Escolar Documentos
Profissional Documentos
Cultura Documentos
Coachman Pink QDT 2010 PDF
Enviado por
Lunna FariasTítulo original
Direitos autorais
Formatos disponíveis
Compartilhar este documento
Compartilhar ou incorporar documento
Você considera este documento útil?
Este conteúdo é inapropriado?
Denunciar este documentoDireitos autorais:
Formatos disponíveis
Coachman Pink QDT 2010 PDF
Enviado por
Lunna FariasDireitos autorais:
Formatos disponíveis
Minimally Invasive
Reconstruction in
Implant Therapy:
The Prosthetic
Gingival Restoration
Christian Coachman, CCD, CDT1
Eric Van Dooren, DDS2
Galip Gurel, DDS, MS3
Marcelo A. Calamita, DDS, MSc, PhD1
Murilo Calgaro, CDT4
Juvenal de Souza Neto, CDT5
n spite of the recent developments in periodontal
and peri-implant surgical regenerative procedures,
completely and predictably reestablishing the hard
and soft tissue contours is still a challenge in cases
with three-dimensional (3D) ridge deficiencies (Figs 1
and 2).
This article presents a reliable and consistent alternative to prosthetically restore cases with an uncertain
surgical outcome or for those patients who do not
Private Practice, So Paulo, Brazil.
Private Practice, Antwerp, Belgium.
3
Private Practice, Istanbul, Turkey.
4
Curitiba, Paran, Brazil.
5
Joinville, Santa Catarina, Brazil.
1
2
Correspondence to: Christian Coachman, Rua Bento de Andrade,
116 So Paulo, Brazil 04503-000. Email: ccoachman@hotmail.com
want to undergo regenerative surgical procedures
(Figs 3 to 14). The innovative hybrid prosthetic gingival restoration (Figs 6 to 9) makes it possible to predictably achieve an excellent match between the prosthetic and natural gingiva. Understanding the
indications and procedures involved with this technique requires a paradigm shift for the whole interdisciplinary team, but with considerable benefits to the
patient.
Surgical procedures to reestablish the 3D architecture of hard and soft tissue ridge deformities have
been developed and performed successfully throughout the last 15 years. In some cases, however, even
after several state-of-the-art regenerative procedures
such as bone grafting, soft tissue grafting, and orthodontic relocation, the results are still unpredictable,
with compromised esthetic and functional results.17
QDT 2010
COACHMAN ET AL
Figs 1 and 2 Preoperative situation. The maxillary right lateral incisor and canine are missing, with extensive soft and hard tissue deficiencies. The right central incisor and first premolar will be extracted due to
lack of interdental bone support and a peri-apical lesion.
Fig 3 Try-in of the diagnostic wax-up,
which will guide the 3D implant placement and the design of the final
restoration.
Fig 4 Healing after immediate implant
placement.
Fig 5 Ceramic try-in.
Figs 6 and 7 The gingival part of the restoration, made of pink ceramic, is only a background that will be
overlayed with pink composite resin.
Figs 8 and 9 The restoration after the addition of the direct pink composite resin.
QDT 2010
Minimally Invasive Reconstruction in Implant Therapy: The Prosthetic Gingival Restoration
10
11
12
13
Figs 10 to 13 Final outcome with excellent integration of the restoration.
Figs 14a and 14b Oneyear postoperative radiographs showing acceptable bone levels around
the dental implants
(Nobel Active RP, Nobel
Biocare, Gteborg, Sweden).
14a
The biggest challenge in alveolar ridge augmentation is the vertical aspect of the defect (Figs 15 to
21), including papillae and gingival margin levels,
which are the most esthetically important areas of
the gingiva. Tjan et al8 showed that approximately
80% of the population display part of their gingiva
when smiling, which means that the vast majority of
14b
patients requiring tissue reconstruction will expose
their gingival and ridge deficiencies. This information, in addition to the fact that patients are becoming more and more esthetically demanding, creates
an explosive combination, since all available surgical
procedures are often insufficient to reestablish ideal
esthetics.
QDT 2010
COACHMAN ET AL
Figs 15 to 17 Preoperative
situation with extensive circumferential bone loss. Note
the bone loss on the mesial
aspect of the right central and
left lateral incisors. The size,
location, and shape of the defect would lead to very low
predictability with conventional restorations.
15
18
16
19
Fig 18 Ridge deficiency analysis. The dotted lines indicate
the preoperative bone level (white), soft tissue (pink), and
crown situation (yellow).
Fig 19 Solid lines indicate the ideal position of the bone,
soft tissue, and crown.
The prosthetic gingival restoration in implant therapy can be an esthetic and functional alternative for
reconstructing ridge deformities.2,918 When designed
from the outsetrather than being used as a last resortit can dictate all adjunctive procedures necessary to achieve superior results.2,19
TREATMENT PLANNING
When properly indicated, the prosthetic gingival
restoration can predictably reestablish the esthetics of
the missing soft tissue, reproducing the shape, color,
and texture of the patients natural gingival.1114,16,2022
QDT 2010
17
20
21
Fig 20 The red area indicates the amount of bone that
should be regenerated to support ideal soft tissue esthetics
Fig 21 The red arrow shows the vertical distance between
the preoperative situation and the ideal situation. This vertical gain, which is important for the final esthetic result, is
the most challenging and unpredictable surgical modality.
