Escolar Documentos
Profissional Documentos
Cultura Documentos
DMS. K15a. Connective Tissue Diseases
Enviado por
missirenaDireitos autorais
Formatos disponíveis
Compartilhar este documento
Compartilhar ou incorporar documento
Você considera este documento útil?
Este conteúdo é inapropriado?
Denunciar este documentoDireitos autorais:
Formatos disponíveis
DMS. K15a. Connective Tissue Diseases
Enviado por
missirenaDireitos autorais:
Formatos disponíveis
Connective Tissue
Diseases
School of Medicine
University of Sumatera Utara
Classification of connective tissue
disease
Lupus erythematosus
Dermatomyositis
Scleroderma
Rheumatoid arthritis
sjogrens syndrome
Mixed connective tissue disease
Eosinophilic fascitis
Basic of them all is a complex array of
autoimmune responses
Lupus erythematosus
Discoid lupus erythematosus
Systemic lupus erythematosus
Discoid Lupus erythematosus
Young adult
Women: men = 2:1
Clinnical Findings :
Dull red macule with adherent scale with
follicular plugging, which heal with atrophy,
scarring and pigemantary changing,
telangiekatasis.
Side: usually above the neck. Favorite are
scalp, bridges of the nose, malar areas,
lower lips and ears
Generalized dle is less common than
localized DLE and is usually
suerimposed on alocallized discoid
case.
Progression from DLE to systemic
lupus erythematosus (SLE) is
uncommon.
Differential diagnosis
Seborrheic dermatitis
Rosacea
Lupus vulagris
Sarcoid
Drug eruption
Treatment
Avoid exposure to sunlight, excessive
cold, to heat and trauma
Use a high SPF sun screen
Local:
potent or super potent corticosteroid
Intralesional triamsinolon acetonide 2,5 to
10 mg/ml
Systemic
Anti malarials. Hydroxychloroquine 6,5
mg/kg/day. Chloroquine 250 mg/day
Quinacrine
Systemic corticosteroid for widespread
or disfuguring lesion
Systemic Lupus Erythematosus
Young to middle aged women
Skin involvement occurs in 80% of
cases
Diagnosis of SLE are based on four of
the American Rheumatism
Assosiations 11 criteria
Cutaneus manifestation
Butterfly facial erythemmabullous lesion
Diffuse, non scarring hair loss
Mucous membrane lesion eq
conjunctivitis, episcleritis, vaginal ulcer
Leg ulcer
Cutaneeous angiitis
Calcinosis cutis
Systemic manifestation
Arthralgia
Renal involvement
Myocarditis
CNS involvement
Vasculitis
Convulsion
Epilepsy
Retinitis
Idiopathic trombocytopenic purpura
Etiology
Genetic
Altered immune respon
Drugs such as hydralazine, procainamid,
sulfonamid, penicillin, anticonvulsan,
minocycline and isoniazid
Laboratory findings
Anemia hemolytic
Thrombocytopenia
Lymphopenia
Leukopenia
Erythrocyte sedimentation rate is
elevated
Coombs tes positif
Rgeumatoid factor positif
Immulogic findings
ANA test
LE cell test
Ds DNA
Anti SM antibody
Lupus band test
ANA pattern
Differential diagnosis
Dermtaomyositis
Toxic erytema multiforme
Acute rheumatoid fever
Drug eruption
Sjogrens syndrome
Treatment
Avoid exposure to sunlight and use a high SPF
sun screen
Antimalarial: hydroxychlotoquin or chloroquin
Corticosteroid: 1000 mg of prednisolone IV
daily for 3 days , followed bt oraal prednisone
0,5 to 1 mg/kg/dailly
Immunosuppressive therapy: azathiopreine,
methotrexate and cyclophosphamide
Scleroderma
Scleroderma is sclerosis of the skin
characterized by the appearance of
circumscribe or diffuse, hard,
smooth, ivory colored areas that are
immobile and give the appearance of
hidebound skin
Form of Scleroderma :
Localized scleroderma: morphea and
linear scleroderma
Systemic scleroderma: Progressive
systemic sclerosis and CREST syndrome
Morphea
Twice common in women as in men
Occurs in childhood as well as adult
Skin findings:
Rose aor violaceoous macules with
smooth,, hard, somewhat depressed,
yellowish whte or ivory-coloured lesion.
