Escolar Documentos
Profissional Documentos
Cultura Documentos
Appendix 15
Enviado por
Toms Reza0 notas0% acharam este documento útil (0 voto)
3 visualizações1 páginaThis document provides information on calculating postoperative fluid deficits and replacement. It outlines how to calculate a patient's estimated fluid requirement per hour based on their weight in kilograms. The estimated fluid deficit is calculated by multiplying the estimated fluid requirement by the number of hours the patient has been nil per os (nothing by mouth). The total postoperative fluid deficit takes into account the estimated fluid deficit, crystalloid fluid replacement for blood loss at three times the estimated blood loss, and any intraoperative fluid replacement. The document also lists various intravenous fluid solutions and their electrolyte and calorie content.
Descrição original:
jhkuhkhhiphjoph
Direitos autorais
© © All Rights Reserved
Formatos disponíveis
PDF, TXT ou leia online no Scribd
Compartilhar este documento
Compartilhar ou incorporar documento
Você considera este documento útil?
Este conteúdo é inapropriado?
Denunciar este documentoThis document provides information on calculating postoperative fluid deficits and replacement. It outlines how to calculate a patient's estimated fluid requirement per hour based on their weight in kilograms. The estimated fluid deficit is calculated by multiplying the estimated fluid requirement by the number of hours the patient has been nil per os (nothing by mouth). The total postoperative fluid deficit takes into account the estimated fluid deficit, crystalloid fluid replacement for blood loss at three times the estimated blood loss, and any intraoperative fluid replacement. The document also lists various intravenous fluid solutions and their electrolyte and calorie content.
Direitos autorais:
© All Rights Reserved
Formatos disponíveis
Baixe no formato PDF, TXT ou leia online no Scribd
0 notas0% acharam este documento útil (0 voto)
3 visualizações1 páginaAppendix 15
Enviado por
Toms RezaThis document provides information on calculating postoperative fluid deficits and replacement. It outlines how to calculate a patient's estimated fluid requirement per hour based on their weight in kilograms. The estimated fluid deficit is calculated by multiplying the estimated fluid requirement by the number of hours the patient has been nil per os (nothing by mouth). The total postoperative fluid deficit takes into account the estimated fluid deficit, crystalloid fluid replacement for blood loss at three times the estimated blood loss, and any intraoperative fluid replacement. The document also lists various intravenous fluid solutions and their electrolyte and calorie content.
Direitos autorais:
© All Rights Reserved
Formatos disponíveis
Baixe no formato PDF, TXT ou leia online no Scribd
Você está na página 1de 1
Table A15-1 Fluid Deficits
Calculation of postoperative fluid deficit
Estimated fluid requirement (EFR) per hour:
First 10kg: 4cc/kg (100cc/kg/day)
Second 10kg: 2cc/kg (50cc/g/day)
Above 20kg: 1cc/kg (25cc/kg/day)
Example: EFR for a 70 kg patient = (10 4) + (10 2) + (50 l)
= 40 + 20 + 50
= 110 cc/h
Estimated fluid deficit (EFD)=EFR times the number of hours since last oral intake:
Example: EFD for 70-kg patient NPO (nothing by mouth) for 8 hours
EFR 8=110cc/h8h=880cc
Replacement of blood losses:
Crystalloid fluid: 3 times estimated blood loss (EBL)
Colloid or blood: 1 times EBL
Example: For EBL of 400cc, crystalloid fluid replacement should be 3400=1,200cc
Total postsurgical fluid deficit (TPFD):
EFD+(blood losses 3)fluid replaced by anesthesia during surgery
Example: A 70-kg patient is NPO for 8 hours, has 400cc of surgical blood loss, and receives
1,500cc of crystalloid during surgery
TPFD=880cc+1,200cc1,500cc=580cc
Insensible losses are generally negligible in most orofacial procedures.
