Escolar Documentos
Profissional Documentos
Cultura Documentos
Breast Anatomy
Enviado por
Hossamuldin Aly El NemrDescrição original:
Direitos autorais
Formatos disponíveis
Compartilhar este documento
Compartilhar ou incorporar documento
Você considera este documento útil?
Este conteúdo é inapropriado?
Denunciar este documentoDireitos autorais:
Formatos disponíveis
Breast Anatomy
Enviado por
Hossamuldin Aly El NemrDireitos autorais:
Formatos disponíveis
CLINICALLY ORIENTED ANATOMY
105
enter directly into the corresponding and nearby brachiocephalic veins. The posterior intercostal veins of the 2nd and 3rd (and occasionally 4th) intercostal spaces unite to form a trunk, the superior intercostal vein (Fig. 1.60A & B). The right superior intercostal vein is typically the final tributary of the azygos vein, before it enters the SVC. The left superior intercostal vein, however, usually empties into the left brachiocephalic vein. This requires the vein to pass anteriorly along the left side of the superior mediastinum, specifically across the arch of the aorta or the root of the great vessels arising from it and between the vagus and phrenic nerves (Fig. 1.60B). It usually receives the left bronchial veins and may receive the left pericardiacophrenic vein as well. Typically, it communicates inferiorly with the accessory hemiazygos vein. The internal thoracic veins are the companion veins (L. venae comitantes) of the internal thoracic arteries.
THE BOTTOM LINE: The pattern of distribution of neurovascular structures to the thoracic wall reflects the construction of the thoracic cage. These structures course in the intercostal spaces, parallel to the ribs, and serve the intercostal muscles as well as the integument and parietal pleura on their superficial and deep aspects. Because plexus formation does not occur in relationship to the thoracic wall, the pattern of peripheral and segmental (dermatomal) innervation is identical in this region. The intercostal nerves run a posterior to anterior course along the length of each intercostal space, and the anterior and posterior intercostal arteries and veins converge toward and anastomose in approximately the anterior axillary line. The posterior vessels arise from the thoracic aorta and drain to the azygos venous system, and the anterior vessels arise from the internal thoracic artery, branches, and tributaries and drain to the internal thoracic vein, branches, and tributaries.
num to the midaxillary line and vertically from the 2nd through 6th ribs. Two thirds of the bed of the breast are formed by the pectoral fascia overlying the pectoralis major; the other third, by the fascia covering the serratus anterior (Figs. 1.19 and 1.20). Between the breast and the pectoral fascia is a loose connective tissue plane or potential spacethe retromammary space (bursa). This plane, containing a small amount of fat, allows the breast some degree of movement on the pectoral fascia. A small part of the mammary gland may extend along the inferolateral edge of the pectoralis major toward the axillary fossa (armpit), forming an axillary process or tail (of Spence). Some women discover this (especially when it may enlarge during a menstrual cycle) and become concerned that it may be a lump (tumor) or enlarged lymph nodes. The mammary gland is firmly attached to the dermis of the overlying skin, especially by substantial skin ligaments (L. retinacula cutis), the suspensory ligaments (of Cooper). These condensations of fibrous connective tissue, particularly well developed in the superior part of the gland, help support the mammary gland lobules. During puberty (ages 815 years), the breasts normally enlarge, owing in part to glandular development but primarily from increased fat deposition. The areolae and nipples also enlarge. Breast size and shape are determined by genetic, ethnic, and dietary factors. The lactiferous ducts give rise to buds that form 1520 lobules of glandular tissue, which constitute the parenchyma of the mammary gland. Each lobule is drained by a lactiferous duct, which usually opens independently on the nipple. The ducts converge toward the nipple like the spokes of a bicycle wheel. Deep to the areola, each duct has a dilated
Sternum
Breasts
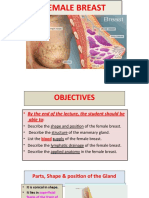
Both men and women have breasts (L. mammae); normally they are well developed only in women (Fig. 1.19). The mammary glands in the breasts are accessory to reproduction in women but are rudimentary and functionless in men, consisting of only a few small ducts or epithelial cords. Usually, the fat present in the male breast is not different from that of subcutaneous tissue elsewhere, and the glandular system does not normally develop. The breasts are the most prominent superficial structures in the anterior thoracic wall, especially in women. The mammary glands are in the subcutaneous tissue overlying the pectoralis major and minor muscles. The amount of fat surrounding the glandular tissue determines the size of non-lactating breasts. At the greatest prominence of the breast is the nipple, surrounded by a circular pigmented area of skin, the areola (L. small area).
Female Breasts
Axillary tail of breast Axilla Lobules of fat Nipple
Areola Serratus anterior Anterior view
The roughly circular body of the female breast rests on a bed that extends transversely from the lateral border of the ster-
Figure 1.19. Superficial dissection of female pectoral region. The pectoral fascia has been removed, except where it lies deep to the breast. The bed of the breast extends from the 2nd through the 6th ribs. The axillary tail of the breast extends toward or into the axillary fossa. The non-lactating breast consists primarily of fat.
