Escolar Documentos
Profissional Documentos
Cultura Documentos
Case Presentation: History
Enviado por
Saya Menang0 notas0% acharam este documento útil (0 voto)
14 visualizações45 páginasOA
Título original
OCDoftheKnee
Direitos autorais
© © All Rights Reserved
Formatos disponíveis
PPT, PDF, TXT ou leia online no Scribd
Compartilhar este documento
Compartilhar ou incorporar documento
Você considera este documento útil?
Este conteúdo é inapropriado?
Denunciar este documentoOA
Direitos autorais:
© All Rights Reserved
Formatos disponíveis
Baixe no formato PPT, PDF, TXT ou leia online no Scribd
0 notas0% acharam este documento útil (0 voto)
14 visualizações45 páginasCase Presentation: History
Enviado por
Saya MenangOA
Direitos autorais:
© All Rights Reserved
Formatos disponíveis
Baixe no formato PPT, PDF, TXT ou leia online no Scribd
Você está na página 1de 45
Case Presentation: History
J.B. is an 18 year old male football, ice
hockey, and lacrosse player
3-4 year h/o medial right knee pain
S/p blunt trauma to the medial right knee
Cleared to return to play by Ortho
No MRI done
Intermittent giving out pretty often
Occasional locking
Unable to fully extend
Case Presentation: History
Right knee becomes painful, swollen, and
red after ice hockey practice x 1 week
Pain localized to medial aspect
Ambulates without problems otherwise
Denies day-to-day functional impairment
Denies numbness, tingling, or motor
weakness in either LE
Otherwise healthy; ROS negative otherwise
Case Presentation: Exam
Right knee
Mild ecchymosis overlying anterio-medial
aspect of the knee
Mild quadriceps atrophy compared to L knee
Moderate joint effusion
Medial joint line TTP
Increased pain with full flexion
Extension ~ 5 less than left knee
Case Presentation: Exam
Right knee (Continued)
Valgus stress testing
No ligamentous laxity
Increased pain
Varus stress testing
No laxity or increased pain
Lachmans, anterior drawer, and posterior
drawer testing all without laxity
Equivocal pivot shift
Case Presentation: Exam
Right knee (Continued)
Positive Steinmans test
medially
Joint line pain when the tibia
is rotated internally and
externally while the knee is
flexed over the examination
table
Case Presentation: Exam
Right knee (Continued)
Medial joint pain with
McMurrays Testing
Flexing the patient's hip
and knee and palpating for
a pop or click along the
joint line as the tibia is
internally and externally
rotated, while extending &
flexing the knee
Case Presentation: Exam
Right knee (Continued)
Distally NV intact
Left knee
No abnormalities
Gait
No gross stance or swing phase abnormalities
Case Presentation
Differential Diagnosis?
Meniscal injury
Extensor mechanism injury
Cruciate ligament injury
Collateral ligament injury
Case Presentation
What do you want to order / do now?
Plain films?
Ottawa knee rules?
Which views?
MRI?
Bone scan?
Refer to Ortho?
Pray?
Case Presentation: Plain
Radiographs
AP View
Lateral View
Case Presentation: Plain
Radiographs
Oblique View
Sunrise View
(aka: Merchant View)
Case Presentation: Plain
Radiographs
Tunnel View
Case Presentation:
Radiographs & MRI
Right Knee Plain Radiographs
OCD involving lateral half of the articular surface of the
medial femoral condyle, with associated 1 cm loose body
Right Knee MRI
OCD @ inner edge of medial femoral condyle, 2 cm in
diameter, with adjacent bone edema
Mild thinning of tibial ACL insertion
Tiny tear at the undersurface if the posterior horn of the
medial meniscus
Joint effusion
Osteochondral Defects of the Knee
Garry W. K. Ho, M.D.
VCU / Fairfax Family Practice
April 11, 2005
Osteochondral Defect: What It Be
A fragment of cartilage and subchondral bone
separates from the articular surface
2 distinct populations of patients
Differentiated by the status of their physes
Juvenile Knee OCD
5-15 year olds who have open physes
Adult Knee OCD
Older teens & adults with closed physes
Symptoms depend on stage of the lesion
Untreated, may lead to early OA with chronic pain
and functional impairment
Osteochondral Defect:
Pathophysiology
Cause unclear & debated
Many etiologies proposed
Trauma
Direct (less likely) trauma transchondral
fracture?
