocumento9 páginasTissue RepairSakidu LegionAinda não há avaliações
- Tissue RepairDocumento22 páginasTissue RepairWania ZaibAinda não há avaliações
- Granulation Tissue 13102015Documento33 páginasGranulation Tissue 13102015Widi Widurai100% (1)
- 4.biologic and Synthetic Skin SubstitutesDocumento13 páginas4.biologic and Synthetic Skin SubstitutesFanny Indra WarmanAinda não há avaliações
- Hyperbaric Oxygen Therapy. Part 2Documento9 páginasHyperbaric Oxygen Therapy. Part 2Yun AkbarAinda não há avaliações
- Reviewer in Perioperative NursingDocumento12 páginasReviewer in Perioperative NursingIrish Jane Gallo100% (11)
- The Frequencies of Rifing From The First Frequencies DiscoveredDocumento2.340 páginasThe Frequencies of Rifing From The First Frequencies Discovereddragana8moracaAinda não há avaliações
- Ceu RevalidaDocumento421 páginasCeu RevalidaKENT DANIEL SEGUBIENSEAinda não há avaliações
- Tissue RepairDocumento45 páginasTissue RepairTewodros Teshome100% (1)
- Healing and RepairDocumento50 páginasHealing and RepairVrushali BhoirAinda não há avaliações
- Week 9 - Ch. 31 - SkinDocumento31 páginasWeek 9 - Ch. 31 - SkinMary SingletonAinda não há avaliações
- The Miracle of Q RAK CultivationDocumento308 páginasThe Miracle of Q RAK CultivationRafyta100% (4)
- Wound Healing (James)Documento127 páginasWound Healing (James)Ronak Upadhyay100% (5)
- Integumentary System: Quick Review Notes Chapter 5No EverandIntegumentary System: Quick Review Notes Chapter 5Nota: 5 de 5 estrelas5/5 (1)
- Delayed Surgical Recovery Nursing Care PlanDocumento3 páginasDelayed Surgical Recovery Nursing Care PlanMichala100% (3)
- Wound HealingDocumento45 páginasWound HealingmaleehaAinda não há avaliações
- Awareness and Utilization of Senior High School Students On Herbal Medicinal PlantsDocumento18 páginasAwareness and Utilization of Senior High School Students On Herbal Medicinal PlantssiahkyAinda não há avaliações
- Wound HealingDocumento36 páginasWound Healingkiran kcAinda não há avaliações
- Panacea Photonics User ManualDocumento36 páginasPanacea Photonics User Manualliterarysh1980Ainda não há avaliações
- Skin and Soft Tissue Injuries & InfectionsDocumento221 páginasSkin and Soft Tissue Injuries & InfectionsMario Espinosa100% (1)
- CH 3 PDFDocumento2 páginasCH 3 PDFKgerbAinda não há avaliações
- Unit 4.2Documento5 páginasUnit 4.2Bloody MarieAinda não há avaliações
- Healing and RepairDocumento44 páginasHealing and RepairHariharan DevarajAinda não há avaliações
- Session 13 Mechanisms of Tissue Healing and RepairDocumento40 páginasSession 13 Mechanisms of Tissue Healing and RepairGodfrey GeorgeAinda não há avaliações
- Phato HealingDocumento41 páginasPhato HealingDawit ashebrAinda não há avaliações
- Healing Definition of Healing: Assist Prof. Mustafa GheniDocumento15 páginasHealing Definition of Healing: Assist Prof. Mustafa GheniOmar MaanAinda não há avaliações
- MoD S 4 Wound Healig and Repair L1 2021-2022 (Autosaved)Documento30 páginasMoD S 4 Wound Healig and Repair L1 2021-2022 (Autosaved)حسن ميري ناصر حسونAinda não há avaliações
- By Luying Liu M.D. Department of PathologyDocumento52 páginasBy Luying Liu M.D. Department of PathologysaimAinda não há avaliações
- Organization & RepairDocumento23 páginasOrganization & Repairmilton7777Ainda não há avaliações
- 5 - HealingDocumento29 páginas5 - HealingShna SaadiAinda não há avaliações
- Lecture NotesDocumento5 páginasLecture NotesErnest Patrick MatiasAinda não há avaliações
- Healing: RegenerationDocumento14 páginasHealing: RegenerationElvisAinda não há avaliações
- Wound .Healing& Hemodynamic DisordersDocumento87 páginasWound .Healing& Hemodynamic Disordersahmed mahamedAinda não há avaliações
- Wound HealingDocumento70 páginasWound HealingRegi SeptianAinda não há avaliações
- Biology of PeriodontalDocumento78 páginasBiology of PeriodontalSudip SenAinda não há avaliações
