Escolar Documentos
Profissional Documentos
Cultura Documentos
I - Shoulder Dystocia
Enviado por
Manoharan ViswanathanDescrição original:
Direitos autorais
Formatos disponíveis
Compartilhar este documento
Compartilhar ou incorporar documento
Você considera este documento útil?
Este conteúdo é inapropriado?
Denunciar este documentoDireitos autorais:
Formatos disponíveis
I - Shoulder Dystocia
Enviado por
Manoharan ViswanathanDireitos autorais:
Formatos disponíveis
1
I: Shoulder Dystocia
ob Cobbo, M.D.
tiabetb ate,, M.D.
0ojecl|ves
At the end of this chapter participants will be able to:
1. List the risk factors for shoulder dystocia.
2. Utilise a systematic approach to managing a shoulder dystocia using the
HELPERR mnemonic.
3. Demonstrate appropriate manoeuvres to reduce a shoulder dystocia using a
maternal-fetal mannequin.
lrlroducl|or
All in the delivery suite are tired yet exhilarated; the long process of birth is soon to
be completed. After two hours of pushing, the infants head squeezes over the
perineum and you wait for the shoulders to restitute and birth, but there is no
movement. You attempt to facilitate the birth of the anterior shoulder with gentle
assistance, but the head appears to be retracting back into the birth canal. The
anterior shoulder is stuck, impeded by the pubic bone of his mothers pelvis. You
realise that you are dealing with a shoulder dystocia. The atmosphere in the room
changes from one of excitement and anticipation to one filled with confusion, anxiety
and fear. A focused calm approach to this emergency is needed. It is essential that
you perform the manoeuvres to free the impaction skilfully, and that you direct
assisting caregivers efforts effectively.
0efinition
Shoulder dystocia is defined as impaction of the anterior shoulder against the
maternal symphysis pubis after the fetal head has birthed, and occurs when the
bisacromial diameter (breadth of the shoulders) exceeds the diameter of the pelvic
inlet. Attempts to standardise this somewhat subjective definition have referred to
head-to-body time intervals of equal to, or more than, 60 seconds, or the use of any
ancillary procedures to effect birth as criteria for making this diagnosis.
1,2
l: 3rou|der 0ysloc|a
2
lncidence
The overall incidence of shoulder dystocia varies based on fetal weight, occurring in
0.3 to one percent of infants with a birth weight of 2500 to 4000 grams, and
increasing to five to seven percent in infants weighing 4000 to 4500 grams. Over 50
percent of shoulder dystocias occur in the normal birth weight fetus and are
unanticipated.
Risk Factors
A number of antenatal and intrapartum factors have been associated with an
increased incidence of encountering a shoulder dystocia. Associated antenatal
factors include prior shoulder dystocia, gestational diabetes, post-dates pregnancy,
macrosomia, short stature, and abnormal pelvic anatomy. Intrapartum warning signs
that should signal a potential shoulder dystocia are protracted active phase of the
first stage of labour, prolonged second stage with head bobbing, and use of forceps
or vacuum to effect delivery.
Operative vaginal deliveries with either vacuum or forceps carry a significant risk for
subsequent shoulder dystocia. The fetus is normally in a position of flexion and
shoulder adduction while in the birth canal. As the instrument is placed on the fetal
vertex and traction instituted, the vertex is pulled away from the body causing the
neck to elongate and the shoulder to abduct. This produces an increased bisacromial
diameter or in a sense, wider shoulders making shoulder entrapment by the
maternal symphysis pubis more likely. Vacuum and forceps deliveries increase the
risk of a brachial plexus injury to odds ratio 2.7 (95 percent CI 2.4 to 3.1) and 3.4
percent (95 percent CI 2.7 to 4.3) respectively.
5
(Category C)
There is not enough evidence to evaluate the use of symphysis-fundal height
measurements for predicting macrosomia.
2
(Category C) Unfortunately, ultrasound is
a poor predictor of birth weight in diabetic or non-diabetic pregnancies complicated
by macrosomia.
4,9
(Category C) Based on existing evidence, routine late pregnancy
ultrasound in low risk or unselected populations does not confer benefit for mother or
baby.
4
(Category A)
Voro|d|ly ard Vorla||ly
Soft tissue injuries are the most common maternal complication, with increased rates
of third and fourth degree extension or tear, and subsequent potential for
rectovaginal fistula formation. Post-partum haemorrhage due to uterine atony or birth
canal trauma is also more common. Symphyseal diastasis and uterine rupture occur
rarely, although symphyseal separation and transient femoral neuropathy have been
associated with the McRoberts manoeuvre.
6
(Category C).
Among the most common fetal complications of shoulder dystocia are brachial plexus
palsies, occurring in seven to 20 percent of infants whose births were diagnosed with
shoulder dystocia. Nearly all recover within six to 12 months, with only one to two
l: 3rou|der 0ysloc|a
3
percent risking permanent injury. Erbs palsy is the more common, involving C5-6
nerve roots. Klumpkes palsy involves C8-T1 and is less common. Although shoulder
dystocia is commonly blamed for these palsies, in-utero positioning of the fetus may
contribute to their aetiology.
