Escolar Documentos
Profissional Documentos
Cultura Documentos
Peripheral Vascular Medicine - Dr. Deduyo PDF
Enviado por
Medisina101Descrição original:
Título original
Direitos autorais
Formatos disponíveis
Compartilhar este documento
Compartilhar ou incorporar documento
Você considera este documento útil?
Este conteúdo é inapropriado?
Denunciar este documentoDireitos autorais:
Formatos disponíveis
Peripheral Vascular Medicine - Dr. Deduyo PDF
Enviado por
Medisina101Direitos autorais:
Formatos disponíveis
PERIPHERAL VASCULAR MEDICINE 2014 -2015
Dr. Deduyo CARDIOLOGY
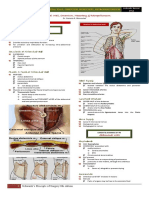
PERIPHERAL VASCULAR MEDICINE 35% - stable claudication
Definition 9% - chronic critical limb ischemia
a clinical disorder in which there is a stenosis or occlusion in 3% - acute limb ischemia
the aorta or arteries of the limbs
emboli or thrombus-> occlusion/stenotic -> blood flow is
compromised, pwedeng mag stuck sya,di nakapag flow ng
maayos ->results to manifestations of dec blood flow such
as ischemia -> claudications (leg pain)
Causes
Atherosclerosis patients >40 years old
Thromobosis
Embolus
Vascultits
Fibromuscular dysplasia Figure 1. PAD Statistics
Entrapment (Masmarami pa ang asymptomatic kaysa sa may
Cystic adventitial disease mga symptoms)
Trauma
Sixth and seventh decades of life The most common symptom is intermittent claudication
Patients with atheros of the coronary and defined as a pain, ache, cramp, numbness or a sense of
cerebral vasculature fatigue in the muscles; it occurs during exercise and is
relieved by rest
Increased risk of developing PAD in : o The site of claudication is distal to the location of
Cigarette smokers the occlusive lesion
DM Sumasakit ang legs on prolonged
Hypercholesterolemia walking tapos nawawala kapag
HPN nagpapahinga
Hyperhomocysteinemia o For example, buttocks, hip and thigh discomfort
occur in patients with aortoiliac dse, whereas calf
Pathology: claudication develops in px with femoral popliteal
Segmental lesions causing stenosis or occlusion dse.
are usually localized to large and medium sized Buttocks pain is least to be
vessels noticed,minsan akala UTI
Foot pain and leg pain are the MOST
The pathology of the lesion includes: COMMON MANIFESTATION in the
elderly, sometimes mistaken as arthritis
1. Atheros plaque with calcium deposition
2. Thinning of the media DIAGNOSIS
3. Patchy destruction of muscle and elastic fibers
4. Fragmentation of the internal elastic lamina I. HISTORY
5. Thrombi composed of platelets and fibrin Individuals with Asymptomatic PAD
Identified in order to offer therapeutic interventions
The primary sites of involvement: known to diminish their increased risk of MI, stroke and
death
1. Femoral and popliteal arteries (80-90% of px) A history of walking impairment, claudication and ischemic
2. The more distal vessels, including the tibial and peroneal arteries rest pain
(40-50% of px)
3. The abdominal aorta and iliac arteries (30% of symptomatic px) II. ROS
Atheros lesions occur preferentially: Recommended as a required component of a standard ROS for:
1. Adults >/ 50 yrs who have atheros R/F
1. Arterial branch points 2. Adults >/ 70 yrs
2. Sites of increased turbulence
3. Altered shear stress, and internal injury Key Components of the Vascular Review of Systems and Family
4. Involvement of the distal vasculature is most History
common I elderly individuals and px with DM 1. Any exertional limitation of the lower extremity
muscle or any hx of walking impairment
Manifestations of PAD o Claudication of this limitation:
Fatigue
53% - asymptomatic PAD Aching
o We need to identify this (since silent assassin ito) Numbness
o If patient has CAD+PAD -> worse prognosis Pain
o Patient has PAD+ CVD -> worse prognosis too
MagnoOpereSomnia Dura Page 1 of 14 STEF AND SHAY
PERIPHERAL VASCULAR MEDICINE 2014 -2015
Dr. Deduyo CARDIOLOGY
o Primary sites of discomfort Pag binaba, ok na ulit ang kulay ng paa,
Buttocks same color na
Thigh
Calf IV. LABORATORY
Foot
2. Any poor healing or nonhealing wounds of the legs or 1. Routine
feet a. CBC with platelets
3. Any pain at rest localized to the lower leg or foot and b. FBS
its assoc with the upright or recumbent position c. HBA1c levels
4. Postprandial abdominal pain that reproducibly is d. Renal fxn (BUN and creatinine)
provoked by eating and is assoc with weight loss e. Fasting lipid profile
5. Family hx of a first degree relative with an AAA f. UA (for microalbuminemia
g. 12 lead ECG
III. PE
V. HEMODYNAMIC NON-INVASIVE TESTING
Key components of the vascular PE a. Resting Ankle Brachial Index (ABI)
b. Exercise ABI
1. Measurement of BP in both arms and notation of any c. Segmental pressure exam
interim asymmetry d. Pulse volume recordings
2. Palpation of the carotid pulses and notation of the carotid
uprstroke and amplitude and presence of bruits 1. ANKLE BRACHIAL INDEX
3. Auscultation of the abdomen and flank for bruits
4. Palpation of the abdomen and notation for the presence of ***ABI =
aortic pulsation and its maximal diameter Lower extremity systolic pressure
5. Palpation of pulses at the brachial, radial, ulnar, femoral, Brachial artery systolic pressure
popliteal, dorsalis pedis and posterior tibial sites.
Performance of Allens test when knowledge of hand The ABI is 95% sensitive and 99% specific for PAD
perfusion is needed. Establishes the PAD dx
6. Auscultation of both femoral arteries for the presence of Identifies a pop at high risk of CV ischemic events
bruits Pop at risk can be clinically and epidemiologically defined:
7. Pulse intensity should be assessed and should be recorded o Exertional leg sx, non healing wounds, age >70
numerically as follows: years, age >50 years with hx of smoking and DM
o 0 - absent Toe brachial index (TBI) useful in individuals with non
o 1 diminished compressible pedal pulses
o 2 normal
o 3 bounding ABI Classification System (this is the new classification) Only used
8. The shoes and socks should be removed, the feet inspected, for prognosticating and staging of PAD:
the color, temp and integrity of the skin and intertriginous >1.4 incompressible
areas evaluated, and the presence of ulcerations recorded o Di na accurate ang ABI,present in DM and old age
9. Additional findings suggestive of severe PAD should o Calcified arteries present, abnormal vessel
be sought and recorded. This includes: o Get other important modalities
a. Distal hair loss 1.0-1.4 normal
b. Trophic skin changes 0.91 0.99 equivocal/borderline
c. Hypertrophic nails o Do an exercise ABI to unmask the PAD
0.70 0.90 mild to mod
MANIFESTATIONS OF SEVERE PAD 0.40 0.69 - mod to severe
<0.40 severe -> requires amputation (ito yung isasagot
Acute limb ischemia natin sa part ng management pag binigyan tayo ng case
Pain tapos ganito na ang ABI nya,so goodbye legs/paa )
Pallor
Pulselessness ** ABI alone can diagnose the patient. Get BP of the brachial artery of
Paresthesia both right and left and the BP of dorsalis pedis or posterior tibial
Paralysis artery r and l. Get the higher of both upper and lower ex and divide.