- Tissue Repair: Banun Kusumawardani Dept. Biomedic-Faculty of Dentistry Univ. JemberDocumento35 páginasTissue Repair: Banun Kusumawardani Dept. Biomedic-Faculty of Dentistry Univ. JemberNabilah Maulina AmandaniAinda não há avaliações
- 5.tissue RepairDocumento30 páginas5.tissue Repairyaqeenallawi23Ainda não há avaliações
- 09 - L5 Inflam 2019Documento42 páginas09 - L5 Inflam 2019sagaAinda não há avaliações
- HealingDocumento7 páginasHealingapi-3699557Ainda não há avaliações
- Skin and Soft TissuesDocumento122 páginasSkin and Soft TissuesNagulan ChanemougameAinda não há avaliações
- Wound Healing and Tissue RepairDocumento27 páginasWound Healing and Tissue RepairKELVIN MAYOMBOAinda não há avaliações
- Kuliah Pemulihan JaringanDocumento38 páginasKuliah Pemulihan JaringanBrigitha Rahmadini PaputunganAinda não há avaliações
- Wound Healing and RepairDocumento67 páginasWound Healing and RepairAnicet MwaitalaAinda não há avaliações
- PBL 4 Wound Healing and Tissue AtrophyDocumento3 páginasPBL 4 Wound Healing and Tissue AtrophyadaumedAinda não há avaliações
- الاصلاحDocumento9 páginasالاصلاحNajwa AbdualgaderAinda não há avaliações
- Luka & Penyembuhan Jaringan (23 Jun 2015)Documento21 páginasLuka & Penyembuhan Jaringan (23 Jun 2015)pithoweety86Ainda não há avaliações
- Dr. Suhad Faisal HatemDocumento13 páginasDr. Suhad Faisal HatemIlyes RaniAinda não há avaliações
- Healing and Repair Flash PointsDocumento3 páginasHealing and Repair Flash PointsHassan AhmadAinda não há avaliações
- 4 Tissue-PhysiologyDocumento34 páginas4 Tissue-PhysiologyMhykhaela CaparasAinda não há avaliações
- Repair, Power-Point Bhs - InggrisDocumento24 páginasRepair, Power-Point Bhs - InggrisWildan MentalisAinda não há avaliações
- 2 - Healing & Repair2Documento36 páginas2 - Healing & Repair2aimi BatrisyiaAinda não há avaliações
- GMS511Documento29 páginasGMS511Mahmoud NafeaAinda não há avaliações
- Wound Healing-1Documento63 páginasWound Healing-1sunday danielAinda não há avaliações
- Chronic InflammationDocumento9 páginasChronic Inflammationapi-292954931Ainda não há avaliações
- Chronic Inflammation Healing and RepairDocumento51 páginasChronic Inflammation Healing and Repairahmed mokhtarAinda não há avaliações
- Wound Healing: Healing by First Intention (Primary Union)Documento31 páginasWound Healing: Healing by First Intention (Primary Union)Muhammad Masoom AkhtarAinda não há avaliações
- Pathology Week3 TissueRepairHealingAndFibrosisDocumento7 páginasPathology Week3 TissueRepairHealingAndFibrosisSalifyanji SimpambaAinda não há avaliações
- 3a. Wound HealingDocumento37 páginas3a. Wound HealingOlivia Avriyanti HanafiahAinda não há avaliações
- Inflammation and RepairDocumento34 páginasInflammation and RepairJoshua HonoridezAinda não há avaliações
- Tissue Repair: Jan Laco, MD, PHDDocumento13 páginasTissue Repair: Jan Laco, MD, PHDTni JolieAinda não há avaliações
- Wa0058.Documento33 páginasWa0058.artmanx112Ainda não há avaliações
- Wound HealingDocumento70 páginasWound HealingSachin KpAinda não há avaliações
- Regeneration. The Processes of Adaptation and Compensation: Phd. Oksana V. KaluzhynaDocumento70 páginasRegeneration. The Processes of Adaptation and Compensation: Phd. Oksana V. Kaluzhynaсветлый поповAinda não há avaliações
- Basic Mechanism Involved in Process of Inflammation and RepairDocumento32 páginasBasic Mechanism Involved in Process of Inflammation and RepairDeepakAinda não há avaliações
- Lec # 6 Inflammation & HealingDocumento31 páginasLec # 6 Inflammation & HealingsamotherlianAinda não há avaliações
- Healing and Repair: Presented By: Mahnoor Zafar Roll NO: 86Documento40 páginasHealing and Repair: Presented By: Mahnoor Zafar Roll NO: 86Mahnoor ZafarAinda não há avaliações
- Acute InflammationDocumento6 páginasAcute InflammationAnonymous ftGUywTJAinda não há avaliações