Teamwork and an interdisciplinary treatment plan
are paramount to the diagnosis, execution, and longterm success of this restoration. After identifying the
patients needs and expectations, the implantologist,
periodontist, prosthodontist, and dental technician
must recognize all obstacles to attaining the ideal pink
and white esthetic results, and should discuss the
technical and biologic limitations of each specialists
role. All diagnostic data must be clearly communicated to the patient. Because many of these patients
have already undergone unsuccessful regenerative
procedures, they should be aware of the possibility of
a compromised final outcome.
The prosthetic gingival restoration is a consistent alternative to restore the patients dentogingival complex.
Minimally Invasive Reconstruction in Implant Therapy: The Prosthetic Gingival Restoration
Fig 22 Diagnostic wax-up showing the amount of missing soft tissue and the
ideal tooth shape. Managing the space was challenging because of the mesiodistal distance, which was smaller for the left central incisor than for the right central
incisor. To solve this problem, the future crown was planned to maintain the buccal position as in the preoperative situation.
Figs 23 and 24 Surgical guide. The
two black lines on the stent show the
cementoenamel junction and the apical limit of the pink wax. The second
line will be the depth guide for implant
placement. The coronal part of the implant body should be located apically
of this second surgical stent line and
must allow for palatal screw access.
23
Advantages:
Improves the predictability of pink and white esthetic restorations.
Reduces the need for and complexity of techniquesensitive surgical procedures.
Is not dependent on the patients previous treatments and restorations. [Au: Correct?]
Improves intraoral comfort and air sealing during
speech because of the smooth, uniform, and cleansable interface of the prosthetic gingiva with the remaining tissues.17,23
Simplifies technical and clinical procedures, thus decreasing cost and time.
Makes it possible to compensate for inadequate
maxillomandibular relationships.21
Disdvantages:
Requires proper patient education during treatment
planning; otherwise, the patient may get frustrated
when comparing the prosthetic gingival restoration
to a removable partial denture.
Requires an individualized maintenance program to
ensure long-term success and patient discipline to
accomplish rigorous hygiene procedures. This disadvantage can be minimized when the implants, grafts,
24
tissue conditioning, and restoration design are
planned specifically for this technique.
IMPLANT PLACEMENT:
DENTOGINGIVAL DIAGNOSTIC
WAX-UP
The dentogingival diagnostic wax-up (Fig 22) will produce an ideal esthetic restoration and will be the ultimate guide for the surgical (Figs 23 and 24), restorative, and laboratory procedures. The dental technician
must have a deep understanding of the 3D tooth and
implant positioning, gingival esthetics, and soft tissue
management to design and execute an adequate
dentogingival wax-up and restorations with harmony,
balance, and continuity of form between the natural
and prosthetic gingiva.14,17,20,22,2426
During this stage, the dental team will analyze the
3D volume of tissue loss, implant position, and gingival interfaces, based on the Quadrants Concept (Figs
25 to 29),19 to minimize the visibility of this junction,
restore the asymmetry of the gingival architecture,
and replace papillae form.14,15,17,18,24,27 This wax-up will
generate a multifunctional guide with three important
roles:
QDT 2010
COACHMAN ET AL
25
26
27
28
Fig 25 Implant positioning for gingival restoration. Computed tomography scan showing
the ideal position of the crown and gingiva.
Fig 26 The intersection of the pink line and dotted line (actual position of the gingiva) determines the horizontal line (yellow).
Fig 27 The blue line determines the axial position of the implant, aiming for a screwretained restoration.
Fig 28 The intersection of the yellow and blue lines determines the ideal position of the
implant for the pink restoration.
Fig 29 Final design of the restoration.
29
Figs 30 to 32 Immediate implant placement, palatally positioned to facilitate a screw-retained restoration. This is mandatory for a prosthetic gingival restoration. No attempt was made for vertical augmentation. A filler material (Bio-Oss,
Geistlich, Zrich, Switzerland) was used to fill the gap between the implant and the buccal cortical plate to minimize horizontal resorption.
1. Radiographic guide that will allow the team to visualize the 3D volume of tissue loss28 in the computed
tomography images.
2. Surgical guide for implant placement in prosthetic
gingival restoration cases, dictating the number, lo-
QDT 2010
cation, axis and, most importantly, the depth of the
implants (Figs 30 to 39).
3. Surgical guide for hard and soft tissue recontouring
to minimize the visibility of the junction between
natural and prosthetic gingiva and to maximize
comfort and hygiene procedures.
Minimally Invasive Reconstruction in Implant Therapy: The Prosthetic Gingival Restoration
Figs 33 and 34 The patients natural tooth was used as an
immediate provisional restoration, bonded to the adjacent
teeth. Care was taken to give the ideal prosthetic support to
the buccal gingival contour to minimize horizontal resorption.
