Escolar Documentos
Profissional Documentos
Cultura Documentos
AcutePerio Class
Enviado por
Bala Raghavendra G N0 notas0% acharam este documento útil (0 voto)
25 visualizações36 páginasTítulo original
AcutePerio class
Direitos autorais
© Attribution Non-Commercial (BY-NC)
Formatos disponíveis
PPT, PDF, TXT ou leia online no Scribd
Compartilhar este documento
Compartilhar ou incorporar documento
Você considera este documento útil?
Este conteúdo é inapropriado?
Denunciar este documentoDireitos autorais:
Attribution Non-Commercial (BY-NC)
Formatos disponíveis
Baixe no formato PPT, PDF, TXT ou leia online no Scribd
0 notas0% acharam este documento útil (0 voto)
25 visualizações36 páginasAcutePerio Class
Enviado por
Bala Raghavendra G NDireitos autorais:
Attribution Non-Commercial (BY-NC)
Formatos disponíveis
Baixe no formato PPT, PDF, TXT ou leia online no Scribd
Você está na página 1de 36
Acute Periodontal Conditions
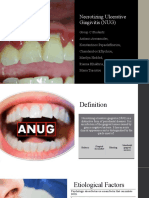
Acute Necrotising Ulcerative
Gingivitis - Clinical Features
Sudden onset
Red, shiny gingivae which bleed easily
Ulceration of interdental papillae, with tissue
destruction
Pseudomembranous slough
Halitosis
Metallic taste
Very painful
Submental/Submandibular lymphadenitis
ANUG - Occurrence
M=F
Majority 18 - 30 years
Rare in young children, middle-age and elderly
Recurrent episodes common unless adequately
treated
In deprived regions of Africa may spread to affect the
facial tissues - cancrum oris or noma
ANUG - Aetiology
Probably caused by opportunistic infection of the
gingival tissue by commensal micro-organisms
Classically a fuso-spirochaetal complex, but more
recent studies suggest a mixed anaerobic infection
Predisposing factors:
– Inadequate Oral Hygiene
– Smoking
– Mental Stress
– Underlying Systemic Disease esp. HIV
– Post-viral infection
ANUG - Treatment
Thorough debridement if not too painful with
ultrasonics
In severe cases remove loose debris with cotton wool
pellets soaked in 3% hydrogen peroxide
OHI - soft toothbrush
Mouthwashes - sodium perborate (Bocasan) may be
helpful in dislodging the slough and have a direct
effect on the bacteria. Can also use CHX
ANUG - Treatment (II)
Systemic Treatment - if adequate debridement
impossible - Metronidazole 200mg tds 3 days.
Penicillin is an alternative
Follow-up Care - OHI and monitor gingival healing
and contour. Severe destruction may need surgical
intervention
Acute Herpetic Stomatitis - Aetiology
Systemic infection with Herpes simplex virus (usually
type 1) which manifests by widespread intraoral
vesicles and ulceration
Often a disease of early childhood when dismissed as
“teething” - much more severe in adulthood
Highly contagious
Acute Herpetic Stomatitis -
Clinical Features
Sudden onset with high fever, cervical
lymphadenopathy and pain in mouth and throat
Gingivae may become acutely inflamed, oedematous
and tender
Intra-epithelial vesicles form with 24 hours usually on
tongue, buccal mucosa, palate and gingivae
Vesicles rupture early to give numerous small
round/irregular superficial greyish-yellow ulcers with a
red halo
Pain may interfere with eating, drinking and swallowing
Acute Herpetic Stomatitis -
Treatment
Mainly supportive
Includes soft diet with adequate fluid intake, bed rest
and analgesics
Oral ulceration is managed with chlorhexidine
mouthwash
Antiviral agents reserved for the
immunocompromised
Re-activation
Primary illness leads to infection of trigeminal
ganglion
Subsequent re-activation of the virus may occur.
Most commonly manifests as Herpes Labialis
Intra-oral re-activation may occur following trauma
such as surgery or infiltration anaesthesia.
