Escolar Documentos
Profissional Documentos
Cultura Documentos
Nefropathy Contras
Enviado por
balthier37Direitos autorais
Formatos disponíveis
Compartilhar este documento
Compartilhar ou incorporar documento
Você considera este documento útil?
Este conteúdo é inapropriado?
Denunciar este documentoDireitos autorais:
Formatos disponíveis
Nefropathy Contras
Enviado por
balthier37Direitos autorais:
Formatos disponíveis
N-Acetylcysteine in the Prevention of Contrast-Induced
Nephropathy
Steven Fishbane
Winthrop-University Hospital, Mineola, New York, and State University of New York School of Medicine, Stony
Brook, New York
Background and objectives: Contrast-induced nephropathy (CIN) is a common clinical problem that is growing in importance
as an increasing number of tests and procedures that utilize contrast media are performed.
Design, setting, participants, and measurements: The biological and pharmacological properties of n-acetylcysteine (NAC)
are reviewed, as well as the current literature relevant to the ability of NAC to prevent CIN.
Results: After publication of a seminal study by Tepel et al. in 2000, there has been a surge in interest regarding the ability
of NAC to reduce the risk for CIN. Since then a large number of studies, mostly with relatively small sample sizes, have been
published.
Conclusions: The results have been remarkably varied with some studies finding great efficacy with NAC but most finding
no significant benefit.
Clin J Am Soc Nephrol 3: 281287, 2008. doi: 10.2215/CJN.02590607
ontrast-induced nephropathy (CIN) is most precisely
defined as an acute deterioration in renal function
after exposure to, and as a result of, contrast media
(CM). In actuality, however, acute renal failure (ARF) occurring
after procedures associated with contrast administration may
be caused by several different factors including volume depletion, atheroembolic disease, congestive heart failure, and a
functional increase in serum creatinine (SCr) after preprocedure
hydration. Because it is not always possible to clinically differentiate the cause of the renal dysfunction, it may be more
appropriate to term this condition contrast-associated nephropathy.
It is certain that different causes of contrast-associated renal
dysfunction require different preventive strategies. Prevention
of renal failure that is truly caused by contrast requires interventions based on our knowledge of the pathophysiology of
this disorder. Consequences of exposure to CM may include
renal vasoconstriction and redistributed blood flow (1 6), tubular epithelial cell toxicity (disruption of cell integrity, oxygen
radical generation, and apoptosis (713), intratubular obstruction, and hemoglobin oxygen saturation curve shifts. A variety
of therapeutic agents aimed at ameliorating these changes have
been studied. This article discusses one specific agent, n-acetylcysteine (NAC).
Published online ahead of print. Publication date available at www.cjasn.org.
Correspondence: Dr. Steven Fishbane, 200 Old Country Road, #135, Mineola, NY
11501. Phone: 516-663-2169; Fax: 516-663-2179; E-mail: sfishbane@winthrop.org
Copyright 2008 by the American Society of Nephrology
N-Acetylcysteine
NACs primary use in clinical medicine has been as a mucolytic
agent, where inhalation leads to splitting of disulfide linkages
between the glycopeptides in mucus and loosening of obstructive plugs (14,15). In addition, NAC plays an important role in
the treatment of acetaminophen overdose, where administration of large doses results in improved outcomes (16 18). Hepatic metabolism of acetaminophen results in production of
N-acetyl benzoquinoneimine, which depletes cellular glutathione stores, leaving the liver vulnerable to oxidative injury
(19,20). Administration of NAC provides cysteine as a substrate
to replenish glutathione stores and reduce hepatic damage
(21,22).
Pharmacology
N-acetylcysteine is an acetylated derivative of the amino acid
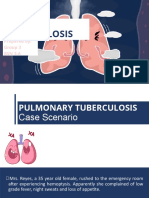
cysteine. The chemical formula is C5H9NO3S, and the molecular mass is 163.2 g/mol (Figure 1). The drug can be administered via oral, intravenous, or respiratory routes. Early studies
of NAC pharmacology were hindered by the complexity of the
analysis. The problem is caused by the drugs highly reactive
sulfhydryl group, which rapidly binds to and reacts with
plasma and tissue proteins, forming disulfide linkages, with
oxidation of the drug (23). The drug may circulate free in
plasma or may become associated with other proteins in a wide
variety of forms (24). Analytic systems testing the concentration
of NAC in plasma must be able to differentiate between reduced and oxidized NAC as well as free and bound NAC
found in proteinaceous complexes in the sample.
Older studies reported NAC to have a plasma half-life of
several hours, but with modern techniques the bioavailability
ISSN: 1555-9041/3010281
282
Clinical Journal of the American Society of Nephrology
Figure 1. Structure of N-acetylcysteine.
has been found to be poor and the actual half-life closer to 6 to
40 min. After oral administration, Moldeus and Cotgreave were
able to detect only very small quantities of oxidized drug in
circulation, with no free drug detectable (23). Bioavailability
was 5%, probably because of extensive first-pass hepatic metabolism. Numerous other investigators have confirmed the
low bioavailability of oral NAC including slow-release preparations (2528). After intravenous injection, Harada et al. found
that NAC was highly bound to plasma and tissue proteins,
forming various disulfide compounds. Only small amounts of
NAC were found in circulation despite the intravenous route of
administration (29). It is clear from these reports that, after oral
administration, NAC is almost completely metabolized before
entering the systemic circulation. When considering the mechanism by which NAC can have a potential benefit in preventing
CIN, its poor bioavailability must somehow be reconciled.
The poor bioavailability of NAC after oral dosing is the result
of extensive first-pass metabolism. With intestinal transit and
absorption, NAC is effectively deacetylated by the enzyme
acylase I in the intestines and liver (30 35). The resulting free
amino acid cysteine has a highly reactive sulfhydryl group that
readily reacts with plasma and tissue proteins yielding a variety of sulfur-containing molecules and compounds. In rats, the
major metabolites entering the circulation include cysteine, cystine, inorganic sulfites, homodisulfides of NAC, and labile disulfide protein complexes (34,36). In the circulation of the portal
vein, the deacetylation of NAC is so efficient that the concentration of metabolites is 300% to 500% higher than that of NAC
(34). The liberated cysteine molecules can be used by cells as
precursors for glutathione production.