106
1 / THORAX
Suspensory ligaments Fat lobule Lactiferous sinus Areola Nipple
Alveolus 2nd rib Retromammary space (bursa) Subcutaneous tissue Pectoralis minor Pectoralis major 4th intercostal space Mammary gland lobules (resting) Pectoral fascia 6th rib
secreting alveoli (L. small hollow spaces) are arranged in grapelike clusters. In most women, the breasts enlarge slightly during the menstrual period from increased release of the gonadotropic hormonesfollicle-stimulating hormone (FSH) and luteinizing hormone (LH)on the glandular tissue.
Changes in the Breasts
Changes, such as branching of the lactiferous ducts, occur in the breast tissues during menstrual periods and pregnancy (Ferguson et al., 1992). Although mammary glands are prepared for secretion by midpregnancy, they do not produce milk until shortly after the baby is born. Colostrum, a creamy white to yellowish premilk fluid, may secrete from the nipples during the last trimester of pregnancy and during initial episodes of nursing. Colostrum is believed to be especially rich in protein, immune agents, and a growth factor affecting the infants intestines. In multiparous women, the breasts often become large and pendulous. The breasts in elderly women are usually small because of the decrease in fat and the atrophy of glandular tissue.
Lactiferous ducts Mammary gland lobules (lactating) Medial view
Figure 1.20. Sagittal section of female breast and anterior thoracic wall. The breast consists of glandular tissue and fibrous and adipose tissue between the lobes and lobules of glandular tissue, together with blood vessels, lymphatic vessels, and nerves. The superior two thirds of the figure demonstrates the suspensory ligaments and alveoli of the breast with resting mammary gland lobules; the inferior part shows lactating mammary gland lobules.
Breast Quadrants
For the anatomical location and description of tumors and cysts, the surface of the breast is divided into four quadrants (Fig. B1.5). For example, a physicians record might state: A hard irregular mass was felt in the superior medial quadrant of the breast at the 2 oclock position, approximately 2.5 cm from the margin of the areola.
portion, the lactiferous sinus, in which a small droplet of milk accumulates or remains in the nursing mother. As the infant begins to suckle, compression of the areola (and the lactiferous sinus beneath it) expresses the accumulated droplets and encourages the infant to continue nursing as the hormonally mediated let-down reflex ensues and the mothers milk is secreted intonot sucked from the gland bythe babys mouth. The areolae contain numerous sebaceous glands, which enlarge during pregnancy and secrete an oily substance that provides a protective lubricant for the areola and nipple, which are particularly subject to chaffing and irritation as mother and baby begin the nursing experience. The nipples are conical or cylindrical prominences in the centers of the areolae. The nipples have no fat, hair, or sweat glands. The tips of the nipples are fissured with the lactiferous ducts opening into them. The nipples are composed mostly of circularly arranged smooth muscle fibers that compress the lactiferous ducts during lactation and erect the nipples in response to stimulation, as when a baby begins to suckle. The mammary glands are modified sweat glands; therefore, they have no special capsule or sheath. The rounded contour and most of the volume of the breasts are produced by subcutaneous fat, except during pregnancy when the mammary glands enlarge and new glandular tissue forms. The milk-
Axillary tail
12 oclock
Superior lateral
Superior medial Areola Nipple
9 Inferior lateral
3 Inferior medial
6 Right breast
Figure B1.5
CLINICALLY ORIENTED ANATOMY
107
Vasculature of the Breast
The arterial supply of the breast (Fig. 1.21A & B) derives from the: Medial mammary branches of perforating branches and anterior intercostal branches of the internal thoracic artery, originating from the subclavian artery. Lateral thoracic and thoracoacromial arteries, branches of the axillary artery. Posterior intercostal arteries, branches of the thoracic aorta in the 2nd, 3rd, and 4th intercostal spaces.
Subclavian a. Brachial a. Axillary a. Thoracoacromial trunk Lateral thoracic a. Lateral mammary branches
The venous drainage of the breast is mainly to the axillary vein, but there is some drainage to the internal thoracic vein (Fig. 1.21C). The lymphatic drainage of the breast is important because of its role in the metastasis of cancer cells. Lymph passes from the nipple, areola, and lobules of the gland to the subareolar lymphatic plexus (Fig. 1.22A & B). From this plexus: Most lymph ( 75%), especially from the lateral breast quadrants, drains to the axillary lymph nodes, initially to the anterior or pectoral nodes for the most part. However,
Internal thoracic artery and its perforating branches Medial mammary branches
Dorsal branch of posterior intercostal a.
Lateral mammary branches of lateral cutaneous branches of posterior intercostal arteries (A) Arteries of mammary gland Anterior (and slightly oblique) view Internal jugular v. Subclavian v. Cephalic v. Axillary v. Lateral thoracic v. Lateral mammary vv. Anterior intercostal a. Medial mammary branch (B) Transverse section of thorax (T9 level) Anterosuperior view Internal thoracic a.
Posterior intercostal a.
Thoracic aorta Perforating branch
Internal thoracic vein and its perforating branches Medial mammary v. (C) Veins of mammary gland Anterior (and slightly oblique) view
Figure 1.21. Vasculature of breast. A. The mammary gland is supplied from its medial aspect mainly by perforating branches of the internal thoracic artery and by several branches of the axillary artery (principally the lateral thoracic artery) superiorly and laterally. B. The breast is supplied deeply by branches arising from the intercostal arteries. C. Venous drainage is to the axillary (mainly) and internal thoracic veins.