Periodontal Abscess
An infection where the gingival sulcus or periodontal
pocket is the point of entry of the causative organism
An acute suppurative inflammatory lesion arising
from an acute exacerbation of chronic periodontitis
and/or trauma to the gingival sulcus/pocket lining
Aetiology
blockage of drainage from pocket may lead to the
accumulation of pus
trauma, caused by toothbrush bristles or food impaction
orthodontic or occlusal forces
dental procedures such as scaling
host defences compromised e.g. viral illness, diabetes
imbalance in flora
multiple perio abscesses suggests imbalance between
host and flora
Periodontal abscess - clinical features
Sudden onset
Pain on biting, percussion and may be continuous
Swelling and tenderness of overlying gingiva
Increased mobility
Bone loss
Usually drainage along root surface to pocket orifice
Extra-oral swelling is uncommon
Must be differentiated from periapical abscess
Periodontal vs Periapical
Factors which differentiate a periodontal abscess:
– tooth responds to vitality tests
– associated pocketing on affected tooth and other teeth
– in some cases get multiple periodontal abscesses
– different drainage pattern
– associated facial swelling does not normally occur
– pain usually less than periapical abscess
– bone loss pattern on radiographs may help to differentiate
Periodontal Abscess - Treatment
Poor prognosis if a lot of bone destruction - XLA
Drainage by dilating pocket orifice with blunt
instrument or incision
Gentle subgingival scaling to remove plaque, calculus
or foreign objects, usually under LA
Hot salty mouthwash at home
Systemic antibiotics not used unless concern about
permanent destruction or systemic upset
Review to check healing and carry out further
cleaning and OHI
Pericoronitis
A localised purulent infection within the tissue
surrounding the crown of partially-erupted tooth
Most commonly lower 8’s
Clinically:
– localised erythema and swelling, which is painful to the
touch
– maybe purulent exudate
– trismus
– lymphadenopathy
– fever and malaise
Pericoronitis (II)
Treatment:
– goal is to eliminate acute signs and symptoms
– irrigation using saline, CHX or iodine
– debridement, usually with LA
– antibiotics
– tissue re-contouring
– extraction of involved or opposing tooth
– review to determine satisfactory resolution and consider
further treatment e.g. extraction
Acute Traumatic Lesions
Damage due to toothbrushing
Pattern of ulceration of papilla and gingival margin
May be gingival recession and cervical abrasion
Suggest patient uses CHX for a week until ulcers heal
Re-educate
Review
Treat abrasion and sensitivity
References
Palmer & Floyd, A Clinical Guide to Periodontology,
BDJ Books 1996, Chapter 8
American Academy of Periodontology, Parameter on
Acute Periodontal Disease, www.perio.org
Carranza 9th Ed Chapters 45 & 46
Jenkins & Allen, Periodontics: A Synopsis, Wright,
1999, Chapter 20
THANK
YOU
TO WIN IS NOT TO FAIL BUT TO RISE
HIGHER EVERY TIME YOU FAIL
"What the mind of man can conceive and believe, it can achieve."
- Napoleon Hill
Você também pode gostar
- Oral Pathology in Pediatric DentistryDocumento48 páginasOral Pathology in Pediatric DentistryHanin AbukhiaraAinda não há avaliações
- Benign Oral Lesions Guide: Ulcers, Leukoplakia, Lichen Planus & MoreDocumento61 páginasBenign Oral Lesions Guide: Ulcers, Leukoplakia, Lichen Planus & MorecabralmdAinda não há avaliações
- ACUTE PERIODONTAL LESIONSDocumento36 páginasACUTE PERIODONTAL LESIONSDeepshika Saravanan100% (1)
- Ms Report NikolDocumento31 páginasMs Report NikolMinbinAinda não há avaliações