Indirect trauma more likely
Predilection for the posterolateral portion of the
medial femoral condyle
Repetitive impingement of the tibial spine on the
lateral aspect of the medial femoral condyle during
internal rotation of the tibia
Osteochondral Defect:
Pathophysiology
Ischemia
1990: Enneking described the vascular supply to the
subchondral bone with poor anastomoses to
surrounding arterioles, predisposing it to forming
sequestra, making it vulnerable to traumatic insult,
fracture, and separation
Rogers and Gladstone: found numerous anastomoses to
intramedullary cancellous bone in the distal femur
Chiroff and Cooke: found no signs of avascular
necrosis in sections of excised osteochondral loose
bodies
Osteochondral Defect:
Pathophysiology
Other proposed etiologies & predisposing
conditions
Skeletal maturation (accessory centers of ossification)
Genetic conditions (e.g., multiple epiphyseal dysplasias)
Metabolic factors
Hereditary factors
Anatomic variation
Currently believed to be multifactorial
Trauma as the starting point in predisposed individual
Single traumatic event or repetitive microtrauma may interrupt
the vascular supply
Vascular insufficiency ultimately leads to fragment
separation
Osteochondral Defect:
Epidemiology in U.S.
OCD of femoral condyles
6 cases per 10,000 men
3 cases per 10,000 women
Average age: 10-20 years old, but may
occur in any age
Males-to-Female ratio 2-3:1
Bilateral in 30-40%
21-40% have some history of trauma
Osteochondral Defect:
Epidemiology in U.S.
Medial femoral condyle: 75-85%
70% occur in the posterolateral aspect
Lateral femoral condyle: 10-25%
Osteochondral Defect:
Symptomatology
History of trauma
Vague and poorly localized knee pain, swelling,
and stiffness in varying degrees
Especially activity-related swelling
Possible clicking or popping
Symptoms often intermittent & exacerbated by
activity or twisting / cutting movements
Locking or catching may occur
Giving way of the knee may occur
Due to quadriceps weakness
Prolonged course leads to progressive
degenerative arthritis
Osteochondral Defect: Exam
Joint effusion may be present
Quadriceps atrophy and weakness may be evident
Quad Girth measured @ 10 cm proximal to superior
pole of the patella
Palpable loose body, occasionally
Decreased ROM
Especially in knee extension
Joint line tenderness
Gait abnormalities
External rotated tibia on stance phase
Quadriceps disuse atrophy or weakness
Osteochondral Defect : Exam
Meniscal Tests may be
positive
Steinmans Test (Meniscal)
Joint line pain when the tibia
is rotated internally and
externally while the knee is
flexed over the examination
table
Osteochondral Defect : Exam
McMurrays Test
(Meniscal)
Flexing the patient's hip
and knee and palpating for
a pop or click along the
joint line as the tibia is
internally and externally
rotated, while extending &
flexing the knee
Osteochondral Defect : Exam
Apley Test (Meniscal)
With patient prone, rotate the tibia on
the femur and applying axial
compression to reproduce joint line
pain
Osteochondral Defect: Exam
Wilson Test (OCD)
OUCH!