Fig 35 Radiograph showing the relationship between the
implant and provisional. Note the apical placement of the
implant in relation to the cementoenamel junction of the
adjacent teeth.
Figs 36 to 39 Postoperative computed tomography scan. Note the apical and palatal implant placement coinciding exactly
with the intersection of the yellow and blue lines, as planned on the preoperative scan.
Fig 40 Customized ceramic shade
tabs were produced for gingiva shade
selection.
Fig 41 Bisque-bake try-in to check the
shade and shape of the crown. The
shape of the pink ceramic and the interface between the prosthetic and
natural gingiva should also be examined.
40
SOFT TISSUE CONDITIONING
The soft tissue design under the artificial gingiva is key
for the biologic, functional, and esthetic success of
this restoration and differs completely from that of a
conventional implant restoration. The need for soft tissue conditioning should be planned on the wax-up,
developed during the surgical and provisional phase,
and refined when seating the final prosthesis, depend-
41
ing on the extension of the area to be conditioned
(Figs 40 to 44).29
The alveolar ridge must be flat to generate an esthetic and cleansable interface between prosthetic
and natural gingiva.17,23 The lingual aspect of the prosthetic gingival restoration should resemble the natural
palatal contours to achieve comfort during mastication and proper phonetics, avoid food entrapment,
and promote air sealing.
QDT 2010
COACHMAN ET AL
Figs 42 and 43 If too much pressure is observed at the interface, the area can be conditioned further to relieve the
pressure.
45
46
47
Fig 44 Shaping the submergence profile to control the
pressure and design the interface between natural and artificial gingiva.
48
49
50
Fig 45 Final shape, texture, and glaze.
Fig 46 to 50 Metal-ceramic restoration after glazing and polishing.
MATERIAL SELECTION
The materials available for the prosthetic gingiva are
ceramics, composite resin, and acrylic resin. Each has
its own advantages, disadvantages, and indications.
For cemented fixed partial restorations, ceramics
are usually the material of choice to reproduce pink
and white esthetics.1118 Due to the fact that ceramic is
a delicate and challenging material to handle, with issues such as baking shrinkage, number of bakes, color
matching, and moisture control, the final pink esthetic
outcome may be compromised by an easily noticeable
interface between the prosthetic and natural gingiva.
To overcome these limitations, a hybrid technique
was developed to make the prosthetic gingiva
QDT 2010
restoration more attractive and predictable.30 The hybrid technique is defined by a screw-retained implant
partial denture with the white esthetics and the background of the pink esthetics developed in ceramic
and the final overlay of the pink contours developed
in composite resin, directly in the mouth. Various kits
of pink composite resins designed for this technique
with different colors and stains allow for a customized
restoration.
This hybrid technique offers some remarkable advantages (Figs 45 to 91):
Preservation of the optical and physical properties of
the porcelain by decreasing the number of ceramic
bakes.
Minimally Invasive Reconstruction in Implant Therapy: The Prosthetic Gingival Restoration
Fig 51 First stage of the two-stage prosthetic gingiva technique. At the first insertion appointment, the patients soft tissue
is not in an ideal condition due to the procedures performed,
such as numbing and reshaping. This makes matching the
shape, color, and texture too difficult. The best solution is to install the restoration only with the ceramic part finished and then
add the pink composite resin at a second appointment after soft
tissue healing.
Figs 52 to 59 Second stage. Preparing the restoration for the direct pink
composite resin: (left to right) mechanical retention, sandblasting, acid etching, vapor steam, silane, adhesive,
flowable composite, light curing.
52
54
55
Fig 60 The restoration in place, ready
for the direct composite buildup.
56
53
57
58
59
Fig 61 Schematic illustration showing the amount of pink ceramic that should be
placed and the space that should be left for the pink composite resin (yellow line).
More predictability and greater control of pink esthetic factors such as shape, color, and texture.
Possibility of repair, addition, recontouring, and uncomplicated maintenance, even after years of use,
without having to refire the ceramic.
QDT 2010
COACHMAN ET AL
Fig 62 The pink composite resin kit
with different colors and translucencies
(Anaxgum, Anaxdent, Stuttgart, Germany).
Fig 63 The composite resin is added
with a spatula, starting with a darker
color as a background.
Fig 64 Overlaying the composite resin
with a lighter color.
Fig 65 The margins are blended with
a flat brush.
Fig 66 With a fine-tipped probe, the
grooves and the illusion of a gingival
sulcus are created.
Fig 67 Light curing is performed after
each layer is placed.
Figs 68 to 70 Light-curing stains can be used to customize the color.
Fig 71 A brush is used to create the
superficial texture.
10
QDT 2010
Fig 72 The finished composite resin
buildup.
Fig 73 The restoration is unscrewed so
the pink composite resin can be finished chairside. Because of the interproximal extensions, the path of insertion should have two directions: first
horizontal and then vertical. To accomplish this, the implant should have an
external connection or a very short internal connection.