7
Clavicular and humeral fractures are additional potential injuries associated with
shoulder dystocia. Fractures of the clavicle typically heal without complication, but
may be associated with injury to lung and underlying vascular structures. Fractures of
the humerus typically heal without deformity.
Fetal hypoxia is a serious potential complication and can result in permanent
neurological damage or even death if there are significant delays in reduction of the
impacted shoulder and birth of the fetus. Once the fetal head has birthed, it must be
assumed that the umbilical cord is compressed between the fetal body and the
mothers pelvis. During this time, the fetal pH will drop by an estimated .04 per minute
until the condition is corrected. In a non-compromised fetus with an uncomplicated
labour course, it will take seven minutes for the cord pH to decline from a normal of
7.25 to a danger level of 6.97. Resuscitation of these neonates becomes increasingly
difficult, as persistent fetal circulation becomes more common.
Preverl|or
The literature provides no clear evidence to recommend the use of elective
caesarean delivery for the prevention of shoulder dystocia in women at risk. Analytic
decision models have estimated that 3,695 elective caesarean deliveries would be
needed to prevent one permanent brachial plexus injury among non-diabetic women
with an estimated fetal weight greater than 4500 grams.
9
A policy of routine
caesarean delivery for all infants with macrosomia would result in at least a five to six
fold increase in caesarean rate in this group of women. Spontaneous vaginal birth
should be expected for most babies who are estimated antenatally to be
macrosomic, but anticipatory management during labour should be carefully
organised.
Maintenance of good glycaemic control for diabetic women has demonstrated a
reduction in fetal birth weight, which may translate into lower shoulder dystocia and
brachial plexus palsy rates. While women with insulin-requiring gestational diabetes
have a lower incidence of macrosomia when induction of labour at term is performed,
this did not reduce the risk of maternal or neonatal morbidity from shoulder
dystocia.
10
(Category B) Induction of labour for suspected fetal macrosomia in non-
diabetic women also does not appear to alter the risk of maternal or neonatal
morbidity.
11
(Category A)
When shoulder dystocia is anticipated, based on risk factor review, a simple, easy
and effective method of preventing shoulder dystocia is the head and shoulder
manoeuvre to deliver through until the anterior shoulder is visible. This is
accomplished by continuing the momentum of the birth of the fetal head until the
shoulder is visible, without waiting for restitution and rotation of the head.
l: 3rou|der 0ysloc|a
4
Varagererl
Anticipation:
If antenatal or intrapartum risk factors suggest that a shoulder dystocia may be
encountered, many tasks can be accomplished in advance of the birth, through
anticipation and preparation. Key personnel can be called prior to birth and placed on
alert. The woman and her family should be educated about the possibility of a
potentially difficult birth, and can be shown what they may be asked to do in that
event. The womans bladder can be emptied and the room cleared of any
unnecessary clutter, to make room for additional personnel and equipment. A bedpan
should be available to raise the maternal pelvis if stirrups are not available.
Delivering through until the anterior shoulder is visible may be helpful in women
with known shoulder dystocia risk factors.
0eveloping an lnstitutional Plan
A critical step in addressing the emergency management of shoulder dystocia is to
ensure that all hospital personnel who may be involved in the management of this
condition are familiar with their roles and responsibilities. An institutional plan can be
designed to delineate health care providers individual roles, and hospital drills can
be conducted to test and rehearse this plan.
0n-site Assistance
Once shoulder dystocia is diagnosed, the presence of additional assistants in the
birth suite is critical. One person is responsible for recording of events, obtaining
designated equipment and supplies, and notifying the clinician of time intervals.
Documentation of the manoeuvres used and the duration of each manoeuvre may be
valuable to prompt the clinician to move on to other manoeuvres, rather than
persisting in one that is not working.
Additional 8ack-up
A pre-arranged plan should identify members of a team ready to respond to this
emergency. This team may include a general practitioner or an obstetrician, a
paediatrician or neonatologist, one or two midwives to assist with manoeuvres, and a
special care nursery nurse. At least one other provider with maternity or neonatal
skills should be called immediately when a shoulder dystocia is encountered. In large
centres this may be a neonatologist, while at smaller hospitals this may be a GP,
paediatrician or obstetrician. In some rural areas, this individual can be an
emergency room physician or a GP/DMO who comes in from the surgery or home.
An anaesthetist should be called in order to administer medications as needed. A
ward clerk or hospital operator should be available and prepared to assist in
summoning appropriate individuals to the birth suite. This may involve developing a
priority list of individuals to contact, and may be accomplished in part through a
l: 3rou|der 0ysloc|a
5
general overhead page such as Code D: Labour Ward or other appropriate
notification that an obstetric emergency is underway.
Reduction Manoeuvres
Shoulder dystocia becomes obvious after the head emerges and then retracts up
against the perineum, commonly referred to as the turtle sign. Excessive force must
not be applied to the fetal head or neck, and fundal pressure must be avoided. These
activities are unlikely to free the impaction and may cause fetal and maternal injury
while wasting valuable time. If standard levels of traction do not relieve the shoulder
dystocia, the clinician must quickly move to other manoeuvres to aid in birth of the
fetus. The family should be notified of the diagnosis and the staff asked to summon
other personnel.