Osteochondral Defect : Imaging
Plain Radiographs: useful 1
st
line imaging
AP & lateral views: OCD on the condyles
Sunrise or Merchant View: patellar OCD
Notch or Tunnel AP View: medial femoral condyle OCD
MRI with gadolinium
Technetium bone scan
Occult bilateral OCD
Estimates prognosis with conservative vs. operative
treatment
CT scanning: helpful in preop planning when MRI is
contraindicated or not available
Sonography: only advantage is cost
Osteochondral Defect : Imaging
MRIs of Knee showing OCD
Osteochondral Defect : Grading
Osteochondral Fragment Stability
Grade / Stage 1: Depressed OCD
Small area of compressed subchondral bone
Grade / Stage 2: Partial OCD
Partially detached osteochondral fragment
Sclerotic subchondral bone
Grade / Stage 3: Complete nondisplaced OCD
Completely detached fragment that remains within
the underlying crater (nondisplaced)
Most common
Grade / Stage 4: Displaced OCD
Completely detached & displaced fragment
Loose body
Osteochondral Defect : Grading
Osteochondral Fragment Stability
Osteochondral Defect :
Treatment Categories
Based on physeal status and OCD size & stability
Category 1
females < 11 y/o, males < 13 y/o, no loose body on X-Ray
Do well with non-operative treatment
Category 2
females 11-15 y/o, males 13-17 y/o
Near skeletal maturity; treatment depends on location, size,
and stability of the lesion
Category 3
Physeal closure and skeletal maturity have occurred
Treatment based on the location, size, and stability of the
lesion
Osteochondral Defect :
Treatment
Conservative treatment
Category 1 patients & no loose bodies (Juvenile Type)
Category 2 patients with Grade 1 lesions
Questionable: Category 2 patients with Grade 2 lesions
Osteochondral Defect :
Treatment
Referral to orthopaedics for surgical therapy
Lesions > 1 cm in size
Category 3 patients
Loose bodies
Mechanical symptoms (e.g. locking, giving way)
Lateral femoral condyle OCDs
Failure of conservative therapy
No evidence of union after 12 weeks
Children approaching physeal closure within 6 months
Osteochondral Defect :
Conservative Treatment
Pain control
Relative rest for 1-2 weeks
Limit activity
Protected weight bearing
Knee immobilizer
Check serial X-Rays Q 3-6 months
Modified activity for 6-12weeks
Low impact activity only
Full activity, quads strengthening if:
No pain, normal exam, and X-Rays show evidence of
healing
Osteochondral Defect :
Conservative Treatment
If still symptomatic or X-Rays do not show
improvement after 12 weeks
Refer to Ortho for surgery
Incidental OCDs in asymptomatic patients
Refer Category 3 patients
Follow with serial X-Rays Q 4-6 months until the lesion
has healed or until skeletal maturity achieved
If still asymptomatic at skeletal maturity and the X-Rays
have not progressed
Reassure patient
No further treatment is indicated
Osteochondral Defect :
Surgical Therapy
Arthroscopic views of OCDs
Osteochondral Defect :
Surgical Therapy
Microfracture Debridement & Lavage
Osteochondral Defect :
Surgical Therapy
Fixation
Osteochondral Defect :
Surgical Therapy
Osteochondral Allograft Implantation (OCA)
Osteochondral Defect :
Surgical Therapy
Osteochondral
Autologous
Transplantation
(OATS)
Case Presentation: J.B. Revisited
J.B. was seen by Dr. Petrone
Arthroscopic OATS performed
Tolerated well
Physical Therapy
Doing well
In Conclusion
When you think of meniscal injuries, consider
osteochondral injuries as well
Pain & swelling associated with activity is abnormal &
your tip-off for OCDs
While using the Ottawa rules are helpful, dont be
afraid to order X-rays when the Dx isnt clear
Extension of the physical exam
Theres more to knee X-rays than the standard
Knee series
Order the views you need
Thanks!
Questions ?
References
Rogers WM, Gladstone H: Vascular foramina and arterial supply of the distal
end of the femur. J Bone Joint Surg Am 1950 Oct; 32 (A:4): 867-74
Schenck RC, Goodnight JM: Osteochondritis dissecans. J Bone Joint Surg Am
1996 Mar; 78 (3): 439-56
Ralston BM, Williams JS, Bach BR, Bush-Joseph CA, Knopp WD:
Osteochondritis Dissecans of the Knee. Phys Sportsmed 1996 Jun; 24 (6)
Pappas AM: Osteochondrosis dissecans. Clin Orthop 1981; Jul-Aug (158):59-69
Garrett JC: Osteochondritis dissecans. Clin Sports Med 1991;10 (3):569-593
Osteochondritis Dissecans of the Knee
Wang TW, Knopp WD, Bush-Joseph CA, Bach BR: Osteochondritis Dissecans
of the Knee. Phys Sportsmed 1998 Aug; 26 (8)
Cahill BR, Phillips MR, Navarro R: The results of conservative management of
juvenile osteochondritis dissecans using joint scintigraphy. A prospective study.