Minimally Invasive Reconstruction in Implant Therapy: The Prosthetic Gingival Restoration
74
75
76
77
78
79
82
83
Fig 74 The thin edge of the pink composite should be
trimmed, and the concavities underneath should be removed to improve resistance and cleansability.
Fig 75 Ideal profile of the pink composite resin after the intraoral addition.
Fig 76 When the restoration is removed from the mouth, it
shows a thin extension on the edge of the pink composite
resin that must be removed.
Fig 77 Removing the edge with a diamond bur at a 45-degree angle.
Fig 78 The edge is reduced but not removed completely.
The concavity underneath is eliminated by adding an extra
layer of composite resin that will create extra pressure on
the soft tissue and remove the edge.
Fig 79 The concavities and thin edges are eliminated.
80
81
Fig 80 The restoration is placed back in the mouth.
Fig 81 The goal at this stage is to blend the transition between the artificial and natural soft tissue. The removal of the pink
composite resin edge will create a visible and unattractive interface that must be modified.
Fig 82 The visible interface occurs mainly because of the difference in light reflection between the artificial and natural gingival.
Fig 83 A round diamond bur is used to match the profile of the artificial and natural gingiva.
QDT 2010
11
COACHMAN ET AL
Fig 84 The unnatural angle between the artificial
and natural gingiva is removed.
84
Fig 85 The light reflection has a similar direction
on the natural and artificial soft tissue, providing
the illusion of continuity. This mimetic effect will
improve even more with the addition of the
saliva.
85
Fig 86 The adhesive is applied to the
areas where composite resin will be applied, such as undercuts and concavities.
Fig 87 Adding pink composite resin to
the undercuts and concavities may
raise the complexity of the hygiene
procedures.
86
87
Fig 91 During final polishing, care must be taken not
to remove the gingiva-like
texture.
Figs 88 to 90 Final emergence profile after reshaping and adding composite
resin chairside.
88
89
SEATING AND HYGIENE
During the seating process a transitory blenching may
be observed. The intensity will vary depending on the
extension of the tissue conditioning required, the design of the pontics, and the gingival biotype. The
pressure between the natural and prosthetic gingiva
should be checked with dental floss. Flossing in this
12
QDT 2010
90
91
area should have the same intensity of pressure as exists with ideal interproximal contact between adjacent
natural dentition. Excess pressure should be reduced
by reshaping the soft tissue with diamond burs or a
diode laser, or by recontouring the prosthetic gingiva
with specific burs and wheels. The main goal is to create a comfortable, healthy, and cleansable interface
while maintaining high esthetics.
Minimally Invasive Reconstruction in Implant Therapy: The Prosthetic Gingival Restoration
Figs 92 and 93 It is paramount to periodically probe the bone level on the
adjacent teeth to check if the artificial
gingiva flaps overlapping these teeth
are compromising the surrounding tissues.
92
93
94
95
96
97
98
99
100
101
Figs 94 to 101 Hygiene procedures.
The floss should go around the artificial
gingiva on both sides and completely
touch the interface between the natural and prosthetic gingiva.
The hygiene and maintenance procedures should
be carefully discussed with the patient. Follow-up appointments should be scheduled initially 3 months
after insertion and then can be moved up to every 6
months to 1 year, depending on the patients risk assessment.
Probing the bone level of the adjacent natural
teeth is highly recommended before seating the pros-
thesis for further comparison during the follow-up appointments (Fig 92 and 93). During these sessions, the
restoration should be removed to check the health of
the soft tissue and to probe the adjacent teeth. If the
situation of the soft tissues is not ideal, new hygiene
education should be given, followed by reshaping of
the prosthesis, if necessary, to allow ideal hygiene procedures (Figs 94 to 101).
QDT 2010
13
COACHMAN ET AL
Fig 102 Final result.
Fig 103 Six-month postoperative view.
102
103
When properly planned and executed, the hybrid
prosthetic gingival restoration offers predictable functional and esthetic results (Figs 102 and 103).
tive, and technical procedures can be executed to
maximize the biological, functional and esthetic results
and surpass the patients expectations.
CONCLUSION
REFERENCES
The prosthetic regeneration of pink esthetics is a reliable and consistent alternative to resolve cases with
an uncertain surgical outcome or for patients who do
not want to undergo regenerative surgical procedures.
When this type of restoration is planned from the beginning of treatment, the appropriate surgical, restora-
14
QDT 2010
1. Salama H, Salama M, Garber D, Rosenberg ES. 50 years of site
development: Lessons and guidelines from periodontal prosthesis. J Esthet Dent 1998;10:149156.
2. Coachman C, Salama M, Garber D, Calamita MA, Salama H,
Cabral G. Prosthetic gingival reconstruction in a fixed partial
restoration. Part 1: Introduction to artificial gingiva as an alternative therapy. Int J Periodontics Restorative Dent
2009,29:471477.
Minimally Invasive Reconstruction in Implant Therapy: The Prosthetic Gingival Restoration
3. Costello FW. Real teeth wear pink. Dent Today 1995;14:5255.
4. Tarnow DP, Magner AW, Fletcher P. The effect of the distance
from the contact point to the crest of bone on the presence or
absence of the interproximal dental papilla. J Periodontol
1992;63:995996.
