Escolar Documentos
Profissional Documentos
Cultura Documentos
CAPD Pelatihan, 15 April 2011
Enviado por
AndriKusuma0 notas0% acharam este documento útil (0 voto)
179 visualizações66 páginasContinuous ambulatory peritoneal dialysis (CAPD) is a type of peritoneal dialysis that allows patients to filter waste from their blood while being mobile. With CAPD, dialysis solution is infused into the peritoneal cavity through a surgically implanted catheter and remains there for several hours to filter waste before being drained out. The document provides details on the physiology and process of CAPD, including how it works, advantages and disadvantages compared to other forms of dialysis, complications, and guidelines for initiating CAPD treatment.
Descrição original:
Título original
CAPD pelatihan, 15 april 2011.ppt
Direitos autorais
© © All Rights Reserved
Formatos disponíveis
PPT, PDF, TXT ou leia online no Scribd
Compartilhar este documento
Compartilhar ou incorporar documento
Você considera este documento útil?
Este conteúdo é inapropriado?
Denunciar este documentoContinuous ambulatory peritoneal dialysis (CAPD) is a type of peritoneal dialysis that allows patients to filter waste from their blood while being mobile. With CAPD, dialysis solution is infused into the peritoneal cavity through a surgically implanted catheter and remains there for several hours to filter waste before being drained out. The document provides details on the physiology and process of CAPD, including how it works, advantages and disadvantages compared to other forms of dialysis, complications, and guidelines for initiating CAPD treatment.
Direitos autorais:
© All Rights Reserved
Formatos disponíveis
Baixe no formato PPT, PDF, TXT ou leia online no Scribd
0 notas0% acharam este documento útil (0 voto)
179 visualizações66 páginasCAPD Pelatihan, 15 April 2011
Enviado por
AndriKusumaContinuous ambulatory peritoneal dialysis (CAPD) is a type of peritoneal dialysis that allows patients to filter waste from their blood while being mobile. With CAPD, dialysis solution is infused into the peritoneal cavity through a surgically implanted catheter and remains there for several hours to filter waste before being drained out. The document provides details on the physiology and process of CAPD, including how it works, advantages and disadvantages compared to other forms of dialysis, complications, and guidelines for initiating CAPD treatment.
Direitos autorais:
© All Rights Reserved
Formatos disponíveis
Baixe no formato PPT, PDF, TXT ou leia online no Scribd
Você está na página 1de 66
Divisi Ginjal Hipertensi
Bag / SMF Ilmu Penyakit Dalam
FK UNUD / RSUP Sanglah Denpasar
Yenny Kandarini
Integrated Treatment of ESRD
HEMODIALYSIS CAPD
KIDNEY TRANSPLANTATION
RRT
DIALYSIS
Is the process of cleansing or filtering the blood
Intermittent Peritoneal Dialysis
Dialysis
Hemodialysis
Peritoneal dialysis
Peritoneal
Dialysis
Automated Peritoneal Dialysis
Tidal Peritoneal Dialysis
Continuous Ambulatory
Peritoneal Dialysis (CAPD)
1975 CAPD developed by Moncrief & Popovich
1978 Oreopoulus et al pioneered collapsible plastic
containers for dialysat & titanium connector
1980 Buocristiani-Y set, Bazzota-double bag- applied
drainage before fill concept, straight & disconnect
system available
0
20
40
60
80
100
120
81 82 83 84 85 86 87 88 89 90 91 92 93 94 95 96 97
(000's)
Years
115,000 Patients
1993 - 1997
7.3% Annual Growth
Source: 1997 Baxter Patient Report
Definition
PD is a process during which the peritoneal cavity
acts as the reservoir for dialysis fluid and the
peritoneum serves as the semi permeable
membrane across which excess body fluid and
solutes including uraemic toxins, are removed.
(Gutch, Stoner & Corea 1999)
ontinuous
mbulatory
eritoneal
ialysis
Proses dialisis tidak berhenti, secara
berkesinambungan membersihkan darah,
24 jam se-hari, setiap hari
Bebas bergerak, tidak berhubungan dengan
mesin
Menggunakan rongga peritoneum yang bekerja
sebagai filter untuk mengeluarkan sisa
metabolisme dan cairan dari darah
Menyaring dan membuang cairan berlebih
serta sisa metabolisme tubuh.