Polar Example: BP in upper ex R-130, L-120
Chronic limb ischemia Bp lower ex R-120 L-130
Sustained- severe decrease in blood flow in the legs which
if untreated would lead to pain even at rest, ulceration and ABI= 130/130 -> (1)
incipient limb loss ABI of 1 falls under the normal range
At elevation dependency test (like a straight leg test):
o Elevation- pallor results 2. EXERCISE ABI
Pag tinaas,asymmetric ang kulay ng paa Confirms the risk for PAD
o Dependent- rubor Done to unmask the PAD that is normal at rest pero after
exercise lumalabas
MagnoOpereSomnia Dura Page 2 of 14 STEF AND SHAY
PERIPHERAL VASCULAR MEDICINE 2014 -2015
Dr. Deduyo CARDIOLOGY
Assess the final severity of classification PROGNOSIS
Fall ABI after exercise
1/3 of patients with PAD have CAD
Over of CAD cases are confirmed by arteriography
Patients with PAD have 15-30% mortality rate in 5 years and
2-6x increase if present CAD
Mortality is highest in severe PAD
The likelihood of symptomatic progression of PAD appears
less than succumbing CAD (it only means mas ikinamamatay
talaga ang CAD kesa sa PAD)
Approx 70-80% of non DM patients with mild or moderate
claudications remain stable
25-30% of patients with critical limb ischemia will go
amputation within 1 year
Prognosis is worse if patient is SMOKING and those with DM
Figure 2. Natural History of PAD
3. HAND DOPPLER (not in the slide pero demonstrated by doc in
class, si Linuel yung subject.Remember? )
Easiest way to assess PAD
Normal arterial sound- rifling sound, TRIPHASIC
Flat sound- SUGGESTIVE of PAD
4. ARTERIAL DUPLEX SCAN
Detects areas of stenosis and blood flow
Normal: triphasic
Abnormal: absence of downward shift
Can visualize stenotic vessels
Figure 4. PAD Screening and algorithm
TREATMENT
Patient with PAD should receive therapies to
o Reduce the risk of associated CV events such as
MI and death
o Improve limb symptoms
o Prevent progression to critical limb ischemia
o Preserve limb viability
Risk factor modification and antiplatelet therapy should
be initiated to improve CV outcomes
BP control (ACE-I, B-blockers)
Treatment of hypercholesterolemia (statins, recommends
tx to reduce LDL, cholesterol to <100mg/dl )
Platelet inhibitors
o Aspirin sse: bleeding ->so do not give to px with
PUD. If given in px with PUD, give PPI muna then
aspirin
o Clodipogrel- proven MORE effective than aspirin
o Insufficient evidence if dual therapy (aspirin +
clodipogrel) is effective
Figure 3. Arterial duplex scan imaging and arteriography o Warfarin is NOT given because it does not
In the second picture, kita dito yung part na may stenosis and after improve outcome in patients with PAD
the part with stenosis, turbulent na yung blood flow. o Voraxapar
New drug
Dec limb ischemia but increases risk of
bleeding -> so it is not given in px with
bleeding disorders
MagnoOpereSomnia Dura Page 3 of 14 STEF AND SHAY
PERIPHERAL VASCULAR MEDICINE 2014 -2015
Dr. Deduyo CARDIOLOGY
Glycemic Control in DM patients
A. Diabetes control and complications trial
o Aggressive glycemic control resulted to dec
progression of carotid IMT
B. UKPDS subgroup study
o Reductaion in HBA1c by 7% resulted in 18%
reduction in MI, 15% reduction in stroke and
4.2% reduction in PAD
* lower HBA1C <6.5 -> leads to hypoglycaemia
Diabetes Treatment in PAD
o Intensive glycemic control
o HbA1c <7.0%
o No clear benefit on limb events Emerging therapies
o Naftidrofuryl
BP Control o Proprionyl levocarnitine
o L-arginine
1. ACE Inhibitor o Prostaglandins
Hope: Ramipril significantly reduced the rates of o Gene induced angiogenesis
death, MI and styroke in px at high risk for CV
events independent of antihypertensive impact ** Stem cell study conducted in India -> improves claudication but
2. Beta blockers does not decrease size of stenosis, just open up small collaterals, not
Do not aversely affect the walking capacity of the bigger vessels
intermittent claudication with mild to mod PAD
Newer modalities
Supportive measures o Long term parenteral administration of
vasodilating prostaglandins decreases pain and
1. Meticulous care of the feet, which should be kept facilitates healing of ulcer in px with chronic limb
clean and protected against excessive drying, apply ischemia
moisturizing creams. o Intramuscular transfer of DNA encoding
2. Well fitting and protective shoes are advised to endothelial GF, FGF, Hepatocyte GF or hypoxia
reduce trauma inducible factor 1 and also admin of endothelial
3. Elastic support hose should be avoided as they reduce progenitor cells, may promote collateral BV
BF to the skin growth in px with critical limb ischemia
4. Supervised exercise training programs for 30-45 mins
session, 3 to 5 times per week atleast 12 weeks, Revascularization
prolong walking distance o Catheter based surgical interventions are usually
5. Drugs such as: indicated for px with disabling, progressive or
a. Alpha adrenergic antagonist severe sx of intermittent claudication despite
b. CA channel blockers medical therapy and for those with critical limb
c. Papaverine and other vasodilators : effective ischemia
in px with PAD o Nonoperative interventions include PTCA, stent
d. placement and atherectomy
Cilostazol: a phosphodiesterase inhibitor with vasodilator and o PTA and stenting of iliac artery are associated
antiplatelet properties, increases claudication distance by 40-60% and with with higher success rates that PTA and
improves measures of quality of life stenting of femoral arteries
o 90-95% of iliac PTA are initially successful in the 3
Pentoxifylline: a substituted xanthine derivative, has been reported yr patency rate is >75%
to decrease blood viscosity and to increase red cell flexibility, thereby o Patency rates may be higher if placed in the iliac
increasing blood flow to the microcirculation and enhancing tissue artery. The initial success rates for femoral-
oxygenation popliteal PTA and stenting are approx 80%, with
60% 3 yr patency rate
Statins and propionyl-L-carnitine: a drug that affects skeletal muscle o Patency rates are influenced by pretreatment
metabolic fxn, appear promising for tx of intermittent claudication in stenoses, the prognosis of occlusive lesions is
initial clinical trial worse that nonocclusive lesions
o The role of drug eluting stents in PAD is helpful
** cilostazol + aspirin + clodipogrel -> can improve quality of walking o Operative procedures for aortoiliac dse are the ff
SE: headache, fluid retention Aortobifemoral bypass
If patient has CAD, give nitrates to relieve HEADACHES Axillofemoral bypass
If patient has CHF, do not give nitrates,give a diuretic first Femoral-femoral bypass
Aortoilac endarterectomy
MagnoOpereSomnia Dura Page 4 of 14 STEF AND SHAY
PERIPHERAL VASCULAR MEDICINE 2014 -2015
Dr. Deduyo CARDIOLOGY
*** PTA has higher success rates if artery is bigger.It is not Thrombosis
useful if we are going to target small vessels o No obvious cardiac source
Surgery is better option for small arteries o History of claudication
*** stents are used (metal) are used above the knee level o Abnormal pulses in the contralateral limb
Cotton stents are used if below the knee.If very small o Angiography: diffuse atherosclerosis with well
vessels, use the balloon developed collaterals
PROGNOSIS
ACUTE LIMB ISCHEMIA Amputation rate: 6-20%
6% if revascularized within 12 hours
Acute limb ischemia 12% if revascularized within 12-24 hours
Results from sudden cessation of blood flow to the 20% if revascularized after 24 hours
extremity. The severity of the ischemia and the viability of Mortality rate: 6-12%
the extremity depend on the location and the extent of
occlusion and the presence and subsequent development of HISTORY
collateral BV
2 principal causes of occlusion: History of claudication
o embolism thrombus in situ History of heart disease
from proximal sites of atherosclerosis Interventions for poor circulation
and aneurysm of the aorta and large Has other cardiovascular risk factors
vessels
arterial emboli tend to lodge at DIAGNOSIS
bifurcations ** ABI is not of use anymore
most frequently lodge in the femoral
artery, followed by the iliac artery, aorta 1. Physical examination
and popliteal and tibioperoneal arteries
o thrombus
entered the systemic circulation via a
patent foramen ovale or other septal
defect
INCIDENCE
Scanty information available
Estimate at 140 per 100,00
Decreased ALI incidence secondary embolism
Increase incidence of thrombotic acute limb ischemia
ETIOLOGY
Etiology of Arterial Occlusion
Thrombotic vs Embolic
o Embolic Sources
Cardiac- 75 %
Atrial Fibrillation- 51%
Acute Mi- 24%
o Non-Cardiac- 10%
Atheromathous Debris 5%
Aneurysmal 5%
Post CV Surgery 7%
2. Electrocardiogram
3.Standard chemistry
Emboli impact at branching points in arterial tree
4.Complete blood count
Femoral Artery 45%
5.Prothrombin time
Aorta and Iliac Artery -26%
6.Partial thromboplastin time
Poplitial Artery 15%
7.Creatinine phosphokinase level
Tibial Artery -1%
Hypercoagulable state will need additional studies
Clinical differentiation between thrombosis and embolism
Anticardiolipin antibodies
Embolism
Homocysteine concentration
o Obvious cardiac source
Antibody to platelet factor IV
o No history of claudication
o Normal pulses in the contralateral limb
o Angiography: may have minimal atherosclerosis
with few collateral noted
MagnoOpereSomnia Dura Page 5 of 14 STEF AND SHAY
PERIPHERAL VASCULAR MEDICINE 2014 -2015
Dr. Deduyo CARDIOLOGY
Arterial Doppler signals assess level of obstruction and severity of 1. Unfractionated heparin
ischemia
Pedal signals allow time for conventional arteriography and Intravenous heparin at full anticoagulant dosage should be
proper patient preparation given as soon as the diagnosis of acute limb ischemia has
ABI is not of value in acute ischemia been made,provided that heparin is not contraindicated
If it can be measured, the limb is not threatened Conventional Anticoagulation
o Unfractionated adjusted dose
IMAGING STUDIES o IV or subcutaneous Heparin
o Target PTT: 1.5 x control
1. Arteriography o Dosing: Bolus 80-100u/kg
Localize obstruction, visualize distal arterial tree o Drip 15-20 u/kg/h (Rashke Protocol)
Assists in distinguishing patients who will benefit more from o If HIT is present,do not give heparin
percutaneous treatment than from embolectomy or open 2. Analgesia- tramadol, morphine
revascularization procedures 3. Keep foot dependent
Patients with high clinical probability of embolic ischemia 4.Avoid heel pressure
DO NOT need angiography 5.Avoid extreme temperatures- no aircon muna
2. Computed topographic angiography (CTA) 6.Maximum tissue oxygenation
3. Magnetic resonance angiography (MRA) 7.Correct Hypotension- not to sacrifice peripheral veins, give
Diagnose and delineate disease extent inotropics
Advantage of speed, convenience, ability for cross-sectional 8. Treat other co-morbid conditions
imaging of vessel
TREATMENT
** identify first the level of acute ischemia because treatment is
based on the level of the dse
Figure 5. Algorithm of treatment for px with ALI.