5. Salama H, Salama MA, Garber D, Adar P. The interproximal
height of bone: A guidepost to predictable aesthetic strategies and soft tissue contours in anterior tooth replacement.
Pract Periodontics Aesthet Dent 1998;10:11311141.
6. Saadoun AP, LeGall M, Touati B. Selection and ideal three-dimensional implant position for soft tissue aesthetic. Pract Periodontics Aesthet Dent 1999;11:10631072.
7. Kois JC. Predictable single tooth peri-implant esthetics: Five
diagnostic keys. Compend Contin Educ Dent
2001;22:199206.
8. Tjan AHL, Miller GD, The JG. Some esthetic factors in a smile.
J Prosthet Dent 1984;51:2428.
9. Coachman C, Garber D, Salama, M, Salama H, Cabral G,
Calamita MA. The incorporation of tissue colored composite
and a zirconium abutment to solve an esthetic soft tissue
asymmetry. Inside Rest Dent 2008;4:25.
10. Kamalakidis S, Paniz G, Kang KH, Hirayama H. Nonsurgical
management of soft tissue deficiencies for anterior single implant-supported restorations: A clinical report. J Prosthet Dent
2007;97:15.
11. Rosa DM, Souza Neto J. Odontologia esttica e a prtese fixa
dentogengivalConsideraes cirrgicas e protticasCasos
clnicos e laboratoriais: Uma alternativa entre as solues estticas. J Assoc Paul Cir Dent 1999;53:291296.
12. Rosa DM, Zardo CM, Souza Neto J. Prtese Fixa MetaloCermica Dento-Gengival: Uma Alternativa Entre as Solues
Estticas. So Paulo: Artes Mdicas. 2003.
13. Barzilay I, Tamblyn I. Gingival prosthesesA review. J Can
Dent Assoc 2003;69:7478.
14. Duncan JD, Swift E. Use of tissue-tinted porcelain to restore
soft-tissue defects. J Prosthodont 1994;3:5961.
15. Tallents RH. Artificial gingival replacements. Oral Health
1983;73:3740.
16. Botha PJ, Gluckman HL. Gingival prosthesis: A literature review. S Afr Dent J 1999;54:288290.
17. Garcia LT, Verrett RG. Metal-ceramic restorationsCustom
characterization with pink porcelain. Compend Contin Educ
Dent 2004;25:242246.
18. Simon H, Raigrodski AJ. Gingiva colored ceramics for enhanced
esthetics.
Quintessence
Dent
Technol
2002;25:155172.
19. Coachman C, Salama M, Garber D, Calamita MA, Salama H,
Cabral G. Prosthetic gingival reconstruction in the fixed partial
restoration. Part 2: Diagnosis and treatment planning. Int J Periodontics Restorative Dent (in press).
20. Hannon SM, Colvin CJ, Zurek DJ. Selective use of gingivaltoned ceramics: Case reports. Quintessence Int
1994;25:233238.
21. Cronin RJ, Wardle WL. Loss of anterior interdental tissue: Periodontal and prosthodontic solutions. J Prosthet Dent
1983;50:505509.
22. Goodacre CJ. Gingival esthetics. J Prosthet Dent
1990;64:112.
23. Behrend DA. The design of multiple pontics. J Prosthet Dent
1981;46:634638.
24. Priest GF, Lindke L. Gingival-colored porcelain for implant-supported prostheses in the aesthetic zone. Pract Periodontics
Aesthet Dent 1998;10:12311240.
25. Priest GF. The esthetic challenge of adjacent implants. J Oral
Maxillofac Surg 2007;65:212.
26. Harel S. Esthetic applications of gingiva-colored ceramics in
implant prosthodontics. Presented at the 21st Annual Meeting
of the Academy of Osseointegration, Seattle, 2006.
27. Garber DA. The esthetic dental implant: Letting restoration be
the guide. J Am Dent Assoc 1995;126:319325.
28. Ganz SD. Presurgical planning with CT derived fabrication of
surgical guides. J Oral Maxillofac Surg 2005;63:5971.
29. Johnson GK, Leary JM. Pontic design and localized ridge augmentation in fixed partial denture design. Dent Clin North Am
1992;36:591605.
30. Coachman C, Salama M, Garber D, Calamita MA, Salama H,
Cabral G. Prosthetic gingival reconstruction in the fixed partial
restoration. Part 3. Int J Periodontics Restorative Dent (in
press).