Supraclavicular lymph nodes Infraclavicular lymph nodes Axillary artery and vein Apical lymph nodes Humeral (lateral) lymph nodes Axillary lymph nodes Central lymph nodes Pectoral (anterior) lymph nodes Subscapular (posterior) lymph nodes Interpectoral nodes Pectoralis minor Pectoralis major Subareolar lymphatic plexus
Subclavian lymphatic trunk Inferior deep cervical lymph nodes Internal jugular vein Right lymphatic duct Subclavian vein Right brachiocephalic vein and artery Parasternal lymph nodes
To left breast
To abdominal (subdiaphragmatic) lymphatics
(A) Location of lymph nodes Central nodes Apical nodes Clavicular (supraclavicular and infraclavicular) nodes Internal jugular vein Right jugular lymphatic trunk Humeral nodes Subscapular nodes Pectoral nodes Right lymphatic duct Subclavian vein Right bronchomediastinal lymphatic trunk Right brachiocephalic vein Right subclavian lymphatic trunk
L. jugular trunk Internal jugular vein Thoracic duct Left venous angle R. brachiocephalic vein L. subclavian vein Clavicle L. brachiocephalic vein Superior vena cava L. bronchomediastinal vein L. subclavian trunk
(C) Left venous angle Anterior view
(B) Pattern of lymphatic drainage of axillary lymph nodes Anterior (and slightly oblique) views
Figure 1.22. Lymphatic drainage of breast. A. The lymph nodes in the region are shown. B. The red arrows indicate lymph flow from the right breast. Most lymph, especially that from the superior lateral quadrant and center of the breast, drains to the axillary lymph nodes, which, in turn, are drained by the subclavian lymphatic trunk and then into the venous system via the right lymphatic duct. C. Most lymph from the left breast returns to the venous system via the thoracic duct, which enters the left venous angle.
CLINICALLY ORIENTED ANATOMY
109
some lymph may drain directly to other axillary nodes or even to interpectoral, deltopectoral, supraclavicular, or inferior deep cervical nodes. (The axillary lymph nodes are covered in detail in Chapter 6.) Most of the remaining lymph, particularly from the medial breast quadrants, drains to the parasternal lymph nodes or to the opposite breast, whereas lymph from the inferior quadrants may pass deeply to abdominal lymph nodes (subdiaphragmatic inferior phrenic lymph nodes). Lymph from the skin of the breast, except the nipple and areola, drains into the ipsilateral axillary, inferior deep cervical, and infraclavicular lymph nodes and also into the parasternal lymph nodes of both sides. Lymph from the axillary nodes drains into clavicular (infraclavicular and supraclavicular) lymph nodes and from them into the subclavian lymphatic trunk, which also drains lymph from the upper limb. Lymph from the parasternal nodes enters the bronchomediastinal lymphatic trunk, which also drains lymph from the thoracic viscera. The termination of these lymphatic trunks varies; traditionally, these
trunks are described as merging with each other and with the jugular lymphatic trunk, draining the head and neck to form a short right lymphatic duct on the right side or entering the termination at the thoracic duct on the left side. However, in many (perhaps most) cases, the trunks open independently into the junction of the internal jugular and subclavian vein, the venous angle, to form the brachiocephalic veins (Fig. 1.22C). In some cases, they open into both of these veins.
Nerves of the Breast
The nerves of the breast derive from anterior and lateral cutaneous branches of the 4th6th intercostal nerves (Fig. 1.13). The anterior primary rami of T1T11 are called intercostal nerves because they run within the intercostal spaces. Rami communicantes connect each anterior ramus to a sympathetic trunk. The branches of the intercostal nerves pass through the deep fascia covering the pectoralis major to reach the skin, including the breast in the subcutaneous tissue overlying this muscle. The branches of the intercostal nerves thus convey sensory fibers to the skin of the breast and sympathetic fibers to the blood vessels in the breasts and smooth muscle in the overlying skin and nipple.
Carcinoma of the Breast
Understanding the lymphatic drainage of the breasts is of practical importance in predicting the metastasis of carcinoma of the breast (breast cancer). Carcinomas of the breast are malignant tumors, usually adenocarcinomas arising from the epithelial cells of the lactiferous ducts in the mammary gland lobules (Fig. B1.6A). Metastatic cancer cells that enter a lymphatic vessel usually pass through two or three groups of lymph nodes before entering the venous system. Interference with the lymphatic drainage by cancer may cause lymphedema (edema, excess fluid in the subcutaneous tissue), which in turn may result in deviation of the nipple and a thickened, leather-like appearance of the skin. Prominent or puffy skin between dimpled pores give it an orange-peel appearance ( peau dorange sign). Larger dimples (fingertip size or bigger) result from cancerous invasion of the glandular tissue and fibrosis (fibrous degeneration), which causes shortening or places traction on the suspensory ligaments. Subareolar breast cancer may cause inversion of the nipple by a similar mechanism involving the lactiferous ducts. Breast cancer typically spreads by means of lymphatic vessels (lymphogenic metastasis), which carry cancer cells from the breast to the lymph nodes, chiefly those in the axilla. The cells lodge in the nodes, producing nests of tumor cells (metastases). Abundant communications among lymphatic pathways and among axillary, cervical, and parasternal nodes may also cause metastases from the breast to develop in the supraclavicular lymph nodes, the opposite
breast, or the abdomen. Because most of lymphatic drainage of the breast is to the axillary lymph nodes, they are the most common site of metastasis from a breast cancer. Enlargement of these palpable nodes suggests the possibility of breast cancer and may be key to early detection. However, the absence of enlarged axillary lymph nodes is no guarantee that metastasis from a breast cancer has not occurred because the malignant cells may have passed to other nodes, such as the infraclavicular and supraclavicular lymph nodes. The posterior intercostal veins drain into the azygos/hemiazygos system of veins alongside the bodies of the vertebrae (Fig. 1.31B) and communicate with the internal vertebral venous plexus surrounding the spinal cord. Cancer cells can also spread from the breast by these venous routes to the vertebrae and from there to the cranium and brain. Cancer also spreads by contiguity (invasion of adjacent tissue). When breast cancer cells invade the retromammary space (Fig. 1.20), attach to or invade the deep pectoral fascia overlying the pectoralis major, or metastasize to the interpectoral nodes, the breast elevates when the muscle contracts. This movement is a clinical sign of advanced cancer of the breast. To observe this upward movement, the physician has the patient place her hands on her hips and press while pulling her elbows forward to tense her pectoral muscles.