The clinician attending the birth should direct the activities of the personnel in the
room, much like running a cardiopulmonary arrest code. It is important that other
personnel listen to the directions being given and all act in a team-like fashion to
address this emergency. An individual recording the events should keep time.
Awareness of time duration is essential so that, if one manoeuvre is not successful
after a reasonable amount of time, another manoeuvre can be attempted.
The HELPERR mnemonic is a clinical tool that can provide maternity care providers
with a structured framework in which to deal with an extremely difficult and charged
situation. Although there is no indication that any one of these techniques are
superior to another, together they represent a valuable tool to help clinicians take
effective steps in relieving the impacted shoulder.
14
(Category C) The steps need not
always be done in the same order as the mnemonic suggests; it is more critical that
they be employed efficiently and appropriately. Thirty to 60 seconds is recommended
as the appropriate amount of time to spend on each manoeuvre. Although three to
five minutes may seem like a brief window of time in which to act, it is adequate for
following all of the manoeuvres described in the HELPERR mnemonic. These
manoeuvres are designed to do one of three things:
Increase the functional size of the bony pelvis.
Decrease the bisacromial diameter.
Change the relationship of the bisacromial diameter within the bony pelvis.
h - Call for help
This step refers to activating the pre-arranged plan for personnel to respond with
necessary equipment to the birth suite. If such a pre-arranged plan has not yet been
developed, the appropriate equipment and personnel should be requested, including
someone to assist in neonatal resuscitation, and anaesthesia personnel to assure
that appropriate medications will be immediately available.
l: 3rou|der 0ysloc|a
E - Evaluate for Episiotomy
Episiotomy should be considered in the management of shoulder dystocia. Shoulder
dystocia is a bony impaction, so simply performing an episiotomy will not cause the
shoulder to release. Since the majority of cases of shoulder dystocia can be relieved
with McRoberts manoeuvre and suprapubic pressure, many women can be spared a
surgical incision unless it becomes necessary to make room for the clinicians hand in
the vagina for performing internal manoeuvres. However, as episiotomy is very
difficult to perform when the fetal head is tight against the perineum, clinical
judgement may dictate performing an episiotomy before birth if shoulder dystocia is
strongly anticipated.
L - Legs [7he McRoberts Manoeuvre}
The simplicity of the McRoberts manoeuvre, and its proven effectiveness, make it an
ideal first step in management. The procedure involves flexing the maternal hips,
thus positioning the maternal thighs up onto the maternal abdomen. This simulates
the squatting position, with the advantage of increasing the inlet diameter. Midwives
and family members present at the birth can provide assistance for this manoeuvre.
When anticipated, it is helpful to demonstrate this to family members in advance.
The McRoberts manoeuvre also straightens the lumbosacral lordosis, flattening the
sacral promontory as an obstruction. This procedure simultaneously flexes the fetal
spine, often pushing the posterior shoulder over the sacral promontory and allowing it
to fall into the hollow of the sacrum. When this occurs, the symphysis may rotate over
the impacted shoulder. Finally, the direction of maternal force in this position is
perpendicular to the plane of the inlet. When this manoeuvre is successful, normal
traction should birth the fetus. Birth should be attempted in this position for
approximately 30 to 60 seconds.
The McRoberts manoeuvre alone is believed to relieve more than 40 percent of all
shoulder dystocias and combined with suprapubic pressure and/or episiotomy, over
50 percent of dystocias can be delivered.
15,16
(Category C)
6.7
P - 3uprapubic Pressure
An assistant should attempt external manual suprapubic pressure for approximately
30 to 60 seconds while the delivering clinician continues gentle traction. The
suprapubic hand should be placed over the fetus anterior shoulder, applying
pressure in a CPR style in such a way that the shoulder will adduct or collapse
anteriorly and pass under the symphysis. The pressure should be applied from the
side of the mother that will allow the heel of the assistants hand to move in a
downward and lateral motion on the posterior aspect of the fetus shoulder. The
delivering clinician should direct the assistant as to the correct direction and to the
effectiveness of the effort. Initially, the pressure can be continuous, but if birth is not
accomplished, a rocking motion is recommended to dislodge the shoulder from
behind the pubic symphysis. If this procedure fails, the next procedure should be
immediately attempted. Fundal pressure is never appropriate and only serves to
l: 3rou|der 0ysloc|a
7
worsen the impaction, potentially injuring the fetus or mother. For the same reason,
the woman should not be asked to push until the shoulder has been released.
E - Enter - lnternal manoeuvres [see page 13}
These manoeuvres attempt to manipulate the fetus to rotate the anterior shoulder
into an oblique plane and under the maternal symphysis. This can be accomplished
with either the Rubin or Woods Screw manoeuvre:
1. Alan Rubin, in 1964, described two manoeuvres, now sometimes called
Rubins manoeuvre I and II. The first manoeuvre is to rock the fetus
shoulders from side to side once or twice by pushing on the mothers lower
abdomen. This is the PRESSURE component of the ALSO
HELPERR
mnemonic. The Rubin II manoeuvre consists of inserting the fingers of one
hand vaginally behind the anterior fetal shoulder and pushing the shoulder
toward the fetus chest. Rubin makes the point that this pressure will adduct,
or collapse, the fetus shoulder girdle, reducing its diameter. The ALSO
recommended method refers to pressure behind the anterior shoulder as
Rubin II, and is the basis for the first part of the ENTER component of the
HELPERR mnemonic. The McRoberts manoeuvre can still be applied during
this manoeuvre, and may help facilitate its success.