QDT 2010
15
Você também pode gostar
- Coachman Pink QDT 2010 PDFDocumento15 páginasCoachman Pink QDT 2010 PDFHugoMoralesTecnicoDentalAinda não há avaliações
- Patología Bucal - Bruch (Ingles)Documento176 páginasPatología Bucal - Bruch (Ingles)MarielEsmeraldaAinda não há avaliações
- Removable Denture Prosthetics - Technical Protocol PDFDocumento42 páginasRemovable Denture Prosthetics - Technical Protocol PDFDaniel DidiAinda não há avaliações
- Volume 7, No. 8 October The Journal of Implant & Amp Advanced Clinical Dentistry. The Keyless Partially Guided Implant ProtocolDocumento54 páginasVolume 7, No. 8 October The Journal of Implant & Amp Advanced Clinical Dentistry. The Keyless Partially Guided Implant ProtocolAndré NunesAinda não há avaliações
- Getting The Most Out of Panoramic Radiographic Interpretation - Allan G. FarmanDocumento6 páginasGetting The Most Out of Panoramic Radiographic Interpretation - Allan G. FarmanTudor-George GherasimAinda não há avaliações
- DENTURES: The Ultimate Guide to Dentures & Denture Care for a Beautifully Restored SmileNo EverandDENTURES: The Ultimate Guide to Dentures & Denture Care for a Beautifully Restored SmileAinda não há avaliações
- Zygomatic ImplantDocumento18 páginasZygomatic ImplantsmritinarayanAinda não há avaliações
- Centric RelationDocumento50 páginasCentric RelationHarini Padmanabhan100% (1)
- STANDARDIZED DIGITAL PHOTOGRAPHY FOR VIRTUAL ORTHOGNATHIC SURGICAL PLANNINGCintra20.3G - Web PDFDocumento20 páginasSTANDARDIZED DIGITAL PHOTOGRAPHY FOR VIRTUAL ORTHOGNATHIC SURGICAL PLANNINGCintra20.3G - Web PDFCalderon RafaAinda não há avaliações
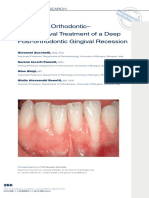
- Combined Orthodontic - .Vdphjohjwbm5Sfbunfoupgb Q 1ptupsuipepoujd (Johjwbm3FdfttjpoDocumento16 páginasCombined Orthodontic - .Vdphjohjwbm5Sfbunfoupgb Q 1ptupsuipepoujd (Johjwbm3FdfttjpobetziiAinda não há avaliações
- Dental Implant PlanningDocumento4 páginasDental Implant PlanningDr. Hamid RaihanAinda não há avaliações
- Diagnosis & Treatment PlanningDocumento46 páginasDiagnosis & Treatment PlanningNeha ChughAinda não há avaliações
- Atlas of Mandibular and Maxillary Reconstruction With The FibulaDocumento115 páginasAtlas of Mandibular and Maxillary Reconstruction With The FibulaOmar VillamizarAinda não há avaliações
- Craniomandibular Function and Dysfunction: Leaf GaugeDocumento7 páginasCraniomandibular Function and Dysfunction: Leaf GaugeAkanksha MahajanAinda não há avaliações
- 18 1994 - John Preston - The Golden Proportion RevistedDocumento5 páginas18 1994 - John Preston - The Golden Proportion RevistedSilvia KriAinda não há avaliações
- Fiber Post Techniques For Anatomical Root VariationsDocumento21 páginasFiber Post Techniques For Anatomical Root VariationsnromadhanyAinda não há avaliações
- Optimization of Emergence Profile of Implant ProstDocumento8 páginasOptimization of Emergence Profile of Implant ProstAya Ibrahim YassinAinda não há avaliações
- FPD DesignDocumento9 páginasFPD DesignMohamed AliAinda não há avaliações
- Entrevista Do OKESONDocumento10 páginasEntrevista Do OKESONWanniely KussAinda não há avaliações
- Red ProportionDocumento14 páginasRed ProportionBenjamin Santiago100% (1)
- Sinus Lift PDFDocumento4 páginasSinus Lift PDFEctoDermaPolyklinika100% (1)
- Management of Orbital FracturesDocumento12 páginasManagement of Orbital FracturesMarisol Gallego DuqueAinda não há avaliações
- Optimizing Smile Composition and Esthetics With Resin Composites and Other Conservative Esthetic ProceduresDocumento16 páginasOptimizing Smile Composition and Esthetics With Resin Composites and Other Conservative Esthetic ProceduresTiagoAinda não há avaliações
- Direct vs. Indirect Sinus Lift Procedure: A Comparison: March 2012Documento8 páginasDirect vs. Indirect Sinus Lift Procedure: A Comparison: March 2012Sooraj SAinda não há avaliações
- Peri Implant Tissue EvaluationDocumento129 páginasPeri Implant Tissue EvaluationDrMohamed Assadawy100% (1)
- Peri-Implant Health, Peri-Implant Mucositis, and Peri-Implantitis: Case Definitions and Diagnostic ConsiderationsDocumento9 páginasPeri-Implant Health, Peri-Implant Mucositis, and Peri-Implantitis: Case Definitions and Diagnostic ConsiderationsFrancisca Cardenas OñateAinda não há avaliações