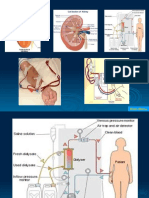
Physiology of
Peritoneal Dialysis
The peritoneum is a serosal membrane
that lines the peritoneal cavity
Thin
Semipermiable
Large surface area (0,55 m
2
)
Divide into 2 parts:
Parietal peritoneum (20% area)
Visceral peritoneum (80% area)
Contains 100 ml or less of fluid
Adult can tolerate 2 L or more fluid without
pain or alteration to the respiratory function
Male: peritoneal cavity is closed
Female: peritoneal cavity is continuous with
the Fallopian tubes.
Rarely PD fluid become blood-stained during a
menstrual period
Total peritoneal blood supply is
estimated to be 60 100 mL/min.
Only 25% of the peritoneal capillaries are
perfused
The number of perfused peritoneal
capillaries is the most important
determinant of peritoneal solute and
water transport, rather than the total
anatomical surface area.
PD utilities the peritoneal membrane as a natural dialysis
filter.
A PD catheter inserted surgically into the peritoneal
cavity
PD solution is infused into the peritoneal cavity via the
catheter and remain there for up to 6-10 hours, during
which time uraemic toxins and fluid are removed by
diffusion and UF across the peritoneal membrane
Time on dialysis
Blood flow
Peritoneal surface area
Membrane permeability
Peritoneal lymphatics
Ultra filtration
Transfer of fluid
Jeremy Levy et al, Oxford Handbook of Dialysis, 2003
Definition
Selective diffusion- movement of solutes
from area of high solute concentration to an
area of low solute concentration across a
semi-permeable membrane.
Driving Force - Concentration gradient
Initial
Final
Solutes flux
Driving force: concentration
gradient
The transport rate of small solutes is higher than that of
large solutes. Small solutes diffuse faster than large solutes
Diffusion
Solute
removal
Dwell Time
Increasing solute size
Diffusion
Definition
Osmosis - movement of water from an area of
high water concentration to an area of low water
concentration across a semi-permeable
membrane.
Or the movement of water from an area of low solute
concentration to an area of high solute concentration.
Driving force - concentration gradient
Osmosis occurs between two solutions separated by a
membrane which is non-permeable (or partially
permeable) to the solutes
Definition
The movement of solutes with a water-flow,
"solvent drag", e.g. the movement of membrane-
permeable solutes with water.
Start of Dialysis
Fluid removal by
osmosis include
solutes removed by
convection
Lost into the dialysate Absorbed into the
circulation
Small molecules (e.g. urea,
creatinine)
Dextrose (if dextrose-containing
PD solution)
Some electrolytes (notably
potassium)
Calcium
Protein (up to 5 10 g/d)
Amino acids, trace minerals,
hormones, drugs
Glucose 1.5%, 2.3%, 4.25%
Sodium 134 mmol/l
Calcium 1 mmol/l, 1.75mmol/l
Magnesium 0.5 mmol/l
Chloride 102 mmol/l
Lactate 35 mmol/l
Note:- No potassium, no urea and no
creatinine
After a two litre bag has dwelled for four
hours average ultrafiltration
1.5% 200 ml ultrafiltrate
2.3% 200 - 400 ml ultrafiltrate
4.25% 600 ml 800 ml ultrafiltrate
Indications for PD in preference to HD
Very small/very young patients
Lack of vascular access
Contraindications to anticoagulation
Cardiovascular instability
Poorly controlled hypertension /
hypertensive cardiomiopathy (relative)
Lack of proximity to pediatric HD center (relative)
Desire for normal school attendance
More liberal fluid intake
Absolute
Abdominal wall stoma
high risk of peritonitis
Diaphragmatic fluid leak
peritoneal dialysis fluid causes
Adhesions
hinder flow of peritoneal dialysis fluid