Biological Actions of NAC
The pharmacology of NAC, particularly its deacetylation and
poor bioavailability, make clear that the drugs in vitro effects
must be considered separately from its in vivo actions. The
beneficial therapeutic effects of NAC may well be a result of
indirect effects such as induction of glutathione synthesis. NAC
has a variety of biological actions. The following discussion will
highlight those most relevant to the pathogenesis of CIN.
The antioxidant properties of NAC have been studied exten-
Clin J Am Soc Nephrol 3: 281287, 2008
sively. Bursts of oxidative stress occur naturally, and the bodys
cells and tissues possess antioxidant systems to protect against
oxidative damage (37). After exposure to CM there is a surge in
oxidative stress that may overwhelm these systems and result
in tissue injury (38). The most plausible mechanism of NACs
putative protective effect against CIN is supplementation of the
bodys antioxidant capacity.
NAC is very effective in neutralizing certain free radicals in
vitro. The drug reacts with and deactivates hydroxyl radicals
(39,40); the reaction is rapid, with a rate constant of 1.36 1010
M1sec1, yielding NAC thiol radical intermediates and ultimately NAC disulfide (39). Regarding other reactive oxygen
species, such as superoxide anion and hydrogen peroxide,
NAC is a somewhat less effective antioxidant (40).
Because NAC is extensively degraded in vivo (as discussed
above), it is likely that any antioxidant effects it exerts in
humans would be indirect. For example, NAC might work by
inducing glutathione synthesis. Glutathione plays a central role
in the bodys defense against cellular oxidative damage (41,42).
It generally cannot enter cells; instead it must be synthesized
intracellularly from glycine, glutamate, and cysteine. Cysteine
is the moiety that supplies glutathiones active sulfhydryl
group and plays a critical role as the rate-limiting factor in
glutathione synthesis. After deacetylation in the intestines and
liver, NAC yields cysteine as one of its metabolites. This circulating cysteine may enter renal cells and serve as a precursor for
glutathione production. In fact, several studies have found that
NAC prevents glutathione depletion (43,44). The relevance for
the kidney is suggested by the demonstration of glutathione
depletion in ischemia reperfusion injury (46,47). In rats, administration of NAC has been found to increase renal glutathione
levels (48).
In addition to its antioxidant properties, NAC has other
biological actions that might be helpful for preventing CIN.
Vasoconstriction has often been considered as a factor contributing to the pathogenesis of CIN. By stabilizing nitric oxide,
NAC may have a vasodilatory effect in certain situations (49
51). In addition, NACs sulfhydryl group may inhibit angiotensin-converting enzyme, reducing production of the vasoconstrictor angiotensin II (52). The vasoconstriction in CIN may be
somewhat selective, particularly affecting the kidneys medullary circulation (53). In a study of ARF induced by inferior vena
cava obstruction, a model with reduced medullary blood flow,
Conesa et al. found that NAC reduced medullary vasoconstriction and improved blood flow (54). Heyman and colleagues
(55) found that NAC administration in rats resulted in reduced
total, cortical, and medullary vascular resistance by 7% to 10%.
Another recently demonstrated action of NAC is in reducing
urinary albumin excretion (56).
Clinical Studies of NAC in the Prevention of
CIN
The salutary properties of NAC described in the previous section form the rationale for why NAC might be helpful in the
prevention of CIN. Tepel et al. published the first clinical study
on this subject in 2000 (57). Since that time there have been
many published studies with great heterogeneity in results,
Clin J Am Soc Nephrol 3: 281287, 2008
some finding substantial benefit for NAC, others reporting no
effect. Most of the studies included patient populations at relatively increased risk for CIN, generally defined by an increased baseline SCr. ARF developing after contrast exposure
has generally been defined as an increase in SCr of 0.5 mg/dl
or 25% above the baseline value. Studies generally did not
attempt to differentiate ARF induced by CM from other possible causes.
In Tepels seminal report, 83 patients undergoing contrastenhanced CT scanning were studied. Only subjects with SCr
1.2 mg/dl or creatinine clearance 50 ml/min were studied.
Randomization was followed by double-blind treatment with
either oral NAC 600 mg twice daily on the day before and the
day of the CT scan or with placebo. ARF, defined as an increase
in SCr of 0.5 mg/dl, occurred in 21% of placebo subjects
compared with 2% in the NAC group (P 0.01). This dramatic
reduction in risk with NAC drew great attention and led to an
almost immediate change in clinical practice (57).
Shortly after Tepels publication, our group attempted to
reproduce the finding in patients undergoing cardiac angiography. Subjects with SCr 1.7 mg/dl were randomized to
double-blind administration of placebo or NAC 1200 mg orally
with doses 1 h before the procedure and 3 h afterwards. ARF
was defined as an increase in SCr of 0.5 mg/dl. We found no
significant difference in the rate of CIN between the NAC and
placebo groups (26.3% versus 22.0%). The remarkable disparity
between our results and those of Tepel et al. presaged the
literature that has paralleled this pattern of great heterogeneity
of results (58).
Other Studies
There are 20 published studies investigating NAC for the
prevention of CIN, with 30 to 487 subjects enrolled in each
study. Studies with negative results outnumber those with
positive results by a 2-to-1 margin. However, the magnitude of
benefit in some of the positive studies was substantial. Studies
by Tepel et al., Shyu et al., Kay et al., and Diaz-Sandoval et al.
reported that NAC reduced the risk of CIN by 90.5%, 86.6%,
67.7%, and 82.2%, respectively (57,59 61). There are few areas
in clinical medicine where a treatment has demonstrated such
a dramatic magnitude of benefit. There are even fewer examples in which such a small number of studies found a substantial benefit, whereas most other studies found no benefit at all.
For this reason the literature on NAC has been so difficult to
interpret and synthesize into clinical treatment recommendations.