- Logbook Spring 2023Documento79 páginasLogbook Spring 2023Horn DudeAinda não há avaliações
- Dentsply Sirona Anterior Posterior Tooth Arrangement Manual 2Documento43 páginasDentsply Sirona Anterior Posterior Tooth Arrangement Manual 2Eslam ElghazoulyAinda não há avaliações
- Morphology of Permanent CaninesDocumento15 páginasMorphology of Permanent Caninesamanita238Ainda não há avaliações
- Introduction To OcclusionDocumento56 páginasIntroduction To OcclusionSuvasish SuvasishAinda não há avaliações
- Direct Vs Indirect Sinus LiftDocumento6 páginasDirect Vs Indirect Sinus LiftShounak GhoshAinda não há avaliações
- Best Completes The Statement or Best Answers The QuestionDocumento6 páginasBest Completes The Statement or Best Answers The QuestionChintan PatelAinda não há avaliações
- A Beginners Guide To Lateral Cephalometric RadiographsDocumento4 páginasA Beginners Guide To Lateral Cephalometric RadiographsClaudiaAinda não há avaliações
- Smile Analysis Part 2Documento11 páginasSmile Analysis Part 2Mircea Ilie100% (1)
- Aaoms 2010 Sinus Grafting SymposiumDocumento63 páginasAaoms 2010 Sinus Grafting SymposiumNAPCO123100% (1)
- ANKYLOSIS of TMJ Oral SurgeryDocumento52 páginasANKYLOSIS of TMJ Oral SurgeryAbhishek ChauhanAinda não há avaliações
- Paolucci Visagism QDTDocumento14 páginasPaolucci Visagism QDTDumitruChele100% (1)
- Multimedia PDFDocumento16 páginasMultimedia PDFadamAinda não há avaliações
- Cross Finger FlapDocumento36 páginasCross Finger FlapvenuAinda não há avaliações
- Platelet Rich FibrinDocumento7 páginasPlatelet Rich FibrinNelly AndriescuAinda não há avaliações
- Endodontic Emergencies and Its ManagementDocumento40 páginasEndodontic Emergencies and Its Managementsonalbatra100% (1)
- Modellherstellungsfibel en PDFDocumento45 páginasModellherstellungsfibel en PDFcontinentdriftAinda não há avaliações
- Impact of Lateral Occlusion Schemes: A Systematic ReviewDocumento12 páginasImpact of Lateral Occlusion Schemes: A Systematic ReviewCristobalVeraAinda não há avaliações
- Mandibular Condylar and Subcondylar Fractures PDFDocumento16 páginasMandibular Condylar and Subcondylar Fractures PDFWayan Sutresna YasaAinda não há avaliações
- CAD CAM Splints For The Functional and Esthetic Evaluation of Newly Defined Occlusal Dimensions PDFDocumento12 páginasCAD CAM Splints For The Functional and Esthetic Evaluation of Newly Defined Occlusal Dimensions PDFEsme ValenciaAinda não há avaliações
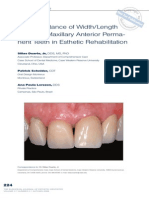
- The Importance of Width and Length Ratios in Anterior Pemanent Dentition PDFDocumento11 páginasThe Importance of Width and Length Ratios in Anterior Pemanent Dentition PDFEddy Mazariegos100% (1)
- Essentials of Orthognathic Surgery, 2nd Edition: Book ReviewsDocumento1 páginaEssentials of Orthognathic Surgery, 2nd Edition: Book ReviewsPae Anusorn AmtanonAinda não há avaliações
- Armamentarium FOR Basic Oral Surgery: Deepthi P.R. Intern Dept. of Oral SurgeryDocumento140 páginasArmamentarium FOR Basic Oral Surgery: Deepthi P.R. Intern Dept. of Oral SurgeryGabriela Cocieru MotelicaAinda não há avaliações
- Prosthetic Complication of Dental ImplantsDocumento42 páginasProsthetic Complication of Dental ImplantsDr. Abdulsalam Awas Dental Center0% (1)
- Evaluation and Management of Orofacial PainDocumento7 páginasEvaluation and Management of Orofacial PainLisbethOrtegaAinda não há avaliações
- MC - Seven Signs and Symptoms of Occlusal DiseaseDocumento5 páginasMC - Seven Signs and Symptoms of Occlusal DiseaseMuchlis Fauzi E100% (1)
- Dental Anatomy Slides Part 3 PDFDocumento27 páginasDental Anatomy Slides Part 3 PDFSinan A. ShwailiyaAinda não há avaliações
- Davis Nicholas C. An Artistic Approach To Smile Design.Documento24 páginasDavis Nicholas C. An Artistic Approach To Smile Design.Trần Thị Như Ngọc100% (1)
- 3 - D CephalometricDocumento68 páginas3 - D CephalometricMu'taz ArmanAinda não há avaliações
- Hand Surgery Trauma OrthoDocumento59 páginasHand Surgery Trauma OrthoFiki A RisentaAinda não há avaliações
- GolDen ProportIon in ProsthoDontICs Part-1Documento6 páginasGolDen ProportIon in ProsthoDontICs Part-1Jonathan Jaramillo100% (2)
- Bopt PanizDocumento9 páginasBopt PanizIvan CarreraAinda não há avaliações