Mammography
Radiographic examination of the breasts, or mammography, is one of the techniques used to detect breast masses (Fig. B1.6B). A carcinoma appears as a large, jagged density in the mammogram (upper two arrows in Fig. B1.6C).
110
1 / THORAX
Skin dimpling Cancer Dimpling
Retracted nipple
Retracted signs (B) Mammography
Edema of the skin (Peau d'orange sign)
Nipple retraction and deviation
Abnormal contours (A) Carcinoma of the breast (C) Mammogram
Figure B1.6
The skin is thickened over the tumor. The lower arrow points to the depressed nipple. Surgeons use mammography as a guide when removing breast tumors, cysts, and abscesses.
Surgical Incisions of the Breast
Incisions are placed in the inferior breast quadrants when possible because these quadrants are less vascular than the superior ones. The transition between the thoracic wall and breast is most abrupt inferiorly, producing a line, crease, or deep skin foldthe inferior cutaneous crease. Incisions made along this crease will be least evident and may actually be hidden by overlap of the breast. Incisions that must be made near the areola or on the breast itself are usually directed radially to either side of the nipple (Langer tension lines run transversely here; see the Introduction) or circumferentially. Mastectomy (breast excision) is not as common as it once was as a treatment for breast cancer. In simple mastectomy, the breast is removed down to the retromammary
space. Radical mastectomy, a more extensive surgical procedure, involves removal of the breast, pectoral muscles, fat, fascia, and as many lymph nodes as possible in the axilla and pectoral region. In current practice, often only the tumor and surrounding tissues are removeda lumpectomy or quadrantectomy (known as breast-conserving surgery, a wide local excision)followed by radiation therapy (Goroll, 2000).
Polymastia, Polythelia, and Amastia
Polymastia (supernumerary breasts) or polythelia (accessory nipples) may occur superior or inferior to the normal pair, occasionally developing in the axillary fossa or anterior abdominal wall (Figs. B1.7 and SA1.5). Supernumerary breasts usually consist of only a rudimentary nipple and areola, which may be mistaken for a mole (nevus) until they change pigmentation with the normal nipples during pregnancy. However, glandular tissue may also be present and further develop with lactation. Extra breasts may appear
CLINICALLY ORIENTED ANATOMY
111
Breast Cancer in Men
Approximately 1.5% of breast cancers occur in men. As in women, the cancer usually metastasizes to lymph nodes but also to bone, pleura, lung, liver, and skin. Carcinoma of the breast affects approximately 1000 men per year in the United States (Swartz, 2002). A visible and/or palpable subareolar mass or secretion from a nipple may indicate a malignant tumor. Breast cancer in males tends to infiltrate the pectoral fascia, pectoralis major, and apical lymph nodes in the axilla. Although breast cancer is uncommon in men, the consequences are serious because they are frequently not detected until extensive metastases have occurredfor example, in bone.
Accessory breast Accessory nipples
Mammary ridge
Gynecomastia
Slight temporary enlargement of the breasts is a normal occurrence (frequency 70%) in males at puberty (age 1012 years). Breast hypertrophy in males after puberty (gynecomastia) is relatively rare ( 1%) and may be age related or drug related (e.g., after treatment with diethylstilbestrol for prostate cancer). Gynecomastia may also result from an imbalance between estrogenic and androgenic hormones or from a change in the metabolism of sex hormones by the liver. Thus a finding of gynecomastia should be regarded as a symptom, and an evaluation must be initiated to rule out important potential causes, such as suprarenal and testicular cancers or cirrhosis (Goroll, 2000). Approximately 40% of postpubertal males with Klinefelter syndrome (XXY trisomy) have gynecomastia (Moore et al., 2000).
Figure B1.7
anywhere along a line extending from the axilla to the grointhe location of the embryonic mammary ridge (the milk line) from which the breasts develop (Moore and Persaud, 2003), and along which breasts develop in animals with multiple breasts. In either sex, there may be no breast development (amastia), or there may be a nipple and/or areola, but no glandular tissue.