Most published studies have been underpowered to adequately test efficacy end points. In the largest published study,
by Webb et al., 487 patients with renal dysfunction were randomized to receive either placebo or NAC 500 mg intravenously before undergoing cardiac catheterization. The study
was terminated prematurely by the Data Safety Monitoring
Committee because of futility and the lack of any trend toward
benefit with NAC treatment (62). Because of the larger sample
size of this study compared with other NAC studies, the negative findings carry particular weight.
In contrast to Webbs findings is the recent publication of
NAC in the Prevention of CIN
283
Marenzi et al., which reports on 354 patients with myocardial
infarction undergoing coronary angiography with primary angioplasty (63). Patients were randomized to treatment with
placebo, a standard dose of NAC (600 mg by intravenous bolus
before primary angioplasty and 600 mg orally twice daily for
48 h after angioplasty), or a double dose of NAC (1200 mg by
intravenous bolus and 1200 mg orally twice daily for 48 h after
intervention). ARF was defined as a 25% increase in SCr level.
The risk for CIN was reduced by 54.5% in the standard-dose
NAC group and by 75.8% in the high-dose NAC group. This
gradient of effect was particularly impressive and not found in
prior studies. More remarkable, the risk for death was also
reduced by the use of NAC at both dosage strengths (63). The
most likely explanation for this find is that NAC may have had
a cardioprotective effect, as has been recently suggested (64).
However, this result would be strengthened by confirmation by
other investigators. It should be noted that intravenous NAC is
associated with a small risk for anaphylactoid reactions. The
findings of Marenzi et al. stand in stark contrast to the other
large study, that of Webb et al., and further add to the murkiness of the literature on NAC for prevention of CIN. Another
recent publication found benefit for the combination of NAC
with intravenous bicarbonate. Briguori and colleagues studied
patients with CKD undergoing coronary or peripheral vascular
procedures (65). Subjects were randomly assigned to administration of 0.9% saline infusion plus NAC (n 111), sodium
bicarbonate infusion plus NAC (n 108), or 0.9% saline plus
ascorbic acid plus NAC (n 107). An increase of 25% in serum
creatinine occurred in 9.9% in the saline plus NAC group,
compared with 1.9% in the bicarbonate plus NAC group (P
0.019) and 10.3% in the saline plus ascorbic acid plus NAC
group. The authors concluded that NAC was more effective
paired with bicarbonate compared with saline hydration (65).
Because most of the studies published on NAC for the prevention of CIN are quite small in size (even the studies of Webb
et al. and Marenzi et al. were not adequately powered to fully
evaluate the spectra of efficacy and safety), meta-analyses have
been performed to increase the probability of explaining the
full spectrum of utility for NAC. To date, 11 meta-analyses have
been published on this subject (66 76), seven of these reports
found a net benefit for NAC in the prevention of CIN. However, a recent review by Bagshaw et al. noted the marked
heterogeneity in study results; indeed 10 of the 11 meta-analyses found statistically significant heterogeneity to be present.
Bagshaw et al. cautioned that pooling of data to arrive at a
summary estimate for treatment efficacy should generally be
avoided in situations where the trials exhibit significant statistical and/or clinical heterogeneity (77). Because clinical heterogeneity has been an important feature of these studies, it is not
clear whether meta-analyses are a useful tool to clarify the role
of NAC.
Publication bias is an important issue to consider with respect to NAC. Vaitkus and Brar reported that this appears to be
a substantial problem, noting that, among abstracts presented
at scientific meetings, far fewer negative studies on NAC resulted in publications (78). Therefore, the results of meta-anal-
284
Clinical Journal of the American Society of Nephrology
yses probably reflect an overly optimistic view of NACs treatment efficacy.
NAC and Measurement of SCr
Because almost all studies of NAC in the prevention of CIN
defined ARF as a small increase in SCr, any interference by
NAC on measurement of SCr could be problematic. In 2001,
Izzedine et al. reported on in vitro testing of NAC with respect
to its effect on SCr determinations by adding NAC to samples
of human plasma to achieve different concentrations (79). Izzedine and coworkers estimated that plasma NAC levels
achieved in the study of Tepel et al. would probably have been
approximately 465 mg/L, and they tried to approximate this
concentration in vitro. They measured SCr using the modified
Jaffe method and found no analytic interference for SCr for
NAC concentrations of 102 to 600 mg/L. Only at very high
concentrations of NAC (50,000 mg/L), well above what would
occur after typical dosing, were SCr levels significantly affected, decreasing by 50% (79). Somewhat at odds with these
results, was the work of Hoffmann et al., who studied the effect
of NAC in vivo (80). Fifty volunteers with normal renal function
were given NAC 600 mg twice daily for 2 d. Cystatin C, used as
the assay for GFR, was unchanged, indicating that NAC had no
substantive effect on actual renal function. In contrast, SCr level
was significantly decreased. The magnitude of the change,
however, was quite small; a mean decrease in SCr at 4 h after
dosing from 0.85 0.14 mg/dl to 0.82 0.13 mg/dl (P 0.05).
Even at 2 SD below the mean (2.5% of patients), the reduction
in SCr would have been only 0.29 mg/dl (80). These results
indicate that although NAC may have a small effect on measurement of SCr, it is probably not large enough to diminish the
value of SCr as a study end point.
Clin J Am Soc Nephrol 3: 281287, 2008
understanding would help in the design of future agents as
well as help better guide dose timing, route of administration,
and other aspects of treatment. In particular, there remains
controversy about whether the oral or intravenous route of
administration of NAC is preferred. Because the efficacy of
NAC has not been completely established, research on newer
agents must continue to be encouraged.
Treatment Recommendations
The only well established treatment for the prevention of CIN
is intravenous hydration. With the remarkable heterogeneity in
study results, it is difficult to determine whether NAC is truly
effective in preventing CIN. Until a well-powered definitive
study is performed, use of NAC in higher-risk patients undergoing CM-enhanced procedures is probably reasonable. The
drug is inexpensive, safe, and well tolerated by patients. The
oral route of administration is probably acceptable as it is less
expensive and avoids the minor risk for anaphylaxis. However,
the decision to perform CM-enhanced tests and procedures on
high-risk patients requires a careful balancing of risk and benefit. The availability of NAC should not sway these decisions
since its efficacy is not clearly established. Contrast-enhanced
tests and procedures should be avoided, if possible, in high-risk
patients when alternative tests are available.