Loss of peritoneal function or integrity
peritoneal dialysis not technically possible
Severe inflammatory bowel ds
Medical contraindications to peritoneal dialysis
Medical contraindications to peritoneal dialysis
Relative
Large muscle mass-potentially
inadequate dialysis
Obesity
difficulty with catheter insertion
Intestinal disease
potential to initiate peritonitis
Respiratory disease
intolerance of splinting of diaphragm by intraperitoneal
fluid
Hernia
exacerbated by peritoneal dialysis fluid it not surgically
correctable
Relative contraindications to PD
Imminent living-related transplantation
Impending/recent major abdominal surgery
Lack of an appropriate caregiver
PERITONEAL DIALYSIS ADVANTAGES
Continuous dialysis
Self care dialysis
Home based dialysis
Simple to learn and perform
Minimal dietary restrictions
No needle puncture required
No blood access problems
Mobility during dialysis
Ease of travel
Minimal cardiovascular stress
No blood loss
PERITONEAL DIALYSIS DISADVANTAGES
Peritonitis
Protein loss
Potential for elevated blood lipid (fat) and
triglyceride levels
Peritoneal catheter
Daily dialysis schedules
Possible weight gain
o Systemic metabolic effects of glucose dialysate
o Dyslipidemia
o Protein loss
o Hyponatremia / hypernatremia
o Hypokalemia / hyperkalemia
o Hypocalcemia / hypercalcemia
o Hemoperitoneum
o Encapsulating peritoneal sclerosis
o Hydrothorax
o Hernia
o Abdominal and genital leaks
Noninfectious Complications
of Peritoneal Dialysis
Gram-positive (50%)
Gram-negative,non pseudomonas
Pseudomonas
Fungal (2%)
Tuberculosis
Biofilm
(15%)
External appearance of a
perfect exit (magnified 4.5X)
Natural color, no scab, no
granulating tissue, no
redness, no drainage
Sinus appearance of perfect
exit strong and mature,
cover visible sinus
Acutely Infected
Exit
Painful
Swollen
Red with erythema > 13
mm in diameter
Exuberant granulation
tissue
Bleed easily upon touch
Visible around exit
and/or in visibly sinus
Drainage
Purulent and / or bloody
Wet exudates on dressing
Crust or scab around exit
(or in the sinus)
Chronically Infected
Exit
Evolved from acute infection that
is unresolved for > 4 weeks
Signs of pain, swelling and
redness are absent
Granulation tissue : exuberant
around exit and/or sinus
Epithelium: absent or covers only
part of sinus
Sometimes visible sinus and exit
appears normal
Drainage:
Purulent or bloody,
spontaneous or after pressure
on sinus
Wet exudate on dressing
Crust or scab around the exit or
in the sinus
External cuff gets infected
Tunnel Infection
Functional parts of the peritoneal catheter
Symptoms:
- cloudy fluid; and/or
- abdominal pain (79%); and/or
- fever (53%)
Look for :
CLOUDY BAGS
Stomach Pain Fever
Do your exchanges just as
you are taught
Dialysate volume : 2 L for 4 cycle exchange
schedule :
08.00, 12.00, 16.00, 24.00
(before bed time)
Ultrafiltration:
08.00, 12.00, 16.00 1.5%
24.00 2.5%
CAPD
0
500
1000
1500
2000
2500
Time (24 hour clock)
V
o
l
u
m
e
Spent dialysate is drained out.
This process takes approximately 10-20 minutes
Fresh dialysate is flushed from the fresh solution bag
into the drain bag.
This process takes approximately 5 seconds
Fresh dialysate is infused into the peritoneal cavity.
This takes 8-10 minutes
O
Dialysate remains in the peritoneal cavity for 4 8 hours
During this time waste products and excess fluid is removed
Ultra Bag Disconnect System
Andy -Twin Bag Disconnect
system
CAPD system in Indonesia
Initiation to CAPD
Implant catheter
Provide educational materials to caregivers, patients
Immediate PD required?