THE BOTTOM LINE: The mammary glands are in the subcutaneous tissue of the breast, overlying the pectoralis major and serratus anterior muscles and associated deep fascia (the bed of the breast). Lobules of glandular tissue converge toward the nipple, each having its own lactiferous duct, which opens there. The superior lateral quadrant of the breast has the most glandular tissue, largely owing to an extension toward or into the axilla (axillary process) and, therefore, is the site of most tumors. The breast is served by the internal thoracic and lateral thoracic vessels, and the 2nd6th intercostal vessels and nerves. Most lymph from the breast drains to the axillary lymph nodes; this is significant in breast cancer. Because the mammary glands and the axillary lymph nodes are superficial, the ability to palpate primary and metastatic tumors during routine breast examination enables early detection and treatment.
Surface Anatomy of the Thoracic Wall Musculature and Breasts
The breasts are the most prominent surface features of the anterior thoracic wall, especially in women. Except when there is an overabundance of subcutaneous tissue, the breasts in men are mostly an accentuation of the contour of the pectoralis major muscles, highlighted by the presence of the nipple in the 4th intercostal space, lateral to the MCL. In the moderately athletic individual, the contour of the pectoralis major muscles is apparent, separated in the midline by the intermammary cleft overlying the sternum, with the lateral border forming the anterior axillary fold (Fig. SA1.4). Inferolaterally, forming about a third of the bed of the breast, finger-like slips, or digitations of the serratus anterior, have a
112
1 / THORAX
Axilla Lateral border of pectoralis major Lateral border of latissimus dorsi Digitations of serratus anterior External abdominal oblique Ribs
Figure SA1.4
serrated (sawtooth) appearance as they attach to the ribs and interdigitate with the external oblique. The inferior ribs and costal margins are often apparent, especially when the abdominal muscles are contracted to pull the belly in. The intercostal musculature per se is not normally evident; however, in (rare) cases in which there is an absence or atrophy of the intercostal musculature, the intercostal spaces become apparent during inspiration, when they are concave, and expiration, when they protrude. Variation in the size, shape, and symmetry of female finger-like slips, or digitations of the serratus anterior, have a serrated (sawtooth) appearance as they attach to the ribs and intergitate with the external oblique. The inferior ribs and costal margins are often apparent, especially when the abdominal muscles are contracted to pull the belly in. The intercostal musculature per se is not evident
normally; however, in (rare) cases where there is an absence or atrophy of the intercostal musculature, the intercostal spaces become apparent during inspiration, when they are concave, and expiration, when they protrude. Variation in the size, shape, and symmetry of female breastseven between the two breasts of one personis the rule, not the exception. Their flattened superior surfaces show no sharp demarcation from the anterior surface of the thoracic wall, but laterally and inferiorly, their borders are well defined (Fig. SA1.5). The median depression separating the breasts is the intermammary cleft. A venous pattern over the breasts is often visible, especially during pregnancy. The nipple is surrounded by the slightly raised and circular pigmented areola, the color of which depends on the womans complexion. The areola usually darkens during pregnancy and retains the darkened pigmentation thereafter. The areola is normally dotted with the papular openings of the areolar glands (sebaceous glands in the skin forming the areola). On occasion, one or both nipples are inverted; this minor congenital anomaly may make breast feeding difficult. In men and young nulliparous womenthose who have never borne a viable childwith moderate breast size, the nipple lies anterior to the 4th intercostal space, approximately 10 cm from the AML. However, the position of nipples varies considerably with breast size in women, especially multiparous womenthose who have given birth to viable children at least twice. Consequently, because of variations in size and shape, the nipples are not a reliable guide to the 4th intercostal spaces in adult females.
Site of axillary tail Anterior axillary fold Areola Nipple
Body of sternum Intermammary cleft
Site of xiphoid process Supernumerary nipple (polythelia)
Figure SA1.5
Viscera of the Thoracic Cavity
When sectioned transversely, it is apparent that the thoracic cavity is kidney shaped: a transversely ovoid space deeply indented posteriorly by the thoracic vertebral column and the posteromedial parts of the ribs (heads and necks), which ar-
ticulate with it (Fig. 1.23A). The thoracic cavity is divided into three compartments (Figs. 1.23A & C ): Right and left pulmonary cavities, bilateral compartments, which contain the lungs and pleurae (lining membranes) and occupy the majority of the thoracic cavity.
