Escolar Documentos
Profissional Documentos
Cultura Documentos
The Anatomy of The Liver: Sub To: DR Suguna Rao Professor Dept of Vet Path
Enviado por
AdarshBijapurTítulo original
Direitos autorais
Formatos disponíveis
Compartilhar este documento
Compartilhar ou incorporar documento
Você considera este documento útil?
Este conteúdo é inapropriado?
Denunciar este documentoDireitos autorais:
Formatos disponíveis
The Anatomy of The Liver: Sub To: DR Suguna Rao Professor Dept of Vet Path
Enviado por
AdarshBijapurDireitos autorais:
Formatos disponíveis
12/6/2011
The Anatomy of the Liver
LIVER FUNCTION TESTS
Sub to: Dr Suguna Rao
Professor
Dept of Vet Path
Sub by:
Shravankumar Gaddi
MVHK - 1040
Battery of tests performed to know the functional
status of the liver.
One specific test cannot be considered as a reliable
indicator of functioning of liver.
Liver performs various functions which are not equally
affected in disease.
Hepatic functional reserve is so great that 80% of the
organ may be destroyed before some abnormalities
can be detected.
Liver cell regeneration is so highly active that the
function of new tissue will quickly compensate for the
loss unless damage is generalized.
Liver Histology
12/6/2011
Normal histology of the liver
The Functions of Liver
3.
Liver is largest and most complex internal organ
All blood flow from intestine and pancreas reaches liver via
portal venous system
Liver is a multifunctional organ that is involved in diverse
body functions.
4.
1.
Metabolic Functions
Liver actively participates in carbohydrate metabolism, lipid,
protein, mineral and vitamin metabolisms.
2. Excretory Functions
Bile pigments, bile salts and cholesterol are excreted in bile
into intestine.
Protective functions & detoxification
Kupffer cells of liver perform phagocytosis to eliminate
foreign compounds. For example ammonia is detoxified to
urea and metabolism of xenobiotics (detoxification).
Clearance of hormones such as insulin, parathyroid
hormone, oestrogen, cortisol.
5.
Storage functions
Glycogen, vitamins A, D and B12.
6.
Serum enzymes
Acting as markers of liver damage.
Hematological and synthetic functions
Liver participates in formation of blood (particularly in
embryo).
Synthesis of plasma proteins (albumin and prothrombin),
hormones e.g angiotensinogen, insulin-like growth factor
and triiodothyronine.
Destruction of erythrocytes (Bilirubin).
Indications for liver function tests
Classification of liver function tests
Tests based upon the metabolism and excretion of biliary pigments.
Serum bilirubin - Icterus index, van den Berghs test.
Urine bilirubin - Ictotest.
Urine urobilinogen.
Fecal urobilin (Stercobilin).
Tests based upon serum enzyme activity.
Serum glutamic pyruvic transaminase (SGPT).
Serum glutamic oxaloacetic transaminase (SGOT).
Serum alkaline phosphatase (SAP).
Lactic dehydrogenase (LDH) 1.
Sorbitol dehydrogenase (SDH).
Glutamic dehydrogenase (GLDH).
Arginase.
Ornithine carbamyl transferase (OCT).
12/6/2011
Liver function tests and their site of
origin
Bromsulphalein (BSP, sulfobromophthalein) excretion test.
Cholesterol.
Tests based upon the activity of the liver in protein
metabolism.
Total serum protein
Albumin.
Globulins.
Albumin: globulin ratio (A/G).
Prothrombin.
Urea or urea nitrogen.
Blood ammonia.
Uric acid.
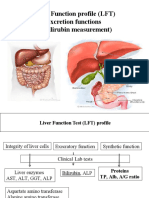
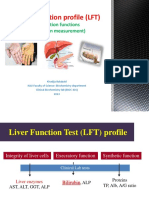
Liver chemistry test
Clinical implication of abnormality
ALT
Hepatocellular damage
AST
Hepatocellular damage
Bilirubin
Cholestasis, impair conjugation, or biliary
obstruction
ALP
Cholestasis, infiltrative disease, or biliary
obstruction
PT
Synthetic function
Albumin
Synthetic function
GGT
Cholestasis or biliary obstruction
Bile acids
Cholestasis or biliary obstruction
5`-nucleotidase
Cholestasis or biliary obstruction
LDH
Hepatocellular damage, not specific
Tests based upon the metabolism and
excretion of biliary pigments
Serum bilirubin
Icterus index
Principle The yellow color of serum or plasma is due
chiefly to the presence of bilirubin.
The intensity of the yellow color is compared with
a standard potassium dichromate solution.
The standards are expressed as units and
numbered according to the quantity of potassium
dichromate in 10,000 parts of water.
Method Obtain 5 ml of blood and allow to clot.
Separate the serum from the clot, centrifuge the serum,
and place in a test tube of the same diameter as the
standard; compare with the standard.
The plasma in the Wintrobe hematocrit tube can be used,
or the plasma in the microhematocrit capillary tube can
also be judged.
If the color is too intense to be compared, dilute the serum
with equal parts of distilled water, and multiply the reading
by 2 to express the icterus index.
Icterus index values can be read more accurately in a
photoelectric colorimeter.
12/6/2011
Normal values Dog - under 5 units
Cat - under 5 units
Pig - under 5 units
Sheep - under 5 units
Man - 2 to 6 units
Horse 25 to 30
(Varies with type of feed and time of reading.)
Interpretation
Increased
Increased blood destruction due to hemolysis
Hepatocellular damage
Biliary obstruction
Fasting or reduced fluid intake in large animals
Decreased
Bone marrow depression
van den Bergh's test
Disadvantages The icterus index is a relatively crude test, as it
measures a color that may result from other
substances than bilirubin, such as carotene,
carotenoids, and xanthophyll from ingested
plants.
It does not differentiate between the sources
of increased bilirubin.
Solution A:
Sulfanilic acid
Principle Bilirubin in the serum from obstructive jaundice reacts
immediately with Ehrlich's diazo reagent, while serum
with hemolytic jaundice requires the addition of
alcohol and a longer time interval for the reaction.
Measurement of direct (1-min) bilirubin demonstrates
the glucuronide compounds, while 30-min bilirubin
represents total bilirubin.
The quantity of free (indirect-reacting) bilirubin is the
difference between the total (30-min) and direct (1min) values.
Qualitative method -
The contact zone between the serum and the
reagent is examined against a good
background for the development of a reddishpurple ring in 30 sec, which indicates a
positive immediate direct reaction.
If the color develops after 30 sec, it is a
delayed direct reaction and has the same
significance as an indirect reaction.
Indirect reaction
After the determination of the direct reaction, shake
the tube containing the serum and diazo reagent, add 3
ml of 95% alcohol, and mix.
If a definite pinkish color fails to appear in 15 min, and
only a white turbidity occurs, the reaction is recorded
as negative.
If a definite pink color develops, or if the color already
present from a positive direct test deepens upon the
addition of alcohol, the reaction is recorded as positive
for the indirect test.