Am J Sports Med 1989 Sep-Oct; 17(5): 601-606
Osteochondral Defects: A Brief
History
1558: Ambrose Pare removed loose bodies from the knee joint
1870: Paget described quiet necrosis within the knee
1888: Knig coined the term "osteochondritis dissecans," proposing
this condition was caused by spontanous inflammation
(osteochondritis) to necrosis & a separation (dissecans) of the fragment
Advent of X-rays: osteochondrotic conditions in other joints, primarily
the hip, were recognized
1910: Legg, Calve, and Perthes independently identified a condition of the
hip joint in children, which is now known as Legg-Calve-Perthes disease.
1921: Waldenstrm introduced the term coxa plana (ie, disintegration of
capital femoral epiphysis.)
Since the introduction of radiographs, 50 additional anatomic sites within
the body where OCD can occur have been identified
Investigators have failed to identify inflammatory cells in histologic
sections of excised osteochondral loose bodies. Nevertheless, the name
osteochondritis dissecans has persisted
Você também pode gostar
- Distal Clavicle Osteolysis, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo EverandDistal Clavicle Osteolysis, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsAinda não há avaliações
- Departement of Orthopaedic and TraumatologyDocumento89 páginasDepartement of Orthopaedic and TraumatologyMukhizalAinda não há avaliações
- Pengayaan Koass Ortho - Update 5 VersionDocumento122 páginasPengayaan Koass Ortho - Update 5 Versionanon_967171484Ainda não há avaliações
- Handout Lat Elbow Pain PDFDocumento47 páginasHandout Lat Elbow Pain PDFgemichan26Ainda não há avaliações
- New Introduction To Ortho 1 Jan 20016Documento67 páginasNew Introduction To Ortho 1 Jan 20016BIOLOGY BY ISMAIL ANSARIAinda não há avaliações
- Foot and Ankle Injuries Kylee Phillips - 0Documento74 páginasFoot and Ankle Injuries Kylee Phillips - 0Charlez OhanuAinda não há avaliações
- OA - Ahmad Aulia Rizaly - DR Andry Usman SpOTDocumento34 páginasOA - Ahmad Aulia Rizaly - DR Andry Usman SpOTNur Syamsiah MAinda não há avaliações
- Spinal Deformities NewDocumento79 páginasSpinal Deformities Newapi-26159412100% (3)
- 9 Orthopaedic EmergenciesDocumento68 páginas9 Orthopaedic EmergenciesAndrew WdsmithAinda não há avaliações
- Foot and Ankle Injuries Kylee Phillips - 0Documento74 páginasFoot and Ankle Injuries Kylee Phillips - 0rizwan.mughal1997Ainda não há avaliações
- Hip ProblemsDocumento46 páginasHip ProblemsDhiya' VinaAinda não há avaliações
- Orthopedic Conditions in PaedsDocumento57 páginasOrthopedic Conditions in PaedsAsma AlamAinda não há avaliações
- 18 Mandibular Fractures 2016-Presented LectureDocumento34 páginas18 Mandibular Fractures 2016-Presented LectureHanin AbukhiaraAinda não há avaliações
- S T O P: Ports Rauma and Veruse ReventionDocumento37 páginasS T O P: Ports Rauma and Veruse ReventionNabiha AjmalAinda não há avaliações
- Anterior Knee Pain Syndrome ReferatDocumento28 páginasAnterior Knee Pain Syndrome ReferatnurulAinda não há avaliações
- Ankle and Foot: Common Acute Injuries: Kevin Deweber, MD, Faafp Director, Sports Medicine Fellowship Usuhs/DewittDocumento57 páginasAnkle and Foot: Common Acute Injuries: Kevin Deweber, MD, Faafp Director, Sports Medicine Fellowship Usuhs/DewittShora JariAinda não há avaliações