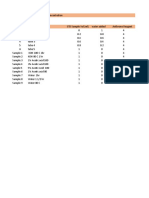
Table A15-2 Types of Intravenous Fluid (Milliequivalents/L)
IV solution NA K Cl Bicarbonate Calories
Ringers lactate 130 4 109 28 0
Ringers solution 147 4 155 0 0
Normal saline (0.9%) 154 0 154 0 0
Lactated Ringers with dextrose 130 4 109 28 170
Dextrose 2.5% in NaCl 0.45% 77 0 77 0 85
Dextrose 5% in Ringers lactate 148 4 156 0 170
Dextrose 5% in 2% NaCl 34 0 34 0 170
Dextrose 5% in 0.33% NaCl 56 0 56 0 170
Dextrose 5% in 0.45% NaCl 77 0 77 0 170
Dextrose 5% in 0.9% NaCl 154 0 154 0 170
Dextrose 10% in 0.9% NaCl 154 0 154 0 340
Dextrose 5% in water 0 0 0 0 200
Dextrose 10% in water 0 0 0 0 400
Você também pode gostar
- VELP Application Note Water-Sludge E-K-001-2015 1Documento3 páginasVELP Application Note Water-Sludge E-K-001-2015 1Nur Rizky InayahAinda não há avaliações
- Pedia NotesDocumento7 páginasPedia Noteseyakoy100% (4)
- Fluids: Presenter: Atwebembere Raymond Faciliitator: Dr. KibengoDocumento34 páginasFluids: Presenter: Atwebembere Raymond Faciliitator: Dr. KibengoNinaAinda não há avaliações
- Tatalaksana Syok Hipovolemik & HipoglikemiaDocumento40 páginasTatalaksana Syok Hipovolemik & HipoglikemiaMuhammad Daviq0% (1)
- Management Terapi CairanDocumento60 páginasManagement Terapi CairanHayat Hamzah DawiAinda não há avaliações
- Separation Processes - I (CHE F244) Total Marks - 15 Due Date & Time: 01/07/2020, 5:00 PM AssignmentDocumento4 páginasSeparation Processes - I (CHE F244) Total Marks - 15 Due Date & Time: 01/07/2020, 5:00 PM AssignmentElliot AldersonAinda não há avaliações
- Buffers and Stock SolutionsDocumento3 páginasBuffers and Stock SolutionsDr. Kaushal Kishor SharmaAinda não há avaliações
- IV Fluids and Electrolyte PhysiologyDocumento64 páginasIV Fluids and Electrolyte PhysiologypaulaAinda não há avaliações
- Et Iso 14673-2.2012Documento19 páginasEt Iso 14673-2.2012dcardonasterAinda não há avaliações
- 1073A DS.v1006DaDocumento2 páginas1073A DS.v1006DaElfohArvinAinda não há avaliações
- Management Terapi CairanDocumento60 páginasManagement Terapi Cairanpeter singalAinda não há avaliações
- Fluid and Electrolyte MGT in SurgeryDocumento40 páginasFluid and Electrolyte MGT in SurgeryJohn AgamahAinda não há avaliações
- Dasar - Dasar Terapi: Cairan Dan ElektrolitDocumento60 páginasDasar - Dasar Terapi: Cairan Dan ElektrolitdedeAinda não há avaliações
- Teknik Boom Ekstraksi RNADocumento4 páginasTeknik Boom Ekstraksi RNAZulkifli AsAinda não há avaliações
- 01 Mini ExtractionDocumento4 páginas01 Mini ExtractionToni D.Ainda não há avaliações
- Figure 1 Sulfolane UnitDocumento2 páginasFigure 1 Sulfolane Unittusen krishAinda não há avaliações
- METHOD #: 325.1 TitleDocumento4 páginasMETHOD #: 325.1 TitleKarimah SabilaAinda não há avaliações
- 0018 USP Terazosin MMDocumento4 páginas0018 USP Terazosin MMari anggoroAinda não há avaliações
- Practical Orientation To Recombinant DNA TechnologyDocumento35 páginasPractical Orientation To Recombinant DNA TechnologyShikha YashveerAinda não há avaliações
- Buffer Preparation PDFDocumento6 páginasBuffer Preparation PDFbiotech_vidhyaAinda não há avaliações
- Practical Hand Outs-Molecular Biology (BIO302)Documento33 páginasPractical Hand Outs-Molecular Biology (BIO302)Anaya MalikAinda não há avaliações
- Commonly Used ReagentsDocumento5 páginasCommonly Used Reagents石子Ainda não há avaliações
- DR - Sabah Noori 1Documento26 páginasDR - Sabah Noori 1Mighty AbodyAinda não há avaliações
- Buffers and Stock SolutionsDocumento3 páginasBuffers and Stock SolutionsJohnAinda não há avaliações
- Fluid and Electrolyte BalanceDocumento3 páginasFluid and Electrolyte BalanceAdebisiAinda não há avaliações
- Buffer Preparation (Shi Lab) : 1. 1 M Tris-Hcl BuffersDocumento6 páginasBuffer Preparation (Shi Lab) : 1. 1 M Tris-Hcl BuffersEstari MamidalaAinda não há avaliações