Direct reaction
1g
Concentrated hydrochloric acid
15 ml
Distilled water q.s. to make
1000 ml
Place 1 ml of nonhemolyzed serum from a fasting animal in
a graduated centrifuge tube.
Solution B:
Allow 0.5 ml of Ehrlich's diazo reagent to run down the side
of the tube so that it will overlay the serum. Ehrlich's diazo
reagent must be freshly prepared each day by mixing 10 ml
of solution A with 0.3 ml of solution B (kept in brown bottle
in refrigerator).
Sodium nitrite
0.5 g
Distilled water
100 ml
Quantitative method
Add 2 ml of nonhemolyzed serum to 18 ml of distilled
water to make a 1:10 dilution, and mix well.
Prepare the diazoreagent by adding 10 ml of solution A to
0.3 ml of solution B just before using.
To prepare the standard, place 10 mg of bilirubin in a 100ml volumetric flask and dilute to 100 ml with chloroform.
Transfer 10 ml of the stock standard to a 100-ml volumetric
flask and dilute to 100 ml with methyl alcohol.
(The dilute standard contains 0.01 mg bilirubin/ml and is
prepared just prior to use.)
12/6/2011
Into 4 colorimeter tubes measure
Distilled water, ml
Absolute methyl alcohol, ml
HC1 (1.5%), ml
Tube 1
Tube 2
Direct
blank
5
Direct
test
5
...
1
Tube 3
Tube 4
Total
blank
...
...
...
Total
test
...
...
Diazo reagent, ml
...
...
1:10 dilution serum, ml
Stopper, shake, let stand (min)
30
30
Factor
Reaction with diazo reagent
Structure
Conjugated
Unconjugated
Direct
Indirect
Bilirubin
diglucuronide
Bilirubin
For direct bilirubin, set the direct blank (tube 1) at zero
optical density at a wavelength of 540 nm, so that the
optical density of direct bilirubin (tube 2) can be read
exactly 1 min after the addition of the diluted serum.
For total bilirubin, read the optical density of the
unknown (tube 4) after it stands 30 min, with the total
blank (tube 3) set at zero optical density.
To determine the standard, place 4 ml of dilute
standard in a colorimeter tube, add 5 ml of methyl
alcohol and 1 ml of diazo reagent. Mix. Set total blank
(tube 3) at zero optical density, remove, and after 30
min read the optical density (OD) of the standard.
In water
In alcohol
normal
In bile
In urine
Unconjugated
insoluble
soluble
0.2-0.9 mg/dl
Absent
Always absent
Conjugated
soluble
soluble
0.1-0.4 mg/dl
Present
Normally absent
Not absorbed
Solubility (water)
Type of compound
Polar
Nonpolar
Absorption gut
Absorbed
Hemolytic jaundice
to +
++
Hepatocellular and obstructive jaundice
+++
Diffusion into
tissues
Diffuses yellow Doesnt diffuse
colour
Affinity for the central nervous system
(lipid soluble and can enter cells of
CNS)
Van den bergh
Indirect +
Presence in urine
Direct +
Calculation
(a) Direct reaction:
OD of direct test/OD of standard x 0.04 x 10/4 x 100 = mg
direct-reacting bilirubin/dl serum
(b) Total bilirubin:
OD of total test/OD of standard
total bilirubin/dl serum
0.04 x 10/4 x 100 = mg
(c) Indirect bilirubin:
Total bilirubin (mg/dl) direct-reacting bilirubin (mg/dl) =
indirect bilirubin (mg/dl)
Normal values
Species
Dog
Cat
Cattle
Horse
Sheep
Goat
Pig
Total bilirubin (mg/dl)
Range
Mean
0.07-0.61
0.250.1
0.15-0.20
0.01-0.47
0.21
0.2- 2
1
0-0.39
0.19
0-0.1
0-0.6
0.20.2
Conjugated bilirubin (mg/dl)
Range
0.06-0.12
0.04-0.44
0-0.4
0-0.27
0-0.3
Mean
0.14
0.18
0.1
0.12
0.10. 1
Urine bilirubin
Interpretation
Increased bilirubin values
Prehepatic
Excessive hemolysis - initially will have more
unconjugated bilirubin, but will be followed in 3
to 4 days by an increase in conjugated bilirubin,
which is probably due to the insult of the hepatic
excretory system by anemic hypoxia; decreased
PCV
Cholestasis - if 50% or more of the bilirubin is
conjugated, cholestasis is the most likely cause of
the hyperbilirubinemia.
Intrahepatic cholestasis (regurgitation jaundice)
a. Hepatocellular injury - increase in both conjugated and
unconjugated bilirubin due to the continuity of the biliary
canaliculi being compromised or obstructed as a result of
damage to the hepatic cells, as well as a decreased uptake of
unconjugated bilirubin by the impaired hepatic cells; will be
accompanied by greater increases in transaminase than
alkaline phosphatase
b. Bile duct injury
Posthepatic or extrahepatic cholestasis - bilirubin and alkaline
phosphatase will be very high
Inflammation
Neoplastic
Parasites
Congenital atresia
Azopigment conjugate of glucuronic acid.
Method - Ictotest
Normal
No reaction - in most animals
Dogs may show bilirubinuria when serum
bilirubin is greater than 0.4 mg.
Small amount of bilirubinuria is seen even in
healthy animals also.
Hemolytic jaundice - Bilirubiurmia may be seen
in small amounts.
12/6/2011
Urine urobilinogen
Increased
Small amounts
Any febrile reaction in the dog and cat
When the liver disturbance is not sufficiently severe to
cause clinical jaundice
Moderate to marked reaction
Obstructive and hepatocellular jaundice - often the first
test to become positive and frequently precedes
measurable values for serum bilirubin
Acute enteritis
Intestinal obstruction
Normal colour production is at dilution of 1:32 or 1:64.
Decreased amount or absence of urine urobilinogen
Biliary obstruction (In animals with complete biliary obstruction,
bilirubin glucuronide does not reach the intestinal tract and is not
formed).
Decreased destruction of erythrocytes
Impaired intestinal absorption
Polyuria associated with renal disease results in a dilution of the
urine urobilinogen.
Administration of antibiotics may inhibit intestinal bacteria and
interfere with urobilinogen formation.
Any delay in running the test can result in a loss of urobilinogen.
Increased amounts
Hepatocellular damage - urobilinogen cannot
be effectively removed from the circulation
because of the damaged liver cells
Hemolytic jaundice - excessive hemolysis of
erythrocytes results in an increased amount of
bilirubin, an increase in the production of
urobilinogen in the intestine, and an increased
amount of urobilinogen excreted in the urine
Bile stasis - liver shows prominent bile
plugs in dilated bile canaliculi
Cholestasis - Hepatocytes are swollen and
bile stained (feathery degeneration)
Fecal urobilin (stercobilin)
A product of urobilinogen decomposition.