- Common CasesDocumento44 páginasCommon CasesRebecca WongAinda não há avaliações
- SPONDYLOLISTHESISDocumento27 páginasSPONDYLOLISTHESISJulioYoko100% (1)
- Management of Back Pain in AdultsDocumento41 páginasManagement of Back Pain in AdultsMadhusree GhoshAinda não há avaliações
- Knee Anatomy and InjuriesDocumento120 páginasKnee Anatomy and Injurieserfan mohammadi100% (2)
- OsteoarthritisDocumento34 páginasOsteoarthritisLaiba KhanAinda não há avaliações
- Management of Fracture Acetabulum in Geriatric Age Group Saturday 12 15Documento44 páginasManagement of Fracture Acetabulum in Geriatric Age Group Saturday 12 15tarikeopsAinda não há avaliações
- Lecture 11aDocumento40 páginasLecture 11aElliya Rosyida67% (3)
- Osteoarthritis: Dr. C. C. VisserDocumento85 páginasOsteoarthritis: Dr. C. C. VisserAhmad Fathira FitraAinda não há avaliações
- ScoliosisDocumento99 páginasScoliosismarjan dronjakAinda não há avaliações
- Osteoarthritis: Dr. Angelo Smith M.D WHPLDocumento51 páginasOsteoarthritis: Dr. Angelo Smith M.D WHPLChuks LeviAinda não há avaliações
- Thoracic and Lumbar SpineDocumento49 páginasThoracic and Lumbar Spinemanucv23Ainda não há avaliações
- Kuliah Spine TraumaDocumento91 páginasKuliah Spine Traumatutor tujuhAinda não há avaliações
- Spinal Injury & Spinal Cord Injury: For General PracticeDocumento60 páginasSpinal Injury & Spinal Cord Injury: For General PracticeRheselle LacuataAinda não há avaliações
- Low Back Pain - 1-07Documento39 páginasLow Back Pain - 1-07Nur Sabriany LihawaAinda não há avaliações
- CBD-Fracture of Shaft FemurDocumento34 páginasCBD-Fracture of Shaft FemurBONG AIKCHINGAinda não há avaliações
- Pediatric OrthopedicsDocumento28 páginasPediatric OrthopedicsEdwin OkonAinda não há avaliações
- Distal Humeros PedDocumento55 páginasDistal Humeros PedSuad StambulieAinda não há avaliações
- Child Abuse ImagingDocumento47 páginasChild Abuse ImagingDmitry DudinAinda não há avaliações
- 20.nyeri PunggungDocumento53 páginas20.nyeri PunggungAy'oe Ithyu RezthuAinda não há avaliações
- Approach To Low Back PainDocumento39 páginasApproach To Low Back Painpradosh chandAinda não há avaliações
- FractureDocumento125 páginasFractureKlara Devina VanessaAinda não há avaliações
- Tibial Plateau Fractures: Yasser AlwabliDocumento35 páginasTibial Plateau Fractures: Yasser AlwabliPin Han NaAinda não há avaliações
- Femoral Shaft FracturesDocumento40 páginasFemoral Shaft FracturesOlasinde AnthonyAinda não há avaliações
- Bilateral Knee OADocumento35 páginasBilateral Knee OAMu'iz Beatforteen50% (2)
- Injuries of Femur and Knee: Dr. Andrianto Wisnu Nugroho, SP - OT RSU Karsa Husada BatuDocumento34 páginasInjuries of Femur and Knee: Dr. Andrianto Wisnu Nugroho, SP - OT RSU Karsa Husada Batuandre wisnuAinda não há avaliações
- Lumbar Canal StenosisDocumento19 páginasLumbar Canal StenosisMohamed ElMeligieAinda não há avaliações
- Radiology of The SpineDocumento50 páginasRadiology of The SpineAsem AlhazmiAinda não há avaliações
- # RT TibiaDocumento169 páginas# RT TibiaCatherine MilkhaAinda não há avaliações
- Extremity Trauma Board Review 2018Documento80 páginasExtremity Trauma Board Review 2018rigo montejoAinda não há avaliações
