Escolar Documentos
Profissional Documentos
Cultura Documentos
Costa Rica
Enviado por
api-337713711Título original
Direitos autorais
Formatos disponíveis
Compartilhar este documento
Compartilhar ou incorporar documento
Você considera este documento útil?
Este conteúdo é inapropriado?
Denunciar este documentoDireitos autorais:
Formatos disponíveis
Costa Rica
Enviado por
api-337713711Direitos autorais:
Formatos disponíveis
Absorbent Products and Skin Integrity in the Adult Incontinent Population
Paloma Garcia Duran, Sury Hacker, Sophia Jones, Amanda Mudge, and Kelsey Tolar
Sam Houston State University School of Nursing
Clinical Question
What are the effects of incontinence and the use of absorbent
products on skin integrity of patients in an inpatient setting?
Literature Review
Urinary incontinence increases with age and affects 46% to 72% nursing
home residents (Shigeta et al., 2010).
56 to 67 % of nursing home residents with urinary incontinence use
absorbent products, such as pads and briefs, as a urinary collection
strategy (Shigeta et al., 2010).
Skin damage, such as incontinence-associated dermatitis (IAD) and
pressure ulcers, is a common complication of pad use (Shigeta et al.,
2010).
Due to the decreasing cell replacement rates that occur with age, elderly
people have thinner skin, which increases the risk for skin breakdown
(Shigeta et al., 2010).
The prevalence rates of IAD varies between 5-50%, while the
prevalence of IAD and simultaneous use of diaper and absorbent pads is
prevalent in a 17% of the Japanese older patients with incontinence
(Sugama et al., 2012).
The cost of treating pressure ulcers is more than $10 billion per year to
Medicare, Medicaid, private insurance, and patients (Twersky et al.,
2012).
Method
Systematic Reviews,
Meta-Analysis, EBP
Guidelines
Randomized
Controlled
Trials
Controlled Trials
without
Randomization
Strong Evidence
Weak Evidence
Shigeta et al. (2010). Factors Influencing Intact Skin in
Women with Incontinence Using Absorbent Products:
Results of a Cross-sectional, Comparative Study.
controlled trial without randomization, fourth level of
hierarchy.
Sugama et al. (2012). Efficacy of an improved absorbent
pad on an incontinence-associated dermatitis in older
women: cluster randomized controlled trial.
Twersky et al. (2012). A Randomized, Controlled Study to
Assess the Effect of Silk-like Textiles and High-absorbency
Adult Incontinence Briefs on Pressure Ulcer Prevention.
Evaluation
Skin hydration and pH were significantly higher in the dual incontinent group
(both urine and feces) compared to only fecal incontinent group (Shigeta et al.,
2010).
Absorbent pad surface pH and excessive sweating were significantly related to
skin pH, and that a relationship between pad environment and skin integrity
was present (Shigeta et al., 2010).
The experimental group that received the new more absorbent pad, which
incorporates frontal absorption and a backflow prevention mechanism,
recovered from IAD significantly quicker than the control group (Sugama et
al., 2012).
Moisture content of the stratum corneum, nor skin pH, was significantly
different among the groups being compared on Sugama et al. (2012) study.
The number of adverse events between the experimental group receiving silklike linens and the control group was not significantly different, meaning that
silk-like linens did not increase the risk for falls (Twersky et al., 2012).
The experimental group using silk-like textiles and higher absorbent pads
developed less facility-acquired pressure ulcers than the control group
(Twersky et al., 2012).
More research is necessary because of several limitations of the studies.
Shigeta et al. (2010) studys limitations: (a) researchers fail to provide
methodological details and proof of reliability, (b) the sample size is
unclear and inadequate, (c) the perineal care method of the facility is not
evaluated nor considered as an extraneous variable, (d) the study only
focused on the effect of one type and brand of adult diapers, and (e) the
researchers excluded men from the study which limits the generalizability
of the study.