2-to 6-weeks healing period, then start dialysis with 4-
8 excahnges using 300 mL/m
2
BSA volume,* increase
fill volume to 1100 mL/m
2
BSA within 7-14 days
Start supine dialysis with 12-24 exchanges using
300 mL/m
2
BSA volume* for 7 days, increase fill
volume to 1100 mL/min
2
BSA within 14-21 days
Establish maximally tolerable fill volume by either repeated IPP measurements or clinical
judgment. Adjust to maximally tolerable fill volume
Initial prescription: 3 3-to 5-hour daytime + 1 9- to 12-hour nighttime cycles with macimally
tolerable fill volume (usually 1100 mL/m
2
BSA
Preformed PET, measure urinary and dialysate creatinine and urea clearances at the end of
training (preferably 4 weeks after start of PD
Use PD dosing tables or software (PD adequest or renalsoft PD Rx Management) to adjust PD
prescription
No Yes
* 200 mL/m
2
BSA during infancy
Criteria of CAPD adequacy
Total Kt / V
urea
> 2.0/week
Total CrCI / 60 L/1.73 m
2
/week in high / high average
transporters, > 50 in low/low average transporters
Clearance associated with normal status for hydration,
electrolyte balance, blood pressure, growth, nutrition and
psychomotor development
Outcome evaluation
Monthly assessment of growth and weight gain, head circumference
(infants); blood pressure, acid-base status, electrolytes, serum
creatinine, BUN, hemoglobin/hematocrit, serum albumin, record urine
output and daily ultra filtration
Serum ferritin, serum iron, total iron binding capacity (monthly until
stable, then every 2-3 months)
Every 3 months assessment of intact PTH, alakaline phosphatase
Every 4 months assessment of 24-hour dialysate and urine collection for
CrcI, Kt/Vurea; possibly more frequent if prior assessment reveals failure
adequacy targets; school evaluation
Every months neurodevelopmental assessment in infants < 4 years of age
Consider annual:
Ambulatory blood pressure monitoring (ABPM), especially if casual
BP frequently borderline or discrepant from home measurements,
echocardiography
Hand and wrist X-ray (especially if intact PTH frequently outside
therapeutic range
Outcome evaluation
Practice Points
Peritoneal dialysis should be considered in all
patients approaching ESRF
Planning for peritoneal dialysis is a multidisciplinary
process that should be instituted well before the
requirement for dialysis
Patients maintained on peritoneal dialysis should be
assessed regularly for the adequacy of solute
clearance and ultra filtration; inadequate dialysis is
associated with increased morbidity and mortality
Infective complications of peritoneal dialysis,
particularly peritonitis, must be identified and treated
promptly.
Você também pode gostar
- Intradialytic Hypertension Time To Act 10Documento7 páginasIntradialytic Hypertension Time To Act 10Nia FirdiantyAinda não há avaliações
- Gensan Medical Center Renal Dialysis Catheter Care PolicyDocumento5 páginasGensan Medical Center Renal Dialysis Catheter Care PolicyCynthia RinosAinda não há avaliações
- Peritoneal DialysisDocumento17 páginasPeritoneal Dialysisellya theresiaAinda não há avaliações
- CASE REPORT: 75-YEAR-OLD WOMAN WITH 25% BODY SURFACE AREA BURNSDocumento64 páginasCASE REPORT: 75-YEAR-OLD WOMAN WITH 25% BODY SURFACE AREA BURNSabdul100% (1)