Você também pode gostar
- The Anatomy of the Human Peritoneum and Abdominal Cavity: Considered from the Standpoint of Development and Comparative AnatomyNo EverandThe Anatomy of the Human Peritoneum and Abdominal Cavity: Considered from the Standpoint of Development and Comparative AnatomyAinda não há avaliações
- Documents - Pub Surgical Anatomy of Breast Management of Advanced Carcinoma BreastDocumento53 páginasDocuments - Pub Surgical Anatomy of Breast Management of Advanced Carcinoma BreastРоман ПолежаевAinda não há avaliações
- Anatomy 06 - Axilla (Pre Med 101)Documento8 páginasAnatomy 06 - Axilla (Pre Med 101)Navoda Dulshan PereraAinda não há avaliações
- 4) Mammary Gland 220413 Upnm2Documento22 páginas4) Mammary Gland 220413 Upnm2AaronMaroonFive100% (1)
- Nerve Entrapment SyndromeDocumento8 páginasNerve Entrapment SyndromeHengameh JavaheryAinda não há avaliações
- Idoc - Pub Anatomy-Viva PDFDocumento6 páginasIdoc - Pub Anatomy-Viva PDFhieulee84Ainda não há avaliações
- Popliteal Fossa and LegDocumento40 páginasPopliteal Fossa and LegRaj Shekhar SinghAinda não há avaliações
- Anatomy (302) - 1Documento82 páginasAnatomy (302) - 1Shehzad Noman SajidAinda não há avaliações
- 5 - Anatomy of The BreastDocumento18 páginas5 - Anatomy of The Breasthabtsh habshaAinda não há avaliações
- Peritoneal Anatomy Lecture NotesDocumento4 páginasPeritoneal Anatomy Lecture Noteschc300Ainda não há avaliações
- Section 2 The Female Genital Organs: Gonad - Conveying Ducts - Accessory GlandsDocumento29 páginasSection 2 The Female Genital Organs: Gonad - Conveying Ducts - Accessory Glandssomebody_maAinda não há avaliações
- Curs Pelvis PerineuDocumento101 páginasCurs Pelvis PerineuCiprianTeodorulAinda não há avaliações
- Surgical Anatomy of The Biliary TractDocumento5 páginasSurgical Anatomy of The Biliary TracthoangducnamAinda não há avaliações
- Pectoral Region & AxillaDocumento18 páginasPectoral Region & AxillaMohammad PharaonAinda não há avaliações
- BREAST Development TSADocumento62 páginasBREAST Development TSAshirley_ling_15100% (1)
- Femoral Sheath and Femoral TriangleDocumento23 páginasFemoral Sheath and Femoral TriangleSamiha Haq100% (2)
- Arteries of Upper Limb.Documento16 páginasArteries of Upper Limb.Shimmering Moon100% (1)
- Face and Scalp ANATOMYDocumento60 páginasFace and Scalp ANATOMYpuliyogareAinda não há avaliações
- Thoracic and Lumbar Spine Anatomy: DR .S.NizamudeenDocumento57 páginasThoracic and Lumbar Spine Anatomy: DR .S.NizamudeenPogo LocoAinda não há avaliações
- Lymphatic Drainage of Breast FINALDocumento30 páginasLymphatic Drainage of Breast FINALMuhammad Azhar Qureshi100% (1)
- Anatomy Lecture Notes Unit 7 Circulatory System - The Blood VesselsDocumento10 páginasAnatomy Lecture Notes Unit 7 Circulatory System - The Blood VesselsIssac LauAinda não há avaliações
- Anterior Triangle of The Neck IIDocumento49 páginasAnterior Triangle of The Neck IIvrajAinda não há avaliações
- 104 Skull, Mandible & The Facial BonesDocumento68 páginas104 Skull, Mandible & The Facial BonesSam Tagarda100% (1)
- Anatomy Levator AniDocumento10 páginasAnatomy Levator Anidr_diyanAinda não há avaliações
- Neck Triangles (Regional Anatomy) Anterior Triangle Borders Arteries Veins Nerves MiscDocumento6 páginasNeck Triangles (Regional Anatomy) Anterior Triangle Borders Arteries Veins Nerves Misczara_emmeAinda não há avaliações
- Brachial PlexusDocumento9 páginasBrachial PlexusKhadeeja NaqviAinda não há avaliações
- Joints of Upper LimbDocumento70 páginasJoints of Upper LimbHaania KhanAinda não há avaliações
- Neuro AnatomyDocumento23 páginasNeuro AnatomysachinylibAinda não há avaliações
- Genital ProlapseDocumento9 páginasGenital Prolapsesher singhAinda não há avaliações
- Pelvis and Perinium 2019Documento59 páginasPelvis and Perinium 2019Vuluwa GeorgeAinda não há avaliações
- Gross Anatomy of The Pelvis & Perineum DR Ogedengbe O.ODocumento162 páginasGross Anatomy of The Pelvis & Perineum DR Ogedengbe O.OKolawole Adesina KehindeAinda não há avaliações
- Upper LimbDocumento54 páginasUpper LimbMar YAinda não há avaliações
- Anatomy SpleenDocumento32 páginasAnatomy SpleenBijo K BennyAinda não há avaliações
- Nerves of Upper LimbDocumento24 páginasNerves of Upper LimbShimmering MoonAinda não há avaliações
- A Respiratory System Histology 16-12-14Documento33 páginasA Respiratory System Histology 16-12-14Suhas KapseAinda não há avaliações
- Anatomy VivaDocumento5 páginasAnatomy Vivantege stuartAinda não há avaliações
- 16-Genital ProlapseDocumento37 páginas16-Genital Prolapseapi-3703352Ainda não há avaliações
- Axilla and Brachial PlexusDocumento22 páginasAxilla and Brachial Plexusromaisa akhtarAinda não há avaliações
- Obturator NerveDocumento3 páginasObturator NerveDr santoshAinda não há avaliações
- Anatomy Lower LimbDocumento4 páginasAnatomy Lower Limbch yaqoobAinda não há avaliações
- Upper LimbDocumento31 páginasUpper LimbNandhana Kattuparambil SunojAinda não há avaliações
- Erb's PointDocumento14 páginasErb's PointRohit SharmaAinda não há avaliações