- Sequalae of Wearing Complete DenturesDocumento34 páginasSequalae of Wearing Complete DenturesAyeshaAslamAinda não há avaliações
- Periodontal EmergenciesDocumento47 páginasPeriodontal EmergenciesSubramanyam AarthiAinda não há avaliações
- Acute Periodontal Conditions: PeriodonticsDocumento9 páginasAcute Periodontal Conditions: Periodonticsmonica896Ainda não há avaliações
- Oral Lesions ....Documento104 páginasOral Lesions ....Yonas YemidiralemAinda não há avaliações
- Management of Patients With Oral and Esophageal Disorders PDFDocumento85 páginasManagement of Patients With Oral and Esophageal Disorders PDFNixi Mbuthia100% (1)
- Children's Periodontal Problems and TreatmentsDocumento49 páginasChildren's Periodontal Problems and TreatmentsRaksmey PhanAinda não há avaliações
- physicalandchemicalinjuriesoforalcavity-180120174153 (1)Documento71 páginasphysicalandchemicalinjuriesoforalcavity-180120174153 (1)draryajyoti1Ainda não há avaliações
- Acute Gingival LesionsDocumento70 páginasAcute Gingival LesionsIesha Crawford100% (1)
- acute periodontal coditionDocumento40 páginasacute periodontal coditionAzza AbushamaAinda não há avaliações
- Management of Patients With Oral and Esophageal Disorders 1Documento80 páginasManagement of Patients With Oral and Esophageal Disorders 1AndreAinda não há avaliações
- YCYSt DocumentDocumento24 páginasYCYSt DocumentDodo AlsunaidiAinda não há avaliações
- 3.EVALUATION AND EXAMINATION OF DENTAL PATIENTSDocumento77 páginas3.EVALUATION AND EXAMINATION OF DENTAL PATIENTScreativejoburgAinda não há avaliações
- Minor Oral Surgical Procedures in Children ClassDocumento65 páginasMinor Oral Surgical Procedures in Children ClassReenaChauhanAinda não há avaliações
- StomatitisDocumento44 páginasStomatitisNessa Layos Morillo100% (1)
- Oral Medicine: (I. Penyakit Mulut)Documento165 páginasOral Medicine: (I. Penyakit Mulut)Susanna Arie KAinda não há avaliações
- Oral UlcerationDocumento29 páginasOral UlcerationMINI DHABAAinda não há avaliações
- Acute Gingival InfectionsDocumento38 páginasAcute Gingival Infectionshoormunaf8Ainda não há avaliações
- Oral MedicineDocumento136 páginasOral Medicineganang19Ainda não há avaliações
- Oral Medicine: (I. Penyakit Mulut)Documento178 páginasOral Medicine: (I. Penyakit Mulut)claudiaciwiAinda não há avaliações
- Dentoalveolar Abscess GuideDocumento21 páginasDentoalveolar Abscess GuidePruthvish Patel50% (4)
- Actinomycosis: DR Maleeha Zia Mufti Lecturer Pathology Department AmcDocumento21 páginasActinomycosis: DR Maleeha Zia Mufti Lecturer Pathology Department Amcmaleeha100% (1)
- ميدسنDocumento43 páginasميدسنjuren.zafat.05Ainda não há avaliações
- Salivary GlandDocumento64 páginasSalivary GlandDanielicah Cruz100% (1)
- Pericoronitis Is Defined As The Inflammation of The Soft Tissues of Varying Severity Around An Erupting or Partially Erupted Tooth With Breach of The FollicleDocumento7 páginasPericoronitis Is Defined As The Inflammation of The Soft Tissues of Varying Severity Around An Erupting or Partially Erupted Tooth With Breach of The FollicleRavan WidiAinda não há avaliações
- Acute apical periodontitis causes and symptomsDocumento37 páginasAcute apical periodontitis causes and symptomsTri Deasy Permata Hati100% (1)
- 9acutegingivalinfections Pdabscess 160503154630Documento141 páginas9acutegingivalinfections Pdabscess 160503154630kishore KumarAinda não há avaliações
- Salivary Glands Disorders: Dr. Sirwan Abdullah Ali Fasmbs Ifso ASO Fach DR - Med.univDocumento56 páginasSalivary Glands Disorders: Dr. Sirwan Abdullah Ali Fasmbs Ifso ASO Fach DR - Med.univAbdelrahman GalalAinda não há avaliações