When NAC is to be used, the original Tepel dose should be
used (600 mg twice daily on the day before and the day of
exposure to contrast). Alternatively, a higher dose may be
given only on the day of the procedure. The intravenous route
of administration is reasonable when oral treatment is not
possible. In addition to NAC, intravenous hydration should be
used where clinically appropriate.
Disclosures
Research Directions
The published literature on NAC in the prevention of CIN is
composed of many studies, although almost all are inadequately powered. The primary end point used in these studies
has always been a relatively small increase in SCr. It is unclear
the extent to which this is a reasonable surrogate for higherlevel outcomes such as need for dialysis, extended hospital
stays, or death. Moreover, the small magnitude of change in
SCr used to define CIN increases the vulnerability of this outcome measure, requiring larger sample sizes. This factor is
probably responsible for much of the heterogeneity in study
results.
At this point in time, no additional underpowered studies
should be performed as they will have no impact on clinical
practice, meta-analyses, or practice guidelines. A large, wellpowered, preferably multicenter study is needed to clarify the
current murky literature and determine the true utility of NAC.
Clinically relevant high-level outcomes should be used.
Additional areas for research include explorations of NACs
mechanism of action in CIN and further studies on the pathobiology of CIN. Without a more complete understanding of the
pathogenesis of CIN, selection of new candidate drugs will
remain somewhat arbitrary. Although NAC shows promise, its
mechanism of action has not been fully elucidated. A better
None.
References
1. Arend LJ, Bakris GL, Burnett JC, Mergerian C, Spielman
WS: Role for intrarenal adenosine in the renal hemodynamic response to contrast media. J Lab Clin Med 110:
406 411, 1987
2. Katzberg RW, Schulman G, Meggs LG, Caldicot WJH,
Damieno MM, Hollenberg NK: Mechanism of renal response to contrast medium in dogs: Decrease in renal
function due to hypertonicity. Invest Radiol 18: 74 80, 1983
3. Larson JS, Hudson K, Mertz JI, Romero JC, Knox FG: Renal
vasoconstrictive response to contrast medium: The role of
sodium balance and the renin-angiotensin system. J Lab
Clin Med 101: 385391, 1983
4. Schick CS, Haller C: Comparative cytotoxicity of ionic and
non-ionic radiocontrast agents on MDCK cell monolayers
in vitro. Nephrol Dial Transplant 14: 342347, 1999
5. Talner LB, Davidson AJ: Renal hemodynamic effects of
contrast media. Invest Radiol 3: 310 317, 1968
6. Nygren A: Contrast media and regional renal blood flow:
A study of the effects of ionic and non-ionic monomeric
and dimeric contrast media in the rat. Acta Radiol 378:
123135, 1992
7. Humes HD, Hunt DA, White MD: Direct toxic effect of the
Clin J Am Soc Nephrol 3: 281287, 2008
8.
9.
10.
11.
12.
13.
14.
15.
16.
17.
18.
19.
20.
21.
22.
23.
24.
25.
26.
radiocontrast agent diatrizoate on renal proximal tubule
cells. Am J Physiol 252: F246 F255, 1987
Messana JM, Cieslinski DA, Nguyen VD, Humes HD:
Comparison of the toxicity of the radiocontrast agents,
iopamidol and diatrizoate, to rabbit renal proximal tubule
cells in vitro. J Pharmacol Exp Ther 244: 1139 1144, 1988
Bakris GL, Lass N, Gaber AO, Jones JD, Burnett JC Jr:
Radiocontrast medium-induced declines in renal function:
A role for oxygen free radicals. Am J Physiol 258: F115
F120, 1990
Yoshioka T, Fogo A, Becman JK: Reduced activity of antioxidant enzymes underlies contrast media-induced renal
injury in volume depletion. Kidney Int 41: 1008 1015, 1992
Parvez Z, Rahman Ma, Moncada R: Contrast media-induced renal injury in volume depletion. Invest Radiol 24:
697702, 1989
Zager RA, Johnson AC, Hanson SY: Radiographic contrast
media-induced tubular injury: Evaluation of oxidant stress
and plasma membrane integrity. Kidney Int 64: 128 139,
2003
Beeri R, Symon Z, Brezis M, Ben-Sasson SA, Baehr PH,
Rosen S, Zager RA: Rapid DNA fragmentation from hypoxia along the thick ascending limb of rat kidneys. Kid Int
47: 1806 1810, 1995
Lieberman J: The appropriate use of mucolytic agents. Am J
Med 49: 1 4, 1970
Sheffner AL: The mucolytic action of acetylcysteine. Tuberculol Thorac Dis 23: 3133, 1966
Prescott LF, Illingworth RN, Critchley JA, Stewart MJ,
Adam RD, Proudfoot AT: Intravenous N-acetylcystine:
The treatment of choice for paracetamol poisoning. BMJ 2:
10971100, 1979
Yip L, Dart RC: A 20-hour treatment for acute acetaminophen overdose. N Engl J Med 348: 24712472, 2003
Breen KJ, Bury RW, Desmond PV, Forge BH, Mashford
ML, Whelan G: Paracetamol self-poisoning: diagnosis,
management, and outcome. Med J Aust 1: 7779, 1982
Dahlin DC, Nelson SD: Synthesis, decomposition kinetics,
and preliminary toxicological studies of pure N-acetyl-pbenzoquinone imine, a proposed toxic metabolite of acetaminophen. J Med Chem 25: 885 886, 1982
Mitchell JR, Jollow DJ, Potter WZ, Gillette JR, Brody BB:
Acetaminophen-induced hepatic necrosis. IV. Protective
role of glutathione. J Pharmacol Exp Ther 187: 211217, 1973
Lauterburg BH, Corcoran GB, Mitchell JR: Mechanism of
action of N-acetylcysteine in the protection against the
hepatotoxicity of acetaminophen in rats in vivo. J Clin
Invest 71: 980 991, 1983
Corcoran GB, Wong BK: Role of glutathione in prevention
of acetaminophen-induced hepatotoxicity by N-acetyl-Lcysteine in vivo: Studies with N-acetyl-D-cysteine in mice.