- CASP Checklist: Case Control Study How To Use This Appraisal ToolDocumento6 páginasCASP Checklist: Case Control Study How To Use This Appraisal Toolanon_770867052Ainda não há avaliações
- EBM CYCLE AND PICO QUESTIONDocumento40 páginasEBM CYCLE AND PICO QUESTIONmuthia saniAinda não há avaliações
- Manage Anemia in CKD Patients: Iron Therapy GuidelinesDocumento36 páginasManage Anemia in CKD Patients: Iron Therapy GuidelinesLaurensia Erlina NataliaAinda não há avaliações
- Transfusi Darah: Indikasi, Komponen, Golongan Darah dan Tes KompatibilitasDocumento17 páginasTransfusi Darah: Indikasi, Komponen, Golongan Darah dan Tes KompatibilitasRenggaSuhardijantoAinda não há avaliações
- Peritoneal Dialysis: An OverviewDocumento62 páginasPeritoneal Dialysis: An OverviewM. Tarmizi TaherAinda não há avaliações
- Algorithms For IV Fluid Therapy in Children and Young People in Hospital Set of 6 PDF 2190274957 PDFDocumento6 páginasAlgorithms For IV Fluid Therapy in Children and Young People in Hospital Set of 6 PDF 2190274957 PDFFurqon AfandriAinda não há avaliações
- Anemia in Chronic Kidney DiseaseDocumento38 páginasAnemia in Chronic Kidney DiseaseHemodialisa LindimaraAinda não há avaliações
- Kuliah 3. Pengaturan Osmolalitas UrinDocumento19 páginasKuliah 3. Pengaturan Osmolalitas UrinAnnisa DamayantiAinda não há avaliações
- (CKD-MBD) : Chronic Kidney Disease - Mineral and Bone DisorderDocumento41 páginas(CKD-MBD) : Chronic Kidney Disease - Mineral and Bone DisorderronyheryadiAinda não há avaliações
- AKI & Indikasi CRRTDocumento25 páginasAKI & Indikasi CRRTMaya Sari BaharumAinda não há avaliações
- Principlesofhemodialysisfinal2017 171216103708 PDFDocumento53 páginasPrinciplesofhemodialysisfinal2017 171216103708 PDFJoao FonsecaAinda não há avaliações
- Dr. Risna Weil's DiseaseDocumento36 páginasDr. Risna Weil's DiseasedrroytambunanAinda não há avaliações
- Terapi Plasma Konvalesen PERDICIDocumento25 páginasTerapi Plasma Konvalesen PERDICIHening Shanti SemestaAinda não há avaliações
- DR Arwedi Inisiasi HD Pit 2018Documento28 páginasDR Arwedi Inisiasi HD Pit 2018Aulia Achmad Yudha PratamaAinda não há avaliações
- Vascular Acces in Hemodyalisi - DR DjoniDocumento50 páginasVascular Acces in Hemodyalisi - DR DjoniMohamad ZulfikarAinda não há avaliações
- Guidelines For The Clinical Management of ThalassemiaDocumento205 páginasGuidelines For The Clinical Management of ThalassemiaAmalia Muchammad BafagihAinda não há avaliações
- Hemodialysis Adequacy: Assessing Urea ClearanceDocumento58 páginasHemodialysis Adequacy: Assessing Urea ClearanceAbdee Tarmizi IIAinda não há avaliações
- Pancytopenia As Initial Presentation of Acute Lymphoblastic Leukemia and Its Associationwith Bone MarrowresponseDocumento6 páginasPancytopenia As Initial Presentation of Acute Lymphoblastic Leukemia and Its Associationwith Bone MarrowresponseIJAR JOURNALAinda não há avaliações
- Mengenal Resusitasi Pada Anak Dan Bayi Bagi Perawat PemulaDocumento15 páginasMengenal Resusitasi Pada Anak Dan Bayi Bagi Perawat PemulaSiti Krisan WijayaAinda não há avaliações
- Taco and Trali: Savita HandayaniDocumento12 páginasTaco and Trali: Savita HandayaniAnna Puteri GozaliAinda não há avaliações
- Congenital Adrenal HyperplasiaDocumento14 páginasCongenital Adrenal HyperplasiabangkitayuAinda não há avaliações