- Low Back Pain:: Approach To The Patient in The E.DDocumento39 páginasLow Back Pain:: Approach To The Patient in The E.DLidiaAMonroyRAinda não há avaliações
- Femoral Neck FractureDocumento28 páginasFemoral Neck FractureayuegpAinda não há avaliações
- Pathology and Management of Low Back PainDocumento33 páginasPathology and Management of Low Back PainSam100% (1)
- Orthopaedics Diagnosis & Therapy: Dr. Su Djie To Rante, M.Biomed, SP - OTDocumento75 páginasOrthopaedics Diagnosis & Therapy: Dr. Su Djie To Rante, M.Biomed, SP - OTDiana MarcusAinda não há avaliações
- 1 Materi Kuliah Spine, Dr. AzharuddinDocumento59 páginas1 Materi Kuliah Spine, Dr. AzharuddinfazliahAinda não há avaliações
- Skeletal Trauma-Plain Film Trauma Terminology ReviewDocumento35 páginasSkeletal Trauma-Plain Film Trauma Terminology Reviewbjpalmer100% (3)
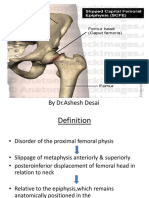
- Slipped Capital Femoral EpiphysisDocumento40 páginasSlipped Capital Femoral EpiphysisDrAshesh Desai100% (2)
- Kuliah Spine TraumaDocumento91 páginasKuliah Spine TraumaEvi MaisyariAinda não há avaliações
- Ankylosing Spondylitis - YafiDocumento28 páginasAnkylosing Spondylitis - YafiyafidyAinda não há avaliações
- 06-Dr. Bajammal Hip Disorders 2017Documento48 páginas06-Dr. Bajammal Hip Disorders 2017MuathAinda não há avaliações
- Lecture 11aDocumento39 páginasLecture 11aSourabh KulkarniAinda não há avaliações
- Knee Case Study 1Documento4 páginasKnee Case Study 1superhoofy7186100% (1)
- Climbing PresentationDocumento18 páginasClimbing PresentationDaniel SloskyAinda não há avaliações
- Orthopaedic Physical ExaminationDocumento94 páginasOrthopaedic Physical ExaminationPriza RazunipAinda não há avaliações
- Disc Herniation and McKenzie MethodDocumento80 páginasDisc Herniation and McKenzie MethodRodrigo Cardoso Mousinho Fisioterapeuta ManualAinda não há avaliações
- Vitamin of Seizure Vascular Idiopathic Autoimmune Metabollic Infection NeoplasmDocumento1 páginaVitamin of Seizure Vascular Idiopathic Autoimmune Metabollic Infection NeoplasmSaya MenangAinda não há avaliações
- Sample Referral LetterDocumento2 páginasSample Referral LetterSaya Menang100% (1)
- Physics PEKA Scoring Check ListDocumento2 páginasPhysics PEKA Scoring Check ListSaya MenangAinda não há avaliações
- Basketball Students Attendance List 2017 Dates Class 9/1 16/1 23/1 6/2 13/2 20/2 27/2 6/3 13/3 27/3 3/4 10/4 17/4 24/4Documento2 páginasBasketball Students Attendance List 2017 Dates Class 9/1 16/1 23/1 6/2 13/2 20/2 27/2 6/3 13/3 27/3 3/4 10/4 17/4 24/4Saya MenangAinda não há avaliações
- Presentation 1Documento1 páginaPresentation 1Saya MenangAinda não há avaliações
- Physics PEKA Scoring Check ListDocumento2 páginasPhysics PEKA Scoring Check ListSaya MenangAinda não há avaliações
- Cerebellar ExaminationDocumento1 páginaCerebellar ExaminationSaya MenangAinda não há avaliações
- Rates of Reaction TestDocumento10 páginasRates of Reaction TestSaya MenangAinda não há avaliações
- Bacterialcornealulcer 140129095140 Phpapp02Documento48 páginasBacterialcornealulcer 140129095140 Phpapp02Saya MenangAinda não há avaliações