- Applications-Application - C.3. Nitrate in Aqueous Samples and Eluates - EnglishDocumento3 páginasApplications-Application - C.3. Nitrate in Aqueous Samples and Eluates - EnglishGabriela Alejandra Benito MoralesAinda não há avaliações
- MAN0016351 2162373 PierceHighCapacityEndotoxRemovalResin UGDocumento4 páginasMAN0016351 2162373 PierceHighCapacityEndotoxRemovalResin UGRam KishoreAinda não há avaliações
- Pluronic NF GradesDocumento2 páginasPluronic NF GradesAdamAinda não há avaliações
- KF Titration BasicsDocumento4 páginasKF Titration Basicsammuluhai333Ainda não há avaliações
- Isolation of Plant Genomic DNA (Draft - 2)Documento4 páginasIsolation of Plant Genomic DNA (Draft - 2)Prayash NayakAinda não há avaliações
- Nitrile Film Dipping Procedures LabDocumento8 páginasNitrile Film Dipping Procedures LabsomehailimAinda não há avaliações
- Hla-Hypernatremia HandoutDocumento30 páginasHla-Hypernatremia HandoutdeahadfinaAinda não há avaliações
- Digital TitratorDocumento3 páginasDigital TitratorNura RikuoAinda não há avaliações
- Clinica Chimica Actn, 59 155-160 0Documento6 páginasClinica Chimica Actn, 59 155-160 0Paulo Nunes CesarAinda não há avaliações
- CTAB DNA ExtractionDocumento2 páginasCTAB DNA ExtractionHumam-bmAinda não há avaliações
- Alkaline Lysis Buffer A RecipeDocumento5 páginasAlkaline Lysis Buffer A Recipeme_dayakarAinda não há avaliações
- NITROGENDocumento3 páginasNITROGENCarol KalinAinda não há avaliações
- APES ToxicologyLabLD50Documento4 páginasAPES ToxicologyLabLD50caleb.311006Ainda não há avaliações
- Enzyme Report 4Documento8 páginasEnzyme Report 4Hema KannanAinda não há avaliações
- Efficacity Liq-Lia ExtractionDocumento7 páginasEfficacity Liq-Lia ExtractionZAKARIA BOUNOUAILAinda não há avaliações
- Iv FluidsDocumento1 páginaIv FluidsrodtanchoAinda não há avaliações
- Urea 275Documento12 páginasUrea 275ckpellegrino5809Ainda não há avaliações
- Tarif Pelayanan HemodialisaDocumento7 páginasTarif Pelayanan HemodialisaNur IffahAinda não há avaliações
- Distillation LabDocumento18 páginasDistillation LabWong XimeiAinda não há avaliações
- Wrd-Ot-Neutralization 445273 7Documento44 páginasWrd-Ot-Neutralization 445273 7Sheik Abdullah BakrudeenAinda não há avaliações
- AN5391 Determination of TKN in Water by Using KT8000 SeriesDocumento7 páginasAN5391 Determination of TKN in Water by Using KT8000 SeriesJaysonAbenirCabahugAinda não há avaliações
- Preparation of Taq DNA PolymeraseDocumento3 páginasPreparation of Taq DNA PolymeraseGerardo David Gonzalez EstradaAinda não há avaliações
- Determination of DextroseDocumento2 páginasDetermination of DextroseRajesh RaviAinda não há avaliações
- Fluid TherapyDocumento56 páginasFluid TherapyHabibie El RamadhaniAinda não há avaliações
- TubeDocumento2 páginasTubeAlex XanderAinda não há avaliações
- Hydration of Propylene Via Sulfation HydrationDocumento4 páginasHydration of Propylene Via Sulfation HydrationDineshAinda não há avaliações
- Anthrone ReagentDocumento6 páginasAnthrone ReagentMitchellMarkMarmitaAinda não há avaliações
- Method Water QualityDocumento8 páginasMethod Water Qualityazilah harisAinda não há avaliações
- N.C.A Lu177 Reference Radiolabeling ProcedureDocumento4 páginasN.C.A Lu177 Reference Radiolabeling ProcedureFadhil Muhammad A.100% (1)
- The Chemistry of Dairy Products - A Chemical Analysis of Milk, Cream and ButterNo EverandThe Chemistry of Dairy Products - A Chemical Analysis of Milk, Cream and ButterAinda não há avaliações
- The Chemistry of Fertilisers and Manure - Including Information on the Chemical Constituents and Types of Fertilisers and ManuresNo EverandThe Chemistry of Fertilisers and Manure - Including Information on the Chemical Constituents and Types of Fertilisers and ManuresNota: 5 de 5 estrelas5/5 (1)