- K-5 Pathophysiology of Cyanotic Congenital Heart DefectsDocumento15 páginasK-5 Pathophysiology of Cyanotic Congenital Heart DefectsJessica GintingAinda não há avaliações
- Sepsis Update 2017 - 2Documento49 páginasSepsis Update 2017 - 2Ahmad Fathul Adzmi100% (1)
- Terapi Cairan PediatriDocumento74 páginasTerapi Cairan PediatriAnonymous 0SYzMqje2100% (1)
- What Do We Know About Patent Dustus Arteriosus - Dr. Adhi Teguh, Sp.a (K)Documento39 páginasWhat Do We Know About Patent Dustus Arteriosus - Dr. Adhi Teguh, Sp.a (K)laurentiaAinda não há avaliações
- Hormon Paratiroid: Dr. Muniroh, SP - PKDocumento10 páginasHormon Paratiroid: Dr. Muniroh, SP - PKFuadi FaisalAinda não há avaliações
- Fluid Therapy in DengueDocumento54 páginasFluid Therapy in DengueVithiya Chandra SagaranAinda não há avaliações
- Burat-Buret Echo Romi Revised PDFDocumento2 páginasBurat-Buret Echo Romi Revised PDFAsma.denmiAinda não há avaliações
- Penyakit Ginjal Kronik Dan Indikasi Dialisis DR Ratih Tri KD MAJUDocumento56 páginasPenyakit Ginjal Kronik Dan Indikasi Dialisis DR Ratih Tri KD MAJUFitriana WijayatiAinda não há avaliações
- (INFEKSI) - FKUI - Nelwan Score Typhoid Fever.2016Documento10 páginas(INFEKSI) - FKUI - Nelwan Score Typhoid Fever.2016Yolanda FitrianiAinda não há avaliações
- Differential Diagnosis of Microcytic Anemia PDFDocumento5 páginasDifferential Diagnosis of Microcytic Anemia PDFayms99Ainda não há avaliações
- Tatalaksana Awal Koreksi Cairan pada Kasus SyokDocumento60 páginasTatalaksana Awal Koreksi Cairan pada Kasus Syokmuhammad benyAinda não há avaliações
- Konas Perdatin 2019Documento66 páginasKonas Perdatin 2019Akreditasi RSPC19Ainda não há avaliações
- Congenital Adrenal HyperplasiaDocumento2 páginasCongenital Adrenal HyperplasiaesyAinda não há avaliações
- Malaria Management Asep MCU FinalDocumento65 páginasMalaria Management Asep MCU FinalTommy JunaidiAinda não há avaliações
- Tarif Pelayanan HemodialisaDocumento7 páginasTarif Pelayanan HemodialisaNur IffahAinda não há avaliações
- AML Patient with Bleeding and AnemiaDocumento17 páginasAML Patient with Bleeding and AnemiaHarisAinda não há avaliações
- Ozid Iv (Omeprazole) : Cedocard Iv (Isosorbid Dinitrat)Documento15 páginasOzid Iv (Omeprazole) : Cedocard Iv (Isosorbid Dinitrat)Galih Aryo UtomoAinda não há avaliações
- DR Rudi IPDI2017 Insersi Kateter Peritonel Dan Komplikasiny 1Documento73 páginasDR Rudi IPDI2017 Insersi Kateter Peritonel Dan Komplikasiny 1julia sianturi100% (1)
- Wsop Asma - Prof Bambang SDocumento67 páginasWsop Asma - Prof Bambang SSiti Arieanni KesumaAinda não há avaliações
- Basic IV FluidDocumento77 páginasBasic IV FluiddaaaniiisAinda não há avaliações
- Kuliah: Renjatan Hipovolemi Pada Anak (Hypovolemic Shock in Children)Documento17 páginasKuliah: Renjatan Hipovolemi Pada Anak (Hypovolemic Shock in Children)DillaAinda não há avaliações
- Balans Cairan & Elektrolit RSTDocumento59 páginasBalans Cairan & Elektrolit RSTdianAinda não há avaliações
- Management Terapi Cairan Dr. AW 01Documento60 páginasManagement Terapi Cairan Dr. AW 01Umhy GumianaAinda não há avaliações
- Thalassemia: A New Concept in ScreeningDocumento10 páginasThalassemia: A New Concept in ScreeningNoer HafniAinda não há avaliações
- Trombositosis Esensial: (Essential Thrombocytosis)Documento9 páginasTrombositosis Esensial: (Essential Thrombocytosis)shahrasyiddAinda não há avaliações
