Escolar Documentos
Profissional Documentos
Cultura Documentos
Cranial Neuralgias
Enviado por
Habib G. Moutran BarrosoDireitos autorais
Formatos disponíveis
Compartilhar este documento
Compartilhar ou incorporar documento
Você considera este documento útil?
Este conteúdo é inapropriado?
Denunciar este documentoDireitos autorais:
Formatos disponíveis
Cranial Neuralgias
Enviado por
Habib G. Moutran BarrosoDireitos autorais:
Formatos disponíveis
Review Article
Cranial Neuralgias
Address correspondence to
Dr William P. Cheshire Jr,
Mayo Clinic, 4500 San Pablo
Road, Jacksonville, FL 32224,
cheshire@mayo.edu. William P. Cheshire Jr, MD, FAAN
Relationship Disclosure:
Dr Cheshire has received
personal compensation
for manuscript preparation ABSTRACT
from Turner White Purpose of Review: Pain arising from cranial neuralgias represents a significant health
Communications, Inc.
Unlabeled Use of
burden. Successful treatment depends on accurate diagnosis, which requires knowledge
Products/Investigational of neuroanatomy and pathophysiology as well as familiarity with the varied clinical
Use Disclosure: presentations encountered in neurologic practice. This article delineates the relevant
Dr Cheshire discusses the
unlabeled/investigational use
anatomy, clinical features, and management of the most common primary and secondary
of oxcarbazepine, baclofen, cranial neuralgias.
phenytoin, fosphenytoin, Recent Findings: Trigeminal neuralgia, which can result from neurovascular compres-
gabapentin, botulinum toxin,
tizanidine, pimozide, and
sion or demyelination, is a particularly severe form of facial pain. Herpes zoster virus is a
motor cortex stimulation for common cause of neuralgia that causes herpes zoster ophthalmicus acutely and post-
the treatment of trigeminal herpetic neuralgia chronically. Rarer facial pain syndromes arising from a single nerve
neuralgia; tricyclics, pregabalin,
opioids, tramadol, and capsaicin
include glossopharyngeal neuralgia, nervus intermedius neuralgia, and paratrigeminal
for the treatment of postherpetic oculosympathetic syndrome.
neuralgia; carbamazepine, Summary: In patients presenting with a cranial neuralgia, unless the etiology is
gabapentin, lamotrigine, and
tricyclics for the treatment of
apparent (eg, herpes zoster), cranial imaging studies should be undertaken to look
nervus intermedius neuralgia; for structural abnormalities such as neoplasm, granulomatous disease, demyelin-
and nonsteroidal anti-inflammatory ating disease, or vascular malformations. Management of both common and rare
drugs, muscle relaxants, tricyclics,
gabapentin, and occipital nerve
cranial neuralgias is often challenging and is best guided by the most recent
stimulators for the treatment available evidence.
of occipital neuralgia.
* 2015, American Academy Continuum (Minneap Minn) 2015;21(4):10721085.
of Neurology.
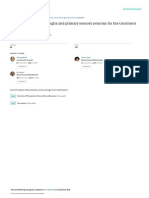
INTRODUCTION neuralgias involve the trigeminal nerve,
Cranial neuralgias encompass some of which comprises ophthalmic, maxillary,
the most debilitating forms of neuro- and mandibular divisions (Figure 9-11).
pathic pain that come to the attention The trigeminal nerve also mediates pain
of neurologists. One reason may be that arising from co-innervated structures, such
the face, which is disproportionately rep- as the optic nerve and ocular motor mus-
resented on the homunculus of the pri- cles. The sensory branches of the facial
mary somatosensory cortex, is the main and glossopharyngeal nerves and the
portal through which the nervous sys- second cervical nerve can also transmit
tem encounters the world. Facial pain pain (Table 9-12).
also impacts patients psychologically and
socially, as the face is integral to inter-
CLINICAL APPROACH TO
personal communication and ones sense
DIAGNOSIS
of personal identity.
The clinical evaluation of the patient
NEUROANATOMICAL BASIS with facial pain requires an organized ap-
Nociceptive pain can arise from any area proach beginning with localization. Is
of the scalp, face, or deeper cranial struc- the pain unilateral or bilateral? Can it be
tures in response to injury. Neuropathic traced to a single cranial nerve, or is
pain, which occurs in the absence of it more broadly distributed, which may
an ongoing tissue injury, can arise from indicate a central or multiple cranial
any of the sensory nerves that innervate nerve pain syndrome? Are colocalizing
these structures. The majority of cranial neurologic deficits present?
1072 www.ContinuumJournal.com August 2015
Copyright American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
KEY POINTS
h Most cranial neuralgias
involve the trigeminal
nerve; however, the
sensory branches of
the facial and
glossopharyngeal nerves
and the second cervical
nerve can also
transmit pain.
h An organized clinical
approach is key to
reaching the correct
diagnosis in patients
with facial pain.
h Trigeminal neuralgia is
the most intensely
painful of the
cranial neuralgias.
h The pain of trigeminal
neuralgia is paroxysmal
FIGURE 9-1 Sensory innervation of the face by the trigeminal nerve. The trigeminal nerve root and classically sharp
exits the pons and gives rise to the trigeminal (gasserian or semilunar) ganglion, which
divides into ophthalmic, maxillary, and mandibular divisions of the trigeminal nerve. or electrical in quality.
Reprinted from Gray H, Lea & Febiger.1
The next question to address is etiol- nerve V). Trigeminal neuralgia is also the
ogy. Can the onset of the pain be traced most intense of the cranial neuralgias.
to an identifiable insult, such as trauma, Also known as tic douloureux, its prev-
a viral rash, an infectious or inflammatory alence is estimated at between 5 and 29 per
process, or a structural intracranial lesion? 100,000 person-years.3Y6 Onset is most
The temporal profile, quality of pain, often after the age of 50, and its incidence
and associated features are also helpful to increases with advancing age. Women are
narrow the diagnosis. Is the pain paroxys- affected 1.7 times more often than men.
mal or continuous? How long do episodes The International Headache Society
last? What factors trigger, worsen, or re- (IHS) defines trigeminal neuralgia as a
lieve the pain? Does the pain correlate disorder characterized by recurrent uni-
with the menstrual cycle, time of day, spe- lateral brief electric shock-like pains, abrupt
cific activities, or certain types of physical in onset and termination, limited to the
stimulation of the painful area or remote distribution of one or more divisions of
facial areas? Is the pain dull, aching, throb- the trigeminal nerve and triggered by
bing, pulsing, sharp, stinging, prickling, innocuous stimuli.2 The maxillary and
burning, or electrical in quality? Are there mandibular branches are most often af-
autonomic accompaniments? What types fected at about equal frequency. The sharp
of medications have been effective? Are or electrical paroxysms last seconds to
imaging abnormalities present? minutes and may occur in rapid succes-
sion. Painful attacks may be followed by
TRIGEMINAL NEURALGIA a brief refractory period.
The most common cranial neuralgia Patients may notice a sensitive trig-
involves the trigeminal nerve (cranial ger zone, which, although on the same
Continuum (Minneap Minn) 2015;21(4):10721085 www.ContinuumJournal.com 1073
Copyright American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
Cranial Neuralgias
TABLE 9-1 International Headache Society Classification of Cranial Neuralgias Organized
Neuroanatomicallya
International Headache
Level Nerve Society Classification
Cranial nerve II Optic nerve Headache associated with optic neuritis
Cranial nerves III, Oculomotor, trochlear, Headache attributed to ischemic oculomotor nerve palsy
IV, VI and abducens nerves
Cranial nerve V Trigeminal nerve Classical trigeminal neuralgia, purely paroxysmal
Classical trigeminal neuralgia with concomitant persistent
facial pain
Trigeminal autonomic cephalalgias
Painful trigeminal neuropathy attributed to acute herpes zoster
Painful trigeminal neuropathy attributed to postherpetic neuralgia
Painful trigeminal neuropathy, posttraumatic
Painful trigeminal neuropathy attributed to space-occupying lesion
Persistent idiopathic facial pain
Burning mouth syndrome
Cranial nerve VII Facial nerve Nervus intermedius neuralgia
Cranial nerve IX Glossopharyngeal nerve Glossopharyngeal neuralgia
Cervical nerve 2 Occipital nerve Occipital neuralgia
CNS Central neuropathic pain Painful trigeminal neuropathy attributed to multiple sclerosis
a
Data from Headache Classification Committee of the International Headache Society (IHS), Cephalalgia.2 www.ihs-classification.org/
_downloads/mixed/International-Headache-Classification-III-ICHD-III-2013-Beta.pdf.
side of the face, does not always coincide months or years later. For most patients,
with the location of pain. The trigger pain frequency and intensity progres-
zone may be located near the nasolabial sively increase over time. When tri-
fold; on the lateral aspect of the nares; geminal neuralgia is active, patients are
or along the lip, gum line, or tongue. The usually asymptomatic between attacks,
slightest touch of the trigger zone during although in a minority of cases, contin-
routine daily activities, such as brushing uous dull or burning background pain
or flossing the teeth, shaving, washing may precede or linger after the more
the face, applying facial cosmetics, smil- severe paroxysms. The IHS terms this
ing, speaking, or eating, will unleash ex- classical trigeminal neuralgia with con-
cruciating pain (Case 9-1). In severe cases, comitant persistent facial pain.2 The
patients may lose weight from not eat- continuous component is presumably
ing. Pain triggered by exposure to wind owing to central sensitization and may
or a cool breeze may confine the pa- respond poorly to treatment.