Interpretation
Increased amount - feces are usually dark orange
in color
Hemolytic jaundice
Decreased amount
Biliary obstruction - clay colored feces may
indicate total biliary obstruction
Tests based upon serum enzyme
activity
Serum glutamic pyruvic transaminase (SGPT) /
Alanine amino transferase (ALT)
Enzyme (IU/L)
Dog
SGOT
SGPT
ALP
6.2 13
4.8-24
3-16
Cat
6.7 -11
1.7-14
2-7
Horse
58-94
1-6.7
11-31
Sheep
Goat
Pig
20-34
7911
43-132
8.2-21.6
4-11
Cattle
111
7-24
9-17
0-38
5-30
7-30
9-31
ARGINASE
0-4.7
0-70
1-30
0-4.5
GLUTAMIC
DEHYDROGENASE
0-11.8
ISOCITRATE
DEHYDROGENASE
0.4-7.3
2-11.7
4.8-18
9.4-21.9
0.4-8
LACTIC
DEHYDROGENASE
10-35
16-69
41-104
176-365
60-111
31-99
96-160
ORNITHINE
CARBAMYL
TRANSFERASE
2.70.7
3.81
3.34.2
4.70.3
SORBITOL
DEHYDROGENASE
2.9-8.2
3.9-7.7
1.9-5.8
4.3-15.3
5.8-27.9
14-23.6 1-5.8
Catalyze the transfer of an amino (NH2) group from an
alpha-amino acid to an alpha-keto acid, forming a new
amino acid and a new keto acid.
Alpha ketoglutaric acid + alanine
pyruvic acid +
glutamic acid.
Major sources of SGPT
The greatest amounts are found in hepatocytes in the liver
of dogs, cats, and primates, providing an enzyme that is
specific for hepatocellular damage in these species.
Little SGPT is present in the hepatic tissues of the horse,
cattle, sheep, and the pig, so its use in these species is not
indicated.
Very low concentrations of GPT are found in other tissues.
12/6/2011
Interpretation
Increased value
Hepatic cell damage (Hepatic necrosis is not necessary for the
elevation of SGPT, since an alteration in cell membrane
permeability is all that is required to leak this cytoplasmic
enzyme into the blood.) (There is poor correlation between
hepatic cell necrosis and SGPT elevation.)
Normal to moderate SGPT elevations will be seen in:
Passive congestion of the liver
Fatty metamorphosis
Hepatocellular necrosis will produce moderate to marked
elevations.
Hepatotoxins - marked elevation because of the extensive liver
cell damage
Individual circumscribed nodules or tumors may not involve a
large number of cells at any given time, and the SGPT will be
proportionately lower.
Catalyzes the transfer of the alpha-amino group of aspartic acid to
alpha-ketoglutaric acid, resulting in the formation of oxaloacetic
acid and glutamic acid respectively.
Alpha-ketoglutaric acid + aspartic acid
oxaloacetic acid +
glutamic acid
Major sources of SGOT
The highest concentrations are located in the muscle cells, with
slightly lesser amounts in the liver and heart muscle.
SGOT is not organ-specific.
Small amounts are found in many other body cells.
Kidney
Pancreas
Brain
Erythrocytes - concentration varies with the species
Dogs and cats
Myopathies
Liver necrosis
Primary and metastatic tumors
Myocardial degeneration or necrosis - minor elevations
Cardiac insufficiency - minor elevations
Drugs responsible for increases in SGOT
Salicylates
Corticosteroids
Estrogens
Androgens
Antibiotics - Erythromycin, Lincomycin, Gentamycin
Phenothiazine
Anesthetic agents capable of causing liver damage
Specific diseases produce elevated levels.
Leptospirosis
Infectious canine hepatitis
Feline infectious peritonitis
Fatty liver changes - Diabetes mellitus, Hypothyroidism, Hypoxia
Liver neoplasia
Serum glutamic oxaloacetic
transaminase (SGOT) /
Aspartate aminotransferase
Drugs
Corticosteroids, estrogens, androgens
Antibiotics chloramphenicol, Ampicillin, Gentamycin, Lincomycin,
Erythromycin
Dilantin, Primidone
Salicylates
Interpretation of increased values of SGOT
Horse
Skeletal muscle system dominates the serum levels
Exercise - increases values to 150 IU from a normal range of
50 to 110 IU; hard-working horses may show values up to
300 IU
Muscular damage - increase from 200 to 2000 IU or above
[1]
Azoturia (Tying-up syndrome)
Liver damage
In acute liver damage, levels increase from 200 to 1000 IU.
Myocardial infarction
Intestinal complications
Septicemia
Serum alkaline phosphatase (SAP)
Cattle and sheep
Muscle necrosis
Downer animals - values over 1000 IU would suggest a
serious problem
White muscle disease
Blackleg
Hepatic damage
Liver necrosis primary or secondary to traumatic
reticulitis, metritis
Ketosis
Passive congestion
Liver abscesses
Constitute a group of enzymes that are involved in the
hydrolysis of phosphate monoesters at an alkaline pH (9).
Alkaline phosphatases are important in the transport of sugar
and phosphate in the intestinal mucosa, kidney tubule, bone,
and placenta.
All the cells in the body utilizing glucose for energy contain
phosphatase.
Major sources of alkaline phosphatase
Osteoblasts and chondroblasts
Hepatobiliary system
Gastrointestinal mucosa
Renal tubules
Placenta
Spleen
Alkaline phosphatase is a microsomal enzyme, with its
principal activity being intracellular, except in the case of
osteoblasts, where it acts mainly in an extracellular location.
12/6/2011
Methods
Useful for the dog and cat, but not for the horse and cattle because of
its limited range
Principle
A buffered phenolphthalein phosphate substrate remains colorless until
decomposed by the phosphatase enzyme in the serum.
The amount of phenolphthalein liberated is determined by a color
change and is a measure of alkaline phosphatase activity.
Procedure
Place one Phosphatab tablet in a small tube provided in the kit.
Add 4 drops of serum or plasma. (If plasma is used, any anticoagulant
may be used except EDTA.) (Hemolysis will give false readings.)
Crush the tablet with the applicator stick.
Allow mixture to stand 12 to 30 min, the time being determined by
consulting the room temperature incubation table.
Add one drop of color developer.
Compare the color in the tube with the color chart.
Interpretation of increased values
Bone apposition or resorption - Osteoblasts secrete alkaline
phosphatase into the osteoid matrix in the form of
calcinous bone
Normally elevated during periods of rapid bone growth in
young animals
Healing fractures
During pregnancy because of the contributions of the fetal
bones and placenta
Osteomalacia
Osteogenic sarcoma - inconsistent
Hyperparathyroidism - primary and secondary (nutritional
and renal)
Hepatobiliary conditions
The increased amount of enzyme in hepatobiliary disease is
in response to increased pressure within the biliary system.
This is the overproduction or regurgitation theory and
evidence seems to favor this hypothesis.
It is not known whether it is the hepatocytes or the biliary
tree epithelium that produce the most alkaline
phosphatase, but it appears that the hepatocytes are the
major contributors.
Biliary obstruction - intrahepatic and extrahepatic
cholestasis results in marked SAP elevation
Secondary biliary obstruction, as with high intestinal
obstruction, causes marked elevation.