The marfin surrounded by llight
violaceous zone or by telangiectases
Site: trunk, extremities
Generallized morphea : widespread
involvement by indurated plaques with
hypo or hperppigmentation . There is no
systemic involvement
Linear scleroderma: linear lession extend
the lenght oh the arm or leg, beginning in
the first decade of life. May also occur
parasagittally onthe frontal scalp and
extend part way down the forehead (en
coup de sabre)
Systemic scleroderma
Progressive syastemic sclerosis (PSS)
is a generalized disorder of
connective tissue in which there is
fibrous thickening of the skin
combine with fibrosis and vascular
abnormalities in certain internal
organs.
Women are affected three times
more commonly than men
Peak age onset between the third
abbbnd fifth decade
Raynauds phenomenon is the first
manifestation
Skin findings:
Raynauds phenomenon
Ski becomes smooth, yellowish, and
firm and shrink
Site:
face expressionless
Hands: clawllike (sslerodactily)
Internal involvement
Gastrointestinal: esophageal atony
Pulmonary fibrosis
Cardiac involvement: dyspnea,
palpitation
Renal failure
Skeletal involvement: articular pain,
swelling and inflammation
CREST
Systemic sclerosis that limited to the
hands, or somtime hands and lower
face. If it is associated with calcinosis,
Raynauds phenomena, esophageal
dysnotility, sclerodactily and
telangiectasia is called CREST syndrome
Laboratory findings
ANA test
antibodies to nuclear RNP
Differential diagnosis
Myxedema
Scleredema
scleromyxedema
Pathogenesis
Primary vascular damage
Autoimmune mechanism
Microchimerism
infection
Treatment
calcium channel blocker nifedipin 10 mg
four times daily.
Oral calcitriol
Azathioprine or cyclophosphamide
Prednisone
D-penisilamine
Low dose UVA 1
Você também pode gostar
- Dms. k24. Skin Manifestations of Nutritional DisordersDocumento33 páginasDms. k24. Skin Manifestations of Nutritional DisordersmissirenaAinda não há avaliações
- Major MineralsDocumento31 páginasMajor MineralsmissirenaAinda não há avaliações
- DMS. K22. Obat TopikalDocumento23 páginasDMS. K22. Obat TopikalmissirenaAinda não há avaliações
- DMS. K05. Other Parasitic InfectionsDocumento17 páginasDMS. K05. Other Parasitic InfectionsmissirenaAinda não há avaliações
- DMS. K13. Antifungal + AntilepraDocumento37 páginasDMS. K13. Antifungal + AntilepramissirenaAinda não há avaliações
- K19 - Pharmacology of NAPZAededDocumento62 páginasK19 - Pharmacology of NAPZAededwlmhfpAinda não há avaliações
- Fungal Infections of the Skin, Hair and NailsDocumento120 páginasFungal Infections of the Skin, Hair and NailsmissirenaAinda não há avaliações
- DMS. K12. DermatopathologyDocumento64 páginasDMS. K12. DermatopathologymissirenaAinda não há avaliações
- Delirium, Dementia, Amnestic & Other Cognitive and Mental KBKDocumento18 páginasDelirium, Dementia, Amnestic & Other Cognitive and Mental KBKIndah Permata SariAinda não há avaliações
- DMS. K09b. LeprosyDocumento41 páginasDMS. K09b. LeprosymissirenaAinda não há avaliações
- Defense MechanismDocumento19 páginasDefense MechanismmissirenaAinda não há avaliações
- Kuliah CardiovascularDocumento60 páginasKuliah CardiovascularmissirenaAinda não há avaliações
- K - 7 & K - 8 Female Reproduction Hormone (Biokimia)Documento36 páginasK - 7 & K - 8 Female Reproduction Hormone (Biokimia)missirenaAinda não há avaliações
- DMS. K02a. Struktur Dasar Dan Fungsi KulitDocumento54 páginasDMS. K02a. Struktur Dasar Dan Fungsi KulitmissirenaAinda não há avaliações
- K1 - Histo Skin 2013Documento36 páginasK1 - Histo Skin 2013Desi Indah LaisAinda não há avaliações
- K - 11 Physiology of Pregnancy (Fisiologi)Documento46 páginasK - 11 Physiology of Pregnancy (Fisiologi)missirenaAinda não há avaliações
- K - 13 Perkembangan Morfologi Dan Fungsional Janin (Obgyn)Documento53 páginasK - 13 Perkembangan Morfologi Dan Fungsional Janin (Obgyn)missirenaAinda não há avaliações