J Pharmacol Exp Ther 238: 54 61, 1986
Moldeus P, Cotgreave IA: N-acetylcysteine. Methods Enzymol 234: 482 492, 1994
Harada D, Naito S, Hiraoka I, Otagiri M: In vivo kinetic
analysis of covalent binding between N-acetyl-L-cysteine
and plasma protein through the formation of mixed disulfide in rats. Pharm Res 19: 615 620, 2002
Olsson B, Johansson M, Gabrielsson J, Bolme P: Pharmacokinetics and bioavailability of reduced and oxidized
N-acetylcysteine. Eur J Clin Pharmacol 34: 77 82, 1988
Borgstrom L, Kagedal B, Paulsen O: Pharmacokinetics of
NAC in the Prevention of CIN
27.
28.
29.
30.
31.
32.
33.
34.
35.
36.
37.
38.
39.
40.
41.
285
N-acetylcysteine in man. Eur J Clin Pharmacol 31: 217222,
1986
Bridgeman MM, Marsden M, MacNee W, Flenley DC, Ryle
AP: Cysteine and glutathione concentrations in plasma
and bronchoalveolar lavage fluid after treatment with
N-acetylcysteine. Thorax 46: 39 42, 1991
Tsikas D, Sandmann J, Ikic M, Fauler J, Stichtenoth DO,
Frolich JC: Analysis of cysteine and N-acetylcysteine in
human plasma by high-performance liquid chromatography at the basal state and after oral administration of
N-acetylcysteine. J Chromatogr B Biomed Sci Appl 708: 55
60, 1998
Harada D, Naito S, Kawauchi Y, Ishikawa K, Koshitani O,
Hiraoka I, Otagiri M: Determination of reduced, proteinunbound, and total concentrations of N-acetyl-L-cysteine
and L-cysteine in rat plasma by postcolumn ligand substitution high-performance liquid chromatography. Anal Biochem 290: 251259, 2001
Thor H, Moldeus P, Orrenius S: Metabolic activation and
hepatotoxicity. Effect of cysteine, N-acetylcysteine, and
methionine on glutathione biosynthesis and bromobenzene toxicity in isolated rat hepatocytes. Arch Biochem Biophys 192: 405 413, 1979
Sjodin K, Nilsson E, Hallberg A, Tunek A: Metabolism of
N-acetyl-L-cysteine. Some structural requirements for the
deacetylation and consequences for the oral bioavailability.
Biochem Pharmacol 38: 39813985, 1989
Uttamsingh V, Keller DA, Anders MW: Acylase I-catalyzed deacetylation of N-acetyl-L-cysteine and S-alkyl-Nacetyl-L-cysteines. Chem Res Toxicol 11: 800 809, 1998
Uttamsingh V, Baggs RB, Krenitsky DM, Anders MW:
Immunohistochemical localization of the acylases that catalyze the deacetylation of N-acetyl-L-cysteine and haloalkene-derived mercapturates. Drug Metab Dispos 28: 625 632,
2000
Cotgreave IA, Berggren M, Jones TW, Dawson J, Moldeus
P: Gastrointestinal metabolism of N-acetylcysteine in the
rat, including an assay for sulfite in biological systems.
Biopharm Drug Dispos 8: 377386, 1987
Sheffner AL: Metabolic studies with acetylcysteine. Biochem Pharmacol 15: 15231535, 1966
Burgunder JM, Varriale A, Lauterburg BH: Effect of N-acetylcysteine on plasma cysteine and glutathione following
paracetamol administration. Eur J Clin Pharmacol 36: 127
131, 1989
Cooke MS, Evans MD, Dizdaroglu M, Lunec J: Oxidative
DNA damage: Mechanisms, mutation, and disease. FASEB
J 17: 11951214, 2003
Bakris GL, Lass N, Gaber AO, Jones JD, Burnett JC Jr:
Radiocontrast medium-induced declines in renal function:
A role for oxygen free radicals. Am J Physiol 258: F115
F120, 1990
Aruoma OI, Halliwell B, Hoey BM, Butler J: The antioxidant action of N-acetylcysteine: Its reaction with hydrogen
peroxide, hydroxyl radical, superoxide, and hypochlorous
acid. Free Radic Biol Med 6: 593597, 1989
Harrison PM, Keays R, Bray GP, Alexander GJ, Williams R:
Improved outcome of paracetamol-induced fulminant hepatic failure by late administration of acetylcysteine. Lancet
335: 15721573, 1990
Reed DJ: Glutathione: Toxicological implications. Annu Rev
Pharmacol Toxicol 30: 603 631, 2990
286
Clinical Journal of the American Society of Nephrology
42. Shan XQ, Aw TY, Jones DP: Glutathione-dependent protection against oxidative injury. Pharmacol Ther 47: 6171,
1990
43. Skrzydlewska E, Farbiszewski R: Protective effect of N-acetylcysteine on reduced glutathione, reduced glutathionerelated enzymes and lipid peroxidation in methanol intoxication. Drug Alcohol Depend 57: 61 67, 1999
44. Nakano H, Boudjema K, Alexandre E, Imbs P, Chenard
MP, Wolf P, Cinqualbre J, Jaeck D: Protective effects of
N-acetylcysteine on hypothermic ischemia-reperfusion injury of rat liver. Hepatology 22: 539 545, 1995
45. Pastor A, Collado PS, Almar M, Gonzalez-Gallego J: Antioxidant enzyme status in biliary obstructed rats: effects of
N-acetylcysteine. J Hepatol 27: 363370, 1997
46. Sehirli AO, Sener G, Satiroglu H, Ayanoglu-Dulger G:
Protective effect of N-acetylcysteine on renal ischemia/
reperfusion injury in the rat. J Nephrol 16: 75 80, 1993
47. Paller MS: Renal work, glutathione and susceptibility to
free radical-mediated postischemic injury. Kidney Int 33:
843 849, 1988
48. Scaduto RC, Martin VH: Elevation of renal glutathione
enhances ischemic injury. Renal Physiol Biochem 14: 259