Liver necrosis - moderate elevation
Lactic dehydrogenase (LDH) 1
Fatty metamorphosis of the liver - normal to moderate
Diabetes mellitus
Hypothyroidism
Hyperadrenocorticism
Passive congestion normal to moderate elevation
Infiltrative lesions of the liver
Tumors
Amyloidosis
Granulomatous diseases
LDH catalyzes the following reaction:
Lactate + NAD*
Pyruvate + NADH + H*
LDH is located in body tissues that utilize glucose for
energy.
Because of its high concentration in many tissues, it is
not organ-specific unless isoenzyme analysis employed.
Isoenzymes of LDH - Five can be separated by
electrophoresis.
LDH-1, LDH-2 - heart, erythrocytes, kidney, brain
LDH-3 - lung, pancreas, adrenals, spleen, thymus,
thyroid, lymph nodes, leukocytes
LDH-4, LDH-5 - myocardium, skeletal muscle, brain
Renal disease - inconsistent
Gastrointestinal lesions
Diseases of the spleen
Hemolysis
Administrations of drugs
Corticosteroids
Estrogens
Androgens
Antibiotics - erythromycin
Phenothiazine
Interpretation of increased LDH levels
LDH may be elevated in many processes in which there is
cell necrosis, but because of the ubiquitous distribution of
the enzyme, it cannot be considered specific for any tissue
or pathognomonic for any specific condition.
Tissue-specific isoenzymes are helpful in identifying the
tissue of origin.
Hepatocellular necrosis
Muscle necrosis
Renal necrosis
Pancreatic necrosis
Pulmonary necrosis
Myocardial damage
Malignant neoplasms and leukemia
LDH elevation often occurs in lymphosarcoma, especially in
cattle, and is probably associated with necrosis of the
neoplasm or secondary necrosis of affected tissues.
Hemolysis
Sorbitol dehydrogenase (SDH)
12/6/2011
Catalyzes the reaction for sorbitol production from
glucose in liver.
Major sources of SDH
SDH is relatively liver-specific in most species.
It has been reported in high concentration in the
livers of man; the dog, cat, horse, pig, rabbit,
mouse, guinea pig, and frog; and in cattle and
sheep.
Kidneys - in lower concentrations
Pig - activity of the kidney is roughly 50% that of the
liver
Man
Sheep
Small intestine
Horse - less enzyme than in the liver, but more than in the
kidney
Skeletal muscle and erythrocytes contain minimal amounts
of SDH.
Hemolysis will not produce falsely elevated results.
There is no elevation after intramuscular injections as may
be the case for GOT and CPK.
Interpretation of increased values of SDH
Marked increase
Liver necrosis
Enzyme of choice for detection of liver lesions in the horse
Disappears in 24 hr, which is twice as fast as GOT and 10
times as fast as ornithine carbamyl transferase (OCT)
Glutamic dehydrogenase (GLDH)
Moderate increase
Pancreatitis
Cirrhosis
Obstructive jaundice
Diabetes mellitus
Acute intestinal obstruction - in the horse
Acute enteritis - in the horse
Grass sickness - in the horse
Mild increase
Severe azoturia - after a few days
Influenza
Arteritis
Prolonged corticosteroid administration.
Arginase
Sources
GLDH is quite liver-specific and is mainly localized in the
mitochondria.
Other organs such as muscle may contain a certain amount
of this enzyme but do not appear to influence the serum
level in a way that has clinical significance.
Interpretation of increased values
Liver disease - an elevation of its serum activity may
indicate a more severe cellular lesion than an elevation of
sorbitol dehydrogenase or transamine, especially in cattle
It is probably the liver enzyme of choice for cattle, as it is
much more sensitive than transaminase.
Limitation: Commercial kits are no longer available, which
limits the use for testing in many laboratories.
Ornithine carbamyl transferase (OCT)
Arginase is liver-specific for the horse, and values increase
in the serum following liver damage.
Arginase is found in significant concentrations within the
livers of
Horse
Dog
Cattle
Sheep
Rat
Man
Method is by gel filtration, which limits its widespread use.
OCT is liver-specific, but does not provide any
more information than SGPT, except in large
animals.
Method - cumbersome and requires several
hours for results, so easier tests are usually
preferred.
Bromsulphalein excretion test
Principle
After the injection of BSP intravenously, the dye is bound to
plasma albumin.
It is mainly confined in the vascular compartment except in
the liver, where it readily moves across the sinusoidal
endothelium and results in an accumulation within the
hepatocytes.
Unlike capillaries in other tissues of the body, the sinusoids are
freely permeable to proteins.
At the cell boundary of the hepatocyte, the dye dissociates
from the plasma albumin, moves across the cell membranes,
then associates again on the other side with proteins of the
cytoplasm.
Within the hepatocytes much of the BSP is conjugated with
glutathione.
Both conjugated BSP and unconjugated BSP are excreted into
the canaliculi and the bile.
12/6/2011
Methods
Variations may be due to
The amount of dye injected and the time interval
of the testing period
Most of the dye is removed from the plasma
relatively early, with the remaining amount
becoming progressively less as time passes.
Hepatic blood flow
Ability of the hepatic parenchymal cell mass to
remove the dye
Bile duct patency through which the excreted
products pass to the intestine
Interpretation
Normal
Dog - less than 5% retention at 30 min is considered to be within
normal limits
Horse - the normal average T1/2 value is 2.80.5 min, with a range of
2 to 3.7 min.
Cattle
Mature dairy cow - 3.1 0.6 min with a range of 2.5 to 4 min
Yearling feeder steers - average T1/2 value of 4.5 0.32 min
Sheep - the normal T1/2 value is 2 0.3 min
Increased
Parenchymal hepatic disease
Fatty metamorphosis - mild increase
Cirrhosis (Averaged 28% retention in the dog)
Toxic hepatic injury
Hepatic necrosis, especially if acute and diffuse
Biliary tract disease
Bile duct obstruction
Clearance method - for large animals
First obtain a 5-ml sample of heparinized blood.
Administer 1 g of BSP to any animal weighing
between 181.5 to 544.3 kg
Wait 5 min, then take 2 heparinized blood
samples before 12 min have elapsed, preferably
at 4 min intervals, such as 5 and 9 min, or 7 and
11 min.(Record the exact time of the collection
on the respective tubes.)
Obtain plasma by centrifuging the samples.
Place 2 ml of the respective plasmas into colorimeter tubes.
Tube 1 (blank) - presample plasma
Tube 2 - 1st postinjection sample
Tube 3 - 2nd postinjection sample
Add 1 ml of distilled water and 3 ml of 0.1 N hydrochloric
acid to tube 1 (blank).
Add 3.0 ml of 0.1 N sodium hydroxide to each of the three
tubes. Mix.
Read the percent transmission of tubes 2 and 3 against the
blank in a spectrophotometer with a wavelength set at 565
nm.
A standard curve for BSP can be made with instructions
supplied in the box of ampoules (Hynson, Westcott &
Dunning, Inc.).