tient indoors. Neurologic examination in trigeminal
Although many patients will experi- neuralgia is usually normal or may dis-
ence spontaneous remissions, not all do, close a subtle trigeminal sensory def-
and severe pain may return suddenly icit. The patient presenting with newly
1074 www.ContinuumJournal.com August 2015
Copyright American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
Case 9-1
A 67-year-old man presented with a 2-year history of paroxysmal pain affecting his right cheek. The first
time he experienced this pain was while shaving, and he wondered if his electric razor had a short circuit,
because the pain felt like an electric shock shooting through his face. The pain had increased in frequency,
occurring numerous times during the day, and although each episode lasted only a few seconds, he described
the pain as excruciating and rated it as 10 times more severe than the pain he had experienced from a
kidney stone years earlier. Episodes of pain were easily triggered by the slightest breeze against his face,
by brushing his teeth, and at times by speaking or eating. Sneezing was particularly painful, although
he had no sinus discharge. He had been thoroughly evaluated by his dentist, who assured him that the pain was
not coming from his teeth. Whereas treatment with ibuprofen and oxycodone failed to prevent or reduce the
pain, carbamazepine at 200 mg 3 times a day had almost eliminated it. Neurologic examination was normal,
except that touching a wisp of cotton to his right nasolabial fold provoked the patients pain, causing him to
wince and withdraw. MRI of the brain disclosed a large prepontine mass (Figure 9-2). The diagnosis was
trigeminal neuralgia affecting the right maxillary division secondary to a prepontine epidermoid cyst.
Comment. Although the majority of patients with trigeminal neuralgia will have normal cranial
imaging results, a structural cause may be found in up to 15% of cases of trigeminal neuralgia.7
FIGURE 9-2 Axial brain MRI disclosing a large nonenhancing T1 hypointense (A) and T2
hyperintense (B) prepontine epidermoid cyst causing posterior displacement of
the brainstem and deforming the anterior aspect of the right brachium pontis. The
mass encases the cisternal portion of the right trigeminal nerve, which is not visualized, whereas at the
same level, the left trigeminal nerve root is seen as a linear structure just lateral to the basilar artery.
diagnosed trigeminal neuralgia should un- search should be undertaken for an KEY POINT
dergo gadolinium-enhanced MRI of the underlying tumor, including repeated h The patient presenting
brain with fine cuts through the trigem- cranial imaging with attention to the en- with newly diagnosed
trigeminal neuralgia
inal nerves. A structural cause may be tire course of the trigeminal nerve. The
should undergo
found in up to 15% of cases of trigem- differential diagnosis for trigeminal neu-
gadolinium-enhanced
inal neuralgia.7 When unmistakable or ralgia includes invasive squamous cell MRI of the brain with
progressive facial sensory loss is detected, carcinoma of the face, meningioma, ves- fine cuts through the
unless explained by prior trigeminal nerve tibular schwannoma, epidermoid cyst or trigeminal nerves.
surgery, or if other cranial nerve or focal other skull base tumor, Chiari malforma-
neurologic deficits are present, a careful tion, or saccular aneurysm or arteriovenous
Continuum (Minneap Minn) 2015;21(4):10721085 www.ContinuumJournal.com 1075
Copyright American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
Cranial Neuralgias
KEY POINTS
h Neurovascular malformation compressing the trigeminal pine is considered one of the diagnos-
compression, which is nerve root.8 tic features of trigeminal neuralgia as
believed to be the basis Many cases of trigeminal neuralgia, distinguished from other types of facial
for pain in most cases of if not the majority, result from trigem- pain.8 A low dose, 100 mg 2 to 3 times
trigeminal neuralgia, is inal neurovascular compression. Ac- daily, may be effective initially, as the
usually not visible by cording to this model, a redundant or lowest effective dose is preferable to
standard MRI. tortuous vascular loop, most often the minimize side effects, particularly in pa-
h Trigeminal neuralgia that superior cerebellar artery, impinges on tients with multiple sclerosis, some of
occurs bilaterally or in the trigeminal nerve root in the poste- whom may have dizziness, ataxia, or im-
younger patients may rior fossa. Over time, pulsatile indenta- paired coordination at baseline. Un-
suggest a diagnosis of tion induces a focus of demyelination, fortunately, over time larger doses are
multiple sclerosis. which leads to aberrant discharge of the typically required to maintain pain con-
h Carbamazepine is the drug nerve spontaneously or in response trol, and eventually carbamazepine may
of first choice in treating to normally innocuous afferent traffic. not be effective. Level B evidence exists
trigeminal neuralgia. Ephaptic spillover to adjacent fibers for oxcarbazepine, and Level C evidence
within the trigeminal nerve reaches a exists for baclofen and lamotrigine.7
critical threshold, which ignites a pain- Gabapentin or, for acute crisis, phe-
ful crescendo of maximal discharge. Cur- nytoin or fosphenytoin may be useful
rently, routine MRI techniques lack the in some patients.17,18 Several small short-
resolution to identify neurovascular com- term studies have indicated that intra-
pression with sufficient sensitivity or spe- dermal injection of onabotulinumtoxinA
cificity.9 Neurovascular compression may, may be effective in the treatment of
however, be visualized in some cases by trigeminal neuralgia.19,20 Limited, low-
high-resolution imaging, including con- quality evidence suggests that tiza-
structive interference in steady state (CISS) nidine and pimozide may be helpful in
coronal imaging.10 some patients.21
Compared to the general population, For patients with severe, debilitat-
patients with multiple sclerosis have a ing pain refractory to medical therapy,
20-fold increased risk of developing tri- surgical options should be considered.
geminal neuralgia, with a prevalence of The choice of procedure often depends
2% to 5%.11,12 Whereas idiopathic or neu- on the neurosurgeons preference and
rovascular trigeminal neuralgia is almost experience.22 Level C evidence exists for
always (97%) unilateral, when trigeminal microvascular decompression, gasserian
neuralgia occurs in multiple sclerosis, it ganglion percutaneous techniques, and
may be bilateral in up to 30% of pa- gamma knife radiation therapy.7 The
tients.8,11 Thus, it is important to con- level of evidence for comparative effi-
sider a diagnosis of multiple sclerosis cacy and durability of these surgical pro-
in the patient who presents with bilateral cedures is low, as they have not been
trigeminal neuralgia, particularly if the subjected to randomized trials or well-
patient is relatively young or has other designed long-term studies.23
neurologic signs or symptoms. Ultrastruc- Microvascular decompression is the
tural studies have shown demyelination one procedure that uniquely addresses,
in the proximal centrally myelinated por- with the aim of reversing, the underly-
tion of the trigeminal root.13 ing neurovascular pathology, and it
The first line of therapy in the treat- appears to lead to the most enduring long-
ment of trigeminal neuralgia is carbamaz- term outcomes. This procedure carries
epine, which carries Level A evidence potential complications of cranial neu-
(Table 9-214Y16). Resolution of pain within ropathies, cerebellar hematoma or con-
a few days of beginning carbamaze- tusion, meningitis, or CSF leakage.8,24,25
1076 www.ContinuumJournal.com August 2015
Copyright American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
Percutaneous procedures reach the niques include radiofrequency thermoco-
gasserian ganglion via the foramen ovale agulation, injection of neurotoxins such as
and induce a partial injury. Available tech- alcohol or glycerol, or compression of the
a
TABLE 9-2 Pharmacologic Treatment of Trigeminal Neuralgia
Level of Common Adverse Serious Adverse
Evidenceb Drug Initial Dose Typical Dose Effectsc Effectsc
A Carbamazepined,e 100 mg 100Y200 mg Dizziness, nystagmus, Atrioventricular block,
2 times/d 3 times/d nausea, constipation, hepatotoxicity, bone
ataxia, fatigue, marrow suppression
drowsiness, blurry vision including aplastic anemia
or agranulocytosis,
Stevens-Johnson
syndrome, toxic epidermal
necrolysis, hyponatremia,
hypocalcemia, pancreatitis,
nephrotoxicity, multiorgan
hypersensitivity,
angioedema, suicidal
thoughtsc
B Oxcarbazepined,e 300 mg 600Y1200 mg Dizziness, nystagmus, Hyponatremia, erythema
2 times/d 2 times/d nausea, ataxia, fatigue, multiforme, Stevens-
drowsiness, blurry vision Johnson syndrome, toxic
epidermal necrosis,
anaphylaxis, bone marrow
suppression, suicidal
thoughts, angioedema
C Baclofen 5 mg 10Y20 mg Drowsiness, hypotension, Gastrointestinal
3 times/d 3 times/d constipation, nausea, hemorrhage, pneumonia,
hypotonia or muscle drug withdrawal seizures
weakness, fatigue, if stopped abruptly
dizziness
Gabapentind 100 mg 100Y900 mg Peripheral edema, Stevens-Johnson
3 times/d 3 times/d fatigue, drowsiness, syndrome, suicidal
dizziness, nausea, ataxia thoughts
Lamotrigined 25 mg every 50Y200 mg Rash, abdominal pain, Erythema multiforme,
other day 2 times/d diarrhea, nausea, Stevens-Johnson
dizziness, ataxia, syndrome, toxic
diplopia, insomnia, epidermal necrolysis,
headache, blurry vision, anemia, leukopenia,
anxiety, tremor, eosinophilia,
depression, rhinitis, disseminated intravascular
dysmenorrhea coagulation,
hepatotoxicity, aseptic
meningitis, drug
hypersensitivity syndrome,
neuroleptic malignant
syndrome, angioedema,
suicidal thoughts
Continued on page 1078
Continuum (Minneap Minn) 2015;21(4):10721085 www.ContinuumJournal.com 1077
Copyright American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
Cranial Neuralgias
a
TABLE 9-2 Pharmacologic Treatment of Trigeminal Neuralgia Continued from page 1077
Level of Common Adverse Serious Adverse
Evidenceb Drug Initial Dose Typical Dose Effectsc Effectsc
C Phenytoind 50 mg 300Y400 mg at Rash, gingival hyperplasia, Stevens-Johnson
3 times/d bedtime (single ataxia, dizziness, syndrome, toxic epidermal
nightly dosing refers nystagmus, nausea, necrolysis, systemic lupus
to the extended slurred speech, erythematosus, bullous
release form) confusion, drowsiness, dermatosis, bone
hirsutism, vitamin D marrow suppression
deficiency, blurred including agranulocytosis
vision/double vision or aplastic anemia,
hepatotoxicity,
nephrotoxicity, suicidal
thoughts
a
In general, the same pharmacologic strategy may be utilized when treating glossopharyngeal neuralgia and nervus intermedius neuralgia.