- Infectious Diseases of the Mouth: Bacteria, Viruses & Fungi That Cause Cold Sores, Tooth Decay, Gingivitis & MoreDocumento39 páginasInfectious Diseases of the Mouth: Bacteria, Viruses & Fungi That Cause Cold Sores, Tooth Decay, Gingivitis & MoreClancy Anne Garcia NavalAinda não há avaliações
- Management of Patients With Oral and Esophageal DisordersDocumento81 páginasManagement of Patients With Oral and Esophageal DisordersEdmond ChanAinda não há avaliações
- Oral MedicineDocumento174 páginasOral Medicineindah100% (1)
- Intranet.tdmu.Edu.ua Data Kafedra Internal Stomat Hir Classes Stud en Stomat Стоматология Ptn Хирургическая Стоматология 5 10 Semestr 25. Phlegmons of Submandibular, Submental Areas.htmDocumento1 páginaIntranet.tdmu.Edu.ua Data Kafedra Internal Stomat Hir Classes Stud en Stomat Стоматология Ptn Хирургическая Стоматология 5 10 Semestr 25. Phlegmons of Submandibular, Submental Areas.htmTri Sakti Sunda RomdhoniAinda não há avaliações
- Apical PeriodontitisDocumento30 páginasApical PeriodontitisTooba Sd100% (1)
- Abscess of THE PeriodontiumDocumento57 páginasAbscess of THE PeriodontiumSandeep SunilAinda não há avaliações
- Diseases of Periapical Tissues: Pulpitis, Apical Periodontitis, Granuloma, Cyst and AbscessDocumento41 páginasDiseases of Periapical Tissues: Pulpitis, Apical Periodontitis, Granuloma, Cyst and AbscessoladunniAinda não há avaliações
- Oral Surgery in Pediatric DentistryDocumento54 páginasOral Surgery in Pediatric DentistryRavi Gowda100% (2)
- Periapical LesionsDocumento36 páginasPeriapical LesionsGaddafi HamzaAinda não há avaliações
- Externa Otitis FinalDocumento11 páginasExterna Otitis Finalmalika.hirachan007Ainda não há avaliações
- Ulcerative Lesions of The Oral CavityDocumento39 páginasUlcerative Lesions of The Oral CavityIntania FadillaAinda não há avaliações
- Anatomy and Disorders of the Oral CavityDocumento24 páginasAnatomy and Disorders of the Oral CavityMuhammad SalmanAinda não há avaliações
- Oral PathologyDocumento19 páginasOral PathologyMaryjoy PaladanAinda não há avaliações
- Importance of Medical History in ProstthodonticsDocumento8 páginasImportance of Medical History in ProstthodonticsPavithra BalasubramaniyamAinda não há avaliações
- Period On Tit IsDocumento6 páginasPeriod On Tit Isanon_44979535Ainda não há avaliações
- Oral Cavity & GI TractDocumento17 páginasOral Cavity & GI TractMadiha MadiAinda não há avaliações
- Chapter 17 - Oral PathologyDocumento50 páginasChapter 17 - Oral PathologyShoyo HinataAinda não há avaliações
- DX of Pulpal N Apical Dis. NICEDocumento29 páginasDX of Pulpal N Apical Dis. NICEnoreenmyanmarAinda não há avaliações
- Oral Submucous FibrosisDocumento59 páginasOral Submucous Fibrosisvishalzenia100% (3)
- Upper GastrointestinalDocumento31 páginasUpper GastrointestinalGabriel EliAinda não há avaliações
- Salivary Glands PDFDocumento21 páginasSalivary Glands PDFAbdullah BhattiAinda não há avaliações
- Oral Manifestations of Abused Complete Denture UsageDocumento53 páginasOral Manifestations of Abused Complete Denture UsageBharanija100% (2)
- Otitis Exter Na: Jennifer WippermanDocumento9 páginasOtitis Exter Na: Jennifer Wippermandifa fatayaAinda não há avaliações
- Gingival EnlargementDocumento34 páginasGingival EnlargementNael AlmasriAinda não há avaliações
- Traslate Bab 8 TopazianDocumento87 páginasTraslate Bab 8 TopazianAnonymous bLf4glCRffAinda não há avaliações
- Sistem Pencernaan (Oral Soft Tissues) : Drg. Ade Ismail Abdul Kodir, MDSCDocumento71 páginasSistem Pencernaan (Oral Soft Tissues) : Drg. Ade Ismail Abdul Kodir, MDSCNismalaAinda não há avaliações
- PPK DOKTER GIGI EDIT Bareng (23102014) .2 PDFDocumento10 páginasPPK DOKTER GIGI EDIT Bareng (23102014) .2 PDFeatmyfleasAinda não há avaliações