- Contraindications of Eswl B Pass Bleeding Diathesis Pregnancy Aneursym Sepsis Stone More Than 2MmDocumento1 páginaContraindications of Eswl B Pass Bleeding Diathesis Pregnancy Aneursym Sepsis Stone More Than 2MmSaya MenangAinda não há avaliações
- Esa Waterpark D Weekday, Mon - Tue / Thu - Fri (Adult) : Ticket To Desa WaterparkDocumento1 páginaEsa Waterpark D Weekday, Mon - Tue / Thu - Fri (Adult) : Ticket To Desa WaterparkSaya MenangAinda não há avaliações
- ENT Short Cases Records & OSCE Questions: 1 EditionDocumento15 páginasENT Short Cases Records & OSCE Questions: 1 EditionSaya MenangAinda não há avaliações
- Factors Affecting Rate of Reaction CatalystDocumento1 páginaFactors Affecting Rate of Reaction CatalystSaya MenangAinda não há avaliações
- Case Report in Psychiatry051.03Documento4 páginasCase Report in Psychiatry051.03Saya MenangAinda não há avaliações
- Trial Terengganu SPM 2013 PHYSICS Ques - Scheme All PaperDocumento0 páginaTrial Terengganu SPM 2013 PHYSICS Ques - Scheme All PaperCikgu Faizal67% (3)
- Trial Terengganu Biologi SPM 2014 K2 SkemaDocumento12 páginasTrial Terengganu Biologi SPM 2014 K2 SkemaCikgu Faizal100% (1)
- Physics p2 Trial SPM 2007 (Kedah)Documento14 páginasPhysics p2 Trial SPM 2007 (Kedah)Saya MenangAinda não há avaliações
- Chemistry Chapter 5 Form 5Documento1 páginaChemistry Chapter 5 Form 5Saya MenangAinda não há avaliações
- ADD MATHS Progressions FORM 5Documento6 páginasADD MATHS Progressions FORM 5Cik NursharwaniAinda não há avaliações
- Sleep Apnea - Could It Be Robbing You of Rest?Documento4 páginasSleep Apnea - Could It Be Robbing You of Rest?Saya MenangAinda não há avaliações
- 01 - 012 Obstructive Sleep ApneaDocumento2 páginas01 - 012 Obstructive Sleep ApneaSaya MenangAinda não há avaliações
- Chemistry Chapter 5 Form 5Documento1 páginaChemistry Chapter 5 Form 5Saya MenangAinda não há avaliações
- IAU Case Write UpDocumento4 páginasIAU Case Write UpSaya MenangAinda não há avaliações
- Su20140331031237x52 609594142 1403057431Documento14 páginasSu20140331031237x52 609594142 1403057431Saya MenangAinda não há avaliações
- Casewriteup Ent 110911092915 Phpapp01Documento8 páginasCasewriteup Ent 110911092915 Phpapp01Saya MenangAinda não há avaliações
- Trachy 121106090823 Phpapp02Documento46 páginasTrachy 121106090823 Phpapp02Saya MenangAinda não há avaliações
- Ent Instruments 100503041754 Phpapp02Documento59 páginasEnt Instruments 100503041754 Phpapp02Krittin NaravejsakulAinda não há avaliações
- Larynx (Anatomy, Laryngomalacia, Laryngeal Web)Documento12 páginasLarynx (Anatomy, Laryngomalacia, Laryngeal Web)Saya MenangAinda não há avaliações
- Cancer LaryncDocumento35 páginasCancer LaryncSaya MenangAinda não há avaliações
- Comprehensive Key For ENT Cases: CSOM Never Painful Except inDocumento21 páginasComprehensive Key For ENT Cases: CSOM Never Painful Except inSaya Menang100% (1)
- Maxillary Sinus Bone GraftingDocumento181 páginasMaxillary Sinus Bone GraftingTuấn Hành TrầnAinda não há avaliações
- Plantar ReflexDocumento3 páginasPlantar Reflexhalu89Ainda não há avaliações
- Lower Limb BlocksDocumento5 páginasLower Limb BlocksParvathy R NairAinda não há avaliações
- Con TroveDocumento75 páginasCon TroveNgurah AndhikaAinda não há avaliações