- Departemen Ilmu Kesehatan AnakDocumento5 páginasDepartemen Ilmu Kesehatan Anakagus rasidAinda não há avaliações
- Nutrisi - Dr. Afiatin PDFDocumento68 páginasNutrisi - Dr. Afiatin PDFekorahmanadiAinda não há avaliações
- Dr. Nyoman - Neuropsychiatric Systemic Lupus Erythematosus (NPSLE) .Documento41 páginasDr. Nyoman - Neuropsychiatric Systemic Lupus Erythematosus (NPSLE) .hum2Ainda não há avaliações
- ANEMIA PADA KEBIDANANDocumento18 páginasANEMIA PADA KEBIDANANHarry ChristamaAinda não há avaliações
- Anemia Pada CKD - 2015Documento61 páginasAnemia Pada CKD - 2015Anonymous wVgEAr6Ainda não há avaliações
- Final Announcement Book 26th ASMIHA 2017-1Documento47 páginasFinal Announcement Book 26th ASMIHA 2017-1d.ramadhanAinda não há avaliações
- TELAAH KRITIS JURNAL Kel 2 - RCTDocumento20 páginasTELAAH KRITIS JURNAL Kel 2 - RCTNama ManaAinda não há avaliações
- Peritonitis in PD PatientsDocumento64 páginasPeritonitis in PD PatientsDaniel SitungkirAinda não há avaliações
- Peritoneal DialysisDocumento10 páginasPeritoneal DialysisPdianghunAinda não há avaliações
- Renal Nursing 4 April 2021Documento30 páginasRenal Nursing 4 April 2021Benard Were100% (1)
- Acute N Chronic Complication of HD - YennyDocumento77 páginasAcute N Chronic Complication of HD - YennyAndriKusumaAinda não há avaliações
- Dialyzer Reuse For DialysisDocumento25 páginasDialyzer Reuse For DialysisAndriKusuma100% (3)
- Anticoagulant TherapyDocumento47 páginasAnticoagulant TherapyAndriKusuma75% (4)
- Dialyzer Reuse For DialysisDocumento25 páginasDialyzer Reuse For DialysisAndriKusuma100% (3)
- Medication Safety Anticoagulation ManagementDocumento39 páginasMedication Safety Anticoagulation ManagementAndriKusumaAinda não há avaliações
- DialysisDocumento14 páginasDialysisAndriKusumaAinda não há avaliações
- Dialyzer Reuse For DialysisDocumento25 páginasDialyzer Reuse For DialysisAndriKusuma100% (3)
- Anticoagulant TherapyDocumento47 páginasAnticoagulant TherapyAndriKusuma75% (4)
- Acute N Chronic Complication of HD - YennyDocumento77 páginasAcute N Chronic Complication of HD - YennyAndriKusumaAinda não há avaliações
- Composition and Regulation of Body FluidsDocumento32 páginasComposition and Regulation of Body FluidsAndriKusumaAinda não há avaliações
- Effects of Hypotonic, Isotonic & Hypertonic SolutionsDocumento19 páginasEffects of Hypotonic, Isotonic & Hypertonic SolutionsTanesh SelvarajuAinda não há avaliações
- Cadmium Tolerance in Schinus Molle Trees Is Modulated by Enhanced Leaf Anatomy and PhotosynthesisDocumento8 páginasCadmium Tolerance in Schinus Molle Trees Is Modulated by Enhanced Leaf Anatomy and PhotosynthesisPaulinho TemoteoAinda não há avaliações
- Integrating Seed Systems For Annual Food CropsDocumento329 páginasIntegrating Seed Systems For Annual Food Cropskiranreddy9999Ainda não há avaliações
- Quirino State University Self-Paced Module on Genetic Trait ModificationsDocumento5 páginasQuirino State University Self-Paced Module on Genetic Trait ModificationsNel McMahon Dela PeñaAinda não há avaliações
- Péptidos de Colágeno para Salud y Nutrición - Colombia May17Documento57 páginasPéptidos de Colágeno para Salud y Nutrición - Colombia May17Irene Serna100% (1)
- Happ Chapter 8 TransesDocumento13 páginasHapp Chapter 8 TransesFrencess Kaye SimonAinda não há avaliações