- K - 16 Congestive Heart Failure (Fisiologi)Documento23 páginasK - 16 Congestive Heart Failure (Fisiologi)missirenaAinda não há avaliações
- K - 5 Coronary Artery Disease (Kardiologi)Documento32 páginasK - 5 Coronary Artery Disease (Kardiologi)missirenaAinda não há avaliações
- K - 4 Aterioskleoris & Penyakit Jantung Koroner (Fisiologi)Documento34 páginasK - 4 Aterioskleoris & Penyakit Jantung Koroner (Fisiologi)missirenaAinda não há avaliações
- K - 7 Demam Rematik (Kardiologi)Documento40 páginasK - 7 Demam Rematik (Kardiologi)missirenaAinda não há avaliações
- K - 16 Congestive Heart Failure (Fisiologi)Documento23 páginasK - 16 Congestive Heart Failure (Fisiologi)missirenaAinda não há avaliações
- K - 15 Myocarditis (Kardiologi)Documento51 páginasK - 15 Myocarditis (Kardiologi)missirenaAinda não há avaliações
- K - 9 Male Reproductive Hormone (Biokimia)Documento14 páginasK - 9 Male Reproductive Hormone (Biokimia)missirenaAinda não há avaliações
- K - 12 Heart As A Pump (Fisiologi)Documento36 páginasK - 12 Heart As A Pump (Fisiologi)missirenaAinda não há avaliações
- K - 6 Acute Rheumatic FeverDocumento31 páginasK - 6 Acute Rheumatic FeverEster SibaraniAinda não há avaliações
- K - 4 Valvular Heart Disease (Fisiologi)Documento19 páginasK - 4 Valvular Heart Disease (Fisiologi)missirenaAinda não há avaliações
- Histology of Cardiovascular System (Histologi)Documento57 páginasHistology of Cardiovascular System (Histologi)missirena100% (1)
- K - 8 Cardiac Infection (Mikrobiologi)Documento81 páginasK - 8 Cardiac Infection (Mikrobiologi)missirenaAinda não há avaliações
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeNo EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeNota: 4 de 5 estrelas4/5 (5794)
- The Little Book of Hygge: Danish Secrets to Happy LivingNo EverandThe Little Book of Hygge: Danish Secrets to Happy LivingNota: 3.5 de 5 estrelas3.5/5 (399)
- Never Split the Difference: Negotiating As If Your Life Depended On ItNo EverandNever Split the Difference: Negotiating As If Your Life Depended On ItNota: 4.5 de 5 estrelas4.5/5 (838)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceNo EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceNota: 4 de 5 estrelas4/5 (895)
- The Yellow House: A Memoir (2019 National Book Award Winner)No EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Nota: 4 de 5 estrelas4/5 (98)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryNo EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryNota: 3.5 de 5 estrelas3.5/5 (231)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureNo EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureNota: 4.5 de 5 estrelas4.5/5 (474)
- Team of Rivals: The Political Genius of Abraham LincolnNo EverandTeam of Rivals: The Political Genius of Abraham LincolnNota: 4.5 de 5 estrelas4.5/5 (234)
- The Emperor of All Maladies: A Biography of CancerNo EverandThe Emperor of All Maladies: A Biography of CancerNota: 4.5 de 5 estrelas4.5/5 (271)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersNo EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersNota: 4.5 de 5 estrelas4.5/5 (344)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaNo EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaNota: 4.5 de 5 estrelas4.5/5 (266)
- The Unwinding: An Inner History of the New AmericaNo EverandThe Unwinding: An Inner History of the New AmericaNota: 4 de 5 estrelas4/5 (45)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyNo EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyNota: 3.5 de 5 estrelas3.5/5 (2219)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreNo EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreNota: 4 de 5 estrelas4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)No EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Nota: 4.5 de 5 estrelas4.5/5 (120)