b
A = Established as effective, ineffective or harmful (or established as useful/predictive or not useful/predictive) for the given condition in
the specified population. (Level A rating requires at least two consistent Class I studies.) (In exceptional cases, one convincing Class I
study may suffice for an A recommendation if 1) all criteria are met, 2) the magnitude of effect is large [relative rate improved outcome 95
and the lower limit of the confidence interval is 92].)
B = Probably effective, ineffective or harmful (or probably useful/predictive or not useful/predictive) for the given condition in the specified
population. (Level B rating requires at least one Class I study or two consistent Class II studies.)
C = Possibly effective, ineffective or harmful (or possibly useful predictive or not useful/predictive) for the given condition in the
specified population. (Level C rating requires at least one Class II study or two consistent Class III studies.)
U = Data inadequate or conflicting; given current knowledge, treatment (test, predictor) is unproven.
c
Lists of potential adverse affects are incomplete and the prescribing physician should refer to the Physicians Desk Reference or its equivalent
for a complete list.
d
In 2008, on the basis of a meta-analysis, the US Food and Drug Administration (FDA) issued an alert warning that antiepileptic drugs in
general carry an increased risk for suicidality. Uncertainty whether those studies controlled adequately for relevant comorbidities has
caused some to question the strength of that association.14Y16 Since trigeminal neuralgia itself carries an increased risk for suicide, when
prescribing antiepileptic drugs for cranial neuralgia, the physician should inform the patient of the possible increased risk of suicidality
and assess the overall benefits versus risks of the drug.
e
The risk of serious and sometimes fatal dermatologic reactions to carbamazepine may be tenfold higher in patients of Asian ancestry who
have the HLA-B*1502 genotype.
ganglion with an inflatable balloon.22,26 radiation facial paresthesia and dyses-
All result in some degree of facial numb- thesia exists.27
ness or paresthesia and, especially follow- Motor cortex stimulation has shown
ing multiple procedures, can potentially initial promise in treating selected pa-
cause deafferentation pain, which is tients, not with trigeminal neuralgia but
termed anesthesia dolorosa. The bal- with severe medically intractable trigemi-
loon compression technique appears nal deafferentation pain, which can be
to have efficacy similar to that of the quite severe and, unlike the brief
others with less risk of corneal anes- paroxysmal pain of trigeminal neuralgia,
thesia or anesthesia dolorosa.26 is typically continuous and dull, aching, or
Gamma knife stereotactic radiation burning in quality.28 The procedure in-
therapy may be an appropriate inter- volves an open craniotomy and implan-
vention for patients unable to tolerate a tation of a strip of electrodes over the
surgical procedure. This technique targets motor cortex, connected to a subcutane-
the trigeminal nerve root entry zone at ously tunneled stimulator.
the level of the pons with ionizing radia- The role of surgical intervention in
tion. Reported outcomes have varied treating trigeminal neuralgia in patients
greatly, and a high incidence of post- with multiple sclerosis is less certain,
1078 www.ContinuumJournal.com August 2015
Copyright American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
KEY POINTS
especially when neurovascular com- HERPES ZOSTER h Unilateral eye pain
pression is not demonstrated.7,8 Varicella-zoster virus (VZV) is a ubiq- accompanied by Horner
uitous and highly neurotropic herpes- syndrome can be a clue
PARATRIGEMINAL virus that causes varicella (chickenpox) to carotid artery dissection.
OCULOSYMPATHETIC SYNDROME infection in children, after which the h Glossopharyngeal
(RAEDER SYNDROME) virus remains latent for decades in tri- neuralgia causes
Paratrigeminal oculosympathetic syn- geminal, dorsal root, and autonomic pharyngeal pain with
drome consists of constant unilateral ganglia. With age-related decline in cell- swallowing and may
pain in the distribution of the ophthal- mediated immunity or in immunocom- trigger reflex bradycardia
mic division of the trigeminal nerve promised patients, VZV may reactivate or syncope.
as herpes zoster (shingles), which pre- h Herpes zoster frequently
along with ipsilateral ptosis and miosis
sents with a painful vesicular cutaneous involves the trigeminal
(Horner syndrome). The pain is wors-
eruption typically in the distribution of nerve, 80% of the time
ened by eye movement and may ex-
a single dermatome. Pain may precede involving the ophthalmic
tend also to the maxillary division. This the emergence of rash by several days. division of this nerve,
clinical presentation is indicative of a Occasionally, herpes zoster may cause with the potential for
lesion in the carotid artery or middle dermatomal neuropathic pain in the visual impairment.
cranial fossa and should alert the neu- absence of a rash (zoster sine herpete).
rologist to the possibility of a carotid In such cases, evidence in support of a
artery dissection.29,30 viral basis has included the detection of
VZV DNA or intrathecal synthesis of anti-
GLOSSOPHARYNGEAL VZV IgG in CSF and pathologic findings
NEURALGIA of active viral ganglionitis.35 The inci-
Similar in quality to the pain of trigem- dence increases with age: 70% to 80%
inal neuralgia but less severe, glossopha- of herpes zoster occurs after the age of
ryngeal neuralgia affects the auricular 50. Groups at particular risk are patients
and pharyngeal branches of the vagus with transplanted organs, human immu-
nerve (cranial nerve X) and branches of nodeficiency virus (HIV), lymphoma, or
tuberculosis. The age-adjusted incidence
the glossopharyngeal nerve (cranial nerve
of herpes zoster is approximately 3.9 and
IX). The incidence of glossopharyngeal
3.2 per 1000 person-years for women and
neuralgia is 0.2 to 0.8 per 100,000 person-
men, respectively, and the lifetime risk of
years.2,5,31 It may coexist with trigem-
herpes zoster is estimated at 30%.36,37
inal neuralgia. Herpes zoster affects the trigeminal
Patients report unilateral pain deep nerve in 8% to 28% of cases, 80% of
in the pharynx, posterior aspect of the which occur in the ophthalmic division
tongue, or ear that is triggered by swal- (herpes zoster ophthalmicus). This is in
lowing.32 Paroxysms of pain may cause contrast to trigeminal neuralgia, which
reflex bradycardia or syncope. Some pa- involves the ophthalmic division in less
tients will also manifest coughing, diffi- than 5% of cases.37,38 In addition to pain,
culty with swallowing, or hoarseness. herpes zoster eye involvement can lead
Pharmacologic treatment is similar to that to ptosis, keratitis, uveitis, iritis, conjunc-
for trigeminal neuralgia. tivitis, or acute retinal necrosis with the
In some cases, MRI has shown vagal potential for permanent visual loss in
neurovascular compression, which re- nearly 7%.39
sponded to microvascular decompres- The pain of herpes zoster ophthalmicus
sion.33 Recurrent refractory syncope may is typically multimodal, with burning,
require placement of a cardiac pacemaker shooting, stabbing, aching, tingling, prick-
in some patients.34 ling, and itching components (Case 9-2).
Continuum (Minneap Minn) 2015;21(4):10721085 www.ContinuumJournal.com 1079
Copyright American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
Cranial Neuralgias
KEY POINTS
h Postherpetic neuralgia
occurs in more than
Case 9-2
A 72-year-old woman sought neurologic evaluation for pain in the forehead.