Factors for consideration in choosing intervention for acute
limb ischemia
Choice as to which intervention should be used for
acute limb ischemia should be based on
o Location and anatomy of lesion
o Duration of acute limb ischemia
o Type of clot
o Patient-related risks
o Surgery-related risks
o Contraindications to thrombolysis
Pharmacologic thrombolysis
Treatment of choice if degree of severity allows time
i.e. severity levels I and IIa
Recent advances in endovascular devices and
techniques allow rapid clot removal
Permit treatment of more advanced degree of
** measure then the level of bleeding before giving drugs. After
ischemia
giving the drug measure the PTT. Once drug is given, measure PTT
Thrombolytic therapy reduces risk of endothelial
every 6 hours and it should reach >1.5
trauma & clot lysis in branch vessels too small for
MagnoOpereSomnia Dura Page 6 of 14 STEF AND SHAY
PERIPHERAL VASCULAR MEDICINE 2014 -2015
Dr. Deduyo CARDIOLOGY
embolectomy balloons Decrease hemorrhagic complications and improve
Systemic thrombolysis has no role in the treatment of outcome
patients with ALI Complications
Absolute Contraindications to pharmacologic thrombolysis o Hemolysis
o Established cerebrovascular event (excluding TIA o Possible renal failure secondary to release of
within previous 2 months) free haemoglobin
o Active bleeding diathesis Surgery
o Recent gastrointestinal bleeding (within previous For profoundly ischemic limb ( class IIb)
10 days) For profound sensory and motor deficits of very short
o Neurosurgery (intracranial, spinal) within previous duration
3 months o Revascularization completed within a few hours
o Intracranial trauma within previous 3 months after onset of severe symptoms may produce
remarkable recovery
Catheter-directed thrombolysis
Previously, urgency of treatment made surgery the treatment of
Intra-arterial medications: Urokinase, tPA, alteplase, choice in many cases
reteplas Injection technique variable
o Lacing In suprainguinal occlusion (no femoral pulse), open surgery
o Pulse-spray dosing may be the preferred choice of treatment
o Low continuous dose o E.g. large embolus in common proximal iliac
o May need 4-24 hrs of thrombolytics artery or distal aorta may most effectively be
o Intracranial hemorrhage rate: 1-2% treated with catheter embolectomy
Suprainguinal graft occlusion may best be treated with
Thrombolysis after arteriography in acute limb ischemia surgery
If the decision is made to proceed with thrombolysis Done if involved limb has no underlying atherosclerosis
afterarteriography, the intrathrombus infusion method Intraoperative assessment of adequacy of clot removal
should be used require
o Percutaneouos aspiration thrombolectomy (PAT) o completion angiography
and percutaneous mechanical thrombolectomy o Ultrasound-based methods
(PMT) Distal clot may be treated by intraoperative thrombolysis
PMT is the one to use if the thrombus is with instillation of high doses of thrombolytic agents for a
organized and if thrombus cannot be brief period followed by irrigation or additional passages of
aspirated anymore balloon catheter
o Alternative non-surgical modalities for ALI Repeat angiography followed by clinical & Doppler
o Combination with pharmacologic thrombolysis examination should be performed on the operating table
may substantially speed up clot lysis
Important in more advanced ALI where Limits of thromboembolectomy
time to revascularization is critical Leaves residual thrombus (35-85%)
Cannot clear branch vessel occlusion
Percutaneous aspiration thrombectomy (PAT) Causes endothelial injury
Uses thin-wall, large lumen catheters and suction with a Unless there is good evidence that adequate
50-ml syringe to remove embolus or thrombus from native circulation has been restored, intraoperative
arteries, bypass grafts and run-off vessels angiography should be performed to identify any
Adjunct to thrombolysis in acute arterial occlusion or can residual occlusion or critical arterial lesions requiring
be used as salvage therapy to remove distal emboli further treatment
Percutaneous aspiration thrombectomy as rapid and
effective way of removing thrombus in thromboembolic Studies regarding surgery as treatment (additional readings)
occlusions of the limb arteries below the inguinal ligament
and can be a very good alternative to surgery in selected 1. Rochester Series
patients. Prospective, randomized, single-center study with 114
patients
Percutaneous mechanical thrombectomy (PMT) Intra-arterial urokinase versus surgical revascularization
Hydrodynamic recirculation Results:
Efficiency depends mainly on age of thrombus o Outcome @12 months:
Fresh thrombus responds better than older organized clot o Lower 1-year amputation rate with thrombolytics
Small Clinical series have demonstrated short term (30 (16%) versus surgery (42%)
day) salvage of 80-90% Conclusion: Especially in medically compromised group, ALI
Only Angiojet MTD approved for peripheral arterial use of <7 days duration should receive thrombolytics
Ouriel K, Shortell CK, DeWeede JA et al J Vasc Surg 1994
Percutaneous mechanical thrombectomy (PMT) with thrombolysis
Reduce thrombus burden
Reduce length of time and total dose of thrombolytic
therapy
MagnoOpereSomnia Dura Page 7 of 14 STEF AND SHAY
PERIPHERAL VASCULAR MEDICINE 2014 -2015
Dr. Deduyo CARDIOLOGY
2. Surgery or Thrombolysis for the Ischemic Lower Extremity (STILE)
** amputation is done if there is increased bleeding in use of
Prospective, randomized, multi-center study with 393 anticoagulants. This could be done in stage I and II if there is
patients anticoagulant failure
Intra-arterial thrombolytics (r-TPA, urokinase) versus
surgical revascularization COMPARTMENT SYNDROME
Limb ischemia patients with symptom duration <6months
(mean duration was 6 weeks) not necessarily acute limb Increased pressure within a limited space compromise the
ischemia circulation and function of the tissues within that space -
Death and amputation rates similar in both groups Mates, 1980
First described by Malgaigne
3. SURGERY OR THROMBOLYSIS FOR THE ISCHEMIC LOWER First medical reference by Volkmann, 1881
EXTREMITY Compartment pressures can be measured
o Pressures of greater or equal to 20mmHg are
SUBGROUP ANALYSIS: clear indication for fasciotomy
o Native artery vs. Graft occlusion
o 10% amputation rate in native artery treated with PATHOPHYSIOLOGY
lysis vs. 0% treated with surgery (p=0.0024)
o Amputation rate lower in graft occlusions treated Extremity reperfusion ->Increased capillary permeability ->Local
with lysis vs. Surgery (p=0.026) edema -> Compartment hypertension -> Regional venule obstruction
CONCLUSION -> Nerve dysfunction ->Capillary and arteriolar obstruction -> Muscle
o Lysis more beneficial in acute graft occlusion < 14 and nerve infarction
days
o Symptoms < 14 days duration: thrombolytics CLINICAL PRESENTATION
yielded lower amputation rate at 1 year
o Symptoms > 14 days duration: thrombolytics Pain out of proportion to physical signs
yielded no difference in amputation rate but had Paresthesia
higher recurrent ischemia rate at 1 year Edema
o If symptom duration <14 days: Thrombolytics,
otherwise surgery TREATMENT
o If bypass graft occlusion: Thrombolysis, Treatment of choice
especially if symptom duration <14 days four-compartment fasciotomy
4. THROMBOLYSIS or PERIPHERAL ARTERIAL SURGERY ( TOPAS ) BUERGERS DISEASE
Similar amputation- free survival rate at 1 year:
Thromboangiitis Obliterans (Buergers Disease)
thrombolysis (65%) vs. Surgery (70%)
A vasculopathy involving distal arteries and veins of both
Half of thromboytic patients averted need for open
upper and lower extremities with a distinctive thrombus at
revascularization procedure
sites of vessel wall inflammation in its acute face
Rate of intracranial hemorrhage with thrombolytics in first nd th
A disease of 2 thru 4 decades seen predominantly in
62 patients= 4.8%
men
Subsequent intracranial hemorrhage rate with
Tobacco use is universally associated with the active phase
thrombolytics (without heparin)= 1.6%
but the exact etiologic mechanisms are not defined
It causes clauditication and a significant incidence Of digit
5. COMPARISON OF CATHETER-DIRECTED THROMBOLYSIS AND
and limb loss in the young (nagkakatanggalan ang digits)
SURGICAL REVASCULARIZATION IN TREATMENT OF LIMB ISCHEMIA
PATHOGENESIS
Definitive etiology is unknown
Occurs in active smokers and cessation of smoking brings
remission
Genetic predisposition and immunologic mechanisms were
implicated
HLA typing done and patterns vary with ethnic population
Autoimmune disease remains the most plausible cause:
o Cytokine production altered production of IL-6,
IL-12, IL-10, the increased apoptosis, and elevated
levels of circulating immune complexes could be
the reason for persisting immune inflammation
o Anticardiolipin autoantibodies- seen in some
All studies proved that surgery is superior to CDT. patients with Buergers disease
MagnoOpereSomnia Dura Page 8 of 14 STEF AND SHAY
PERIPHERAL VASCULAR MEDICINE 2014 -2015
Dr. Deduyo CARDIOLOGY
o Plasma Endothelin 1- plays a role in exacerbation LABORATORY
of clinical symptoms nd endothelial injury is
connected with increase in concentration of Laboratory Tests Exclude:
selecting P in patients serum risk factor of hyperlipidemia and DM
o T cell mediated inflammation was a significant collagen vascular disease test for ANA, complement, ESR,
event in the development of Buergers disease VDRL
clotting disorders and dysproteinemias
Gross features of TAO in amputated limbs serum electrophoresis, CBC platelet count
focal, segmental, and sometimes long thrombotic hypercoagulable state antiphospholipid antibody, protein
occlusions of arteries and adjacent vein, involvement of C and S, antithrombin lll, etc.