2. If this is unsuccessful, the Woods Screw manoeuvre can be combined with
the Rubin II manoeuvre. First described by Dr. C. E. Woods in 1943, this
manoeuvre calls for the provider to use the opposite hand to approach the
posterior shoulder from the front of the fetus, and rotate the shoulder toward
the symphysis in the same direction as with the Rubin II manoeuvre.
17
Thus, in
this combination, the provider now has two fingers behind the anterior
shoulder, and two fingers of the other hand in front of the posterior shoulder.
The Rubin II manoeuvre adducts or flexes either the anterior or posterior
shoulder while the Woods screw manoeuvre abducts or extends the posterior
shoulder. This is why the combination of the two manoeuvres may be more
successful than the Woods Screw alone. With this movement, the infants
shoulders rotate and birth much like the turning of a threaded screw. The
Woods Screw manoeuvre frequently requires a large episiotomy to provide
room for posterior manipulation, while the Rubin II manoeuvre generally does
not.
18
3. If the Rubin or Woods manoeuvres fail, the Reverse Woods Screw
manoeuvre may be tried. In this manoeuvre, the fingers of the entering hand
are placed on the posterior shoulder from behind and the attempt is to rotate
the fetus in the opposite direction as the Woods Screw manoeuvre. The
Reverse Woods Screw manoeuvre is identical to the Rubin II manoeuvre
when performed on the posterior shoulder. This rotates the fetal shoulders out
of the impacted position and into an oblique plane from which they can birth.
Much confusion has occurred regarding these manoeuvres, and even leading
obstetric texts have described them differently.
18
These manoeuvres can be very
difficult to perform, particularly when the anterior shoulder is partially wedged
l: 3rou|der 0ysloc|a
8
underneath the symphysis. At times it is necessary to push the posterior shoulder, or
sometimes the anterior shoulder, back up into the pelvis slightly in order to
accomplish the manoeuvres.
R - Remove the Posterior Arm
In this manoeuvre, the posterior arm is removed from the birth canal, so reducing the
bisacromial diameter. This allows the anterior shoulder to collapse as the fetus drops
into the pelvic hollow, freeing the impaction anteriorly. In order to effect this
manoeuvre, the clinician must insert his or her hand far into the vagina and attempt
to locate the posterior arm. Sometimes the arm is displaced behind the fetus and
must be nudged anteriorly. Once the forearm is located, the elbow should be flexed
so that the forearm may be delivered in a sweeping motion over the anterior chest
wall of the fetus. The fetal upper arm should never be grasped and pulled directly, as
this may fracture the humerus. If done correctly, first the posterior hand, then arm
and finally shoulder will be reduced, facilitating birth of the infant. Often, the fetus
rotates in a corkscrew manner as the arm is removed. The anterior shoulder will then
rotate backwards under the symphysis and birth.
R - Roll the woman and 0eliver the Posterior 3houlder
The all-fours McRoberts or Gaskin manoeuvre is a safe, rapid and effective
technique for the reduction of shoulder dystocia. The woman must roll from the
dorsal position to an all-fours McRoberts position. The precise mechanism by which
the Gaskin manoeuvre acts to relieve the shoulder dystocia is unknown. The pelvic
diameters increase when labouring women change from the dorsal recumbent
position.
19
Radiographic studies indicate that pelvic measurements are least
favourable for birth in the dorsal lithotomy position. By rotating to the all-fours
McRoberts position, the true obstetrical conjugate increases by as much as 10 mm
and the sagittal measurement of the pelvic outlet increases up to 20 mm.
20
The fetal shoulder often dislodges during the act of turning from a supine to all-fours
McRoberts position, indicating that this movement alone may be sufficient to allow
enough pelvic change to dislodge the impaction. Additionally, once the position
change is completed, gravitational forces may aid in disimpaction of the fetal
shoulders.
The all-fours McRoberts manoeuvre may be difficult for a woman who is fatigued or
restricted by IVs, fetal monitors, epidural anaesthesia or Foley catheter. The woman
will often need assistance to re-position, given these entrapments. At one facility, all
women with epidural anaesthesia are instructed to perform a shoulder dystocia drill
and practice getting into the all-fours position, in case it is needed later.
21
Consideration should be given to including this as part of antenatal education.
By providing gentle traction downward, the clinician can deliver the posterior shoulder
first with the aid of gravity. The all-fours McRoberts position is compatible with all
intra-vaginal manipulations for shoulder dystocia, but it is incompatible with
suprapubic pressure. The average provider may be disoriented with a birth in this
l: 3rou|der 0ysloc|a
9
position. Some tips are to remember to always go with gravity first, thus provide
gentle traction downward to birth the shoulder closest to the ceiling first. Performing a
few normal births in this position, before encountering an acute need to do so, may
assist the provider in being prepared for more emergent situations.