270, 1991
49. Salom MG, Ramirez P, Carbonell LF, Conesa EL, Cartagena J, Quesada T, Parrilla P, Fenoy FJ: Protective effect of
N-acetyl l-cysteine on the renal failure induced by inferior
vena cava occlusion. Transplantation 65: 13151321, 1998
50. Girouard H, Chulak C, Wu L, Lejossec M, de Champlain J:
N-acetylcysteine improves nitric oxide and alpha-adrenergic pathways in mesenteric beds of spontaneously hypertensive rats. Am J Hypertens 16: 577584, 2003
51. Loscalzo J: N-Acetylcysteine potentiates inhibition of platelet aggregation by nitroglycerin. J Clin Invest 76: 703708,
1985
52. Boesgaard S, Aldershvile J, Poulsen HE, Christensen S,
Dige-Petersen H, Giese J: N-acetylcysteine inhibits angiotensin converting enzyme in vivo. J Pharmacol Exp Ther 265:
1239 1244, 1993
53. Prasad PV, Priatna A, Spokes K, Epstein FH: Changes in
intrarenal oxygenation as evaluated by BOLD MRI in a rat
kidney model for radiocontrast nephropathy. J Magn Reson
Imaging 13: 744 747, 2001
54. Conesa EL, Valero F, Nadal JC, Fenoy FJ, Lopez B, Arregui
B, Salom MG: N-acetyl-L-cysteine improves renal medullary hypoperfusion in acute renal failure. Am J Physiol
Regul Integr Comp Physiol 281: R730 R737, 2001
55. Heyman SN, Goldfarb M, Shina A, Karmeli F, Rosen S:
N-acetylcysteine ameliorates renal microcirculation: Studies in rats. Kidney Int 63: 634 641, 2003
56. Levin A, Pate GE, Shalansky S, Al-Shamari A, Webb JG,
Buller CE, Humphries KH. N-acetylcysteine reduces urinary albumin excretion following contrast administration:
Evidence of biological effect. Nephrol Dial Transplant 22:
2520 2524, 2007
57. Tepel M, van der Giet M, Schwarzfeld C, Laufer U, Liermann D, Zidek W: Prevention of radiographic-contrastagent-induced reductions in renal function by acetylcysteine. N Engl J Med 343: 180 184, 2000
58. Durham JD, Caputo C, Dokko J, Zaharakis T, Pahlavan M,
Keltz J, Dutka P, Marzo K, Maesaka JK, Fishbane S: A
randomized controlled trial of N-acetylcysteine to prevent
Clin J Am Soc Nephrol 3: 281287, 2008
59.
60.
61.
62.
63.
64.
65.
66.
67.
68.
69.
70.
71.
72.
73.
contrast nephropathy in cardiac angiography. Kidney Int
62: 22022207, 2002
Shyu KG, Cheng JJ, Kuan P: Acetylcysteine protects
against acute renal damage in patients with abnormal renal
function undergoing a coronary procedure. J Am Coll Cardiol 40: 13831388, 2002
Kay J, Chow WH, Chan TM, Lo SK, Kwok OH, Yip A, Fan
K, Lee CH, Lam WF: Acetylcysteine for prevention of acute
deterioration of renal function following elective coronary
angiography and intervention: a randomized controlled
trial. JAMA 289: 553558, 2003
Diaz-Sandoval LJ, Kosowsky BD, Losordo DW: Acetylcysteine to prevent angiography-related renal tissue injury
(the APART trial). Am J Cardiol 89: 356 358, 2002
Webb JG, Pate GE, Humphries KH, Buller CE, Shalansky S,
Al Shamari A, Sutander A, Williams T, Fox RS, Levin A: A
randomized controlled trial of intravenous N-acetylcysteine for the prevention of contrast-induced nephropathy
after cardiac catheterization: Lack of effect. Am Heart J 148:
422 429, 2004
Marenzi G, Assanelli E, Marana I, Lauri G, Campodonico J,
Grazi M, De Metrio M, Galli S, Fabbiocchi F, Montorsi P,
Veglia F, Bartorelli AL: N-acetylcysteine and contrast-induced nephropathy in primary angioplasty. N Engl J Med
354: 27732782, 2006
Yesilbursa D, Serdar A, Senturk T, Serdar Z, Sag S, Cordan
J: Effect of N-acetylcysteine on oxidative stress and ventricular function in patients with myocardial infarction.
Heart Vessels 21: 3337, 2006
Briguori C, Airoldi F, DAndrea D, Bonizzoni E, Morici N,
Focaccio A, Michev I, Montorfano M, Carlino M, Cosgrave
J, Ricciardelli B, Colombo A: Renal insufficiency following
contrast media administration trial (REMEDIAL): A randomized comparison of 3 preventive strategies. Circulation
115: 12111217. 2007
Birck R, Krzossok S, Makowetz F, Schnulle P, van der
Woude F, Braun C: Acetylcysteine for prevention of contrast nephropathy: Meta-analysis. Lancet 362: 598 603,
2003
Isenbarger D, Kent S, OMalley P: Meta-analysis of randomized clinical trials on the usefulness of acetylcysteine
for prevention of contrast nephropathy. Am J Cardiol 92:
1454 1458, 2003
Alonso A, Lau J, Jaber B, Weintraub A, Sarnak M: Prevention of radiocontrast nephropathy with N-acetylcysteine in
patients with chronic kidney disease: A meta-analysis of
randomized, controlled trials. Am J Kidney Dis 43: 19, 2004
Kshirsagar A, Poole C, Mottl A, Shoham D, Franceschini N,
Tudor G, Agrawal M, Denu-Ciocca C, Magnus Ohman E,
Finn WF: N-acetylcysteine for the prevention of radiocontrast induced nephropathy: A meta-analysis of prospective
controlled trials. J Am Soc Nephrol 15: 761769, 2004
Pannu N, Manns B, Lee H, Tonelli M: Systematic review of
the impact of N-acetylcysteine on contrast nephropathy.