digital arteries, presence of normal vessels proximally, and
absence of atheroscierosis Vascular Lab:
Digital artery pressures and waveforms Segmental
Acute phase/lesion Doppler pressure and waveforms of the limbs
Considered diagnostic Arterial duplex ultrasound
artery or vein is modestly swollen Laser flow velocities; assess occlusive disease of thefingers
moderate infiltration of adventitia and media and potential response to sympathetic block
lumen is occluded by a highly cellular, unique thrombus Thallium-202 scan-determine healing potential of distal
with microabscesses ischemia
lymphocytes and occasionally giant cells and eosinophils
TREATMENT
Subacute phase/lesion
less cellularity and thrombus Cornerstone of tx total abstinence from tobacco use halt
disappearance of microabscesses the progress & prevent recrudescence
recanalization has begun Adequate pain control dysesthesia & minor lesions (OPD
Tx) but with rest pain, ulceration, or infection warrant
Late Phase hospitalization
organized and recanalized thrombus in fibrotic, small o continuous IV narcotics or epidural anesthesia
vessels o periodic debridement of wound
intact architecture of vessel wall, internal elastic membrane Anticoagulation during acute phase due to thrombus
no necrosis seen formation.
Antiplatelet agents chronic cases(?)
TAO in chronic stage Prostaglandins provide dual benefits of vasodilation and
Theres marked increase in elastic lamina and near total antiplatelet activity.
occlusion of the lumen by fibrotic, partly recanalized Vasodilators (ca channel and aadrenergic blockers)
thrombus with mixed inflammatory cell infiltrates greatest on vasomotor changers; efficacy on ischemic pain
and wound healing?
CLINICAL ASPECTS Pulse-therapy with glucocortucoids and cyclophosphamide
- anti-inflammatory effect (decrease BVAS, ESR, CRPV and
Diagnosis should be considered in all tobacco users (male lowers frequency of amputations)
and female) presenting with:
o digital ischemia of feet or hands RAYNAULDS PHENOMENON
o distal claudication
o migratory superficial thrombophlebitis or Raynauds phenomenon is characterized by episodic
o Raynauds phenomenon digital ischemia, manifested clinically by the sequential
development of digital blanching, cyanosis, and rubor
Angiography and biopsy, when feasible, used for of the fingers or toes following cold exposure and
confirmation or clarification subsequent rewarming.
Bilateral involvement is usual, involving 3 or 4 limbs; begins Emotional stress may also precipitate Raynauds
distally and progresses cephalad. phenomenon
Interval from onset o tissue loss is only 2-5 years; foot The color changes are usually well demarcated and
claudication, upper extremity involvement, superficial confined to fingers and toes
phlebitis, and Raynauds phenomenon are common but rare o when patient is exosed to a cold env or touch
in atherosclerotic diseases of the limb cold obj.
Onset is between 19 and 45 years of age (median = 30- o The blanching, pallor represents ischemic
35years) phase of the phenomenon and results from
vasospasm of digital arteries.
Initial presentation: paresthesia of digits often accompanies the phases of pallor
cold sensitivity, dysesthesias, coolness and rubor or and cyanosis
cyanosis of food (33%) With rewarming, the digital vasospasm resolves, and blood
rest pain (10-80%) flow into the dilated arterioles and capillaries increases
digital ulceration or gangrene (18-60%) dramatically.
pedal claudication (15-25%)
MagnoOpereSomnia Dura Page 9 of 14 STEF AND SHAY
PERIPHERAL VASCULAR MEDICINE 2014 -2015
Dr. Deduyo CARDIOLOGY
In addition to rubor and warmth, patients often experience TREATMENT
a throbbing, painful sensation during the hyperemic phase
TREATMENT
PRIMARY RAYNUADS DISEASE 1.) Conservative Therapy
Vasospastic disease reversible, localized or diffuse Keep fingers warm (mittens better than gloves)
vasoconstriction of arteries or smaller blood vessels; may Avoid pressure or exposure to cold
cause irreversible damage in prolonged attacks. Avoid smoking
Idiopathic or primary type unknown cause; usually benign
with little permanent ischemic damage 2.) Drug Therapy
Calcium Channel Blockers; several small RCTs of CCBs for
Prevalence primary RD showed clinical improvement in frequency and
General population: 3.7 30% severity of attacks.
Higher prevalence in cooler climates Reserpine and guanethedine interfere with sympathetic
vasoconstriction and shown to increase digital capillary
PATHOLOGY blood flow (no RCT)
Prazocin (Alpha1-Adreneceptor Antagonist) shown to
Mild disease: normal digital arteries decrease frequency, duration or severity of vasospasm
Severe disease: intimal hyperplasia, narrowing or total NTG (direct acting vasodilator) is used as transdermal paste
occlusion of digital arteries, or presence of thrombi; but with variable results Prostaglandins induce vasodilation
inflammatory destruction of the capillary bed or fibrinoid and inhibit platelet aggregation but with variable results
degeneration of capillaries and abnormalities in basement Thyroid preparation decrease frequency, duration and
membrane severity vasospasm but caused increase BP and PR.