Sugama et al. (2012) studys limitations: (a) the lack of enough
experimental diapers for the study, and (b) interaction of treatment and
setting, due to the specific frequency, procedures, and skin care routines
determined by the care standards of the Japanese facility where the study
was taking place.
Twersky et al. (2012) studys limitations: (a) conflict of interest due to the
involvement and financial backing of the companies that produce the new
textile being analyzed, (b) lack of information to determine that the
instruments were valid and reliable to collect the data, and (c) the length of
the study, (d) the difference in the washing process between the control
and experimental textiles, (e) the lack of sampling randomization, (f) only
men participated in the study when target population were all residents of
the facility that served as platform for the study, and (g) the lack of
information regarding how perineal care was performed in the facility.
Decision about Practice
Cohort Studies or Case
Control Studies
Evidence from Systematic
Reviews of Descriptive and
Qualitative Studies
Evidence from the Opinion of
Authorities and/or Reports of Expert
Committees
Synthesis of Findings
randomized controlled trial, fifth level of hierarchy.
randomized controlled trial, fifth level of hierarchy.
Based on the research and strength of evidence, our clinical recommendation
is the use of silk-like textiles and highly absorbent products to protect the skin
integrity of the older incontinent adult population.
Closer assessment and monitoring of skin integrity in incontinent adult
population is recommended as a way to early detect the development of skin
breakdown.
Discussion
Many factors may contribute to a patient developing skin damage,
including the type of material of which the absorbent product is made,
cleansing techniques, frequency of changing briefs, skin pH, and excessive
sweating. These factors have to be taken into consideration in future
studies.
Researchers need to develop their studies carefully, which includes
evaluating the type of design, variables, population, and unpredictable
events.
More studies are necessary to develop EBP guidelines and such studies
should include participants from both genders.
References
Schmidt, N. A., & Brown, J. M. (2015). Evidence-based practice for nurses: Appraisal and application of
research (3rd ed). Sudbury, MA: Jones & Bartlett.
Shigeta, Y., Nakagami, G., Sanada, H., Konya, C., & Sugama, J. (2010). Factors influencing intact skin in
women with incontinence using absorbent products: Results of a cross-sectional, comparative study. Ostomy
Wound Management, 56(12), 26, 1-14. Retrieved from http://www.o-wm.com.ezproxy.shsu.edu/content/crosssectional-comparative-study-factors-influencing-intact-skin-women-incontinence
Sugama, J., Sanada, H., Shigeta, Y., Nakagami, G., & Konya, C. (2012). Efficacy of an improved absorbent pad
on incontinence associated dermatitis in older women: Cluster randomized controlled trial. BMC Geriatrics,
12(22), 17. doi:10.1186/147123181222
Twersky, J., Montgomery, T., Sloane, R., Weiner, M., Doyle, S., Mathur, K., ... & Schmader, K. (2012). A
randomized, controlled study to assess the effect of silk-like textiles and high-absorbency adult incontinence
briefs on pressure ulcer prevention. Ostomy Wound Management, 58(12), 18-24. Retrieved from
http://www.owm.com.ezproxy.shsu.edu/article/randomized-controlled-study-assess-effect-silk-textiles-and-highabsorbency-adult-incontinen
Você também pode gostar
- The Yellow House: A Memoir (2019 National Book Award Winner)No EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Nota: 4 de 5 estrelas4/5 (98)
- 5 THDocumento2 páginas5 THapi-337713711Ainda não há avaliações
- CallistaroyDocumento10 páginasCallistaroyapi-337713711Ainda não há avaliações