The order in which these manoeuvres are attempted may be flexible. However, a
logical progression of various efforts is essential to allow adequate time for each one
to potentially accomplish birth. The suggested length of time for each manoeuvre is
meant only as a guideline. Clinical judgment should always guide the progression of
procedures used.
Methods of Last Resort
If the manoeuvres described in the HELPERR mnemonic are unsuccessful after
several attempts, the following techniques have been described as last resort
manoeuvres:
1. Deliberate clavicle fracture
Direct upward pressure on the midportion of the fetal clavicle will result in
fracture and reduce the shoulder-to-shoulder distance.
2. The Zavanelli manoeuvre
Cephalic replacement followed by caesarean delivery involves turning the fetal
head into direct occipito-anterior position (if it has restituted), then flexing the
head and pushing it back into the birth canal. This mechanism is the exact
reverse of birth of the head. Continuous upward pressure is then maintained
on the fetal head until caesarean delivery can be accomplished. Tocolysis
may be a valuable adjunct to this procedure. Before considering cephalic
replacement, an operating team, anaesthesia, and physicians capable of
performing a caesarean delivery must be present. This manoeuvre should
never be attempted if a nuchal cord has been previously clamped and cut.
3. Muscle Relaxation
Musculoskeletal or uterine relaxation can be induced with halothane or other
general anaesthetic. Alternatively, oral or IV nitroglycerin may be used for
uterine relaxation.
4. Abdominal Surgery and Hysterotomy
This technique has been reported to facilitate vaginal birth of the fetus in a
case of severe shoulder dystocia. In a small series of case reports of severe
shoulder dystocia, general anaesthesia was induced and caesarean delivery
performed. The surgeon would then rotate the infant transabdominally through
the hysterotomy incision, allowing the shoulders to rotate, much like a Woods
l: 3rou|der 0ysloc|a
10
Screw manoeuvre. Vaginal extraction was then accomplished by another
clinician.
25
(Category C)
5. Symphysiotomy
Intentional division of the fibrous cartilage of the symphysis pubis under local
anaesthesia has been used successfully in developing countries more than in
Australasia. Reports in the U.S. are related to its use after failed Zavanelli
manoeuvres.
22
Because the procedure takes at least two minutes from the
time a decision is made, if needed, it should be initiated within five to six
minutes of birth of the fetal head and should only be used when all other
manoeuvres have failed and caesarean delivery capability is not available.
23,24
0ocurerlal|or
Documentation of the management of shoulder dystocia should concentrate on the
manoeuvres performed and the duration of the event. Terms like mild, moderate, or
severe shoulder dystocia offer little information about the maternity care that was
provided or future legal issues. The documentation should also include other team
members present and umbilical cord venous and arterial cord pH, if obtained. In case
subsequent nerve palsy develops, it is worthwhile to document which arm was
impacted against the pubis and on which arm manoeuvres were performed for
removal.
3urrary
Shoulder dystocia is a relatively common and dangerous event, but it is difficult to
predict. Almost 50 percent of shoulder dystocias have no antecedent factors.
Anticipation and preparation are key to successful management. In those women
with risk factors, the maternity provider should use the head and shoulder
manoeuvre to continue the momentum and allow the fetus to deliver through until
the anterior shoulder is birthed (rather than waiting for restitution and rotation of the
head to occur). An institutional plan is recommended, in which each member of the
team has an assigned duty. The recommended management of shoulder dystocia is
based on the mnemonic HELPERR, which provides a memory guide and a
structured framework for action which is useful in this crisis. The elements of the
HELPERR mnemonic are all effective, and they should be tried in a logical and calm
sequence. Practice on the mannequin is an essential aid to clinicians who are likely
to encounter this obstetric emergency. The time allotted to each manoeuvre, and the
exact sequence, are best determined by the clinical circumstances and the clinicians
best judgment.
l: 3rou|der 0ysloc|a
11
3urrary ol Tao|e Recorrerdal|ors
Category A
Based on existing evidence, routine late pregnancy ultrasound in low risk or
unselected populations does not confer benefit in predicting macrosomia or reducing
morbidity.
4
Induction of labour for suspected fetal macrosomia in non-diabetic women does not
appear to alter the risk of maternal or neonatal morbidity.
11
Category 8
There is no evidence to support elective birth at term in pregnant women with insulin-
requiring diabetes. While women with insulin-requiring gestational diabetes have a
lower incidence of macrosomia when elective birth is done, this did not reduce the
risk of maternal or neonatal morbidity.
10
Category C
In those women with risk factors, the maternity provider should use the head and
shoulder manoeuvre to continue the momentum and allow the fetus to deliver
through until the anterior shoulder is birthed, without waiting for restitution and
rotation of the head to occur.
7
There is not enough evidence to evaluate the prediction of fetal size by fundal height,
palpation, or ultrasound.
2,3
Shoulder dystocia is associated with instrumental vaginal birth
.5
An institutional plan is recommended, in which each member of the team has an
assigned duty. The team should include a member of the anaesthesia staff.
15
The elements of the HELPERR mnemonic are effective. They should be instituted in
a logical and calm sequence.
18
The majority of shoulder dystocias can be relieved by McRoberts manoeuvre and
suprapubic pressure.