- GINGIVAL Disease KulpakDocumento61 páginasGINGIVAL Disease KulpakAditya ZulfikarAinda não há avaliações
- 2003, Vol.21, Issues 1, Oral Medicine and Oral DermatologyDocumento212 páginas2003, Vol.21, Issues 1, Oral Medicine and Oral DermatologyRizweta DestinAinda não há avaliações
- Necrotizing PeriodontitisDocumento9 páginasNecrotizing Periodontitisعبدالملك المسفرAinda não há avaliações
- Chemical Periodontal TherapyDocumento23 páginasChemical Periodontal Therapyneji_murniAinda não há avaliações
- Capítulo 4 Carranza 11 Ed.Documento21 páginasCapítulo 4 Carranza 11 Ed.Estefanía Paz Torrejón GuzmánAinda não há avaliações
- Target MDS 1Documento44 páginasTarget MDS 1aftabssmAinda não há avaliações
- Oral Cavity Genetic Disorders Affecting The Oral Mucosa and LipsDocumento17 páginasOral Cavity Genetic Disorders Affecting The Oral Mucosa and LipsLakshya J BasumataryAinda não há avaliações
- ISSN: 0975-833X: Case StudyDocumento4 páginasISSN: 0975-833X: Case StudyantonAinda não há avaliações
- Burton's Microbiology For The Health Sciences: Chapter 19. Bacterial InfectionsDocumento29 páginasBurton's Microbiology For The Health Sciences: Chapter 19. Bacterial Infectionsmirai desuAinda não há avaliações
- Birao Sas 12 Microbiology and ParasitologyDocumento8 páginasBirao Sas 12 Microbiology and ParasitologyFrancis Jacob Dejecacion GarcesAinda não há avaliações
- DermatologytherapyDocumento642 páginasDermatologytherapyDhyna MutiarasariAinda não há avaliações
- k2 Stom F EngDocumento28 páginask2 Stom F Engdmd1983aminAinda não há avaliações
- Acute Necrotizing Ulcerative GingivitisDocumento5 páginasAcute Necrotizing Ulcerative GingivitisVictor GiraldezAinda não há avaliações
- Life If Soldiers in Trenches TrenchesDocumento13 páginasLife If Soldiers in Trenches TrenchesAmir FaheemAinda não há avaliações
- 2.oral Manifestation of Bacterial InfectionDocumento18 páginas2.oral Manifestation of Bacterial Infectionhesti_margarethaAinda não há avaliações
- Ceu Revalida Word97 2003docDocumento874 páginasCeu Revalida Word97 2003docChelo Jan Geronimo82% (11)
- STG 2017 Final November 2017 PDF For SharingDocumento389 páginasSTG 2017 Final November 2017 PDF For SharingVitalis Mbuya100% (2)
- Acute Ulcerative Stomatitis.Documento5 páginasAcute Ulcerative Stomatitis.Manar AlsoltanAinda não há avaliações
- 349 DR - Alyaa 3-2016Documento55 páginas349 DR - Alyaa 3-2016Kartik R. MorjariaAinda não há avaliações
- Acute Necrotizing Ulcerative GingivitisDocumento7 páginasAcute Necrotizing Ulcerative GingivitisdonnyAinda não há avaliações
- Diagnostico PeriodontalDocumento16 páginasDiagnostico PeriodontalLizeth GalvizAinda não há avaliações
- Pediatric Soft Tissue Lesions: Andres Pinto, DMDDocumento18 páginasPediatric Soft Tissue Lesions: Andres Pinto, DMDHanin AbukhiaraAinda não há avaliações
- Case Report AnugDocumento6 páginasCase Report AnugAzi Pertiwi HussainAinda não há avaliações
- Jaypee's Dental Dictionary (2009) (PDF) (UnitedVRG)Documento619 páginasJaypee's Dental Dictionary (2009) (PDF) (UnitedVRG)baselrehawiAinda não há avaliações
- NBDE Remembered 2 New YorkDocumento242 páginasNBDE Remembered 2 New YorkR MAinda não há avaliações
- Articol Parodontologie Parodontology Article English RomanianDocumento4 páginasArticol Parodontologie Parodontology Article English RomanianStefana NanuAinda não há avaliações
- Ulcerative Vesicular Bullous Lesions 2Documento30 páginasUlcerative Vesicular Bullous Lesions 2Mustafa AliAinda não há avaliações
- Corpsman Pt3Documento266 páginasCorpsman Pt3DonT_RN100% (1)
- Final PresentationDocumento14 páginasFinal PresentationMarilynAinda não há avaliações