Kidney Int 65: 1366 1374, 2004
Guru V, Fremes S: The role of N-acetylcysteine in preventing radiographic contrast-induced nephropathy. Clin
Nephrol 62: 77 83, 2004
Bagshaw S, Ghali WA: Acetylcysteine for prevention of
contrast-induced nephropathy: A systematic review and
meta-analysis. BMC Med 2: 38, 2004
Misra D, Leibowitz K, Gowda R, Shapiro M, Khan I: Role
Clin J Am Soc Nephrol 3: 281287, 2008
of N-acetylcysteine in prevention of contrast-induced nephropathy after cardiovascular procedures: a meta-analysis. Clin Cardiol 27: 607 610, 2004
74. Nallamothu BK, Shojania KG, Saint S, Hofer TP, Humes
HD, Moscucci M, Bates ER: Is acetylcysteine effective in
preventing contrast-related nephropathy? A meta-analysis.
Am J Med 117: 938 947, 2004
75. Liu R, Nair D, Ix J, Moore D, Bent S: N-acetylcysteine for
prevention of contrast-induced nephropathy: A systematic
review and meta-analysis. J Gen Intern Med 20: 193200,
2005
76. Duong M, MacKenzie T, Malenka D: N-Acetylcysteine prophylaxis significantly reduces the risk of radiocontrastinduced nephropathy. Catheter Cardiovasc Interv 64: 471
479, 2005
NAC in the Prevention of CIN
287
77. Bagshaw SM, McAlister FA, Manns BJ, Ghali WA: Acetylcysteine in the prevention of contrast-induced nephropathy: A case study of the pitfalls in the evolution of evidence. Arch Intern Med 166: 161166, 2006
78. Vaitkus PT, Brar C: N-acetylcysteine in the prevention of
contrast-induced nephropathy: Publication bias perpetuated by meta-analyses. Am Heart J 153: 275280, 2007
79. Izzedine H, Guerin V, Launay-Vacher V, Bernard M, Deray
G: Effect of N-acetylcysteine on serum creatinine level.
Nephrol Dial Transplant 16: 1514 1515, 2001
80. Hoffmann U, Fischereder M, Kruger B, Drobnik W,
Kramer BK: The value of N-acetylcysteine in the prevention of radiocontrast agent-induced nephropathy seems
questionable. J Am Soc Nephrol 15: 407 410, 2004
Você também pode gostar
- The Yellow House: A Memoir (2019 National Book Award Winner)No EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Nota: 4 de 5 estrelas4/5 (98)
- Kunci Jawaban To 2Documento1 páginaKunci Jawaban To 2balthier37Ainda não há avaliações
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceNo EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceNota: 4 de 5 estrelas4/5 (895)
- Duty ReportDocumento10 páginasDuty Reportbalthier37Ainda não há avaliações
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeNo EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeNota: 4 de 5 estrelas4/5 (5794)
- Sobreviviendo A La Sepsis 2016 PDFDocumento74 páginasSobreviviendo A La Sepsis 2016 PDFEsteban Parra Valencia100% (1)
- The Little Book of Hygge: Danish Secrets to Happy LivingNo EverandThe Little Book of Hygge: Danish Secrets to Happy LivingNota: 3.5 de 5 estrelas3.5/5 (399)
- Duty Report IvoDocumento8 páginasDuty Report Ivobalthier37Ainda não há avaliações
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaNo EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaNota: 4.5 de 5 estrelas4.5/5 (266)
- Pancreatic Diabetes Mellitus: Frequency and DiagnosisDocumento10 páginasPancreatic Diabetes Mellitus: Frequency and Diagnosisbalthier37Ainda não há avaliações
- 03 Irjcm 1 (4) Oa03 20160607 PDFDocumento4 páginas03 Irjcm 1 (4) Oa03 20160607 PDFbalthier37Ainda não há avaliações
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureNo EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureNota: 4.5 de 5 estrelas4.5/5 (474)
- 1 s2.0 S0272735815000914 Main PDFDocumento20 páginas1 s2.0 S0272735815000914 Main PDFJuan C. VargasAinda não há avaliações
- Never Split the Difference: Negotiating As If Your Life Depended On ItNo EverandNever Split the Difference: Negotiating As If Your Life Depended On ItNota: 4.5 de 5 estrelas4.5/5 (838)
- Daftar PustakaDocumento3 páginasDaftar Pustakabalthier37Ainda não há avaliações
- Toxoplasma Gondii Recombinant Antigens As Tools For Serodiagnosis of Human Toxoplasmosis: Current Status of StudiesDocumento2 páginasToxoplasma Gondii Recombinant Antigens As Tools For Serodiagnosis of Human Toxoplasmosis: Current Status of Studiesbalthier37Ainda não há avaliações
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryNo EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryNota: 3.5 de 5 estrelas3.5/5 (231)
- MR 25 Dec 2015-UpdateDocumento2 páginasMR 25 Dec 2015-Updatebalthier37Ainda não há avaliações
- Tehnik Safety DSC 8% - SafetyDocumento1 páginaTehnik Safety DSC 8% - Safetybalthier37Ainda não há avaliações
- The Emperor of All Maladies: A Biography of CancerNo EverandThe Emperor of All Maladies: A Biography of CancerNota: 4.5 de 5 estrelas4.5/5 (271)
- Systematic Review and Meta-Analysis of Transdiagnostic Psychological Treatments For Anxiety and Depressive Disorders in AdulthoodDocumento2 páginasSystematic Review and Meta-Analysis of Transdiagnostic Psychological Treatments For Anxiety and Depressive Disorders in Adulthoodbalthier37Ainda não há avaliações
- 12-Lead Ekg Interpretation PDFDocumento56 páginas12-Lead Ekg Interpretation PDFTnem NatAinda não há avaliações
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyNo EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyNota: 3.5 de 5 estrelas3.5/5 (2259)
- MR 25 Dec 2015-UpdateDocumento2 páginasMR 25 Dec 2015-Updatebalthier37Ainda não há avaliações
- DAFTAR ISI Diatesis HemoragikDocumento1 páginaDAFTAR ISI Diatesis Hemoragikbalthier37Ainda não há avaliações