15,16
Documentation of shoulder dystocia management should include manoeuvres
performed, duration, actions of team members, cord pH, and on which arm any
manoeuvres were performed.
5,7
References
1. 8ea|| Vl., el.a|. 0ojecl|ve del|r|l|or ol srou|der dysloc|a: a prospecl|ve eva|ual|or. Ar J 0oslel 0yreco|.
1998:1Z9:931-3Z. (Leve| lll)
2. Ne||sor JP. 3yrprys|s-lurda| re|grl reasurererl |r pregrarcy (Cocrrare Rev|eW). lr: Tne 0ocnrane l|orary, lssue
2, 2000. 0xlord: updale 3ollWare. (Leve| l)
l: 3rou|der 0ysloc|a
12
3. Jorrslore F0, Prescoll RJ, 3lee| JV, el a|. C||r|ca| ard u|lrasourd pred|cl|or ol racrosor|a |r d|aoel|c pregrarcy. 8r J
0oslel 0yreco| 199;103:Z1Z. (Leve| lll)
1 8r|c|er L, Ne||sor JP. Roul|re u|lrasourd |r |ale pregrarcy (aller 21 Wee|s geslal|or) (Cocrrare Rev|eW). lr: Tne
0ocnrane l|orary, lssue 2, 2000. 0xlord: updale 3ollWare. (Leve| l)
5. 0||oerl wV, Neso|ll T3, 0ar|e|sor 8. Assoc|aled Faclors |r 111 cases ol oracr|a| p|exus |rjury. 0oslel 0yreco| 1999
Apr;93(1):53-10. (Leve| lll)
. 0rerrar R8, el a|, 3yrprysea| separal|or ard lrars|erl lerora| reuropalry assoc|aled W|lr lre VcRooerl's
rareuver. ArJ0o0yr, Varcr 1998;1Z8:09-10. (Leve| lll)
Z. 0rerrar R8; 0oodW|r TV. 3rou|der 0ysloc|a; Curr 0p|r 0oslel 0yreco| 0ec, 1998;10():159-3. (Leve| lll)
8. 0rerrar R8, 0uzor|ar J0, 0oodW|r TV. 0oslelr|ca| Vareuvers lor srou|der dysloc|a ard assoc|aled lela| roro|d|ly.
Ar J 0oslel 0yreco|, Jure 1998;1Z8():112-1130. (Leve| lll)
9. Rouse 0J, 0Wer J. 0o|deroerg RL, C||ver 3P. Tre ellecl|veress ard cosls ol e|ecl|ve cesarear de||very lor lela|
racrosor|a d|agrosed oy u|lrasourd. JAVA 199;2Z:1180-. (Leve| lll)
10. 8ou|va|r V, 3lar C, lr|or 0. E|ecl|ve de||very |r d|aoel|c pregrarl Worer (Cocrrare Rev|eW). lr: Tne 0ocnrane
l|orary, lssue 2, 2000. 0xlord: updale 3ollWare. (Leve| l)
11. lr|or 0, 8ou|va|r V. lrducl|or ol |aoour lor suspecled lela| racrosor|a (Cocrrare Rev|eW). lr: Tne 0ocnrane l|orary,
lssue 2, 2000. 0xlord: updale 3ollWare. (Leve| l)
12. Corer 8F, el. a|. Tre |rc|derce ard sever|ly ol srou|der dysloc|a corre|ales W|lr a sorograpr|c reasurererl ol
asyrrelry |r pal|erls W|lr d|aoeles. 1999;1:19Z-201 (Leve| lll)
13. verspyc| E, 0oll|rel F. le||ol VF, el. A|. NeWoorr srou|der dysloc|a W|dlr: a prospecl|ve sludy ol 2222 corsecul|ve
reasurererls. 8r J 0oslel 0yreco| 1999;10:589-93. (Leve| lll)
11. Arer|car Co||ege ol 0oslelr|c|ars ard 0yreco|og|sls. 3rou|der dysloc|a. AC00 Pracl|ce Pallerrs 0clooer, 199Z;(Z):1-
Z. (Leve| lll)
15. VcFar|ard el a|, Per|rala| 0ulcore ard lre lype ol rareuvers |r srou|der dysloc|a. lrl Jourra| 0yreco| 0oslel 55;219-
21,199. (Leve| lll)
1. 0rerrar el a|. Tre VcRooerls Vareuver lor a||ev|al|or ol srou|der dysloc|a; roW successlu| |s |l. Ar J ol 0oslel
0yreco| 199Z;1Z;5-1199Z. (Leve| lll)
1Z. woods CE. A pr|rc|p|e ol prys|cs as app||cao|e lo srou|der de||very Ar J 0oslel 0yreco| 1913;15:Z9. (Leve| lll)
18. Rarsey P3, el a|. 3rou|der dysloc|a: Rolal|ora| rareuvers rev|s|led. J Reprod Ved 2000;15:85-88. (Leve| lll)
19. 8rurer J, el a|. A|| lours rareuver lor reduc|rg srou|der dysloc|a dur|rg |aoor. Jourra| ol Reproducl|ve Ved|c|re;
1998;13;5:139-112. (Leve| lll)
20. 8ore|| u ard Ferdslror l. A pe|v|relr|c relrod lor lre assessrerl ol pe|v|c ro|dao|||ly. Acla Rad|o| 195Za;1Z:35-3Z0.