The two BSP serum concentrations are plotted on semilog
paper on the vertical axis, with time in minutes on the
horizontal axis. The half-time (T1/2) is the time required for
the serum concentration to be halved.
Retention method - for small animals
Weigh the animal and calculate the dosage of BSP on a
basis of mg/kg body weight.
Inject into the cephalic vein slowly, taking 1 min and
avoiding infiltration of the dye outside the vein.
30 min after injection, withdraw 4 to 5 ml of blood from the
cephalic vein in the opposite limb.
If an anticoagulant has not been used, allow the blood to
clot, then centrifuge and collect the clear
serum or plasma.
Two clean test tubes are marked "test" and "blank."
To each tube add 1 ml of clear serum or plasma.
To the "test" tube add 4.0 ml of 0.1 N sodium
hydroxide and mix by gentle inversion.
To the "blank" tube add exactly 4.0 ml of 0.1 N
hydrochloric acid and mix by gentle inversion. (1)
The full reddish violet color develops in the alkaline
solution, and the dye is colorless in acid solution.
Read the optical density (OD) of the "test" tube at 575
nm, setting the zero with the "blank" tube.
Refer the OD reading to the calibration curve to obtain
the percentage of the dye remaining in the blood after
the 30-min interval.
Extrahepatic disease
Circulation
o Congestive heart failure
o Shock
o Fever - increases hepatic blood flow, but decreases BSP
extraction
o Hepatic vein occlusion
o Spinal cord injury
Infiltrative lesions of the liver from systemic disease
Metastatic neoplasms
Granulomatous disease (Histoplasmosis)
Amyloidosis
Relative increases in canine liver disease
Condition
Passive
congestion
Fatty
degeneration
Necrosis
Biliary
obstruction
SGOT
AP
BSP
SGPT
+
+ +
+++
+ +
+++
++
+++
+++
10
12/6/2011
Cholesterol
Cholesterol is a steroid alcohol with lipid like solubility.
It is produced by almost every cell in the body, with the
following tissues being especially active in its synthesis:
Liver
Adrenal cortex
Ovaries and testes
Intestinal epithelium
Besides the manufacture of cholesterol, the liver also:
Esterifies it, chiefly with linoleic acid
Converts a portion of it to cholic acid
Excretes it in the bile
Contraindications
Increased bilirubin levels in the blood - especially if
over 4 mg/dl (The BSP will almost always be elevated
due to competition for conjugation with free bilirubin.)
Drugs that compete for conjugation with BSP or
interfere by sharing transport steps
Cholate
Telepaque
Phenolsulfonphthalein
Iodine
Tests based upon the activity of the
liver in protein metabolism
Increased (hypercholesterolemia)
Intrahepatic and posthepatic cholestasis
Severe liver disease decreases cholesterol esters due to a
decreased release of liver enzymes that influence
esterification
Nonhepatic causes to be considered in differential
diagnosis
Diabetes mellitus
Hyperadrenocorticism
Hypothyroidism
Nephrotic syndrome
Pregnancy
Normal values (in mg/dl)
Dog
125 to 250
Cat
Goat
95 to 130
80 to 130
Sheep
52 to 76
Cattle
80 to 120
Horse
75 to 150
Pig
Rat
36 to 54
49.9 11.7
Serum protein
Dog
Cattle
Sheep
Goat
Total protein
Serum (g/dl)
5.4 7.1 5.4 7.3 5.7 7.8
6.7 - 7.4
6 7.9
6.4 7.9 7.9-8.9
Albumin (g/dl)
2.3 3.2 2.1 - 3.3
2.3 3.8
3 3.5
2.7 3.9 2.7 3.9 1.8-3.3
Globulin (g/dl)
2.7 4.4 2.6 -5.1
2.6 - 4
3 3.4
3.5 5.7 2.7 4.1 5.2-6.4
Alpha 1
0.2-0.5
0.2-1.1
0.06-0.7
0.75-0.8
0.3-0.6
Alpha 2
0.3-1.10
0.4-0.90
0.31-1.31
Beta 1
0.6-1.20
0.3-0.90
0.4-1.58
0.70-1.2
0.70-1.2
0.60-1.0
0.29-0.89
0.4-1.40
0.3-0.60
1.2-1.6
0.3-2.50
0.55-1.90
0.7-2.20
0.9-3.00
2.2-2.4
0.6-1.26
0.3-0.5
Beta 2
Gamma 1
0.5-1.30
Cat
Gamma 2
0.4-0.90
1.4-1.90
Alb : Glob Ratio
0.5-1.11
0.4-1.19
Horse
0.6-1.46
0.5-0.7
Pig
0.3-0.4
1.2-1.5
0.8-1.12
1.6-2.25
0.2-1.10
0.8-0.94
0.4-0.76
Albumin, alpha globulin, beta globulin, and
fibrinogen are synthesized in the liver from
amino acids.
Gamma globulin (immunoglobulin) is
produced by the lymphoreticular system from
amino acids.
0.1-0.3
Total serum protein
Albumin
The normal range for most animals will vary between 5 and
8 g/dl
The total serum protein concentration is usually of little
value in the assessment of liver function or disease.
The albumin fraction can be diminished and the globulin
fraction increased; the sum of the two fractions may yield a
wide range of values, from low to high, in the presence of
hepatic disease.
It is more reliable to consider the significance of
abnormalities in albumin and in globulin separately,
although a significant hypoproteinemia is usually going to
be the result of a hypoalbuminemia.
11
12/6/2011
Methods
Chemical - salt, alcohol, or isoelectric precipitation
Physical - electrophoresis, chromatography, or
ultracentrifuge
HABA dye
This is the method used in many automated clinical
chemistry instruments such as the SMA 12 of Technicon
and blood analyzer systems such as the Ames/BMI.
It produces consistently lower albumin values for animals
than for man when compared to chemical or
electrophoretic methods, as different species have different
dye-binding activities.
In the dog, the ratio of the electrophoretic albumin values
to the HABA dye method values is not too consistent, the
average ratio being 1.56.
Hypoalbuminemia
Chronic diffuse liver disease, especially cirrhosis
Failure of hepatic parenchymal synthesis of serum albumin
is not an early alteration. (The normal half-life of canine
albumin varies from 7 to 10 days, so that alterations in
serum albumin are not seen in acute hepatic failure.)
In portal cirrhosis the characteristic finding is a decrease in
serum albumin and an increase in gamma globulin.
Nonhepatic causes
Renal disease - glomerulonephritis, amyloidosis, nephrotic
syndrome
Inadequate intake or absorption
Inadequate diet
Malabsorption
Pancreatic hypoplasia or atrophy
Protein-losing gastroenteropathy
Gastrointestinal parasitism
Increased protein need - pregnancy, lactation
Globulins
Substance
Cirrhosis
Hepatocellular
Transaminase
Normal to
increased
Elevated
Bromsulphalein
Increased
Increased
Serum albumin
Low
Normal
Low A/G ratio
Either a relative or absolute increase in globulin
and/or a decrease in albumin
Chronic inflammation
Antigenic stimulation
Elevated A/G ratio
Usually the result of decreased globulin, as
increases in albumin are not likely to occur
Newborn animal before nursing
Flocculation or turbidity tests based upon the
alteration of the A/G ratio
Usually unreliable in animals, since the tests are
based upon the A/G ratio for human serum,
which does not correspond to the A/G ratios in
many animals, so false positive reactions occur.