40% of patients older
Symptoms began 1 month previous with a burning sensation that she initially
than 60 years of age
thought was sunburn, but it affected only the right side. Two days later, blisters
following acute
erupted in the same area, and the headache intensified with sharp, throbbing,
herpes zoster.
stinging, and tingling components. She was seen at an urgent care clinic and
h Nervus intermedius given valacyclovir 1 g orally 3 times a day for 1 week and hydrocodone 10 mg
neuralgia typically 4 times a day. Her pain gradually subsided from 10/10 to 6/10 in intensity, but
causes sharp pain felt was worsened by wearing reading glasses or by anything that touched the right
deep in the ear canal. eyebrow, forehead, or lateral aspect of the nose. Her past medical history was
remarkable only for hypertension. She reported that she had been under some
stress recently, caring for a terminally ill family member. Neurologic examination
showed 20/20 visual acuity in each eye. Facial sensory examination was abnormal
with patchy hyperesthesia involving the ophthalmic division of the right
trigeminal nerve.
Comment. This is a typical presentation for herpes zoster ophthalmicus.
It is important to consider herpes zoster ophthalmicus in the differential
diagnosis of new-onset unilateral frontal or temporal headache in the
elderly patient, as a rash may not be present initially.
Cutaneous allodynia is frequently pres- of the trigeminal nerve that persists or
ent. Antiviral drugs, such as valacyclovir recurs for at least 3 months.2 This pain can
or famciclovir, have been shown to accel- be difficult to treat. First-line treatments
erate healing of the rash and shorten the include tricyclics, gabapentin, pregabalin,
duration of pain and are US Food and and topical lidocaine. Second- and third-
Drug Administration (FDA) approved for line treatments include opioids, tramadol,
treatment of acute herpes zoster. Severely and topical capsaicin (Table 9-3).42
affected or neurologically complex pa- Preventive efforts by vaccination are
tients may require IV acyclovir.35 Whereas showing promise. Herpes zoster vaccine
antiviral agents have been shown to de- administered to adults older than 60 years
crease zoster-associated pain during the of age is 51% effective for prevention of
first few weeks,40 strong evidence indi- zoster and 66% effective for prevention
cates that antiviral agents do not reduce of postherpetic neuralgia, although ef-
the incidence of postherpetic neuralgia.41 ficacy beyond 5 years is uncertain.43,44
Geniculate zoster involving cranial
nerve VII presents with ipsilateral facial NERVUS INTERMEDIUS
palsy and sometimes painful vesicles in NEURALGIA
the external auditory canal, anterior two- Also known as geniculate neuralgia, ner-
thirds of the tongue, or hard palate vus intermedius neuralgia is a very rare
(Ramsay Hunt syndrome). Herpes zos- disorder in which pain arises from the
ter can involve any of the other cranial sensory branch of the facial nerve (cra-
nerves acutely or in the days and weeks nial nerve VII), which innervates the
that follow the rash.35 external auditory meatus, pinna, and a
More than 40% of patients older than small area of skin below the ear lobe.
60 years of age with acute herpes zoster Patients present with paroxysmal unilat-
will experience chronic pain. Postherpetic eral sharp or stabbing pain deep in the
trigeminal neuropathy is a form of post- auditory canal triggered by swallowing,
herpetic neuralgia defined as pain caused speaking, or stimulation of the posterior
by herpes zoster in one or more branches wall of the auditory canal. The pain may
1080 www.ContinuumJournal.com August 2015
Copyright American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
TABLE 9-3 Pharmacologic Treatment of Postherpetic Neuralgia
Level of Common Adverse Serious Adverse
Evidencea Drug Typical Dose Effectsb Effectsb
A Lidocaine 5% 1Y3 patches Paresthesia or skin Systemic effects such as
applied topically irritation at the hypotension or bradycardia
for up to 12 out application site are unlikely with appropriate
of 24 hours use of the patch
Nortriptyline or 10Y75 mg at Constipation, dry mouth, Prolonged QT interval,
amitriptyline bedtime weight gain, dizziness heart block, myocardial
infarction, paralytic ileus,
hyponatremia, bone
marrow depression,
increased intraocular
pressure, depression,
urinary retention
Gabapentin 100Y900 mg Peripheral edema, Stevens-Johnson
3 times/d fatigue, drowsiness, syndrome, suicidal
dizziness, nausea, ataxia thoughts
Pregabalin 75Y300 mg Peripheral edema, weight Hepatotoxicity, increased
2 times/d gain, constipation, dry creatine kinase, suicidal
mouth, fatigue, dizziness, thoughts, angioedema
ataxia, blurry vision,
disturbance in thinking,
nasopharyngitis
B Opioids (eg, hydrocodone, Oral or topical, Constipation, nausea, Confusion, hypotension,
oxycodone, morphine, titrate based on pruritus, dizziness, peripheral edema,
hydromorphone, pain response somnolence, headache, prolonged QT interval
methadone, fentanyl) and side effects difficulty swallowing, (particularly for
tremor methadone), respiratory
depression, urinary
retention, serotonin
syndrome (when combined
with other drugs that
increase serotonin levels)
Tramadol 25Y100 mg Flushing, pruritus, Myocardial infarction,
4 times/d constipation, nausea, pancreatitis, anaphylaxis,
dizziness, headache, seizure, dyspnea,
insomnia, somnolence serotonin syndrome
C Capsaicin Single 1-hour Erythema, pain, nausea Hypertension, blistering
application of
8% patch every
3 months
a
A = Established as effective, ineffective or harmful (or established as useful/predictive or not useful/predictive) for the given condition in
the specified population. (Level A rating requires at least two consistent Class I studies.) (In exceptional cases, one convincing Class I
study may suffice for an A recommendation if 1) all criteria are met, 2) the magnitude of effect is large [relative rate improved
outcome 95 and the lower limit of the confidence interval is 92].)
B = Probably effective, ineffective or harmful (or probably useful/predictive or not useful/predictive) for the given condition in the specified
population. (Level B rating requires at least one Class I study or two consistent Class II studies.)
C = Possibly effective, ineffective or harmful (or possibly useful predictive or not useful/predictive) for the given condition in the specified
population. (Level C rating requires at least one Class II study or two consistent Class III studies.)
U = Data inadequate or conflicting; given current knowledge, treatment (test, predictor) is unproven.
b
Lists of potential adverse affects are incomplete and the prescribing physician should refer to the Physicians Desk Reference or its equivalent
for a complete list.
Continuum (Minneap Minn) 2015;21(4):10721085 www.ContinuumJournal.com 1081
Copyright American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
Cranial Neuralgias
KEY POINTS
h Persistent idiopathic also extend to the auricle, facial mus- BURNING MOUTH SYNDROME
facial pain (formerly culature, and over the parieto-occipital Related to persistent idiopathic facial
termed atypical facial region, as well as to the palate and pain is burning mouth or burning tongue
pain) may be difficult to tongue, but unlike the pain of glos- syndrome. This condition occurs in 5 to
treat because of central sopharyngeal neuralgia is not triggered 10 per 100,000 population, most commonly
sensitization and by swallowing.2,38 Nervus intermedius in middle-aged and elderly women.47
psychological comorbidity. neuralgia may develop as a complication Burning mouth syndrome is frequently
h Granulomatous of herpes zoster. Impaired lacrimation, idiopathic, although some patients have
inflammation of the orbit, salivation, or taste may occur. chronic hyposalivation, which may be
superior orbital fissure, Treatment is similar to that for tri- induced by anticholinergic medication
or cavernous sinus presents geminal neuralgia, with the first line or Sjogren syndrome. The differential
with unilateral orbital pain of treatment being carbamazepine. diagnosis also includes vitamin B12 de-
with ophthalmoplegia. Gabapentin, lamotrigine, and tricyclics ficiency, oral candidiasis, and lichen planus.
have brought improvement to some pa- Lubricating oral rinses may be helpful.
tients. For patients in whom medical
therapy has failed, anecdotal reports of HEADACHE WITH
successful surgical treatments include OPHTHALMOPLEGIA
transection of the nervus intermedius, (TOLOSA-HUNT SYNDROME)
microvascular decompression of the Unilateral orbital pain accompanied by
nervus intermedius, and extracranial in- ocular motor (cranial nerve III, IV, or VI)
fratemporal division of the cutaneous paresis should arouse strong suspicion
branches of the facial nerve.45,46 for a structural lesion. This is the char-
acteristic presentation of Tolosa-Hunt
PERSISTENT IDIOPATHIC syndrome, which is caused by granulo-
FACIAL PAIN matous inflammation in the orbit, su-
Previously termed atypical facial pain, perior orbital fissure, or cavernous sinus,
persistent idiopathic facial pain refers to and may be the presenting symptom of
the clinical syndrome of continuous or neurosarcoidosis.48 MRI may disclose a
daily recurring facial or oral pain in the focal enhancing mass.49 The granulo-
absence of a clinical neurologic deficit. matous inflammation typically responds
Its presentations are highly variable. well to corticosteroids. Other potential
The pain may be unilateral or bilateral, etiologies include orbital tumors, cavern-
regional, diffuse, superficial, deep, or ous carotid aneurysm, carotid-cavernous
fistula, carotid dissection, vasculitis, men-
poorly localized. Patients may report pain
ingitis, and diabetes mellitus.2,50
that is dull, nagging, burning, or aching.