- PMUS1-11 Biology of Muscles IDocumento68 páginasPMUS1-11 Biology of Muscles IVictor ChanAinda não há avaliações
- Gross Anatomy of The Muscular System: ExerciseDocumento8 páginasGross Anatomy of The Muscular System: ExerciseJericho CarenaAinda não há avaliações
- Taping and BracingDocumento14 páginasTaping and BracingShorya SinghAinda não há avaliações
- Corrective ExercisesDocumento47 páginasCorrective ExercisesZachary Lee100% (10)
- Iyengar Headstand PDFDocumento15 páginasIyengar Headstand PDFFelice Chew100% (3)
- Tmi Lumbar Fusion Rehabilitation ProtocolDocumento2 páginasTmi Lumbar Fusion Rehabilitation ProtocolJackyAinda não há avaliações
- Scapula Fracture: DR Jaseem ShamsudeenDocumento32 páginasScapula Fracture: DR Jaseem ShamsudeenJaseemshams ThottiyilAinda não há avaliações
- OIA-SA-H Cat Muscles MegatableDocumento6 páginasOIA-SA-H Cat Muscles MegatablePerseus Evangelio100% (2)
- Shoulder Injuries in Dogs - Ridge ReferralsDocumento5 páginasShoulder Injuries in Dogs - Ridge ReferralsZullyAinda não há avaliações
- Index: Acinetobacter BaumanniiDocumento11 páginasIndex: Acinetobacter BaumanniiHeruWidartAinda não há avaliações
- Ultrasound-Guided Truncal Blocks For PerioperativeDocumento15 páginasUltrasound-Guided Truncal Blocks For PerioperativeRuxandra GrigorescuAinda não há avaliações
- 01 Hamelynck 1Documento82 páginas01 Hamelynck 1Mihaela DoniciAinda não há avaliações
- Final Announcement Konker IOA Bandung 2018Documento33 páginasFinal Announcement Konker IOA Bandung 2018MutiaRahmatiaAinda não há avaliações
- Workbook 031512 With Cover PDFDocumento197 páginasWorkbook 031512 With Cover PDFIndah Yulantari100% (2)
- AOI APState August10Documento141 páginasAOI APState August10Anoop BabuAinda não há avaliações
- Anatomy and Physiology of Tibia and FibulaDocumento3 páginasAnatomy and Physiology of Tibia and FibulaVel Georgia-Franco50% (2)
- Axillary NerveDocumento17 páginasAxillary Nerveshrishti shadangiAinda não há avaliações
- Study of Scapular Measurements and Scapular Indices of Andhrapradesh RegionDocumento4 páginasStudy of Scapular Measurements and Scapular Indices of Andhrapradesh RegionInternational Organization of Scientific Research (IOSR)Ainda não há avaliações
- Hand and Wrist Swelling Management Jul18Documento2 páginasHand and Wrist Swelling Management Jul18testAinda não há avaliações
- Dissection Guide On The Frog Muscular SystemDocumento6 páginasDissection Guide On The Frog Muscular SystemNeileene Joy Simeon DomingoAinda não há avaliações
- Case Analysis DMDDocumento15 páginasCase Analysis DMDNicole Villanueva, BSN - Level 3AAinda não há avaliações
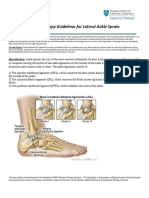
- PT Guidelines For Ankle SprainDocumento5 páginasPT Guidelines For Ankle SprainKirti GunjikarAinda não há avaliações
- OMM Study GuideDocumento53 páginasOMM Study Guideshadowcrest12100% (5)
- Week 3-4Documento6 páginasWeek 3-4Bhargav ThankiAinda não há avaliações
- Evolution of The Vertebrate Skeleton: Morphology, Embryology, and DevelopmentDocumento17 páginasEvolution of The Vertebrate Skeleton: Morphology, Embryology, and DevelopmentRandom Thoughts - Baskar ArumugamAinda não há avaliações
- Approach To Arthritis PatientDocumento20 páginasApproach To Arthritis Patientapi-3716867Ainda não há avaliações