- Orbital Anatomy: JI Georgemar V. Arana JRDocumento49 páginasOrbital Anatomy: JI Georgemar V. Arana JRGeorgemar AranaAinda não há avaliações
- Anatomy TopoDocumento62 páginasAnatomy TopoDoina GoreanuAinda não há avaliações
- BreastDocumento49 páginasBreastcryphonexyAinda não há avaliações
- Upper Limb - Pectoral Region, Scapular Region, Axilla & Brachial PlexusDocumento12 páginasUpper Limb - Pectoral Region, Scapular Region, Axilla & Brachial Plexusewijayapala100% (1)
- ORGAN OF VISION. Clinical Anatomy and Physiology (Lecture by M. Bezugly MD, PH.D.)Documento9 páginasORGAN OF VISION. Clinical Anatomy and Physiology (Lecture by M. Bezugly MD, PH.D.)Azra AzmunaAinda não há avaliações
- AIIMS November 2006 AnatomyDocumento5 páginasAIIMS November 2006 Anatomyprasun_vAinda não há avaliações
- BonesDocumento27 páginasBonesADELAJA SAMUELAinda não há avaliações
- The Shoulder JointDocumento17 páginasThe Shoulder JointBhargavAinda não há avaliações
- Upper Limb: Organization FunctionDocumento33 páginasUpper Limb: Organization FunctionAhmed Nabiel El-Jaliel100% (1)
- Orbital AnatomyDocumento45 páginasOrbital AnatomyDevdutta NayakAinda não há avaliações
- AnatomyDocumento74 páginasAnatomyhafeez khanAinda não há avaliações
- Joint of Lower LimbDocumento16 páginasJoint of Lower LimbZA ID100% (1)
- The Upper Extremity: Arm Muscles, Axilla, Brachial PlexusDocumento37 páginasThe Upper Extremity: Arm Muscles, Axilla, Brachial Plexusdrkadiyala2Ainda não há avaliações
- 1) Femal Pelvis&fetal SkullDocumento36 páginas1) Femal Pelvis&fetal SkullHayder MuthanaAinda não há avaliações
- Anatomy Lab 6Documento16 páginasAnatomy Lab 6Mariam2180Ainda não há avaliações
- Histology SummaryDocumento24 páginasHistology SummaryaelsehamyAinda não há avaliações
- Nerves of Lower Limb and Their Injuries: Learning ObjectivesDocumento8 páginasNerves of Lower Limb and Their Injuries: Learning ObjectivesUloko ChristopherAinda não há avaliações
- Female Reproductive SystemDocumento2 páginasFemale Reproductive SystemMarian FloresAinda não há avaliações
- ThesisDocumento108 páginasThesisvasantvj100% (2)
- Characterization of A Preclinical Model of Simultaneous Breast and Ovarian Cancer ProgressionDocumento6 páginasCharacterization of A Preclinical Model of Simultaneous Breast and Ovarian Cancer ProgressionYuda AlhabsyAinda não há avaliações
- BreastDocumento104 páginasBreastRamesh ReddyAinda não há avaliações
- Seminar On Physiology of PuerperiumDocumento15 páginasSeminar On Physiology of Puerperiumvarshasharma05100% (3)
- Bovine Mastitis SVDocumento62 páginasBovine Mastitis SVSatyavrat SinghAinda não há avaliações
- reviewAP BreastDocumento16 páginasreviewAP BreastPriyankaAinda não há avaliações
- New NORMAL PUERPERIUMDocumento21 páginasNew NORMAL PUERPERIUMvarshaAinda não há avaliações
- Breast Feeding GuideDocumento22 páginasBreast Feeding GuideAnonymous SQNcItqXQnAinda não há avaliações
- Experiment 1: Isolation of Casein, Hydrolysis and NeutralizationDocumento7 páginasExperiment 1: Isolation of Casein, Hydrolysis and NeutralizationNhess EstradaAinda não há avaliações
- PuerperiumDocumento36 páginasPuerperiumGirish WaruAinda não há avaliações
- A. Comprehensive NCP For Case Study and Case Presentation IDocumento33 páginasA. Comprehensive NCP For Case Study and Case Presentation IFaith BugtongAinda não há avaliações
- Artículo Adipocitos Blancos, Pardos y RosadosDocumento13 páginasArtículo Adipocitos Blancos, Pardos y RosadosCarlos Felipe MeloAinda não há avaliações
- Physiology of Lactation: Prepared By: Fy MSC NursingDocumento32 páginasPhysiology of Lactation: Prepared By: Fy MSC NursingSùjâl PätídàrAinda não há avaliações
- NCM 107: Rle Module 3M: Cebu Doctors' University College of Nursing Mandaue City, CebuDocumento29 páginasNCM 107: Rle Module 3M: Cebu Doctors' University College of Nursing Mandaue City, CebuDominic De GraciaAinda não há avaliações
- Milk - A Review On Its Synthesis, Composition, and Quality Assurance in Dairy IndustryDocumento5 páginasMilk - A Review On Its Synthesis, Composition, and Quality Assurance in Dairy IndustryAdhiAinda não há avaliações
- Anatomy and Physiology BreastDocumento3 páginasAnatomy and Physiology BreastJames Daniel CodamonAinda não há avaliações
- Obg PresentationDocumento53 páginasObg PresentationpriyankaAinda não há avaliações
- Review For The 2° Semester Exam Alessandro Mo6a, UVVG, 3 YearDocumento9 páginasReview For The 2° Semester Exam Alessandro Mo6a, UVVG, 3 Yeardjxela89Ainda não há avaliações
- Physiology of LactationDocumento3 páginasPhysiology of LactationAswathy Chandran100% (1)
- Efficient MilkingDocumento60 páginasEfficient MilkingOman SetiyantoAinda não há avaliações
- Human Patho Practical 1 WorksheetDocumento3 páginasHuman Patho Practical 1 Worksheetcheng eugeneAinda não há avaliações
- Brest Lump History TakingDocumento3 páginasBrest Lump History Takinganon_619577898Ainda não há avaliações
- Module 5 Case Study PresentationDocumento93 páginasModule 5 Case Study PresentationEDULLANTES ANA MAEAinda não há avaliações
- Kuliah Kelainan PayudaraDocumento44 páginasKuliah Kelainan PayudaradewiswahyuAinda não há avaliações