(Leve| lll)
21. Veerar AL, 0as||r lV, lurl P, el a|. A reW (o|d) rareuver lor lre raragererl ol srou|der dysloc|a. J Far Pracl
1991;32;25-29. (Leve| lll)
22. 0oodW|r TV, el. a|. Calaslropr|c srou|der dysloc|a ard erergercy syrprys|olory. Ar J 0oslel 0yreco|
199Z;1ZZ:13-1. (Leve| lll)
23. Cr|crlor 0, 3eedal EK. Tre lecrr|que ol syrprys|olory. 3 Alr|car Ved J 193;3Z:22Z-31. (Leve| lll)
21. Varagererl ol |aoor ard de||very corp||cal|ors. (|r) 0oug|as-3lrorre 0peral|ve 0oslelr|cs, 5lr Ed|l|or. Zuspar FP,
0u||||gar EJ (eds.) App|elor ard Large. NorWa||,Correcl|cul. Pages 33Z-8, 1988. (Leve| lll)
25. 0'3raugrressy VJ, lyslerolory lac|||lal|or ol lre vag|ra| de||very ol lre posler|or arr |r a case ol severe srou|der
dysloc|a, 0oslel 0yreco| 0cl 1998;92(1 Pl 2):93-5. (Leve| lll)
l: 3rou|der 0ysloc|a
13
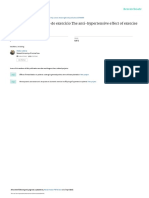
Rubin II
Rubin II + Wood Screw
Reverse Wood Screw
If no rotation occurs, continue
Rubin II and add Wood Screw
Use fingers of the opposite hand
to apply pressure to the front of
the posterior shoulder**
This can help rotation in the same
direction as Rubin II
If shoulders now move into the
oblique attempt delivery
If unsuccessful try to rotate
through 180 degrees to deliver
If LOT/LOL, insert index &
middle fingers of right hand
through introitus at 5 oclock*
Swing fingers up & apply
pressure with fingertips from
behind the anterior shoulder
++
If shoulders move into the
oblique diameter attempt
delivery
If rotation in that direction cannot
be achieved change to Reverse
Wood Screw
Slide fingers down to the back of
the posterior shoulder***
Apply pressure to rotate in the
opposite direction
Attempt delivery if shoulders
move into the oblique
If unsuccessful, continue rotation
through 180 degrees to deliver
DIAGRAM OI 1HL LN1LR' MANOLUVRLS IOR SHOULDLR DYS1OCIA
(using LO1/LOL' position as an example)
(RLMLMBLR: Rubin I = Suprapubic pressure)
**
*
Remove hand on
side of fetal face
If ROT/ROL, insert fingers
of LEFT hand at 7 oclock
***
ALL ATTEMPTS AT ROTATION SHOULD BE COMPLETED WITHIN 1-2 MINUTES
(This page created by Mr Kim Hinshaw MRCOG)
IF UNSUCCESSFUL - MOVE ON TO OTHER MANOEUVRES
++
Você também pode gostar
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeNo EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeNota: 4 de 5 estrelas4/5 (5794)
- S.P Chengalvaraya Naidu v. JagannathDocumento3 páginasS.P Chengalvaraya Naidu v. JagannathManoharan ViswanathanAinda não há avaliações
- The Little Book of Hygge: Danish Secrets to Happy LivingNo EverandThe Little Book of Hygge: Danish Secrets to Happy LivingNota: 3.5 de 5 estrelas3.5/5 (399)
- 2011 Indlaw NCDRC 443Documento3 páginas2011 Indlaw NCDRC 443Manoharan ViswanathanAinda não há avaliações
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryNo EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryNota: 3.5 de 5 estrelas3.5/5 (231)
- 980008002Documento8 páginas980008002Manoharan ViswanathanAinda não há avaliações
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceNo EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceNota: 4 de 5 estrelas4/5 (894)
- Standard For 150Documento86 páginasStandard For 150Mayank GuptaAinda não há avaliações
- The Yellow House: A Memoir (2019 National Book Award Winner)No EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Nota: 4 de 5 estrelas4/5 (98)
- Uniform RulesDocumento23 páginasUniform RulesManoharan ViswanathanAinda não há avaliações
- BIOEN 345: Failure Analysis of Physiology: Lecture 4 May 4, 2020: Vessel PathologiesDocumento45 páginasBIOEN 345: Failure Analysis of Physiology: Lecture 4 May 4, 2020: Vessel PathologiesasdfghjklAinda não há avaliações
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureNo EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureNota: 4.5 de 5 estrelas4.5/5 (474)
- 485 5032 Assignment 1 Greenwich University PassDocumento27 páginas485 5032 Assignment 1 Greenwich University PassThy ThơAinda não há avaliações
- Never Split the Difference: Negotiating As If Your Life Depended On ItNo EverandNever Split the Difference: Negotiating As If Your Life Depended On ItNota: 4.5 de 5 estrelas4.5/5 (838)
- Practice Questions 1 - YoungDocumento12 páginasPractice Questions 1 - Youngejyoung928100% (1)