- Resin Modified Glass Ionomer Cement: The Holy Grail of Cements?Documento3 páginasResin Modified Glass Ionomer Cement: The Holy Grail of Cements?DentalLearningAinda não há avaliações
- Freehand Vs Guided Implant Surgery ResearchDocumento4 páginasFreehand Vs Guided Implant Surgery ResearchSandeep Kumar SenguptaAinda não há avaliações
- Step by Step Root Canal TreatmentDocumento157 páginasStep by Step Root Canal TreatmentconchaasimoesAinda não há avaliações
- Biomechanics in Lingual Orthodontics What The Fut - 2018 - Seminars in Orthodon PDFDocumento9 páginasBiomechanics in Lingual Orthodontics What The Fut - 2018 - Seminars in Orthodon PDFOmy J. CruzAinda não há avaliações
- Orthodontic Pearls PDFDocumento2 páginasOrthodontic Pearls PDFortho123Ainda não há avaliações
- Atypical Extractions-Oral Surgery / Orthodontic Courses by Indian Dental AcademyDocumento36 páginasAtypical Extractions-Oral Surgery / Orthodontic Courses by Indian Dental Academyindian dental academyAinda não há avaliações
- Kelly and Kay HallDocumento7 páginasKelly and Kay HallSatyendra KumarAinda não há avaliações
- Wettability of Some Dental MaterialsDocumento5 páginasWettability of Some Dental MaterialsSatya AsatyaAinda não há avaliações
- Diagnosis in Implant TreatmentDocumento8 páginasDiagnosis in Implant TreatmentEduardo AyubAinda não há avaliações
- Manuscript of Case Report On Amelogenesis ImperfectaDocumento12 páginasManuscript of Case Report On Amelogenesis ImperfectaIndrani DasAinda não há avaliações
- The Z-Plasty Technique On The Frenectomy ApproachDocumento5 páginasThe Z-Plasty Technique On The Frenectomy ApproachVineet ArunAinda não há avaliações
- Development of The MaxillaDocumento7 páginasDevelopment of The MaxillaShinta Syafe'iAinda não há avaliações
- SD RPD DiscussionDocumento4 páginasSD RPD DiscussionRona TabingAinda não há avaliações
- Functional Assessment of Removable Complete Dentures: Riginal RticleDocumento3 páginasFunctional Assessment of Removable Complete Dentures: Riginal Rticlelaur112233Ainda não há avaliações
- DR - Ritty Arouje Recent Question Paper FileDocumento118 páginasDR - Ritty Arouje Recent Question Paper Filemuneer024Ainda não há avaliações
- Application of Functional Orthodontic Appliances To Treatment of Mandibular Retrusion Syndrome PDFDocumento18 páginasApplication of Functional Orthodontic Appliances To Treatment of Mandibular Retrusion Syndrome PDFThu Trang Pham100% (1)
- Carta de Formas de Dientes GeneralDocumento16 páginasCarta de Formas de Dientes Generaldachu_64Ainda não há avaliações
- Pediatric Dentistry Thesis TopicsDocumento7 páginasPediatric Dentistry Thesis Topicsamandagraytulsa100% (2)
- DNH Pinning Program - 2021Documento3 páginasDNH Pinning Program - 2021Christina QuirosAinda não há avaliações
- of Morphology of Maxillary Permanent DentitionDocumento77 páginasof Morphology of Maxillary Permanent DentitionashokAinda não há avaliações
- Dent 596 - OrthodonticsDocumento6 páginasDent 596 - OrthodonticsAndrei JardanAinda não há avaliações
- Amelogenesis ImperfectaDocumento46 páginasAmelogenesis Imperfectapinky parulAinda não há avaliações
- Landmarks For Maxilla and MandibleDocumento25 páginasLandmarks For Maxilla and Mandibleوجيه الوجيهAinda não há avaliações
- Free DTRBN Professional Exam Past QuestionsDocumento5 páginasFree DTRBN Professional Exam Past QuestionsCharles Obaleagbon75% (4)
- Max Arch Distalization Tads'Documento9 páginasMax Arch Distalization Tads'Rohini TondaAinda não há avaliações
- Espertise Magazine 25Documento24 páginasEspertise Magazine 25BatmanAinda não há avaliações
- Face-Bow Transfer in Prosthodontics - A Systematic Review of The - LiteratureDocumento7 páginasFace-Bow Transfer in Prosthodontics - A Systematic Review of The - LiteratureCaioSelaimenAinda não há avaliações
- 2 Treatment of Pulpitis With Biological, Vital Amputational and Extirpation Methods-1Documento107 páginas2 Treatment of Pulpitis With Biological, Vital Amputational and Extirpation Methods-1Bikku Negi100% (1)
- Flolis Propolis Fluoride - DRG ANGKY - UIDocumento18 páginasFlolis Propolis Fluoride - DRG ANGKY - UIDevin HendrawanAinda não há avaliações
- 008 Uk Geoff Knight Riva Star v2 1Documento2 páginas008 Uk Geoff Knight Riva Star v2 1api-240710651Ainda não há avaliações