- Pforams@Mikrotax - Globigerinoides ConglobatusDocumento2 páginasPforams@Mikrotax - Globigerinoides ConglobatusAhmad Lumban GaolAinda não há avaliações
- Interpretation of Histograms and Peripheral Smear FindingsDocumento5 páginasInterpretation of Histograms and Peripheral Smear FindingsrezqiAinda não há avaliações
- Dunhan R.A. Aquaculture and Fisheries BiotechnologyDocumento385 páginasDunhan R.A. Aquaculture and Fisheries BiotechnologyAleksey DubinAinda não há avaliações
- IB Biology Notes - 1 Working With DataDocumento1 páginaIB Biology Notes - 1 Working With DataWanda Wawa EvirhaAinda não há avaliações
- B VIDAS T4 enDocumento7 páginasB VIDAS T4 enInn MironAinda não há avaliações
- Gender and Human Evolution PDFDocumento49 páginasGender and Human Evolution PDFSimio PensanteAinda não há avaliações
- Different Types of VaccinesDocumento2 páginasDifferent Types of VaccinesBhuvaneshAinda não há avaliações
- A4 QB-MC Ch06 Nutrition in HumansDocumento18 páginasA4 QB-MC Ch06 Nutrition in HumansReg ChooAinda não há avaliações
- Facial Esthetics in FPDDocumento8 páginasFacial Esthetics in FPDrayavarapu sunilAinda não há avaliações
- A Conceptual Framework of Consumer Food Choice Behaviour: CEFAGE-UE Working Paper 2009/06Documento26 páginasA Conceptual Framework of Consumer Food Choice Behaviour: CEFAGE-UE Working Paper 2009/06Krishnendu Kizhakedathu SudhakaranAinda não há avaliações
- Chemistry in Everyday LifeDocumento14 páginasChemistry in Everyday LifeAkhil NandanAinda não há avaliações
- My Home To School RoadmapDocumento22 páginasMy Home To School RoadmapDarlene Joyce ApolinarioAinda não há avaliações
- Do Genes Determine Champions?Documento6 páginasDo Genes Determine Champions?mensrea0Ainda não há avaliações
- Biology StandardsDocumento5 páginasBiology Standardsapi-323917812Ainda não há avaliações
- Basic Hydroponic Systems and How They WorkDocumento13 páginasBasic Hydroponic Systems and How They WorkJaime HernandezAinda não há avaliações
- SP4 Memes - UmaliDocumento6 páginasSP4 Memes - UmaliSheryl Anne Benigno UmaliAinda não há avaliações
- Cardiology Ebook Notes PDFDocumento26 páginasCardiology Ebook Notes PDFsugisweAinda não há avaliações
- Sticky Trap Monitoring of Insect Pests: Steve H. DreistadtDocumento8 páginasSticky Trap Monitoring of Insect Pests: Steve H. DreistadtBryan AbarcaAinda não há avaliações
- Genetic Landscapes GISDocumento21 páginasGenetic Landscapes GISjuanAinda não há avaliações
- Learning Activity Sheet: SUBJECT: Earth and Life Science Mastery Test For Quarter 2 - Week 1&2Documento1 páginaLearning Activity Sheet: SUBJECT: Earth and Life Science Mastery Test For Quarter 2 - Week 1&2Kiara Ash BeethovenAinda não há avaliações
- The Neuropsychology of EmotionDocumento532 páginasThe Neuropsychology of EmotionLarisa Ev-a Elena95% (43)
- Sunscreens and Photoaging: A Review of Current Literature: Linna L. Guan Henry W. Lim Tasneem F. MohammadDocumento10 páginasSunscreens and Photoaging: A Review of Current Literature: Linna L. Guan Henry W. Lim Tasneem F. MohammadMatea KalacAinda não há avaliações
- Colposcopy, Cervical Screening, and HPV: A Guide to Prevention and ManagementDocumento155 páginasColposcopy, Cervical Screening, and HPV: A Guide to Prevention and ManagementAnnca RoXanna100% (1)