Pathophysiology 3.) Sympathectomy
Normal subjects: sympathectomy of upper extremity may benefit 50-60% of
o Digital blood flow is controlled by sympathetic patients but vasospastic attacks often recur within 6
nervous system months to 2 years
Decreased by activation of SNS More success with digital sympathectomy in severe disease
increased by withdrawal of SNS activity Lumbar sympathectomy for RD in the toes have >80%
o Reflex sympathetic digital vasoconstriction results success rate
from body coolng or application of cold to other
body parts CHRONIC VENOUS DISEASE
o AV anastomoses shunts allow large food flow to
the digits in warm conditions but close during cold Normal Venous Anatomy and Function
exposure. Functions as a reservoir to store blood and as a conduit
to return blood to the heart
Raynauds disease: Carries blood from the legs up to the heart
Decreased finger blood flow or vasospastic attack is Proper functioning depends on a series of valves and
unknown muscle pumps
2 classic theories:
Blood that enters into the lower extremity venous
o Local fault (abnornmality at the level of digital
system must travel against gravity and against
artery)
fluctuating thoracoabdominal pressures to return to
o Overactivity of the SNS
the central circulation in a person in an erect position
DIAGNOSIS Peripheral Venous System
Superficial Venous System
Criteria to Distinguish Primary from Secondary Type:
Deep Venous System
1.) Vasospastic attack precipitated by exposure to cold or emotional
Perforator Veins
stimuli
2.) Bilateral involvement of the extremities
Perforator Veins
3.) Absence of gangrene, or if present, limited to the skin of fingertips
Connects the superficial venous to the deep venous
4.) No evidence of underlying disease
system
5.) A history of symptoms for the last 2 years
Located in the thigh and legs
Diagnostic Modalities to Distinguish Primary from Secondary Type: Contain one- way valves that prevent reflux of blood
1.) Hand perfusion scintigraphy with 99Tc-DTPAObjectively reflects from the deep veins into the superficial system
global and regional microcirculatory abnormalities in the hand and
provides quantitavie data for follow up. Bicuspid Valves (venous valve)
2.) Nailfold capillaries visualized using microscope opthalmoscope Located throughout the deep and superficial veins and
o Normal pattern in primary Rd ensure that:
o Decrease number of capillaries that are enlarge Blood moves in the cephalad direction
and deformed with avascular areas in the Prevent the return of blood toward the feet
scleroderma, mixed CT disease, dermatomyositis while in the upright posture
MagnoOpereSomnia Dura Page 10 of 14 STEF AND SHAY
PERIPHERAL VASCULAR MEDICINE 2014 -2015
Dr. Deduyo CARDIOLOGY
Frequency increases from proximal to the White blood cell trapping in the capillaries or
distal leg to prevent an increase in pressure postcapillary venules
within the distal veins resulting from the Adhesion of WBCs with activation releases
effects of gravity inflammatory mediators and proteolytic
The venous pressure is neutral while lying down, enzymes with endothelial damage that may
increases by 50% while sitting down, it increases by increase permeability or impede flow leading
100% while standing up. to occlusion
Professions that entail prolonged standing will
eventually have venous insufficiency. Classify your patients from C0 to C6
A Damaged Vein
If heredity, an injury, or a blood clot weakens a vein,
the wall near the valve begins to sag. The valve may no
longer close fully, allowing blood to move in both
directions when the muscle relaxes.
Most vein problems begin with damaged veins
Dapat kasi, your bicuspid valve, meron syang
preferential flow going up. When this valve weakens, it
leads to a bidirectional flow due to gravity.
Two components that determine venous pressure
Hydrostatic Component
Related to the weight of the column of blood
from the right atrium to the foot
Hydro dynamic Component
Related to pressures generated by
contractions of the skeletal muscles of the
leg and the pressure in the capillary network
Yung calf pump? on the normal limb. So yung calf
pump mo, nagsstop pag umuupo ka, when you walk, it C0 no venous disease)
leads to a good circulation kaya narerelieve ka while But at this level, meron ka ng symptom leg
walking. heaviness (first manifestation)
In PAD, meron kang claudication, magkakaroon ka ng C1 you develop telangiectasia and reticular veins, better
symptoms when walking. lookat your legs, kungmeron ka ng makikitang bluish
Sa venous disease, baliktad, you have the symptoms discoloration at maliliit na veinscalf mo
while lying still(pagnakaupo or nakatayo ka) when you C2 pag malaki na ung blood vessel mo, varicose veins na
walk, the leg heaviness will be relieved. Ang tawag sya.
dun, reverse claudication C3 pag meron ka ng varicose + telangiectasia + edema
C4 skin changes/discoloration sa foot and distal legs
Venous pathology ascribed to be venous disease
Develops when venous pressure is increased and C5 healed ulcer
return of blood is impaired C6 active ulcer
Mechanism
Valvular incompetence (deep, superficial, perforator) Risk Factors
Venous obstruction ( previous DVT, venous stenosis, Age
May-Thumer syndrome) Gender
Combination of both Occupation(prolonged standing)
Macrocirculatory hemodynamic disturbance Sedentary Lifestyle
Exacerbated by muscle pump dysfunction Long Flights or automobile journeys (more than3 hours)
Venous microangiopathy Sports that increase intra-abdominal pressure(weightlifting
and wresling)
VENOUS MICROANGIOGRAPHY Tight clothig(skinny jeans)
Mechanisms: High heels(the higher the heels the higher the chance)
Fibrin cuff formation Pregnancy
Accumulation of fluid containing fibrin into Immobility
the pericapillary space Heredity
Increase diffusion barrier, inhibit repair Obesity
process
Maintain the inflammatory process Symptoms
Growth factor trapping by fibrin and other Cramping
macromolecules, making them unavailable to facilitate Burning pain
healing Heaviness
MagnoOpereSomnia Dura Page 11 of 14 STEF AND SHAY
PERIPHERAL VASCULAR MEDICINE 2014 -2015
Dr. Deduyo CARDIOLOGY
Fatigue Reticular Veins
Itching Dilated bluish subdermal veins usually
Tension from 1mm to < 3mm in diameter
Throbbing pain Generally tortuous
Restless legs Excludes normal visible veins in people
Tingling with transparent skin
Prevalence: about 50% (male
Signs andfemale)
Dermatitis C2
Hemorrhage Varicose veins
Superficial Thrombophlebitis Subcutaneous dilated veins > or equal to 3mm in
Ulceration diameter in the upright position
Usually tortuous
Lipodermatosclerosis
Prevalence: 10-15% of total population of which
Atrophic blanche
67% have symptoms
C3
Other causes:
Edema
Acute venous problems such as DVT
Perceptible increase in volume of fluid in the skin
Systemic causes of edema such as:
and subcutaneous tissue characterized by
Heart failure
indentation with pressure
Nephrosis
Usually occur in the ankle region, but may extend
Liver Disease
to the leg and foot
Endocrine Disorders
Prevalence: 5-10% ; 85% have symptoms
Side effect of a medication such as CCB, NSAIDS,
C4
oral hypoglycaemic agents
Skin changes ascribed to venous disease
Differentials: if meron kang lower extremity edema,
A. Pigmentation
meron ba yang systemic cause?
Brownish darkening of the skin initiated
Meron ba yang venous insufficiency?
by extravasated blood, which usually
Meron ba yang DVT?
occurs in the ankle region, but may
Meron ba yang PAD?
extend to the leg and foot darkening is
extensive which starts at thefoot then
Other regional considerations:
goes upwards
Ruptured popliteal cyst
B. Eczema
Soft tissue hematoma or mass Erythematous dermatitis which may
Chronic exertional compartment syndrome progress to a blistering, weeping or
Cellulitis scaling eruption of the skin of the leg
Arthritis of the knee or ankle joint Often located near varicose veins
Swelling following recent hip or knee surgery C. Lipodermatosclerosis
Gastrocnemius tear Localized chronic inflammation and
Lymphedema fibrosis of the skin and subcutaneous
Neurogenic pain tissue sometimes associated with
scarring or contracture of the Achilles
Classification of chronic lower extremity venous disease tendon
C Clinical stage (grade 0-6) Sometimes preceded by diffuse
Supplemented by: inflammatory edema of the skin, which
(A) for asymptomatic may be painful and which is often
(S) for symptomatic referred to as hypodermatitis
E Etiological Classification(Congenital, Primary, Secondary ) Can be differentiated from cellulitis by
A Anatomic Distribution(Superficial, Deep, or Perforator, the absence of fever
alone or in combination ) A sign of severe chronic venous disease
P Pathophysiologic Dysfunction(Reflux or Obstruction, alone D. Atrophied Blanche or White Atrophy
or in combination) usually found at the area of the distal
leg
C0S Localized, often circular, whitish and
No visible or palpable signs of venous disease atrophic skin areas surrounded by
Prevalence is 15-20% in the total population dilated capillary spot and sometimes
First level of the classification and was especially hyperpigmentation
created to emphasize that symptoms have to be A sign of severe chronic venous disease
considered as the first signal of the disease C5
C1 Skin changes with healed ulcer
Telangiectasia Full thickness defect of the skin most frequently
A confluence of dilated intradermal at the ankle that fails to heal and is spontaneously
venules of <1mm in caliber sustained by chronic venous disease
MagnoOpereSomnia Dura Page 12 of 14 STEF AND SHAY
PERIPHERAL VASCULAR MEDICINE 2014 -2015
Dr. Deduyo CARDIOLOGY
C6 Move your toes with your legs slightly
Skin changes with active ulcer raised and extended: alternately bend
Most severe manifestation of CVD and unbend your toes(up to 20
Increase markedly with age times)Other basic measures
Prevalence: C4 to C6 is 0.3% -1% ; 78 % are Reverse bicycle
Symptomatic Other Basic Measures
Do:
Leg ulcers Wash in cold water after shower
Regular deep breathing exercises
Arterial ulcer most likely nasa toes and plantar aspect Appropriate sports:walking, swimming,
Mixed type - + venous and arterial disease mahirap itreat cycling, running on soft ground
Arterial appearance atropic, dry, shiny, hairloss signs of severe Avoid:
arterial disease Saunas
Restrictive clothing, girdles
Weight-lifting, skiing, tennis, marathons,
immobile sunbathing
Sclerotherapy
Is the most commonly performed treatment
option for patients with venous telangiectasia and
reticular veins often for cosmetic reasons alone
Injection of a sclerosing agent direct into the
vessel
Pwede injection at pwede laser, mawawala sya
pero it will recur because you do not address the
primary problem. The primary problem is the
pathology in your deep vein.