- Researchappraisal2 g3 TWCDocumento16 páginasResearchappraisal2 g3 TWCapi-337713711Ainda não há avaliações
- PicotDocumento1 páginaPicotapi-337713711Ainda não há avaliações
- Final Version Scholarly PaperDocumento10 páginasFinal Version Scholarly Paperapi-337713711Ainda não há avaliações
- Running Head: Community of Trinity Health Assessment 1Documento40 páginasRunning Head: Community of Trinity Health Assessment 1api-337713711Ainda não há avaliações
- InhalantsDocumento1 páginaInhalantsapi-337713711Ainda não há avaliações
- 9 THDocumento2 páginas9 THapi-337713711Ainda não há avaliações
- Girl InterruptedDocumento17 páginasGirl Interruptedapi-337713711100% (1)
- 10 THDocumento1 página10 THapi-337713711Ainda não há avaliações
- 8 THDocumento1 página8 THapi-337713711Ainda não há avaliações
- Safety HuddleDocumento1 páginaSafety Huddleapi-337713711Ainda não há avaliações
- 7 THDocumento2 páginas7 THapi-337713711Ainda não há avaliações
- 4 THDocumento2 páginas4 THapi-337713711Ainda não há avaliações
- 5731Documento2 páginas5731api-3377137110% (1)
- 2 NDDocumento1 página2 NDapi-337713711Ainda não há avaliações
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeNo EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeNota: 4 de 5 estrelas4/5 (5794)
- The Little Book of Hygge: Danish Secrets to Happy LivingNo EverandThe Little Book of Hygge: Danish Secrets to Happy LivingNota: 3.5 de 5 estrelas3.5/5 (400)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureNo EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureNota: 4.5 de 5 estrelas4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryNo EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryNota: 3.5 de 5 estrelas3.5/5 (231)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceNo EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceNota: 4 de 5 estrelas4/5 (895)
- Team of Rivals: The Political Genius of Abraham LincolnNo EverandTeam of Rivals: The Political Genius of Abraham LincolnNota: 4.5 de 5 estrelas4.5/5 (234)
- Never Split the Difference: Negotiating As If Your Life Depended On ItNo EverandNever Split the Difference: Negotiating As If Your Life Depended On ItNota: 4.5 de 5 estrelas4.5/5 (838)
- The Emperor of All Maladies: A Biography of CancerNo EverandThe Emperor of All Maladies: A Biography of CancerNota: 4.5 de 5 estrelas4.5/5 (271)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaNo EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaNota: 4.5 de 5 estrelas4.5/5 (266)
- The Unwinding: An Inner History of the New AmericaNo EverandThe Unwinding: An Inner History of the New AmericaNota: 4 de 5 estrelas4/5 (45)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersNo EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersNota: 4.5 de 5 estrelas4.5/5 (345)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyNo EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyNota: 3.5 de 5 estrelas3.5/5 (2259)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreNo EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreNota: 4 de 5 estrelas4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)No EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Nota: 4.5 de 5 estrelas4.5/5 (121)
- Seminar HD-RSUD Sleman 2019Documento36 páginasSeminar HD-RSUD Sleman 2019herkamaya100% (1)
- Clpna Self-Assessment ToolDocumento9 páginasClpna Self-Assessment Toolapi-306022321Ainda não há avaliações
- 51 Worst Diseases and Conditions To Treat With Black Seed OilDocumento9 páginas51 Worst Diseases and Conditions To Treat With Black Seed Oilsyndicate_mauliAinda não há avaliações
- (Treatments That Work) Gail Steketee, Randy O. Frost - Compulsive Hoarding and Acquiring - Therapist Guide-Oxford University Press (2006)Documento237 páginas(Treatments That Work) Gail Steketee, Randy O. Frost - Compulsive Hoarding and Acquiring - Therapist Guide-Oxford University Press (2006)mdmonzurh1100% (2)