- Advanced Pharmaceutical analysisNo EverandAdvanced Pharmaceutical analysisNota: 4.5 de 5 estrelas4.5/5 (2)
- ECG Praktis-Sesi 1Documento45 páginasECG Praktis-Sesi 1Jenny CandraAinda não há avaliações
- Obs&GYN 1Documento5 páginasObs&GYN 1AbedelrahmanShekhAhmadAinda não há avaliações
- Literature Review Ectopic PregnancyDocumento4 páginasLiterature Review Ectopic Pregnancyakjnbowgf100% (1)
- Research Objective ResultDocumento2 páginasResearch Objective ResultTriciaAinda não há avaliações
- Histology of Oral Mucous Membrane and GingivaDocumento86 páginasHistology of Oral Mucous Membrane and GingivahazeemmegahedAinda não há avaliações
- Basal Body Temperature Monitoring Contraceptive MethodDocumento5 páginasBasal Body Temperature Monitoring Contraceptive Methodpriya vermaAinda não há avaliações
- Handouts For Normal PediatricsDocumento54 páginasHandouts For Normal Pediatricsapi-3842758Ainda não há avaliações
- Triage System in Accident and EmergencyDocumento8 páginasTriage System in Accident and EmergencySherry SinghAinda não há avaliações
- Instructions For Use - IncostressDocumento2 páginasInstructions For Use - IncostressGaynor MorganAinda não há avaliações
- My Resume...Documento5 páginasMy Resume...Kat TangonanAinda não há avaliações
- ProofcorrectionsDocumento10 páginasProofcorrectionsRicardo QuintanaAinda não há avaliações
- Use of Injection Solcoseryl For The Treatment of OligohydramniosDocumento7 páginasUse of Injection Solcoseryl For The Treatment of OligohydramniosJosselle Sempio CalientaAinda não há avaliações
- Neonatal ResuscitationDocumento15 páginasNeonatal ResuscitationAmruta GadeAinda não há avaliações
- Sliwa Et Al-2010-European Journal of Heart FailureDocumento12 páginasSliwa Et Al-2010-European Journal of Heart FailurealfredoibcAinda não há avaliações
- Jurnal ICH 2008Documento6 páginasJurnal ICH 2008Yusuf Agung NugrohoAinda não há avaliações
- Fmge Blue Print PDFDocumento1 páginaFmge Blue Print PDFLesbputih Gelap100% (1)
- Keeping Birth Normal: Position StatementDocumento3 páginasKeeping Birth Normal: Position StatementCatur ErtyAinda não há avaliações
- European Journal of Obstetrics & Gynecology and Reproductive BiologyDocumento7 páginasEuropean Journal of Obstetrics & Gynecology and Reproductive BiologyLydia OliviaAinda não há avaliações
- PasdfDocumento8 páginasPasdfHuy LeAinda não há avaliações
- GCM Clerks Guide CPCMH v1.3Documento114 páginasGCM Clerks Guide CPCMH v1.3savan patelAinda não há avaliações
- ORE - UK Dental Reference BooksDocumento4 páginasORE - UK Dental Reference BooksKisshore ReddyAinda não há avaliações
- Intestin Gros Si AnorectalDocumento282 páginasIntestin Gros Si AnorectalPatricia IoanaAinda não há avaliações
- Clinical Case Presentation:: Premature Rupture of MembranesDocumento31 páginasClinical Case Presentation:: Premature Rupture of Membranesjoshua remonAinda não há avaliações
- Midwifery Pharmacology-9Documento1 páginaMidwifery Pharmacology-9georgeloto12Ainda não há avaliações
- ACR 2018 TXIT Exam RationalesDocumento94 páginasACR 2018 TXIT Exam Rationalesgermanfutbol7100% (3)
- Words of Wisdom From and To PhlebotomistsDocumento7 páginasWords of Wisdom From and To PhlebotomistsDanhil RamosAinda não há avaliações
- Factors Influencing The Role of Primary CareDocumento10 páginasFactors Influencing The Role of Primary CareAdhiw AmanAinda não há avaliações
- SURGICAL CARE COMPLEX POLICY (OsMak-CLN-SD-SCC) PDFDocumento2 páginasSURGICAL CARE COMPLEX POLICY (OsMak-CLN-SD-SCC) PDFpatientsafetyAinda não há avaliações
- Clinical Tips For The Management of Perimenopausal Syndrome by DR - Deepti ChawlaDocumento19 páginasClinical Tips For The Management of Perimenopausal Syndrome by DR - Deepti ChawlaHomoeopathic PulseAinda não há avaliações
- Shunt Calculation, NICVDDocumento31 páginasShunt Calculation, NICVDNavojit ChowdhuryAinda não há avaliações