Treatment Majority of the treatment failure in sclerotherapy
Chronic Venous Disease is due to the failure to use compression stockings
General measures after the treatment
Leg elevation pag mabigat yung legs mo, itaas
mo sya para mabawasan ung pain or gawin mo Sclerotherapy complications:
yung exercise na ginagawa saeroplano, or para Pain or cramping
mas mabilis, ilakad mo sya para mabawasan ung Hyperpigmentation
symptom Telangiectatic matting
Control of body weight Blistering or necrosis
Exercise of calf muscles with periodic flexion of Superficial thrombophlebitis
ankles and transfer of weight Deep vein thrombosis
Avoid heat (mas matagal exposure sa heat, mas Urticaria
madadamage ung vein. Hot showers pwede.) Edema
Avoid standing for long periods
Cold showers to delay progression of disease Laser therapy
Lying flat on the healthy side in the presence of much better compared to doing your injectable
unilateral varicose veins sclerotherapy
Controlling vein problems Indications:
When you sleep, you need to elevate your legs Superficial, fine-caliver venous telangiectasia
with 2-3pillows Telangiectatic matting
Raise your feet above heart level Patient afraid of needles
Elevate your feet at work to prevent worsening of Poor responders to sclerotherapy
leg edema Adverse side effects from sclerotherapy
Anti-stasis exercises Application of laser and light source indirectly over the
Exercises to improve venous circulation vessels
Walk on your heels Pero not allpatients will respond to laser therapy, mas
Stand on tiptoe maliit, mas magrerespond, the larger the varicose veins, di
Rock from your toes to your heels tatalab ung laser hanggang telangiectasia lang sya saka
Point your toes together and then apart reticular veins saka it will also depend on the type of the
Cycling movement: move your legs with laser that you are using.
energetic movements (15-20 times). Older lasers (5yrs ago) will not work lesser treatment
Cross and uncross your legs in a scissors success compared to the ones that came out 2-3 years ago
movement(10-15 times) Endovascular laser therapy(EVLT)
Move each leg in a small circle up to 10 Newer modality
times You need to puncture your femoral vein, papasok
ung ___?sa femoral vein tapos papasok sa greater
MagnoOpereSomnia Dura Page 13 of 14 STEF AND SHAY
PERIPHERAL VASCULAR MEDICINE 2014 -2015
Dr. Deduyo CARDIOLOGY
saphenous vein kasi ultrasound guided din sya But if the problem is yung from the femoral downwards,
hanggang umabot sya dun sa bleeding vein. Once kailangan talaga na thigh stockings ung susuotin
the bleeding vein is identified, mag aapply sya ng Instruct the patient to wear the stockings immediately sa
laser, pwede syang sound frequency, pwededin moring and remove it at night
syang laser tapos iisclerose mo na yung Compression stockings will last approximately 6 months
telangiectasia saka ung reticular veins then eventually, kasi stockings yan so ung elasticity nya
Kaya ng EVLT ang varicose veins. nawawala, Elastic bandage pwede pa kaso mas matagal
Although maramipa rin ang gumagawa ng vein sya ikabit
stripping, Better success rate pa rin ang EVLT
Elastic stockings
Other causes(hindi to binanggit pero sinali ko na rin just in They should be worn daily
case) Put other socks over them if youre concerned
Obstruction of the deep veins about their appearance
DVT with inadequate recanalization Elastic stockings: tips for wear and care
Venous stasis Once your stockings are on, make sure the top of
Extrinsic compression, as in may the stockings is about two fingers width below
thumer syndrome(compression of the the crease of the knee or the groin. If a stocking is
left common iliac vein as is traverses too high, it will cut off blood flow
between the right common iliac artery Wound and skin care
and the lumbosacral region) Progressive CVI may lead to compromised skin
Dysfunction of muscle pumps integrity, it is important to keep the affected area
Neuro muscular conditions or muscle well moisturized to reduce the risk of skin
wasting syndromes breakdown and possibility of infection
Development of stasis dermatitis needs to be
Conservative management treated with a topical steroid
Toreduce symptoms and help prevent the With venous ulcers, bacterial overgrowth control
development of secondary complications and the and aggressive wound care are required to
progression of disease minimize infections complications
Behavioural measures such as elevating the legs
to minimize edema and reducing intraabdominal Pharmacologic therapy
pressure should be advocated Four groups of drugs evaluated for CVI:
The use of compressive stocking is the mainstay Coumarins(alpha-benzopyrones)
of conservative treatment Flavonoids (gamma-benzopyrones)
Prescription for elastic stockings includes Saponosides (horse chestnut extracts)
information about the tension and length. The Rutosides
tension is based on the clinical severity: With venoactive properties, widely used in Europe but not
20-30mmHg for CEAP 2-3 venous approved for use in the USA
insufficiency Principle for use of venoactive drugs: improve venous tone
30-40mmHg for ceap 4-6dvt or and capillary permeability.
recurrent ulcer Yung available lang sa market natin ay ung Daflon and ung
40-50mmHg for recurrent ulcers generic nya
Pagpostsclerotherapy, you have to use your
Sa Europe merong antistax = main component red leaf
stockings
Antistax vs daflon
Daflon-better symptom control - 1tab 2x per day
In patients with hemorrhoids, 2tabs 2x per day
In some patients with severe venous insufficiency,
2 tabs 2xper day.
Best response for venous insufficiency daflon 3-6 months
plus your compression stockings
2 months of treatment with daflon will be equivalent to a
pair of compression stockings O_O
Depends on the type ofcompression stockings.
Care for your stockings
Pwede ka mag start out using your lower compression You just need to wash them with ordinary soap
stockings, pag ____yung symptoms, you need yo give your and water wag mo silang ilalagay sa washing
higher compression machine at wag ibilad sa araw..