- Regeneration, Healing and Fibrosis - Ris - 10072023Documento37 páginasRegeneration, Healing and Fibrosis - Ris - 10072023Ricky LapianAinda não há avaliações
- Tissue Repair:Regeneration Healing and FibrosisDocumento50 páginasTissue Repair:Regeneration Healing and FibrosisRenas AmanAinda não há avaliações
- Wound Phases 101Documento2 páginasWound Phases 101TaraKyleUyAinda não há avaliações
- Practicum 1Documento4 páginasPracticum 1armin509Ainda não há avaliações
- Lesson 19Documento6 páginasLesson 19armin509Ainda não há avaliações
- Electrochemistry: NotesDocumento14 páginasElectrochemistry: Notesarmin509Ainda não há avaliações
- Lesson 10Documento13 páginasLesson 10armin509Ainda não há avaliações
- Carbohydrate Metabolism: NotesDocumento15 páginasCarbohydrate Metabolism: Notesarmin509Ainda não há avaliações
- Assignment QualityDocumento1 páginaAssignment Qualityarmin509Ainda não há avaliações
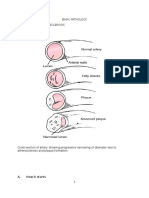
- Basic Pathology Chapter 11: Artherosclerosis: A. How It StartsDocumento2 páginasBasic Pathology Chapter 11: Artherosclerosis: A. How It Startsarmin509Ainda não há avaliações
- ABS Cell PathologyDocumento26 páginasABS Cell Pathologyarmin509Ainda não há avaliações
- PRP in Facial Rejuvenation - Dras. Rawashdeh y TorricoDocumento68 páginasPRP in Facial Rejuvenation - Dras. Rawashdeh y TorricoDra. Andrea Jiménez BelloAinda não há avaliações
- Healing Effect of Mallungay Moringa Oliefera Leaf Extract On The Wounds of Mice Mus Mulucus (AutoRecovered)Documento6 páginasHealing Effect of Mallungay Moringa Oliefera Leaf Extract On The Wounds of Mice Mus Mulucus (AutoRecovered)Edrian Cubon VillodresAinda não há avaliações
- Plant-Derived Medicines With Potential Use in WounDocumento12 páginasPlant-Derived Medicines With Potential Use in WounFatamorgana AbdullahAinda não há avaliações
- AFMM2023 - 5 - Antibacterial Electrospun Nanofibrous Materials For Wound HealingDocumento23 páginasAFMM2023 - 5 - Antibacterial Electrospun Nanofibrous Materials For Wound Healingmaolei0101Ainda não há avaliações
- Stages of Bone HealingDocumento2 páginasStages of Bone HealingArra Beatriz100% (1)
- Deskripsi Dillenia Indica LDocumento17 páginasDeskripsi Dillenia Indica LEly SavitriAinda não há avaliações
- Wound Healing: Ziv Peled, M.DDocumento8 páginasWound Healing: Ziv Peled, M.Dapi-26007957Ainda não há avaliações
- Ultrasound TherapyDocumento8 páginasUltrasound Therapyrussel786Ainda não há avaliações
- Inflammation and RepairDocumento38 páginasInflammation and RepairIsaac Nsiah Acheampong100% (1)
- Wound Healing Activity of Ipomoea Batatas Tubers (Sweet Potato)Documento14 páginasWound Healing Activity of Ipomoea Batatas Tubers (Sweet Potato)anggita ningratAinda não há avaliações
- Aloe Vera As A Treatment For Wound HealingDocumento5 páginasAloe Vera As A Treatment For Wound HealingJeffllanoAinda não há avaliações
- Anatomy, Biology, and Biomechanic of The Tendon and LigamentDocumento44 páginasAnatomy, Biology, and Biomechanic of The Tendon and LigamentsilvyaAinda não há avaliações
- Types of Burns ArticleDocumento7 páginasTypes of Burns ArticleSeltri 'ceti' SeptianiAinda não há avaliações
- Placental Therapy: An Insight To Their Biological and Therapeutic PropertiesDocumento7 páginasPlacental Therapy: An Insight To Their Biological and Therapeutic PropertiesIkaSugihartatikAinda não há avaliações
- csb0001011 Full PDFDocumento30 páginascsb0001011 Full PDFNate AlveyAinda não há avaliações
- By Raymond FrancisDocumento3 páginasBy Raymond FrancisCedric S100% (1)
- Trauma (Wound & Burn Injury) : Dr. Onarisa Ayu, SpotDocumento79 páginasTrauma (Wound & Burn Injury) : Dr. Onarisa Ayu, SpotDini YulidarAinda não há avaliações
- Bambusa BoneDocumento9 páginasBambusa BoneAulia RahadianAinda não há avaliações