- L-02 - Evaluation of Mammary GlandsDocumento30 páginasL-02 - Evaluation of Mammary GlandsNadirAliAinda não há avaliações
- A Case Study of A Patient With PIHDocumento19 páginasA Case Study of A Patient With PIHJellou MacAinda não há avaliações
- N64.4 Mastodynia: C73 Malignant Neoplasm of Thyroid GlandDocumento1 páginaN64.4 Mastodynia: C73 Malignant Neoplasm of Thyroid Glanddebby nirmasariAinda não há avaliações
- Managementtoimproveneonatepigletsurvival Oliviero 2013Documento8 páginasManagementtoimproveneonatepigletsurvival Oliviero 2013Eduardo ViolaAinda não há avaliações
- Anatomy of The Breast: Alison J. DarlingtonDocumento8 páginasAnatomy of The Breast: Alison J. DarlingtonValir HusleAinda não há avaliações
- Love Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)No EverandLove Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)Nota: 3 de 5 estrelas3/5 (1)
- LIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionNo EverandLIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionNota: 4 de 5 estrelas4/5 (404)
- By the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsNo EverandBy the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsAinda não há avaliações
- The Age of Magical Overthinking: Notes on Modern IrrationalityNo EverandThe Age of Magical Overthinking: Notes on Modern IrrationalityNota: 4 de 5 estrelas4/5 (31)
- Summary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisNo EverandSummary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisNota: 4.5 de 5 estrelas4.5/5 (42)
- ADHD is Awesome: A Guide to (Mostly) Thriving with ADHDNo EverandADHD is Awesome: A Guide to (Mostly) Thriving with ADHDNota: 5 de 5 estrelas5/5 (3)
- Think This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeNo EverandThink This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeNota: 2 de 5 estrelas2/5 (1)
- Summary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedNo EverandSummary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedNota: 4.5 de 5 estrelas4.5/5 (82)
- Cult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryNo EverandCult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryNota: 4 de 5 estrelas4/5 (46)
- The Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaNo EverandThe Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaNota: 4.5 de 5 estrelas4.5/5 (266)
- The Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsNo EverandThe Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsNota: 4 de 5 estrelas4/5 (4)
- The Obesity Code: Unlocking the Secrets of Weight LossNo EverandThe Obesity Code: Unlocking the Secrets of Weight LossNota: 4 de 5 estrelas4/5 (6)
- Manipulation: The Ultimate Guide To Influence People with Persuasion, Mind Control and NLP With Highly Effective Manipulation TechniquesNo EverandManipulation: The Ultimate Guide To Influence People with Persuasion, Mind Control and NLP With Highly Effective Manipulation TechniquesNota: 4.5 de 5 estrelas4.5/5 (1412)
- Raising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsNo EverandRaising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsNota: 5 de 5 estrelas5/5 (1)
- Dark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.No EverandDark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Nota: 4.5 de 5 estrelas4.5/5 (110)
- Why We Die: The New Science of Aging and the Quest for ImmortalityNo EverandWhy We Die: The New Science of Aging and the Quest for ImmortalityNota: 4 de 5 estrelas4/5 (5)
- Raising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsNo EverandRaising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsNota: 4.5 de 5 estrelas4.5/5 (170)
- Summary: Limitless: Upgrade Your Brain, Learn Anything Faster, and Unlock Your Exceptional Life By Jim Kwik: Key Takeaways, Summary and AnalysisNo EverandSummary: Limitless: Upgrade Your Brain, Learn Anything Faster, and Unlock Your Exceptional Life By Jim Kwik: Key Takeaways, Summary and AnalysisNota: 5 de 5 estrelas5/5 (8)
- When the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisNo EverandWhen the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisNota: 3.5 de 5 estrelas3.5/5 (2)
- Mindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessNo EverandMindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessNota: 4.5 de 5 estrelas4.5/5 (328)
- Troubled: A Memoir of Foster Care, Family, and Social ClassNo EverandTroubled: A Memoir of Foster Care, Family, and Social ClassNota: 4.5 de 5 estrelas4.5/5 (27)
- Dark Psychology: Learn To Influence Anyone Using Mind Control, Manipulation And Deception With Secret Techniques Of Dark Persuasion, Undetected Mind Control, Mind Games, Hypnotism And BrainwashingNo EverandDark Psychology: Learn To Influence Anyone Using Mind Control, Manipulation And Deception With Secret Techniques Of Dark Persuasion, Undetected Mind Control, Mind Games, Hypnotism And BrainwashingNota: 4 de 5 estrelas4/5 (1138)
- The Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeNo EverandThe Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeNota: 4.5 de 5 estrelas4.5/5 (253)