This pain may follow minor or insignifi- OPTIC NEURITIS
cant facial trauma or dental procedures
Pain behind one or both eyes, which may
and frequently is associated with psycho-
be worse with eye movement, accompa-
logical comorbidity and psychosocial
nied by impaired visual acuity may signal
disability.2 Clinical management can
optic neuritis, which is caused by demy-
be very difficult.
elination of the optic nerve. Optic neuri-
The evaluation of persistent idiopathic
tis can occur as an isolated syndrome
facial pain should assess for a possible or as a manifestation of either multiple
underlying connective tissue disorder, sclerosis51 or neuromyelitis optica.52
such as mixed connective tissue disorder, Diagnostic evaluation includes dilated
scleroderma, sarcoidosis, or Sjogren syn- funduscopic examination, MRI of the
drome. Cranial imaging is required when brain and orbits, and CSF analysis. Op-
focal neurologic deficits are found. tical coherence tomography is useful to
1082 www.ContinuumJournal.com August 2015
Copyright American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
KEY POINT
measure retinal axonal loss. Treatment REFERENCES h Because of central
with high-dose corticosteroids shortens 1. Gray H. Anatomy of the human body.
convergence of trigeminal
the time of acute visual impairment but Philadelphia, PA: Lea & Febiger, 1918.
and cervical innervation,
does not affect the final visual outcome.53 2. Headache Classification Committee of the occipital neuralgia
International Headache Society (IHS). The may radiate pain to
international classification of headache
OCCIPITAL NEURALGIA disorders, 3rd edition (beta version).
the ipsilateral
Occipital neuralgia can arise from the Cephalalgia 2013;33(9):629Y808. fronto-orbital region.
greater occipital nerve, which originates doi:10.1177/0333102413485658.
from the dorsal ramus of C2, or from 3. van Hecke O, Austin SK, Khan RA, et al.
the lesser occipital or third occipital nerves, Neuropathic pain in the general population:
a systematic review of epidemiological
which originate from C2 and C3 in the studies. Pain 2014;155(4):654Y662.
cervical plexus.54 The pain is unilateral doi:10.1016/j.pain.2013.11.013.
in 85% of patients, who may present with 4. Hall GC, Carroll D, Parry D, McQuay HJ.
paroxysmal pain associated with dyses- Epidemiology and treatment of neuropathic
thesia or allodynia in the posterior scalp. pain: the UK primary care perspective. Pain
2006;122(1Y2):156Y162. doi:10.1016/j.pain.
The paroxysms are shooting or stabbing 2006.01.030.
in quality and last from seconds to min-
5. Katusic S, Williams DB, Beard CM, et al.
utes. In some cases the pain may radiate Epidemiology and clinical features of
to the ipsilateral fronto-orbital region be- idiopathic trigeminal neuralgia and
cause of trigeminocervical interneuro- glossopharyngeal neuralgia: similarities
and differences, Rochester, Minnesota,
nal connections in the trigeminal spinal 1945Y1984. Neuroepidemiology 1991;
nuclei. Physical examination may disclose 10(5Y6):276Y281.
tenderness over the affected nerve 6. Mueller D, Obermann M, Yoon MS, et al.
branches, in which case the diagnosis Prevalence of trigeminal neuralgia and
is confirmed by temporary relief of pain persistent idiopathic facial pain: a
population-based study. Cephalalgia
by injection of local anesthetic.2,55,56 2011;31(15):1542Y1548. doi:10.1177/
Anesthetic block of the greater or lesser 0333102411424619.
occipital nerves combined with injection
7. Gronseth G, Cruccu G, Alksne J, et al. Practice
of a corticosteroid is efficacious in the parameter: the diagnostic evaluation and
majority of patients.55 Conservative in- treatment of trigeminal neuralgia (an
terventions, such as warm or cold com- evidence-based review): report of the Quality
Standards Subcommittee of the American
presses, massage, and physical therapy Academy of Neurology and the European
directed to improving posture, may also Federation of Neurological Societies.
be helpful. Nonsteroidal anti-inflammatory Neurology 2008;71(15):1183Y1190.
doi:10.1212/01.wnl.0000326598.83183.04.
medications, muscle relaxants, tricyclics,
and gabapentin have been reported to 8. Cheshire WP. Trigeminal neuralgia: for one
nerve a multitude of treatments. Expert
be helpful.55 Limited evidence suggests Rev Neurother 2007;7(11):1565Y1579.
that implanted occipital nerve stimula- doi:10.1586/14737175.7.11.1565.
tors may be effective in some patients 9. Cheshire WP. Can MRI distinguish injurious
refractory to standard treatments.57 from innocuous trigeminal neurovascular
contact? J Neurol Neurosurg Psychiatry
2005;76(11):1470Y1471. doi:10.1136/jnnp.
CONCLUSION 2005.072595.
Cranial neuralgias can be very challeng-
10. Granata F, Vinci SL, Longo M, et al.
ing problems. A thorough organized clin- Advanced virtual magnetic resonance
ical approach is essential to reaching a imaging (MRI) techniques in neurovascular
specific diagnosis, on which depend ef- conflict: bidimensional image fusion
and virtual cisternography. Radiol Med
fective disease-specific pharmacologic or, 2013;118(6):1045Y1054. doi:10.1007/
when indicated, surgical interventions. s11547-013-0928-9.
Continuum (Minneap Minn) 2015;21(4):10721085 www.ContinuumJournal.com 1083
Copyright American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
Cranial Neuralgias
11. De Santi L, Annunziata P. Symptomatic cranial outcome in the surgical management
neuralgias in multiple sclerosis: clinical of trigeminal neuralgia. J Neurol Surg B
features and treatment. Clin Neurol Skull Base 2013;74(2):75Y81.
Neurosurg 2012;114(2):101Y107. doi:10.1016/ doi:10.1055/s-0033-1333617.
j.clineuro.2011.10.044.
23. Zakrzewska JM, Akram H. Neurosurgical
12. Cruccu G, Biasiotta A, Di Rezze S, et al. interventions for the treatment of trigeminal
Trigeminal neuralgia and pain related to neuralgia. Cochrane Database Syst Rev
multiple sclerosis. Pain 2009;143(3):186Y191. 2011;(9):CD007312. doi:10.1002/14651858.
doi:10.1016/j.pain.2008.12.026. CD007312.pub2.
13. Love S, Gradidge T, Coakham HB. Trigeminal
24. Oesman C, Mooij JJ. Long-term follow-up of
neuralgia due to multiple sclerosis:
microvascular decompression for trigeminal
ultrastructural findings in trigeminal
neuralgia. Skull Base 2011;21(5):313Y322.
rhizotomy specimens. Neuropathol Appl
doi:10.1055/s-0031-1284213.
Neurobiol 2001;27(3):238Y244. doi:10.1046/
j.0305-1846.2001.00318.x. 25. Sekula RF Jr, Frederickson AM, Jannetta PJ,
14. Hesdorffer DC, Berg AT, Kanner AM. An et al. Microvascular decompression for
update on antiepileptic drugs and suicide: elderly patients with trigeminal neuralgia:
are there definitive answers yet? Epilepsy a prospective study and systematic review
Curr 2010;10(6):137Y145. doi:10.1111/j. with meta-analysis. J Neurosurg 2011;114(1):
1535-7511.2010.01382.x. 172Y179. doi:10.3171/2010.6.JNS10142.
15. Siamouli M, Samara M, Fountoulakis KN. 26. Stomal-Slowinska M, Slowinski J, Lee TK,
Is antiepileptic-induced suicidality a et al. Correlation of clinical findings and
data-based class effect or an exaggeration? results of percutaneous balloon compression
A comment on the literature. Harv Rev for patients with trigeminal neuralgia. Clin
Psychiatry 2014;22(6):379Y381. doi:10.1097/ Neurol Neurosurg 2011;113(1):14Y21.
HRP.0000000000000039. doi:10.1016/j.clineuro.2010.08.005.
16. Bell GS, Mula M, Sander JW. Suicidality in 27. Yen CP, Schlesinger D, Sheehan JP. Gamma
people taking antiepileptic drugs: what KnifeA radiosurgery for trigeminal
is the evidence? CNS Drugs 2009;23(4): neuralgia. Expert Rev Med Devices
281Y292. 2011;8(6):709Y721. doi:10.1586/erd.11.46.
17. Cheshire WP. Fosphenytoin: an intravenous 28. Esfahani DR, Pisansky MT, Dafer RM,
option for the management of acute Anderson DE. Motor cortex stimulation:
trigeminal neuralgia crisis. J Pain Symptom functional magnetic resonance
Manage 2001;21(6):506Y510. doi:10.1016/ imaging-localized treatment for three
S0885-3924(01)00269-X. sources of intractable facial pain.
18. Cheshire WP Jr. Defining the role for J Neurosurg 2011;114(1):189Y195.
gabapentin in the treatment of trigeminal doi:10.3171/2010.5.JNS091696.
neuralgia: a retrospective study. J Pain 29. Solomon S, Lustig JP. Benign Raeders syndrome
2002;3(2):137Y142. doi:10.1054/jpai. is probably a manifestation of carotid artery
2002.122944. disease. Cephalalgia 2001;21(1):1Y11.
19. Hu Y, Guan X, Fan L, et al. Therapeutic doi:10.1046/j.1468-2982.2001.00139.x.
efficacy and safety of botulinum toxin type 30. Salvesen R. Raeders syndrome. Cephalalgia
A in trigeminal neuralgia: a systematic 1999;19(suppl 25):42Y45.
review. J Headache Pain 2013;14:72.
doi:10.1186/1129-2377-14-72. 31. Koopman JS, Dieleman JP, Huygen FJ, et al.