- Bahia Slave RevoltDocumento73 páginasBahia Slave Revoltalexandercarberry1543Ainda não há avaliações
- Ponnu ThomasDocumento155 páginasPonnu ThomasWinston KennethAinda não há avaliações
- Mercyhurst Magazine - Winter 1989-90Documento36 páginasMercyhurst Magazine - Winter 1989-90hurstalumniAinda não há avaliações
- Soderstrom - Circuit Modeling of Cyanex 272Documento17 páginasSoderstrom - Circuit Modeling of Cyanex 272Anonymous OnoowoAinda não há avaliações
- Risk Management Framework and ProcessDocumento16 páginasRisk Management Framework and ProcessIuliana T.Ainda não há avaliações
- Cinderella Play ScriptDocumento6 páginasCinderella Play ScriptKhayla Khairunnisa81% (21)
- European Management Journal: Rainer Lueg, Ronny RadlachDocumento14 páginasEuropean Management Journal: Rainer Lueg, Ronny RadlachPutri MutiraAinda não há avaliações
- SCL9. UV-Vis Spectroscopy - Zamir Sarvari 180410101Documento3 páginasSCL9. UV-Vis Spectroscopy - Zamir Sarvari 180410101ZamirAinda não há avaliações
- Demo TeachingDocumento27 páginasDemo TeachingVince BulayogAinda não há avaliações
- Indikasi, Teknik Pembuatan Stoma, ReanastomosispptDocumento43 páginasIndikasi, Teknik Pembuatan Stoma, ReanastomosispptErwin Aritama Ismail100% (1)
- Organization and Operation of Partnerships and LLPsDocumento50 páginasOrganization and Operation of Partnerships and LLPsAliaa Hosam100% (1)
- dll-4th QTR.-MUSIC-MAY-3-4-2023Documento5 páginasdll-4th QTR.-MUSIC-MAY-3-4-2023Dennis MartinezAinda não há avaliações
- Puddu v. 6D Global Tech. - Securities Complaint PDFDocumento57 páginasPuddu v. 6D Global Tech. - Securities Complaint PDFMark JaffeAinda não há avaliações
- PR Out of Nothing by Kate BurvillDocumento11 páginasPR Out of Nothing by Kate BurvillCulture Comms0% (1)
- (2019) 7 CLJ 560 PDFDocumento12 páginas(2019) 7 CLJ 560 PDFhuntaAinda não há avaliações
- 11Documento24 páginas11anil.gelra5140100% (1)
- The Nazi Master PlanDocumento28 páginasThe Nazi Master PlanFolad109Ainda não há avaliações
- Strict Liability Offences ExplainedDocumento7 páginasStrict Liability Offences ExplainedJoseph ClarkAinda não há avaliações
- The Effect of Work Discipline and Leadership On Organizational Commitments With Work Satisfaction As Intervening Variables (Case Study at Asam Jujuhan Sub-District Office Dharmasraya Regency)Documento11 páginasThe Effect of Work Discipline and Leadership On Organizational Commitments With Work Satisfaction As Intervening Variables (Case Study at Asam Jujuhan Sub-District Office Dharmasraya Regency)International Journal of Innovative Science and Research TechnologyAinda não há avaliações
- 1 Calimutan v. People - G.R. No. 152133Documento1 página1 Calimutan v. People - G.R. No. 152133eiram23100% (1)
- Learning Activity Sheet in 3is (Inquiries, Investigation, Immersion)Documento5 páginasLearning Activity Sheet in 3is (Inquiries, Investigation, Immersion)Roselyn Relacion LucidoAinda não há avaliações
- Double Crush SyndromeDocumento14 páginasDouble Crush SyndromeJosip SulenticAinda não há avaliações
- DFA vs NLRC Immunity DisputeDocumento7 páginasDFA vs NLRC Immunity DisputeThrees SeeAinda não há avaliações
- Transits of The Year 2008: Text by Robert HandDocumento27 páginasTransits of The Year 2008: Text by Robert HandjasminnexAinda não há avaliações
- Notes For MDES PsychologyDocumento31 páginasNotes For MDES Psychologyvct64677Ainda não há avaliações
- Historic Struggle For Pakistan 1857 - 1947Documento32 páginasHistoric Struggle For Pakistan 1857 - 1947The CSS Point82% (79)
- Ambien Withdrawal TreatmentDocumento6 páginasAmbien Withdrawal TreatmentSurvival SabariAinda não há avaliações
- Realiability of Digital Micromirror Device Final VersionDocumento13 páginasRealiability of Digital Micromirror Device Final VersionRaj MistryAinda não há avaliações
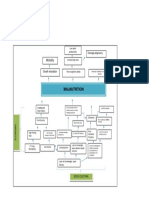
- Problem Tree Analysis MalnutritionDocumento1 páginaProblem Tree Analysis MalnutritionMho Dsb50% (6)