The problem lang, pag nasa tropical country, a lot of
patients will complain na lalo silang nagpapawis when using
the compression stockings
If the problem is only on the bifurcation vessles, you will
need to wear your below the knee stockings
MagnoOpereSomnia Dura Page 14 of 14 STEF AND SHAY
Você também pode gostar
- Understand Cancer & Reduce Cancer Risk - Based On The Teachings Of Dr. Andrew Huberman: Empowering You To Safeguard Against ItNo EverandUnderstand Cancer & Reduce Cancer Risk - Based On The Teachings Of Dr. Andrew Huberman: Empowering You To Safeguard Against ItAinda não há avaliações
- Demonstration and Mechanism of Brudzinski and KernDocumento3 páginasDemonstration and Mechanism of Brudzinski and KernYamamoto YuichiAinda não há avaliações
- Suppositories: Abenol (CAN)Documento2 páginasSuppositories: Abenol (CAN)Mikko McDonie VeloriaAinda não há avaliações
- Products For PCNL BrochureDocumento8 páginasProducts For PCNL Brochuremusic43562981Ainda não há avaliações
- Measles (Rubeola) : Sabah Mohsin Al-Maamuri MDDocumento2 páginasMeasles (Rubeola) : Sabah Mohsin Al-Maamuri MDAndegokilAinda não há avaliações
- Warfarin Q and ADocumento40 páginasWarfarin Q and AAbdul-Rhman Hamdy KishkAinda não há avaliações
- Total Parenteral Nutrition: Presented byDocumento46 páginasTotal Parenteral Nutrition: Presented byMuhammad YamnainAinda não há avaliações
- Update On Cancer CachexiaDocumento4 páginasUpdate On Cancer CachexiaIyanAinda não há avaliações
- Medication Error 2017Documento51 páginasMedication Error 2017Christina100% (1)
- Measles: PGI Nicole Jenne C. TanDocumento40 páginasMeasles: PGI Nicole Jenne C. TanNicole Jenne TanAinda não há avaliações
- Pleural Infection - Past, Present, and Future DirectionsDocumento15 páginasPleural Infection - Past, Present, and Future DirectionsCamilo VidalAinda não há avaliações
- Acute Arterial OcclusionDocumento39 páginasAcute Arterial Occlusionmaria teresa casili100% (1)
- Urinary Tract Infections PowerpointDocumento22 páginasUrinary Tract Infections Powerpointsamdhathri100% (1)
- Measures of Disease Frequency NOTESDocumento22 páginasMeasures of Disease Frequency NOTESSJ Jung100% (1)
- Epi Confounding AssignmentDocumento4 páginasEpi Confounding Assignmentcharles100% (2)
- Thrombocytopenia Thrombocytopenia Thrombocytopenia ThrombocytopeniaDocumento12 páginasThrombocytopenia Thrombocytopenia Thrombocytopenia ThrombocytopeniaRashed ShatnawiAinda não há avaliações
- Cancer Pain ManagementDocumento38 páginasCancer Pain ManagementZakkyMaulanaRahmat100% (1)
- Patient ChartDocumento2 páginasPatient ChartHydieAinda não há avaliações
- Having A Percutaneous Nephrolithotomy (PCNL)Documento4 páginasHaving A Percutaneous Nephrolithotomy (PCNL)Mukesh KumarAinda não há avaliações
- Retroperitoneal and Soft TissueDocumento59 páginasRetroperitoneal and Soft TissueLucas Phi100% (1)
- DR Tommy - Cancer PainDocumento60 páginasDR Tommy - Cancer Painrisalbalu100% (1)
- Keeping Older Adults Safe at Home: Fall Risks Add UpDocumento6 páginasKeeping Older Adults Safe at Home: Fall Risks Add UpBj DuquesaAinda não há avaliações
- Leg UlcersDocumento22 páginasLeg UlcersMarera DomnicAinda não há avaliações
- Screening Case Study Exercises - Hannah TurnerDocumento4 páginasScreening Case Study Exercises - Hannah Turnerapi-457299309Ainda não há avaliações
- Name: Abdirahman Sheikh Abdillahi Farah Faculty: Clinical Officers (CO8) Course: Pediatric Lecturer: DR Amin Assingment: Pleural EffusionDocumento46 páginasName: Abdirahman Sheikh Abdillahi Farah Faculty: Clinical Officers (CO8) Course: Pediatric Lecturer: DR Amin Assingment: Pleural EffusionAbdirahman Abdillahi FarahAinda não há avaliações
- Screening and Early Detection: Epidemiological Basis For Disease Control - Fall 2001Documento28 páginasScreening and Early Detection: Epidemiological Basis For Disease Control - Fall 2001Kharisma Rizqiah WahyuniAinda não há avaliações
- FluidDocumento45 páginasFluidloglesb1Ainda não há avaliações
- Glascow Coma ScaleDocumento15 páginasGlascow Coma ScalePaul Henry RoxasAinda não há avaliações
- Cellulitis Oral Case PresDocumento48 páginasCellulitis Oral Case PresLet BorlagdanAinda não há avaliações
- Case Report ThymomaDocumento18 páginasCase Report ThymomaFatur ReyhanAinda não há avaliações
- Post-Operative Nausea, Vomiting, and Pain - Nursing Management and EvidenceDocumento11 páginasPost-Operative Nausea, Vomiting, and Pain - Nursing Management and EvidenceAdrian Castro100% (1)
- Incarcerated Strangulated HerniaDocumento12 páginasIncarcerated Strangulated HerniaamexatoAinda não há avaliações
- Pressure Ulcers and Wounds: by Monica Warhaftig, D.O. Assistant Professor of Geriatrics N.S.UDocumento64 páginasPressure Ulcers and Wounds: by Monica Warhaftig, D.O. Assistant Professor of Geriatrics N.S.UEvaAinda não há avaliações
- Congenital Heart DiseaseDocumento124 páginasCongenital Heart DiseasemulkanmustafaAinda não há avaliações
- GEN GallBladderInstrumentsADocumento10 páginasGEN GallBladderInstrumentsANeo Rodriguez AlvaradoAinda não há avaliações
- Emergency Department Evaluation Back PainDocumento29 páginasEmergency Department Evaluation Back PainRodolfo GorveñaAinda não há avaliações
- ThrombocytopeniaDocumento2 páginasThrombocytopeniaNeoMedica100% (1)
- Inflamatory Bowel Disease: Dr. Samir IsmailDocumento82 páginasInflamatory Bowel Disease: Dr. Samir IsmailGhadeer EbraheemAinda não há avaliações
- Textbook Reference-Unit VI (p449) : Part 1 of 3Documento53 páginasTextbook Reference-Unit VI (p449) : Part 1 of 3glenn johnstonAinda não há avaliações
- Name: Patient X Age: 14 Y/oDocumento4 páginasName: Patient X Age: 14 Y/oRyan Jay Patacsil100% (1)
- Emphysematous Pyelonephritis (EPN)Documento31 páginasEmphysematous Pyelonephritis (EPN)HardiTariqHammaAinda não há avaliações
- Portal Vein Thrombus ChildrenDocumento11 páginasPortal Vein Thrombus ChildrenViswas ChhapolaAinda não há avaliações
- Esophageal Varices: Medication HistoryDocumento4 páginasEsophageal Varices: Medication HistoryNeil Patrick PasuquinAinda não há avaliações
- Eye ExamDocumento43 páginasEye ExamTapon Sarkar100% (1)
- Aneurysm Final (Bentals Procedure)Documento55 páginasAneurysm Final (Bentals Procedure)tejuteju067100% (1)
- Incidence and Prevalence PDFDocumento9 páginasIncidence and Prevalence PDFSreya SanilAinda não há avaliações
- Myocardial Infarction: Practice Essentials, Background, Definitions PDFDocumento12 páginasMyocardial Infarction: Practice Essentials, Background, Definitions PDFMukhtar UllahAinda não há avaliações
- Heart Valve DiseaseDocumento9 páginasHeart Valve DiseaseChaturangaNSenerathAinda não há avaliações
- GBS Management, Medications and Nursing ConsiderationsDocumento4 páginasGBS Management, Medications and Nursing Considerationssouledg3100% (1)
- Vii. Laboratory Results: Hemoglobin 129 MG/DL 140-160 MG/DL LowDocumento2 páginasVii. Laboratory Results: Hemoglobin 129 MG/DL 140-160 MG/DL LowAdrian Dela CruzAinda não há avaliações
- Warfarin: Prof DR Shah MuradDocumento63 páginasWarfarin: Prof DR Shah Muradshahmurad653376Ainda não há avaliações
- Jade R. Dinolan BSN-4: Diagnosi SDocumento5 páginasJade R. Dinolan BSN-4: Diagnosi SJhade Relleta100% (1)
- TetanusDocumento3 páginasTetanusRoma Nova Pascual CabarrubiasAinda não há avaliações
- H.A Assessing Thorax and LungsDocumento68 páginasH.A Assessing Thorax and LungsMc Ramil B. Pradero100% (1)
- INDIVIDUAL CASE ANALYSIS ScribdDocumento2 páginasINDIVIDUAL CASE ANALYSIS ScribdAnusha VergheseAinda não há avaliações
- AMINOGLYCOSIDESDocumento45 páginasAMINOGLYCOSIDESAbdullah EmadAinda não há avaliações
- Interact Sbar FormDocumento24 páginasInteract Sbar FormYaumil Fajri100% (2)