Incidence of facial pain in the general
20. Wu CJ, Lian YJ, Zheng YK, et al. Botulinum population. Pain 2009;147(1Y3):122Y127.
toxin type A for the treatment of trigeminal doi:10.1016/j.pain.2009.08.023.
neuralgia: results from a randomized,
double-blind, placebo-controlled trial. 32. Shephard MK, Macgregor EA, Zakrzewska JM.
Cephalalgia 2012;32(6):443Y450. doi:10.1177/ Orofacial pain: a guide for the headache
0333102412441721. physician. Headache 2014;54(1):22Y39.
doi:10.1111/head.12272.
21. Zhang J, Yang M, Zhou M, et al.
Non-antiepileptic drugs for trigeminal 33. Gaul C, Hastreiter P, Duncker A, Naraghi R.
neuralgia. Cochrane Database Syst Rev Diagnosis and neurosurgical treatment of
2013;(12):CD004029. doi:10.1002/14651858. glossopharyngeal neuralgia: clinical findings
and 3-D visualization of neurovascular
CD004029.pub4.
compression in 19 consecutive patients.
22. Ammori MB, King AT, Siripurapu R, et al. J Headache Pain 2011;12(5):527Y534.
Factors influencing decision-making and doi:10.1007/s10194-011-0349-x.
1084 www.ContinuumJournal.com August 2015
Copyright American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
34. Esaki T, Osada H, Nakao Y, et al. Surgical J Laryngol Otol 2014;128(5):394Y399.
management for glossopharyngeal neuralgia doi:10.1017/S0022215114000802.
associated with cardiac syncope: two case
reports. Br J Neurosurg 2007;21(6):599Y602. 46. Tubbs RS, Mosier KM, Cohen-Gadol AA.
doi:10.1080/02688690701627138. Geniculate neuralgia: clinical, radiologic,
and intraoperative correlates. World
35. Gilden D, Nagel MA, Cohrs RJ, Mahalingam R. Neurosurg 2013;80(6):e353Ye357.
The variegate neurological manifestations doi:10.1016/j.wneu.2012.11.053.
of varicella zoster virus infection. Curr Neurol
Neurosci Rep 2013;13(9):374. doi:10.1007/ 47. Sun A, Wu KM, Wang YP, et al. Burning mouth
s11910-013-0374-z. syndrome: a review and update. J Oral Pathol
Med 2013;42(9):649Y655. doi:10.1111/jop.12101.
36. Yawn BP, Gilden D. The global epidemiology of
herpes zoster. Neurology 2013;81(10):928Y930. 48. Curone M, Tullo V, Peccarisi C, et al. Headache
doi:10.1212/WNL.0b013e3182a3516e. as presenting symptom of neurosarcoidosis.
37. Borkar DS, Tham VM, Esterberg E, et al. Neurol Sci 2013;34(suppl 1):183Y185.
Incidence of herpes zoster ophthalmicus: doi:10.1007/s10072-013-1423-8.
results from the Pacific Ocular Inflammation 49. Jain R, Sawhney S, Koul RL, Chand P. Tolosa-Hunt
Study. Ophthalmology 2013;120(3):451Y456. syndrome: MRI appearances. J Med Imaging
doi:10.1016/j.ophtha.2012.09.007. Radiat Oncol 2008;52(5):447Y451.
38. Hupp WS, Firriolo FJ. Cranial neuralgias. doi:10.1111/j.1440-1673.2008.01988.x.
Dent Clin North Am 2013;57(3):481Y495. 50. Gladstone JP. An approach to the patient
doi:10.1016/j.cden.2013.04.009. with painful ophthalmoplegia, with a focus
39. Yawn BP, Wollan PC, St Sauver JL, Butterfield LC. on Tolosa-Hunt syndrome. Curr Pain
Herpes zoster eye complications: rates and Headache Rep 2007;11(4):317Y325.
trends. Mayo Clinic Proc 2013;88(6):562Y570.
51. Brownlee WJ, Miller DH. Clinically isolated
doi:10.1016/j.mayocp.2013.03.014. syndromes and the relationship to multiple
40. McDonald EM, de Kock J, Ram FS. Antivirals sclerosis. J Clin Neurosci 2014;21(12):2065Y2071.
for management of herpes zoster including doi:10.1016/j.jocn.2014.02.026.
ophthalmicus: a systematic review of high-quality
randomized controlled trials. Antivir Ther 52. Bradl M, Kanamori Y, Nakashima I, et al. Pain in
neuromyelitis opticaVprevalence, pathogenesis
2012;17(2):255Y264. doi:10.3851/IMP2011.
and therapy. Nat Rev Neurol 2014;10(9):529Y536.
41. Chen N, Li Q, Yang J, et al. Antiviral treatment doi:10.1038/nrneurol.2014.129.
for preventing postherpetic neuralgia.
Cochrane Database Syst Rev 2014;2:CD006866. 53. Toosy AT, Mason DF, Miller DH. Optic neuritis.
doi:10.1002/14651858.CD006866.pub3. Lancet Neurol 2014;13(1):83Y99. doi:10.1016/
S1474-4422(13)70259-X.
42. Johnson RW, Rice AS. Clinical practice.
Postherpetic neuralgia. N Engl J Med 54. Cesmebasi A, Muhleman MA, Hulsberg P, et al.
2014;371(16):1526Y1533. doi:10.1056/ Occipital neuralgia: anatomic considerations.
NEJMcp1403062. Clin Anat 2014;28(1):101Y108. doi:10.1002/
ca.22468.
43. Oxman MN, Levin MJ, Johnston GR, et al.; Shingles
Prevention Study Group. A vaccine to prevent 55. Dougherty C. Occipital neuralgia. Curr Pain
herpes zoster and postherpetic neuralgia in Headache Rep 2014;18(5):411. doi:10.1007/
older adults. N Engl J Med 2005;352(22):2271Y2284. s11916-014-0411-x.
doi:10.1056/NEJMoa051016.
56. Jurgens TP, Muller P, Seedorf H, et al. Occipital
44. Hales CM, Harpaz R, Ortega-Sanchez I, nerve block is effective in craniofacial
Bialek SR; Centers for Disease Control and neuralgias but not in idiopathic persistent
Prevention (CDC). Update on recommendations facial pain. J Headache Pain 2012;13(3):199Y213.
for use of herpes zoster vaccine. MMWR Morb doi:10.1007/s10194-012-0417-x.
Mortal Wkly Rep 2014;63(33):729Y731.
57. Jasper JF, Hayek SM. Implanted occipital
45. Tang IP, Freeman SR, Kontorinis G, et al. nerve stimulators. Pain Physician 2008;
Geniculate neuralgia: a systematic review. 11(2):187Y200.