Hyperglobulinemia - in liver disease the change is usually
polyclonal
Alpha globulins - in general, are elevated in trauma, fever,
and certain malignancies
Alpha-1 is not affected in liver disease.
Alpha-2 will have a relative increase in cirrhosis and
hepatitis.
Beta globulins - increased in hepatitis and cirrhosis
Gamma globulins - Kupffer cell proliferation and increased
numbers of plasma cells in the bone marrow may represent
the sources for increased production and elevation
Consistent elevations are seen in hepatitis, carcinoma of
the liver, and cirrhosis.
Excessive loss of protein
Renal disease - with albuminuria
Draining wounds
Burns
Internal losses - acute intestinal obstruction,
pancreatitis, acute peritonitis
Increased protein breakdown for gluconeogenesis
- fever, diabetes mellitus, hyperadrenocorticism
Albumin: globulin ratio (A/G)
Normal species variation in the A/G ratio
Albumin tends to predominate over globulin in:
Dog
Horse
Sheep
Goat
Man
Relative amounts of albumin and globulin are nearly equal
or globulin tends to be in excess of albumin in:
Cattle
Pig
Cat
Prothrombin
Principle - the liver converts vitamin K into
prothrombin
Method
The capillary coagulation time can be used as a
screening test to detect prothrombin deficiencies.
If the capillary coagulation time is prolonged, then the
longer procedure for prothrombin time can be
conducted.
Prothrombin time determination is best performed by
a commercial laboratory or a technologist
experienced in running the test.
Interpretation
Decreased prothrombin levels (increased prothrombin
time)
Two types of liver disturbance
Inability to synthesize prothrombin from vitamin K due
to a reduction of functional hepatic mass
Fat-soluble vitamin K cannot be absorbed from the
intestine with an inadequate amount of bile.
If obstruction of the bile duct occurs, an injection of 50
mg of vitamin K. may decrease coagulation time.
Diffuse parenchymal insufficiency.
12
12/6/2011
Species variation
Dog
Acute hepatic failure, as clotting factors have shorter halflives than albumin
Rather insensitive indicator, except during the acute phase;
not as sensitive as the BSP or alkaline phosphatase
elevation in detecting liver injury
Should be a screening test for coagulation problems before
performing a liver biopsy
Horse
Helpful in prognosis, as the severity of the liver damage is
related to the prolongation of prothrombin time
Levels of prothrombin significantly reduced in acute and
subacute hepatitis, hepatic necrosis with regeneration, and
diffuse fibrosis
Urea or urea nitrogen
Blood ammonia
Principle - urea is produced in the liver from the
catabolism of protein in the ornithine, citrulline,
arginine cycle
Interpretation
Urea or urea nitrogen is quite insensitive as an
indicator of liver damage.
In advanced liver damage, there is a tendency for
the blood urea nitrogen to be low, if there is not
concomitant renal damage resulting in impaired
excretion.
Principle - ammonia is produced in the gastrointestinal
tract and reaches the liver through the portal
circulation.
The ammonia is produced by bacterial action.
Hepatic cell damage
Removal of ammonia is incomplete and can be
aggravated by large amounts of protein in the diet.
Hepatic coma is usually associated with elevated blood
and cerebrospinal fluid ammonia concentrations.
Patent ductus venosus - the laboratory test of choice
for confirmation of this diagnosis
Uric acid
In most mammals, purines are metabolized to
uric acid and then to allantoin.
Exceptions include man, monkey, and the
Dalmatian breed of dog.
In the Dalmatian, only about one-third of the uric
acid is converted to allantoin, while in other
breeds of dogs it is nearly complete.
The site of conversion of uric acid to allantoin is in
the liver, and this is accomplished by the enzyme
uricase.
Interpretation
Increased - in liver cell damage, as the
conversion of uric acid to allantoin is
incomplete; as a result the amount of uric acid
in the blood and urine is elevated
The practical value of uric acid as a liver
function test is questionable, as the enzymes
and other newer tests are more sensitive
indicators of liver damage.
Thank You
13
Você também pode gostar
- Liver Function TestDocumento17 páginasLiver Function TestKarthiyayini .S.JAinda não há avaliações
- Lab 3 LFT BilirubinDocumento22 páginasLab 3 LFT Bilirubinpetemaravich333Ainda não há avaliações
- UROBILINOGEN (60 Seconds)Documento5 páginasUROBILINOGEN (60 Seconds)Margaret Nicole AboAinda não há avaliações
- Urinalysis IN Liver Disease: by Rika NilapsariDocumento27 páginasUrinalysis IN Liver Disease: by Rika NilapsarifitriAinda não há avaliações
- UrineDocumento13 páginasUrineShubham PatwaAinda não há avaliações
- Liver Function TestDocumento25 páginasLiver Function Testshivagovindan.k.pAinda não há avaliações
- Bchn222 Combined Prac Report 2Documento11 páginasBchn222 Combined Prac Report 2NOMKHULEKO ALICEAinda não há avaliações
- Putri Wulandari 024Documento8 páginasPutri Wulandari 024Septi Wulandari AnwarAinda não há avaliações
- AUBF Lec Week#5 Chemical ExaminationDocumento48 páginasAUBF Lec Week#5 Chemical ExaminationLexaNatalieConcepcionJuntadoAinda não há avaliações
- Urine Analysis Lab ConDocumento13 páginasUrine Analysis Lab ConChristineAla63% (8)
- LFT SemDocumento66 páginasLFT Sembeena gracelyn sarahAinda não há avaliações
- Multistix Reagent StripDocumento3 páginasMultistix Reagent StripFrancis TorresAinda não há avaliações
- Liver Function Test: BY Krishnakumar M SDocumento26 páginasLiver Function Test: BY Krishnakumar M SKrishna KumarAinda não há avaliações
- L3 LFTsDocumento5 páginasL3 LFTsHaswika SriyashuAinda não há avaliações
- (WHO) Blood Safety and Clinical TechnologyDocumento4 páginas(WHO) Blood Safety and Clinical TechnologyLabshare MDCAinda não há avaliações
- Biochemistry AnalyzerDocumento23 páginasBiochemistry AnalyzerBunga ExsotikaAinda não há avaliações
- Liver Function TestDocumento50 páginasLiver Function TestJhannAinda não há avaliações