- FUNDA LEC Finals - Medication AdministrationDocumento14 páginasFUNDA LEC Finals - Medication AdministrationNel joy PaurilloAinda não há avaliações
- Anterior Cord SyndromeDocumento8 páginasAnterior Cord SyndromeJanine Erika Julom BrillantesAinda não há avaliações
- MeaslesDocumento20 páginasMeaslessuryanto_malvinAinda não há avaliações
- Infective Endocarditis - Dr. Payawal PDFDocumento6 páginasInfective Endocarditis - Dr. Payawal PDFMedisina101Ainda não há avaliações
- Congestive Heart Failure - Dra. DeduyoDocumento10 páginasCongestive Heart Failure - Dra. DeduyoMedisina101Ainda não há avaliações
- Acute Coronary Syndrome - Dra. Deduyo PDFDocumento6 páginasAcute Coronary Syndrome - Dra. Deduyo PDFMedisina101Ainda não há avaliações
- Arrythmia Part 1 - Dr. Payawal PDFDocumento10 páginasArrythmia Part 1 - Dr. Payawal PDFMedisina101100% (1)
- ECG Part 1 - Dr. Payawal PDFDocumento10 páginasECG Part 1 - Dr. Payawal PDFMedisina101Ainda não há avaliações
- Coronary Artery Disease - Dra. Deduyo PDFDocumento7 páginasCoronary Artery Disease - Dra. Deduyo PDFMedisina101Ainda não há avaliações
- ECG Part 2 - Dr. Payawal PDFDocumento4 páginasECG Part 2 - Dr. Payawal PDFMedisina101Ainda não há avaliações
- Pericardial Diseases - Dr. BartolomeDocumento8 páginasPericardial Diseases - Dr. BartolomeMedisina101Ainda não há avaliações
- PEDIA - Cardio (Esguerra) PDFDocumento9 páginasPEDIA - Cardio (Esguerra) PDFMedisina101Ainda não há avaliações
- Arrythmia Part 2 - Dr. Payawal PDFDocumento8 páginasArrythmia Part 2 - Dr. Payawal PDFMedisina101Ainda não há avaliações
- Valvular Heart Diseases Part 2 - Dr. BartolomeDocumento9 páginasValvular Heart Diseases Part 2 - Dr. BartolomeMedisina101Ainda não há avaliações
- Valvular Heart Diseases Part 1 - Dr. BartolomeDocumento18 páginasValvular Heart Diseases Part 1 - Dr. BartolomeMedisina101Ainda não há avaliações
- Diseases of The Aorta - Dr. Deduyo PDFDocumento11 páginasDiseases of The Aorta - Dr. Deduyo PDFMedisina101Ainda não há avaliações
- Deep Vein Thrombosis - Dr. Deduyo PDFDocumento17 páginasDeep Vein Thrombosis - Dr. Deduyo PDFMedisina101Ainda não há avaliações
- Congenital Heart Diseases - Dr. BartolomeDocumento12 páginasCongenital Heart Diseases - Dr. BartolomeMedisina101Ainda não há avaliações
- Cardiac Tumors - Dr. BartolomeDocumento12 páginasCardiac Tumors - Dr. BartolomeMedisina101Ainda não há avaliações
- Cardiac Tumors Slides - Dr. BartolomeDocumento81 páginasCardiac Tumors Slides - Dr. BartolomeMedisina101Ainda não há avaliações
- Acquired Heart DiseaseDocumento44 páginasAcquired Heart DiseaseMedisina101Ainda não há avaliações
- Pedia Pulmo 3 11.03.16Documento49 páginasPedia Pulmo 3 11.03.16Medisina101Ainda não há avaliações
- SURGERY Lecture 5 - Abdominal Wall, Omentum, Mesentery, Retroperitoneum (Dr. Wenceslao)Documento13 páginasSURGERY Lecture 5 - Abdominal Wall, Omentum, Mesentery, Retroperitoneum (Dr. Wenceslao)Medisina101Ainda não há avaliações
- Pedia Pulmo 2 10.18.16Documento73 páginasPedia Pulmo 2 10.18.16Medisina101Ainda não há avaliações
- Pedia Pulmo I 10.4.16Documento129 páginasPedia Pulmo I 10.4.16Medisina101Ainda não há avaliações
- Pedia Cardiology 2Documento5 páginasPedia Cardiology 2Medisina101Ainda não há avaliações
- SURGERY Lecture 1 - Small Intestine (Dr. Mendoza)Documento16 páginasSURGERY Lecture 1 - Small Intestine (Dr. Mendoza)Medisina101100% (1)
- Head and Neck SurgeryDocumento15 páginasHead and Neck SurgeryMedisina101100% (1)
- SURGERY Lecture 4 - Breast (Dra. Fernandez)Documento15 páginasSURGERY Lecture 4 - Breast (Dra. Fernandez)Medisina101100% (1)
- SURGERY Lecture 3 - Abdominal Hernia (Dr. Mendoza)Documento12 páginasSURGERY Lecture 3 - Abdominal Hernia (Dr. Mendoza)Medisina101100% (1)
- SURGERY Lecture 2 - Liver & Gallbladder (Dr. Wenceslao)Documento19 páginasSURGERY Lecture 2 - Liver & Gallbladder (Dr. Wenceslao)Medisina101100% (1)
- Surgery II - Pancreas 2014Documento20 páginasSurgery II - Pancreas 2014Medisina101Ainda não há avaliações
- Internal Diagnosis II Good NotesDocumento83 páginasInternal Diagnosis II Good Notesbjpalmer100% (2)
- AngE Solutions EN WEBDocumento12 páginasAngE Solutions EN WEBSayed El-MaadawyAinda não há avaliações
- Spot Vital Signs: Service ManualDocumento71 páginasSpot Vital Signs: Service ManualJulio Benancio ZuluagaAinda não há avaliações
- Chapter 2 - Clinical Cardiovascular Examination-2Documento43 páginasChapter 2 - Clinical Cardiovascular Examination-2sarahya.medinaAinda não há avaliações
- Fundamentals of Cardiology For The USMLE and General Medics PDFDocumento287 páginasFundamentals of Cardiology For The USMLE and General Medics PDFCharles Vindo100% (2)
- Ineffective Airway Clearance R/T Tracheobronchial ObstructionDocumento23 páginasIneffective Airway Clearance R/T Tracheobronchial ObstructionGuia Rose SibayanAinda não há avaliações
- Vital SignsDocumento98 páginasVital SignsJamaica LimejuiceAinda não há avaliações
- ABCDE Assessment - Lecturio PDFDocumento11 páginasABCDE Assessment - Lecturio PDFjsw03Ainda não há avaliações
- BIO 12 EX 6 BLOOD PRESSURE WorksheetDocumento9 páginasBIO 12 EX 6 BLOOD PRESSURE WorksheetAnonymous TPCRxkw0jAinda não há avaliações
- Sheu 2003Documento7 páginasSheu 2003CORO CORPSAinda não há avaliações
- Almaghrabi Cardio ExaminationDocumento22 páginasAlmaghrabi Cardio ExaminationSagit Nauman81Ainda não há avaliações
- Aerie 14th Edition Manual PDF FinalDocumento128 páginasAerie 14th Edition Manual PDF FinalAina P. T.Ainda não há avaliações
- NCP RHDDocumento4 páginasNCP RHDlouie john abilaAinda não há avaliações
- 500 Single Best Answers in MedicineDocumento443 páginas500 Single Best Answers in MedicineOmar Ahmed100% (1)
- ST 9 PDFDocumento2 páginasST 9 PDFsorinAinda não há avaliações
- Itas2010 - Indiantakayasu'S Arteritis Activity ScoreDocumento2 páginasItas2010 - Indiantakayasu'S Arteritis Activity ScoreLp Saikumar DoradlaAinda não há avaliações
- Checklist FON 1Documento27 páginasChecklist FON 1Hadan KhanAinda não há avaliações
- Pulse Test DiagnosisDocumento19 páginasPulse Test DiagnosisJavierAinda não há avaliações
- Physical DiagnosisDocumento42 páginasPhysical DiagnosisKhim Yalong100% (1)
- Prelim Examination (Na)Documento6 páginasPrelim Examination (Na)Tessah SanchezAinda não há avaliações
- Fundamentals of Polygraph TestingDocumento31 páginasFundamentals of Polygraph TestingEmmanuel GeronimoAinda não há avaliações
- Pe and Health Quarter 1 - Module 4:: Philippine FolkdanceDocumento14 páginasPe and Health Quarter 1 - Module 4:: Philippine FolkdanceCHEENY TAMAYO100% (11)
- Assembly & User Manual: Compact Upright Seated Gym Cug2Documento28 páginasAssembly & User Manual: Compact Upright Seated Gym Cug2seanAinda não há avaliações
- Patients Will Be Assigned On Aug. 27 2020. Each Group Must Prepare Its Written and PPT PresentationDocumento4 páginasPatients Will Be Assigned On Aug. 27 2020. Each Group Must Prepare Its Written and PPT PresentationMonique BorresAinda não há avaliações
- Clinical Examination - Karen Notes - SHIRI For BD DoctorsDocumento11 páginasClinical Examination - Karen Notes - SHIRI For BD DoctorsHelp LineAinda não há avaliações
- HA Lab PracticalDocumento2 páginasHA Lab Practicalsflower85100% (2)
- WrwerDocumento251 páginasWrwerRaheelAinda não há avaliações
- Invasive Arterial Blood PressureDocumento31 páginasInvasive Arterial Blood PressureYanti PandianganAinda não há avaliações
- Lecture 3 - VITAL SIGNSDocumento50 páginasLecture 3 - VITAL SIGNSابراهيم الشمريAinda não há avaliações
- Secrets of The Pulse Vasant Lad.09743 1Documento19 páginasSecrets of The Pulse Vasant Lad.09743 1nikhil26986Ainda não há avaliações