- Peter Pan Syndrome Is A DeepDocumento3 páginasPeter Pan Syndrome Is A DeeptucklertAinda não há avaliações
- Hydra FacialDocumento34 páginasHydra FacialDrAmit Gaba MdsAinda não há avaliações
- Bio Medical Waste Management PPT 25-06-2019Documento47 páginasBio Medical Waste Management PPT 25-06-2019Dark InvaderAinda não há avaliações
- 2212-02e TPB PAC Liquid 10Documento1 página2212-02e TPB PAC Liquid 10Saefuddin SaefuddinAinda não há avaliações
- Health Teaching PlanDocumento3 páginasHealth Teaching PlanditamandaAinda não há avaliações
- Med-Fit 3: Instruction Manual Betriebsanleitung Manuel D'instructionDocumento52 páginasMed-Fit 3: Instruction Manual Betriebsanleitung Manuel D'instructionCarlos ParraAinda não há avaliações
- Bird FluDocumento3 páginasBird FludocspaAinda não há avaliações
- Introduction To Environmental EngineeringDocumento41 páginasIntroduction To Environmental EngineeringPaul Santos NonatAinda não há avaliações
- Aba Report Multiple BaselineDocumento25 páginasAba Report Multiple BaselinejAinda não há avaliações
- A2 Edexcel Psychology Module 4 Unit 3 Clinical PsychologyDocumento32 páginasA2 Edexcel Psychology Module 4 Unit 3 Clinical PsychologyAyse KerimAinda não há avaliações
- Balut Bidai: (Luthfi Fauzy Asriyanto)Documento63 páginasBalut Bidai: (Luthfi Fauzy Asriyanto)DiahNiatiAinda não há avaliações
- The Effect of Pilates Based Exercise On Mobility, Postural Stability, and Balance in Order To Decrease Fall Risk in Older AdultsDocumento7 páginasThe Effect of Pilates Based Exercise On Mobility, Postural Stability, and Balance in Order To Decrease Fall Risk in Older AdultsMuhammad Cholid AlfahroziAinda não há avaliações
- Sediment Exercise Manual Lymphatic Drainage Massage PDFDocumento5 páginasSediment Exercise Manual Lymphatic Drainage Massage PDF1712013Ainda não há avaliações
- Paul Holmes, Steve Farnfield - The Routledge Handbook of Attachment - Implications and Interventions-Routledge (2014)Documento205 páginasPaul Holmes, Steve Farnfield - The Routledge Handbook of Attachment - Implications and Interventions-Routledge (2014)Pamela Fontánez100% (4)
- Small Animal Clinical NutritionDocumento15 páginasSmall Animal Clinical NutritionJairo Pereira100% (1)
- ENLS V4.0 ME Manuscript FINALDocumento17 páginasENLS V4.0 ME Manuscript FINALkoko komarudinAinda não há avaliações
- Assessment Diagnosis Outcomes Interventions Rationale Expected OutcomeDocumento1 páginaAssessment Diagnosis Outcomes Interventions Rationale Expected OutcomeMatelyn OargaAinda não há avaliações
- Presentasi Pit Perbani 2000Documento16 páginasPresentasi Pit Perbani 2000Meta ParamitaAinda não há avaliações
- Erbe Apc 300 User ManualDocumento108 páginasErbe Apc 300 User ManualDavid HernandezAinda não há avaliações
- Health, Education, Social Protection News & Notes 25/2011Documento32 páginasHealth, Education, Social Protection News & Notes 25/2011Dieter NeuviansAinda não há avaliações
- NURSING CARE PLAN OcdDocumento25 páginasNURSING CARE PLAN Ocdkiran mahal81% (26)
- Stroke Pathophysiology 1Documento5 páginasStroke Pathophysiology 1Jeco ValdezAinda não há avaliações
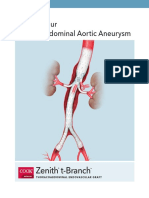
- Zenith T-Branch Patient GuideDocumento20 páginasZenith T-Branch Patient Guidedarkmatter1Ainda não há avaliações
- West Visayas State University Medical Center E. Lopez St. Jaro Iloilo CityDocumento7 páginasWest Visayas State University Medical Center E. Lopez St. Jaro Iloilo CityRegine Marie EspañaAinda não há avaliações
- Action Plan For Rejuvenation of River Tunga 1Documento11 páginasAction Plan For Rejuvenation of River Tunga 1anitha_mathanAinda não há avaliações
- Dewitt 2007Documento6 páginasDewitt 2007Bagus Putra KurniawanAinda não há avaliações