Continuum (Minneap Minn) 2015;21(4):10721085 www.ContinuumJournal.com 1085
Copyright American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
Você também pode gostar
- Intralipid infusion for Myelin Sheath Repair in Multiple Sclerosis and Trigeminal Neuralgia?No EverandIntralipid infusion for Myelin Sheath Repair in Multiple Sclerosis and Trigeminal Neuralgia?Ainda não há avaliações
- Patel BellPalsy 01Documento7 páginasPatel BellPalsy 01ubayyumrAinda não há avaliações
- Neuromodulation in Headache and Facial Pain Management: Principles, Rationale and Clinical DataNo EverandNeuromodulation in Headache and Facial Pain Management: Principles, Rationale and Clinical DataGiorgio LambruAinda não há avaliações
- Chapter 8. Pain Pathways and Mechanisms of The Pulpodentin Complex - CompressedDocumento26 páginasChapter 8. Pain Pathways and Mechanisms of The Pulpodentin Complex - CompressedPaola cruzAinda não há avaliações
- Bell's Palsy: Aetiology, Clinical Features and Multidisciplinary CareDocumento8 páginasBell's Palsy: Aetiology, Clinical Features and Multidisciplinary CareMarsya Yulinesia LoppiesAinda não há avaliações
- Pathophysiology of Headache PDFDocumento2 páginasPathophysiology of Headache PDFJoshua Christian TopahAinda não há avaliações
- BellsPalsy JNNP 2015Documento8 páginasBellsPalsy JNNP 2015Marsya Yulinesia LoppiesAinda não há avaliações
- The Trigeminal (V) and Facial (Vii) CRANIAL NERVES: Head and FaceDocumento6 páginasThe Trigeminal (V) and Facial (Vii) CRANIAL NERVES: Head and FaceRiris SihotangAinda não há avaliações
- MuscleDocumento7 páginasMuscleasenamAinda não há avaliações
- Management of Peripheral Nerve Injuries: Basic Principles of Microneurosurgical RepairDocumento11 páginasManagement of Peripheral Nerve Injuries: Basic Principles of Microneurosurgical RepairPrasad AilamAinda não há avaliações
- Nihms 679297Documento21 páginasNihms 679297Irina HreniucAinda não há avaliações
- Migraine PatophysiologyDocumento21 páginasMigraine PatophysiologyReynard FebrianAinda não há avaliações
- (2015) Functional Neuroanatomy of Nociception and Pain-DikonversiDocumento20 páginas(2015) Functional Neuroanatomy of Nociception and Pain-DikonversiAnes ThesiaAinda não há avaliações
- Focal Peripheral NeuropathiesDocumento6 páginasFocal Peripheral NeuropathiesSeptia P. Mayasari100% (1)
- Trigeminal NerveDocumento11 páginasTrigeminal Nervekio josephAinda não há avaliações
- Cervicogenic HeadacheDocumento7 páginasCervicogenic HeadacheAnonymous GzRz4H50FAinda não há avaliações
- Mechanisms of Neuropathic PainDocumento14 páginasMechanisms of Neuropathic Painfahri azwarAinda não há avaliações
- Pain Classifitation 2 PDFDocumento11 páginasPain Classifitation 2 PDFAnnisa BrilianAinda não há avaliações
- The Nervus IntermediusDocumento5 páginasThe Nervus IntermediusDr. AtheerAinda não há avaliações
- AN C F P: EW Lassification For Acial AINDocumento4 páginasAN C F P: EW Lassification For Acial AINAkmal Niam FirdausiAinda não há avaliações
- Cervicogenic HeadacheDocumento7 páginasCervicogenic Headachemeta456Ainda não há avaliações
- Dores Neuropáticas CentraisDocumento5 páginasDores Neuropáticas CentraisRichard WooliteAinda não há avaliações
- 2023 12 760 JayaramanDocumento3 páginas2023 12 760 JayaramanGregorio Javier Carhuamaca LeónAinda não há avaliações
- Bloqueio de Nervos Cranianos para Tratamento Da CefaleiaDocumento13 páginasBloqueio de Nervos Cranianos para Tratamento Da CefaleiarflschalcherAinda não há avaliações
- Acc 61 - Supp2 96Documento7 páginasAcc 61 - Supp2 96intermediosamberesAinda não há avaliações
- Wilhour-Nahas2018 Article The NeuralgiasDocumento8 páginasWilhour-Nahas2018 Article The NeuralgiasCamilo Benavides BurbanoAinda não há avaliações
- Jurding NeuroDocumento6 páginasJurding NeuroAulia sabrina ramadhantyAinda não há avaliações
- Neuralgias of The Head: Occipital Neuralgia: ReviewDocumento10 páginasNeuralgias of The Head: Occipital Neuralgia: ReviewLuthfia PrasetiaAinda não há avaliações
- Trigeminal Neuralgia: D. LeclercqDocumento9 páginasTrigeminal Neuralgia: D. LeclercqHossam ThabetAinda não há avaliações
- Cranial Nerve Disorders: Ernest E. WangDocumento13 páginasCranial Nerve Disorders: Ernest E. Wangirsyad tsaniAinda não há avaliações
- J Clinph 2005 04 020Documento11 páginasJ Clinph 2005 04 020Andres Rojas JerezAinda não há avaliações
- Facial Neuralgias - ReviewDocumento12 páginasFacial Neuralgias - ReviewDr. AtheerAinda não há avaliações
- Anatomy, Physiology and Pharmacology of PainDocumento7 páginasAnatomy, Physiology and Pharmacology of PainpollodearrozAinda não há avaliações
- Neuroanatomical Correlation of The House-Brackmann Grading System in The Microsurgical Treatment of Vestibular SchwannomaDocumento23 páginasNeuroanatomical Correlation of The House-Brackmann Grading System in The Microsurgical Treatment of Vestibular SchwannomaAskarAinda não há avaliações
- Classificationand Differentialdiagnosisof OralandmaxillofacialpainDocumento14 páginasClassificationand Differentialdiagnosisof OralandmaxillofacialpainClaudiu CherciuAinda não há avaliações
- Neural Prolotherapy For NeuralgiaDocumento4 páginasNeural Prolotherapy For NeuralgiaMariel Yarrod100% (1)
- Dor NeuropaticaDocumento4 páginasDor NeuropaticaRoderley ReisAinda não há avaliações
- Neurophatic PainDocumento4 páginasNeurophatic PainicoanamareAinda não há avaliações
- Facial Nerve: From Anatomy To Pathology: F. ToulgoatDocumento10 páginasFacial Nerve: From Anatomy To Pathology: F. ToulgoatIman PradanaAinda não há avaliações
- Dolor PDFDocumento14 páginasDolor PDFBENITO SEVILLAAinda não há avaliações
- Acupuntura MTC 30Documento7 páginasAcupuntura MTC 30dougmatosAinda não há avaliações
- Dolor Facial PDFDocumento14 páginasDolor Facial PDFsebastian ochoaAinda não há avaliações
- Medicines: Pathological Mechanisms and Therapeutic Targets For Trigeminal Neuropathic PainDocumento16 páginasMedicines: Pathological Mechanisms and Therapeutic Targets For Trigeminal Neuropathic PainFKUPR 2017Ainda não há avaliações
- Central Mechanisms of Pathological PainDocumento9 páginasCentral Mechanisms of Pathological PainRocio DominguezAinda não há avaliações
- Finnerup Et Al 2020 Neuropathic Pain From Mechanisms To TreatmentDocumento44 páginasFinnerup Et Al 2020 Neuropathic Pain From Mechanisms To TreatmentintermediosamberesAinda não há avaliações
- Técnicas Neuroquirúrgicas IDocumento6 páginasTécnicas Neuroquirúrgicas ISociedad de Gerontología y Geriatría del PerúAinda não há avaliações
- Diagnosis and Management of Neuropathic ItchDocumento12 páginasDiagnosis and Management of Neuropathic ItchTony Miguel Saba SabaAinda não há avaliações
- TL 3Documento5 páginasTL 3ĐôngAinda não há avaliações
- 10 1056@NEJMra1914484Documento9 páginas10 1056@NEJMra1914484abhishekjha0082Ainda não há avaliações
- TL 2Documento5 páginasTL 2ĐôngAinda não há avaliações
- O R o F A C I A L P A I NDocumento15 páginasO R o F A C I A L P A I Nsherani999Ainda não há avaliações
- Clinical Review - FullDocumento5 páginasClinical Review - FullBenvenuto AxelAinda não há avaliações
- Neuropathic Orofacial PainDocumento10 páginasNeuropathic Orofacial PainDeema FlembanAinda não há avaliações
- Encephalitis and Brain Abscess Continuum 2021Documento32 páginasEncephalitis and Brain Abscess Continuum 2021geraldine paternina aguas100% (1)
- DRG in Chronic PainDocumento10 páginasDRG in Chronic PainDido KamelAinda não há avaliações
- Trigeminal Neuralgia Recent Approach in ClassificaDocumento9 páginasTrigeminal Neuralgia Recent Approach in ClassificaFKUPR 2017Ainda não há avaliações
- Facial Pain: Clinical Differential Diagnosis: ReviewDocumento11 páginasFacial Pain: Clinical Differential Diagnosis: ReviewsaswepakAinda não há avaliações
- Overview of Craniofacial Pain - UpToDateDocumento24 páginasOverview of Craniofacial Pain - UpToDateNana ShkodinaAinda não há avaliações
- Peripheral Nerve Repair and RegenerationDocumento15 páginasPeripheral Nerve Repair and RegenerationjaimeaquilesrinconAinda não há avaliações
- Pain After SCIDocumento20 páginasPain After SCIanjelikaAinda não há avaliações
- Trastornos Del Ritmo CircardianoDocumento38 páginasTrastornos Del Ritmo CircardianoHabib G. Moutran BarrosoAinda não há avaliações
- Trastornos RBD en Atrofia de Múltiples SistemasDocumento10 páginasTrastornos RBD en Atrofia de Múltiples SistemasHabib G. Moutran BarrosoAinda não há avaliações
- Tratamiento Farmacológico Trastornos Sueño REMDocumento24 páginasTratamiento Farmacológico Trastornos Sueño REMHabib G. Moutran BarrosoAinda não há avaliações
- Trastornos Del Sueño en AMSDocumento17 páginasTrastornos Del Sueño en AMSHabib G. Moutran BarrosoAinda não há avaliações
- REM - RBD ReviewDocumento8 páginasREM - RBD ReviewHabib G. Moutran BarrosoAinda não há avaliações
- Rapid Eye Movement Sleep Behaviour Disorder - ReviewDocumento10 páginasRapid Eye Movement Sleep Behaviour Disorder - ReviewHabib G. Moutran BarrosoAinda não há avaliações
- REM Sleep - ReviewDocumento4 páginasREM Sleep - ReviewHabib G. Moutran BarrosoAinda não há avaliações
- CNS Diseases and UveitisDocumento25 páginasCNS Diseases and UveitisHabib G. Moutran BarrosoAinda não há avaliações
- Neurologist Communicationg The Diagnosis of ELADocumento9 páginasNeurologist Communicationg The Diagnosis of ELAHabib G. Moutran BarrosoAinda não há avaliações