- Personal Development: Understanding Yourself and Building RelationshipsDocumento6 páginasPersonal Development: Understanding Yourself and Building RelationshipsYelhsa Ramos100% (2)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaNo EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaNota: 4.5 de 5 estrelas4.5/5 (265)
- NCM 105 SyllabusDocumento5 páginasNCM 105 SyllabusHazel Rose0% (1)
- Blue and Pink Psychiatrist Medical ResumeDocumento1 páginaBlue and Pink Psychiatrist Medical ResumeChalysia Katsume MichaelAinda não há avaliações
- SCARED Form ScoringDocumento1 páginaSCARED Form ScoringKaty PuiuAinda não há avaliações
- The Emperor of All Maladies: A Biography of CancerNo EverandThe Emperor of All Maladies: A Biography of CancerNota: 4.5 de 5 estrelas4.5/5 (271)
- Efeito Anti-Hipertensivo Do Exercicio The Anti-HypDocumento9 páginasEfeito Anti-Hipertensivo Do Exercicio The Anti-HypRicardo Tavares ArrudaAinda não há avaliações
- Quality Control Circle - Desk File and WorkDocumento26 páginasQuality Control Circle - Desk File and WorkZuhairi MohamedAinda não há avaliações
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersNo EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersNota: 4.5 de 5 estrelas4.5/5 (344)
- Liver Abscess ThesisDocumento7 páginasLiver Abscess Thesisjenniferalexanderfortlauderdale100% (1)
- Team of Rivals: The Political Genius of Abraham LincolnNo EverandTeam of Rivals: The Political Genius of Abraham LincolnNota: 4.5 de 5 estrelas4.5/5 (234)
- School Form 8 Sf8 Learner Basic Health and Nutrition Report AutomaticDocumento12 páginasSchool Form 8 Sf8 Learner Basic Health and Nutrition Report AutomaticYojmhie Joy Ko100% (2)
- The State of Mental Health in The Philippines PDFDocumento4 páginasThe State of Mental Health in The Philippines PDFKatrina Francesca SooAinda não há avaliações
- AbortionDocumento32 páginasAbortionmani_mandeep262519100% (1)
- Acute Sinusitis Diagnosis and TreatmentDocumento27 páginasAcute Sinusitis Diagnosis and Treatment1720209111Ainda não há avaliações
- Drug StudyDocumento3 páginasDrug StudyMelanie Moises JavierAinda não há avaliações
- The Unwinding: An Inner History of the New AmericaNo EverandThe Unwinding: An Inner History of the New AmericaNota: 4 de 5 estrelas4/5 (45)
- Daftar AntibiotikDocumento448 páginasDaftar AntibiotikevaAinda não há avaliações
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyNo EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyNota: 3.5 de 5 estrelas3.5/5 (2219)
- Wilfredo Mallari Resume Safety Supervisor UpdatedDocumento1 páginaWilfredo Mallari Resume Safety Supervisor Updatedwilly mallariAinda não há avaliações
- ResearchDocumento20 páginasResearchapi-413279928Ainda não há avaliações
- Two Step TSTDocumento2 páginasTwo Step TSTBrianHoAinda não há avaliações
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreNo EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreNota: 4 de 5 estrelas4/5 (1090)
- Child Development MilestonesDocumento6 páginasChild Development Milestonesj_______________jAinda não há avaliações
- History and Mental Status Exam GuideDocumento17 páginasHistory and Mental Status Exam Guideyeney armenterosAinda não há avaliações
- Understanding Hepatitis: Causes, Types, and TreatmentsDocumento2 páginasUnderstanding Hepatitis: Causes, Types, and TreatmentsChandra SaputraAinda não há avaliações
- Basic Tools in NutritionDocumento23 páginasBasic Tools in NutritionSeanmarie Cabrales0% (1)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)No EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Nota: 4.5 de 5 estrelas4.5/5 (119)
- Maternity and Newborn MedicationDocumento34 páginasMaternity and Newborn MedicationNicholas ClaytonAinda não há avaliações
- Progestin Only ContraceptionDocumento4 páginasProgestin Only ContraceptionTareq SawanAinda não há avaliações
- 116 Salalima Vs ECC and SSSDocumento4 páginas116 Salalima Vs ECC and SSScharmssatellAinda não há avaliações
- Nurse ExamDocumento17 páginasNurse ExamRn nadeen100% (2)
- Epithelioid Hemangioendothelioma of The Superior Vena - 2022 - Archivos de BroncDocumento1 páginaEpithelioid Hemangioendothelioma of The Superior Vena - 2022 - Archivos de Broncguidance mtisiAinda não há avaliações
- Chitoglucan New OverviewDocumento6 páginasChitoglucan New OverviewmjmorcelliAinda não há avaliações
- A 10-Year Review of Colonoscopy at Aminu Kano Teaching Hospital, Kano NigeriaDocumento5 páginasA 10-Year Review of Colonoscopy at Aminu Kano Teaching Hospital, Kano NigeriaYUSUF MUSAAinda não há avaliações