- Clinical Pathology (Urin and Feces) 4semesterDocumento6 páginasClinical Pathology (Urin and Feces) 4semesterSiddhi KaulAinda não há avaliações
- Liver Assessment of Liver FunctionDocumento25 páginasLiver Assessment of Liver FunctionReman A. AlingasaAinda não há avaliações
- Bilirubin - PackInserts End PointDocumento2 páginasBilirubin - PackInserts End PointNadirAinda não há avaliações
- Chapter Four: Chemical Analysis of UrineDocumento174 páginasChapter Four: Chemical Analysis of UrineRebuma BeleteAinda não há avaliações
- 21-Functional Tests: Principle of Van Den Bergh TestDocumento7 páginas21-Functional Tests: Principle of Van Den Bergh TestadiAinda não há avaliações
- Liver Function TestsDocumento28 páginasLiver Function TestsDr. Ashish Jawarkar100% (2)
- LFT Final-1Documento14 páginasLFT Final-1ManishAinda não há avaliações
- Liver Function Tests... ROHITDocumento61 páginasLiver Function Tests... ROHITJr Jc Rohit SahAinda não há avaliações
- Fouchet's Test 3Documento5 páginasFouchet's Test 3david mchembeAinda não há avaliações
- Assessment of Liver FunctionDocumento14 páginasAssessment of Liver FunctionAaron Jed Tan PaulinoAinda não há avaliações
- Liver Function TestsDocumento16 páginasLiver Function TestsAnjali Devi100% (1)
- Exercise 15: Chemical Examination of Urine: DiscussionDocumento10 páginasExercise 15: Chemical Examination of Urine: DiscussionMarl EstradaAinda não há avaliações
- UMY BLOK 12 LIVER RENAL FUNCTION TEST 30 Maret 2020 SENTDocumento41 páginasUMY BLOK 12 LIVER RENAL FUNCTION TEST 30 Maret 2020 SENTellaAinda não há avaliações
- Examination of Body Fluids (Urinalysis)Documento109 páginasExamination of Body Fluids (Urinalysis)kiedd_04100% (9)
- Liver Function Tests: (LFTS)Documento83 páginasLiver Function Tests: (LFTS)Sreya SanilAinda não há avaliações
- Clinical Pathology-IDocumento188 páginasClinical Pathology-IZain HadiAinda não há avaliações
- Exercise 30: Preparation of ReagentsDocumento3 páginasExercise 30: Preparation of ReagentsAnanya PriyadarshiniAinda não há avaliações
- Abnormal Constituents of UrineDocumento7 páginasAbnormal Constituents of UrineAnjuAinda não há avaliações
- Liver Function Profile (LFT) Excretion Functions (Bilirubin Measurement)Documento22 páginasLiver Function Profile (LFT) Excretion Functions (Bilirubin Measurement)bushra vainceAinda não há avaliações
- Activity 11 Bile BIOCHEMDocumento8 páginasActivity 11 Bile BIOCHEMSoh Rodriguez100% (1)
- Lab Report 1 UrinalysisDocumento7 páginasLab Report 1 UrinalysisAtiqah Yeo86% (21)
- PrelimDocumento64 páginasPrelimRane MandapatAinda não há avaliações
- Aubf Module 10 UrobilinDocumento4 páginasAubf Module 10 UrobilinNelly PeñafloridaAinda não há avaliações
- Kidney Function Tests 2Documento30 páginasKidney Function Tests 2kamalAinda não há avaliações
- Legal S TestDocumento13 páginasLegal S TestTom Anthony Tonguia50% (2)
- BilirubinDocumento21 páginasBilirubinlaucegosaAinda não há avaliações
- Urine AnalysisDocumento98 páginasUrine AnalysisLucia SurduAinda não há avaliações
- Basic Principles of Clinical Chemistry, Glucose Pamphlet, BillirubinDocumento26 páginasBasic Principles of Clinical Chemistry, Glucose Pamphlet, BillirubinEslam NassarAinda não há avaliações
- Urine Examination New-1Documento81 páginasUrine Examination New-1H GondaliyaAinda não há avaliações
- Biochem2 Practical3Documento5 páginasBiochem2 Practical3puhranee nathanAinda não há avaliações
- Urine Analysis-Lab Report Biochem 3Documento8 páginasUrine Analysis-Lab Report Biochem 3Syazmin Khairuddin83% (12)
- Liver FunctionDocumento90 páginasLiver Functionapi-19641337Ainda não há avaliações
- LFT Copy PPT IMS BHUDocumento33 páginasLFT Copy PPT IMS BHUPriyanshu MandalAinda não há avaliações
- (Or Serum Chemistry) Refers To Chemical Assays WhichDocumento12 páginas(Or Serum Chemistry) Refers To Chemical Assays WhichrayevieAinda não há avaliações
- Urinalysis Lab Report 2Documento7 páginasUrinalysis Lab Report 2salman ahmedAinda não há avaliações
- Urinalysis (Part-2) Constituents of Urine: AbnormalDocumento49 páginasUrinalysis (Part-2) Constituents of Urine: AbnormalArnab GhoshAinda não há avaliações
- Upload 00473492 1531131869366Documento5 páginasUpload 00473492 1531131869366Nhan DoAinda não há avaliações
- Chemical Examination of UrineDocumento32 páginasChemical Examination of UrineMarti DeaneAinda não há avaliações
- The Mild Unconjugated Hyperbilirubinemia Respond To: Post - Hepatic HyperbilirubinaemiaDocumento10 páginasThe Mild Unconjugated Hyperbilirubinemia Respond To: Post - Hepatic HyperbilirubinaemiaJockerAinda não há avaliações
- Renal Function Test Amcj 8Documento42 páginasRenal Function Test Amcj 8Md. Saifur Rahman SunnyAinda não há avaliações
- BIO 303-ManualDocumento27 páginasBIO 303-ManualGum Naam SingerAinda não há avaliações
- Pathological Urine ConstituentsDocumento22 páginasPathological Urine Constituentsmanni1001100% (3)
- Tanuvas Surgery Notes 411Documento191 páginasTanuvas Surgery Notes 411AdarshBijapur69% (13)
- 10 Chemical Tests Fecal Occult BloodDocumento11 páginas10 Chemical Tests Fecal Occult BloodAdarshBijapurAinda não há avaliações
- Economic Traits For Sheep and GoatDocumento18 páginasEconomic Traits For Sheep and GoatAdarshBijapur89% (9)
- 04 & 05 - InflamationDocumento31 páginas04 & 05 - InflamationAdarshBijapur100% (1)
- Adarsh GlaucomaDocumento17 páginasAdarsh GlaucomaAdarshBijapurAinda não há avaliações
- VSR 606Documento3 páginasVSR 606AdarshBijapurAinda não há avaliações
- Anatomy AssignDocumento25 páginasAnatomy AssignAdarshBijapurAinda não há avaliações
- Final EchocardiographyDocumento55 páginasFinal EchocardiographyAdarshBijapur100% (1)
- Technical Aspects of ImmunohistochemistryDocumento96 páginasTechnical Aspects of ImmunohistochemistryAdarshBijapurAinda não há avaliações
- Blood Pressure Measurements PDFDocumento5 páginasBlood Pressure Measurements PDFAdarshBijapurAinda não há avaliações