- The Best Evidence For Progressive Myoclonic Epilepsy - A Pathway To Precision TherapyDocumento11 páginasThe Best Evidence For Progressive Myoclonic Epilepsy - A Pathway To Precision TherapyHabib G. Moutran BarrosoAinda não há avaliações
- Approach To Neurologic InfectionsDocumento18 páginasApproach To Neurologic InfectionsHabib G. Moutran Barroso100% (1)
- Brain Injury After Cardiac Arrest - From Prognostication of Comatose Patients To RehabilitationDocumento12 páginasBrain Injury After Cardiac Arrest - From Prognostication of Comatose Patients To RehabilitationHabib G. Moutran BarrosoAinda não há avaliações
- POEMS Syndrome - A Report of 14 Cases and Review of The LiteratureDocumento6 páginasPOEMS Syndrome - A Report of 14 Cases and Review of The LiteratureHabib G. Moutran BarrosoAinda não há avaliações
- The Role of Diet in Multiple Sclerosis - A ReviewDocumento16 páginasThe Role of Diet in Multiple Sclerosis - A ReviewHabib G. Moutran BarrosoAinda não há avaliações
- Dementia, Autonomy, and Unexpected HappinessDocumento5 páginasDementia, Autonomy, and Unexpected HappinessHabib G. Moutran BarrosoAinda não há avaliações
- Afasia Primaria Progresiva y Apraxia Del Habla Continuum 2019Documento27 páginasAfasia Primaria Progresiva y Apraxia Del Habla Continuum 2019Habib G. Moutran BarrosoAinda não há avaliações
- Viva Questions For Even SemestersDocumento22 páginasViva Questions For Even SemestersSiddhanta DuttaAinda não há avaliações
- Design Report of STOL Transport AircraftDocumento64 páginasDesign Report of STOL Transport Aircrafthassan wastiAinda não há avaliações
- Mastering The Art of Self Hypnosis: by Dr. Kenneth GrossmanDocumento46 páginasMastering The Art of Self Hypnosis: by Dr. Kenneth GrossmanguilhermeosirisAinda não há avaliações
- Factors Influencing The Selection Of: MaterialsDocumento22 páginasFactors Influencing The Selection Of: MaterialsMaulik KotadiyaAinda não há avaliações
- Electronic Waste Essay LessonDocumento7 páginasElectronic Waste Essay LessonAna Carnero BuenoAinda não há avaliações
- Flexure Hinge Mechanisms Modeled by Nonlinear Euler-Bernoulli-BeamsDocumento2 páginasFlexure Hinge Mechanisms Modeled by Nonlinear Euler-Bernoulli-BeamsMobile SunAinda não há avaliações
- Marketing Plan Potato Food TruckDocumento25 páginasMarketing Plan Potato Food TruckAhasan h. ShuvoAinda não há avaliações
- Swot Ananlysis of Fintech CompaniesDocumento7 páginasSwot Ananlysis of Fintech CompaniesUyen Le VuAinda não há avaliações
- Study - Id23039 - Travel and Tourism in India Statista Dossier PDFDocumento60 páginasStudy - Id23039 - Travel and Tourism in India Statista Dossier PDFaashmeen25Ainda não há avaliações
- HGP Year End Report 2021-2022 NewDocumento169 páginasHGP Year End Report 2021-2022 Newangelica sungaAinda não há avaliações
- Syllabus Financial AccountingDocumento3 páginasSyllabus Financial AccountingHusain ADAinda não há avaliações
- Opening StrategyDocumento6 páginasOpening StrategyashrafsekalyAinda não há avaliações
- Prayer For Protection PDFDocumento3 páginasPrayer For Protection PDFtim100% (1)
- Ecosystems FYBCom PDFDocumento41 páginasEcosystems FYBCom PDFShouvik palAinda não há avaliações
- Kalsi P S - Organic Reactions and Their Mechanisms 5eDocumento26 páginasKalsi P S - Organic Reactions and Their Mechanisms 5eeasy BooksAinda não há avaliações
- Graph 1: Temperature,° C of Mixture 1 (Naoh-Hcl) Against Time Taken, (Min)Documento8 páginasGraph 1: Temperature,° C of Mixture 1 (Naoh-Hcl) Against Time Taken, (Min)LeeshaaLenee Paramanantha KumarAinda não há avaliações
- Akebono NVH White PaperDocumento4 páginasAkebono NVH White Paperapi-3702571100% (1)
- Product Management Software Director in Austin TX Resume Chad ThreetDocumento2 páginasProduct Management Software Director in Austin TX Resume Chad ThreetChad ThreetAinda não há avaliações
- Sears Canada: Electric DryerDocumento10 páginasSears Canada: Electric Dryerquarz11100% (1)
- Book2Chapter10 and 11 EvaluationDocumento55 páginasBook2Chapter10 and 11 EvaluationEmmanuel larbiAinda não há avaliações
- Personal Tutor: 11 + MATHS Test 6Documento10 páginasPersonal Tutor: 11 + MATHS Test 6siddhant4uAinda não há avaliações
- Axis Bank - Group 4Documento34 páginasAxis Bank - Group 4Deep Ghose DastidarAinda não há avaliações
- Data Sheet 6GK5213-3BB00-2TB2: Transfer RateDocumento6 páginasData Sheet 6GK5213-3BB00-2TB2: Transfer RateClaudiu VlasceanuAinda não há avaliações
- Lecture Notes 1 - Finance - Principles of Finance Lecture Notes 1 - Finance - Principles of FinanceDocumento7 páginasLecture Notes 1 - Finance - Principles of Finance Lecture Notes 1 - Finance - Principles of FinanceKim Cristian MaañoAinda não há avaliações
- Police Log September 24, 2016Documento14 páginasPolice Log September 24, 2016MansfieldMAPoliceAinda não há avaliações
- KC CVDocumento2 páginasKC CVVishal KeshriAinda não há avaliações
- Yusof Ishak Secondary School Humanities Study Tour Ho Chi Minh City, VietnamDocumento19 páginasYusof Ishak Secondary School Humanities Study Tour Ho Chi Minh City, Vietnamadamant751Ainda não há avaliações
- Install Sensor Lsi Fl061Documento14 páginasInstall Sensor Lsi Fl061AlterSon Grafi KalayAinda não há avaliações
- Student EssaysDocumento41 páginasStudent EssaysAsif RahmanAinda não há avaliações
- VtmsDocumento2 páginasVtmsLorenz YatcoAinda não há avaliações
- By the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsNo EverandBy the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsAinda não há avaliações
- ADHD is Awesome: A Guide to (Mostly) Thriving with ADHDNo EverandADHD is Awesome: A Guide to (Mostly) Thriving with ADHDNota: 5 de 5 estrelas5/5 (3)
- LIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionNo EverandLIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionNota: 4 de 5 estrelas4/5 (404)
- The Age of Magical Overthinking: Notes on Modern IrrationalityNo EverandThe Age of Magical Overthinking: Notes on Modern IrrationalityNota: 4 de 5 estrelas4/5 (32)
- Think This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeNo EverandThink This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeNota: 2 de 5 estrelas2/5 (1)
- The Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaNo EverandThe Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaNota: 4.5 de 5 estrelas4.5/5 (266)
- Love Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)No EverandLove Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)Nota: 3 de 5 estrelas3/5 (1)
- Summary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedNo EverandSummary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedNota: 4.5 de 5 estrelas4.5/5 (82)
- The Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsNo EverandThe Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsNota: 4 de 5 estrelas4/5 (4)
- Summary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisNo EverandSummary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisNota: 4.5 de 5 estrelas4.5/5 (42)
- Raising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsNo EverandRaising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsNota: 5 de 5 estrelas5/5 (1)
- The Obesity Code: Unlocking the Secrets of Weight LossNo EverandThe Obesity Code: Unlocking the Secrets of Weight LossNota: 4 de 5 estrelas4/5 (6)
- Manipulation: The Ultimate Guide To Influence People with Persuasion, Mind Control and NLP With Highly Effective Manipulation TechniquesNo EverandManipulation: The Ultimate Guide To Influence People with Persuasion, Mind Control and NLP With Highly Effective Manipulation TechniquesNota: 4.5 de 5 estrelas4.5/5 (1412)
- The Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeNo EverandThe Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeNota: 4.5 de 5 estrelas4.5/5 (254)
- The Marshmallow Test: Mastering Self-ControlNo EverandThe Marshmallow Test: Mastering Self-ControlNota: 4.5 de 5 estrelas4.5/5 (60)
- Summary: Limitless: Upgrade Your Brain, Learn Anything Faster, and Unlock Your Exceptional Life By Jim Kwik: Key Takeaways, Summary and AnalysisNo EverandSummary: Limitless: Upgrade Your Brain, Learn Anything Faster, and Unlock Your Exceptional Life By Jim Kwik: Key Takeaways, Summary and AnalysisNota: 5 de 5 estrelas5/5 (8)
- Dark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.No EverandDark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Nota: 4.5 de 5 estrelas4.5/5 (110)
- Why We Die: The New Science of Aging and the Quest for ImmortalityNo EverandWhy We Die: The New Science of Aging and the Quest for ImmortalityNota: 4 de 5 estrelas4/5 (5)
- To Explain the World: The Discovery of Modern ScienceNo EverandTo Explain the World: The Discovery of Modern ScienceNota: 3.5 de 5 estrelas3.5/5 (51)
- Summary: Thinking, Fast and Slow: by Daniel Kahneman: Key Takeaways, Summary & Analysis IncludedNo EverandSummary: Thinking, Fast and Slow: by Daniel Kahneman: Key Takeaways, Summary & Analysis IncludedNota: 4 de 5 estrelas4/5 (61)
- When the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisNo EverandWhen the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisNota: 3.5 de 5 estrelas3.5/5 (2)
- Cult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryNo EverandCult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryNota: 4 de 5 estrelas4/5 (46)