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersNo EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersNota: 4.5 de 5 estrelas4.5/5 (344)
- 12-Lead Ekg Interpretation PDFDocumento56 páginas12-Lead Ekg Interpretation PDFTnem NatAinda não há avaliações
- COVER Jurnal Endokrin 2Documento1 páginaCOVER Jurnal Endokrin 2balthier37Ainda não há avaliações
- Team of Rivals: The Political Genius of Abraham LincolnNo EverandTeam of Rivals: The Political Genius of Abraham LincolnNota: 4.5 de 5 estrelas4.5/5 (234)
- COVER Jurnal Endokrin 3Documento2 páginasCOVER Jurnal Endokrin 3balthier37Ainda não há avaliações
- DAFTAR ISI Diatesis HemoragikDocumento1 páginaDAFTAR ISI Diatesis Hemoragikbalthier37Ainda não há avaliações
- Optimal Blood Pressure in Patients With Atrial Fibrillation (From The AFFIRM Trial)Documento1 páginaOptimal Blood Pressure in Patients With Atrial Fibrillation (From The AFFIRM Trial)balthier37Ainda não há avaliações
- The Unwinding: An Inner History of the New AmericaNo EverandThe Unwinding: An Inner History of the New AmericaNota: 4 de 5 estrelas4/5 (45)
- Mental Status ExamDocumento10 páginasMental Status ExamSrini VoruAinda não há avaliações
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreNo EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreNota: 4 de 5 estrelas4/5 (1090)
- Intravenous TherapyDocumento30 páginasIntravenous TherapyKoass14 2012Ainda não há avaliações
- List Alat OK Mayor Dan Minor 30 07 2022 20.12Documento72 páginasList Alat OK Mayor Dan Minor 30 07 2022 20.12dehaaAinda não há avaliações
- 16-4 I The Truth About Physician Health ProgramsDocumento5 páginas16-4 I The Truth About Physician Health ProgramslbandrewAinda não há avaliações
- Inhibidores de La ECADocumento16 páginasInhibidores de La ECAFarmaFMAinda não há avaliações
- Anexo 3 Consenso de La Eskka en OsteoartritisDocumento58 páginasAnexo 3 Consenso de La Eskka en OsteoartritisgrimmAinda não há avaliações
- Phenylephrine HydrochlorideDocumento5 páginasPhenylephrine HydrochlorideRoger Jr PumarenAinda não há avaliações
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)No EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Nota: 4.5 de 5 estrelas4.5/5 (121)
- Spleen Diseases DiagnosisDocumento2 páginasSpleen Diseases DiagnosisPraveen VontiAinda não há avaliações
- Aplicación de Un Programa de Entrenamiento de Fuerza en Futbolistas Jovenes PDFDocumento16 páginasAplicación de Un Programa de Entrenamiento de Fuerza en Futbolistas Jovenes PDFEsteban LopezAinda não há avaliações
- NeurontinDocumento3 páginasNeurontinFesto HakiAinda não há avaliações
- Pregnancy Induced HypertensionDocumento16 páginasPregnancy Induced Hypertensiondgraham36Ainda não há avaliações
- ARTICLE - DR.S R PHATAK. Kinjal Dave - 4th BHMCDocumento2 páginasARTICLE - DR.S R PHATAK. Kinjal Dave - 4th BHMCᎧᎷ ᎴᏗᏉᏋAinda não há avaliações
- Patterson - Allergic Diseases 6th EdDocumento370 páginasPatterson - Allergic Diseases 6th Edvasile100% (2)
- A Report On Depression: Mental HealthDocumento12 páginasA Report On Depression: Mental HealthArchiev KumarAinda não há avaliações
- Case GNApsDocumento47 páginasCase GNApsAndhika Hadi WirawanAinda não há avaliações
- Dawn Guided Meditation To RecordDocumento2 páginasDawn Guided Meditation To Recorddiego_guimarães_64Ainda não há avaliações
- Padlet 5z3qwhf8dn00Documento2 páginasPadlet 5z3qwhf8dn00api-266658713Ainda não há avaliações
- Peter SelgDocumento4 páginasPeter SelgAlexandra Maria NeaguAinda não há avaliações
- Homoeopathic Case TakingDocumento10 páginasHomoeopathic Case TakingSudhir GuptaAinda não há avaliações
- Charkoli ProjectDocumento2 páginasCharkoli ProjectckbbbsrAinda não há avaliações
- AscarisDocumento16 páginasAscarisRommy Kurniawan DeskyAinda não há avaliações
- Antifungal Susceptibility Pattern Against Dermatophytic Strains Isolated From Humans in Anambra State, NigeriaDocumento8 páginasAntifungal Susceptibility Pattern Against Dermatophytic Strains Isolated From Humans in Anambra State, NigeriaIJAERS JOURNALAinda não há avaliações
- Hazardous Materials Management Plan SMDocumento26 páginasHazardous Materials Management Plan SMdarmayunitaAinda não há avaliações
- 1998-08 HP JournalDocumento90 páginas1998-08 HP JournalElizabeth WilliamsAinda não há avaliações
- BestDocumento25 páginasBestAlejandro Lopez OsorioAinda não há avaliações
- Application Technique Traction PDFDocumento25 páginasApplication Technique Traction PDFAZOZ 19Ainda não há avaliações
- Suprapubic Prostatectomy HinmanDocumento9 páginasSuprapubic Prostatectomy HinmanputriAinda não há avaliações
- Case 3 Tuberculosis Group 3Documento72 páginasCase 3 Tuberculosis Group 3Antonio EscotoAinda não há avaliações
- Systematic Review - The Effectiveness ofDocumento15 páginasSystematic Review - The Effectiveness ofSabrinaAinda não há avaliações
- BibliopocDocumento4 páginasBibliopocKarlo ReyesAinda não há avaliações
- By the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsNo EverandBy the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsAinda não há avaliações
- Summary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisNo EverandSummary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisNota: 4.5 de 5 estrelas4.5/5 (42)
- Think This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeNo EverandThink This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeNota: 2 de 5 estrelas2/5 (1)