- Usefulness ofDocumento42 páginasUsefulness ofAdarshBijapurAinda não há avaliações
- VSR 421Documento2 páginasVSR 421AdarshBijapur0% (1)
- Chicken Embryo Inoculation As A Diagnostic ToolDocumento29 páginasChicken Embryo Inoculation As A Diagnostic ToolAdarshBijapur100% (1)
- Fluid & ElectrolytesDocumento85 páginasFluid & ElectrolytesAdarshBijapurAinda não há avaliações
- Animal Cytology (Compatibility Mode)Documento13 páginasAnimal Cytology (Compatibility Mode)AdarshBijapurAinda não há avaliações
- Dark Field Microscopy and Its ApplicationDocumento46 páginasDark Field Microscopy and Its ApplicationAdarshBijapur100% (4)
- Usefulness of Enzyme Linked Immune Sorbent Assay: Various Methods For Disease Diagnosis and MonitoringDocumento60 páginasUsefulness of Enzyme Linked Immune Sorbent Assay: Various Methods For Disease Diagnosis and MonitoringAdarshBijapurAinda não há avaliações
- Blood Cell Counts and HematocritDocumento7 páginasBlood Cell Counts and HematocritAdarshBijapurAinda não há avaliações
- Urine AnalysisDocumento63 páginasUrine AnalysisAdarshBijapurAinda não há avaliações
- Canine Mammary GlandsDocumento10 páginasCanine Mammary GlandsAdarshBijapurAinda não há avaliações
- RectumDocumento22 páginasRectumAdarshBijapurAinda não há avaliações
- Udder & TeatDocumento23 páginasUdder & TeatAdarshBijapurAinda não há avaliações
- Affections of The JawDocumento13 páginasAffections of The JawAdarshBijapurAinda não há avaliações
- Affection of Salivary GlandsDocumento16 páginasAffection of Salivary GlandsAdarshBijapurAinda não há avaliações
- H DiagnosticsDocumento26 páginasH DiagnosticsAdarshBijapurAinda não há avaliações
- Mohit Rana Vhk-1233 VTH Bvsc. & AhDocumento26 páginasMohit Rana Vhk-1233 VTH Bvsc. & AhAdarshBijapurAinda não há avaliações
- Canine Ehrlichiosis: (Tick Fever)Documento15 páginasCanine Ehrlichiosis: (Tick Fever)AdarshBijapurAinda não há avaliações
- Snake BiteDocumento37 páginasSnake BiteAdarshBijapurAinda não há avaliações
- Canine SpirocercosisDocumento16 páginasCanine SpirocercosisAdarshBijapurAinda não há avaliações
- Foot RotDocumento10 páginasFoot RotAdarshBijapur100% (1)
- Carrageenan-Induced Paw Edema in The Rat and Mouse: Christopher J. MorrisDocumento7 páginasCarrageenan-Induced Paw Edema in The Rat and Mouse: Christopher J. MorrisraysellaAinda não há avaliações
- Biological InteractionDocumento17 páginasBiological InteractionArchana SharmaAinda não há avaliações
- Cabled Legwarmers: From Knit Picks Design TeamDocumento2 páginasCabled Legwarmers: From Knit Picks Design TeamglezglezmonicaAinda não há avaliações
- Iconicity and Chinese Characters: The Ideographic Nature of Pictograph-Based CharactersDocumento6 páginasIconicity and Chinese Characters: The Ideographic Nature of Pictograph-Based CharactersLawrence J. HowellAinda não há avaliações
- Harga Baru Nestle OkeDocumento8 páginasHarga Baru Nestle OkeFitri 'cwett' WijayantiAinda não há avaliações
- Complete Edition 1st Eso My Workbook OnlineDocumento89 páginasComplete Edition 1st Eso My Workbook OnlineJuan PedroAinda não há avaliações
- Fourth Grade Firework Night Poem Reading Comprehension ActivityDocumento3 páginasFourth Grade Firework Night Poem Reading Comprehension ActivityCharis PatricioAinda não há avaliações
- Monosyllabic Word List in Grammatical CategoriesDocumento18 páginasMonosyllabic Word List in Grammatical CategoriesJoy Peralta100% (1)
- Soal UN BIG 2017 BDocumento11 páginasSoal UN BIG 2017 BasmaAinda não há avaliações
- Toeic 1Documento82 páginasToeic 1hadu480% (1)
- Only Sense Online Vol 9Documento201 páginasOnly Sense Online Vol 9Francisco CornejoAinda não há avaliações
- Ascaris Lumbricoides: Systematic PositionDocumento10 páginasAscaris Lumbricoides: Systematic PositionUnique SolutionAinda não há avaliações
- Prevention and Control of Milk Fever, Hypomagnesemia in Dairy CattleDocumento4 páginasPrevention and Control of Milk Fever, Hypomagnesemia in Dairy CattleMz_SmikleAinda não há avaliações
- FERTILIZATIONDocumento180 páginasFERTILIZATIONPaul Kevin Mendoza67% (3)
- How The Immune System WorksDocumento13 páginasHow The Immune System Worksnishant nagyan100% (2)
- Lower GI BleedingDocumento40 páginasLower GI BleedingMohammad Firdaus100% (2)
- First Aid PresentationDocumento126 páginasFirst Aid PresentationWevinne100% (1)
- Development of Face &it's Applied AspectsDocumento95 páginasDevelopment of Face &it's Applied AspectsHansa KunduAinda não há avaliações
- Aries Kitten: Head & BodyDocumento4 páginasAries Kitten: Head & BodySelena KAinda não há avaliações
- Purina Communications PlanDocumento35 páginasPurina Communications PlanKrista Lane100% (1)
- Ella The Elephant and Her BoyDocumento8 páginasElla The Elephant and Her BoyThimany00Ainda não há avaliações
- Violet Winspear The Awakening of AliceDocumento197 páginasViolet Winspear The Awakening of AliceSaumya Bhasin80% (5)
- VOC2 - Parts of SpeechDocumento14 páginasVOC2 - Parts of SpeechThearith S. MakaraAinda não há avaliações
- The Life and Legacy of Paul Brand by April Rose FaleDocumento2 páginasThe Life and Legacy of Paul Brand by April Rose FaleApril RoseAinda não há avaliações
- Poultry SecretsDocumento94 páginasPoultry SecretsKathryn Bax75% (4)
- 1 Eye of Horus and Count Like An Egyptian 2Documento6 páginas1 Eye of Horus and Count Like An Egyptian 2yin yinAinda não há avaliações
- Group I: DNA Viruses: PoxviridaeDocumento3 páginasGroup I: DNA Viruses: PoxviridaeharoononlineAinda não há avaliações
- Grove Menu 4-14-12Documento2 páginasGrove Menu 4-14-12GroveWineBarAinda não há avaliações
- Directions: Follow The Step-By-Step Instructions For This Exercise Found On The Worksheet Below and in The Virtual Lab and Record YourDocumento4 páginasDirections: Follow The Step-By-Step Instructions For This Exercise Found On The Worksheet Below and in The Virtual Lab and Record YourTiara WilliamsAinda não há avaliações
- The Twilight TombDocumento36 páginasThe Twilight TombVictor Victorovich Khomyak100% (3)